Diversity of parasitic life cycles
1/67
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
68 Terms
Parasite
Living organism dependen of another organism named host
Dependence can be transitory or definitive during the parasite life
Anthroponosis
Parasites only infect humans
Zoonosis
When animal parasites infect humans
Parasitism
Nutrient spoliation of the host towards the parasite
Unilateral physiological dependence
Parasite only gets the profit
Symbiosis
Mutual benefits
Parasite positions
Taxonomic positions: belong to eukaryotes
Anatomic location (ecto or endo parasites)
Protists
Unicellular eukaryotic cells
Helminths
Pluricellular eukaryotes → worms
Eumycytes
Fungi → eukaryotes uni or pluricellular
Ectoparasites
On the host surface → provokes inconvenience (itching): lices
Dwell in teguments → diseases: sarcoptic mange
Endoparasites
Different locations within the host:
Cavities: intestine (taenia)
Blood vessels (schistosomes)
Muscular tissue (trichinella)
Specific cells: erythrocyte (plasmodium), macrophage (leishmania)
Accidental parisitism
Fly larva within a wound
Optional parasitism
Normally saprophytes in the natural under certain conditions → parasites (fungi)
Obligatory parasistism
Temporary: part of its life as a parasite and part as free-living organism (fasciola → liver fluke, strongyloides → anguillulosis)
Permanent: parasite life in one or several hosts (filaria, plasmodium)
Erratic parasitism
Parasite in an unusual host (canin ascaris getting lost in human → larva migrans syndrome)
Parasite specificity
Degree of fidelity between parasite an hosts (stenoxenic or euryxenic)
Stenoxenic parasites
High fidelity degree to a host, only infects species hosts of taxonomically close to each other (plasmodium, anopheles sp.)
Euryxenic
Low fidelity degree to a host (trypanosoma brucei rhodesiense → in human and mammals)
Host
Living organism which harbours a pathogenic agent (parasite)
Final host
Host harbouring the sexual or adult form of the parasite
Intermediate host (IH)
Harbouring the asexual or larval form of the parasite
The parasite should stay within the host
Necessary to get transformations into the inefective form exhibiting contamination habilities
Passive intermediate host
When it harbours the ineffective form without performing any movement to get it or transmit it (molluscus for schistosomes)
Active intermediate host
Vector → when it carries and inoculates the inefective form of the parasite (anopheles sp. for plasmodium, sandflies for leishmania sp.)
Obligate host
When the parasite transforms/matures within a host
Facultative host
Optional host when there is no parasite transformation → paratenic host
Vector
Host for a pathogen and able to transmit it actively to another organism
Hematophagous insect (arthropod) collecting the parasite in infected patients/animals, keeping it, carrying it, and inoculate it in naive patients/animals
Biological vectors
Ensure the parasite maturation or multiplication, essential to the parasite life cycle as an intermediate host (anopheles mosquito → malaria vector). Parasite transformation
Mechanical vectors
Only a role of parasite transport, no necessary to the life cycle (housefly carrying amoebal cysts). No transformation
Parasite reservoir
Animal, plant, or external environment ensuring the parasite's survival, making it available for the different hosts of the life cycle (sheep → parasite reservoir of the liver fluke)
Human parasite reservoir
When infection is strictly human, humans are reservoir (anthroponosis)
Accidental host
Some pathogens carried by animals can be transferred accidentally to humans, minor epidemiologic role (human trichinellosis and hydatidosis) → parasitic dead ends
Animal parasite reservoir
Infection is common to humans and animals
Animals are reservoir promoting transmission to humans, good tolerance and low clinical manifestations
Land based parasite rervoir
Soil, release through feces → intestinal parasite (cyst of amoeba/giardia, eggs of helminths, fungi)
Life cycle
Sequence of mandatory transformations occurring in a precise order for a parasite to get the next parasite generation
Monoxenic life cycle
Direct cycle. Parasite evolution takes place within the same host or partially in external environment, only 1 host
Short direct cycle
Eggs or larvae are directly infectious without necessity of passage within the external environment
Long direct cycle
Eggs or larvae should follow a development in external environment under specific conditions to become infectious
Heteroxenous life cycle
Indirect cycle. Parasite transformation take place in several successive hosts
Polyembryonny
Two or more embryos developing from a single fertilized egg (trematodes)
Forms of resistance
Eggs (worms)
Encysted larvae (nematodes, trematodes)
Cysts (protists)
Types of worms
Nematodes: round
Cestodes: flat, segmented
Trematodes: flat, unsegmented
Quiescent eggs
Require maturation in the environment, not directly infectious (ascaris lumbricoides)
Embryonated eggs
Infectious as soon as eliminated in the stools (enterobius vermicularis)
Encysted larvae
Resealed, larvae mobile encyst and attach, infectious when ingested (metacercarie of liver fluke)
Cysts
Cysts of resistance (entamoeba histolytica)
Vegetative or division cysts: involved in the parasite's life cycle and reproduction
Plasmodium sp.: gametocyte, which undergoes gametogenesis and fertilization.
Toxoplasma:
Forms oocysts that are released into the environment, acting like an "encapsulated egg." Oocysts contain two smaller sacs called sporocysts, and each sporocyst contains four infective sporozoites.
Can also form tissue cysts in the brain that contain slow-growing forms called bradyzoites
Spores (microsporidiae)
Modes of transmission
oral route
muco-cutaneous route
respiratory route
vectorial origin
sexual route
congenital route
transfusion route
transplantation
Oral transmission
By external environment through contaminated water and food
Oral transmission of monoxenous protists via contaminated food and water
Entamoeba hystolytica (amoebosis)
Giardia intestinalis (giardiasis)
Cryptosporidium parvum (cryptosporidiosis)
Enterocytozoon bieneusi (microsporidiosis)
Cyclospora cayetanensis (cyclosporosis)
Isospora belli (isosporose)
Giardiasis
Giardia intestinalis, lamblia or duodenalis
Ingestion of mature cysts in water and food
Diarrhea
Oral transmission
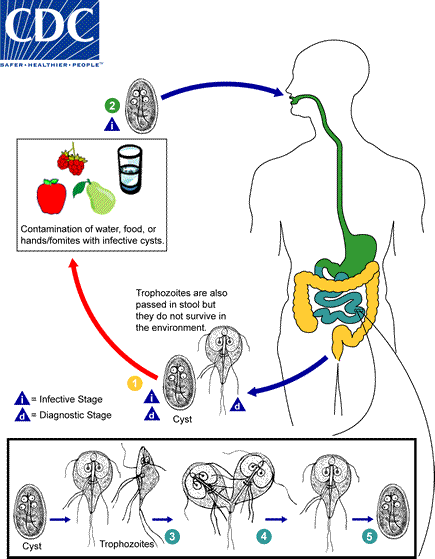
Oral transmission of monoxenous helminths via contaminated food and water
Ascaris lumbricoides (ascaridiosis)
Enterobius vermicularis (oxyurosis)
Toxocara canis (toxocariasis) → human paratenic host
Trichuris trichiura (trichocephalosis)
Oral transmission of heteroxenous helminths via contaminated food and water
Hymenolepis nana (hymenolepiasis)
Echinococcus granulosus (hydatidosis) → human dead-end host
Oral transmission of heteroxenous helminths via contact with animals or plant supports
Toxoplasma gondii (toxoplasmosis)
Angiostrongylus cantonensis (angiostrongylosis) → human accidental host
Toxoplasmosis
Toxoplasma gondii
Heteroxenous life cycle
Human contamination:
Eating uncooked meat
Blood transfusion and organ transplant
Congenital (mother-child)
Able to penetrate nervous and muscular tissues
The cat is the definitive host
Zoonotic disease
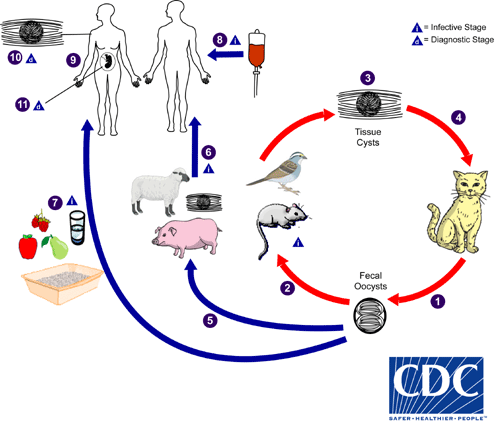
Oral transmission through cyclops
Dracunculus medinensis (dracunculosis)
Passive aquatic intermediate host
Worm lysis can cause alergia if not extracted completely
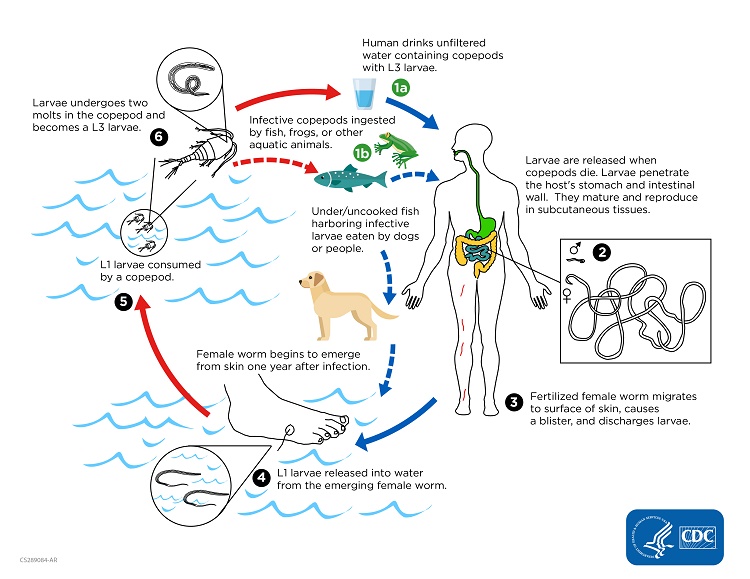
Muco-cutaneous transmission through water and moist soil
Strongyloides stercoralis (strongyloidiasis)
Intestinal hookworm (ancylostomiasis)
Schistosoma spp. (schistomiasis)
Larva migrans → human dead end host
Intestinal hookworm
Ancylostoma duodenale
Humans are the principal host
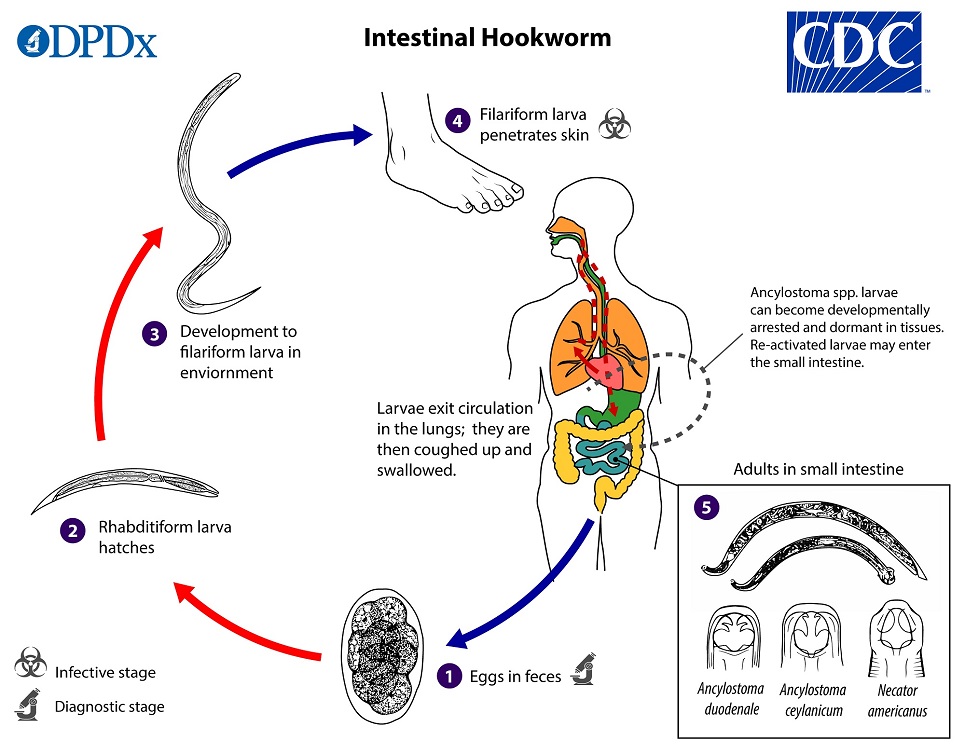
Muco-cutaneous transmission through dry environment
Dermatobia hominis (myiases)
Tunga penetrans (tungiasis)
Muco-cutaneous transmission through human contact
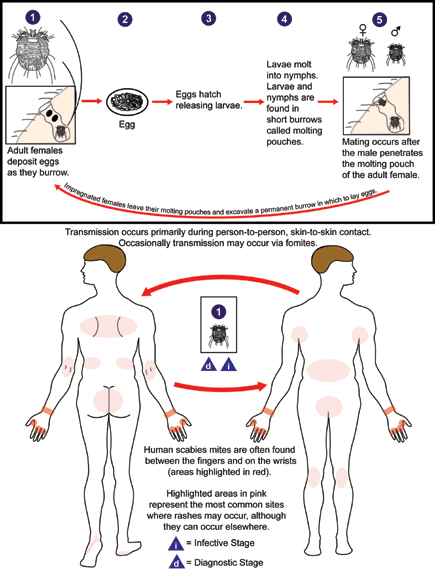
Saecoptes scabiei (scabies)
Contagious dermatitis
Sexually transmitted
Sick person or asymptomatic carrier
Vector-borne transmission by flying evening and night insect vectors
Malaria (anopheles)
Leishmaniases (sandflies)
Lymphatic filariases (culex, anopheles, aedes, mansonia)
Vector-borne transmission by flying diurnal insect vectors
Trypanosomiases (Tse-tse fly)
Loasis (Chrysops)
Onchocercosis (Blackflies)
Mansonellosis (Culicoides)
Vector-borne transmission by terrestial insect vectors
Chagas disease (bug)
Babesiosis (tick)
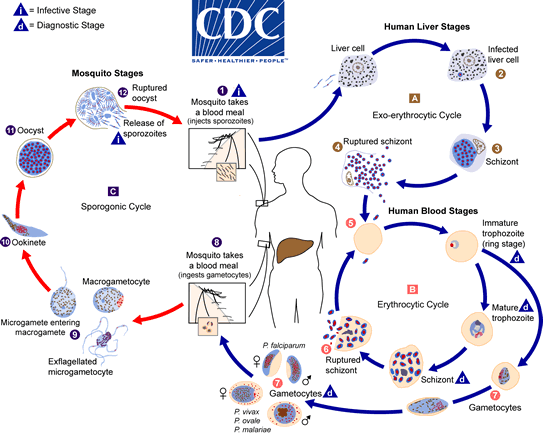
Malaria
Plasmodium vivax
Heteroxenous life cycle
Cyclic fever, anemia
Provoked by protists
Congenital transmission, blood transfusion
Humans are the intermediate host
Airborne transmission
Pneumocystis jirovecii (fungi)
Sexual transmission
Uro-genital trichomoniasis
Human final host
Taenia saginata (taeniasis)
Human secondary host
Dipylidium caninum