lec 3- absorption, distribution and excretion
1/45
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
46 Terms
what does the degree of interaction between toxic substance and receptors depend on
exposure phase: how much of the substance is around you and how much you take in.
kinetic phase/ toxikinetics (ADME): what happens inside the body
dynamic phase: toxicodynamics: actual damage
EKG
whats external exposure vs external load/dose
The exposure phase. With regard to this phase, a distinction is made between external exposure,
which is defined as the amount or concentration of a substance present in the organism's
environment, and external load (dose), which corresponds to the amount of substance available for uptake by the organism.
How is the membrane described as
fluid mosaic model
what is fluid character of membrane determined by
The fluid character of the membranes is determined largely by the structure and relative abundance of unsaturated fatty acids.
more saturated fatty acids what does it mean
The more unsaturated fatty acids membranes contain, the more fluid-like they
are, facilitating more rapid active or passive transport
what are the ways toxicants/ xenobiotics can pass cell membrane
1. passive diffusion through the membrane phospholipids
2. passive filtration trough aqueous pores
3. active transport
4. facilitated diffusion
5. Endocytosis: phagocytosis and pinocytosis
describe passive diffusion
Small molecules up to MW 100-200 (ethanol, ureum)
Down a conc. gradient
Influenced by
• lipophilicity
• ionisation
• blood flow: create gradient across membrane
The degree of transport then is determined primarily by
The degree of transport then is determined primarily by the dissociation constant (pK a) of the substance concerned and the pH in the compartment concerned.
what is pka
defined as the pH at which 50% of the substance is dissociated
is blood flow passive or active
blood flow: create gradient across membrane
Only the non-ionized form (HA) diffuses across membranes, and blood flow maintains the gradient by removing the substance, enabling continuous passive diffusion
describe active transport
Chemicals are moved UP a concentration gradient
The transport system is selective and has the potential for competitive inhibition
Requires energy (ATP): sensitive to inhibition by metabolic inhibitors
The transport system is saturated at high substrate concentrations (Tmax)
Describe facilitates diffusion
● it does not require energy and
● transport down a concentration gradient
two groups integral membrane proteins involved:
● carrier proteins (hexose/glucose transporters)
● ion channels (Cl -, Na+)
how is glucose transported
glucose is transported through facilitated diffusion through a glucose transporter
flavonoid-glycosides can be absorbed via
the glucose transporters in the small intestine
phagocytosis
This is a process where the cell membrane encloses solid particles
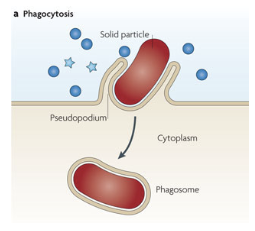
pinocytosis:
small amounts of liquid containing solutes (pinocytosis)
cell drinking , almost all cells, ingestion of drops or small aprticles (<1 mm)
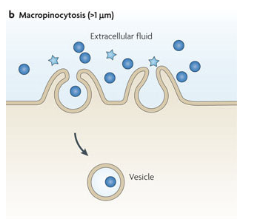
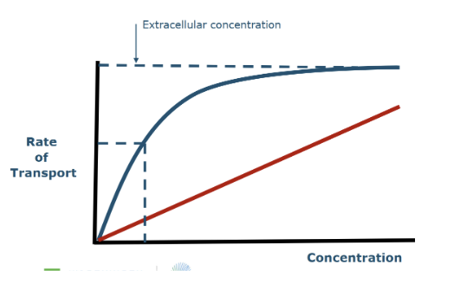
draw graph for uptake kinetics
red line is passive
blue line theres plateau, enzymes become saturated
what are the main exposure routes toxic subtances are taken up by
1. the respiratory system,
2. the digestive or gastrointestinal tract,
3. the skin,
4. alternative routes including the gills (in fish and aquatic invertebrates) or injection of drugs
what is absorption
transfer of chemical from site of exposure into the systemic circulation
what does rate of absorption depend on
- Conc chemical at absorbing surface
- Area of exposed site
- Characteristics of epithelial layer where absorption takes place
- Intensity of sub-epithelial circulation
- Physiological properties of toxicant
what can happen during transfer of chemical from site of exposure
chemical can get eliminated
where does elimination of chemical during transfer from site of exposure occur usually
Liver
GI mucosa -gastrointestinal mucosa
First pass elimination
reduces toxic effects of chemicals that reach their target sites by the way of systematic circulation.
give example of first pass effect
Lidocaine: most important local anaesthtic
- Extensive first pass metabolism in liver
- Useless upon oral dose
Absorption of xenobiotics through the wall of the digestive tract should be considered a
Passive transport
uptake of nutrients taking place through
active transport
what type of compounds are harder to take up through intestinal wall
Generally, highly dissociated substances and hydrophilic
compounds are either hardly taken up through the intestinal wall or not at all, unless the epithelium has
been damaged.
what is the bucco-enteral cycle
Absorbed → excreted via saliva → reabsorbed in intestine
Occurs with: lead, silver, mercury, arsenic
what is the entero-hepatic cycle
Absorbed intestine → liver → bile → intestine → reabsorbed
Example: DES conjugates
what is the name of barrier function layer in skin
horny layer
What plays biggest role in dermal uptake and what doesnt
The pores little importance in uptake as they give little contribution to skins total surface. Dermal uptake increases with increasing temp through hyperaemia (increased blood flow through skin) and hydration (higher water content of horny layer)
Describe distribution
Toxicants leave blood during distribution phase, enter extracellular phase and may penetrate into cells.
what molecules move readily inside cells
Lipid soluble compounds move readily into cells by diffusion unlike ionised and hydrophilic compounds.
what is distribtuion mainly controlled by
Distribution mainly determined by blood circulation.
what are the main routes of distribution
cappilaries
intracellular space
fenestrae
what factors affect distribution speed
blood flow
diffusion rate
tissue affinity
what can cause uneven distribution
substances bind to proteins/tissue causing uneven distribution an longer residence time.
give name of plasma protein
Albumin
what does albumin do
Plasma proteins (Albumin) : It can bind to xenobiotics. reversible binding. In bound form not avialble for distrubution or filtration by kindey. Protects individual to some extent against toxic effects.
what are the 2 organs with high capacity for binding and accumulation
Liver and Kidney
give an example of something that binds in liver and kidney
metallothionein binds cadmium and other metals in the liver and the kindey.
Which substances accumulate in fatty tissue
Substances with high octanol/water partition coefficient ( lipholicic PCBs, PBBs, dioxins, DDT) often accumulate in fatty tissue.
whats another place toxicants can accumulate in
bones - long term storage sites
what is it called when toxicants accumulate in bones
skeltal fluorosis
F- replaces OH- in bones
excessive tea drinking
what is the specific blood brain barrier
CNS (central nervous system)- site less permeable than other sites
no fenestrae
less permeable due to tighter junctions
Low protein content of interstitial fluid
mainly active transport
not fully developed at birth: toxicity for newborn.
these features provide some protection against distribution of toxic chemicals to the CNS and thus against toxcicity.
describe the placental barrier
-Not really a barrier
- toxic agents: pass by passive diffusion
alcohol easily crosses the placental barrier
what are the routes of excretion
kidney: urinary excretion
liver: via bile, fecal excretion
lung: exhalation
other routes: mother milk, saliva, sweat