BIO 203 Module 6 E2
1/47
Earn XP
Description and Tags
85+
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
48 Terms
What is a hemolymph?
The fluid in many invertebrates (like insects) that functions similarly to blood and interstitial fluid combined.
Difference between Open, Open + Tracheal system, and Closed systems of circulation?
Pressure and O2 exchange low in open, Pressure low but O2 exchange high in Open + Tracheal, and Pressure and O2 exchange high in closed system.
Arteries are _____ ?
Pressure reservoirs
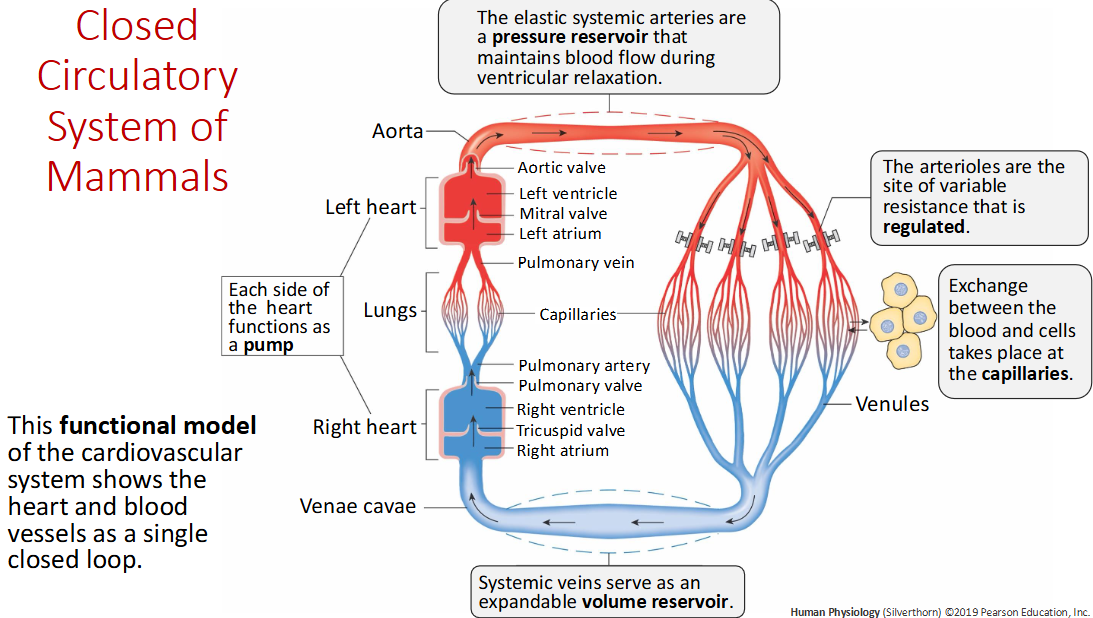
Where does exchange of blood and cells?
Capillaries
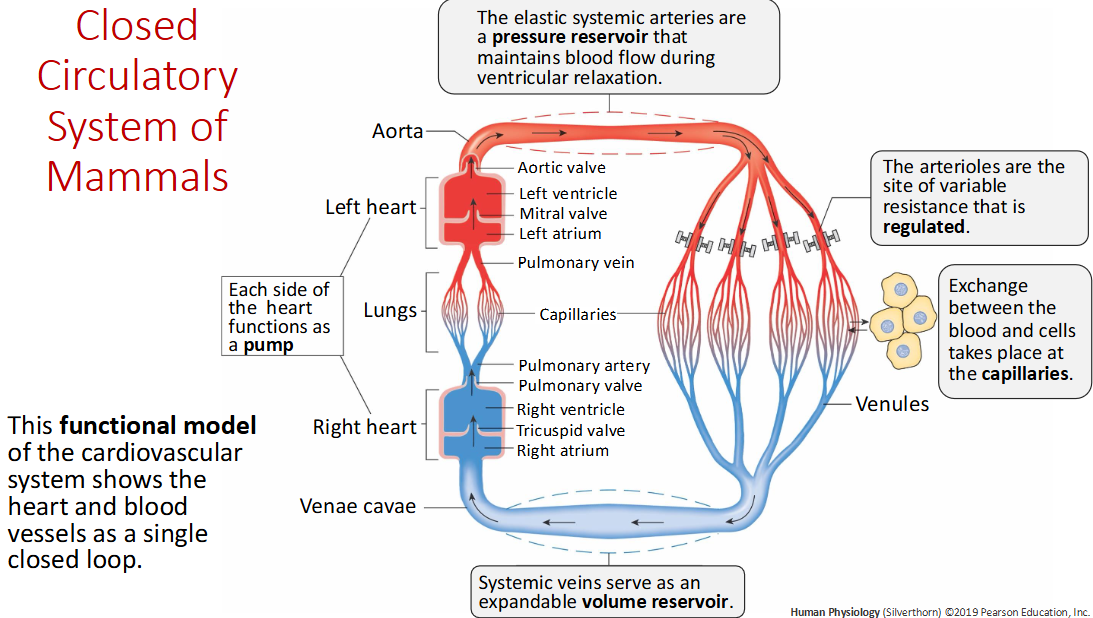
Systematic veins are _____ ?
Expandable volume reservoirs (low pressure)
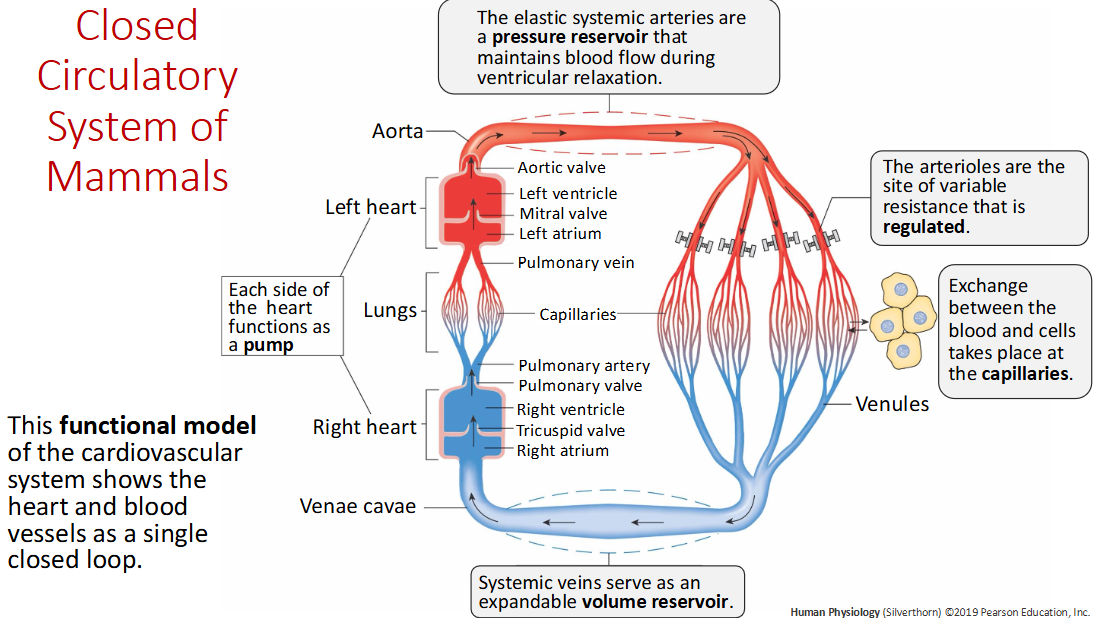
What are veins and arteries made of?
Endothelial cells and smooth muscles
What receptor creates vasoconstriction?
Alpha adrenergic receptors.
What receptor creates vasodilation?
Beta 2 adrenergic receptors.
What are arterioles?
Small branches of arteries that lead into capillary beds. They have smooth muscle in their walls and are the primary site of vascular resistance, meaning they control blood flow and blood pressure by constricting or dilating. Act as control valves after arteries and before capillaries.
What are metarterioles?
small vessels between arterioles and capillaries that regulate entry of blood into capillary beds via precapillary sphincters
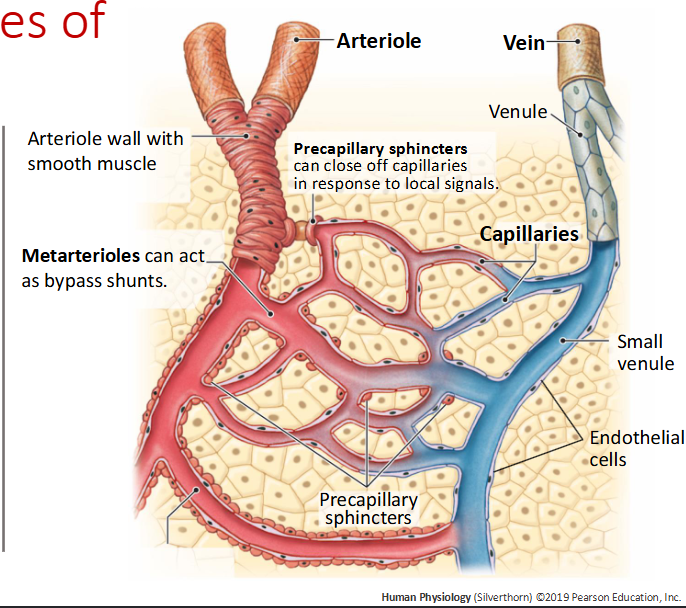
What are venules?
Receive blood from capillary bed (convergent pattern of flow)
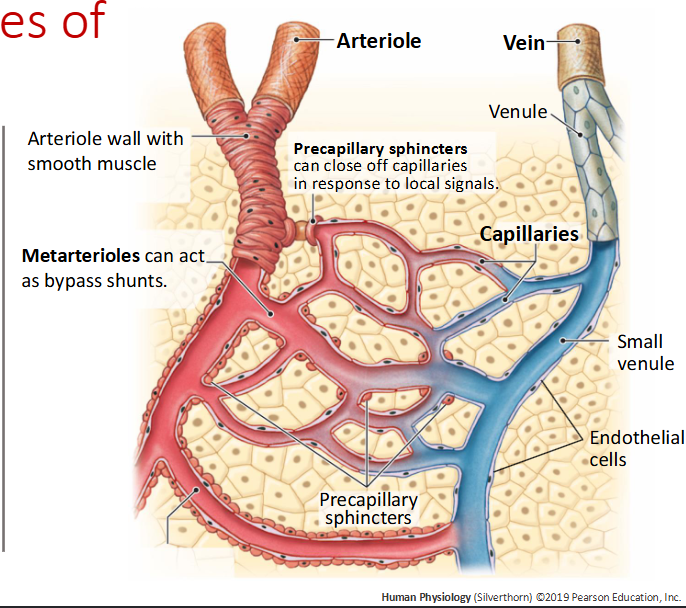
How do veins prevent backward flow?
One way valves
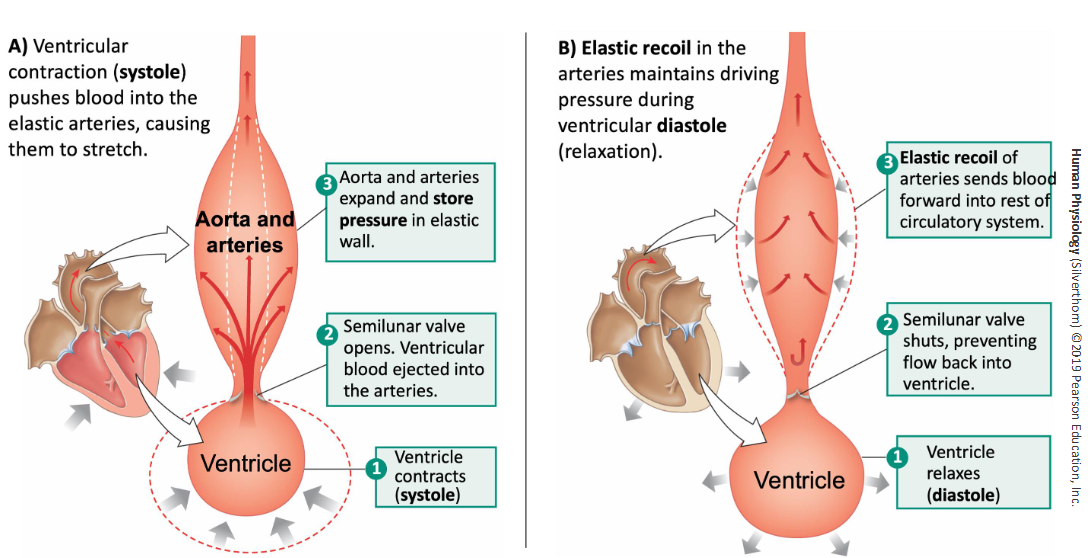
Describe the left ventricle pumping blood through the Aorta artery and the pressure concepts.
Ventricle pumps (systole) and the artery receives the pressure to push blood out into body, then the ventricle shuts the semilunar valve to prevent backflow and relaxes (diastole) but the recoil in the artery keeps a pressure to keep pushing blood into rest of system
Pulse pressure calculation?
Systolic pressure - diastolic pressure
MAP calculation?
Cardiac Output x Resistance
Normal systolic/diastolic pressure?
120/80 mmHg
Vasoconstriction vs Vasodilation effects on blood flow and pressure?
Vasoconstriction = increased resistance, less blood flow, higher blood pressure
Vasodilation = less resistance, more blood flow, lower blood pressure
Epinephrine vs Norepinephrine which binds to alpha adrenergic receptors and beta 2 adrenergic receptors and what do they do?
Epinephrine: Beta 2 adrenergic receptors = dilations
Norepinephrine: Alpha adrenergic receptors = constrictions
Explain capillary exchange of nutrients and oxygen.
Gaps between endothelial cells, also via transcytosis bring macromolecules and nutrients over to interstitial fluid. Oxygen simply diffuses across. Some vesicles can make pores fenestrations for bulk flow.
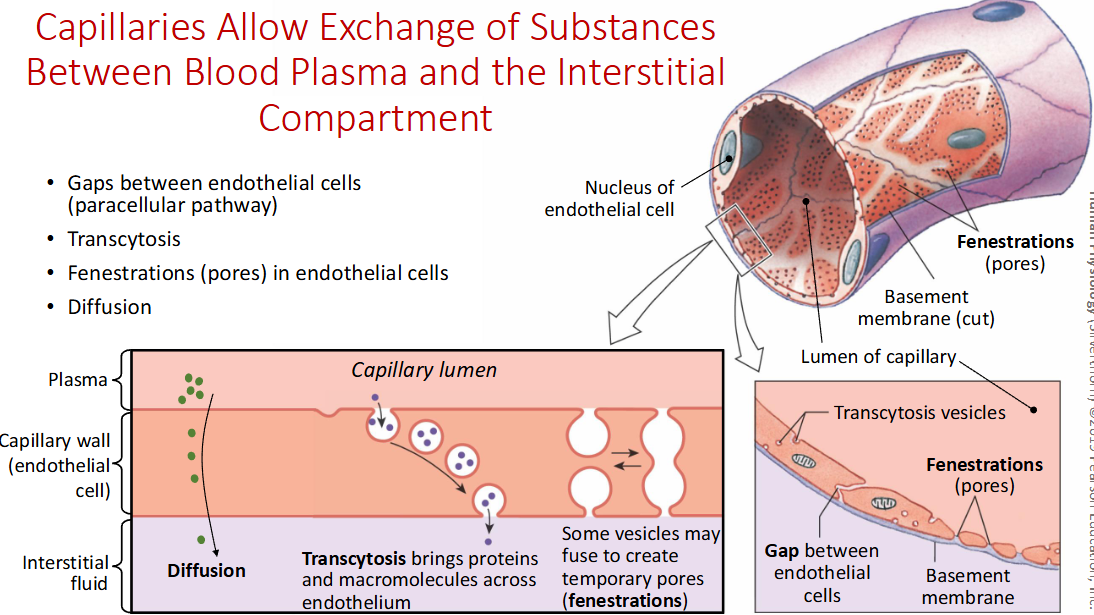
What are paracellular pathways in capillaries?
Gaps between endothelial cells and allow for movement by bulk flow for fluid and small molecules like glucose
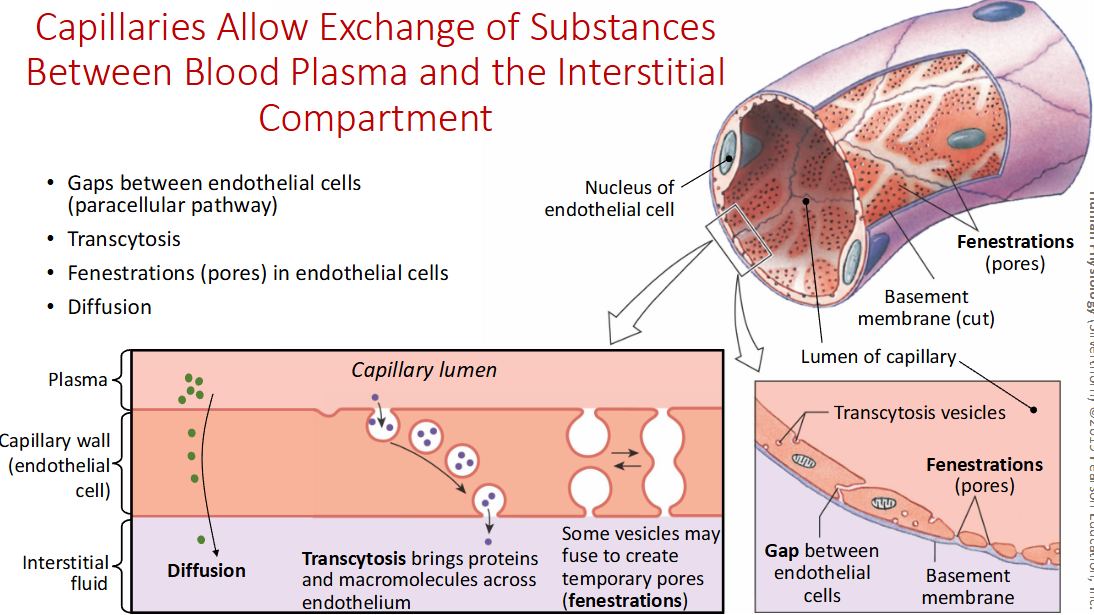
True or False: Capillaries differ per body part?
True: some limit exchange (cerebral capillaries with tight gaps and no fenestrations), others allow substantial exchange (kidneys, intestines, skin, skeletal muscles, lungs, with small gaps and a few fenestrations), others allow extensive exchange (liver, bone marrow, with large gaps between endothelial and fenestrations and transcytosis)
Net pressure formula?
Pnet = Ph - pi
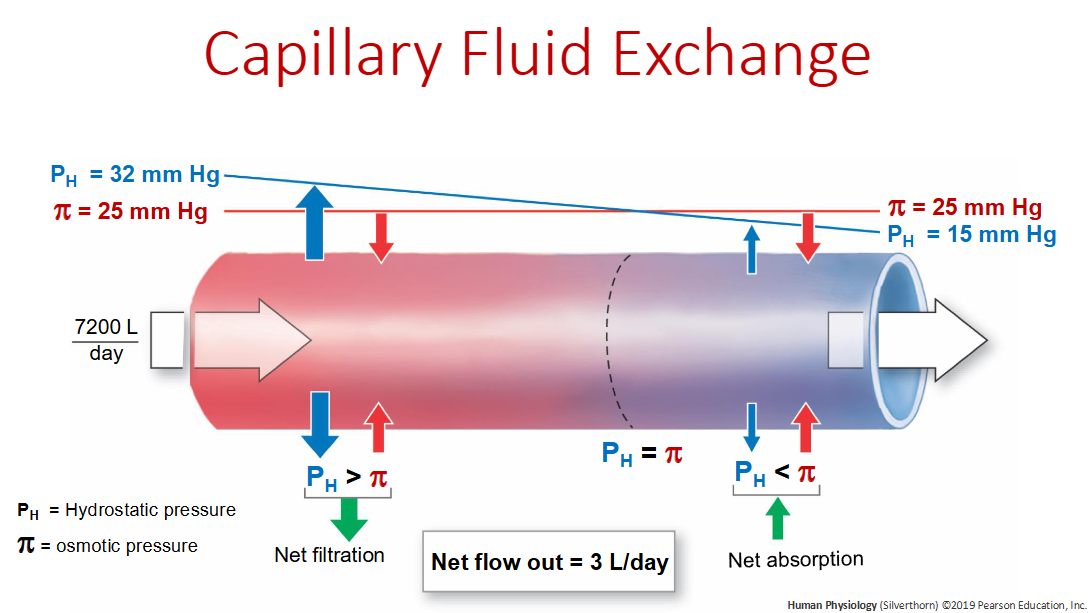
What does the lymphatic system NOT have that the cardiovascular system is known for having?
A centralized pump. Only moves lymphatic fluid via contraction of smooth muscles, body movement, and one-way valves.
Difference between Lymph and Blood
Lymph: white blood cells only, flows through lymph vessels, removes excess interstitial fluid from tissues, immune functions, returns interstitial fluid to circulatory system
RBC: white blood cells and red blood cells and platelets and plasma and proteins, flows through blood vessels, supplies vital substances to tissues and organs, removes waste, immune functions, clot formation, maintain homeostasis
What are lymphatic capillaries? What are lymphatic valves good for?
a one cell layer thick layer of endothelial cells, prevent back flow of interstitial fluid
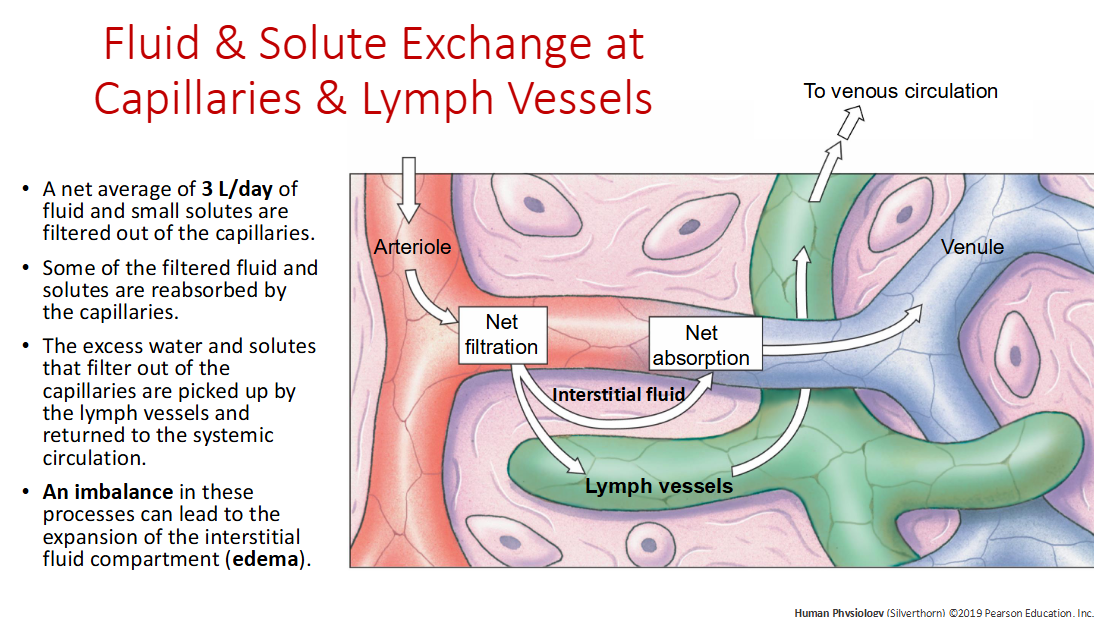
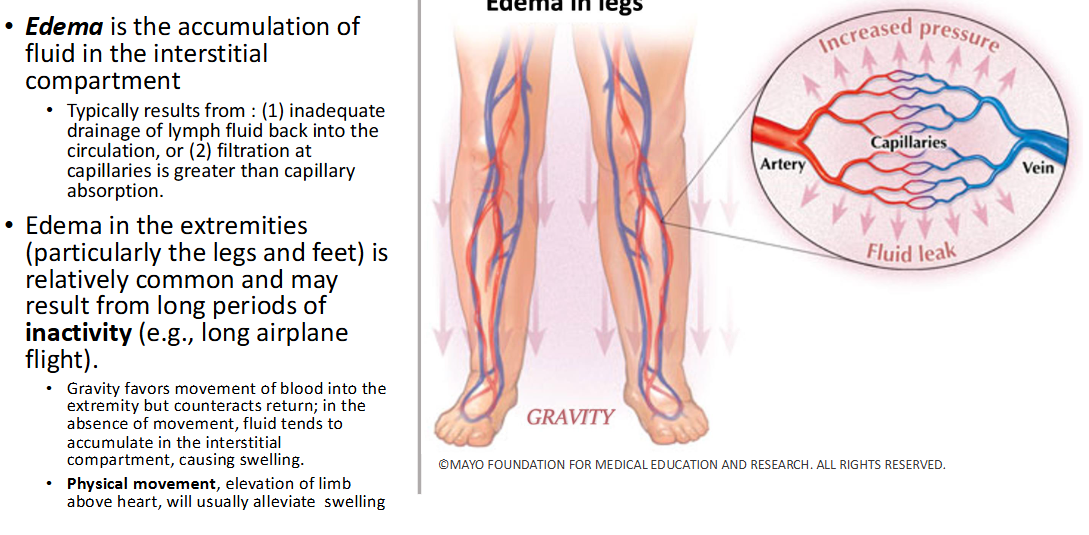
What is an Edema?
accumulation of fluid in interstitial compartment (between cells rather than in circulatory/lymphatic)
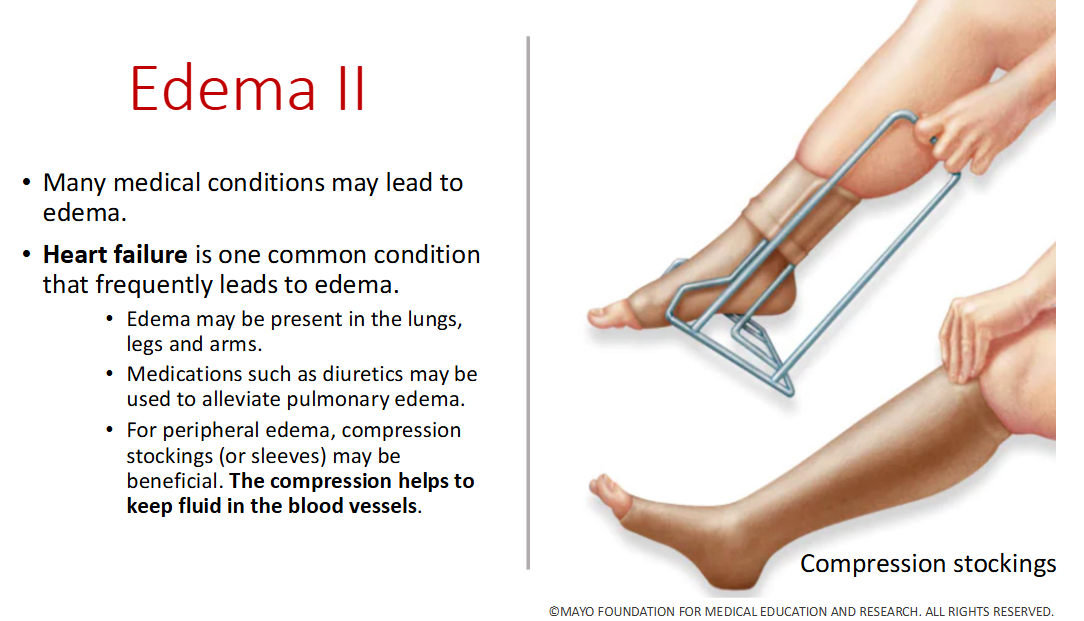
Fun question: Why do they put compression socks on patients?
Keeps fluids in blood vessels to prevent an edema
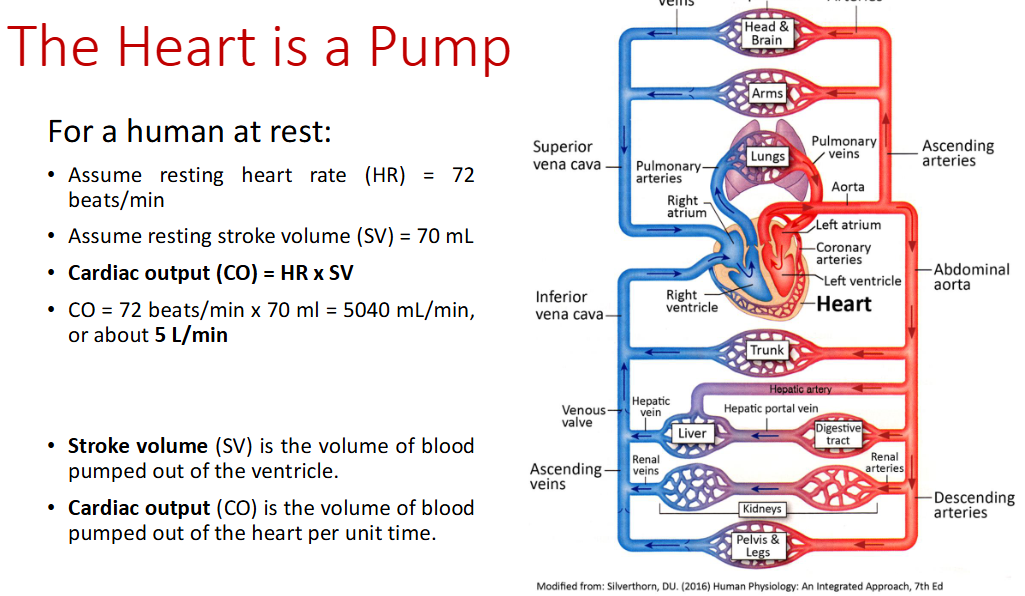
How to calculate cardiac output (CO)?
Heart Rate (HR) x Stroke Volume (SV)
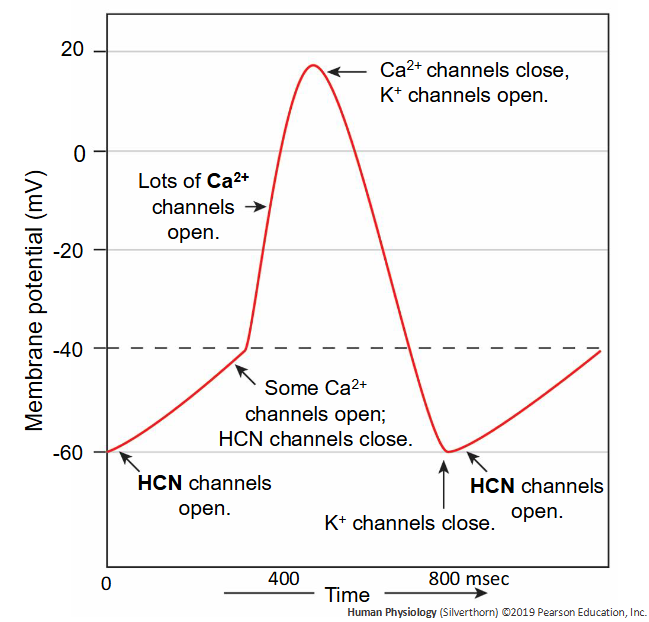
What is a cardiac autorhythmic cell?
specialized muscle cells that spontaneously generate action potentials
What are cardiac conduction cells?
muscle cells specialized for conducting action potentials
What are cardiac contractile cells?
heart muscle cells that generate force and contract to pump blood, activated by electrical signals from pacemaker cells
What are SA node cells?
autorhythmic pacemaker cells in the right atrium that initiate the heartbeat by spontaneously generating electrical impulses
What are HCN Channels?
Hyperpolarization- activated cyclic nucleotide gated channels; these channels open when the membrane potential hyperpolarizes to -60 mV
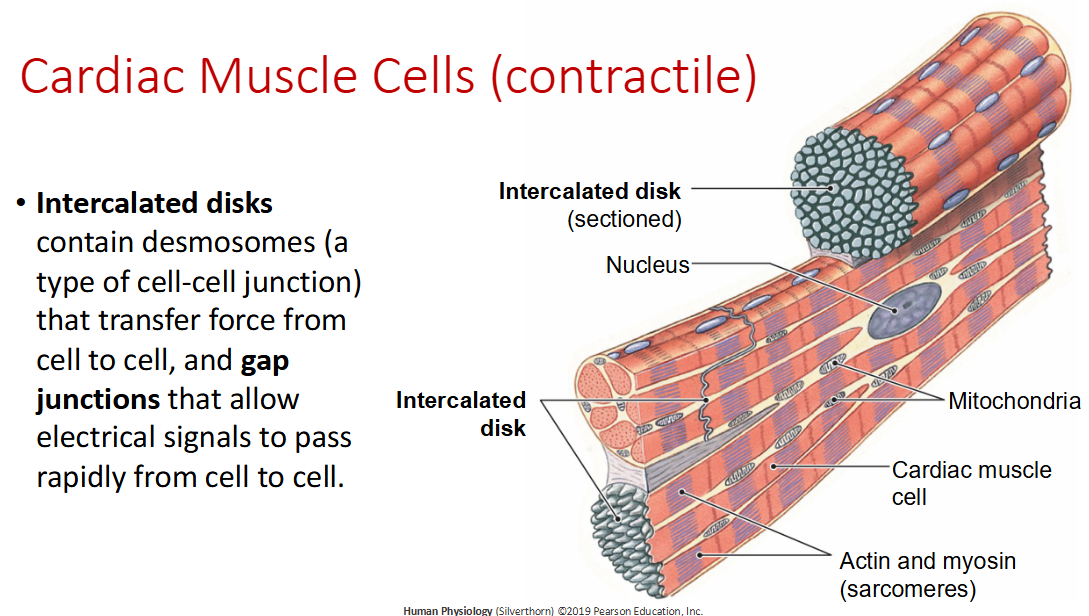
Cardiac Muscle Cells:
contain desmosomes (a type of cell-cell junction) that transfer force from cell to cell, and gap junctions that allow electrical signals to pass rapidly from cell to cell
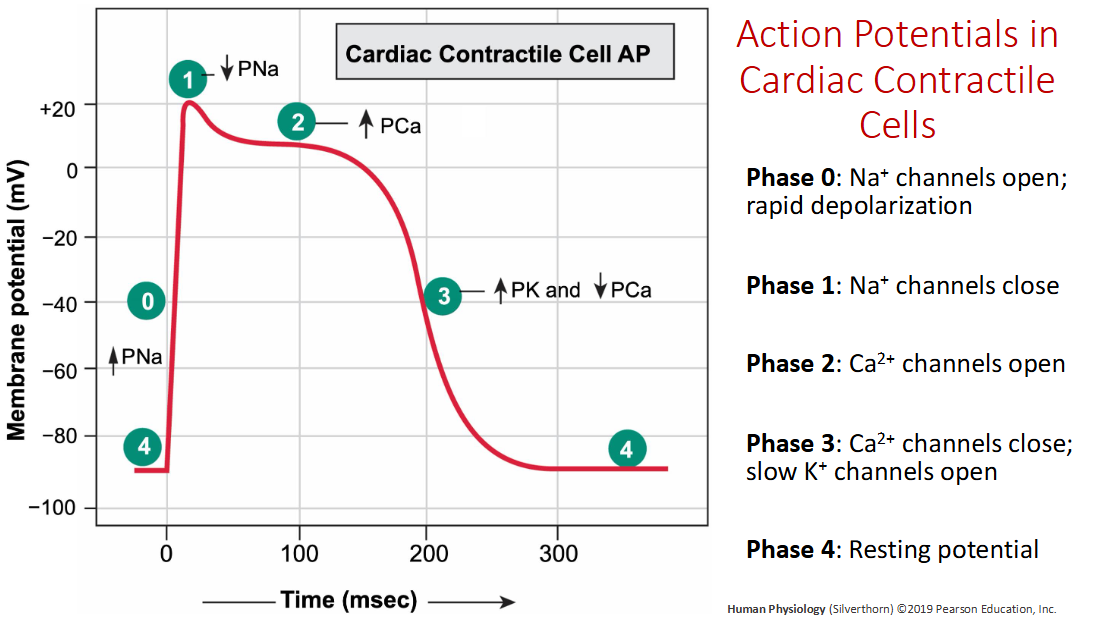
Explain action potential in cardiac contractile cells.
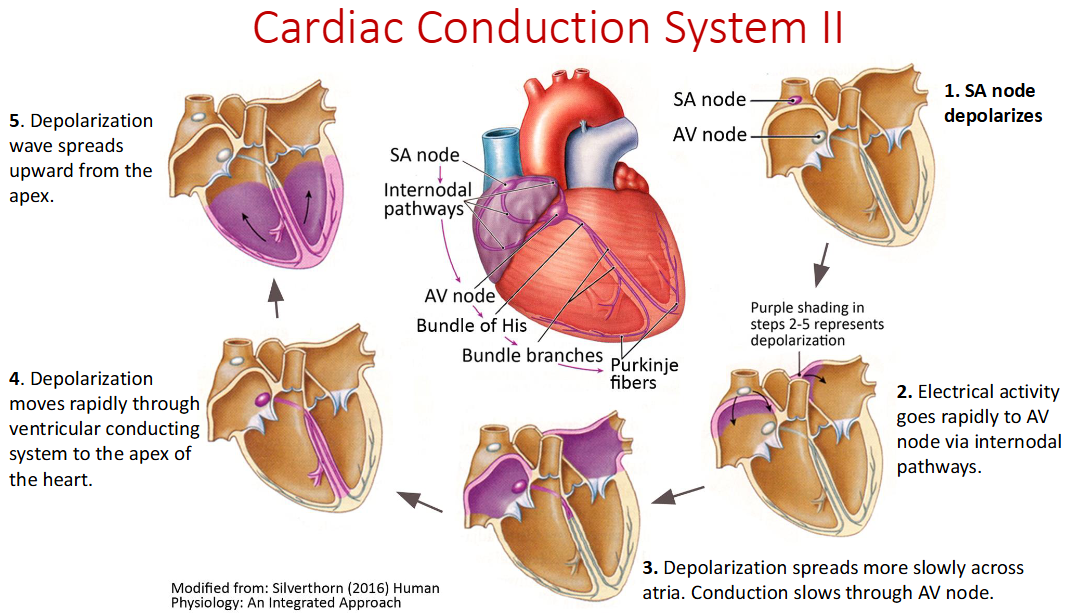
Atria contract in a _____ motion
downward
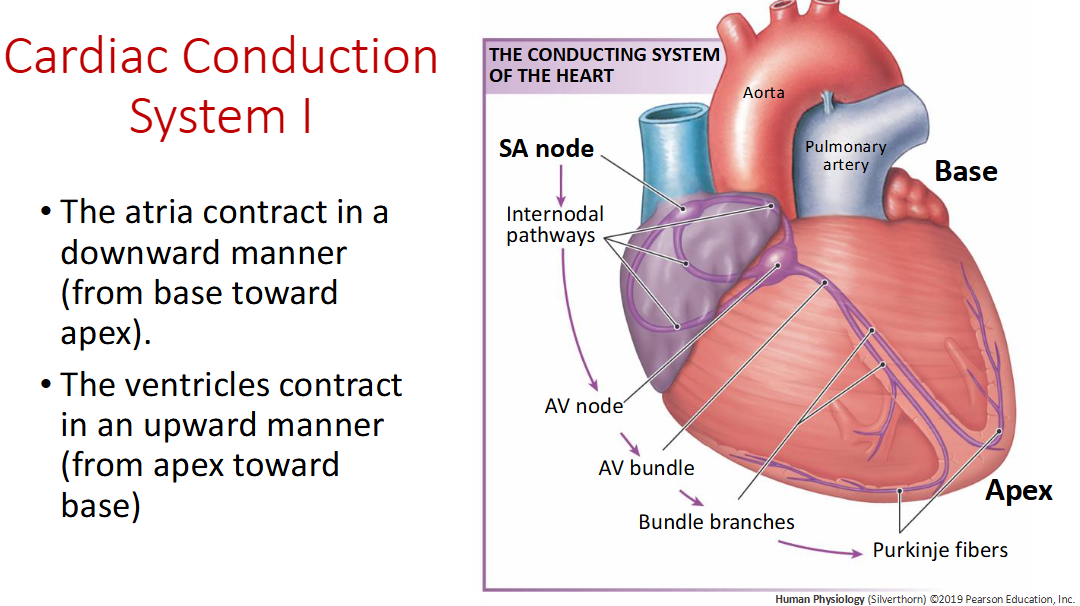
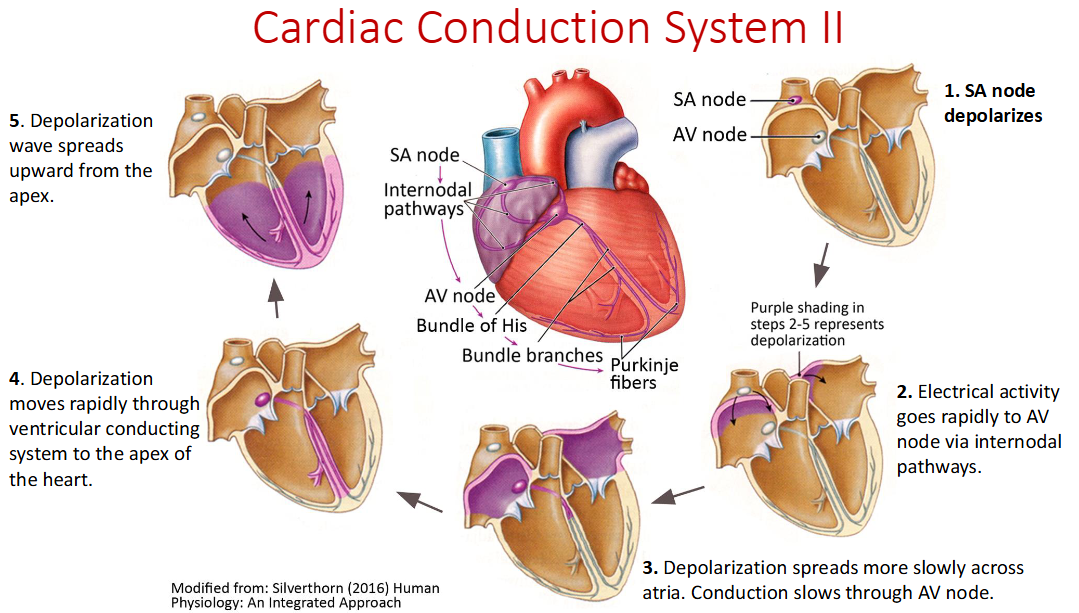
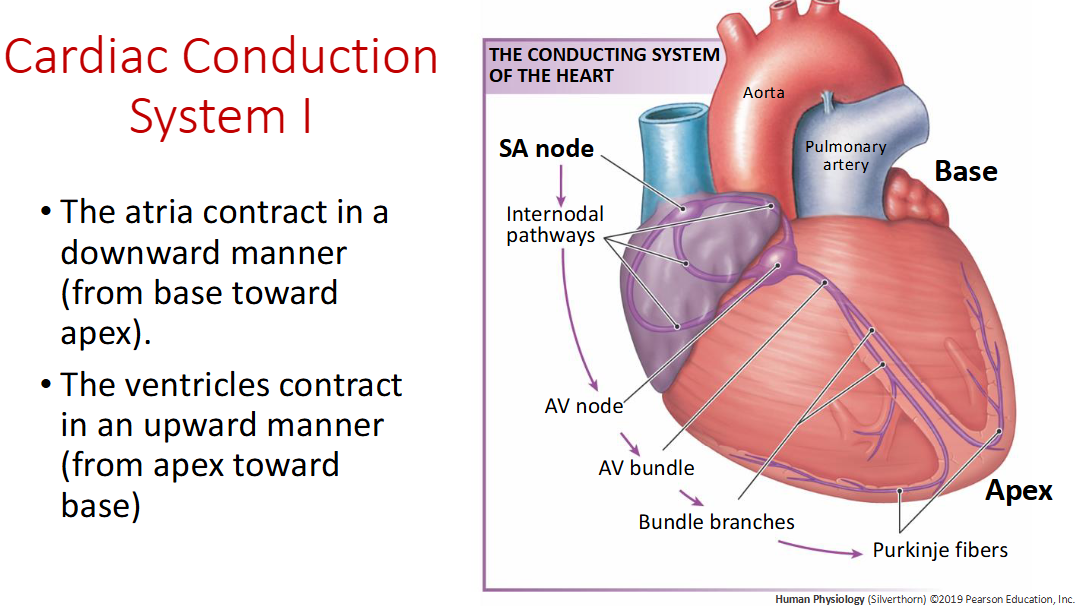
Ventricle contract in a _____ motion
upward
Explain the Wigger diagram and what Lub and Dub sounds mean.
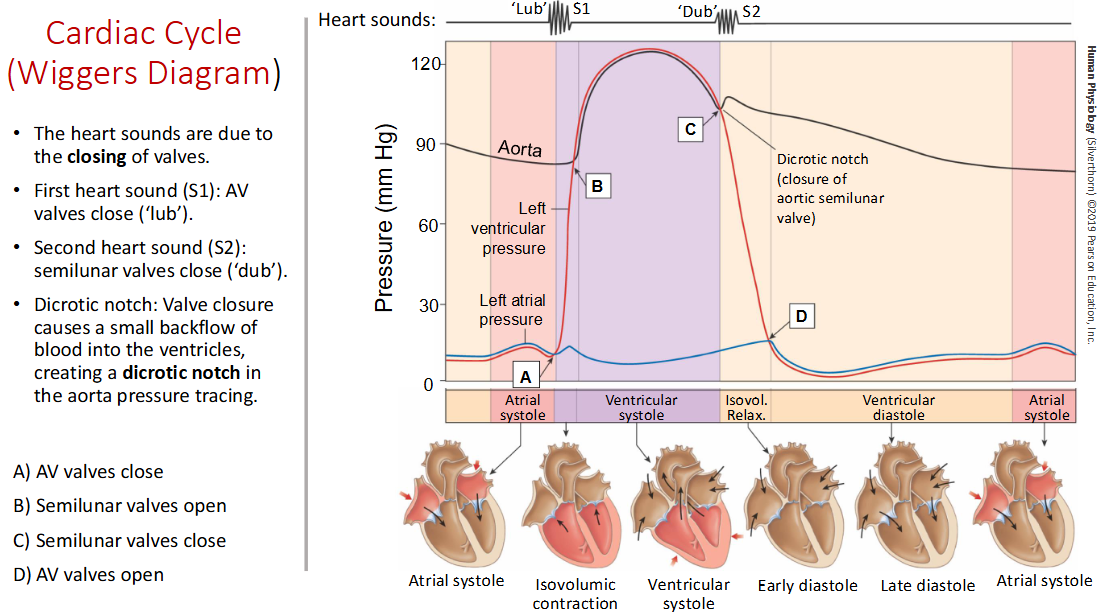
End Diastolic Volume (EDV):
maximum amount of blood in ventricle before contraction
End Systolic Volume (ESV):
minimum amount left in ventricle after contraction
Stroke Volume (SV):
the amount of blood expelled in one contraction
Stroke Volume (SV) =
End Diastolic Volume (EDV) - End Systolic Volume (ESV)
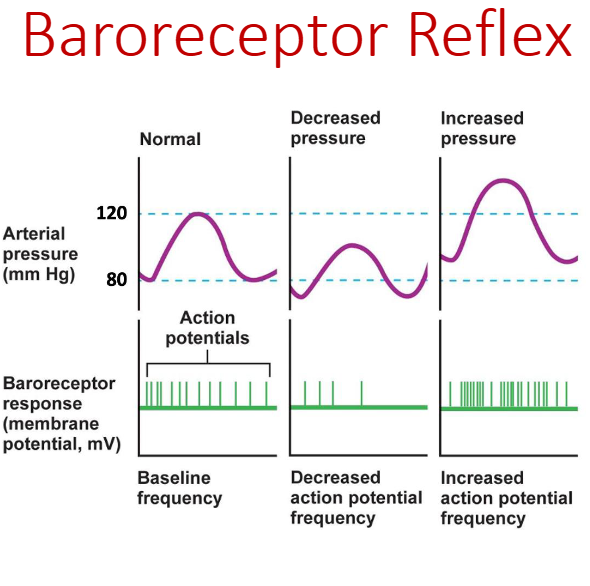
What are Baroreceptors?
stretch receptors in the carotid sinus and aortic arch that detect changes in blood pressure and trigger reflex adjustments to maintain homeostasis
Baroreceptors respond to changes in MAP by firing
action potentials:
• Low MAP = decreased AP frequency
• High MAP = increased AP frequency
MAP = CO x R
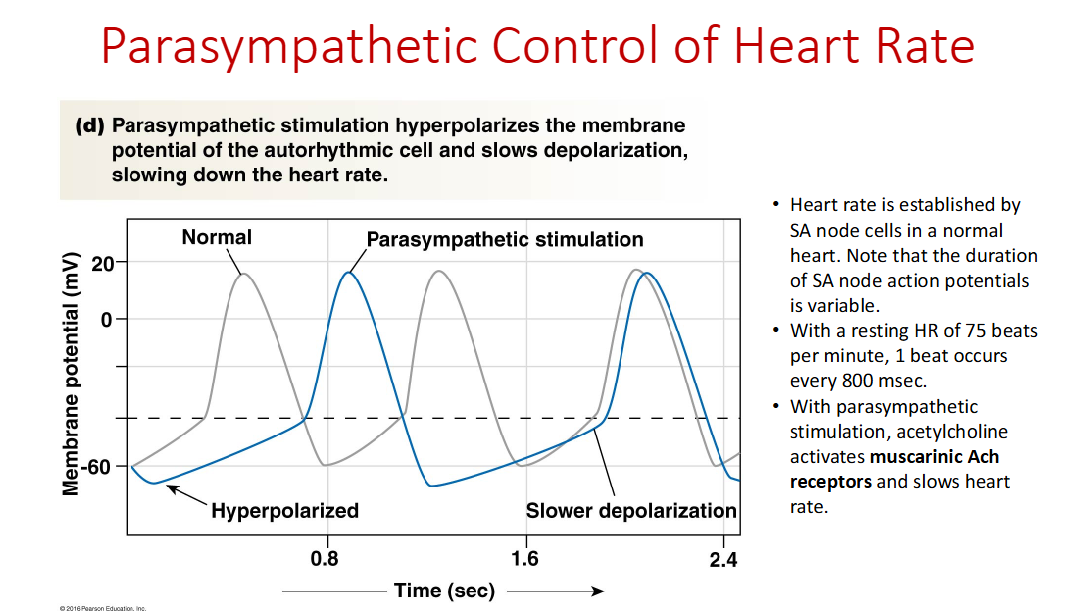
Muscarinic AChRs are found on SA node cells of the heart. So?
Hyperpolarizing graded potential and activation of parasympathetic nervous system will decrease heart rate.
β1-adrenergic receptors are found on SA node cells and contractile cardiac muscle cells. So?
In SA node cells, norepinephrine binding to beta-1 adrenergic receptors increases the funny current (pacemaker potential), such that threshold is reached more rapidly; heart rate is increased
In cardiac contractile muscle cells, norepinephrine binding to beta-1 adrenergic receptors increases intracellular Ca2+, leading to greater force of contraction; stroke volume is increased
MAP =
MAP = (SV x HR) and R = 8nL/pi r^4
Parasympathetic controls _______ ?
Heart Rate (HR)
Sympathetic controls _______ ?
Controls stroke volume (SV), heart rate (HR), and resistance R