PHYSIO: Ch.14 pt.2 - Blood, Heart, Circulation
1/35
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
36 Terms
The ventricles completely empty when they contract in systole.
True
False
False (resulting in EDV)
A medication that blocks the calcium channels in the heart muscle would cause a decrease in heart rate.
True
False
True
The __________ conducts impulses from the AV node to the bundle branches, which lead to the Purkinje fibers.
AV valve
ventricular septum
AV bundle
SA node
AV Bundle (SA node goes SA→ AV)
Within the blood vessels, valves are found in the __________.
arteries
capillaries
arterioles
veins
veins (have least amt. of pressure so needs valves to push blood through)
The action potential of non-pacemaker cells is due to the __________.
inward diffusion of Na+
inward diffusion of Ca2+
inward diffusion of K+
outward diffusion of K+
inward diffusion of Na2+ (just like pacemaker cells)
Closure of the atrioventricular valves occurs at the end of diastole/beginning of systole.
True
False
True (“lub” of ventricular systole - “dub” of ventricular diastole ~ SL valves closed)
Which of the following statements about cardiac muscle cells is FALSE?
the resting membrane potential of autorhythmic cells is maintained by sodium and potassium If channels
in autorhythmic cells, at threshold, calcium flows into the cell
contractile cells have a resting membrane potential of -85mV
when contractile cells are stimulated by nearby cells, sodium flows into the cell
only autorhythmic cells are repolarized by potassium efflux
only autorhythmic cells are repolarized by potassium efflux (autorhythmic cells and contractile cells can both be repolarized)
In a complete AV node block, __________.
no signals pass into the ventricles
the atria will be paced by the SA node
the ventricles contract due to ectopic pacemakers
All of the choices are correct.
All of the choices are correct.
Myocardial cells exhibit a plateau phase instead of quickly repolarizing. This is due to __________.
inward diffusion of calcium through slow Ca2+ channels
inward diffusion of sodium through fast Na+ channels
inward diffusion of potassium through voltage-gated K+ channels
outward pumping of sodium by the Na+/K+ pump
inward diffusion of calcium through slow Ca2+ channels (slow as to avoid tetanus)
The period of time when the atria relax is called:
atrial diastole
atrial systole
ventricular diastole
ventricular systole
atrial diastole
Ventricular fibrillation __________.
occurs when the ventricles contract in a rapid, coordinated manner
is not life threatening
occurs when the ventricles contract in a rapid, uncoordinated manner
is induced by defibrillators
occurs when the ventricles contract in a rapid, uncoordinated manner (hence defibrillators needed to reset heart)
The period of time when the ventricles relax is called:
atrial diastole
atrial systole
ventricular diastole
ventricular systole
ventricular diastole
What causes the semilunar valves to close?
Higher pressure in the ventricles than in the atria
Higher pressure in the aorta and pulmonary trunk than in the ventricles
Higher pressure in the atria than in the ventricles
Higher pressure in the ventricles than aorta and pulmonary trunk
higher pressure in the aorta and pulmonary trunk than in the ventricles (all valves closed)
Which of the following statements about cardiac muscle cells is FALSE?
the resting membrane potential of autorhythmic cells is maintained by sodium and potassium If channels
in autorhythmic cells, at threshold, calcium flows into the cell
contractile cells have a resting membrane potential of -85mV
when contractile cells are stimulated by nearby cells, potassium flows into the cell
both autorhythmic and contractile cells are repolarized by potassium efflux
when contractile cells are stimulated by nearby cells, potassium flows into the cell (No, NA+ channels are opened similar to Autorhythmic)
The action potential of cardiac pacemaker cells is caused by __________.
inward diffusion of Na+
inward diffusion of Ca2+
inward diffusion of K+
outward diffusion of K+
inward diffusion of Ca2+
Resistance to blood flow is controlled most by:
arteries
arterioles
veins
venules
arterioles
Which type of an AV node block occurs when no atrial waves can pass through the AV node?
First-degree
Second-degree
Third-degree
Fourth-degree
third-degree
Which of the following statements about excitation-contraction coupling of myocardial cells is TRUE?
calcium influx from the ECF happens before influx from the SR
the major source of calcium in is from the SR
the sliding filament mechanism is the same as for skeletal muscle
all of the above are TRUE
all of the above are TRUE
The lymphatic system is responsible for all of the following EXCEPT:
transport of ISF/lymph
transport of fat from GI tract to blood
resistance to disease
transport of blood
transport of blood
End diastolic volume is the volume of blood in the:
ventricles after ventricular diastole
ventricles after ventricular systole
atria after atrial diastole
atria after atrial systole
ventricles after ventricular diastole
The __________ are the last part of the electrical conducting system of the heart.
SA node
AV bundle
Bundle of His
Purkinje fibers
Punkinje fibers
The T wave of the ECG represents atrial repolarization.
True
False
False (ventricular depolarization)
If the __________ were not properly functioning, congestion in the venous system would be an expected sign.
tricuspid valve
bicuspid valve
tricuspid valve
Failure of the SA node to depolarize would result in an ECG __________.
lacking a T wave
lacking a QRS complex
lacking a P wave
that is isoelectric
lacking a P wave
Which of the following statements about cardiac muscle cells is FALSE?
The resting membrane potential of autorhythmic cells is maintained by sodium and potassium If channels
In autorhythmic cells, at threshold, calcium flows out of the cell
contractile cells have a resting membrane potential of -85mV
when contractile cells are stimulated by nearby cells, sodium flows into the cell
both autorhythmic and contractile cells are repolarized by potassium efflux.
in autorhythmic cells, at threshold, calcium flows out of the cell
During isovolumetric ventricular contraction, ventricular pressure is __________.
increasing
decreasing
unchanged
increasing
Briefly describe the structure of the heart (chambers, ,circulation path, valves)
2 atria + 2 ventricles separated by septa
Pulmonary (deoxygenated): R.ventricle → lungs → L.Atrium
Systemic (oxygenated): L.Ventricle →Tissues → R.Atrium
AV(tricuspid + bicuspid/mitral) + SL valves (pulmonary/aorta)
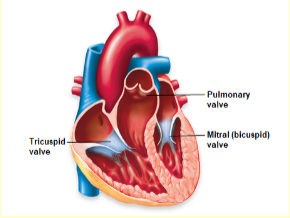
What is the purpose of the valves? How do they function?
Valves prevent the backflow of blood.
AV:
opens when: Atria pressure > Ventricle Pressure; closes inversely
SL:
opens when: Ventricle pressure > Arteries pressure; closes inversely
Define: diastole; systole; end diastolic volume; end systolic volume
Diastole: relaxation
Systole: Contraction
EDV: volume of blood in ventricles after atrial systole (blood before being ejected AKA preload)
ESV: volume of blood in ventricles at the end of ventricular systole and is never 0 (AKA afterload)
Define: isovolumetric contraction, isovolumetric relaxation
Isovolumetric contraction: no blood moving, both valves closed, and ventricles contracted. Ventricular pressure is increasing.
Isovolumetric relaxation: no blood moving, both valves closed, and ventricles relaxed
What causes the heart sounds?
“Lub” = closure of the AV valves
“Dub” = closure of the SL valves
Describe the excitation of autorhythmic cells of the heart. How does the ANS affect excitation?
Autorhythmic cells:
RMB potential more permeable to Ca influx → more positive, sets rhythm of heartbeat
ANS only influences, does not control.
SNS: NE/E speeds up
PSNS: AcH slows down generation, helps hyperpolarize through K+ channels
Describe the excitation of contractile cells of the heart. How is contraction accomplished in contractile cells? What is the significance of the long plateau phase?
Contractile cells are stimulated by nearby cells through intercalated discs/electrical synapse.
Na+ channels open to depolarize cells, letting the Ca+ influx slowly to cause a long refractory period. K+ efflux to repolarize.
The significance of a plateau phase with contractile cells is to prevent tetanus.
List the structures, in order, of the conduction pathway of the heart (5 total)
SA Node → AV node → AV Bundle of His → R/L Bundle branches → Purkinje Fibers @ bottom
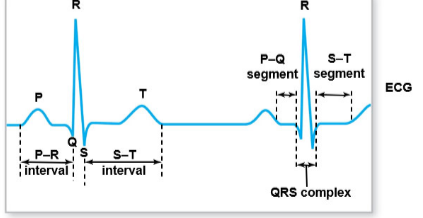
Describe the typical ECG output. What is the name of each wave and what does each wave signify?
P: Atrial Depolarization
QRS: Ventricular Depolarization
“lub”
T: Ventricular Repolarization
“dub”
What types of vessels are considered: distributing; conducting, resistance, exchange ?
Distributing: Muscular arteries (push blood to organs)
Conducting: Elastic arteries (push blood forward)
Resistance: Arterioles (modify resistance to flow by vasoconstriction/dilation)
Exchange: capillaries