Final Exam Study Guide Adult II
1/202
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
203 Terms
From memory, go through the tracheostomy care validation
Validation Steps
|
PRIOR TO ENERING THE ROOM |
Check the medical order. |
Gather supplies: PPE, trach care kit, oxygen equipment, ambu-bag, pulse oximeter (suction canister, and connecting tubing, if not in room). |
UPON ENTERING THE ROOM (PRE-PROCEDURE) |
Pre-Procedure routine (Sandwich!) |
DURING PROCEDURE (INTRA-PROCEDURE) |
Raise the HOB to semi-Fowler’s (30-45 degrees) if conscious and drape the chest with chux pad or towel. |
Adjust the bed to a comfortable working height. |
Lower the side rail. |
Place pulse oximeter on client. |
Prepare supplemental oxygen, ambu-bag, and suction canister with tubing. |
Check suction equipment. Occlude suction tubing on continuous suction and ensure it is at 100-120 mm Hg. |
Open sterile tracheostomy kit, sterile catheter package, and open normal saline solution. |
Don sterile gloves. |
Place sterile drape on overbed table. |
Place items from sterile container onto sterile field. |
Pour sterile saline into 3-4 of the trays/suction cup with non-dominant hand or assistant may pour. |
Pick up sterile catheter with dominant hand wrapping tube around hand, pick up connective suction tubing with non-dominant hand and connect the two together. |
Moisten catheter in sterile saline with dominant hand then occlude suction port with non-dominant hand to check suction in chamber #1. |
Use non-dominant hand to hyperventilate client (3 squeezes of ambu-bag) or assistant may bag. Check pulse ox. |
Advance suction catheter with dominant hand to cough reflex (4-5 inches or 10-11 cm). DO NOT SUCTION WHILE INSERTING CATHETER. |
Apply suction intermittently with non-dominant thumb and rotate while being withdrawn. DO not suction more than 10-15 seconds at a time. |
Hyperventilate client (3 squeezes of ambu-bag) with non-dominant hand or assistant may perform and replace O2 collar. |
Ask client to take several deep breaths and cough. |
Verbalize to instructor: may suction up to 3 times allowing 30 seconds to 1 minute between each time. |
Flush catheter in saline between suctioning in chamber #1. |
Suction oropharynx. Do not reinsert catheter into trachea after suctioning the mouth. |
Disconnect suction tubing from catheter with non-dominant hand and dispose of catheter. Have assistant turn off suction. |
Remove O2 collar with non-dominant hand, have assistant stabilize faceplate. Remove inner cannula with non-dominant hand and place in sterile saline in chamber #2. |
Have assistant replace O2 collar over outer cannula. |
Clean inner cannula with brush keeping dominant hand sterile. |
Place cannula in clean sterile saline chamber #3 with non-dominant hand to rinse. Remove cannula with dominant hand and tap dry on sterile field. |
Reinsert inner cannula with dominant hand using non-dominant hand to stabilize faceplate. Sterility is complete. |
Remove soiled trach dressing and discard in trash. If no assistant available to help leave old ties/Velcro in place. |
Assess skin integrity around stoma. |
Dip a cotton swab into sterile saline in chamber #3 and clean around stoma under faceplate. Use applicator only once per area, moving from stoma outward. |
Pat skin dry with sterile gauze. |
Apply fenestrated 4x4 under faceplate with help of assistant to keep faceplate stable. |
Remove trach ties while stabilizing faceplate. |
Assess skin on the back of the neck. Clean back of neck with sterile gauze dipped in chamber #3 if needed. |
Have assistant hold faceplate in place and apply clean trach holder with a new Velcro holder/tie. |
Replace O2. |
Dispose of items used for procedure. |
Remove pulse oximeter (do not throw away) |
Educated client · trach care performed, · do not pull-on trach · can cough secretions into suction catheter or tissues/gauze · notify if feeling short of breath |
Post-Procedure routine (Sandwich!) |
Verbalize documentation · size ___ French suction catheter · how many times suctioned (1, 2, or 3) · color, clarity, consistency, and amount (scant, small, moderate, large, copious) of secretions · sterile trach care performed · skin integrity around stoma and back of the neck · drainage around stoma and on dressing (sanguineous, serosanguineous, serous, purulent) · oxygen saturation and pulse rate throughout the procedure · how client tolerated procedure (pain level, before, during, after procedure) · client educated and verbalized understanding of education |
What is epistaxis?
What is the cause?
Epistaxis: Hemorrhage from the nose (nosebleed); common problem
Cause:
Caused by the rupture of distended blood vessels (capillaries) in the mucous membranes of the nares (usually in the anterior septum area)
List risk factors for epistaxis.
Use of Aspirin/NSAIDs
Local infections (vestibulitis, rhinitis, rhinosinusitis)
Systemic infections (scarlet fever, malaria)
Drying of nasal mucous membranes
Nasal inhalation of corticosteroids (e.g., beclomethasone) or illicit drugs (e.g., cocaine)
Trauma (digital trauma, blunt trauma, fracture, forceful nose blowing)
Arteriosclerosis
Hypertension
Tumor (sinus or nasopharynx)
Thrombocytopenia
Liver disease
Rendu–Osler–Weber syndrome (hereditary hemorrhagic telangiectasia)
What does tx for epistaxis depend on?
What does the initial tx consist of?
The tx depends on the cause and location of the bleeding site
Initial Tx
Initial treatment usually involves applying direct pressure to the affected nare
During a nosebleed occurrence, the patient is instructed to sit upright; tilt the head forward (so will not swallow or aspirate blood); and pinch the soft outer portion of the nose against the midline septum for 5-10 minutes
What pharmacologic intervention might be used to tx epistaxis?
A nasal decongestant (Phenylephrine) may be used as a vasoconstrictor to aid in stopping the bleeding
If pressure application and a nasal decongestant (phenylephrine) do not stop epistaxis, what interventions might be next?
The nose is examined, suctioned, and the bleeding site(s) are cauterized with silver nitrate or electrocautery
Can also use a Surgicel or Gelfoam patch; a cotton tampon; or a nasal sponge tamponade (contains an agent to promote blood clotting)
What txs can be performed if epistaxis does not stop and the site of bleeding cannot be identified?
The nose can be packed with petroleum gauze or gauze with antibiotic ointment (excessive petroleum jelly into the lungs can cause increased risk for pneumonia)
—>—>A topical anesthetic spray and decongestant may be used before the packing gauze is inserted
Another option of treatment: A balloon-inflated catheter in the affected nare (nasal tamponade)
—>—>Tubes or packing usually removed after 1-3 days
List options for the nursing management of epistaxis.
Continuously assesses airway and breathing (observe for respiratory distress, tolerance of packing/tubes)
Monitor vital signs
Assist with procedures
Provide the patient with tissues and an emesis basin (so patient can blow nose/spit out blood)
Control patient’s anxiety
Humidity, oxygen, bedrest, and/or antibiotics may be prescribed
Once bleeding is controlled, instruct patient to avoid vigorous exercise, hot/spicy foods, tobacco (may cause vasodilation)
Educate the patient on ways to prevent epistaxis (avoid forceful nose blowing, straining, high altitudes, nasal trauma)
Educate patient how to apply direct pressure in case of another nosebleed
Instruct the patient to get medical attention if the nosebleed cannot be stopped
What is glaucoma?
Glaucoma is characterized as a group of ocular conditions where the IOP is elevated; it is an age-related eye disease
What IOP is normal? What if IOP is higher than this range?
Normal IOP is 10-21 mmHg, higher than that = glaucoma
What causes the increased IOP in glaucoma?
Increased IOP results from inadequate drainage of aqueous humor from the canal of Schlemm or overproduction of aqueous humor
In what age group does glaucoma mostly occur in?
This disease occurs mostly in people older than 40
List risk factors for glaucoma
Black or Asian race
Cardiovascular disease
Diabetes
Family history of glaucoma
Migraine syndromes
Myopia (nearsightedness)
Obstructive sleep apnea
Older age
Previous eye trauma
Prolonged use of topical or systemic corticosteroids
Thin cornea
What are the 3 types of glaucoma?
Wide-angle glaucoma (POAG = primary open-angle glaucoma)
Narrow-angle glaucoma (PACG = primary angle closure glaucoma)
Congenital glaucoma
What causes wide angle glaucoma (POAG)?
POAG results from obstruction of the outflow of aqueous humor into the trabecular meshwork = buildup of aqueous humor = increased IOP
Causes:
Hereditary factors
Aging
List late-stage manifestations of wide-angle glaucoma (POAG)
Visual field defects
Possible ocular pain
HAs
List characteristics of wide-angle glaucoma (POAG).
It is the most common type of glaucoma
It usually affects both eyes and has no manifestations in the early stages
In POAG, the anterior chamber angle is open and appears normal
Develops slowly, so tx is not as aggressive
In open-angle glaucoma, the tonometry reading is between 22-32 mmHg.
Considered the “silent thief of sight” b/c most patients are unaware that they have the disease until they have experienced visual changes and vision loss
→—>The patient may not make an appointment with their doctor/NP until they experience blurred vision or “halos” around lights, difficulty focusing, difficulty adjusting eyes in low lighting, loss of peripheral vision, aching or discomfort around the eyes, and/or headaches
How does wide-angle glaucoma (POAG) present?
Usually bilateral, but one eye may be more severely affected than the other
in wide-angle glaucoma, the anterior chamber angle is open and appears normal
Slow development
What occurs in narrow-angle glaucoma (PACG = primary angle closure glaucoma)?
The aqueous humor encounters resistance to flow through the pupil due to complete or partial closure of the anterior chamber angle
How does narrow-angle glaucoma (PACG) manifest, and what is it considered?
Has a sudden onset and is an emergency→requires immediate treatment
List clinical manifestations of narrow-angle glaucoma (PACG).
Manifestations include:
→Rapidly progressive visual impairment
→Periocular pain
→Congestion
→Transient blurring of vision (Refers to a temporary, sudden, and brief [seconds to minutes] loss of clear eyesight in one or both eyes, often described as a "curtain" descending, dimming, or fogginess, followed by full recovery)
→Reduced central vision
—>Rapid rise in IOP (like from 20 to 30) and/or tonometry reading of 30mmHg or higher
List potential causes of narrow-angle glaucoma (PACG).
Lens or pupil dilation from medications
Sympathetic stimulation
What is tonometry?
Used to measure the IOP
Give an example of IOP change that indicates PACG vs POAG
A sudden jump in IOP from 21 to 30 = PACG
Versus
A gradual rise for POAG, such as 21 to 22 b/t appointments
List tests used to diagnose and monitor glaucoma.
Tonometry
Central visual field testing
Gonioscopy
Optic nerve imaging (ophthalmoscopy)
What is gonioscopy used for w/ glaucoma?
Gonioscopy visualizes the anterior chamber angle to assess fluid drainage to determine whether the angle is open or closed (so diagnosing POAG vs PACG)
What is ophthalmoscopy (optic nerve imaging) used for w/ glaucoma?
What abnormal findings might you see in glaucoma?
Ophthalmoscopy is used to inspect the optic nerve to determine the degree of nerve damage present in glaucoma
Abnormal findings that indicate glaucoma:
Pallor and cupping of the optic nerve disc
—>—>Cupping is the exaggerated bending of the blood vessels as they cross the optic disc
→—>Cupping progresses in glaucoma due to the gradual loss of retinal nerve fibers and the loss of blood supply
What is the goal of the management of glaucoma?
Prevent further optic nerve damage
What should patients be educated on about the pathology and treatment of glaucoma?
Glaucoma cannot be cured
—>—>This means lifelong tx therapy
List potential treatment measures for glaucoma
Pharmacologic therapy
Laser procedures
Surgery
Or a combination of these approaches (all of these measures have potential complications and side effects)
Why should nurses stress the importance of f/u appts on glaucoma to patients?
Healthcare professionals want to maintain the IOP within a range unlikely to cause further damage
What is the initial tx target for glaucoma patients?
The initial target for IOP is typically set at 30% lower than the current pressure
What are the preferred initial topical meds for glaucoma, and why?
Beta-blockers are the preferred initial topical medications because of their efficacy, minimal dosing (can be used once each day), and low cost
List the classes of glaucoma meds.
Cholinergics (i.e., miotics)
Beta-blockers
Alpha2-agonists (i.e., adrenergic agents)
Carbonic anhydrase inhibitors
Prostaglandin analogs
Hyperosmolar Agents/Osmotic Diuretics
What hyperosmolar agent/osmotic diuretic is more commonly used to tx glaucoma?
Mannitol (IV)—>draws water from ocular tissues into the bloodstream to be filtered out by the kidneys and urinated out, reducing vitreous fluid volume = decreases IOP
For alpha-adrenergic agonists used in the treatment of glaucoma, list example meds, potential side effects, and nursing implications for their use
Medications:
Brimonidine
Apraclonidine
Side effects
Eye redness
Dry mouth and nasal passages
Nursing Implications
Educate patients about punctal occlusion to limit systemic effects
For cholinergics (miotics) used in the treatment of glaucoma, list example meds, potential side effects, and nursing implications for their use
Medications:
Pilocarpine
Carbachol intraocular
Side effects
Periorbital pain
Blurry vision
Difficulty seeing in the dark
Nursing Implications
Caution patients about difficulty seeing in the dark
Pilocarpine can be stored at room temp for up to 8 wks
For beta-blockers used in the treatment of glaucoma, list example meds, potential side effects, and nursing implications for their use
Medications:
Timolol maleate
Side effects
Can have systemic effects (bradycardia, exacerbation of pulmonary disease b/c of bronchoconstriction, hypotension)
Nursing Implications
Contraindicated in patients with asthma, COPD, 2nd or 3rd degree heart block, brady cardia, or HF
Educate patients about punctal occlusion to limit systemic effects
For carbonic anhydrase inhibitors used in the treatment of glaucoma, list example meds, potential side effects, and nursing implications for their use
Medications:
Acetazolamide
Dorzolamide
Side effects
Oral meds (acetazolamide) are associated w/ serious side effects (anaphylactic reactions, electrolyte loss, depression lethargy, GI upset, impotence, and weight loss)
Topical form (dorzolamide) side effect = potential for topical allergy
Nursing Implications
Do not administer to patients with sulfa allergies
Monitor electrolyte levels
For prostaglandin analogues used in the treatment of glaucoma, list example meds, potential side effects, and nursing implications for their use
Medications:
Latanoprost
Bimatoprost
Side effects
Darkening of the iris
Conjunctival redness
Possible rash
Nursing Implications
Instruct patients to report any side effects
What is the priority nursing intervention for ocular meds?
Give examples.
The priority nursing intervention for ocular meds is education!
Examples:
Do not skip doses
Give medication on time
Wait 5-10 mins between most eye medications
How long must a patient wait b/t different eye drops being administered?
What about eye ointments?
Need to wait 3-5 minutes between eye drops if more than one med needs to be administered
Need to wait at least 10 minutes after eye drop administration to administer an eye ointment
What should patients w/ glaucoma be educated on?
Intraocular pressure measurements
Visual field tests
How eyedrops work
How to administer
Monitor for side effects
Compliance, timely dosing
How is acute angle-closure glaucoma (narrow-angle) treated?
This is an ocular emergency
Hyperosmotics (mannitol IV)
Acetazolamide
Topical ocular hypotensive agents
Possible laser iridotomy (incision in the iris) to release blocked aqueous and reduce IOP
Tx of the other unaffected eye w/ pilocarpine eye drops and/or surgical management to avoid a similar spontaneous attack
When is surgery used to manage glaucoma?
Surgical management of glaucoma is used for patients that are unresponsive to pharmacological treatment of increased IOP levels
List/describe the 4 types of surgeries used to tx glaucoma
Trabeculectomy surgery
—>—>Small incision into the eye to stabilize the optic nerve, restore the eye’s natural fluid balance, and minimize further visual field damage
Laser Trabeculoplasty
—>—>A laser beam is used to open the trabecular meshwork and widen the canal of Schlemm, which allows outflow of the aqueous humor and decreases the IOP
—>—>Contraindicated in patients with narrow-angle glaucoma because the trabecular meshwork is difficult to see
Peripheral (Laser) Iridotomy
—>—>Laser used to make an opening in the iris to eliminate the pupillary blockage
—>—>It is contraindicated in patients with corneal edema because the edema interferes with laser targeting and strength
Filtering Techniques
—>—>Various filtering surgical techniques can be used to create an opening where the aqueous humor can drain out of the anterior chamber while bypassing the usual drainage structures
What does retinal detachment involve?
Retinal detachment involves the separation of the two innermost layers of the retina from each other, the neurosensory area of the retina from the RPE (retinal pigment epithelium)
List risk factors for retinal detachment.
High myopia (near-sidedness)
Aphakia (absence of natural lenses) after cataract surgery
Trauma
Proliferative retinopathy (associated w/ diabetic patients)
Tension Forces
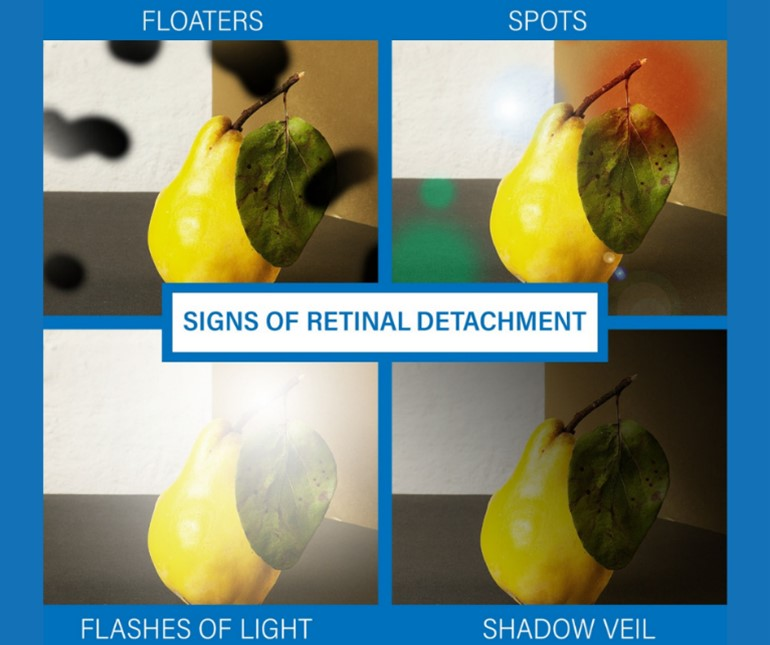
List the clinical manifestations of retinal detachment.
Sensation of a shade or curtain coming into the visual field
Seeing cobwebs
Bright flashing lights
“Floaters”
Typically painless b/c the retina lacks pain receptors
What diagnostic testing does a patient w/ potential retinal detachment require?
Require a dilated fundus examination with an indirect ophthalmoscope and a slit-lamp biomicroscopy
Optical coherence tomography (OCT) and ultrasound are used for a complete retinal detachment assessment, especially if the patient is suspected of having a cataract or vitreal hemorrhage
What non-surgical tx is used for retinal detachment? What is still required after this tx is performed?
Using cryotherapy, photocoagulation, or diathermy, an inflammatory response can be created to bind the retina and choroid together around the break
Surgical repair is still necessary to repair the detachment
How quickly do surgeries to manage retinal detachment need to be completed?
Retina detachment is a medical emergency and reattachment needs to occur the same day as the onset of sx to reduce the likelihood of permanent vision loss
List and describe the 2 common surgical interventions used for retinal detachment.
Scleral buckle
During scleral buckle surgery, the surgeon flattens and presses the sclera with a silicone band, called a buckle
This procedure brings the two retinal layers together and repairs the tear
Vitrectomy
—>—> A gas or oil bubble is placed to apply pressure and hold the retina in place to heal
—>—>If a gas bubble is used in the vitrectomy surgery, the patient has to stay in a prone position so the injected bubble can stay over the area of the detachment
Following surgery to fix a retinal detachment, what post-op instructions should the nurse educate the patient on?
Use of an eye patch and shield
If gas or oil has been placed, then the patient must be placed on his/her abdomen
→—>Lie with head turned so that the affected eye is facing up for several days
Nausea and pain are common post-surgery
Avoid activities that increase IOP→ Avoid lifting, pushing, or pulling objects heavier than 15 pounds
Avoid reading, writing, and close work in the first week after surgery
List signs/sx of post-op complications following a scleral buckle or vitrectomy
Inflammation of the eye
Cataracts
Infection
List the possible complications that can occur after a retinal detachment surgery
Increased IOP
Enopthalmitis (inflammation of the inner eye)
Another retinal detachment
Cataract development
Infection
What is one of the main signs of age-related macular degeneration (AMD)?
One of the main signs is tiny, yellowish spots known as “drusen” beneath the retina
It is normal for people older than 60 to have a small amount of drusen (clusters of debris or waste material) beneath the retina
The drusen become a problem when they are in the macular area of the eye, and they start to affect a person’s vision
What part of the vision does age-related macular degeneration (AMD) affect?
AMD affects central vision the most
Still have peripheral vision
These patients have a wide range of visual loss, but only a few have total blindness

List risk factors for age-related macular degeneration (AMD).
Older age
Family hx of macular degeneration
Smoking
Being Caucasian
HTN
Previous cataract surgery
Describe dry age-related macular degeneration (AMD).
Much more common than wet AMD
Dry AMD is non-neovascular and non-exudative
It is a condition in which the outer layers of the retina slowly break down, and drusen starts to form
If the drusen form outside of the macular area, the patient is asymptomatic
If the drusen forms within the macula, there is a gradual blurring of vision (especially when reading)
What is the treatment for dry age-related macular degeneration (AMD)?
There is no effective therapy for dry AMD
Describe wet age-related macular degeneration (AMD).
Wet AMD is neovascular and exudative
Wet AMD has an abrupt onset and is more damaging to the vision = much worse than dry AMD
Patients with wet AMD often see lines that are crooked or distorted and letters or words that are broken in appearance
With wet AMD, choroidal neovascularization occurs (where the blood vessels leak fluid and blood under the retina→which causes the retina to elevate and affect the vision)
What is the treatment for wet age-related macular degeneration (AMD)?
It can be treated by intravitreal injections of Ranibizumab (Lucentis) and/or Bevacizumab (Avastin), or with laser therapy to stop the leaking blood vessels
In the management of age-related macular degeneration (AMD), what is given to patients to take home and how are patients supposed to use them?
Amsler grids are given to patients to take home
—>—>They use these grids to test their sight and assess if their vision is getting worse (an early sign of AMD)
—>—>If the lines on the Amsler grid are wavy and not straight, they need to call their Dr. and get in immediately b/c either dry is getting worse or injections are not working for wet
Patients should use the grids several times a week (testing one eye at a time)
The patients are informed if the lines/images are distorted, faded, or harder to see, they need to contact their ophthalmologist
How is an otoscopic exam performed?
The pinna is grasped and pulled back to straighten the ear canal so the MD has a clear view of the canal and membrane
Describe a healthy tympanic membrane.
A healthy tympanic membrane is pearly gray, intact, and sits at the base of the ear canal
What is the snellen chart used for?
How are right eye, left eye, and both eyes documented in the chart?
Snellen chart: Is the standardized test for visual acuity (distance: 20 feet) performed on each eye
—>It determines the smallest letters a person can read on a standardized chart from a distance of 20 feet (6 meters)
For documentation:
Right eye (OD)
Left eye (OS)
Both eyes (OU)
What do the numbers mean on a Snellen chart score?
20/20 = normal vision
The first number is the testing distance (always 20 for 20ft)
The 2nd number is the distance at which a person with normal vision could read that line (so for 20/40 vision, a person with normal vision could read that line at 40ft while the person being tested can only read it at 20ft)
What visual acuity is legal blindness
Defined in the U.S. as a visual acuity of 20/200 or worse in the better eye with best correction
How are the 6 cardinal directions of gaze tested? What does checking this area of vision screen for?
The six cardinal directions of gaze: Up, down, left, right, and both diagonals
→Are tested by the patient following the examiner’s finger, a light, etc.
→The six directions of gaze test can screen for any ocular trauma, or neurologic disorders (such as stroke or myasthenia gravis)
What is a direct ophthalmoscopy? What is visualized on this diagnostic test?
Direct Ophthalmoscopy: Handheld instrument with various plus and minus lenses
Lenses can be rotated so examiner can closely view the cornea, lens, and retina
The eye’s fundus, optic nerve, and optic cup can also be visualized
How is a direct ophthalmoscopy performed?
Light is shone in the patient’s left or right eye as he/she gazes at a target
The patient is instructed to keep both eyes open during the examination
An examiner performing direct ophthalmoscopy sees intraretinal hemorrhages. What could this indicate?
HTN
An examiner performing direct ophthalmoscopy sees that the retina has a yellowish appearance. What could this indicate?
If the retina has a yellowish appearance, the patient may have hypercholesterolemia or diabetes
An examiner performing direct ophthalmoscopy sees Drusen. What could this indicate?
Drusen (small, hyaline, globular deposits under the retina area) found in the eye can indicate macular degeneration
What is indirect ophthalmoscopy?
The use of an instrument with a bright and intense light attached to a pair of binocular lenses attached to the examiners head to see the retina w/o magnification
What is slit-lamp examination?
The use of a mounted binocular microscope to magnify the anterior eye structures to identify any abnormality in the cornea, lens, anterior chamber, fundus, or anterior vitreous humor
Can see 10-40 times the real image
Can be used to evaluate patients for cataracts
What does tonometry measure? What is it used for?
Measures intraocular pressure = the pressure used to flatten the cornea (10-20 mmHg is normal)
Can be used to screen for and manage glaucoma
What is typically done before a tonometry test and why?
The tonometry probe touches the cornea (which is sensitive), so a topical anesthetic is usually given before the measurement is done
What should the nurse instruct the patient to avoid while getting an IOP measurement done?
Squeezing the eyelids
Holding their breath
Performing a Valsalva maneuver
Doing any other action that could increase the eye’s IOP
How is color vision checked?
Polychromatic plates can be utilized to establish whether a person’s color vision is within normal range
What is an Amsler grid?
How is an Amsler grid used?
Amsler Grid: A test used for patients with possible macular problems (macular degeneration)
How is an Amsler grid used?
The test uses a geometric grid of identical squares with a central fixation area to test the patient’s vision
The eyes are tested one at a time
What result on the Amsler grid indicates macular problems (macular degeneration)?
Patients with macular problems complain of the squares looking faded or of seeing wavy lanes
What is ultrasonography used for regarding the eyes?
Ultrasonography is used for assessing the orbit and eye for trauma, intraorbital tumors, proptosis (protrusion of the eyeball), and choroidal or retinal detachments
What is angiography used for regarding the eyes?
Used to evaluate macular edema, macular capillary non-perfusion, retinal and choroidal neovascularization (growth of abnormal new blood vessels) which occurs in acute macular degeneration
What tests should be done before angiography?
What is recommended for patients?
What are patients given 1 hour before the angiography?
Before these tests, BUN and Creatinine should be checked to ensure the kidneys can excrete the dye
The patient is encouraged to drink clear liquids up until the exam time, so that he/she is well hydrated
The patient is also given mydriatic drops one hour before the procedure to dilate the pupils
What instructions should be given to the patients prior to angiography?
The patients have to remain immobile during this test, and they are informed that they will feel a brief feeling of warmth in the face, behind the eyes, or in the jaw, teeth, tongue, and lips area
→—>These patients also complain of having a metallic taste in the mouth
The dye may cause skin to be yellow or gold for a few hours (up to 24 hours) and turn urine green, deep yellow, or orange
What is a side effect of indocyanine green used for angiography of the eyes?
When is it contraindicated?
Indocyanine green has side effects of nausea and/or vomiting
Patients allergic to iodine cannot have this dye injected
What is perimetry testing, and what does perimetry testing identify/assess for?
Evaluates the field of vision
This test helps identify which parts of the patient’s central and peripheral visual fields have accurate vision
It assesses for blindness or partially blind visual fields in patients with glaucoma, macular degeneration, or retinitis pigmentosa
How is a whisper test performed, and why is it performed?
How:
Ask the patient to block one external ear canal, while you stand 1-2 feet away and whisper a statement
The patient is then asked to repeat the whispered statement
Why:
Each ear is tested separately to assess high-frequency hearing acuity to detect potential hearing impairment
What are the two tuning fork tests?
Weber test
Rinne test
Weber test
What does this test for?
Describe the procedure
Describe normal results
Describe results that indicate conductive loss w/ an example
Describe results that indicate sensorineural loss w/an example
This test is used to detect unilateral hearing loss
Procedure: Place a vibrating tuning fork stem in the middle of the patient’s head, at midline of the forehead, or above the upper lip over the teeth, and ask whether the sound is heard equally in both ears (normal)
Results
Normal: Sound is heard equally in both ears
Conductive Loss: Sound lateralizes to the affected ear (louder on the side of damage)
→ So if the patient has bone conductive hearing loss, they hear the sound better in the affected (damaged) ear
→Ex: If a person has wax buildup in their right ear, that is “conductive hearing loss”, and they would hear the sound louder in the right ear
Sensorineural Loss: Sound lateralizes to the unaffected (better) ear
→ So if the patient has sensorineural loss (like from cochlear or vestibulocochlear nerve damage), the patient will hear the sound in the unaffected (better) ear, so if the nerve damage is to the right ear, they will hear better in their left ear
Rinne test
What is the Rinne test?
Describe its procedure
What can this test tell you?
Describe the results of a patient with normal hearing
Describe the results of a patient with conductive hearing loss
Describe the results of a patient with sensorineural hearing loss
Uses air conduction (AC) and bone conduction (BC) to test for sound (compares air conduction of sound to bone conduction of sound)
Procedure: Alternate a vibrating tuning fork stem between two positions (2 inches from the opening of the ear canal to test for air conduction) and against the mastoid bone (to test for bone conduction)
→—>The patient is asked as the positions are alternated to let the MD/NP know which tone is louder or when the tones (from air or bone conduction) are no longer audible
This test can be used to tell if the patient has conductive or sensorineural hearing loss
A patient with normal hearing should state that the air conduction sounds are louder than the bone conduction sounds in both ears
A patient with conductive hearing loss hears bone-conducted sound as long or longer than air-conducted sound
A patient with sensorineural hearing loss hears air-conducted sounds longer in the affected ear
What is audiometry?
Who performs audiometry?
During audiometry tests, what parts of hearing are evaluated?
Audiometry: The single most important diagnostic instrument for assessing patients for hearing disorders
Performed by an audiologist
During these tests, three parts of hearing are evaluated:
Frequency
Pitch
Intensity
What is the unit for measuring hearing loss and loudness/intensity of sound?
What is normal hearing?
The unit for measuring hearing loss and loudness or intensity of sound: Decibel
→Normal hearing is 0-15 decibels
Describe what happens during an audiometry exam
During an audiometry exam, the patient wears earphones and raises his/her hand as he/she hears a tone in the earphone
→The responses are plotted on an audiogram (graph)
What does a tympanogram assess for?
What is it used for?
Assesses the mobility of the eardrum and structures of the middle ear by changing air pressure in the ear canal
Used for middle ear problems (is impaired with middle ear disease)
List the 3 types of hearing loss
Conductive
Sensorineural
Mixed conductive-sensorineural
Describe conductive hearing loss
Give example causes
What test is commonly used to determine if a patient has conductive hearing loss?
Caused by any physical obstruction to the transmission of sound waves, impairing sound transmission to the inner ear; a person with conductive hearing loss hears better in the affected ear
Examples of Causes of Conductive Hearing Loss
A disorder of the external ear (impacted cerumen)
A disorder of the middle ear (otitis media or otosclerosis)
A Weber test is used to determine conductive hearing loss
What usually causes sensorineural hearing loss?
A defect in the cochlea, eighth cranial nerve, the vestibulocochlear nerve, or the brain itself