CARTILAGE AND JOINTS
1/94
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
95 Terms
Supporting CT:
are hard tissues are fibrous: that is, they contain abundant collagen fibers
Hard fibrous tissues also include:
cement and dentine of teeth
Enamel:
a hard tissue of teeth but it is not fibrous
Cartilage has more ECM than cells?
Yes
ECM is produced by cartilage-specific cell types:
chondroblasts and chondrocytes
Cartilage ECM contains:
rich in GAGs and proteoglycans
contains type II collagen, type of collagen which is specific of cartilage
There are 3 types of cartilage, depending on:
whether they have type I collagen or elastin fibers in addition to type II collagen
Cartilage has no:
blood vessels and no nerve fibers
Roles of cartilage:
Is tough yet flexible.
Covers bone surfaces which are part of joints, and enables these bones to move smoothly relative to one other.
Forms body structures that require strength and flexibility, such as the tip of the nose.
Serves as precursor tissue for most bones during development (to be discussed in the lecture on bones).
In anatomical diagrams, hyaline cartilage is typically color-coded:
light blue
In anatomical diagrams, bone is typically color-coded:
light yellow or orange
Hyaline cartilage:
only type II collagen
Elastic cartilage:
type II collagen mixed with elastin fibers
Fibrocartilage:
abundant type I collagen with some type II collagen
Hyaline cartilage subtypes have:
type II collagen fibers, but they have different ECM organization or calcium content
Calcified cartilage:
is hyaline cartilage in the process of differentiating into bone; during this process it accumulates a high amount of calcium in the ECM
Articular cartilage:
is the hyaline cartilage at joint surfaces. Its cells and collagen fibers are organized in a complex manner to withstand compression and provide smooth joint movement.
Chondroblasts and chondrocytes are found only in:
cartilage
The cell types producing the cartilage are:
Chondroblasts and chondrocytes
Chondroblasts also produce:
the cartilage ECM and contribute to cartilage growth and formation
Chondrocytes function for ECM:
maintain and renew the cartilage ECM
Chondroblasts eventually mature into:
chondrocytes after losing the ability to divide
Can chondroblasts proliferate?
Yes
Lacunas:
seemingly empty (clear) spaces around chondrocytes in histological sections
are artifacts which appear during the preparation of cartilage for histology sections, as this preparation sometimes causes the ECM surrounding chondrocytes to shrink or retract, creating an artificial clear space around the cells
Isogenous groups:
are clusters of 2-8 chondrocytes that come from the division of a single cell and remain close to each other
Isogenous groups are embedded:
within ECM and are separated from other isogenous groups by this matrix
How are isogenous groups organized?
Irregularly scattered, rather than organized in a regular pattern
ECM occupies:
~90% of the cartilage volume
Type II collagen provides cartilage with:
resistance to compression
Aggrecan:
a cartilage-specific proteoglycan, which holds water and has shock absorbing ability
Chondronectin:
a cartilage-specific glycoprotein connecting GAGs and type II collagen to integrin receptors present at the plasma membrane of chondrocytes
Territorial matrix:
Is the ECM located closest to the cells in isogenous groups
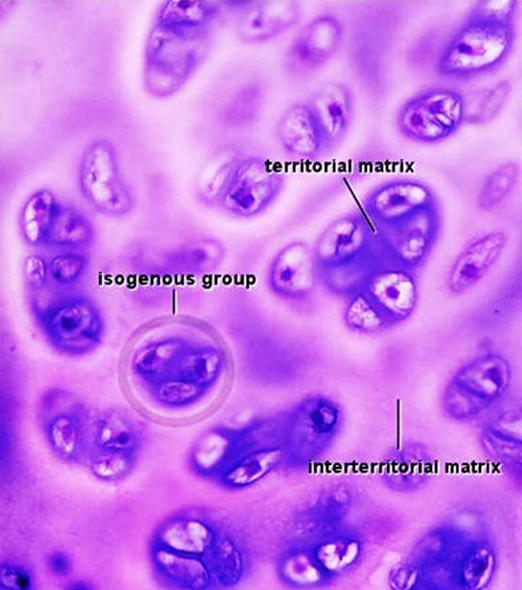
Interterritorial matrix:
lies between isogenous groups
Where is territorial matrix rich?
It is richer in GAGs
How can the territorial matrix and interterritorial matrix be distinguished?
By their staining: the territorial matrix stains more intensely than the interterritorial matrix
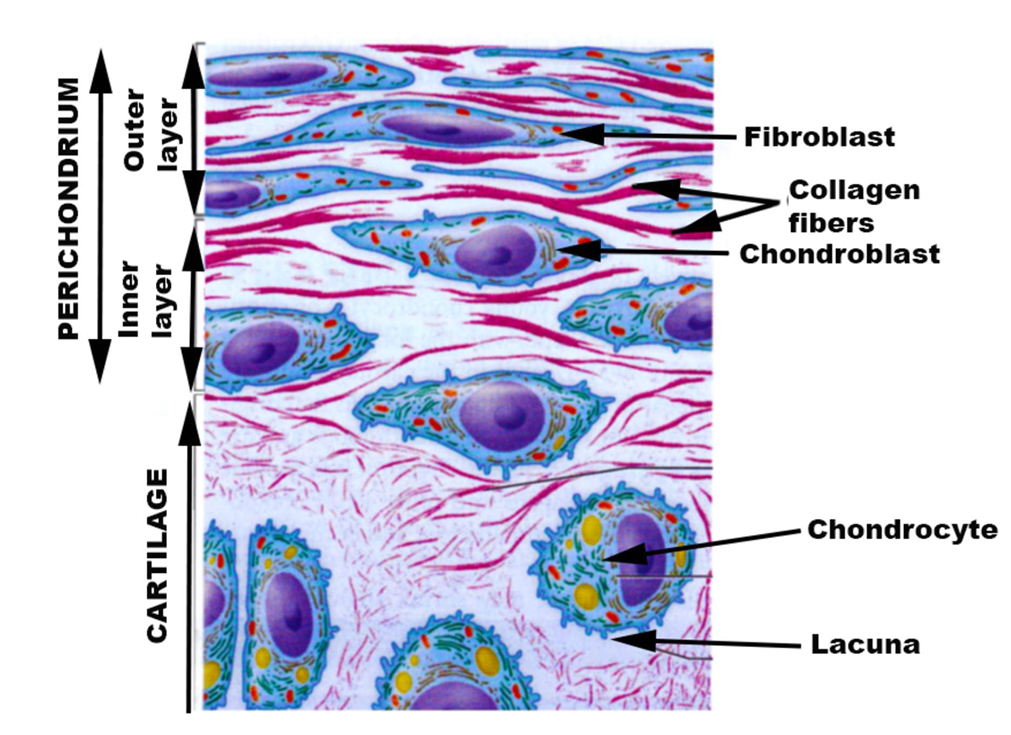
Perichondrium:
Is a thin (0.2-0.4 mm) layer of dense, fibrous connective tissue covering the outer surface of hyaline and elastic cartilages
Does perichondrium cover fibrocartilage and articular cartilage?
No
Perichondrium has abundant:
blood vessels which supply nutrients to cartilage via diffusion
The perichondrium consist of two:
distinct layers: Outer, fibrous layer and Inner, chondrogenic layer
Outer, fibrous layer:
Composed of dense, fibrous connective tissue.
Contains fibroblasts, but not chondrocytes.
Role: protection. Shields the cartilage from mechanical damages (scratches, excess pression).
Inner, chondrogenic layer (in contact with the cartilage):
Contains mesenchymal cells which can differentiate into chondroblasts.
Role: growth. Responsible for to the appositional growth of cartilage (see later in this lecture).
Chondroblasts and chondrocytes receive nutrients and O2 by:
diffusion from the capillaries in the perichondrium
Is cartilage avascular?
Yes, it does contain blood vessels
Does cartilage contain nerve fibers?
No
Why are conditions affecting cartilage painful?
The pain in these conditions comes from nerve fibers present in surrounding structures, such as the perichondrium and adjacent connective tissue.
“Hyaline” means:
glassy, translucent
Hyaline cartilage is named for:
its smooth, shiny, translucent appearance
Hyaline Cartilage general features:
Firm and rubbery.
Durable, but poorly renewable.
Hyaline Cartilage Locations:
most abundant type of cartilage in the body (including articular cartilage).
forms the articular cartilage at the surface of movable joints where it allows smooth gliding between bones.
wall of large respiratory airways (e.g. trachea, bronchi), which are keeps open by its firm consistency.
tip of the nose: provide shape and structure to this body part.
Hyaline Cartilage developmental role:
Can differentiate into bone during fetal development.
Elastic Cartilage Mechanical Properties and Microscopic Features:
Flexible and mechanically strong.
Contains abundant elastin fibers mixed with type 2 collagen.
The outer surface of elastic cartilage is covered by perichondrium.
Elastic Cartilage locations:
Elastic cartilage is present in:
- External ear.
- Some parts of the larynx (voice box).
- Epiglottis (below).
Elastic cartilage has a yellowish appearance.
Fibrocartilage Microscopic Features:
mixture of dense fibrous connective tissue and hyaline cartilage.
contains a mixture of type I and II collagen fibers.
contains a mixture of fibroblasts and chondrocytes.
chondrocytes are either isolated or form linear isogenous groups (as opposed to the oval-shaped isogenous groups in hyaline and elastic cartilages).
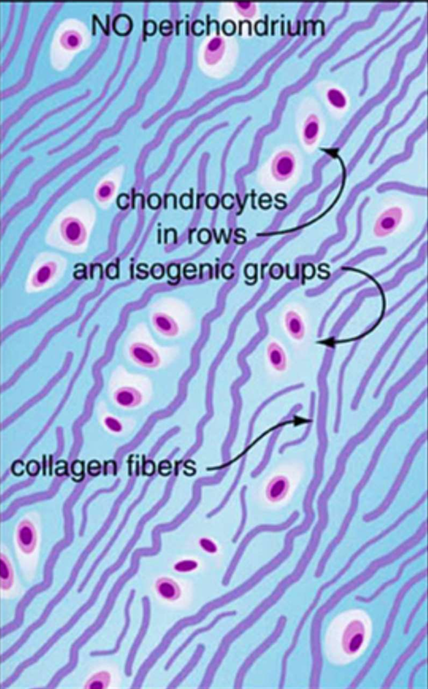
Fibrocartilage distinguishing feature:
in contrast to hyaline and elastic cartilage, the outer surface of fibrocartilage is not covered by perichondrium.
Fibrocartilage locations:
Fibrocartilage is present in areas subjected to high mechanical stress (compression + tension).
1) Some articulations:
- Intervertebral discs.
- Pubic symphysis (junction between the two pubic bones).
- Knee meniscus.
- Temporal mandibular joint (TMJ).
2) The site of insertion of tendons and ligaments into bone.
Fibrocartilage provides:
Resistance to compression at intervertebral joints and knee meniscus.
Resistance to forces pulling puling apart the left and right pubic bones at the pubic symphysis. These forces are especially strong during childbirth.
Chondrogenesis:
the process by which mesenchyme becomes cartilage during embryonic development.
Chondrogenesis Steps:
1) Mesenchyme is the precursor for all types of cartilage
2) Mitosis and cell differentiation produce a tissue with tightly packed rounded cells called chondroblasts. This step is called condensation
3) Chondroblasts produce matrix components and become separated by the ecm that they lay out.
4) Division of chondroblasts with the matrix gives rise to isogenous aggregates surrounded by condensation of ecm.
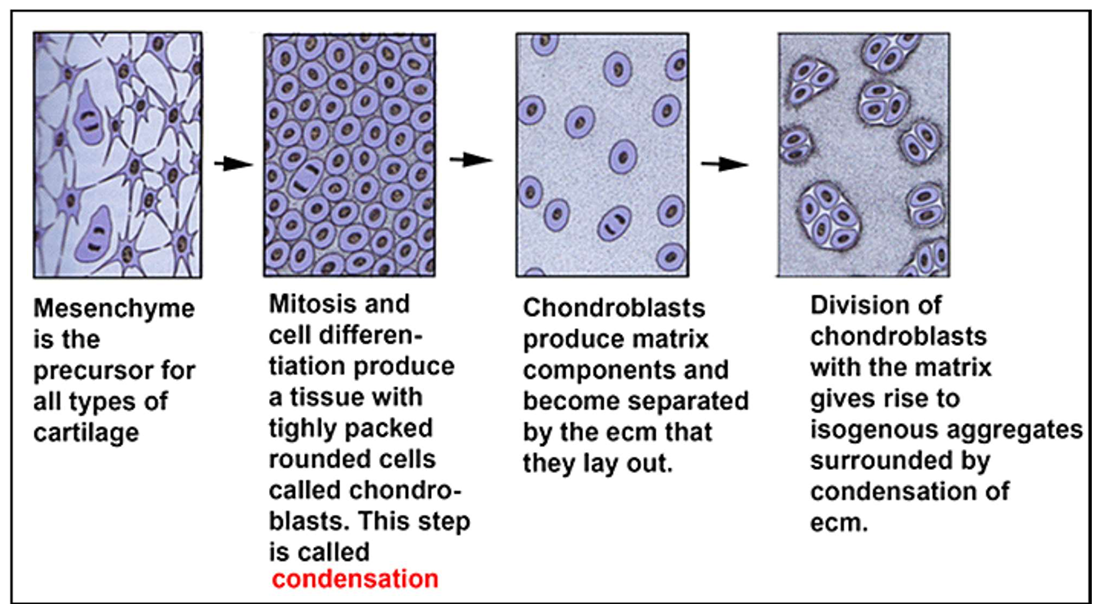
In infants and until the end of puberty, cartilage grows through two concomitant processes:
Appositional growth and Interstitial growth
Appositional growth:
in which the perichondrium adds new layers of cartilage to the outer surface of existing cartilage.- Increases width of cartilage.- Involves differentiation of perichondral cells into chondroblasts.
Interstitial growth:
in which cartilage grows from within.
It is due to chondroblasts proliferation and matrix deposition inside existing cartilage.
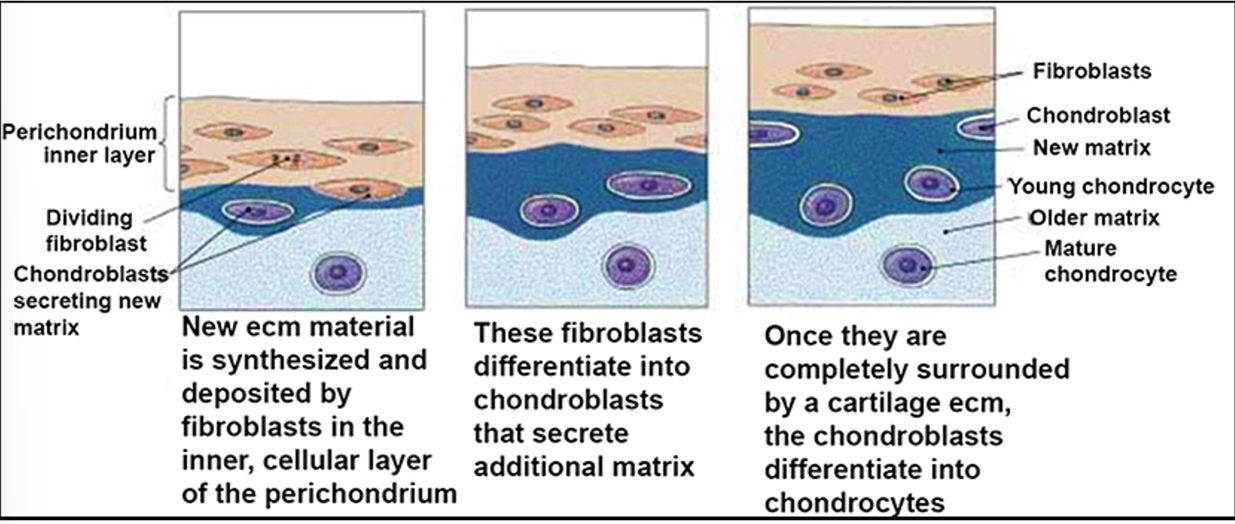
Steps of Appositional Growth of Cartilage:
1) New ecm material is synthesized and deposited by fibroblasts in the inner, cellular layer of the perichondrium
2) These fibroblasts differentiate into chondroblasts that secrete additional matrix
3) Once they are completely surrounded by a cartilage ecm, the chondroblasts differentiate into chondrocytes
Interstitial Growth of Cartilage:
1) Chondrocyte undergo division within a lacuna surrounded by cartilage matrix
2) As the daughter cells secrete additional matrix they move apart, expanding the cartilage from within
Hyaline cartilage capacity for repair:
very limited capacity for repair
Why can’t cartilage repair itself easily?
Because cartilage is avascular (no blood vessels) Therefore key repair cells (macrophages, PMN and platelets) cannot not reach the damaged cartilage to help repair it
After damage, the damaged hyaline cartilage is usually replaced by:
a fibrocartilage scar, which is less functional as original cartilage
Articulations:
is the scientific term for joints. Three types of articulations
Movable joints or synovial joints:
Two bones surfaces covered by cartilage are connected by a synovial membrane and can move relative to each other. Most common type of joints.
Slightly movable articulations:
Two bones are connected by ligaments or fibrocartilage. Allow limited movement.
Immovable Articulations:
Two bones are in direct contact with each other and cannot move relative to each other (e.g. example, bones of the skull). These joints do not contain cartilage.
Articular surfaces:
are the surfaces of bone covered by articular cartilage
Articular capsule:
dense fibrous CT enclosing and holding the articular surfaces together
Ligaments:
strengthen the fibrous capsule
Synovial membrane (synovium)
a specialized connective tissue lining the inner surface of the articular capsule
Synovial cavity:
a sealed space containing the synovial fluid
Synovial fluid:
lubricates the joints and reduces friction between the articular surfaces
Articulate Cartilage:
covers the bone surfaces involved in a synovial joint.
It is a type of hyaline cartilage with unique features in the organization of chondrocytes and collagen fibers, adapted to withstand mechanical stress in joints.
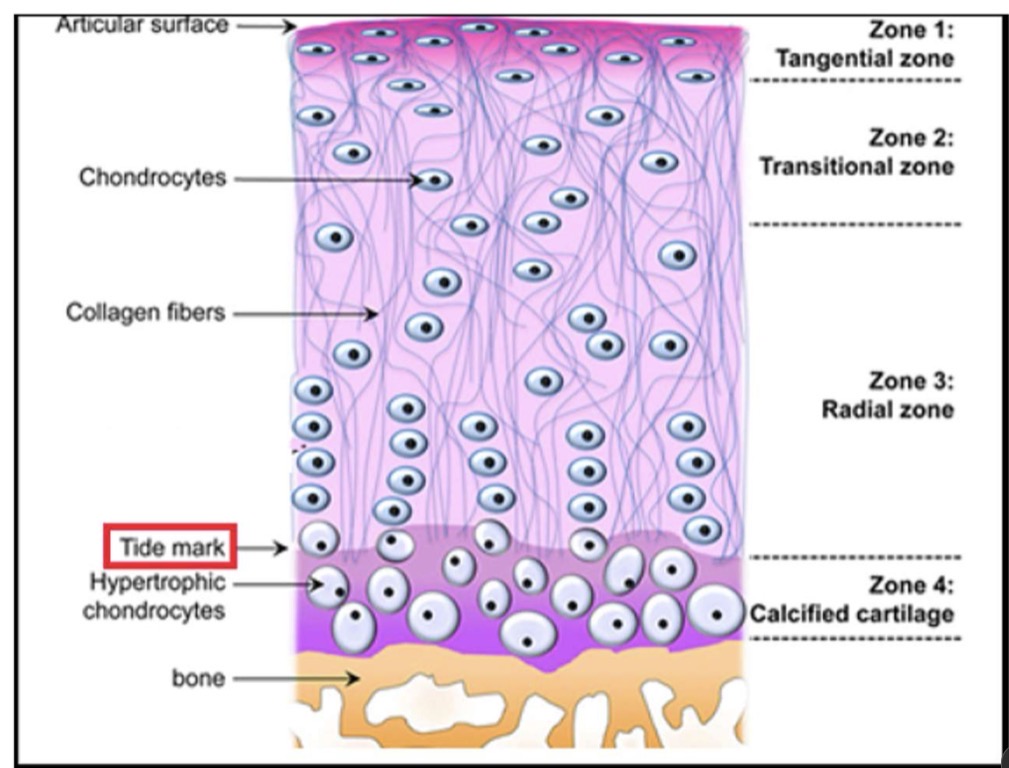
Calcified cartilage (zone 4):
contains hypertrophic chondrocytes and an ECM rich in calcium
Calcified cartilage anchors:
the articular cartilage into the underlying bone
Tidemark:
a thin line separating the calcified cartilage (stains strongly) from uncalcified cartilage (stains weakly)
Hyaline cartilage above the tidemark is divided into three
zones:
Radial, transitional, tangential (superficial) zone
Radial zone:
chondrocytes are spherical and organized in columns or rows
Transitional zone:
chondrocytes are somewhat flattened and randomly arranged
Tangential (superficial) zone:
chondrocytes are flattened shape, adapted to resist compression forces during joint movement
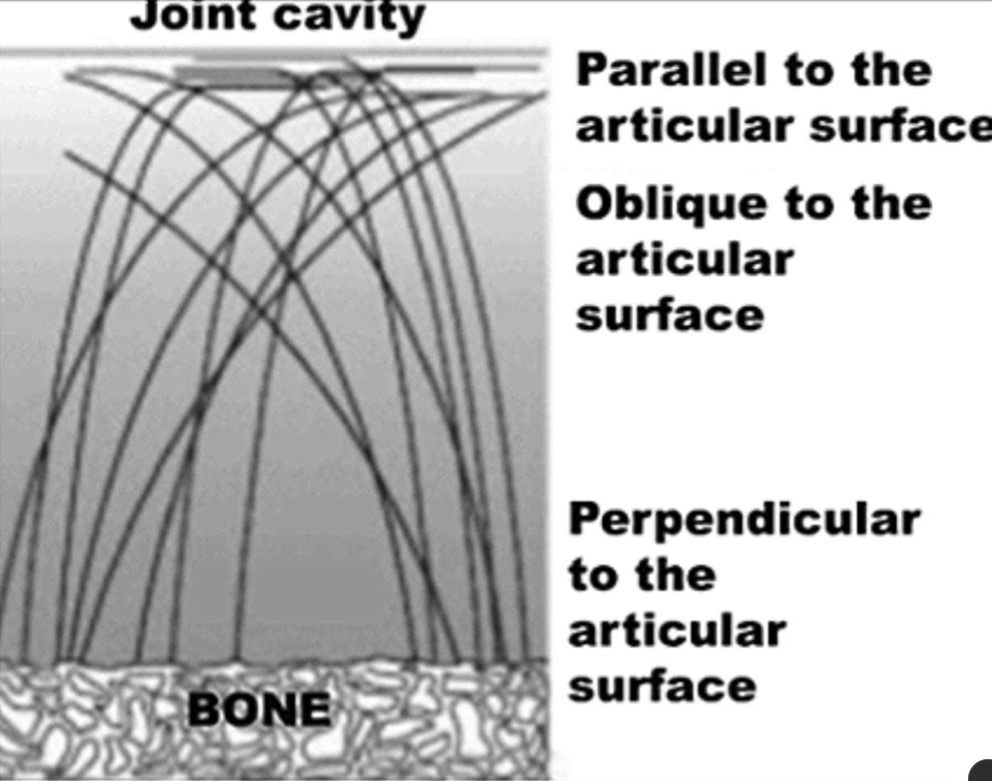
Organization of Collagen Fibers in Articular Cartilage:
In articular cartilage, type II collagen fibers form an arch which base is anchored in the bone. Close to the synovial cavity, the collagen fibers lay parallel to the surface.
This arrangement enables articular cartilage to withstand compression forces during joint movement.
The synovial membrane contains two main cell types:
Type A synovial cells and Type B synovial cells
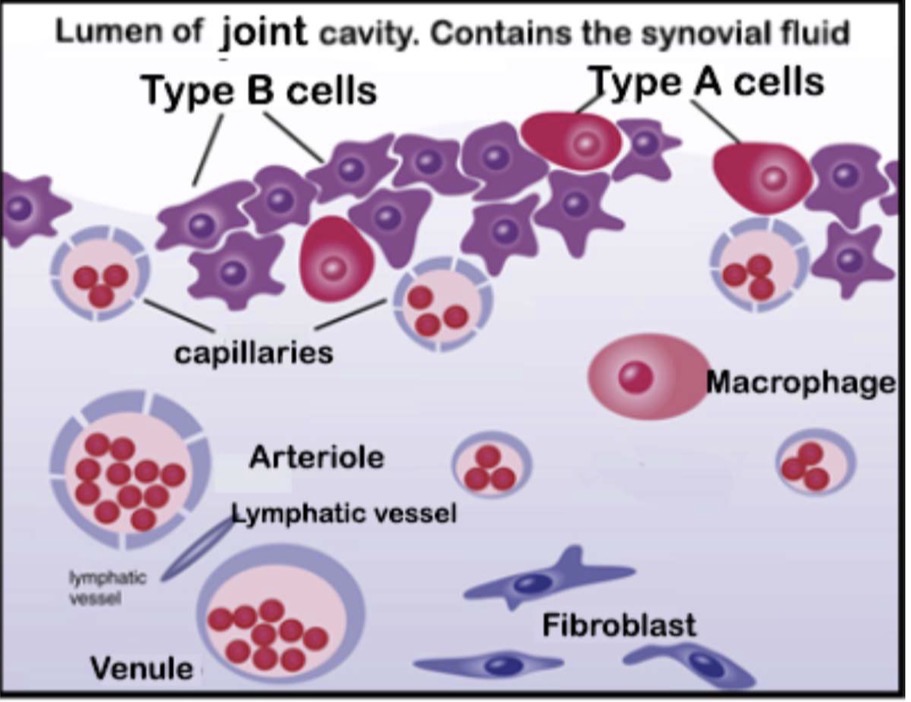
Type A synovial cells:
- mAcrophage-like, phagocytic cells.
- represent ~25% of the cells in the synovial membrane.
- phagocytize wear and tear debris from articular cartilage.
Type B synovial cells:
responsible for the production of synovial fluid
Synovial fluid:
is a clear, viscous fluid produced by type B synovial cells
Composition of synovial fluid:
mainly water, hyaluronic acid, and specific proteoglycans such as lubricin
Synovial fluid fills the joint cavity and forms:
a thin (~50 ųm) layer of fluid between opposing articular cartilage surfaces
Two roles of synovial fluid:
1) Lubrication: reduces the friction between opposing articular cartilage surfaces during joint movement.
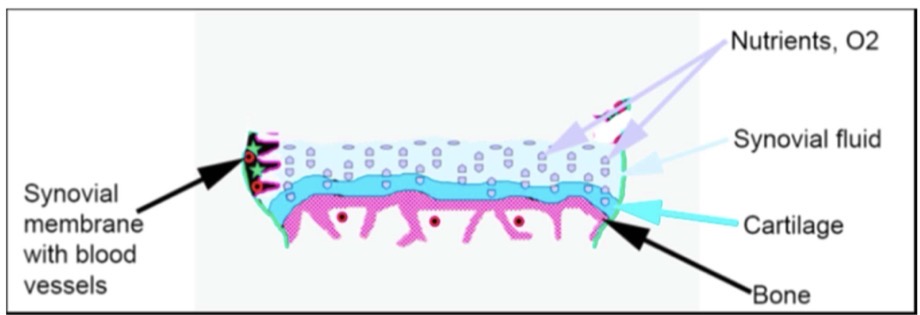
2) Nutrition: serves as a medium for the diffusion of nutrients and O 2 from capillaries in the synovial membrane into the articular cartilage.
Nutrition of Articular Cartilage:
Articular cartilage does not have blood vessels.
Nutrients and O 2 are supplied by capillaries in the synovial membrane.
The compression and decompression of articular cartilage during joint movement facilitate the diffusion of nutrients and O 2 from the synovial fluid into the cartilage.
Rheumatoid arthritis:
is a chronic inflammatory disease of the synovial membrane
Rheumatoid Arthritis occurs when:
macrophages in the synovial membrane release in the synovial cavity enzymes and inflammatory mediators that damage the articular cartilage
affects approximately 1% of the global population