Intro to Sonography: Ultrasound Principles, Techniques, and Reporting
1/131
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
132 Terms
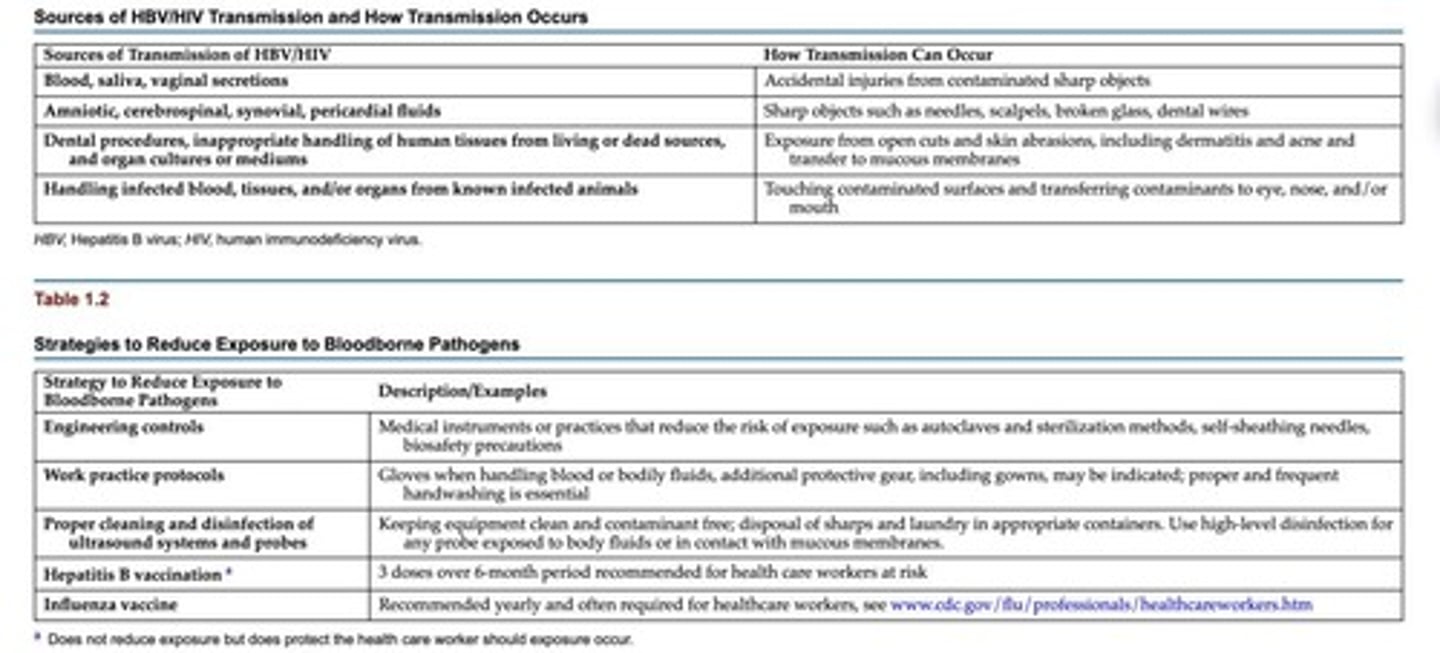
What are Standard Precautions in sonography?
Treating all patients as if they may have HBV/HIV or other bloodborne or infectious diseases.
What is the role of a sonographer?
An ultrasound professional responsible for performing and recording ultrasound studies for physician interpretation.
What is the purpose of reviewing a patient's chart/EMR before an ultrasound exam?
To gather relevant medical history and information that may affect the examination.
What is an Interpretive Report?
A formal, legal report of ultrasound findings provided by the sonologist or radiologist.
What does the Ultrasound Request Form include?
Patient identification data, clinical symptoms, the examination requested, and the reason for the exam.
What is the significance of using two different scanning planes in sonography?
It enhances the accuracy of anatomical visualization and diagnostic information.
What is the Occupational Safety and Health Administration (OSHA)?
An agency that sets standards to protect healthcare workers from bloodborne diseases.
What is the role of a sonologist/radiologist?
A physician responsible for providing the final, legal interpretive report of ultrasound findings.
What are Assessment Notes?
Results of the physical examination, including a listing of the patient's symptoms.
What is Differential Diagnoses?
Multiple pathologic conditions that may be indicated by ultrasound findings.
What is an Electronic Medical Record (EMR)?
A computer-based version of a patient's medical information.
What are Technical Observations/Comments?
Sonographer's written comments and summary of ultrasound findings using sonographic terminology.
What is the importance of handwashing in clinical environments?
To reduce the risk of infection and ensure safety during ultrasound examinations.
What vaccinations are important for healthcare workers in sonography?
Vaccination against HBV and annual influenza vaccinations.
What does proper cleaning and disinfection of ultrasound equipment involve?
Keeping consoles and probes clean and contaminant-free between patients.
What is the primary responsibility of sonographers?
Using ultrasound imaging equipment to produce cross-section images of anatomy and diagnostic data.
What is the significance of scanning competency in sonography?
It is essential for producing high-quality images and requires personal initiative and discipline.
What is the purpose of the American Registry of Diagnostic Medical Sonography (ARDMS)?
To offer certification for sonographers based on professional standards.
What are the key responsibilities of a sonographer?
Excellent communication skills, strong computer skills, and the ability to record patient data.
What is the role of personal protective equipment (PPE) in sonography?
To protect healthcare workers from exposure to bloodborne pathogens.
What is the significance of cross-sectional anatomy in sonography?
It helps in understanding the spatial relationships of structures during imaging.
What is the importance of feedback from instructors and clinical preceptors?
To monitor personal progress and improve scanning skills.
What is the process for high-level disinfection of contaminated probes?
Initial cleaning with an enzymatic cleanser followed by disinfection in a processor.
What does the term 'operator dependent' mean in the context of sonography?
The quality of ultrasound images is highly reliant on the skill of the sonographer.
What is a common requirement for sonography programs?
Previous healthcare experience or a science background is often preferred.
What is the purpose of the SPI exam?
To assess knowledge of ultrasound physics and principles at the time of certification.
What is the significance of personal initiative in sonography?
It is necessary for mastering scanning skills and ensuring image quality.
What is required for all endocavitary probes and probes contaminated with blood?
High-level disinfection procedures.
What should dirty probes be cleaned with before disinfection?
An enzymatic cleanser.
What must be documented for safety compliance in medical facilities?
Logs demonstrating adherence to safety compliance.
Who is typically responsible for providing in-service training on OSHA requirements?
Human Resources or Infection Control departments.
What must sonographers be trained in regarding bloodborne pathogens?
How to reduce exposure to bloodborne pathogens.
What should a sonographer review before an ultrasound exam?
The Order/Requisition/Control Sheet and Patient Chart/Electronic Medical Record (EMR).
What information is included in an ultrasound request form?
Patient identification data, clinical symptoms, type of examination requested, and reason for the examination.
Why is it important to verify patient identifiers before an ultrasound exam?
To ensure the correct patient is being examined.
What key items should sonographers review in a patient's chart?
Assessment notes, laboratory test results, and reports from correlating image modality studies.
What is the significance of the ultrasound request form?
It stresses the information needed for a particular health care facility.
What is the role of a sonographer during the ultrasound exam?
To acquire patient information, perform the examination, and document findings.
What are the essential components to include on image documentation?
Patient name and ID, date and time, scanning site, name of the person performing the study, transducer MHz, patient position, scanning plane, and area of interest.
What are sonographers required to document after the ultrasound exam?
Technical observations and a summary of ultrasound findings.
What should technical observations include?
Descriptions of ultrasound findings based on echo pattern and size.
Why should sonographers not provide diagnoses?
It could be legally compromising.
What is the purpose of case presentation in ultrasound?
To present images and related details of the ultrasound study to the interpreting physician.
What should be included in a case presentation?
Type of examination, reason for it, patient history, lab data, and documentation sequence.
What is the importance of imaging criteria in ultrasound?
It guides transducer selection and anatomy survey.
What knowledge is essential for accomplished scanning techniques?
Location of anatomy, sonographic appearance of normal structures, and interpretation of scanning planes.
What should sonographers do to ensure appropriate exams are performed?
Verify that the ultrasound orders match the indication for the exam.
What is the significance of the patient's clinical symptoms in the ultrasound request?
They provide the rationale for the ultrasound study being ordered.
What is the role of the interpreting physician in relation to the sonographer's findings?
To arrive at a diagnosis based on the ultrasound images and technical observations.
What is the importance of understanding normal sonographic appearance?
It provides a baseline to recognize abnormalities.
What should be included in the summary of ultrasound findings?
Technical observations based on echo pattern, size, origin, location, number, and composition of findings.
What does the term 'knobology' refer to in ultrasound?
The understanding of the controls and settings on the ultrasound machine.
What is the importance of patient care during the ultrasound examination?
To ensure the patient's comfort and safety throughout the procedure.
What is the purpose of the interpretive report?
To document what the radiologist dictates from the ultrasound images.
What does the interpretive report from a sonologist include?
A detailed description and diagnosis of the ultrasound findings.
What is the purpose of the final report in an ultrasound examination?
To provide a definitive or differential diagnosis based on ultrasound findings.
What is the best patient position for evaluating the abdominal aorta?
The supine position.
What transducer frequency is best for imaging superficial structures?
Higher-number megahertz (MHz) transducers.
What transducer frequency is best for evaluating deep structures?
Lower-number megahertz transducers.
What is the recommended way to hold a transducer?
Like a pencil to reduce wrist strain and allow ease of movement.
What are the three primary body planes used in ultrasound?
Sagittal/Longitudinal, Transverse, and Coronal.
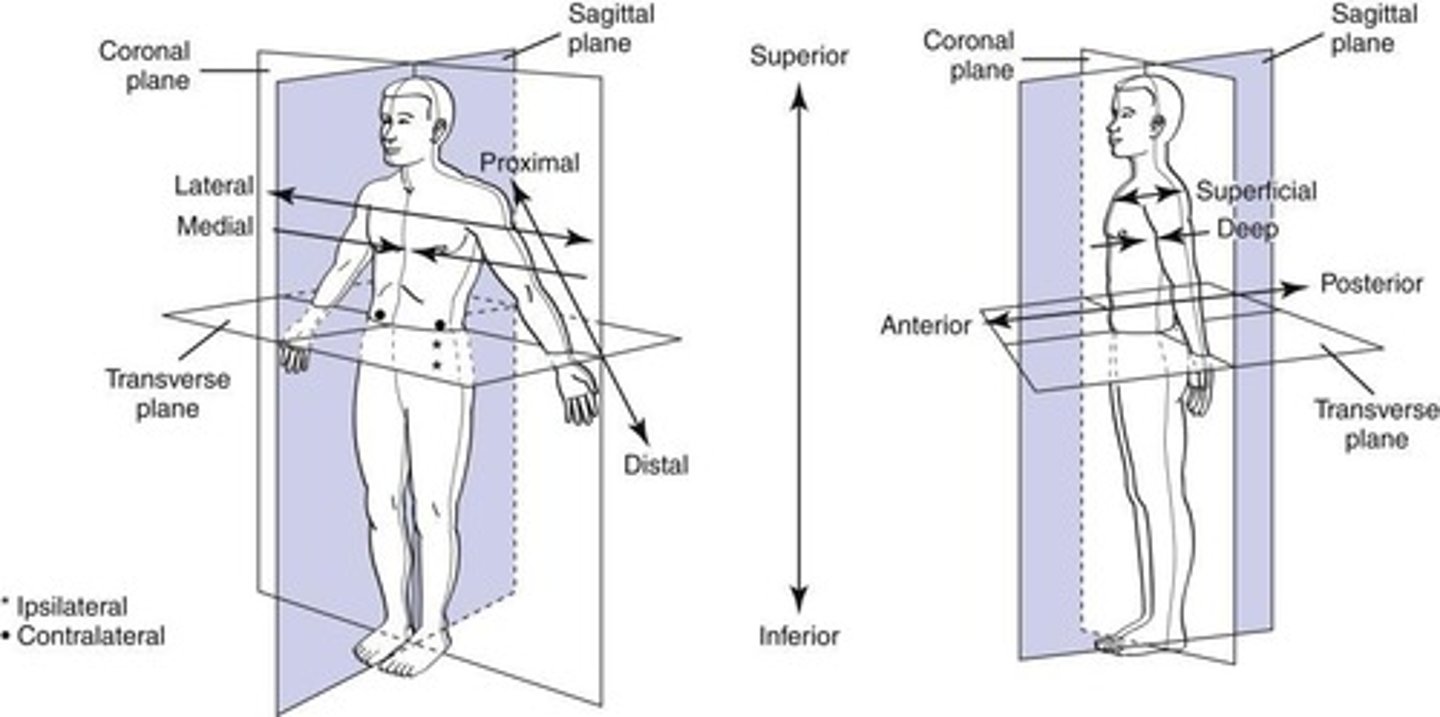
What does the sagittal plane do?
Splits the body into right and left sides.
What does the transverse plane do?
Splits the body into top (superior) and bottom (inferior) parts.
What does the coronal plane do?
Splits the body into front (anterior) and back (posterior) parts.
What are the directional terms used in anatomy?
Superior, inferior, anterior, posterior, medial, lateral, superficial, deep, proximal, distal, ipsilateral, contralateral.
What are the nine regions of the abdomen?
Right hypochondrium, epigastrium, left hypochondrium, right lumbar, umbilicus, left lumbar, right iliac, hypogastrium, and left iliac.
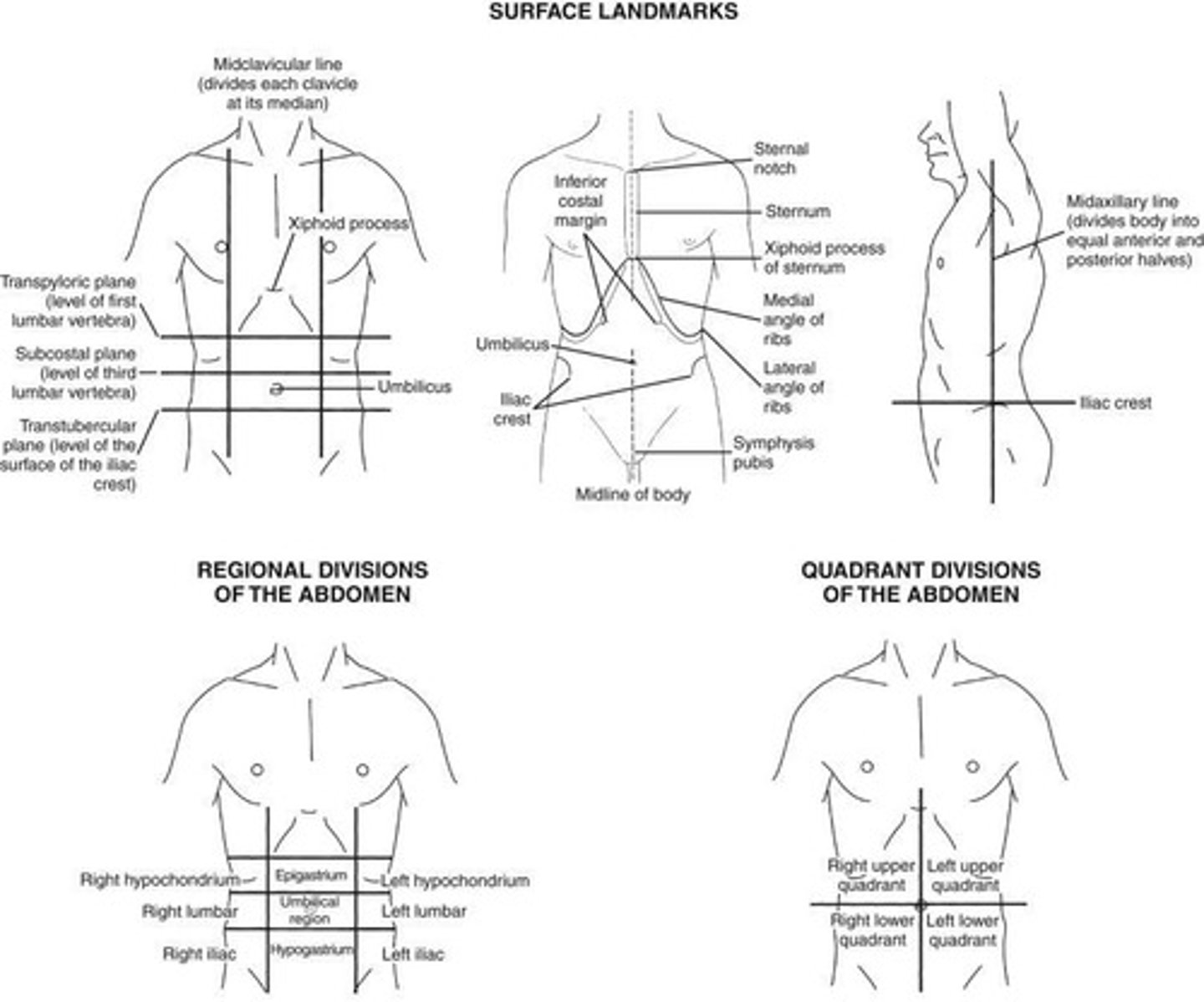
What are the four quadrants of the abdomen?
Right upper quadrant (RUQ), left upper quadrant (LUQ), right lower quadrant (RLQ), and left lower quadrant (LLQ).
What does 'homogeneous' mean in sonographic terminology?
Uniform or similar echotexture.
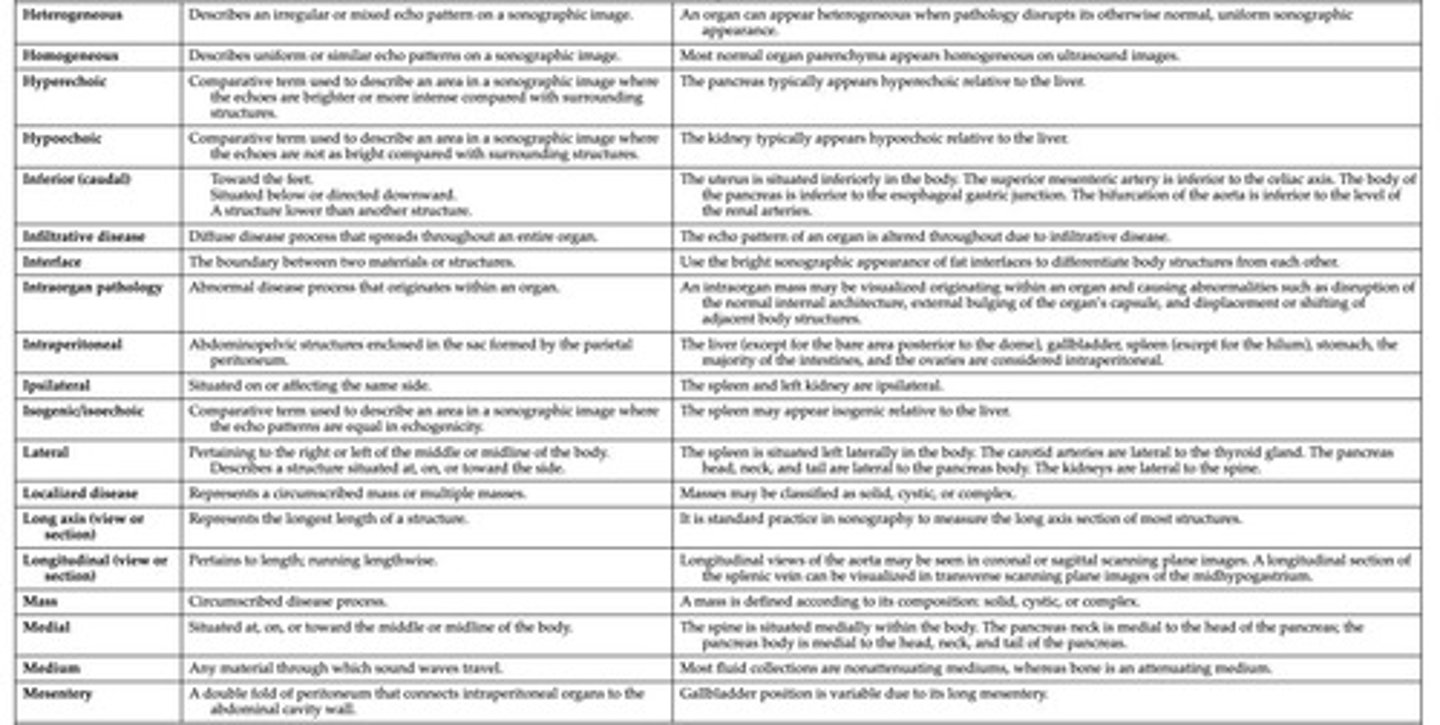
What does 'heterogeneous' mean in sonographic terminology?
An irregular or mixed echo pattern/echotexture.
What does 'anechoic' mean?
Without internal echoes; appears black on ultrasound.
What does 'isoechoic' mean?
Same echogenicity as surrounding structures.
What does 'hypoechoic' mean?
Fewer echoes returning to the transducer; appears darker than surrounding structures.
What does 'hyperechoic' mean?
More echoes returning than usual; appears brighter than surrounding structures.
What is the significance of recognizing changes in echo patterns?
It suggests an abnormality in the structure being examined.
What is the role of ultrasound in diagnosing internal body structures?
To provide comprehensive sonographic details for diagnosis based on typical appearances.
What happens to the sonographic appearance of a structure when pathology is present?
It disrupts the normal appearance by changing its shape, size, contour, or texture.
What is the importance of documenting differences in echo patterns?
To accurately describe abnormalities and assist in diagnosis.
What is the typical appearance of normal organ parenchyma in ultrasound?
Described as homogeneous or uniform in texture.
What is the effect of disease on the echogenicity of soft tissue structures?
It typically causes an irregular or heterogeneous echo pattern.
What is the normal appearance of organ parenchyma on ultrasound?
Homogeneous, or uniform in texture.
How does parenchyma appear when disrupted by disease?
It typically appears heterogeneous with an irregular echo pattern.
What are the two types of changes in parenchyma due to disease?
Diffuse (infiltrative) and localized (mass or multiple masses).
What characterizes infiltrative diffuse disease on ultrasound?
The parenchymal texture is altered and appears heterogeneous with varying echogenicity.
What happens to organ parenchyma as infiltrative diffuse disease advances?
It can become coarse or patchy with necrotic, blood-filled spaces.
What must a sonographer determine when diffuse disease causes organ enlargement?
The extent of increase and whether adjacent structures have been compromised.
How might a sonographer describe an enlarged liver affected by diffuse disease?
The liver appears enlarged and hyperechoic compared with the pancreas.
What is a potential ultrasound description of progressive diffuse disease in the liver?
Liver shape appears altered with coarse, scattered increases in echogenicity and multiple fluid-filled, anechoic spaces.
What can diffuse infiltrative disease of the spleen cause?
It can displace adjacent structures, particularly the left kidney.
What is a common ultrasound finding when the pancreas head is enlarged?
It can dilate the common bile duct (CBD) and compress the inferior vena cava (IVC).
What defines localized disease in ultrasound findings?
A mass or multiple masses circumscribed to a specific area.
What should mass descriptions include when assessing localized disease?
Origin/location, size, composition, number, and any complications with adjacent structures.
What are the two classifications of localized disease origin?
Intraorgan (originates within an organ) and extraorgan (originates outside an organ).
What features characterize intraorgan disease?
Disruption of normal internal architecture, external bulging of organ capsules, and displacement of adjacent structures.
What is the standard practice for measuring a mass in ultrasound?
Measure length, greatest height, and width to calculate volume.
How can the composition of a mass be classified?
As solid, cystic, or complex.
What does a solid mass appear as on an ultrasound image?
Echogenic shades of gray representing its tissue composition.
What terms are used to characterize solid tissue masses sonographically?
Homogeneous, heterogeneous, isoechoic, hyperechoic, and hypoechoic.
What can complicate the determination of a mass's origin?
Large masses that obstruct the organ of origin and affect adjacent structures.
What might a sonographer report for a complex cystic mass?
Right upper quadrant, primarily cystic, complex mass with posterior through transmission noted.
What is the significance of measuring individual tumors in localized disease?
If distinguishable, they should be measured individually to assess their impact on organ size.