Lung Diseases + Integrating Centers
1/19
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
20 Terms
Pressure gradient of an individual gas across the plasma membrane
most important factor in affecting the rate of diffusion
Increase gradient → increase diffusion rate
Decrease gradient → decrease diffusion rate (one cause of hypoxia) due to hypoventilation or high altitude
Surface area over which gas can move
At the internal respiration or external respiration exchange zones
Increase surface area (ex: increase capillary density) → increase diffusion rate
Decrease surface area (as in some resp diseases) → decrease diffusion rate
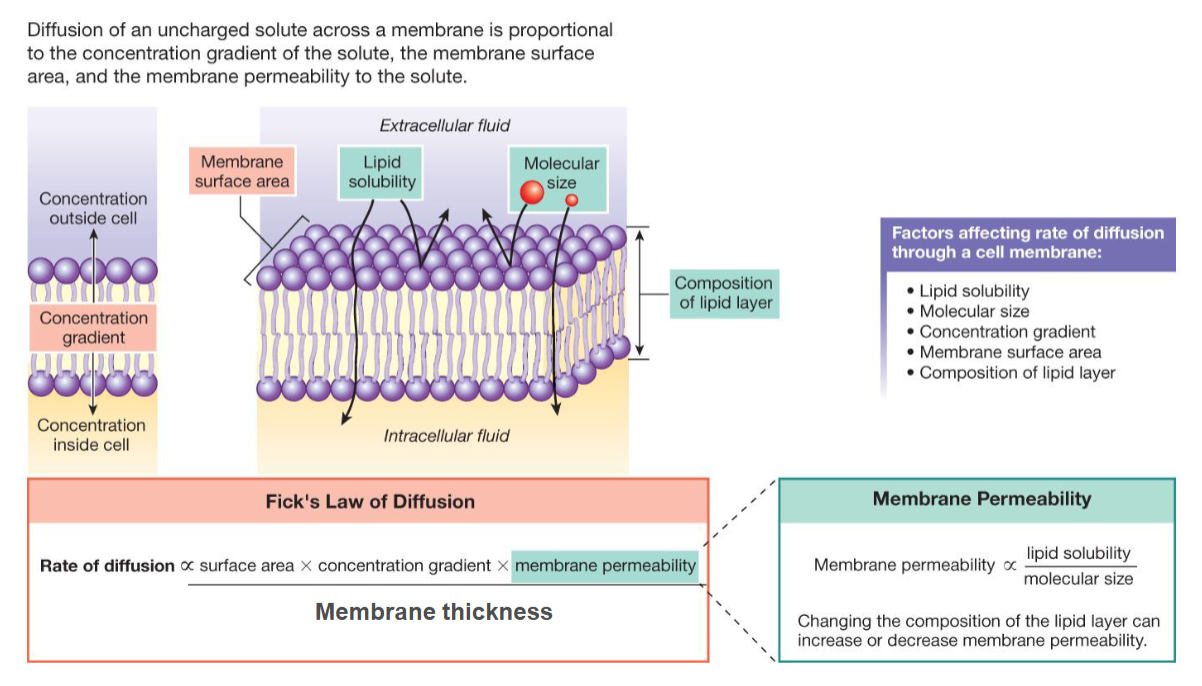
Membrane thickness (permeability)
low and constant (under normal, healthy conditions)
increase thickness (as in some resp. diseases) → decrease diffusion rate
Diffusion distance
low and constant (under normal healthy conditions)
increase distance (as in some resp. diseases) → decrease diffusion rate
Hypoxic hypoxia
Low arterial PO2
High altitude
alveolar hypoventilation
decreased lung diffusion capacity
abnormal ventilation-perfusion ratio
Anemic hypoxia
Decreased total amount of O2 bound to hemoglobin
blood loss
anemia (low concentration of Hemoglobin or altered HbO2 binding
Carbon monoxide poisoning
Ischemic hypoxia
Reduced blood flow
heart failure (whole body hypoxia)
Shock (peripheral hypoxia)
Thrombosis (hypoxia in a single organ
Histotoxic hypoxia
Failure of cells to use O2 because cells have been poisoned
Cyanide and other metabolic poisons
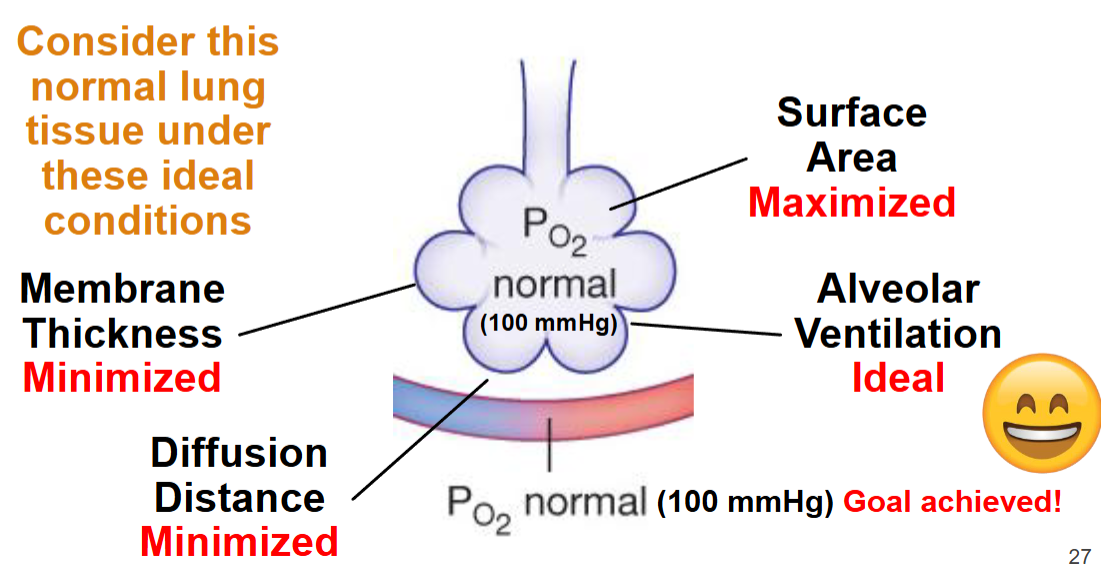
Lung diseases arise when normal pressure gradients, surface area, or diffusion distance no longer exist
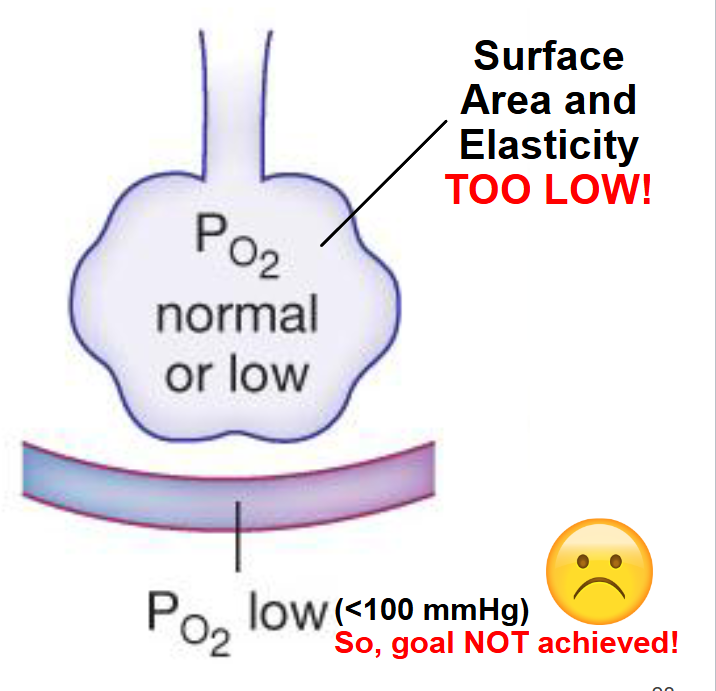
In patients with emphysema, destruction of alveoli from long term smoking leads to less surface area for gas exchange
also, there is a loss of elasticity in lung tissue for these patients, making it difficult to exhale, resulting in poor ventilation of some alveoli
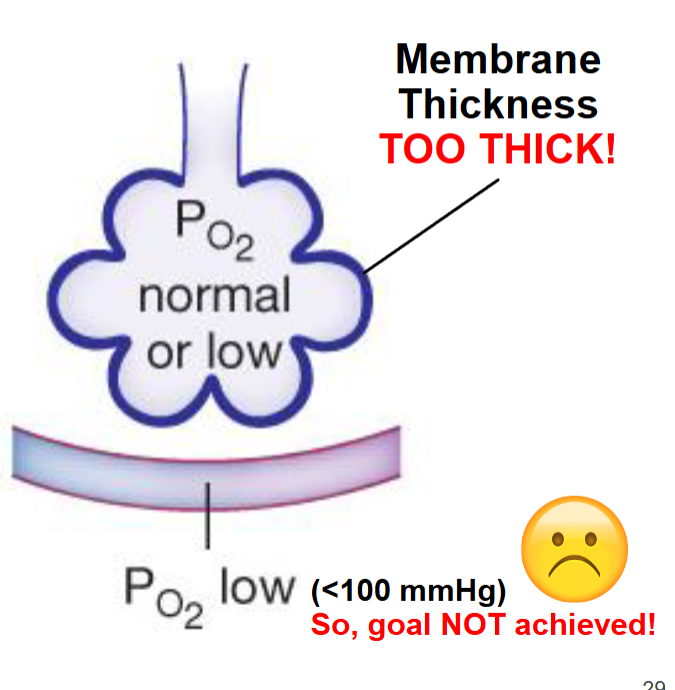
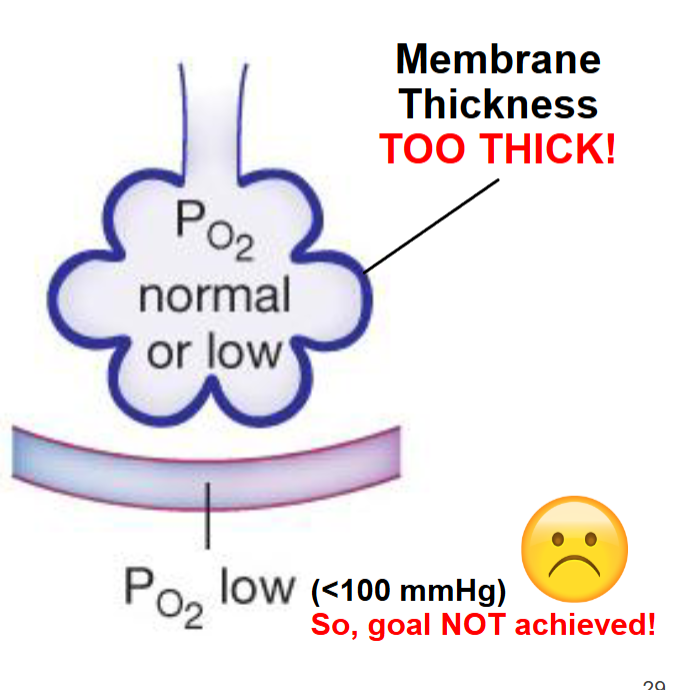
In patients w/ fibrotic lung diseases, thickened alveolar membranes slow gas exchange
may be caused by long term exposure to particulates that scar delicate lung tissues
The same effect can occur with the growth of tumors in the lungs or tuberculosis infection or accumulation of mucus in alveoli (cystic fibrosis)
Fibrotic lung disease also often include a loss of compliance…
which makes it effortful to inhale, leading to poor alveolar ventilation
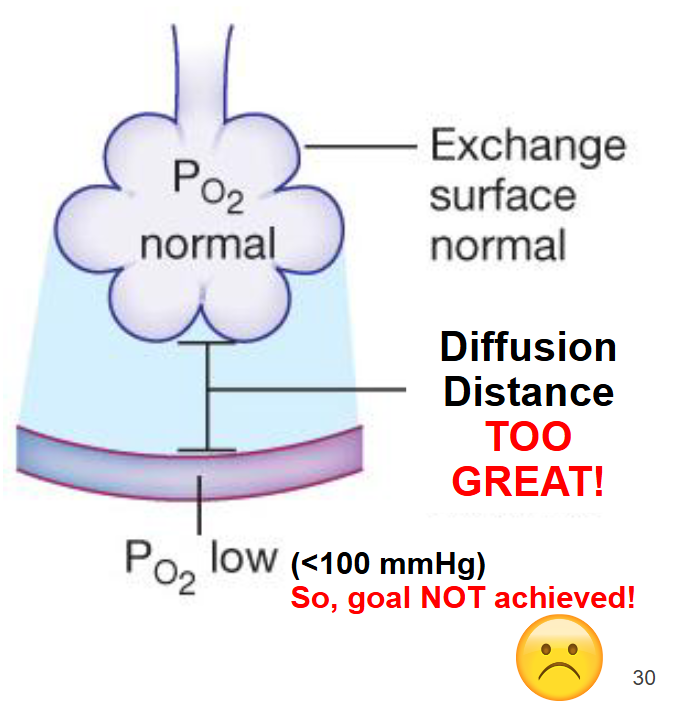
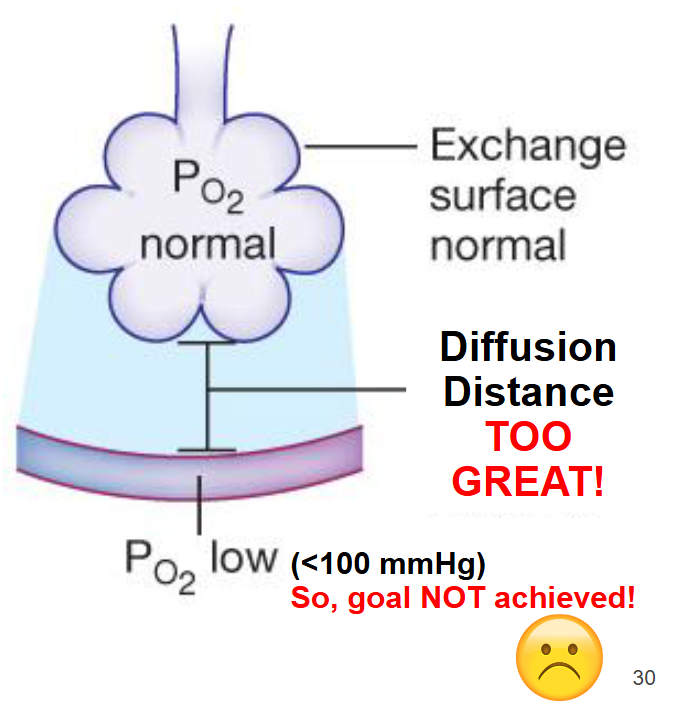
When a patient presents with pulmonary edema, they have fluid accumulation in the interstitial space between the alveoli and pulmonary capillaries
Due to congestive heart failure (left side of the heart no longer pumping properly) or inflammation in the lungs due to respiratory infection (ex: COVID-19)
Blood PO2 levels will be greatly diminished, because O2 does not dissolve well in water
Blood PCO2, however, may be normal due to higher CO2 solubility in water
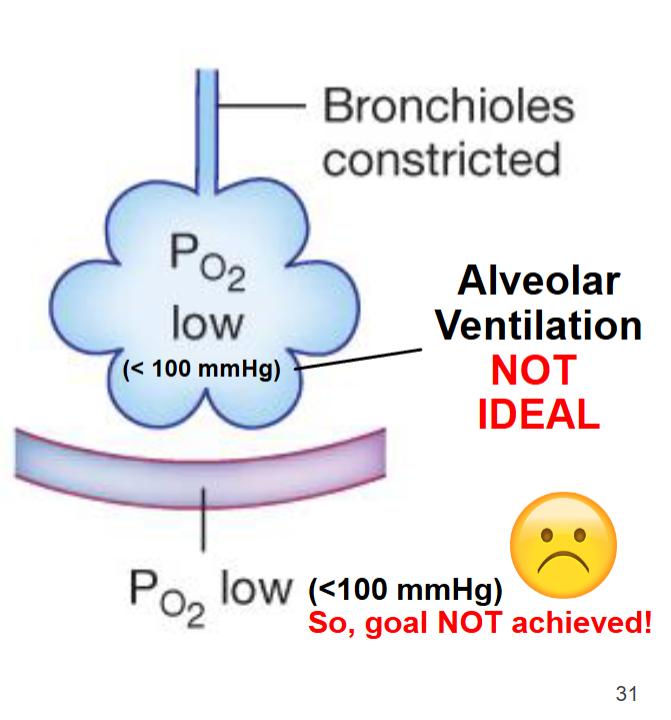
Obstructive lung diseases
for patients with asthma, irritation in the airways (allergic reactions or radical air temp changes) can cause significant bronchoconstriction
This leads to poor ventilation of the alveoli due to increased air flow resistance, a decreased pressure gradient for PO2 and therefore low PO2 in the pulmonary cirulation
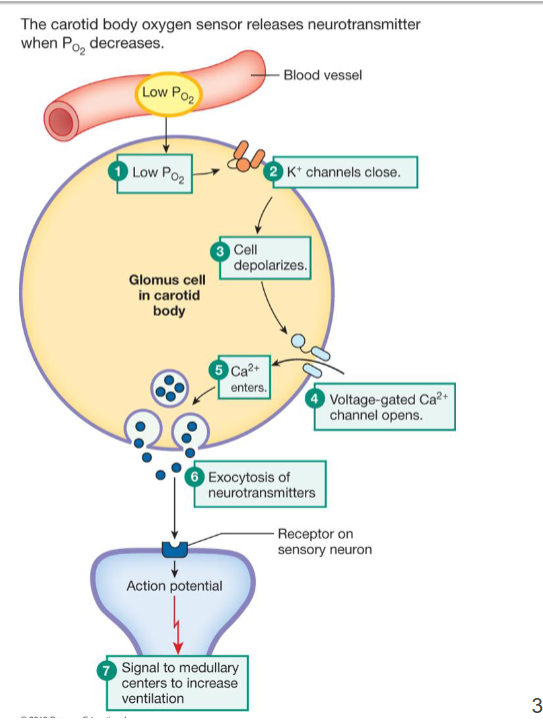
Glomus cells
sensor for PO2, PCO2, and pH
also called peripheral chemoreceptors
Located in the walls of the carotid arteries and aorta
detect decreased pH (increased [H+]) or increased pCO2 in the blood
Also detected very low PO2 (60mmHg) in the blood
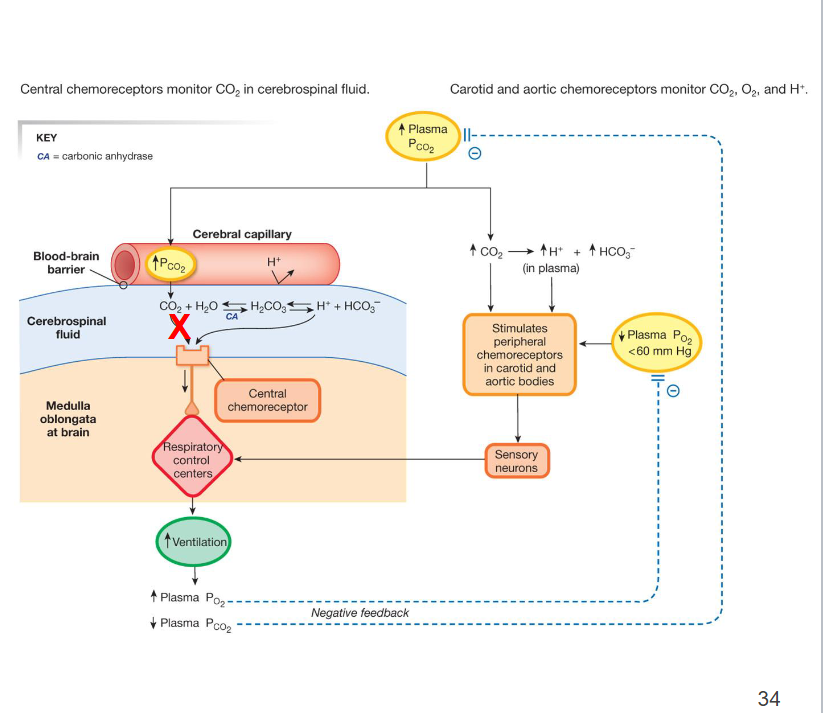
Additional sensors for PCO2 and pH
Central chemoreceptors are located on the ventral surface of the medulla oblongata and monitor H+ and CO2 in cerebrospinal fluid
CO2 is immediately converted to carbonic acid when it enters CSF
→ what does it dissociate into?
Central chemoreceptors actually detect H+
→ Not CO2 directly
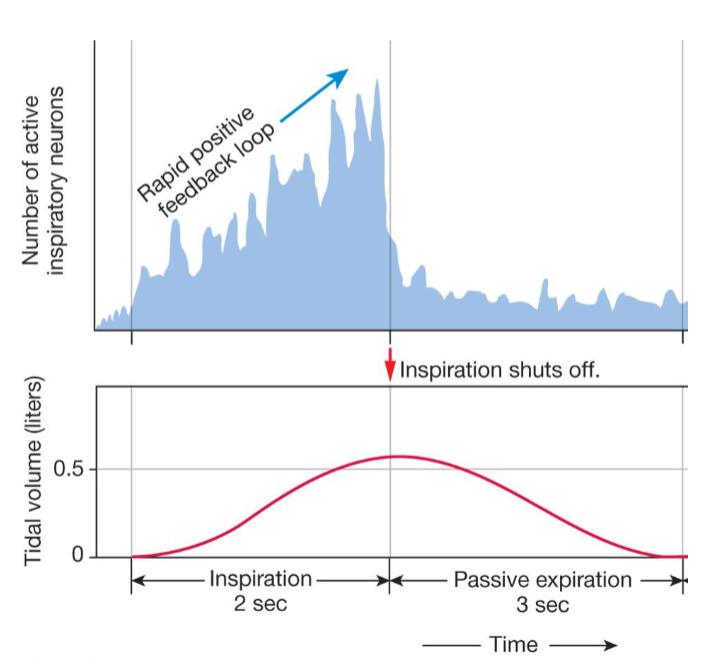
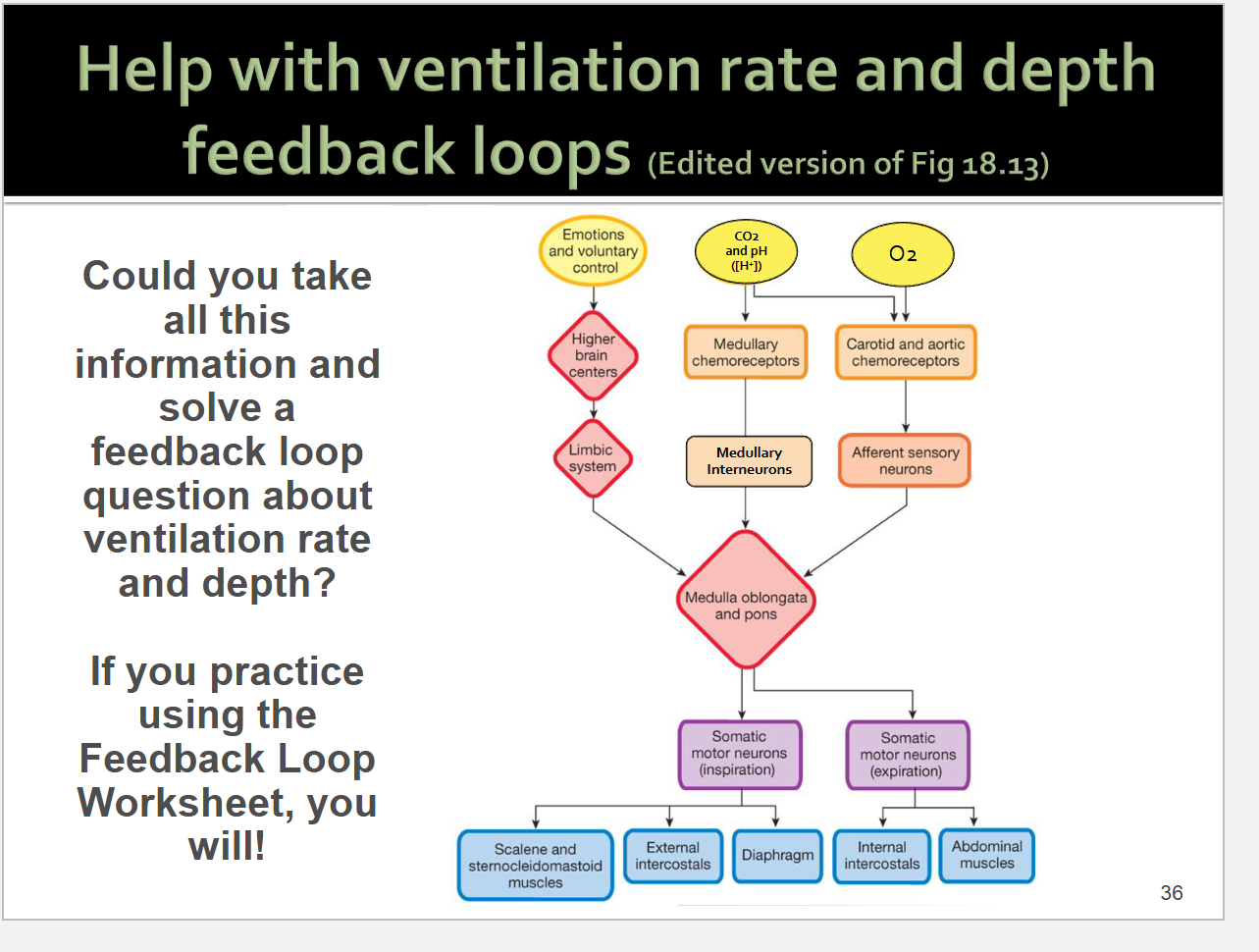
Integrating centers for ventilation: Medulla oblongata
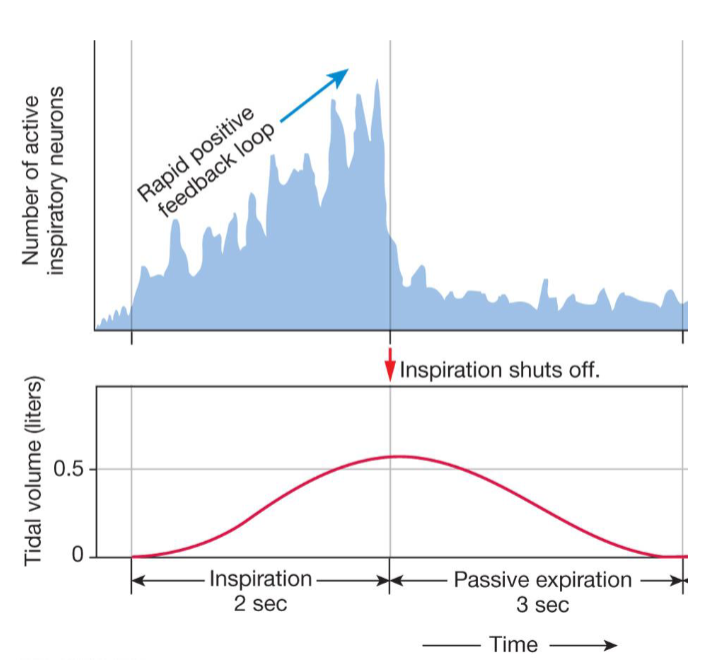
Rhythmic pattern of breathing is controlled by a group of neurons called pre-Botzinger complex
they control the baseline pattern of breathing
stimulate a “ramping” or progressive increase in activity of the phrenic nerve somatic motor neurons that control the diaphragm
When these neurons go silent, expiration largely occurs passively due to relaxation of inspiration muscles and elasticity of the lungs
Integrating centers for ventilation: Pons
Pontine neurons influence the initiation and termination of ventilation, so they modulate ventilation rate and depth
Integrates sensory info from chemoreceptors to module (increase or decrease) ventilation rate and depth as needed
Also allows for higher brain centers to take control of ventilation rate and depth