Eye and Ear
1/89
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
90 Terms
What is the diagram to show the structure of the eye?
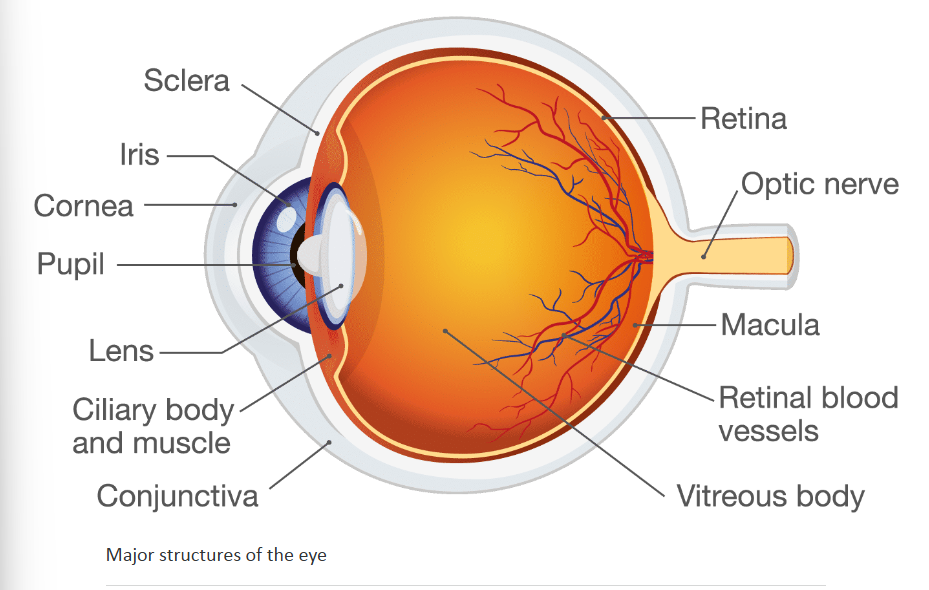
What part of the eye does conjunctivitis affect?
Conjunctiva
What part of the eye conditions affect the eyelids?
Blepharitis, styes
How are our eyes lubricated?
Tears are secreted into the upper and lower conjunctival sacs and lubricate the surface of the eye through blinking, helping to keep the eye healthy
Why do medications to treat eye conditions have a short shelf life?
Must remain sterile to prevent bacteria entering the medication and then into the eyes
What is conjunctivitis?
Inflammation of the conjunctiva - sometimes known as pink eye
What are the main types of conjunctivitis and how can they be split up further?
Infective or allergic - infective includes bacterial and viral
What are the causes of infective conjuncitivis?
Virus or bacteria enters the eye and is contagious, spreading easily from person to person. Can also be a from a cold
What are the causes of allergic conjunctivitis?
Immune system attacks something e.g., pollen, makeup.
What are the symptoms of infective conjunctivitis?
Redness, watery eyes, discomfort, sticky coating of the eyelashes, gritty feeling in the eyes and only 1 eye affected or 1 eye shows symptoms before the other
What are the symptoms of allergic conjunctivitis?
Redness, watery eyes, discomfort, very itchy eyes and both eyes usually affected
What are the warning signs for allergic/infective conjunctivitis?
Anyone who has pain in the eye
Babies and young children
Redness that extends onto the iris (the coloured part of the eye)
Anyone whose vision is affected
If the pupil looks unusual
If the patient also has a rash on the face or scalp
Anyone who complains that light hurts their eyes (photophobia)
If you suspect a foreign body is in the eye
If infective conjunctivitis has been present for more than a few days
If allergic conjunctivitis appears to only be affecting one eye
Anyone who suffers, or has previously suffered from glaucoma
Anyone who has previously had eye surgery or laser treatment
Anyone taking prescribed medication
Women who are pregnant or breastfeeding
Anyone who wears contact lenses
If treatment has not helped.
What is the treatment for allergic conjunctivitis?
Sodium cromoglicate or antihistamine eye drops to counteract the allergic reaction
How is infective conjunctivitis treated?
Can heal on its own but can use chloramphenicol antibiotic eye drops and eye ointment - can be sold for adults and children over 2. 5 days treatment and have to finish the whole length of treatment
What advice must you give patients when purchasing chloramphenicol?
If symptoms do not improve after 48 hours seek advice from your doctor or pharmacist
Do not use for more than 5 days without consulting your doctor
Any remaining product should be discarded after the five day course of treatment
Drops need to be stored in the fridge
A separate product should be used for each affected family member to prevent cross infection.
Patients who wear contact lenses/had eye or laser eye surgery should be referred to the pharmacist
What are the side effects of using chloramphenicol?
Blurred vision, mild stinging/burning on application, possible eye discolouration
Who cannot have chloramphenicol?
Patients who have a history of hypersensitivity/allergy to chloramphenicol or to any other ingredient of the drops
Patients who suffer from recurrent eye infections
Patients with a personal or family history of blood and bone marrow problems
Patients who are pregnant or breastfeeding.
What is propamidine?
Antibacterial ingredient in eye drops/ointments - can be used to treat infective conjunctivitis but not as effective
What are the side effects of propamidine?
Blurred vision, mild stinging/burning on application
What are the cautions with propamidine?
Patients who wear contact lenses referred to pharmacist, if symptoms worsen/don’t improve after 48 hours they should speak to a doctor
What is additional advice you can give for patients suffering with conjunctivitis?
Infective conjunctivitis is very contagious so patients should be advised not to share face cloths and towels to prevent the spread of the infection
To provide relief from symptoms, boil and cool water, then use a cotton wool swab to wipe from the inside edge of the eye to the outside and discard
It is important when using eye drops or ointment to not touch the eye with the nozzle of the container
Washing hands before and after touching the eyes or applying medication will also help prevent the spread of infection
If your patient wears contact lenses they should remove them until the infection has completely cleared.
What tips can you give patients to help prevent conjunctivitis?
People who wear contact lenses are more susceptible to eye infections so good contact lens care and hygiene is very important
Anyone who is suffering from a cold should wash their hands frequently and avoid touching their eyes.
What are the causes of dry eyes?
Increased evaporation from the eye leading to the underproduction of tears
Increased tear drainage
Decreased tear production.
Central heating and air conditioning symptoms
Eye strain e.g. by looking at a computer screen for too long
Some medication can also cause dry eyes by reducing tear secretion.
What are the symptoms of dry eye?
Increased tear production, causing streaming
Irritation
Burning
Grittiness
What patients with dry eyes should be referred to the pharmacist?
Anyone who has pain in the eye
Anyone who has a long term (chronic) dry eye condition
Anyone whose vision is affected
If the pupil looks unusual
If the patient also has a rash on the face or scalp
Anyone who complains that light hurts their eyes (photophobia)
If you suspect a foreign body is in the eye
If your patient suffers, or has previously suffered from glaucoma
Any patient who regularly suffers from eye fatigue as the patient may need to have an eye test
Anyone who has previously had eye surgery or laser treatment
Anyone taking prescribed medication
Babies and children under 6
Anyone who is pregnant or breastfeeding
Anyone who wears contact lenses
If treatment has not helped
Patients with long-term symptoms who have not had their condition diagnosed by a doctor should also be referred to the pharmacist. This is to ensure that the cause of the dry eyes can be accurately identified.
What products can be used to lubricate dry eyes?
Hypromellose, polyvinyl alcohol, carbomer 940, wool fat, sodium hyaluronate
What are the possible side effects of patients who use products for dry eyes?
Blurred vision, mild stinging
What are the cautions for dry eye drop products?
Refer to pharmacist if pregnant or breastfeeding
Patients who wear contact lenses should be referred to the pharmacist
If the patient has not been advised by the doctor to use an artificial tear product, they should be referred to the pharmacist
Stop using if excessive tearing occurs.
What are the treatment options for irritated eyes?
soothing eye lotions or drops, which bathe the eye in liquid, remove particles, and relieve dryness due to eye fatigue. Many of the products available contain an astringent, which refreshes the eyes
What is the shelf life of products that are used for irritated eyes?
Usually 28 days but will be on packaging
What does naphazoline hydrochloride do?
Reduced redness in the eyes - has a maximum dose associated with it
What does witch hazel do for irritated eyes?
Reduced soreness in the eyes - can be used when required
What additional advice can you give patients with irritated eyes?
Set up your computer to minimise eye strain. The monitor should be at (or just below) eye level
Take regular breaks from staring at a screen
Using a humidifier can help to add moisture to surrounding air and reduce symptoms.
What advice can you give to help prevent irritated eyes?
Wraparound sunglasses will help to protect the eyes from the environment
Avoid eye makeup as this can block the glands in the eyelids.
What is a stye?
Infection of an eyelash follicle causing a small, swollen and sometimes painful boil on the eyelid
What are external styes?
Affect the root of the eyelash, self-limiting and
What are internal styes?
Affect the inside of the eyelid - can last longer and need to be referred to the pharmacist
What are the causes of styes?
Caused by a bacterial infection
What are the symptoms of a stye?
Small, painful, pimple-like lump on the edge of the eyelid – external stye
Lump on the inside of the eyelid – internal stye
Watery eye
Redness of the eye and eyelid.
What are the warning signs of a stye?
Anyone who has an internal stye
Anyone who has had a stye for more than one week
Patients who have already tried medication to treat the stye
Anyone who has pain in the eye
If the patient also has a rash on the face or scalp
Anyone who complains that light hurts their eyes (photophobia)
If you suspect a foreign body is in the eye
Anyone who suffers, or has previously suffered from glaucoma
Anyone who has previously had eye surgery or laser treatment
Babies and children under 6
Anyone taking prescribed medication
Anyone who is pregnant or breastfeeding
Anyone who wears contact lenses.
What is the treatment for a stye?
A warm compress held against the eye 3-4 times a day encourages to release pus and speed up healing - once it has burst pain will subside
What additional advice can you give for a stye?
Always wash your hands before touching your eyes
If the patient wears contact lenses they should remove them until the infection has completely cleared.
What tips can you give to prevent styes?
Do not share face cloths and towels to prevent the spread of the infection
Apply a warm compress, such as a cotton bud soaked in warm water to the stye three or four times a day. This may bring it to a head and speed up the healing process.
What are the 2 types of blepharitis?
Anterior and posterior
What is anterior blepharitis?
The inflammation affects the outside margin of the eyelids and is usually caused by a bacterial infection. This can also sometimes be a result of seborrheic dermatitis, a condition that causes oily skin.
What is posterior blepharitis?
The inflammation affects the inside front edge of the eyelid and is usually caused by something affecting the glands on the rim of the eyelids.
What are the symptoms of blepharitis?
Swollen eyelid margins
Itchy, red and sore eyelids
Feeling of grit in the eyes
Eyelids that stick together and difficult to open on waking
Loss/abnormal growth of eyelashes.
What are the warning signs for blepharitis?
Anyone with pain in the eye
Anyone with signs of infection; these patients may require antibiotic treatment
Anyone who has already tried treatment
Anyone taking prescribed medication
Anyone who wears contact lenses.
What treatments options are available for blepharitis?
No medical treatment - products used can be to keep the eyelids clean and reduce infection risk
What can patients do for an eye-cleaning regime to help blepharitis?
Apply a warm cloth/cotton wool to the eyelids
Clean the eyelids using cloth/cotton wool bud with mild baby shampoo and warm water
Avoid eye makeup
What advice can you give patients with blepharitis?
Healthy eye cleaning regimen, use a warm compress and massage eyelids to help push melted oil out of glands
What prevention tips can you give patients with blepharitis?
Avoid eye makeup and use eyelid cleaning solutions 2-3 times a week, even when symptoms aren’t present
How should patients administer eye drops?
wash your hands
tilt the head backwards
look up towards the ceiling
pull the lower eyelid down
hold near as possible
1 drop in the lower eyelid and blink a few times
press gently on the inner eye to make sure its fully absorbed
wipe away excess with a tissue
repeat if multiple drops needed
most throw away after 28 days
How should patients administer eye ointments?
wash hands
tilt the head backwards
look up towards the ceiling
pull the lower eyelid down
put a thin layer of ointment along the inner eye
close the eye and move the eyeball from side to side
wipe excess using a clean tissue
vision may be blurred but is cleared by blinking
most = throw away after 28 days
What is available to help patients struggling to deliver eyedrops themselves?
Devices to help squeeze bottles, align the bottle correctly over the eye or both
What is the diagram to show major structures of the ear?
Can only recommend products for the outer ear
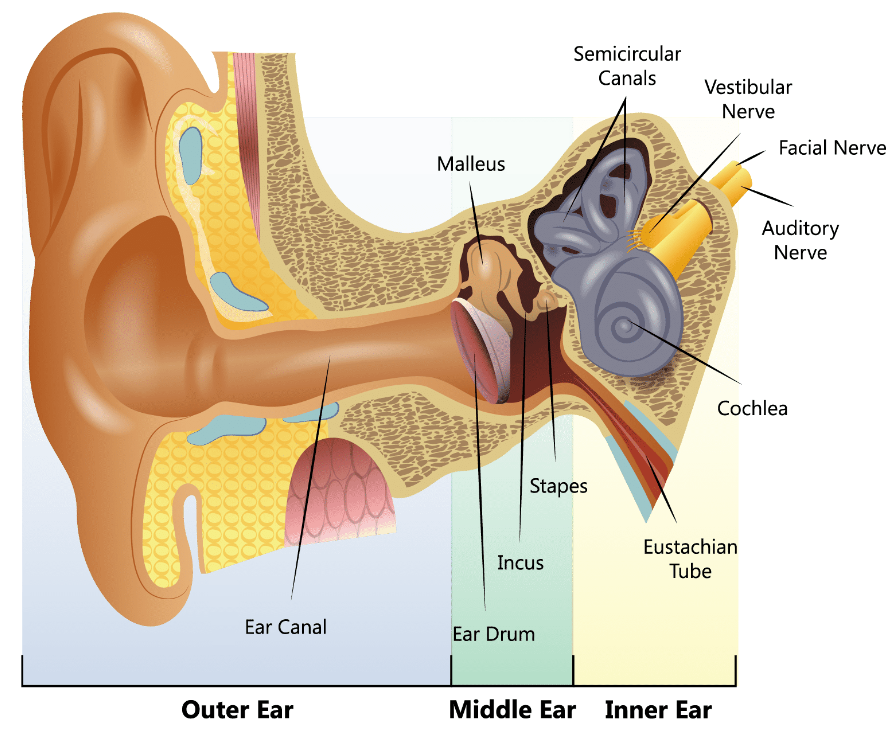
What are the causes of a build up of wax in the ear?
Some people produce wax at a faster rate than others
Elderly people tend to have dryer earwax which can become impacted
Narrow ear canals in some people will lead to a build-up of wax causing a blockage
Misguided attempts to clean the ears, such as with a cotton bud, can push earwax further into the ear causing a blockage.
What are the symptoms of excess earwax?
blocked feeling in the ear
difficulty hearing
itching
earache
What are the warning signs for earache?
Ringing in the ears or dizziness – this indicates a problem in the inner ear
Pain in the ear – if the patient has a lot of pain in the ear this is likely to be an infection
Foreign body – children are the most likely age group to have something stuck in their ear so if you suspect this is the case you must refer them to the pharmacist
Anyone who has already tried medication to remove earwax
Babies and children.
What does OTC treatment for excess earwax aim to do?
Soften and remove the earwax - some may still need to have their ears syringed by a doctor. Important to not insert anything into the ear to remove earwax and could lead to wax further in the ear or perforation of the eardrum
What are the side effects of peroxide based products to remove earwax?
Mild stinging/burning on application
Mild bubbling sensation
Tinnitus (ringing in the ear).
What are the cautions of using peroxides to remove excess earwax?
If symptoms worsen or do not improve after 48 hours the patient should see their doctor or pharmacist
Avoid if the patient suffers from dizziness
Avoid if the ear drum is damaged or there is anything wrong with the ear e.g. pain.
What are the side effects of using docusate to remove excess earwax?
Mild stinging
What are the cautions of using docusate to remove excess earwax?
Avoid if patient has perforated eardrum or if inside of the ear is sore
How does docusate work to remove excess earwax?
Breaks and softens wax, helping to clear the blockage - drops are used for 2 nights
How do peroxide based products work to remove earwax?
Break the earwax into smaller pieces, making it easier to remove
What are the side effects of sodium bicarbonate for excess earwax?
Dryness in the ear canal
What are the cautions of using sodium bicarbonate for earwax?
Avoid if patient has a perforated ear drum
How does sodium bicarbonate work to remove excess earwax?
Softens and dries hardened earwax - easier to remove
How do oils help remove earwax?
Gently soften and remove earwax - used once or twice a day for 3-4 days e.g., arachis oil, almond oil, camphor oil, olive oil
What are the side effects of oils for removing earwax?
Mild irritation
What are the cautions for oils to remove eardrops?
Allergies so direct patients to PIL
What other products can be used to prevent earwax formation?
Audiclean - made of purified seawater and cleanses the ear by dispersing earwax. Can be used from age of 6 months and prevents wax plugs forming
What additional advice can you give patients with excess earwax?
Always advise the patient to read the patient information leaflet before using the product to make sure they use it correctly and get the best from the medicine
Ensure the patient uses the product for the recommended length of time to ensure successful treatment
Some patients will use simple olive oil or almond oil to soften earwax. They may ask to buy the oil and a separate dropper bottle. This may be cheaper than some of the products you can buy OTC however the oil may not be sterile and will not contain any preservatives to kill bacteria.
What tips can you give patients to prevent excess earwax?
Never try to clean the ears or remove wax by inserting an implement in the ear
Patients prone to excess earwax can use a product like Audiclean® to safely clean the ear canal and help prevent the build-up of wax plugs.
What is otitis externa?
Inflammation of the outer ear canal - can be due to infection, allergies etc
What are the possible causes of otitis externa?
Swimming - Otitis externa is five times more common in regular swimmers compared to non-swimmers. This is due to the water, which gets into the ear canal. In fact, otitis externa is sometimes called ‘swimmer’s ear’
Weather - Otitis externa is more likely to develop in hot, humid, and ‘sweaty’ weather. It is more common in hot countries
Skin problems - Eczema or psoriasis are both skin conditions which may affect the ear canal
Ear syringing to clear earwax - This may irritate the ear canal and cause inflammation
Bacterial infection – Bacteria can lead to inflammation and infection.
What are the symptoms of otitis externa?
Swelling of the ear canal
Redness and scaling around the ear canal
Itching
Discomfort and a feeling of pressure in the ear
Pain.
What are the warning signs for otitis externa?
Severe pain – this normally indicates a middle ear infection, otitis media, and requires referral
Fever – this could also be a sign of otitis media
Dizziness, loss of balance
Nausea or vomiting
Anyone who has discharge from the ear
Anyone who has loss of hearing
If the inflammation has spread to the whole of the ear
Anyone who suffers from eczema or psoriasis
If symptoms do not clear up after using 7 days of treatment
Anyone who has tried medication already
Children under 12 years.
What are the main treatment options for otitis externa?
Acetic acid and analgesics e.g., ibuprofen and paracetamol
How does acetic acid work? EARCALM
Acts as an antifungal and antibacterial in the ear calm - only for adults and children over 12. Treatment continues 2 days after symptoms have disappeared - no improvement after 1 week the treatment should be stopped and patient referred to GP.
What are the side effects of using acetic acid for otitis externa?
Stinging/burning in the first few days of treatment
What are the cautions for using acetic acid?
Patient has a perforated ear drum
What advice can be given to patients with otitis externa?
As a rule, do not leave balls of cotton wool in the ear canal. This may block debris which needs to come out. However, if the discharge is heavy, patients may need to place some cotton wool lightly in the outer part of the canal to mop up the discharge. If patients use cotton wool, they should replace it frequently with a fresh piece
Do not try and clean the ear canal with cotton buds. If patients stick buds or other objects into their ear, they may damage/irritate the inflamed skin and make things worse. Patients should just clean the outside of the ear with a cloth after any discharge appears.
What tips can patients be given to prevent otitis externa?
Try not to let soap or shampoos get into the ear canal. Patients can do this when they have a shower by placing a piece of cotton wool coated in petroleum jelly (Vaseline) into the outer ear
Do not use corners of towels or cotton buds to dry any water that does get in the ear canal. This will push things further in; let the ear dry naturally
Try not to scratch or poke the ear canal with fingers, cotton wool buds, towels, etc.
Do not clean the ear canal with cotton buds. Patients may scratch, irritate, and push wax or dirt further into the ear. The ear cleans itself and bits of wax will fall out now and then
Advise swimmers to try and keep their ears dry. They can do this by wearing a tightly fitting cap that covers the ears. Some swimmers use silicone rubber, or wax, earplugs, but these should only be used if they do not irritate the skin in the ear canal.
What is otitis media?
Complication from a cold, build-up of mucus - the Eustachian tube becomes blocked/swollen due to mucus and makes an infection easier to develop
What are the symptoms of otitis media?
Severe earache - throbbing or sharp pain in 1 or both ears
Dizziness
Loss of balance
Nausea and vomiting
Fever and other cold-like symptoms
Pus or discharge from the ear.
What is the treatment for otitis media?
Course of antibiotics - must be referred to the pharmacist
What happens if otitis media isn’t treated properly?
Ruptured eardrum
How should patients administer ear drops?
Hold the bottle in your hand for a few minutes before putting the drops in, to warm the solution.
This makes insertion more comfortable.
Tilt your head to one side with the ear pointing towards the ceiling.
With one hand straighten the ear canal: For adults gently pull the top of the ear up and back, For children gently pull the ear lobe down and back.
With the dropper in the other hand, hold it as near as possible to the ear canal, without touching the ear.
Squeeze the right number of drops into the ear (as directed by the product).
Keep the head in the tilted position for several minutes (some products advise you to insert a cotton wool plug in the ear to keep the drops in).