Ultrasound
1/63
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
64 Terms
how can ultrasound cause different therapeutic effects?
can use continuous energy stream which creates a thermal effect, and pulsed which is a non-thermal application
what temperature must be reached to have the miniaml therapeutic effect?
104 F
what is the tissue response to thermal effects of ultrasound?
collagen extensibility, increase circulation and enzyme activity, decrease muscle spasm, decreased pain, there will be a mild inflammatory response
how does ultrasound create heat generally?
ultrasound causes molecular motion, motion causes friction between particles, friction causes heat
what are the non-thermal effects of ultrasound?
promotes cell function and tissue healing: cell membrane permeability, exchange of metabolites, edema reabsorbed, fibroblast activity and collagen repair, tissue regeneration (bone healing), and circulation
what phase might non-thermal ultrasound be used in?
acute or subacute in which inflammation is still present
how does ultrasound work?
works by emitting high-frequency sound waves that penetrate tissues. These sound waves create mechanical vibrations, leading to both thermal and non-thermal effects in the targeted area.
what is the frequency of therapeutic and diagnostic ultrasound?
therapeutic is around 5.5 mHz, and diagnostic around 16 MHz
what is rarefaction?
lessening of density of a material, opposition of compression (sound is a compression-rarefaction wave)
what does it means when ultrasound wave beams attenuate?
refers to the reduction in intensity and amplitude (reflected/deflected, refracted, or absorbed) of ultrasound wave beams as they pass through tissues, different mediums attenuate more or less
what occurs when the wave beam reaches its target?
only 50% is absorbed, and the rest is reflected/deflected or refracted (bent)
when would be see more attentuation?
higher frequency of US or higher tissue collagen content (bone highest level and blood lowest)
what is acoustic impedance?
how easy/difficult sound waves move through a medium, is based on the absorption coefficient
when might refraction be decreased?
when crossing between tissues with similar acoustic impedances
describe reflection/deflection
Reflection occurs when sound waves bounce off a boundary between different media, while deflection refers to the change in direction of sound waves as they pass through different tissues or interfaces.
how much reflection/deflection occurs between gel and skin, or skin and fat, or fat and muscle, or muscles and bone?
0.1% between gel and skin, 0.9% between skin and fat, 0.8% between fat and muscle, and approx 34% between muscle and bone
what does the sound head contain?
the piezoelectric crystal, which converts mechanical to/from electrical signals, the electricity causes teh crystal to resonate (vibrate)
what is the reverse piezoelectric effect?
the crystal expands and contracts, which produces compression and rarefraction (causing the sound waves)
what are the two main properties of a sound wave?
frequency and amplitude
what is the frequency?
how many cycles of waves per time, heard as pitch of a sound
what is amplitude?
how big the waves are, heard as volume
what frequency produces heat production superficially (0.8-1.6 cm deep)?
3 MHz
what frequency produces deeper attenuation (up to 5 cm)?
1 MHz
what spatial average intensity should be used for 1 MHz vs 3 Mhz (which is the power per unit area)?
1.5 - 2.0 W/cm2 and 0.5 W/cm2 respectively
what is the beam nonuniformity ratio (BNR)?
ratio of spatial peak intensity to spatial average intensity. The low the value, the more uniform the energy distribution, and the less risk of tissue damage. Should be between 2:1 and 6:1
what is the duty cycle?
the fraction of time the US energy is on over one pulse period (time on + time off)
what is frequency?
the rate of compression-rarefaction cycles, or the number of wave cycles per unit time (1 Mhz = 1 million cycles per second)
how is the depth of transmission related to frequency?
inverserely related (1 Mhz is deep, 3 Mhz is superficial)
what is the intensity?
aka the amplitude, the amount of power per unit area.
what intensity should be used for thermal effects?
for 1 Mhz 1.5-2.0 W/cm2 and for 3 Mhz 0.5 W/cm2 (superficial bone with require lower intensity, and should adjust up or down based on patient reports)
what intensity should be used for non-thermal effects?
0.5-1.0 W/cm2 in general, and 0.15 W/cm2 for bone healing (don’t go so high with bone such that is a deep ache, that is a bad sign)
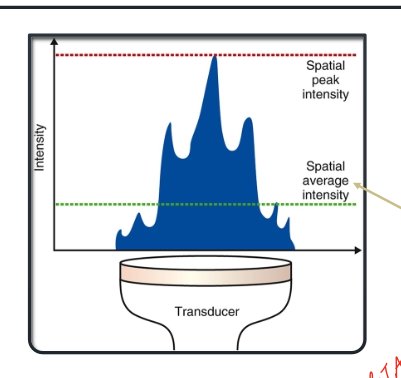
since intensity is not uniform across the transduces in teh near field (as in there is a higher spatial peak intensity than the spatial average intensity, see image), what does that mean for us clinically?
we need to KEEP the sound head MOVING and with constant contact with the skin
what duty cycle should be used for non-thermal effects?
pulsed less than or equal to 20%, this allows time for the heat to disperse
what duty cycle should be used for thermal effects?
continuous, larger duty cycle
what is the equation for duty cycle?
Duty Cycle = (pulse on x 100)/(pulse on + pulse off)
what is the effective radiating area?
the area of the transducer that emits ultrasound energy effectively. It is typically less than the total size of the transducer face and is crucial for determining the intensity of ultrasound delivered to the tissue.
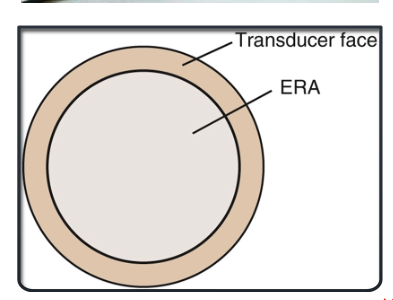
what is the general guideline for selecting a transducers based on the treatment area size?
the treatment are should be about x2 the ERA in 5-10 minutes
what is the general duration that should be used for US treatment?
5-10 minutes for treatment area, may need to increase for larger SA decrease for smaller SA, or if the frequency/intensity is lower or higher
does the speed of the transducer alter temperature affects?
no
what affects tissues temp when using continuous ultrasound?
absorption coefficient (type of tissue/more collagen), intensity, frequency, duration of treatment
what are the additional non-thermal effects of ultrasound?
cavitation, acoustic streaming, microstreaming
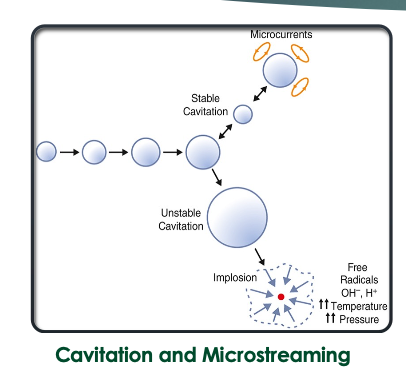
what is cavitation?
formation, growth, and pulsation of gas bubbles in fluids, stable is ok as they just oscillate, and unstable is bad bc they can growth and burst
what is acoustic streaming?
the circular flow of cellular fluids on a large scale
what is microstreaming?
micro fluid current formed around oscillating bubbles, can become harmful energy buildup due to not moving the sound head, rapid volume changes, high temp, and tissue damage
list the temp increase goal and clinical application of non-thermal US
none to 0 degreees celcius (37.5C baseline temp), used for acute injury, edema, healing/inflammation
list the temp increase goal and clinical application of mild thermal US
+1C, used for subacute injury, hematoma
list the temp increase goal and clinical application of moderate thermal US
+2 C, used for chronic inflammation, pain, trigger points
list the temp increase goal and clinical application of vigorous thermal US
+4 C, stretch collagen
what is phonophoresis?
a therapeutic technique that uses ultrasound to enhance the delivery of medications through the skin. works in theory by cavitation increasing the stratum corneum permeability, which allows drugs to move more easily through the skin by diffusion. initially there will be high concentration at the delivery site, then picked up by the circulation, problems with precision of medication dose
how are the parameters for phonophoresis?
massage the drug into the skin, sonate with 20% PUS, 3 MHz, 0.5-1.0 W/cm2, 5-10 minutes
what is the most common transdermal medication you might see?
dexamethasone (which is for inflammation and is a synthetic steroidal anti-inflammatory), also lidocaine is common
what is the evidence like for phonophoresis?
strong anecdotal reports and good basic research, but systematic reviews of clinical evidence no supportive of the basic evidence, poor research quality
what are the contraindications of US?
malignancy, pregnancy, CNS tissues, joint cement and plastics, pacemaker or other implanted device, thrombophlebitis, eyes and reproductive organs
what are precautions of US?
acute inflammation, epiphyseal plates, fractures, breast implants, areas of reduced sensation or circulation
what are adverse effects of US?
burns, standing waves, cross-contamination/infection, pain is NOT a normal response (if fracture present will feel sharp pain, overheating the periosteum will feel a deep ache)
what occurs due to dense reflection at the tissue boundaries with high acoustic impedance (ie bone, tendon)?
the reflected wave will summate with teh transducer wave, which leads to a larger wave intensity, and potential tissue damage, so KEEP ER MOVING
what other modalities can be used with US?
superficial heat can be used before to decrease time needed to heat the deeper tissues
e-stim in combination, this may decrease muscle spasm or reduce trigger point irritability, tho research support is poor
what is the general technique for US application?
eval the pt and determine is US appropriate
screen for contraindications/precautions
expose and drape
apply the transmission medium
select the sound head
select the parameters
apply the sound head to the medium and begin moving the sound head
then push start button
keep the head moving
reassess the patient
document
what is the stroking technique for US?
treatment area should be 1.5-4x the ERA, make sure to couple the medium layer, no air bubbles. keep the sound head in full contact to surface, and keep it moving (rate of movement doesn’t matter)
when should effects be seen for US?
should reassess for immediate response but most effects won’t be immediate and will be observed in 1-3 treatments for most
what should be documented about US?
area treated, US frequency, intensity, duty cycle, duration, if underwater or other non-gel method, sequence within the treatment if paired with another intervention, response to intervention
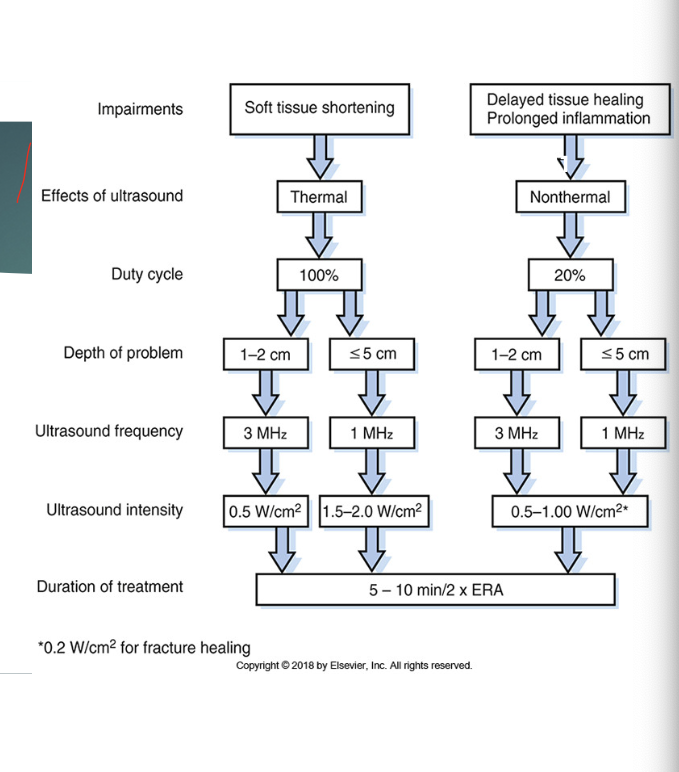
graphic for clinical decision making with US
see image