CHAPTER 2: DYNAMICS OF DISEASE TRANSMISSION
1/30
Earn XP
Description and Tags
Covers Chapter 2 and Lecture 2
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
31 Terms
Carrier
A person who harbors the organism but is not infected enough to be recognized as sick
What is the definition of endemic, epidemic, and pandemic? What is the difference between those three?
Endemic: expected presence of a disease in a population
Epidemic: occurrence of disease in a community that is CLEARLY above the normal expectancy
Pandemic: An epidemic that is spread across many countries or continents
Differences between the three: Endemic is normal levels, epidemic is when the disease is ABOVE what is normally expected, pandemic is epidemic on a global scale
Outbreak
When a disease occurrence rises above expected
Goals when this happen: find out what caused it, how it was transmitted, and how to stop it
Herd Immunity
If a large enough proportion of people are immune, transmission is reduced because the chain of infection gets interrupted
Incubation Period
the time from exposure to an infecitous agent to the appearnce of symtoms
Latent Period
time from infection to becoming infectious
What is the difference between latent and incubation period?
Latent: from exposure to becoming INFECTIOUS
Incubation: from exposure to displaying SYMPTOMS
Cross Tabulation
method of comparing disease occurnece across combinations of exposures
Infectious Dose 50
The amount of a pathogen needed to infect 50% of exposed hosts.
Define attack rate and what is the formula?
Proportion of people who will become ill among those at RISK during an outbreak
Formula: (number of people who becomes ill/total number of people AT RISK) x 100
What does a low infectious dose rate mean?
A low infectious dose means fewer organisms are needed to cause infection, so infection can happen more easily.
What are the 4 parts of the Epidemiologic Triad?
Host (person), AGENT (cause of disease), ENVIRONMENT (outside conditions that allow the transmission or exposure), VECTOR (organism that carries an agent between hosts
What are the 4 types of Agents?
Biologic like bacteria, chemical like heavy metals, physical like trauma, and nutritional
What are the two modes of disease transmission?
Direct transmission and indirect transmission
What are the different kinds of direct transmission?
Airborne, direct contact, fecal-oral, mother to child, and sexual
What are the two types of indirect transmission? What is the difference between them?
Common vehicle and vector-borne transmission; Common vehicle requires a contaminated source shared by multiple people whereas a vector born transmission is transmission through an organism
What are the 3 types of common vehicle exposure?
Single exposure, multiple exposures, continuous exposure
What affects how easily disease spreads?
Rate of growth, route of transmission, how easily it moves person to person, how many susceptible people are in the community
Define clinical and subclinical diseases. What is the difference between them?
Clinical Disease: Symptoms are obvious enough to be recognized
Subclinical disease: Disease is present but there are no obvious symptoms
The difference is how obvious the symptoms are and subclinical disease reveals the iceberg concept
Spectrum of Disease Severity
Inapparent/subclinical, mild disease, moderate disease, severe disease, fatal disease
Common Source Outbreak
When many people are exposed to the same source such as a contaminated water supply or a food at a picnic
What are the three types of common-source outbreaks? How can you analyze that on a graph?
Point Source Outbreak is when everyone is exposed duringa brief, single time period
Continuous common source outbreak is when exposure continues over time
Intermittent common-source outbreak is when exposure happens on and off
On a graph, point source outbreak shows up as a sharp rise then a decline; on a continuous common source outbreak persistent cases across a longer interval and intermittent appears as irregular peaks separated by gaps
Steps in Investigating an Acute Outbreak
Confirm the outbreak and establish a diagnosis
Examine distribution of cases
develop hypotheses
test hypotheses
control further spread
recommend control measures
Prepare a written report
Communicate findings and implement policy
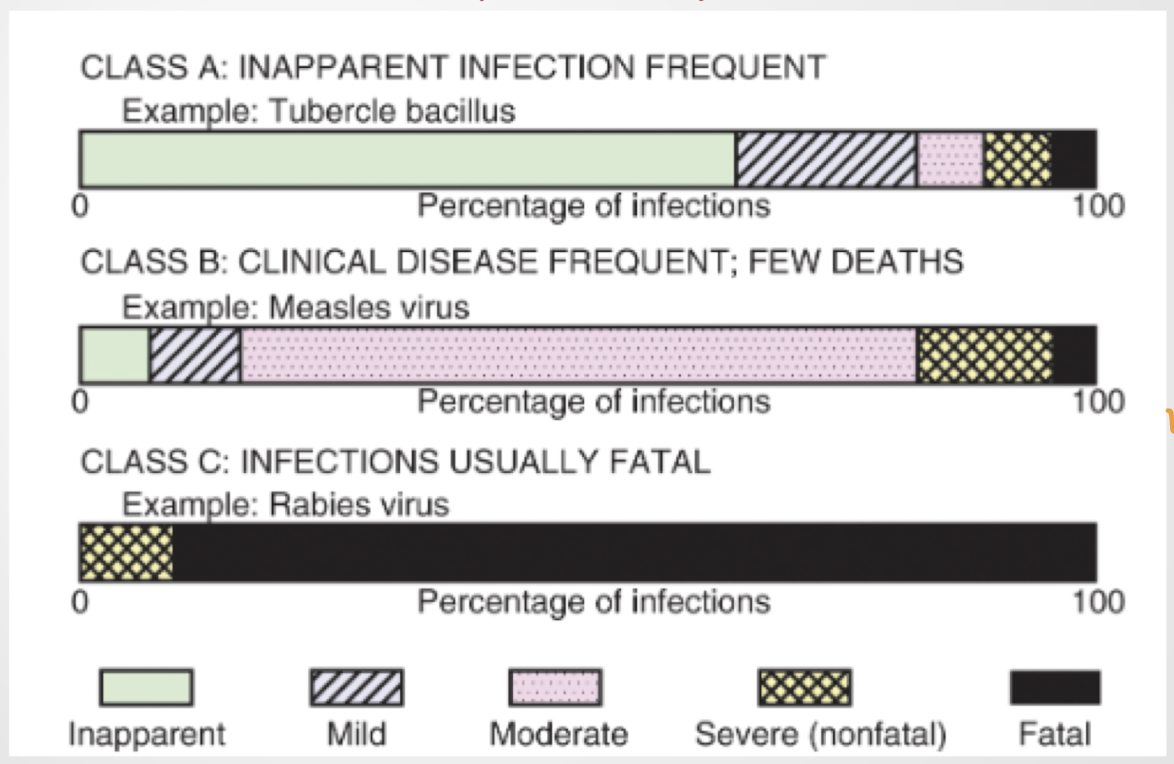
CLICKER QUESTION:From a public health perspective, where should limited public health dollars be spent and why?
Class A: There are potential asymptomatic people because there are a lot of infections that are inapparent, which could worsen the spread. As a result, a potential treatment is to give testing to prevent the spread.
Class B: There is a lot of infections with moderate symptoms so this is an argument. However, the fatality rate is low so you have to consider that.
Class C: very few cases, but the fatality rate is extremely high so it is important to have treatment immediately once you know you have the disease.
Why is exposure not always equal to infection?
Host: Everyone can have different immunity levels/vaccination
Agent: There might not be enough particles to cause disease (think Infectious Dose 50)
Environment: Different environments can harbor different kinds of diseases; some cold or hot climates are not much suitable for the infectious agents.
What is the numerator and denominator for case fatality?
Numerator: Number of deaths
Denominator: Total number of diagnosed cases of that disease
CLICKER QUESTION: An infection was transmitted at a community pool. Out of 200 people who visited the pool, only 100 went into the pool. Ultimately, it was determined that 50 individuals were infected, and 5 of those infected individuals died. What is the Case Fatality Rate (CFR)?
Solution: Numerator is 5 because 5 infected individuals died and denominator is 50 because out of everyone only 50 people were infected.
Answer: 10%
What is the numerator and denominator for attack rate?
Numerator: Number of NEW CASES
Denominator: Total population AT RISK
CLICKER QUESTION: An infection was transmitted at a community pool. Out of 200 people who visited the pool, only 100 went into the pool. Ultimately, it was determined that 50 individuals were infected, and 5 of those infected individuals died. What is the Attack Rate (or incidence)?
Solution: Numerator is 50 because 50 people were infected and 100 is the denominator because 100 of them went into the pool meaning htey were AT RISK for getting the disease. Answer: 50%.
CLICKER QUESTION:An infection was transmitted at a community pool. Out of 200 people who visited the pool, only 100 went into the pool. Ultimately, it was determined that 50 individuals were infected, and 5 of those infected individuals died. The incidence or attack rate was 50% and case fatality rate was 10%.
What are the potential primary, secondary, and tertiary prevention measures?
Primary prevention: Use water sanitation and hygiene rules to stop the infection before it starts; Secondary prevention: Use screening and contact tracing to detect and treat cases early; Tertiary prevention: Provide medical care and rehabilitation to manage the disease and prevent further deaths.
CLICKER QUESTION: There is an outbreak of whooping cough at a childcare center. Among 100 kids ages 2 months to 4 years, 8 kids get whooping cough. Based on your investigation you learn that half of the kids (n=50) have previous vaccine history or had whooping cough: 30 kids are fully vaccinated, 18 are partially vaccinated, and 2 had whooping cough before. What is the attack rate for this outbreak?
Solution: Numerator is 8 because they are getting sick, denominator is 100 (because thats the population) MINUS 30 kids because they are not at risk from the vaccine and MINUS 2 because they have had whooping cough before because again they no longer are at risk. Answer: 11.8%