Lecture 4: Surgery of the Spleen
1/37
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
38 Terms
What is enlargement of the spleen from any cause?
splenomegaly
What is splenectomy?
surgical removal of the spleen
What is congenital or traumatic presence of multiple nodules of normal splenic tissue in the abdomen?
splenosis
What are siderotic plaques?
brown or rust-colored deposits of iron and calcium on splenic surface
What is splenorrhaphy?
suturing of a ruptured spleen
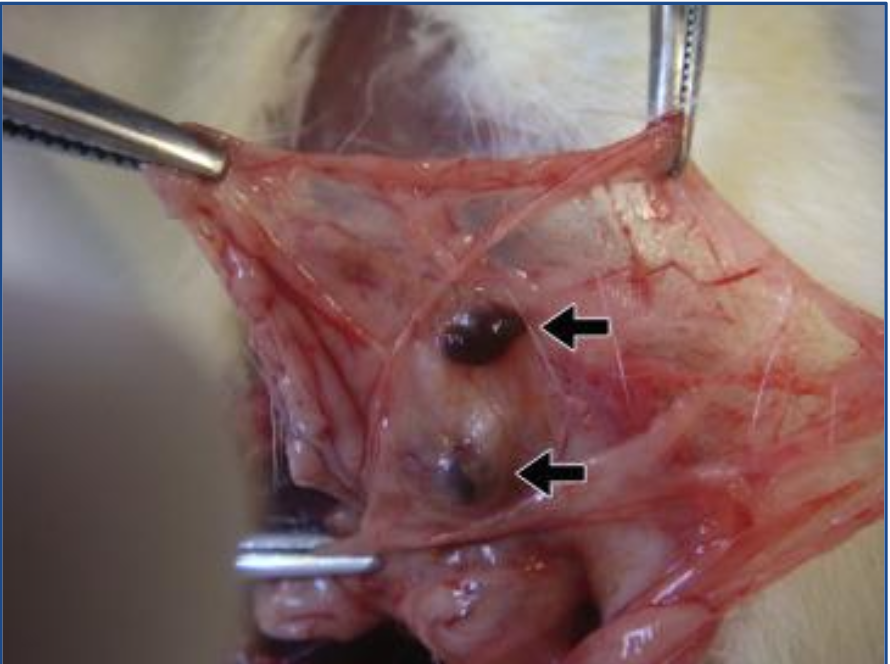
What is this?
splenosis
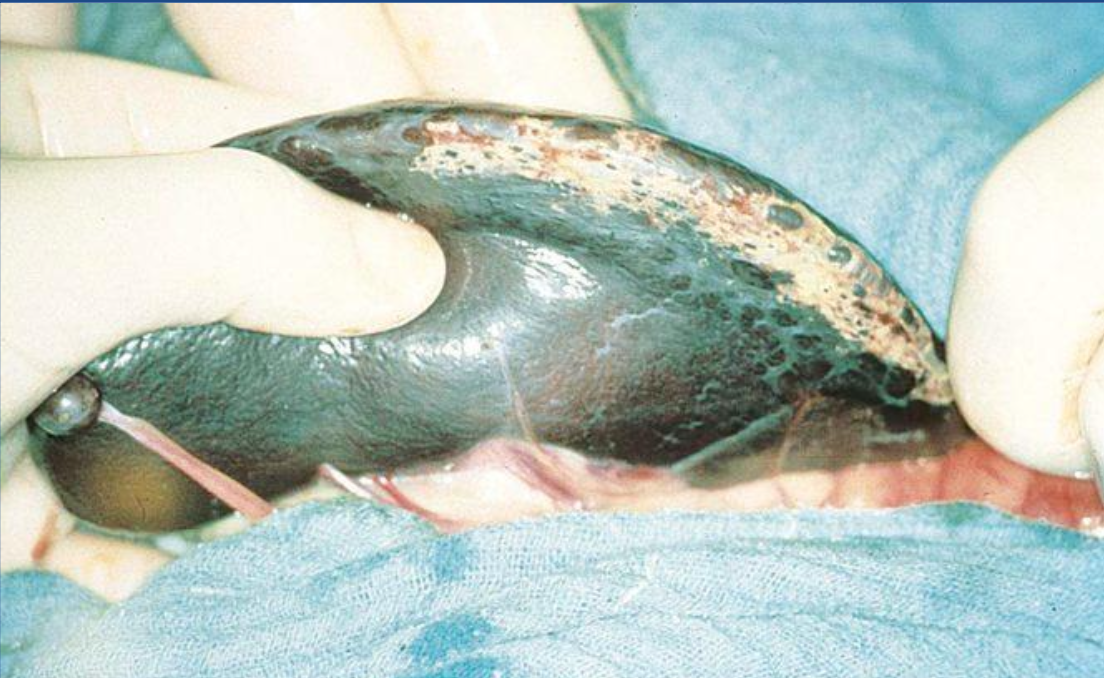
What is this?
siderotic plaques
What is malignant neoplasm arising from blood vessels?
hemangiosarcoma
What are hemangiomas?
benign tumors of dilated blood vessels
What is a swelling or mass of blood (usually clotted) confined to an organ, tissue, or space caused by seepage of any reason?
hematoma
What are the indications for splenic surgery?
Masses
Loss of vascularity secondary torsion: GDV, splenic torsion
trauma
refractive immune-mediated hematologic disorders in some individual cases
True or false: Incidentally found, non-ruptured splenic masses or nodules without associated hemoperitoneum are most commonly benign.
true
What causes diffuse (symmetric) splenomegaly?
• Congestion (Torsion, GDV, Right-sided heart failure, Drugs)
• Infiltration due to infection (Fungal, Bacterial, Rickettsial)
• Splenic foreign body
• Immune mediated disease (IMHA, IM Thrombocytopenia)
• Neoplasia (Lymphosarcoma, Histiocytic sarcoma, Feline mastocytosis)
What are the causes of focal (asymmetric) splenomegaly?
• Benign processes (Nodular regeneration, Hematoma, Trauma)
• Neoplastic processes (Hemangiosarcoma = HSA)
What is one of the most common causes of spontaneous splenomegaly in dogs and cats?
infiltrative splenomegaly from neoplasia
What is splenic torsion most often associated with?
GDV
What happens with splenic torsion?
splenic vein becomes occluded
splenic artery is partially blocked (infarction)
splenomegaly
acute or intermittent signs for weeks
What downstream effects are splenic torsion associated wtih?
cardiovascular collapse and shock, increased likelihood of GDV, septicemia from massive bacterial overgrowth in the necrotic splenic tissue, and hemoabdomen
What may be warranted after splenic torsion because of stretching of gastric ligaments resulting in the increased likelihood of GDV?
prophylactic gastropexy with spenectomy
True or false: it is widely accepted that the absence of a spleen to act as a counterbalance to gastric torsions may warrant a prophylactic gastropexy.
false: research has called this practice into question when splenectomy was not related to a GDV or splenic torsion
What is the most common splenic tumor in dogs and the most common malignant splenic tumor in cats?
hemangiosarcoma
Why is an echocardiogram in non-emergent splenectomy to remove a splenic mass warranted in dogs?
as many as 25% of dogs with splenic HSA may have concurrent right atrial HSA
Where does splenic hemangiosarcoma frequently metastasizing?
liver
omentum
mesentery
brain
True or false: splenic hematomas and hemangiomas are grossly indistinguishable from hemangiosarcomas, so you should let your pathologist make the call.
true
What should be assessed during pre-op management for a splenectomy?
anemia (acute hemorrhage with trauma, rupture of hematoma, underlying disease)
coagulation profiles if trauma not suspected as cause of hemorrhage
consider for blood transfusion
assess for hydration
assess for DIC
When do anemic patients need O2?
prior to induction and during recovery
What drugs should be avoided during splenectomies and why?
barbiturates: cause splenic congestion
acetylpromazine: red blood cell sequestration, hypotension, impact on platelet function
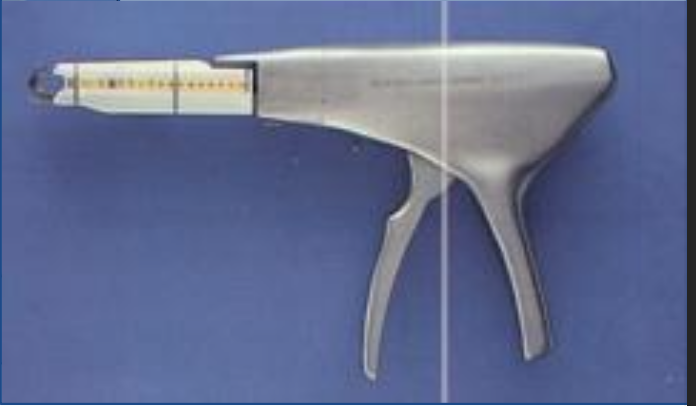
What is this tool?
ligating dividing stapler
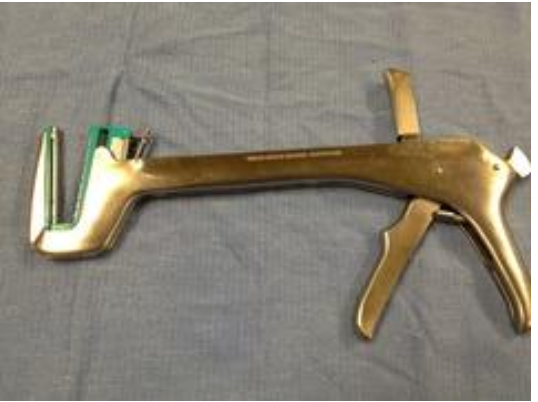
What is this device?
TIA stapler: transverse intestinal stapler
What is the arterial supply of the spleen?
splenic artery, a branch of the celiac artery
Why must you identify the pancreas during a splenectomy?
the first branch of vasculature is usually to the left limb of the pancreas and is its main arterial blood supply → you must identify the pancreatic supply coming off the splenic artery and ligate the splenic artery distal to it
What incision is made for a splenectomy?
ventral midline approach from a xyphoid to a point caudal to the umbilicus (longer for large lesions or complete exploratory for neoplasia)
When is a partial splenectomy indicated?
with trauma or focal lesions to preserve splenic function
What does a total splenectomy result in the loss of?
all splenic function:
RBC reservoir
hematopoiesis
important phagocytic function
help with immunocompetence
When is a total splenectomy contraindicated?
bone marrow hypoplasia
What are the major techniques of total splenectomies?
1. Ligation at splenic hilus
2. Splenic artery ligation
3. Bag Of Rochester Carmalts
4. Laparoscopic
What post-op care and assessment is necessary after a splenectomy?
24 hour observation for hemorrhage and hematocrit every few hours until stable
nasal O2 for anemic patients
fluid therapy
electrolyte and acid-base correction
monitor for cardiac arrhythmias
monitor for DIC
antibiotics after 24 hours if warranted & pain management
What are the commonly seen complications with splenectomies?
hemorrhage (more of an issue with biopsies or partial splenectomy)
traumatic pancreatitis
gastric fistulation due to impairment of gastric blood flow
previous infection with hemoparasites may become apparent after splenectomy