Family Medicine EOR: Cardiovascular (Smarty PANCE)
1/617
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
618 Terms
Sinus tachycardia is a normal sinus rhythm but with a heart rate over ________ bpm
100 bpm
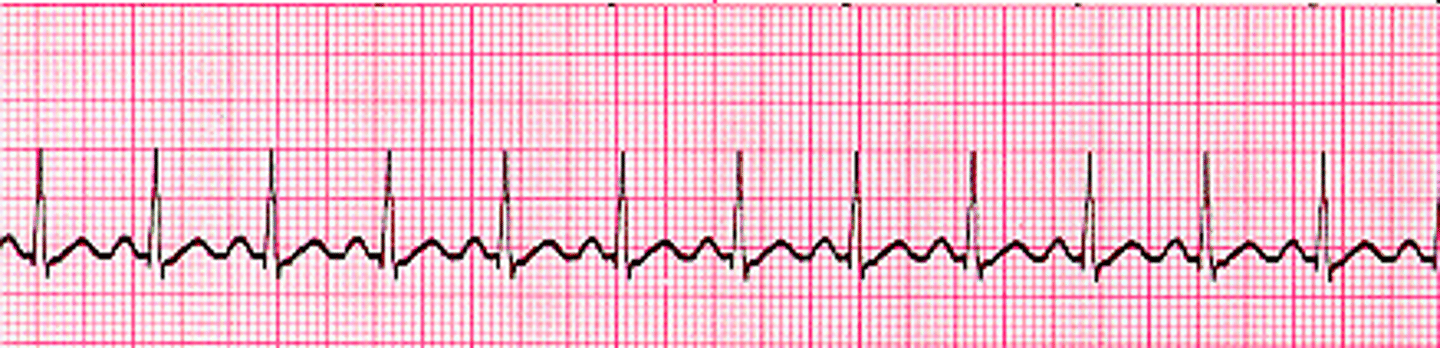
Sinus bradycardia is a normal sinus rhythm with a rate of _________ bpm
< 60 bpm
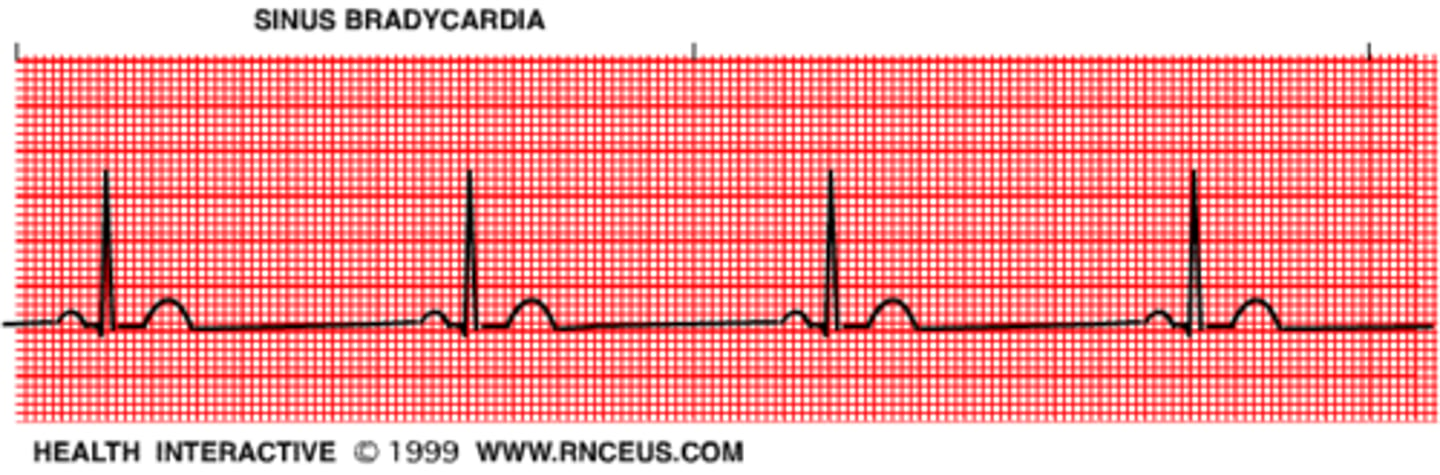
EKG: no discrete P waves and an irregularly irregular pattern of QRS complexes. What's the dx?
Atrial Fibrillation
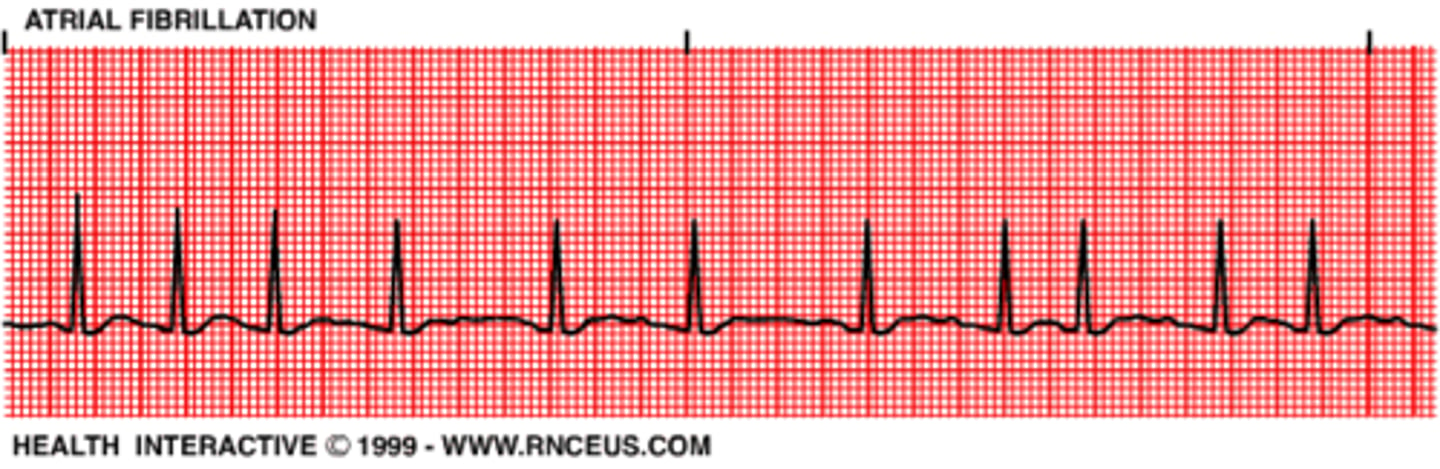
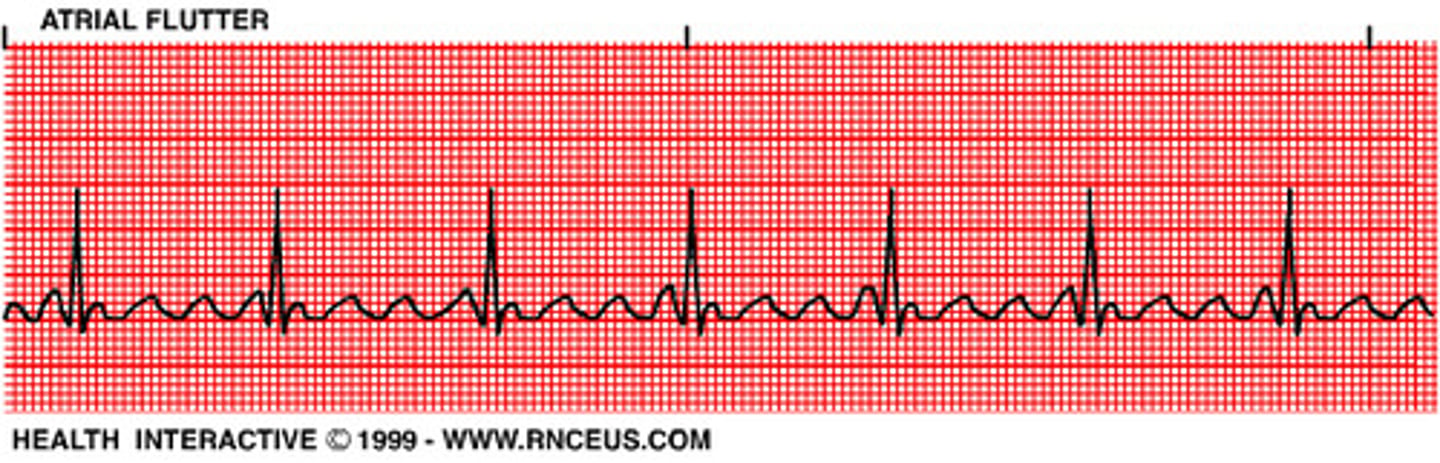
EKG: Regular, sawtooth pattern (F-waves), narrow QRS complex. What's the dx?
Atrial Flutter
EKG: PR interval > .2 seconds. What's the dx?
First degree AV block
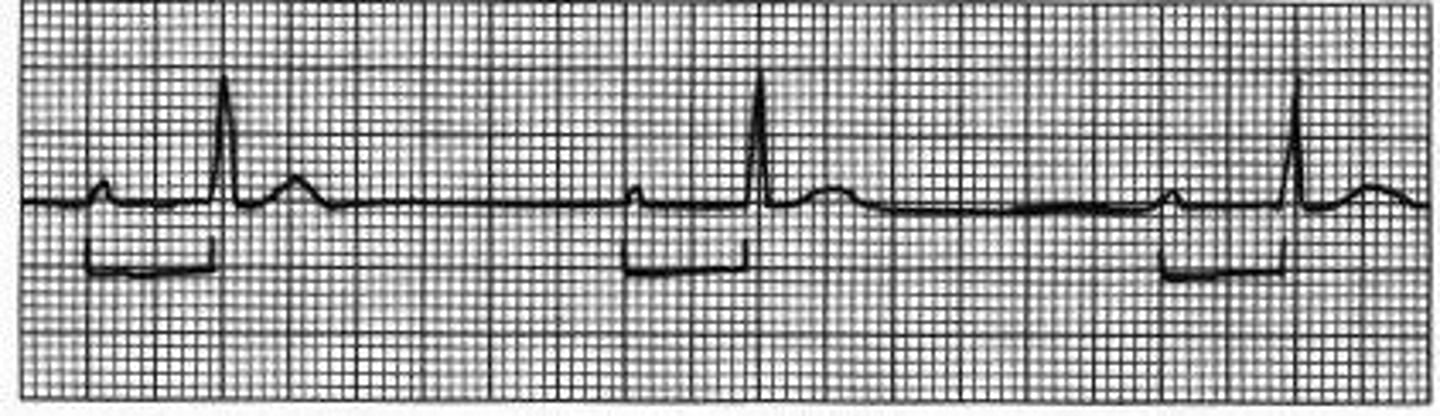
EKG: Progressive *prolongation of the PR* interval culminating in a non-conducted P wave. What's the dx?
Mobitz I Wenckebach block (longer, longer, drop now you've got a Wenckebach)
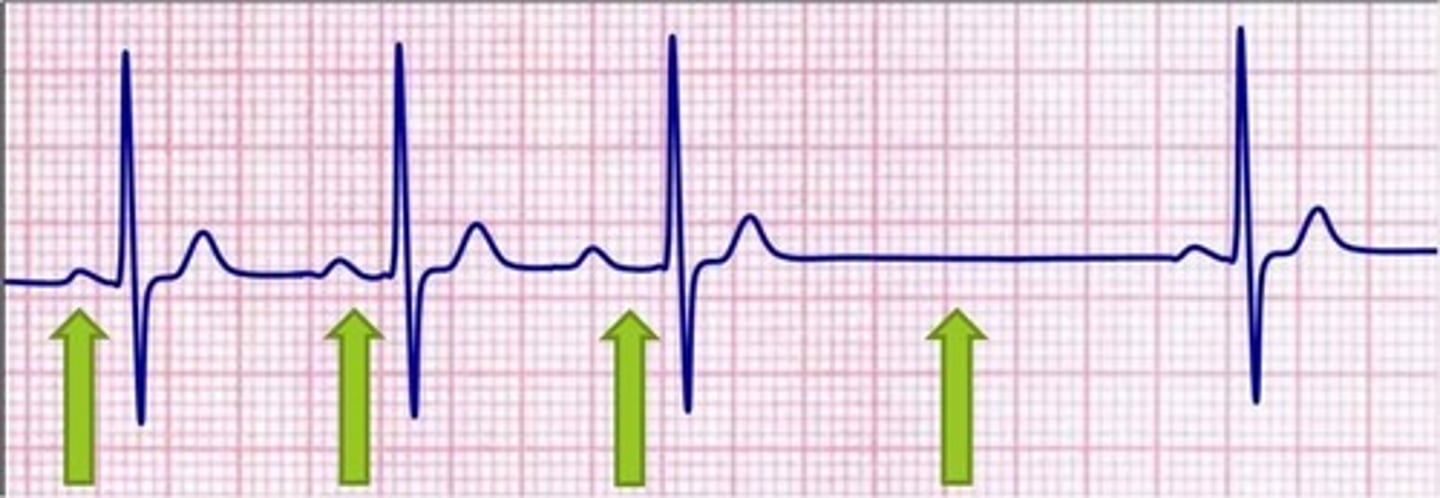
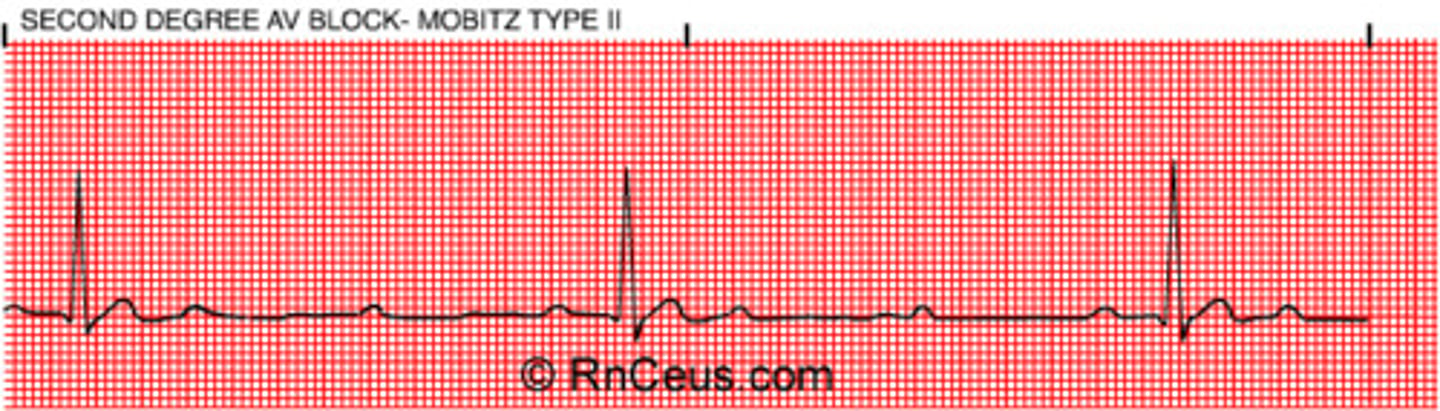
EKG: Intermittent non-conducted P waves without progressive prolongation of the PR interval. What's the dx?
Type II Mobitz block (some get dropped some get through now you've got Mobitz 2)
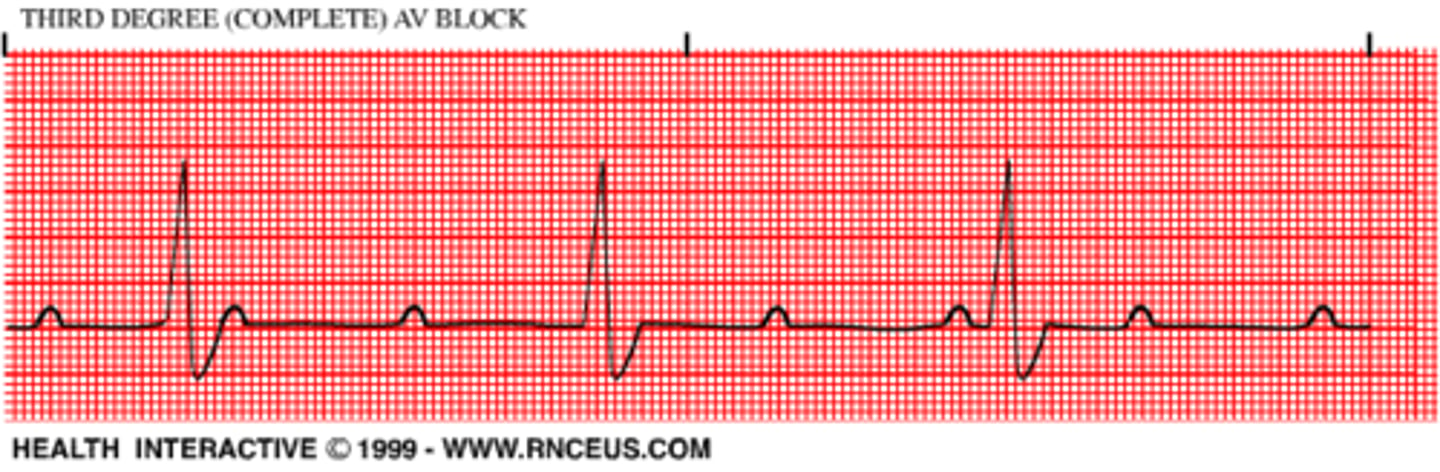
EKG: there is complete absence of AV conduction - none of the supraventricular impulses are conducted to the ventricles. What's the dx?
Third degree AV block (P's and Q's don't agree now you've got a 3rd degree)
EKG: R and R' (upward bunny ears) in V4-V6. What's the dx?
Left bundle branch block
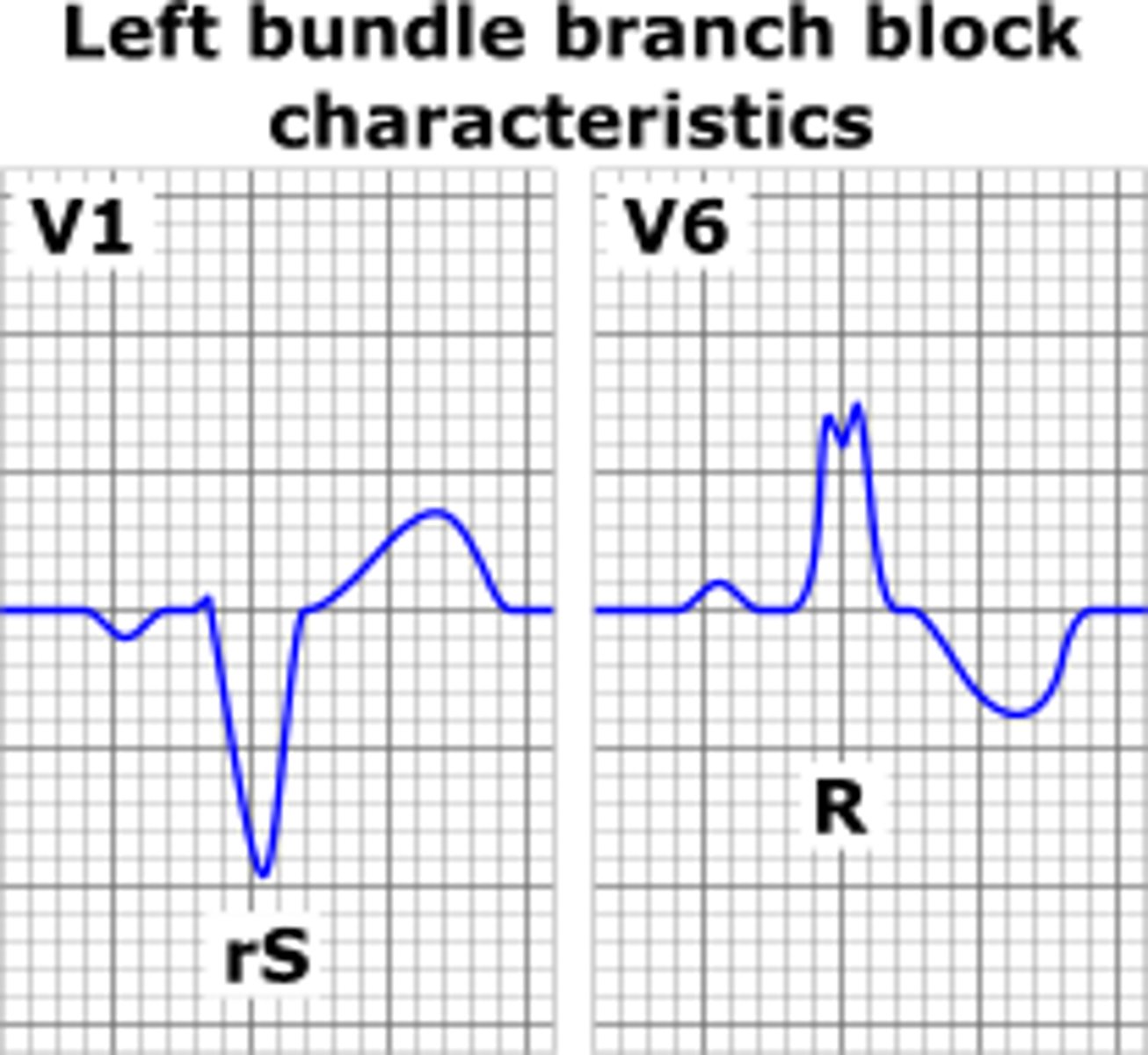
EKG: R and R' (upward bunny ears) in V1-V3. What's the dx?
Right bundle branch block

A faster-than-normal heart rate *beginning* above the heart's two lower chambers *in the atria*, *AV junction* or SA node. What's the dx?
Supraventricular Tachycardia
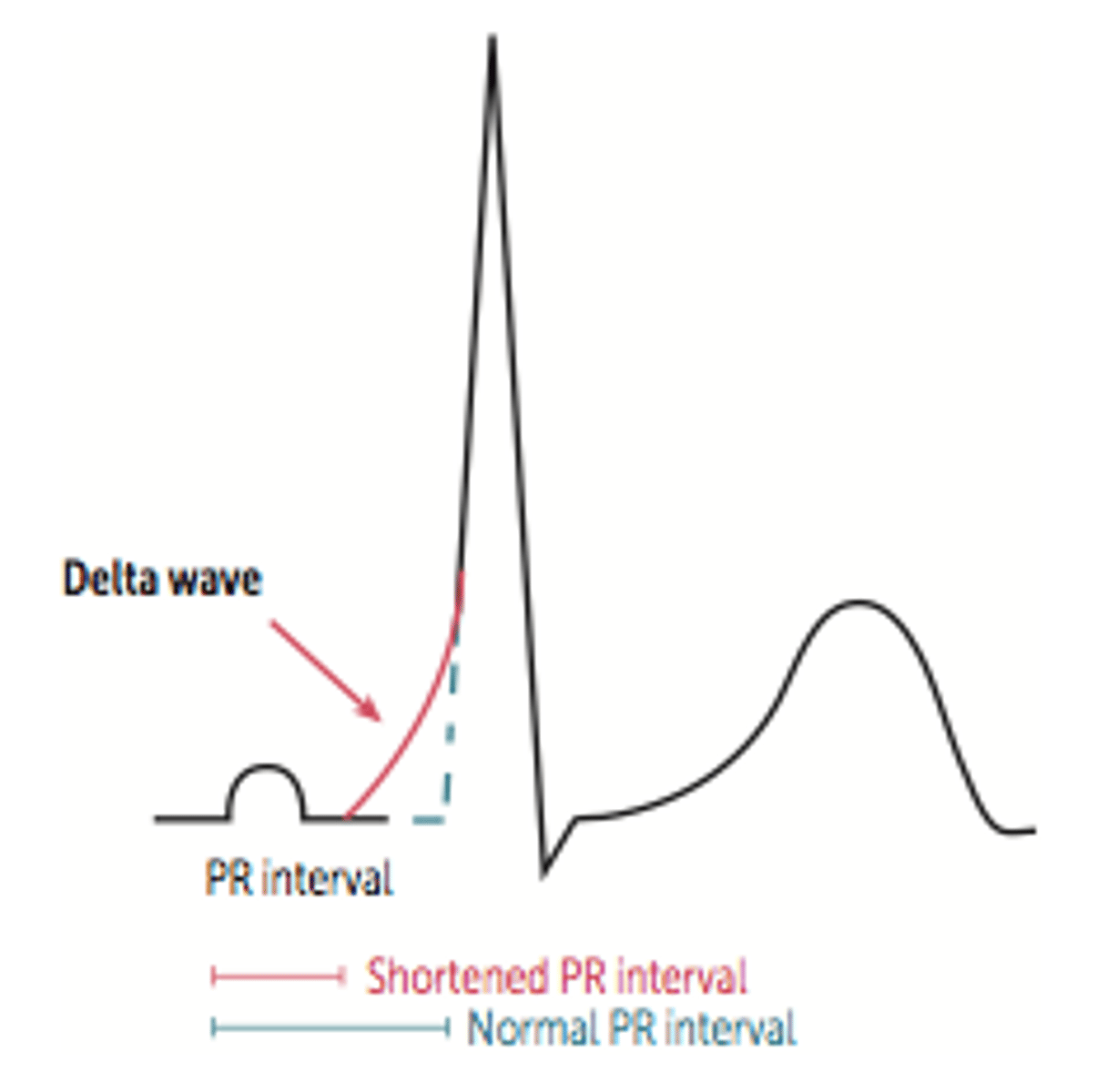
EKG: Shorter PR Interval, longer QRS complex and a delta wave - slurring slow rise of initial portion of the QRS. What's the dx?
Wolff-Parkinson-White Syndrome
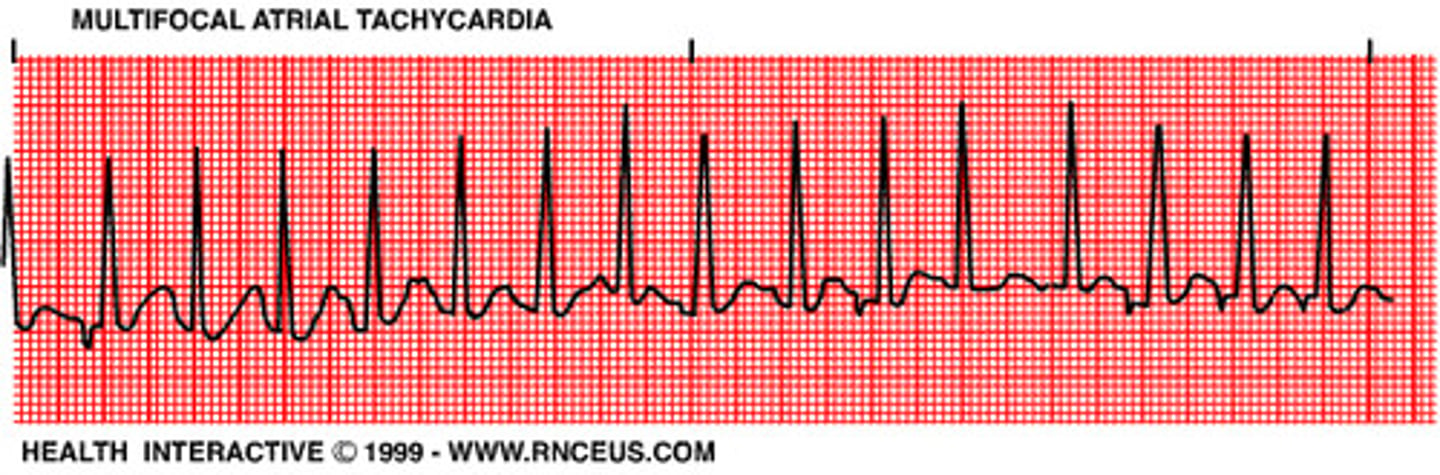
EKG: Rapid irregular rhythm > 100 bpm. At least 3 distinct P-wave morphologies. What's the dx?
Multifocal Atrial Tachycardia
EKG: An abnormal (non-sinus) P wave is followed by a QRS complex. What's the dx?
Premature Atrial Complex (PAC)
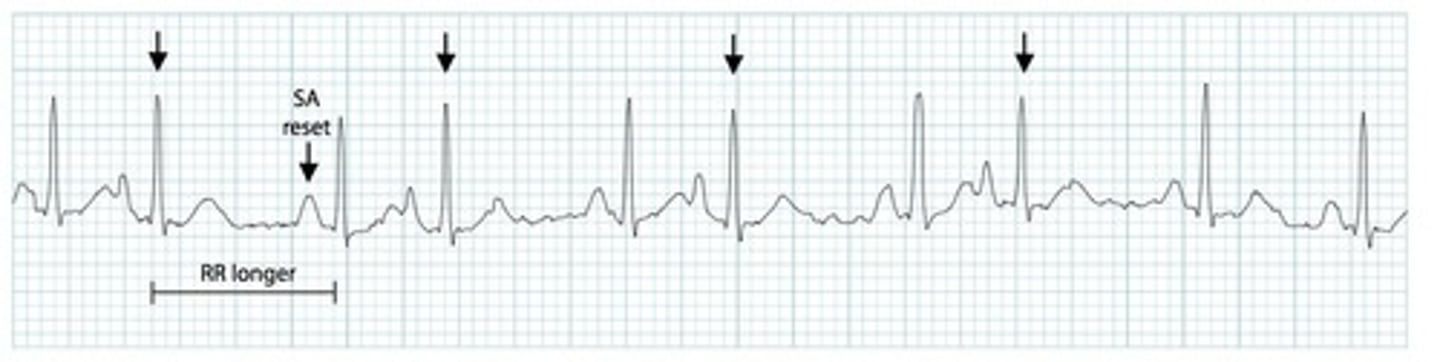
EKG: Narrow QRS complex, either (1) without a preceding P wave or (2) preceded by an abnormal P wave with a PR interval of < 120 ms. What's the dx?
Premature Junctional Complex (PJC)
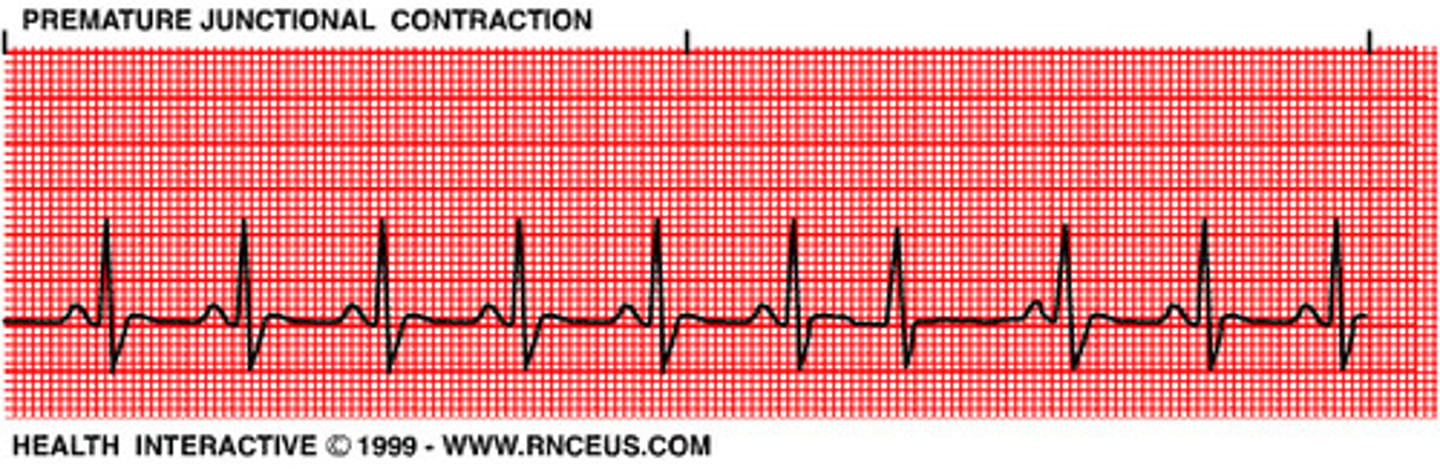
Broad QRS complex (≥ 120 ms) with abnormal morphology. What's the dx?
Premature ventricular contractions (PVC)
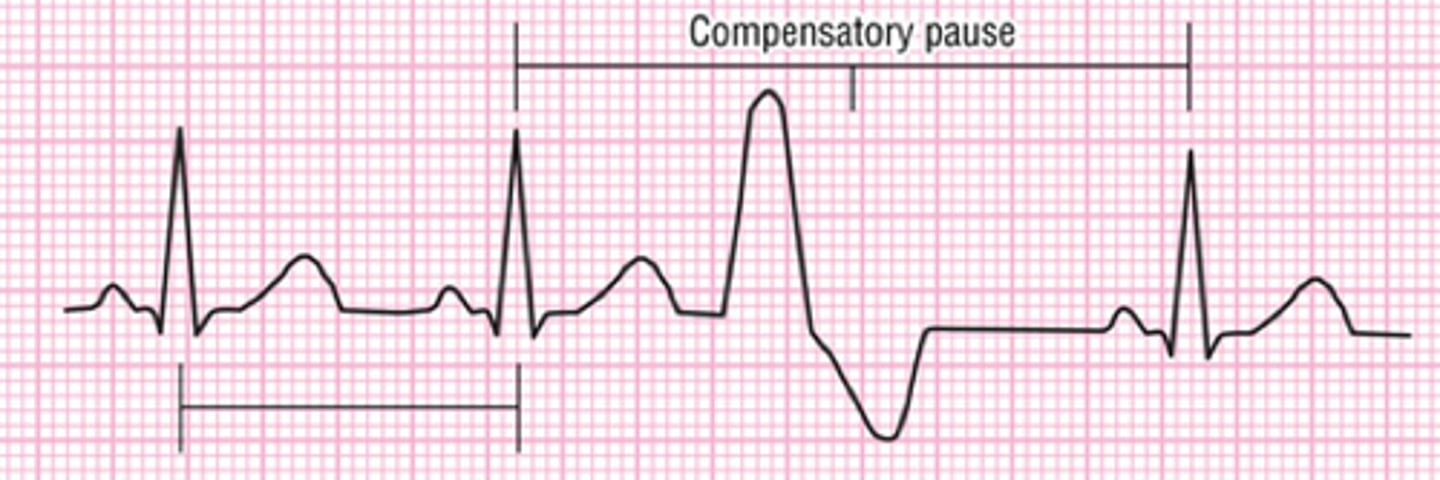
Every 3rd beat is a PVC
Trigeminy
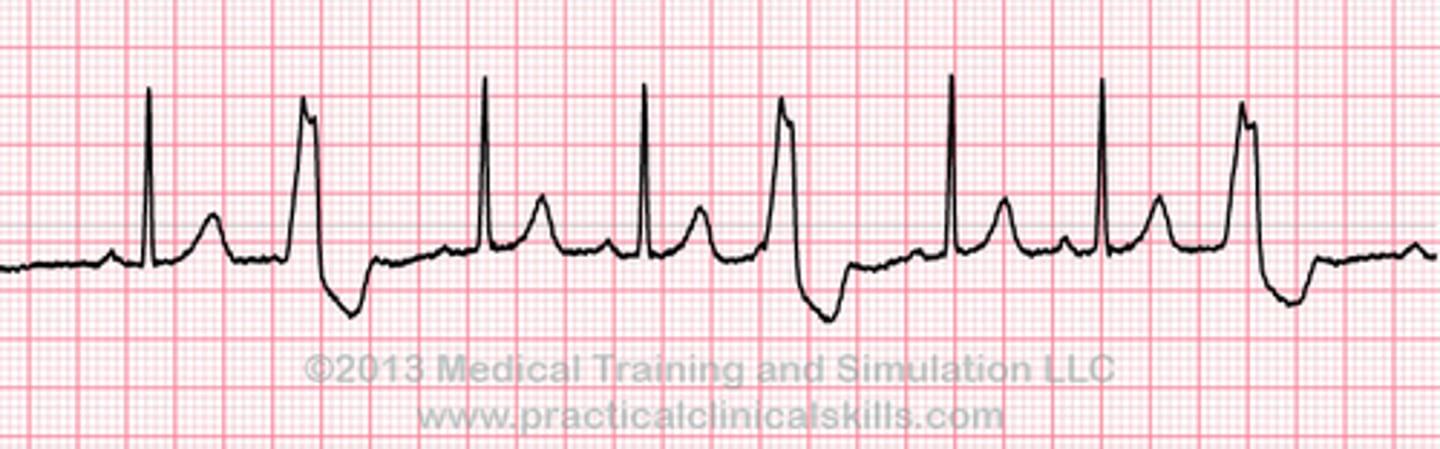
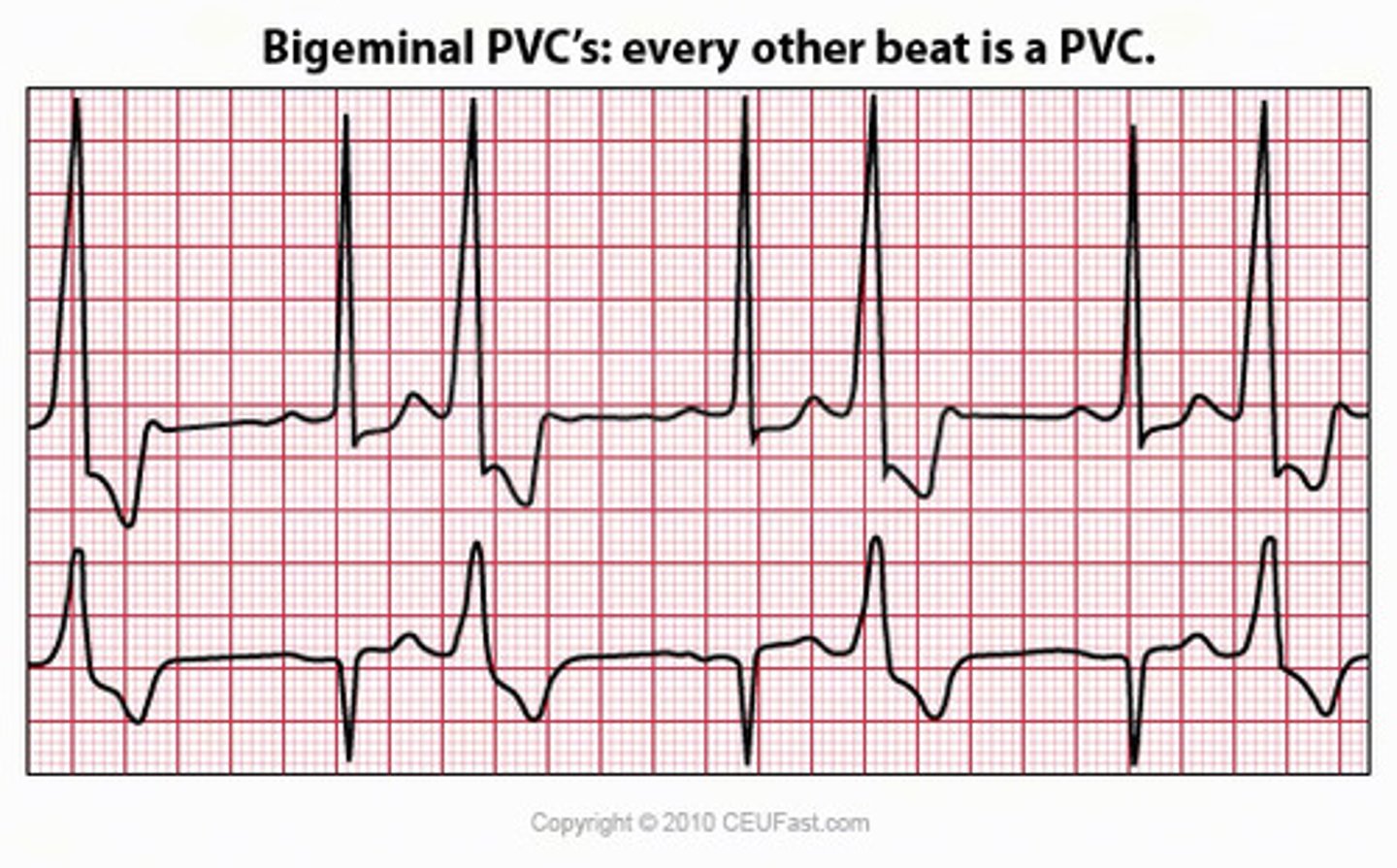
Every other beat is a PVC
Bigeminy
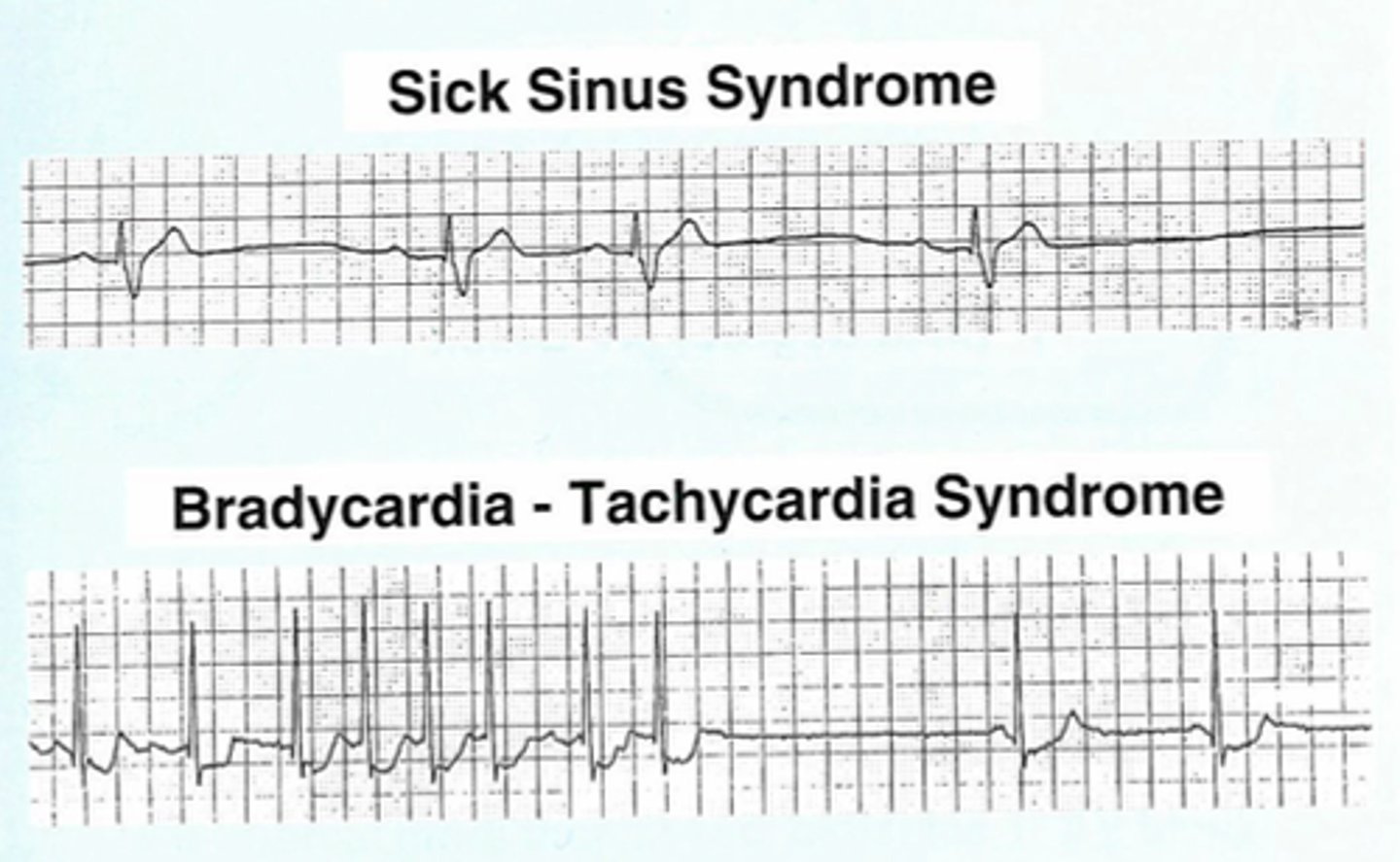
EKG: Alternating bradycardia with paroxysmal tachycardia, often supraventricular in origin. What's the dx?
Sinus Node Dysfunction (Sick Sinus Syndrome)Bradycardia-tachycardia syndrome
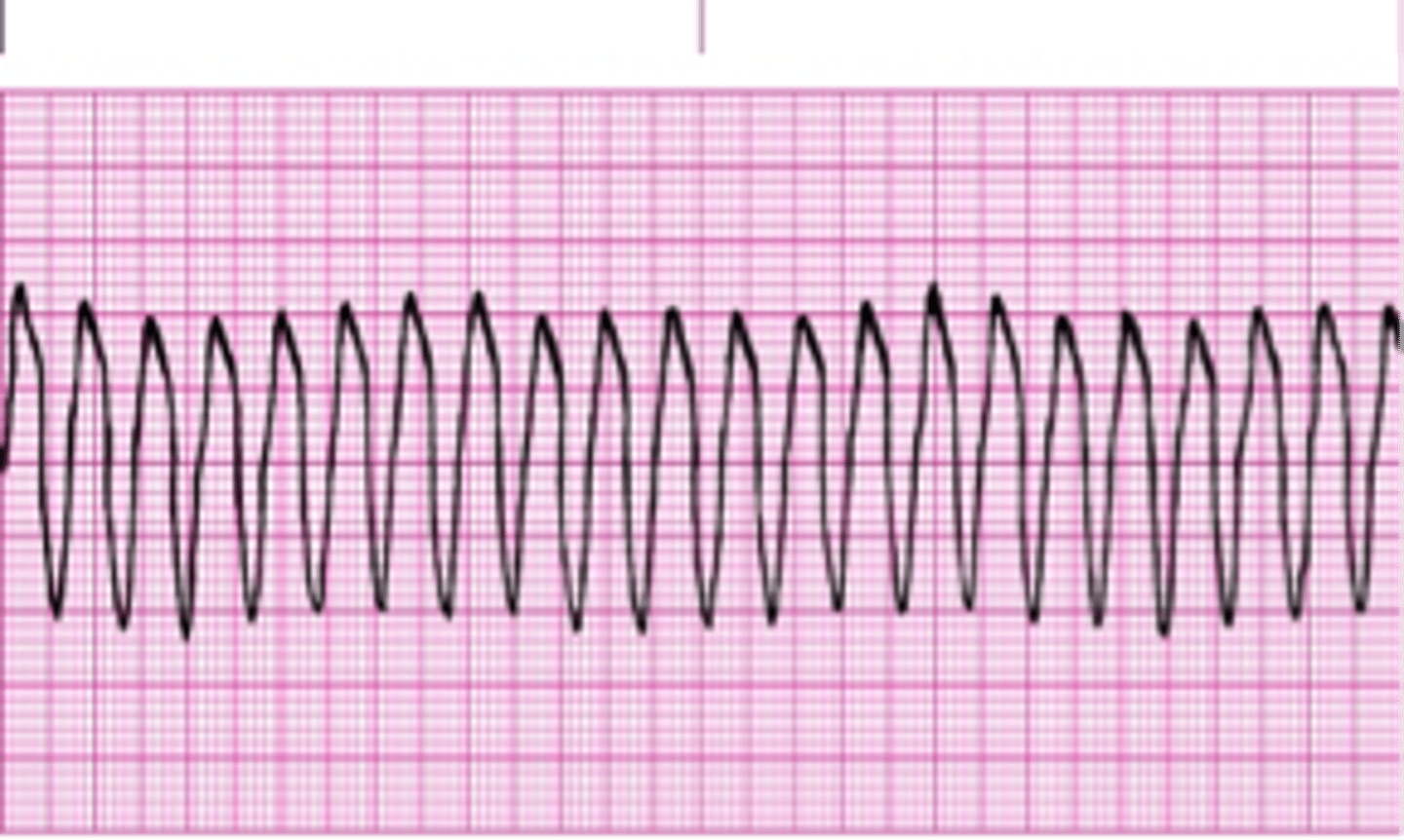
EKG: Broad complex tachycardia originating in the ventricles. What's the dx?
Ventricular Tachycardia (VT)
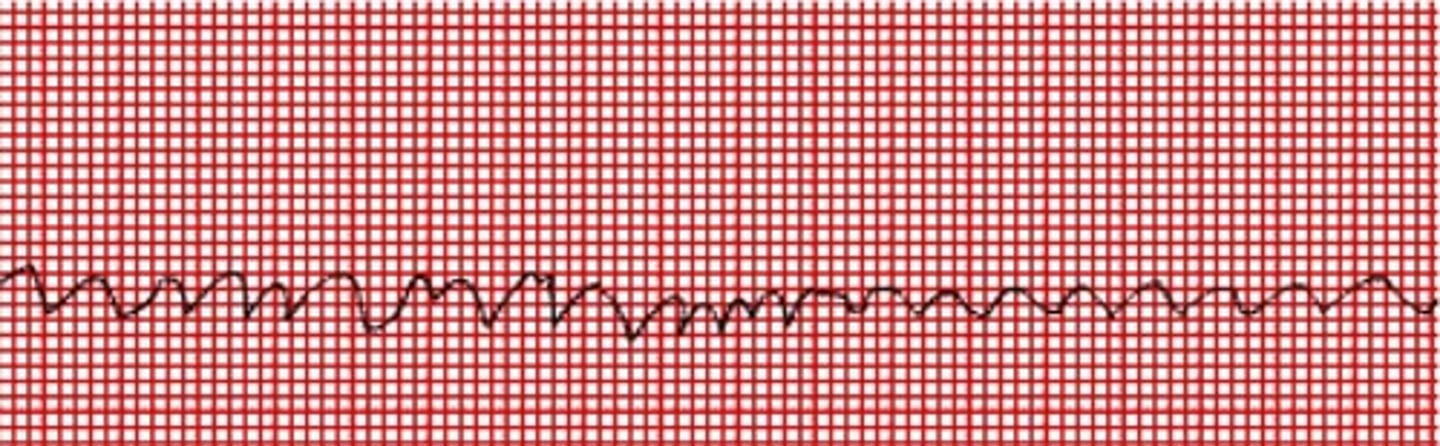
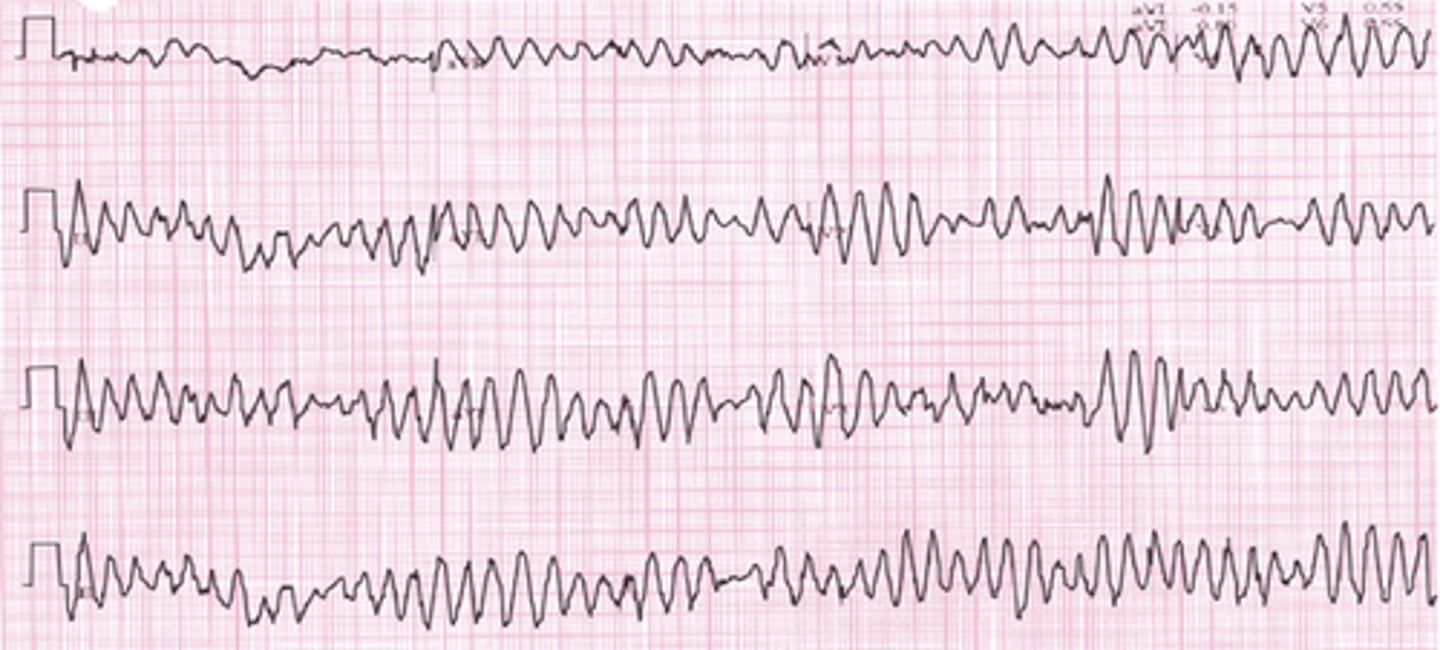
EKG: Chaotic irregular deflections of varying amplitude No identifiable P waves, QRS complexes, or T waves. What's the dx?
Ventricular Fibrillation
EKG: Polymorphic ventricular tachycardia that appears to be twisting around a baseline. What's the dx?
Torsades de Pointes (TdP)
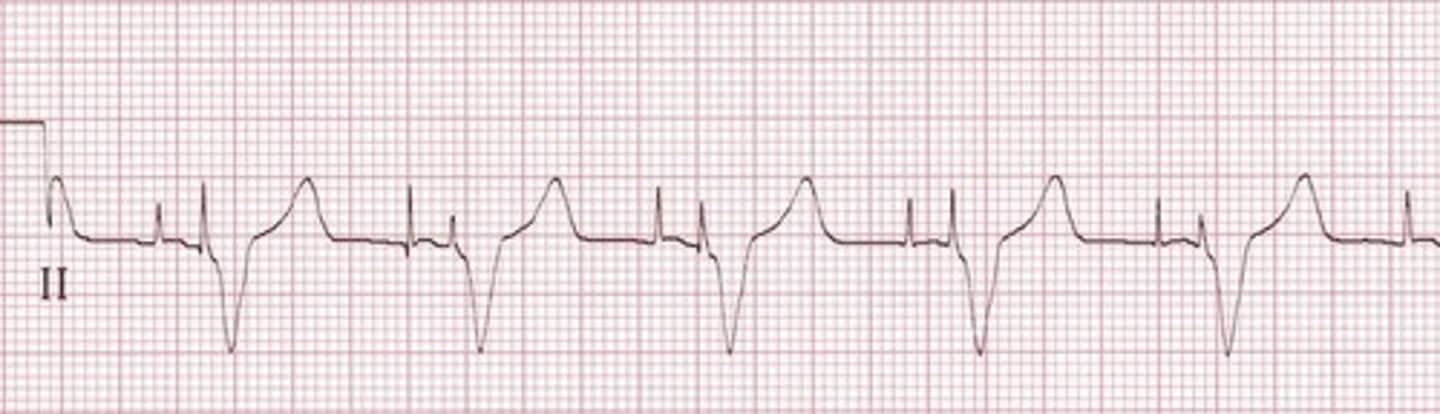
EKG: Vertical spikes of short duration, usually 2 ms. May be difficult to see in all leads
Pacemaker Rhythm with *pacing spikes"
Prolonged absence of sinus node activity (absent P waves) < 3 seconds
Sinus pause
Prolonged absence of sinus node activity (absent P waves) > 3 seconds
Sinus arrest
Which antihypertensive medications can cause bradycardia?
Beta blockers - Non-dihydropyridine CCB - Central agents (clonidine)
Which antihypertensive medications can cause AV block?
Non-dihydropyridine CCB - Central agents (clonidine)
What is the most likely cause of syncope which occurs in a child during an argument?
Long QT syndrome
Non-cardiac hypoxia (e.g. pneumonia, COPD) commonly causes what arrhythmia?
Atrial fibrillation
What arrhythmia can occur with structural changes such as hypertrophy or dilatation of the ventricle?
Ventricular tachycardia
What two murmurs are most associated with atrial fibrillation?
Mitral stenosis - Mitral regurgitation
What HTN med classes can cause bradycardia?
Beta Blockers - Central agents (clonidine) - Verapamil and Cardizem
What arrhythmia is associated with arterial embolism?
Atrial fibrillation
A 24-year-old has a syncopal event. EKG demonstrates a short PR interval with an upswept initial QRS. What underlying condition caused the syncope?
Wolf Parkinson White
A 30-year-old male has a syncopal event three days after taking an antibiotic. EKG at the scene reveals ventricular tachycardia. What disease condition do you suspect?
Acquired long QT syndrome due to the antibiotic or medications
Upon auscultation of a patient's carotid artery they become bradycardic with a three second pause. What is the suspected underlying condition?
Carotid sinus hypersensitivity
A 13-year-old boy passes out while having an argument with his principal. His examination findings are normal. What heart conduction condition do you suspect?
Long QT syndrome
What is Atrial fibrillation (A-fib)?
Atrial fibrillation (A-fib) is an irregular and often very rapid heart rhythm (arrhythmia) that can lead to blood clots in the heart.
What is the most common risk factor for atrial fibrillation?
Hypertension is the most common risk factor for atrial fibrillation. Atrial fibrillation is the most commonly encountered cardiac arrhythmia.
What are thy symptoms of A-fib?
Symptoms include palpitations and sometimes weakness, effort intolerance, dyspnea, and presyncope
What is seen on an ECG tracing of atrial fibrillation?
An ECG tracing of atrial fibrillation shows an erratic baseline and no discrete P waves, in between irregularly spaced QRS complexes
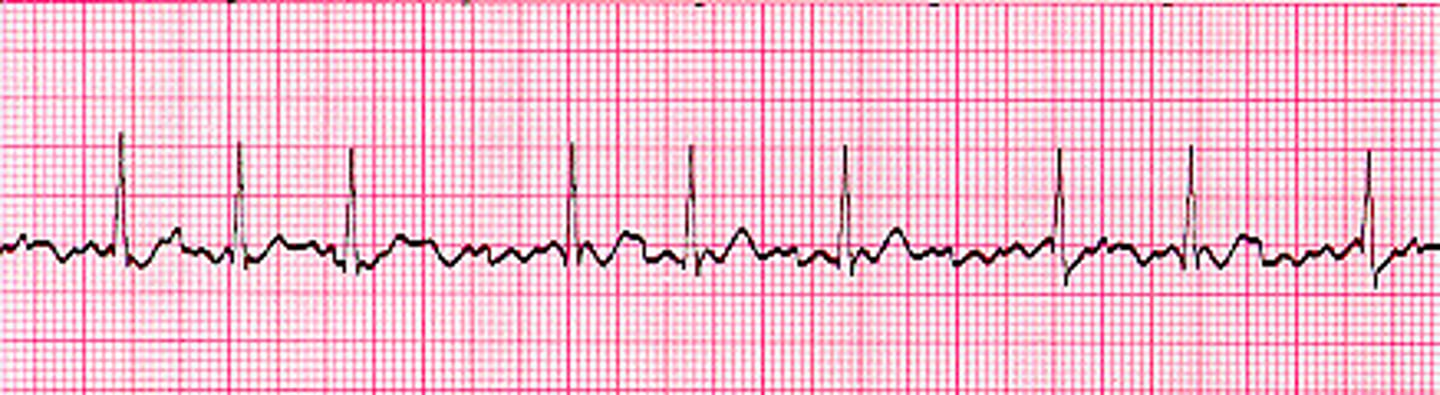
What is a serious complication associated with atrial fibrillation?
A serious complication associated with atrial fibrillation is thrombotic embolism, due to blood stagnation in the atria
What is used to monitor patients on warfarin therapy for the prevention of thrombotic embolism complicating atrial fibrillation?
INR and prothrombin time are used to monitor patients on warfarin therapy for prevention of thrombotic embolism complicating atrial fibrillation
What is the adjusted-dose warfarin target INR for patients with A-fib?
Adjusted-dose warfarin target INR is 2.5 (range 2–3)
Where do the ectopic impulses causing atrial fibrillation most commonly originate?
The ectopic impulses causing atrial fibrillation most commonly originates from the roots of the pulmonary veins
How is the atrial fibrillation rhythm typically described?
The atrial fibrillation rhythm is described as irregularly irregular
How is paroxysmal atrial fibrillation defined?
Paroxysmal atrial fibrillation is defined as intermittent attacks that resolve spontaneously in less than seven days
How is persistent atrial fibrillation defined?
Persistent atrial fibrillation is defined as atrial fibrillation rhythm that lasts more than seven days
Rate control strategy of managing atrial fibrillation aims to keep the heart rate below what rate?
Rate control strategy of managing atrial fibrillation aims to keep the heart rate below 110 beats per minute
What is the scoring system to assess the risk of stroke in patients with Afib?
Anticoagulation is determined by CHA2DS2-VASc or CHADS2 scoring to assess the risk of stroke
What does CHA2DS2-VASc stand for?
CHA2DS2-VASc:
C-Chronic Heart Failure-1 point
H-Hypertension-1 point
A-Age <64-0 point : 64-75-1 point : >75-2 points
D-Diabetes Mellitus-1 point
S-Stroke/TIA-2 points
VA-Vascular disease-1 point
Sc-Gender: Male-0 points : Female - 1 point
What does CHADS2 stand for?
CHADS2:
C=CHF - 1 point
H=HTN - 1 point
A=age>75 yo - 1 point
D=diabetes - 1 point
S2 (stroke or TIA)- 2 points
How are CHADS2 and CHA2DS2-VASc used to determine which patients should receive anticoagulation?
Based on scoring system:
0 points – no therapy or 81–325 mg/day of aspirin
1 point – either 81–325 mg/day of aspirin or anticoagulation
2 or more points – anticoagulation
When indicated, what class of medication is preferable in patients with atrial fibrillation?
Direct oral anticoagulants or DOAC (eg, dabigatran, rivaroxaban, apixaban, or edoxaban) rather than warfarin for most patients in whom oral anticoagulant therapy is chosen
What are some instances warfarin should be chosen over DOACs in patients with Afib.?
Warfarin is preferable to DOACs in patients with mechanical heart valves, mitral stenosis, unacceptable increase in cost, EGFR < 30 ml/min, on certain medications (ex. phenytoin or certain antiretroviral therapy)
What is atrial flutter?
Atrial flutter is similar to atrial fibrillation, a common disorder that causes the heart to beat in abnormal patterns due to a large atrial reentrant circuit
What are the symptoms of atrial flutter?
Symptoms a atrial flutter are the same as A-fib and include palpitations and sometimes weakness, effort intolerance, dyspnea, and presyncope
Diagnosis of atrial flutter?
The diagnosis of atrial flutter is by ECG. In typical flutter, ECG shows continuous and regular atrial activation with a sawtooth pattern, most obvious in leads II, III, and aVF
Treatment of atrial flutter?
Treatment of atrial flutter is the same as that for A-fib and focuses on ventricular rate control, rhythm control, and prevention of thromboembolism.
What is atrioventricular block?
Heart block, also called Atrioventricular (AV) block is partial or complete interruption of impulse transmission from the atria to the ventricles
What is the cause of AV block?
The most common causes of AV block are:
1. Idiopathic fibrosis and sclerosis of the conduction system (about 50% of patients)
2. Ischemic heart disease (40%)
Describe the types of heart block
1. First degree: PR interval > .2 seconds
2. Second degree:
- type 1: longer, longer, drop now you've got a Wenckebach
- type 2: some get dropped some get through now you've got Mobitz 2
3. Third degree (complete block): P's and Q's don't agree now the block is 3rd degree
What are the symptoms of AV block?
As the electrical signal that controls one's heartbeat is partially or completely blocked the heart beats slowly or skip beats and can't pump blood effectively. Symptoms include dizziness, fainting, fatigue, and shortness of breath
A type of second degree atrioventricular block that presents with dropped heartbeats that are not preceded by a change in PR interval length?
Mobitz type II is a type of second degree atrioventricular block that presents with dropped heartbeats that are not preceded by a change in PR interval length. MOBITZ 2 (some get dropped some get through now you've got mobitz 2)
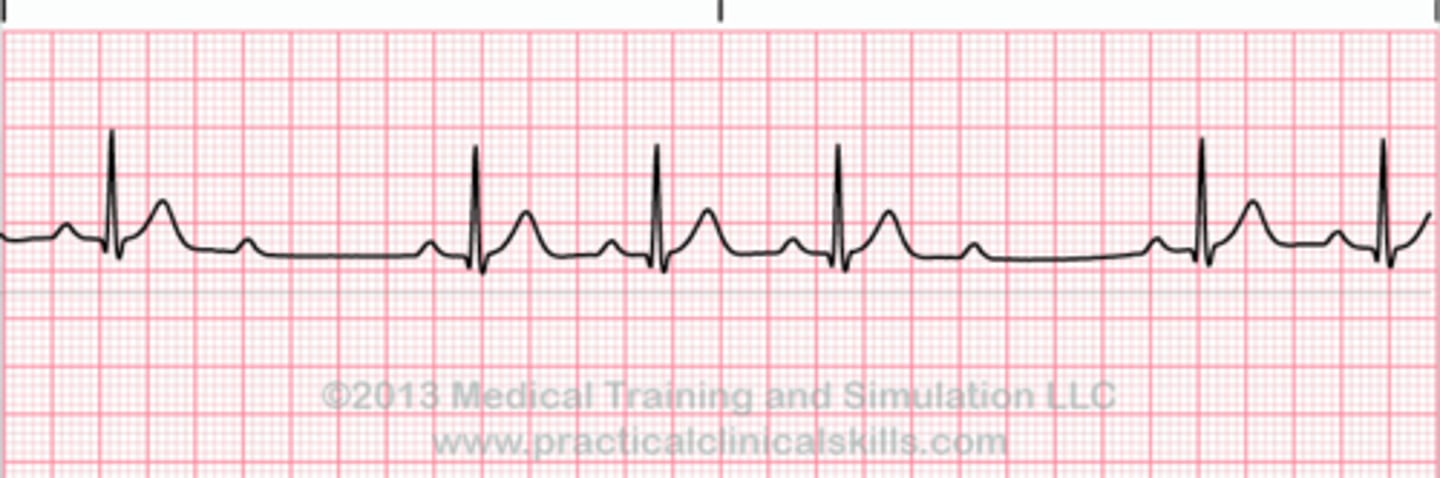
A heart block described as a regularly irregular beat with a progressive lengthening of PR interval until a beat is “dropped”
Mobitz type I (Wenckebach) is a heart block described as a regularly irregular beat with a progressive lengthening of PR interval until a beat is “dropped.” Remember: longer, longer, longer drop now you've got a Wenckebach
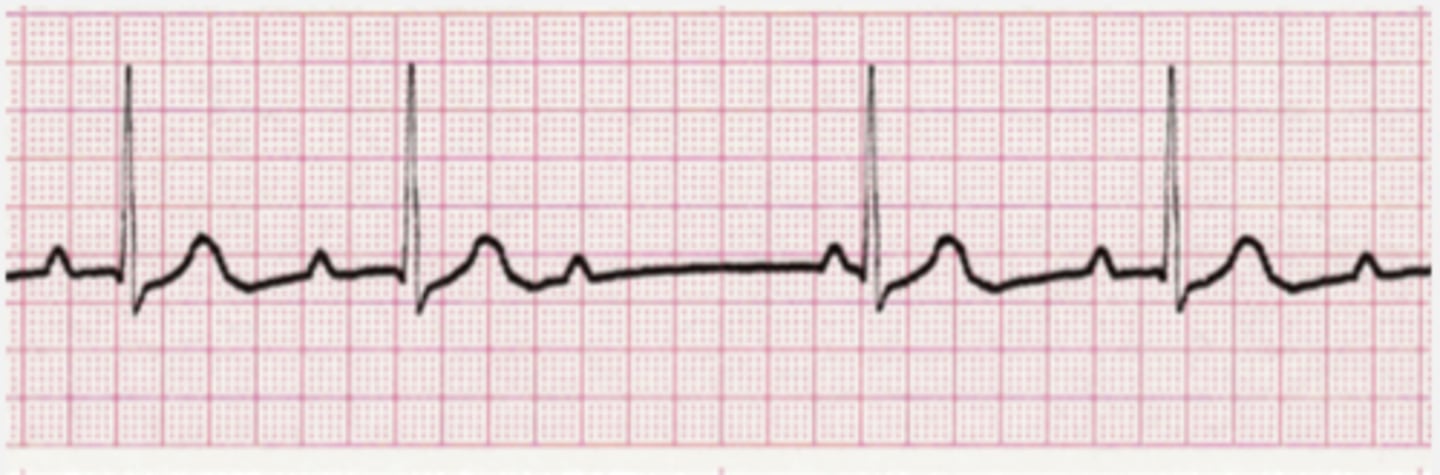
What is the first line of treatment of Mobitz type II?
Mobitz type II is always pathologic. The first line of treatment of Mobitz type II is pacemaker implantation
What is the first line of treatment of Mobitz type I?
Treatment usually unnecessary unless the block causes symptomatic bradycardia and transient or reversible causes have been excluded. Treatment is then pacemaker insertion.
A benign cardiac conduction abnormality where the PR interval is more than 200 milliseconds?
First-degree atrioventricular block is a benign cardiac conduction abnormality where the PR interval is more than 200 milliseconds
First degree atrioventricular block is diagnosed when the PR interval is more than how many small squares in the ECG?
First degree atrioventricular block is diagnosed when the PR interval is more than five small squares in the ECG
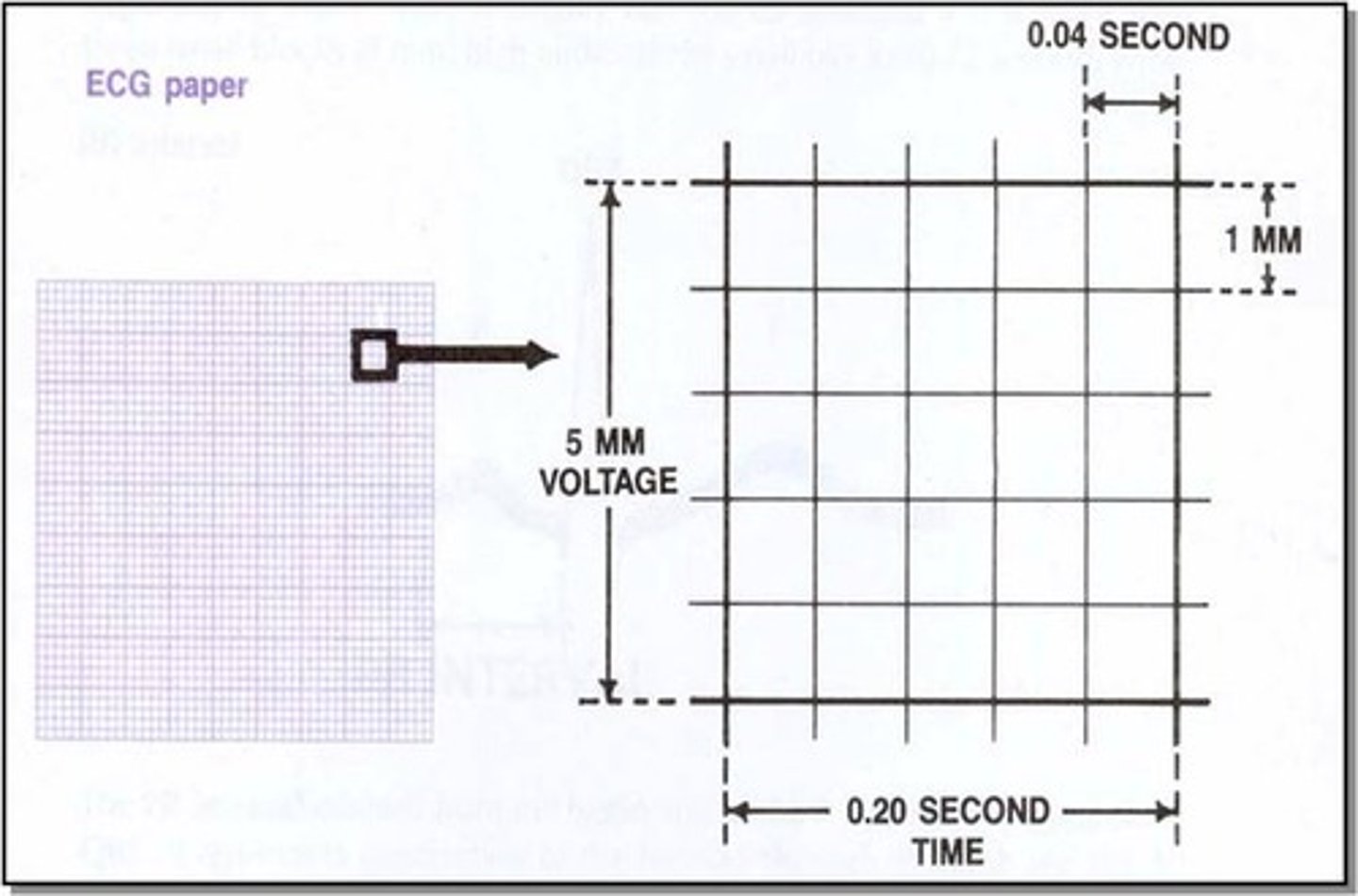
What is the treatment for third degree heart block?
The treatment for third degree heart block is a pacemaker
Atria and ventricles beat independently of each other (P waves have no relation to QRS waves)
In third-degree atrioventricular block, the atria and the ventricles beat independently from each other
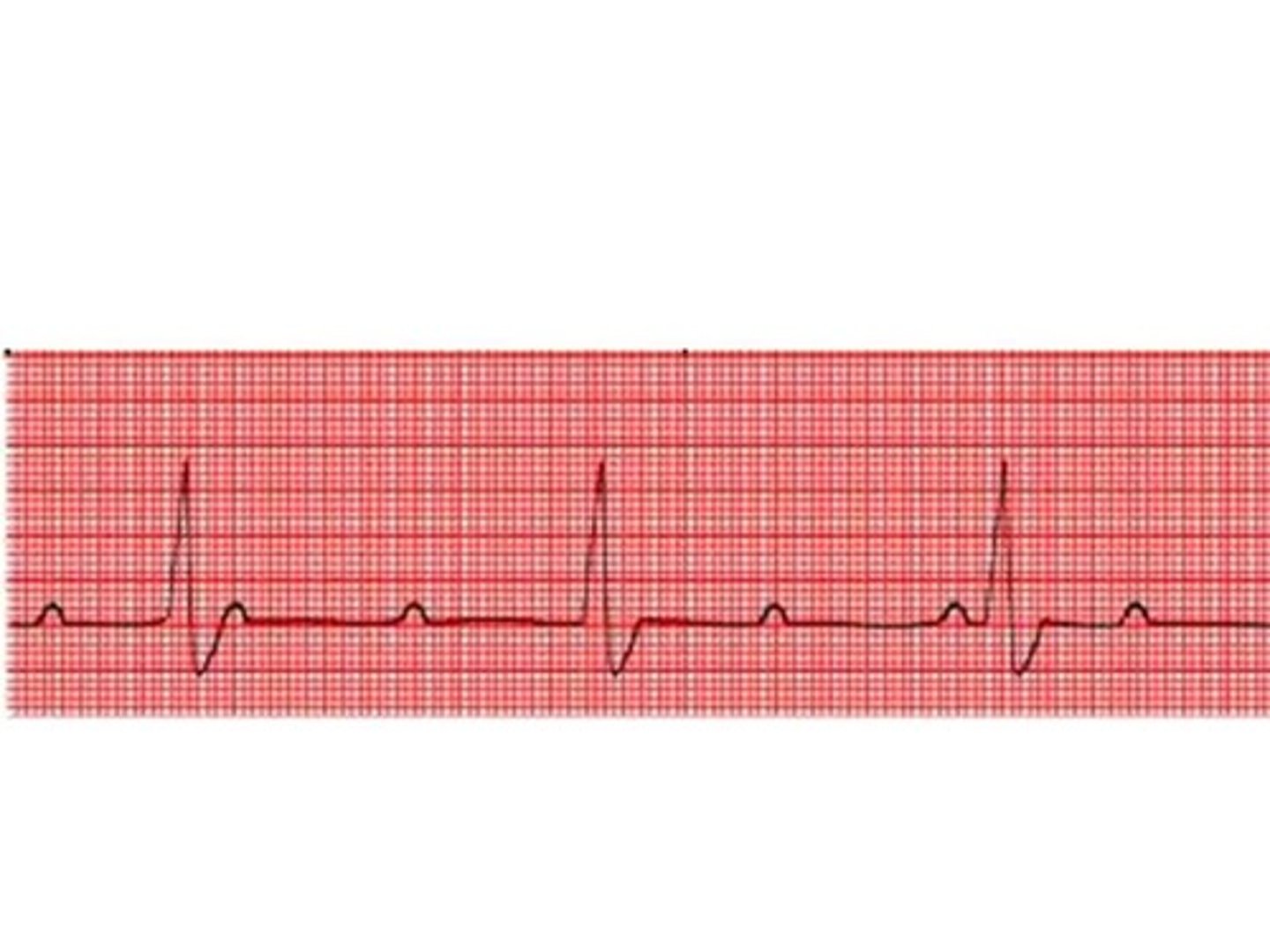
Lyme disease can cause what type of atrioventricular block?
Lyme disease can cause a third degree atrioventricular block
What describes the atrial rhythm in third degree atrioventricular block?
In third-degree atrioventricular block, the atrial rhythm is usually regular
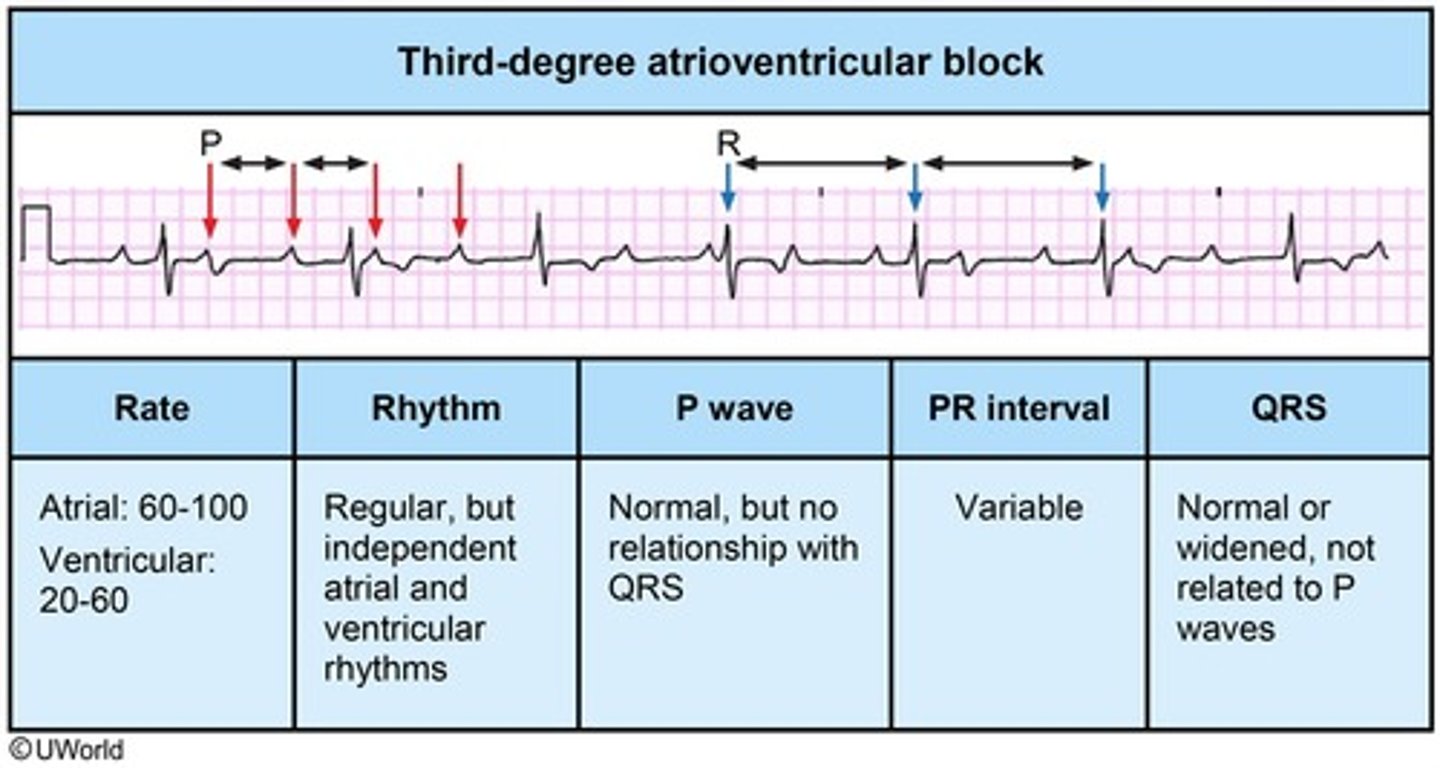
What is the treatment for first degree heart block?
First-degree AV block is rarely symptomatic and no treatment is required, but further investigation may be indicated when it accompanies another heart disorder or appears to be caused by drugs
What is the most common cause of third degree atrioventricular block?
The most common cause of third-degree atrioventricular block is myocardial ischemia
Describe the PR interval on ECG of Mobitz type I second-degree atrioventricular block
Mobitz type I second-degree atrioventricular block (Wenckebach block) has a variable PR interval on ECG
What class of medication is contraindicated in all types of heart block?
Calcium channel blockers are contraindicated in all types of heart block
What is bundle branch block?
A bundle branch block is when the electrical signal from the AV node gets blocked or delayed along one of the bundle branches in the ventricles
What causes a bundle branch block?
In most cases bundle branch block is caused by fibrosis or scarring, that either occurs acutely or chronically
● Acute causes can be things like ischemia, heart attack, or myocarditis
● Chronic conditions include hypertension, coronary artery disease, and cardiomyopathies
Is Right or Left BBB considered to be always pathological?
Right bundle branch block is not always pathological whereas a new left bundle branch block is always pathological and can be a sign of myocardial infarction. Left = Lousy!
A QRS complex duration on ECG of more than _________________ is common in bundle branch block?
Because one of the ventricles is contracting late, a QRS complex of more than 0.12 sec (120 milliseconds) is common to see in a bundle branch block
Which bundle branch blocks have a M shaped R complex in V6?
Left bundle branch blocks have a M shaped R complex in V6. If the QRS looks like W in V1 and M in V6 it is LBBB (WiLLiaM)
Which bundle branch blocks have a M shaped QRS complex in V1?
Right bundle branch blocks have a M shaped QRS complex in V1. If the QRS looks like M in V1 and W in V6 it is RBBB (MoRRoW)
Which bundle branch blocks have a W shaped QRS complex in V1?
Left bundle branch blocks have a W shaped QRS complex in V1. If the QRS looks like W in V1 and M in V6 it is LBBB (WiLLiaM)
Which bundle branch blocks have a W shaped QRS complex in V6 with a deep, wide S waves.
Right bundle branch blocks have a W shaped QRS complex in V6 with a deep, wide S waves. If the QRS looks like M in V1 and W in V6 it is RBBB (MoRRoW)
R and R' (upward bunny ears) in V4-V6
Left BBB
rsR' "bunny ear" pattern in the anterior precordial leads leads V1-V3
Right BBB
What pulmonary disorder is a common cause of right bundle branch block?
Pulmonary embolism is a common cause of right bundle branch block
Treatment of BBB?
No specific treatment is indicated. If there's an underlying condition, such as heart disease, that condition needs treatment. In patients with heart failure, a cardiac resynchronization pacemaker can relieve symptoms as well as prevent death
What is paroxysmal supraventricular tachycardia (PSVT)?
Paroxysmal supraventricular tachycardia (PSVT) is a type of arrhythmia that occurs when a short circuit rhythm develops in the upper chamber of the heart. This results in a regular but rapid heartbeat that starts and stops abruptly.
The short circuit of PSVT is caused by one of three conditions what are they?
The three conditions causing PSVT include:
1. AV nodal re-entrant tachycardia
2. Wolff-Parkinson-White (WPW) syndrome
3. Atrial Tachycardia
AV nodal re-entrant tachycardia?
Atrioventricular nodal reentrant tachycardia (AVNRT) is the most common type of supraventricular tachycardia and occurs when a small extra pathway exists in or near the AV node
Wolff-Parkinson-White (WPW) syndrome?
Wolff-Parkinson-White (WPW) syndrome is a type of PSVT caused by the presence of an abnormal accessory electrical conduction pathway between the atria and the ventricles (Bundle of Kent fibers)
Atrial tachycardia?
Atrial tachycardia is responsible for about 5 percent of PSVTs. It occurs when an electrical impulse fires rapidly from a site outside the sinus node and circles the atria, often due to a short circuit.
Atrioventricular nodal reentrant tachycardia (AVNRT) on EKG?
On the ECG, AVNRT appears as a regular rhythm with a rate ranging between 150 to 250 beats per minute, and a narrow QRS complex. The key is the absence of normal P waves, which tells us that the SA node is no longer in control.
Hallmarks on EKG of Wolff-Parkinson-White syndrome?
Wolff-Parkinson-White syndrome hallmarks on EKG include a shortened PR interval, widened QRS, and delta waves
WPW EKG
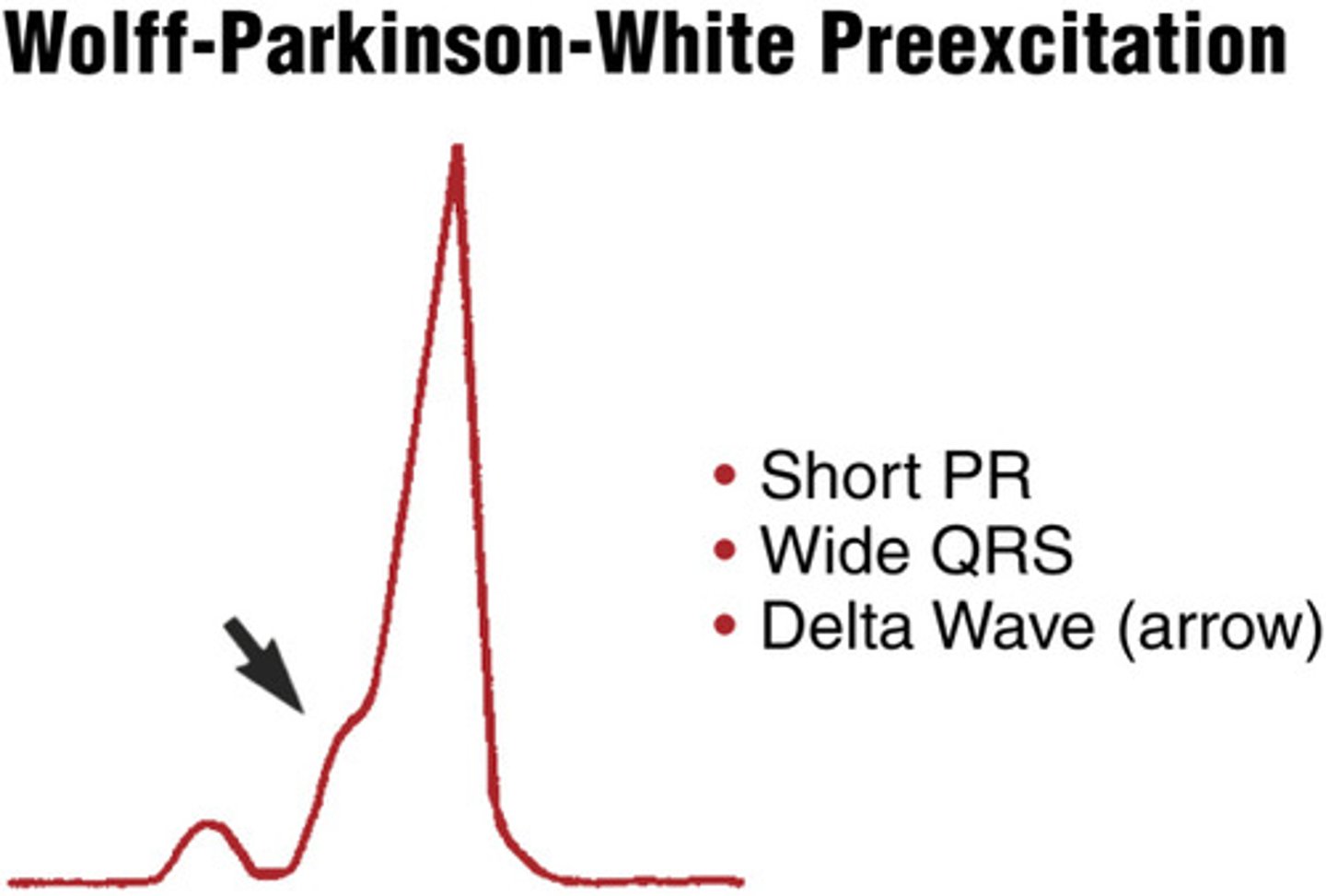
Diagnosis of PSVT?
Holter monitor likely needed to "catch" episodes while patient is symptomatic
First line treatment for PSVT?
PSVTs are classically treated with vagal maneuvers like carotid massage
If vagal maneuvers don’t work, what's the next step for treatment?
If vagal maneuvers don't work, the next step for treatment is adenosine. WPW - do not administer adenosine or calcium channel blockers