BIOL 220 Arthropodborne Diseases
1/45
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
46 Terms
What are some arthropod kingdom, phylum, and classes? What are their features/adaptation? What is their mode transmissions
Kingdom Animalia, Phylum Arthropoda
Class Insecta: Mosquitos, Fleas and Lice
Class Arachnida: Spiders, mites and ticks
Features: Segmented body parts with jointed appendages, well adapted to feed on preys/humans
Mode of Transmission: Vector Transmission (spread of infectious diseases through living organisms like
arthropods)
• Mosquitos, Ticks and fleas. <- DO not cause the disease, only spread!
What are the 2 General methods of vector transmission? What are examples of each method of transmission?
1. Biological vector transmission
• Active transport: Arthropod vector supports life cycle of pathogen inside of its body
• Pathogen is transmitted via bites
Examples:
• Mosquitos (Malaria and Zika virus)
• Ticks (Lyme Disease and Rocky Mountain spotted fever)
• Fleas (black death)
2. Mechanical vector transmission
• Passive transport: Arthropod vector carries the pathogen outside of its body
• No development stage inside the vector
Examples:
• Houseflies spreading salmonella from contaminated food or feces
What is the cycle of interactions of arthropod diseases?
Interaction between 3 organisms :
1. Host/Reservoir (us)
2. Pathogen/Parasite
3. Vector (Arthropod) – Ticks, Fleas, mosquitos
What are general reasons on why Arthropods are considered Highly adaptable vectors
• Has multiple developmental stages (Egg → Nymph → Adult) = complex life cycle
• Reduces competition between members of the same species
• Babies don’t compete with adults for resources
• Can inhabit diverse habitats
• Several types of vertebrate hosts
What Physiological adaptions do Arthropods have to be considered Highly adaptable vectors
• Mosquito has a blood meal where they feed/bite the host
• Mosquito releases chemicals before and after the blood meal to: Numb the area, prevent blood clotting, activate blood clotting post meal
• Bed Bugs can detect Carbon dioxide gas to help locate prey
What behavioral adaptions do Arthropods have to be considered Highly adaptable vectors
Mosquitos bite the host during darker hours
1. Prevent visual detection
2. Increase the likelihood of feeding on a sleeping host
What structural adaptions do Arthropods have to be considered Highly adaptable vectors
• Wings for locomotion: Locate food source + escape predation
• Compound eyes: Wide field of view without moving their heads = Sensitive to movement
• Proboscis: needle like for Blood meal + involved in delivering pathogens
• Antennae: for different senses like Chemoreception (smelling/tasting + mating), touch, hearing, and vibration detection
What are Arboviral diseases?
infections caused by a group of viruses that spread to people by the bite of infected arthropods (insects) such as mosquitos and ticks
What is the history behind the Plague
Bubonic plague pandemic
• 33% - 50% of Europe’s population died
• Still exists today, with small outbreaks
Speed of death: FAST
• Bubonic Plague : 2-8 days
• Septicemic Plague: within 24 hours
• Pneumonic Plague: 1-3 days without treatment
Plague: Causative Agent, Reservoirs, and positive/negative pressure room
Causative agent: Yersinia pestis (Gram negative bacillus)
Primary Reservoir: Rats & wild rodents;
Secondary Reservoir: Human
Use negative pressure room to keep pathogens inside the room
Plague: Mode of Transmission, Virulence Factor, and Types of Plague
Mode of Transmission
• Arthropod vector: Rat Flea
Virulence Factor: Ability to multiply in phagocytes
• Bacterial growth in phagocytes --> bacteremia --> Lymph nodes
• Sudden onset of hard and swollen (inflamed) lymph nodes in axilla (armpit) and groin (buboes)
3 Types of Plague: Bubonic, Septicemic, Pneumonic
Bubonic Plague: S/Sx
S/Sx:
• swollen/painful lymph nodes, fever, chills, body ache
• Acral necrosis – tissue death in the extremities (hands, feet, fingers and toes) due to lack of blood flow
• Most common form of plague
Describe Septicemic & Pneumonic Plague
Septicemic shock:
• Septic shock due to bacteremia
• Near 100% mortality rate*
Pneumonic Plague:
• An infection through airborne/droplet transmission OR bacteremia leading to an infection of the lungs
• Near 100% mortality rate within 3 days if not treated immediately*
Plague: Diagnosis, Predisposing Factors, Prevention, and Treatment
Diagnosis:
• Serology, sputum sample from lungs, fluid aspiration from buboes, S/Sx
Predisposing factors:
• Poor sanitation from rodents
Prevention:
• Eliminate the reservoir (rodents) via pest control; increase sanitation standards
Treatment:
• High doses of antibiotics
• Delaying treatment may significantly increase the risk of infection progressing to more severe forms
Lyme Disease: Causative Agent, Reservoirs, Mode of Transmission, and Common Location and Season
Causative agent: Borrelia burgdorferi (Motile, Spirochete)
Primary Reservoir: Field/deer mice
Secondary Reservoir: deer
Mode of Transmission
Arthropod vector: Ticks
Not capable of Transovarian passage (Disease causing pathogen is passed from female insect to her offspring)
Common Location and Season
• High prevalence in the Northeast United States
• High incidence rate during the summer season
In the Life Cycle of the Tick, what are the 4 Tick Developmental stages/forms? How long does it take to complete the life cycle?
1. Egg
2. Larvae
3. Nymph
4. Adult (not capable of Transovarian passage)
Takes at least 2 years to complete the tick’s lifecycle
Describe the tick lifecycle step by step
Adult female takes blood meal from infected person → tick becomes Infected → tick lays uninfected eggs in the ground during spring Year 1 (Not capable of transovarian passage)
Uninfected eggs hatch and develop into uninfected larvae in Spring Year 1
Uninfected larva takes 1st blood meal on infected wildlife host (Ex: mice) who were infected with B. burgdoferi in Summer Year 1 → uninfected larvae → infected with B. burgdoferi.
After the 1st blood meal, infected larvae detach from wildlife host (mice) and drop to the ground to remain dormant during Fall & Winter Year 1
The infected larvae come out of their dormant stage and develop into an infected nymph during Spring Year 2
The infected nymph takes its 2nd blood meal on uninfected humans/pets during Summer Year 2 = infect the human/pet with B. burgdoferi → Human develop Lyme disease
The infected nymph detaches from the adult/pet after the blood meal → develops into an infected adult tick and Fall year 2
The infected adult tick has its 3rd blood meal on a wild animal (deer) in Fall Year 2 → infect the deer with B. burgdoferi → After this blood meal, adult ticks will mate to continue the cycle*
Lyme Disease: S/Sx
First Phase: Early localized infection
• “Bull’s-Eye Rash”, Flu-like symptoms, and fatigue
Second Phase: Early Disseminated infection
• Bacteria begin to spread throughout the body
• Irregular heartbeat, facial paralysis and encephalitis
Third Phase: Late disseminated infection
• Bacteria spread to the nerves and joints → swollen joints
• Arthritis due to an immune response, persistent nerve pain/numbness/tingling
Lyme Disease: Diagnosis, Prevention, and Treatment
Diagnosis:
• Based on s/sx (like Bullseye's Rash)
• Prevalence in geographic area
• Serology
Prevention:
• Wearing protective clothing, applying tick replant, avoiding rodents/deer
Treatment:
• Can be treated with antibiotics (long treatment time lasting 2-6 weeks)
• Only good in the 1st stages, becomes increasingly difficult to treat in the later disseminated stages
Malaria: Causative Agents and Species Strains
Top 3 deadliest infectious diseases worldwide
Causative agent: Protozoans parasites (from the Genus Plasmodium)
Kingdom Protista, subkingdom Protozoa, Phylum Apicomplexa
• Not bacterial, viral, fungal, or helminthic
• Unicellular eukaryotic heterotrophic organisms
Species cause Malaria in humans:
• Plasmodium vivax - mildest and most common form to cause disease
• Plasmodium falciparum – most deadly form; S/Sx: severe anemia and encephalitis (Cerebral Malaria)
Malaria: Virulence Factor, Reservoir, and Mode of Transmission
Virulence Factor:
Complex lifecycle of Plasmodium pathogen involving two hosts
• Human (Intermediate host; Asexual reproduction of the Plasmodium pathogen)
• Mosquito (definitive host; sexual reproduction of the Plasmodium pathogen)
Frequent gene mutations = high drug resistance
Reservoir: Human
Mode of Transmission/Arthropod vector: Mosquito
Malaria: What are the 4 developmental forms for Plasmodium lifestyle and what are the two hosts needed to complete the pathogen’s lifecycle
4 developmental stages/forms for Plasmodium
1. Sporozoite
2. Merozoite
3. Male and female Gametocytes
4. Zygote
2 hosts: Mosquito and human
Life cycle of Plasmodium vivax
Step 1:
• Infected female mosquito has Plasmodium vivax (in its Sporozoite form)
• Has a blood meal on a human → mosquito transfers Plasmodium vivax (sporozoite form) into the human’s blood stream → travel to the human’s liver
Step 2:
• Asexual reproduction in intermediate (human) host → sporozoites undergo Schizogony in liver cells = merozoites are produced in the liver.
• Schizogony: the division of 1 sporozoite into 8 Merozoites; a form of asexual reproduction
Step 3:
• Merozoites are released from the liver → into bloodstream = cause RBC infection
Step 4:
• Merozoites develop into a ring inside newly infected Red blood cells.
• Observing RBC’s with ring merozoites in a patient’s blood smear = most common diagnostic method for Malaria
Step 5:
• The “ring stage of Plasmodium (merozoites) grow and divide = produce more merozoites
Step 6:
• Rapid growth of Plasmodium (in merozoite form) in RBCs = RBCs rupture → releasing the merozoites to infect other RBC to produce more merozoites via asexual
• Other merozoite develop into male and female gametocytes
• Leads to Paroxysms (intermittent fever and chills in humans) & Anemia (lack of healthy Erythrocytes)
Step 7:
• An uninfected different mosquito takes a blood meal from the infected intermediate host/human that has Plasmodium Gametocytes.
• The mosquito (definitive host) where sexual reproduction will occur → becomes infected and the gametocytes travel into the mosquito’s digestive tract.
Step 8:
• In the infected mosquito’s digestive tract → female and male gametocytes unite to form a zygote (Sexual reproduction)
Step 9:
• Zygotes develop into Sporozoites and go to the salivary glands of the mosquito → Plasmodium parasite is delivered into a new host following the mosquito’s blood meal.
Rickettsial Diseases: (Epidemic Typhus and Rocky Mountain spotted Fever): Causative Agents and Differences arthropod vectors
Causative Agents: Bacteria from the genus Rickettsia (Gram negative bacillus/coccobacillus)
• Obligate intracellular parasite (viruses; can only replicate in human cells only)
• Causative agents of “Typhus Fever” & “Spotted Fever” groups of diseases = both will have similar S/Sx = Both will cause a spotted flat/macular red rash on the body;
Differences in how they develop
• Arthropod vector = reservoir for both diseases
• Differences arthropod vectors between Rickettsia species
Epidemic Typhus – Typhus Fever: Causative agent, Reservoir/arthropod vector, and mode of transmission
Causative agent: Rickettsia prowazekii
Reservoir & arthropod vector: Human body louse
• In certain cases, the vector can act as the reservoir*
• Pathogen in human body louse → Spread to human and becomes diseased
• Unsanitary conditions (wars, homelessness, crowded, jails, concentration camps)
Mode of Transmission: Transmitted when louse feces that has contains Rickettsia prowazekii = rubbed into the bite wound by body louse
Epidemic Typhus – Typhus Fever: S/Sx, Predisposing factors, Diagonsis, Prevention, and Treatment
S/Sx
• Prolonged high fever followed by spotted macular (flat) red rash (due to subcutaneous hemorrhaging)
• Collection of blood under the skin, may be due to small blood vessels breaking open
• Spotted macular red rash begin at chest/trunk → to extremities (Palms and soles)
Predisposing factors:
• Unsanitary conditions (wars, homelessness, crowded jails,
concentration camps)
Diagnosis: type of rash & Location, serology
Prevention: Good personal hygiene and Sanitary living conditions
Treatments: Antibiotics (High mortality rate if left untreated)
Rocky Mountain Spotted Fever: Causative agent, Reservoir and arthropod vector, and Mode of Transmission
Causative agent: Rickettsia rickettsii
• Gram negative bacillus or coccobacillus
• Obligate intracellular parasite (viruses; can only replicate in human cells only)
Reservoir and arthropod vector: Tick
• Capable of transovarian passage = Transferring Rickettsia rickettsii from parent to offspring
Mode of Transmission
• Rickettsia rickettsii is transmitted through transovarian passage
• New larvae are already infected upon hatching from eggs
• Infected adult female tic→ lays infected eggs → Hatch into infected larva → infected nymph (stage is responsible for RMSF in humans)
Rocky Mountain Spotted Fever (RMSF): S/Sx and Diagnosis
S/Sx:
• Fever followed by a spotted macular/flat red rash due to subcutaneous hemorrhaging (bleeding)
• Spotted macular rash begin at extremities (palms and soles) → chest/trunk
Diagnosis: By rash type (where it begins; compare to Typhus Fever), location and serology
Rocky Mountain Spotted Fever (RMSF): Commonly Found, Arthropod vector, Prevention, and Treatment
Commonly Found:
• Spending time outdoors in the Southeast and Appalachian mountain regions, especially during the spring and summertime
Arthropod vector: Tick
Preventions: Insect repellant, long sleeved T shirts and pants, Checking for ticks after being outdoors
Treatment: antibiotics
Compare the life stages between lyme disease vs. rocky mountain spotted fever
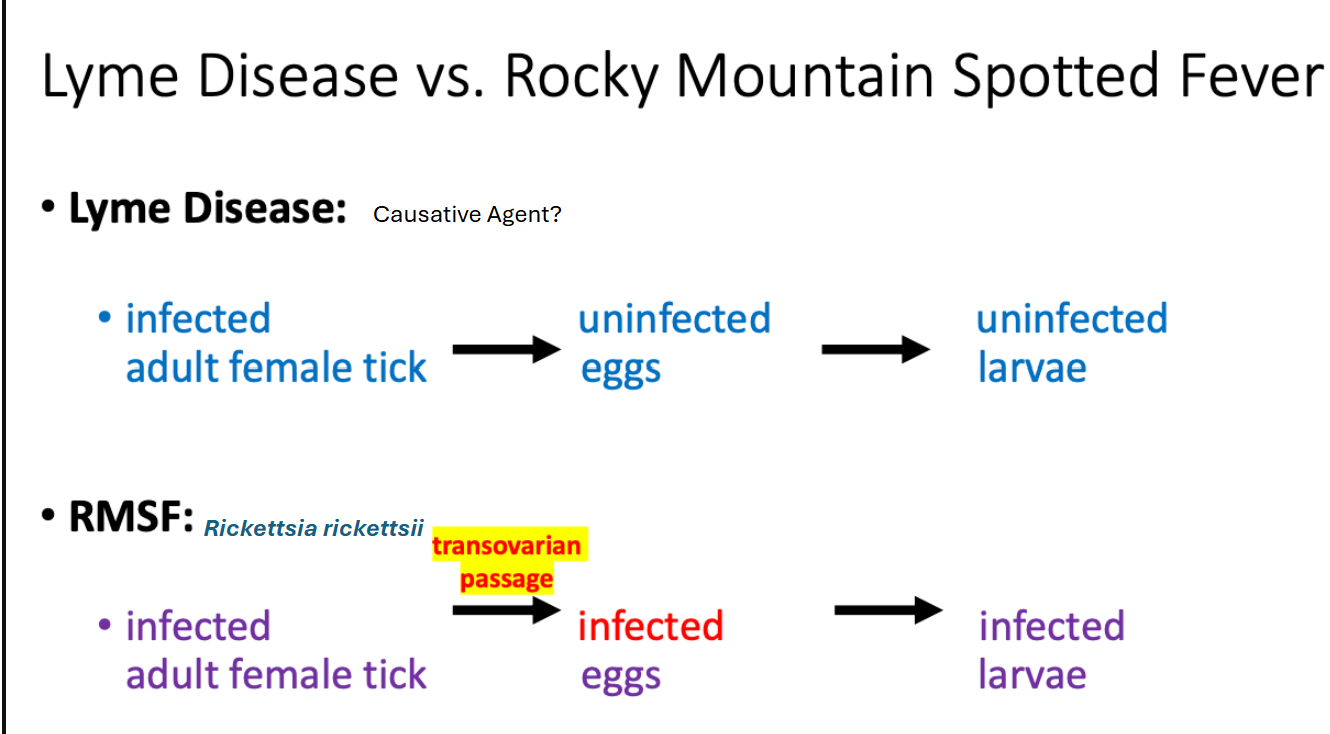
Arborviral diseases: Define arborvirus and what family do they belong to? What are the Arthropod vectors?
Arborvirus – arthropodborne virus
• arborviruses belong to several viral families; Not bacterial or protozoan
Arthropod vector:
• Caused by mosquito-borne viruses
• Mosquitos from the Genera Aedes & Culex
• Some arboviruses are considered Emerging infectious diseases
Arborviral diseases: Common S/Sx
Neurological → Encephalitis
Ex: West Nile Encephalitis, St. Louis Encephalitis, and Eastern Equine Encephalitis
• Inflammation of brain tissue
• Can be mild: Flu like symptoms, confusion, altered mental state, disorientation
• Severe: Brain swelling, loss of consciousness, seizures and coma
Vascular damage → Hemorrhagic Fevers
• Ex: Yellow Fever, Dengue, Emerging hemorrhagic fever: Ebola Virus, and Zika Virus
• bleeding → excessive bleeding
• Damage blood vessels and can cause severe uncontrolled external & internal bleeding which can affect
multiple organ systems
• External bleeding from: Under the skin or from body openings (Eyes, mouth and ears)
• Rash
West Nile Encephalitis: Causative agent, Arthropod vector, Reservoir, and Location to find them
Causative agent: West Nile encephalitis virus
Arthropod vector: Mosquitos from the mosquito genera Culex and Aedes
Reservoir: birds, (especially crows) and rodents
Location: Found all over the United States
West Nile Encephalitis: S/Sx, Prevention, and Treatment
S/Sx:
• fever, headache, neurological symptoms from brain inflammation (confusion and disorientation), sometimes polio-like paralysis
• 1 in 5 infected people develop symptoms, 1 in 150 people develop more severe symptoms
Preventative measures: Vector control; no vaccine available
Treatment: None
St. Louis Encephalitis: Causative agent, Arthropod vector, and Primary reservoir, Location
Causative agent: St. Louis Encephalitis Virus
Arthropod vector: Mosquitos from the genus Culex
Primary reservoir: Birds (not crows)
Location: Mainly found in the Central United States
Pre-disposing factors: Typically affects adults over 40 years old
St. Louis Encephalitis: S/Sx, Treatment
S/Sx:
• Fever, headache, neurological symptoms caused by brain inflammation (confusion and disorientation)
• No Polio-like paralysis (unlike West Nile Encephalitis)
Treatment: None
Eastern Equine Encephalitis: Causative agent, Reservoir, Arthropod Vector, S/Sx, Treatment, and Main Location
• Causative agent: Eastern Equine Encephalitis Virus
• Reservoir: Horses and Birds
• Arthropod Vector: Mosquitos from the genus Aedes
• S/Sx: Fever, headache and neurological symptoms (confusion and disorientation) = Over 30% mortality in humans
• Treatment: None
• Location: Typically found in the Southeastern united states
Yellow Fever– Arboviral Hemorrhagic Fever: Alternative Name, Causative Agent, Reservoir, Arthropod vector, and Treatment
Alt Name: jungle fever
• Yellow in Yellow fever is the jaundice that can occur, causing the skin and eyes of the infected to appear yellow*
Causative Agent: Yellow Fever Virus à
Reservoir: Wild Monkeys
Arthropod vector: Mosquitos from the genus Aedes
Treatment: None
Yellow Fever– Arboviral Hemorrhagic Fever: S/Sx, Prevention, and Treatment
S/Sx:
• Jaundice (via liver damage), fever, muscle pain, rash
• damage to blood vessels & hemorrhage (bleeding) in severe cases; potentially death
Prevention:
• Vector control
• Vaccine is available!
Treatment: None
Dengue: Causative Agent, Reservoir, Mode of Transmission, and Treatment
•Causative Agent: Dengue Virus
• Primary Reservoir: Humans
• Mode of transmission: Bite form a mosquito from the genus Aedes
• Treatment: None
Dengue: S/Sx, Prevention
S/Sx:
very similar to Yellow fever except NO Jaundice*
Fever, joint and muscle pain, rash
Blood vessel damage, hemorrhage in severe cases
Prevention:
Vector control
No vaccine available*
Ebola Virus disease: Causative Agent, Reservoir, Prevention, and Treatment
Causative Agent: Ebola Virus
• Originated from the Ebola River region in Africa
Reservoir: Cave-dwelling fruit bats (Not arboviral)
Preventation:
• Vaccine Available (U.S. Approved December 2019)
• Safe sex practices
Treatment: None
Ebola Virus disease: Mode of Transmission, S/Sx, and Mortality rate
Mode of Transmission:
• Contact with animal blood or waste products (NOT airborne)
• Can also be spread by contact with infected human body fluids (Blood, saliva, urine, sweat, feces, vomit, semen and breast milk)
S/Sx:
• Fever, Muscle pain , rash
• Blood vessel damage, Profuse hemorrhage in severe cases (internal and external bleeding) → Shock and multi organ failure
Mortality rate: 25- 90% ;
Zika Virus Disease: Causative Agent, Origin/Where Currently Found, Mode of Transmission
Causative Agent: Zika Virus
Origin/Where Currently Found:
• Originated from the Zika Forrest region in Africa
• Currently found in Central/South America (Brazil, Colombia & Venezuela)
Mode of transmission:
• Bite from a mosquito form the genus Aedes
• Can be spread through sexual contact (Similar to Ebola)
• Mother to fetus
• Contaminated blood transfusion
Zika Virus Disease: Reservoir and S/Sx
Reservoir: Wild Monkeys
S/Sx:
• Fever, muscle pain, Pink eye, some blood vessel damage
• Neurological symptoms: encephalitis, seizures and myelitis (inflammation of the spinal cord)
Zika Virus Disease: Pathogen During Pregnancy and Prevention
Pathogen During pregnancy can cause Serious damage to the fetus
• Congenital Zika syndrome
• Microcephaly (small underdeveloped brain in infants)
• Fetal loss – Death of fetus before or during birth
Prevention:
• Vector Control
• Avoiding insect bites: Mosquito repellent,
long sleeved shirts & Pants, mosquito net
• Using condoms or abstaining from sex