Bone, Cartilage and Joints 1
1/27
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
28 Terms
What are the different types of connective tissue?
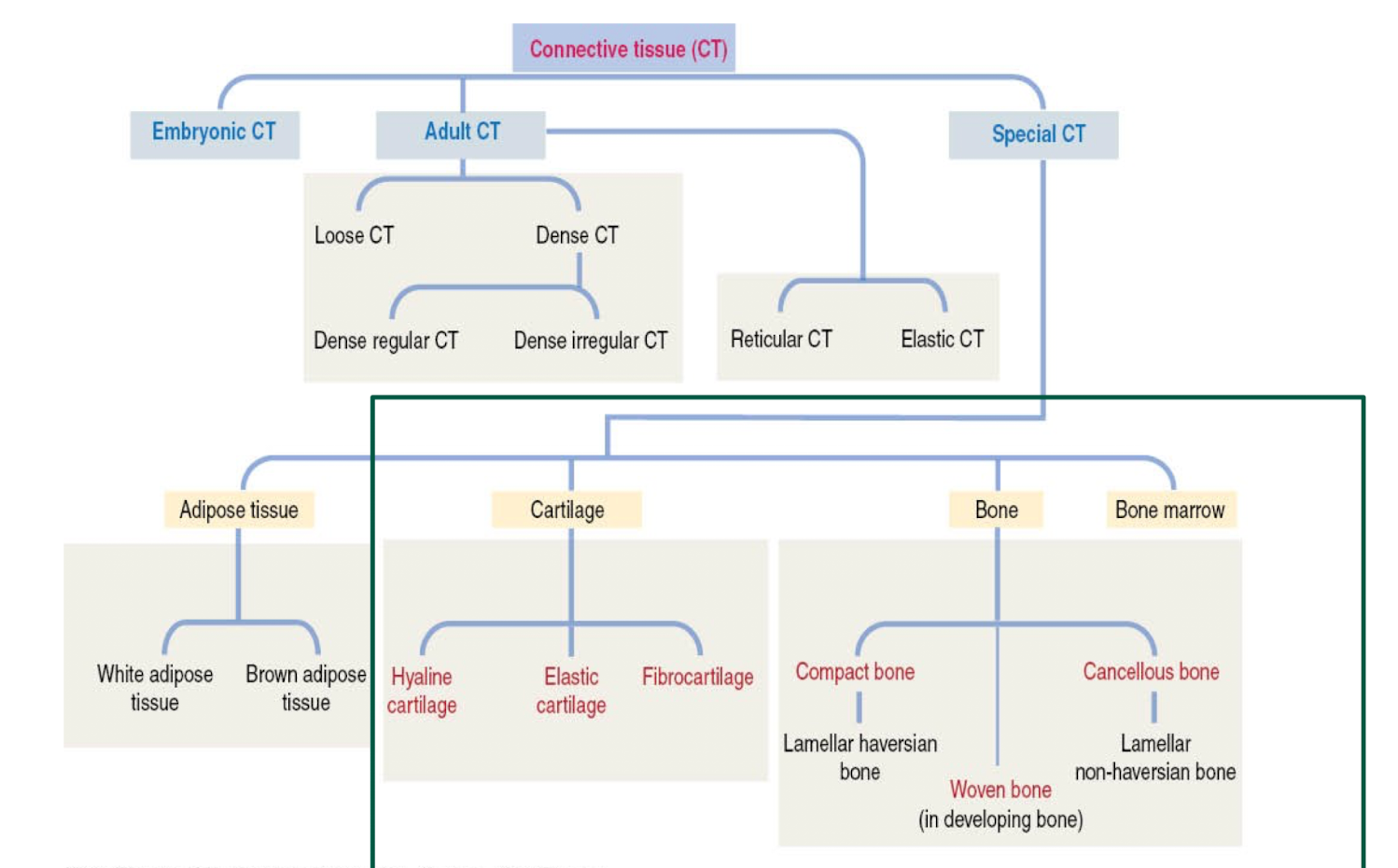
What two cell types compose cartilage?
- Chondroblasts
Chondroblasts are immature cells that produce the cartilage's extracellular matrix
- Chondrocytes
While chondrocytes are the mature, differentiated cells that are trapped within this matrix in lacunae (small chambers) and are responsible for its maintenance and repair
What is the ECM of cartilage?
• Extracellular matrix (ECM)
Unique biomechanical properties
Fibres (depends on type of cartilage)
• Rigidity
Ground substance (abundant):
• Resiliency
Avascular
What types of cartilage are recognized?
Hyalin (clear-looking ground substance)
Fibrocartilage (cells occur in chords or in alignment between strands of collagen fibers)
Elastic Cartilage (Visible elastic fibers throughout matrix)
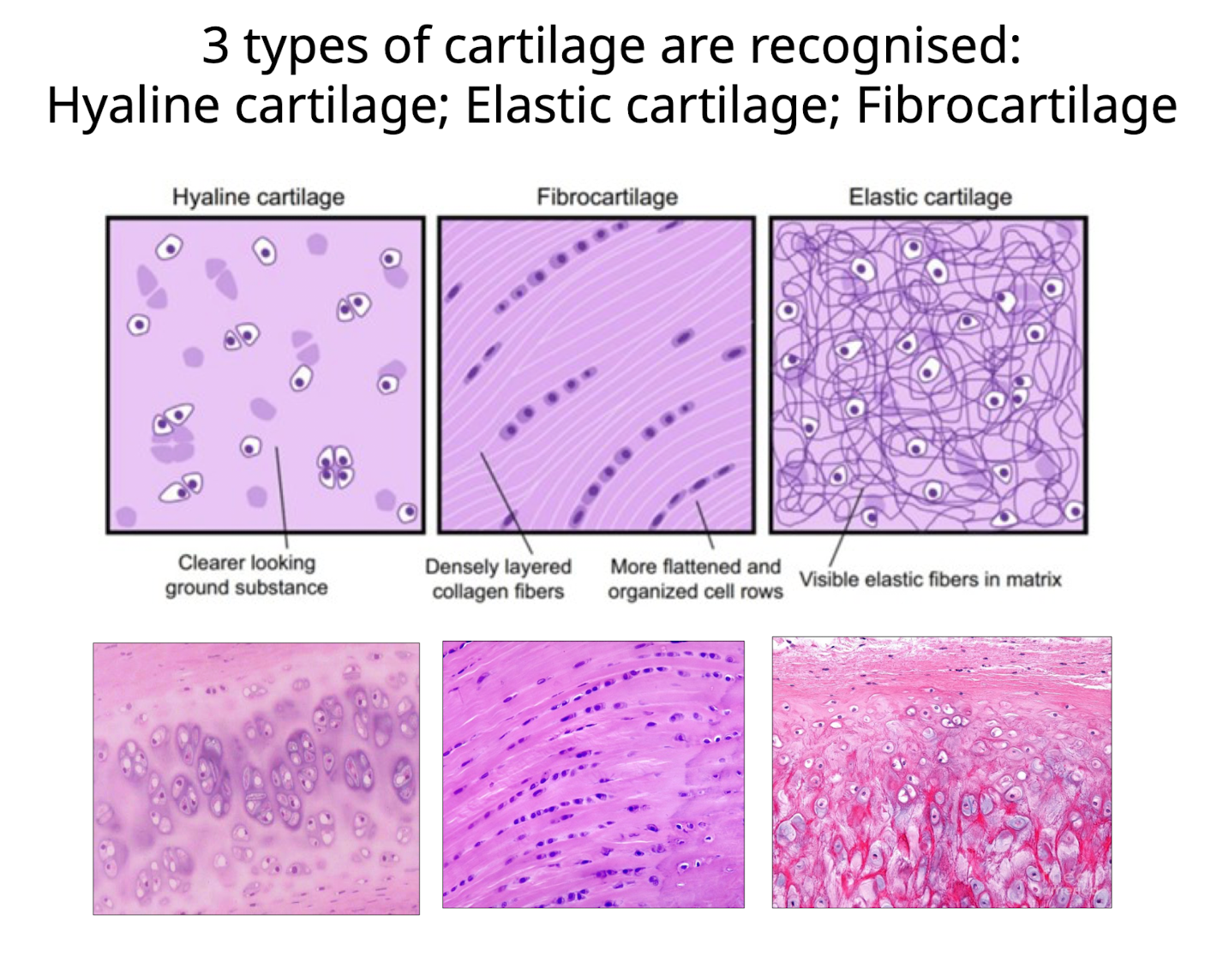
What are the key features of hyaline cartilage?
What does it form, what is the main function and where is it found?
• Most common type of cartilage (glassy app.)
• Forms temporary skeleton in embryo.
Gradually cartilage is replaced by bone
Responsible for growth of long bones
• Abundant ground substance plus few Type II collagen fibres
• Limited distribution in adults
e.g Articular surface of moveable joints. walls of respiratory passages, costal cartilage
What are the key features of elastic cartilage?
Where is it found, what does it contain and what is the main function?
• Found ear pinna, epiglottis
• Contains high content of elastic fibres
Flexible
Elastic fibres + collagen Type II
Less ground substance
Presence of elastin is sometimes demonstrated by special stains (Sometimes mason’s trichrome stain)
What are the key features of fibro-cartilage?
Where is it found, what is the main function?
• Limited distribution
Inter-vertebral discs
Intra-articular discs (menisci)
Attachments ligaments and tendons to bones
• Intermediate between dense regular CT and hyaline cartilage
• Cells (C-chondrocytes) arranged in columns between bundles of collagen (Type 1) fibres (f)
• Minimal ground substance
• Undergoes interstitial (from within) growth only
By what two processes do elastic and hyaline cartilages grow by?
By what process does fibro-cartilage grow by?
Elastic + Hyaline - undergoes both appositional (surface) and interstitial (from within) growth
Fibro-cartilage - undergoes interstitial
What is appositional growth?
New surface layers of matrix are added to the pre-existing matrix by new chondroblasts from the perichondrium.
• New cartilage forms at the edges of existing cartilage
• Involves the perichondrium (Which is the dense layer of connective tissue covering most cartilage in the body, EXCEPT for within joints- ARTICULAR hyaline cartilage)
Fibroblasts differentiate to Chondroblasts in the chondrogenic zone and synthesise cartilage ECM
Chondrocytes maintain ECM
• Occurs in both hyaline and elastic cartilage
What is interstitial growth?
Chondrocytes grow and divide and lay down more matrix inside the existing cartilage.
• Growth occurs from within existing cartilage
• Chondrocytes reactivated - divide to form Isogenous groups that produce additional ECM
• Occurs all types of cartilage
What are isogenous groups?
Feature of interstitial cell growth
Isogenous groups in cartilage are clusters of two or more chondrocytes (cartilage cells) found within a single lacuna (chamber), originating from the mitotic division of a single progenitor chondroblast cell.
What is the synovial membrane or synovium?
What two cell types compose it and what do they do?
What is the sub-intima?
Synovial "membrane" or synovium (Intima) - The synovial membrane, or synovium, is a thin, specialized connective tissue that lines the inner surfaces of some joints, tendon sheaths, and bursae.
- Type A Synoviocyte -Macrophage - maintenance and "clean up" cells, fluid contents or dead cells from surroundings
- Type B Synoviocyte- fibroblastic - secretes hyaluronan (hyaluronic acid)
Sub-intima - a fibrous layer
- Loose connective tissue
- Capillaries - important for maintenance of intima which is avascular
Being nourished by diffusion
Sub-intima surrounds the intima or synovium
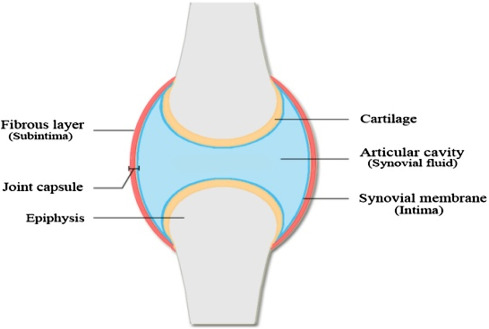
What is the composition of synovial fluid? (3 main components)
Hyaluronan: A glycosaminoglycan that contributes to the fluid's viscosity and lubricating properties.
Lubricin: A glycoprotein that further enhances lubrication and reduces friction in the joint.
Electrolytes and Proteins: These are derived from blood plasma and produced by cells within the joint tissues.
What are the functions of synovial fluid?
• Lubrication: Reduces friction between the articular cartilage of synovial joints during movement, allowing bones to glide smoothly against each other.
• Shock Absorption: Acts as a cushion, absorbing shocks and distributing loads across the joint surfaces, which helps protect the cartilage and underlying bone.
• Nutrient Distribution: Provides nutrients to the avascular articular cartilage and removes waste products, maintaining joint health.
What is athrocentesis used for?
What parameters are normal? What are abnormal?
• (joint tap): Used for cytology and microbial culture
Normal = appearance-viscous like egg white in colour and consistency
Abnormal= Cloudy fluid, blood in the fluid, or excess fluid are all signs of a problem in or around the joint
What IS bone?
A connective tissue with cells and fibres embedded in a hard unbending calcified matrix
Presence of calcium-attracting cells which mineralize
What are the main functions of bone?
• Functions:
- Rigid and hard support (cf. cartilage)
- Protects vital organs
- Contains the bone marrow (haematopoiesis)
- Reservoir for calcium, phosphate and other ions
- Transforms forces of skeletal muscle contraction into bodily movements
Why is bone considered a dynamic tissue?
• Bone is a dynamic tissue - capable of remodelling and repairing itself
Unlike cartilage it is very vascular, the minerals within can be released as well (becoming mobilized)
What are the main types of bone and what are their main features?
Compact (cortical) bone
• Lamellar bone- specific orientation of collagen fibres (biomechanical function)
• Structural organisation - presence of Haversian systems or osteons
Cancellous (spongy or trabecular) bone
• Lamellar bone with lattice -like degree of organisation of collagen fibres
• Lacks haversian systems- Spicules are aggregated into bony trabeculae (plates)
• Reduces weight of bone and supports marrow
Woven bone:
• Feature: Random/y orientation collagen fibres
• Temporary form assoc. developing bone, fracture repair, bone tumours (One of the first types of bones produced during injury or fractue)
• Replaced by lamellar bone in most cases
What are the three main types of cells found in bone?
Where do they reside?
What are their main functions?
1. Osteoblasts:
- Originate from Osteogenic cells (stem) associated with the Periosteum /endosteum
- Function is to form the Osteoid (organic part of ECM)
- Become osteocytes- maintenance
2. Osteocytes
- Located within the calcified 'osteoid' (ECM)
- Communicate with each other by special cellular extensions- canaliculi
- Function is to maintain the bony matrix
3. Osteoclasts:
- Located on external and internal surfaces of bony surfaces
- Large, motile, multinucleated cells
- Characteristic ruffled border
- Origin: bone marrow/ monocytes
- Function- enzymatic digestion of ECM- resorption is important for remodelling of bone, which is what makes bone a dynamic tissue, their antagonistic role with the osteoblasts, allows bones to adapt to different weights and needs over time
What structures mainly compose the bone matrix (ECM)?
• Organic components (Osteoid=bone ecm) produced by osteoblasts:
Fibres - Predom. Collagen Type 1 (spiral arrangement)
GAGS: Chondroitin sulphate and Keratan sulphate
Glycoprotein's (sialo protein and osteocalcin)-calcium binding
• Inorganic component forms after the osteoid is laid down:
- Hydroxyapatite crystals (Ca, (PO)(ОН)2)
- Na, Mg and Fe
What composes the canalicular system and what main function does it have?
Osteocytes are embedded in bony matrix, sit within Lacunae (spaces within the bony matrix), these spaces allow the osteocytes to access nutrition despite being surrounded by bone, effectively enabling them to survive
The lacunar-canalicular system allows
- communication and nutrient/waste exchange for the osteocytes
- role in mechanosensation -helps osteocytes detect mechanical stress and coordinate bone remodelling
Osteocytes stay alive with this system!!
What is lamellae and how does this vary between bone types?
In bone, "lamellar" refers to the mature, mechanically strong structure where collagen fibers are organized into multiple, parallel sheets called lamellae. This highly organized, layered structure makes bone strong and tough, providing the mechanical strength of the adult skeleton by contrasting with the weaker, randomly organized collagen of woven bone.
What is the Osteoid?
Osteoid is the unmineralized form of the bone extracellular matrix (ECM), containing collagen and other proteins, which is subsequently mineralized to form mature bone. Osteoblasts produce osteoid, which serves as a soft, temporary foundation for bone tissue before the deposition of calcium and phosphate crystals, a process called calcification.
What are haversian systems or osteons?
Haversian systems, also known as osteons, are the basic structural and physiological units of compact bone, forming a roughly cylindrical, multi-layered structure that provides the bone's mechanical strength and facilitates nutrient exchange. Each osteon consists of a central Haversian canal, containing blood vessels and nerves, surrounded by concentric rings of mineralized bone tissue called lamellae.
Does cancellous bone have haversian systems?
Cancellous (or spongy) bone lacks Haversian systems and instead is composed of a lattice-like network of bony trabeculae, which are small, irregularly shaped plates and bars of bone. These trabeculae are arranged along lines of mechanical stress and contain osteocytes and can be connected to the bone marrow via canaliculi to receive blood supply
What is an example of hyaline cartilage where only interstitial growth occurs?
Why does this occur?
Articular cartilage, the hyaline cartilage found on the ends of bones in synovial joints, grows exclusively by interstitial growth. The absence of a perichondrium—the dense connective tissue layer needed for appositional growth—means that the only way articular cartilage can expand is from within
Articular cartilage lacks a perichondrium because it is covered by the synovial membrane and synovial fluid of the joint. This is different from most other hyaline cartilage, such as that in the trachea or nose, which is surrounded by a perichondrium and can perform both interstitial and appositional growth.
What is the perichondrium?
Where can it be found? Where can it not be found?
The perichondrium is a dense layer of fibrous connective tissue that covers the surface of most of the cartilage in the body.
The perichondrium is a dense irregular connective tissue sheath overlying most cartilage found in the body. The only place where a perichondrium does not exist is within joint capsules (ex: joints of the ankle, knee, hip and shoulder).