Block 2 ALS Revision Questions
1/142
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
143 Terms
What are the three main stimulations for breathing?
Central neural rhythm
Chemical control (pH, O2, hormones)
Sensory input
What is the main nerve controlling respiration?
Vagus (X)
What solutions increase breathing?
Acidic
What solutions decrease breathing?
Alkaline
In patients with COPD, what drives their breathing?
Hypoxic drive (low oxygen)
What type of respiratory failure is marked by a raise in CO2?
Type 2
What is the main hormone responsible for altering breathing rate?
Adrenaline
Why does hyperventilating lead to tingling sensation in extremeties?
Blows off CO2 so more alkaline blood
This results in a drop in ionised calcium and causes excessive neuronal activity
Where are the main chemoreceptors found?
Aortic arch
Carotid artery
Which muscles of the thoracic wall are involved in inspiration?
External intercostal (elevate ribs)
Which nerves carries impulses for the cough reflex?
Internal laryngeal (branch of vagus)
What are the two functional divisions of the respiratory system?
Conducting portion - all respiratory passages, cleanse, warm and humidify air
Respiratory portion - site of gas exchange
What type of epithelial cells line the nasal cavity?
Pseudostratified ciliated columnar epithelium with goblet cells
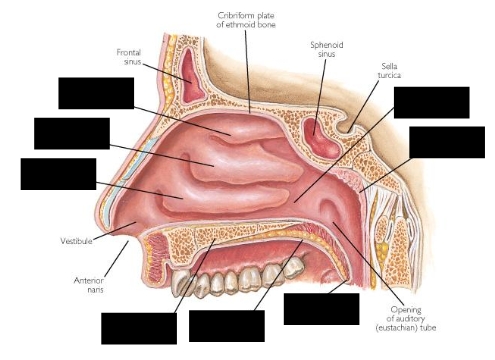
Inferior turbinate
Middle turbinate
Superior turbinate
Choana
Pharyngeal tonsil
Uvula
Soft palate
Hard palate
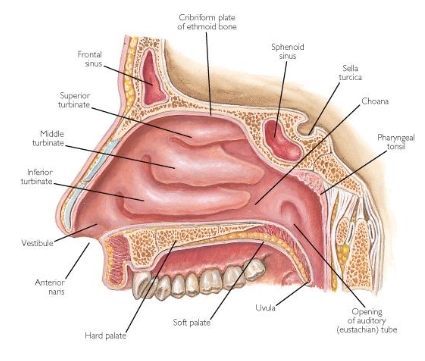
What are olfactory mucosa?
Sensory receptors for smell
What is located superior to the superior turbinate?
Sphenoethmoidal recess
What are the subdivisions of the pharynx?
Nasopharynx
Oropharynx
Laryngopharynx
Where does the nasopharynx begin and end?
Base of skull
Uvula and soft palate
Where does the oropharynx begin and end?
Soft palate
Epiglottis
Where does the laryngopharynx begin and end?
Epiglottis
Cricoid cartilage
What are the three circular muscles of the pharynx?
Superior constrictor
Middle constrictor
Inferior constrictor
What are the three unpaired cartilages of the larynx?
Epiglottis
Thyroid
Cricoid
What are the three paired cartilages of the larynx?
Arytenoid
Cuneiform
Corniculate
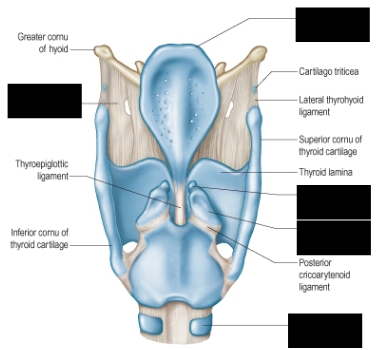
Epiglottis
Thyrohyoid membrane
Corniculate cartilage
Arytenoid cartilage
First tracheal cartilage
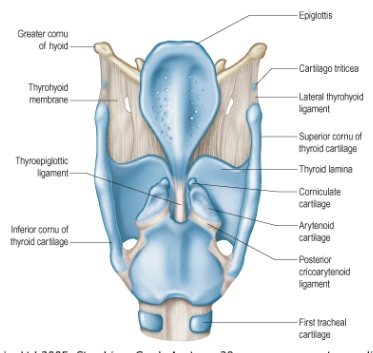
What does the base of an arytenoid cartilage attach to?
Vocal process
What is the function of the laryngeal muscles?
Abduct and adduct the vocal folds
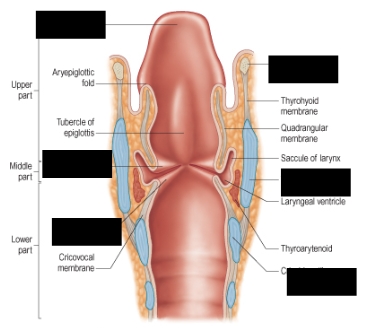
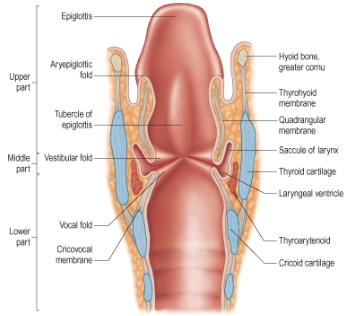
Epiglottis
Hyoid bone, greater cornu
Vestibular fold
Thyroid cartilage
Vocal fold
Cricoid cartilage
At what vertebral level is the thyroid cartilage located?
C3/4
What structures support the trachea?
C-shaped cartilage rings
At what level does the trachea bifurcate?
T4-5
Angle of Louis
In which main bronchus are objects most likely to become lodged and why?
Right main bronchus
Wider, shorter, more vertical
What are the two coverings of the lungs?
Visceral pleura
Parietal pleura
What is the hilum of a lung?
Point where structures enter and leave the lung
What are the three main components of the hilum?
Main bronchus
Pulmonary artery
Pulmonary veins
How many lobes does each lung have?
Right - 3
Left - 2
What is the mechanism of normal inspiration?
Diaphragm contracts and descends
External intercostal muscles contract to raise ribs
Volume of thoracic cavity increases
Intrathoracic pressure drops to below atmospheric
Air moves in down pressure gradient
What effect does the vagus have on the bronchioles?
Constriction
What sympathetic portion dilates the bronchioles?
Sympathetic T2-5
What is the embryological origin of the heart?
Cardiogenic mesoderm
What structure gives rise to the diaphragm?
Septum transversum
What is the mediastinum?
The part of the thoracic cavity between the two pleural cavities
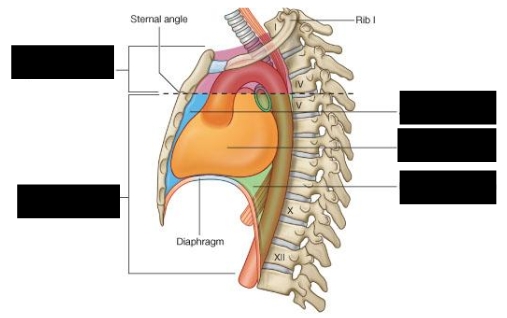
What are the five divisions of the mediastinum?
Superior
Inferior
Middle
Anterior
Posterior
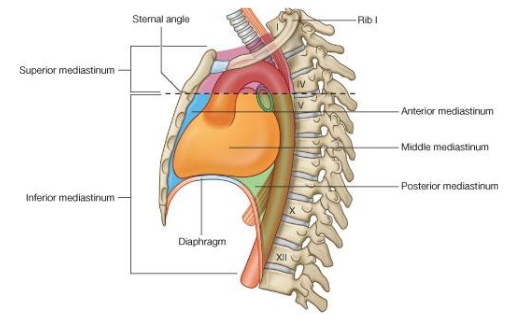
Which portion of the mediastinum do the vagus and phrenic nerves pass through?
Superior
What is the main content of the middle mediastinum?
The heart
What supplies all parasympathetic innervation to the airways?
Vagus nerve
Which spinal segments provide sympathetic innervation to the airways?
T1-6
What are the three cell types in respiratory mucosa?
Ciliated epithelial
Goblet cells
Basal cells
What shape are the mucosa in the bronchioles?
Cuboidal
What is the function of basal cells?
Stem cells that also contribute to structure
What is the ventilation perfusion ratio?
Matching perfusion (blood supply) to areas of greater ventilation
How is the majority of oxygen transported in the blood?
Bound to haemoglobin
What is an alveolar sac?
Two or more alveoli that share a common opening
What epithelial cells line the alveoli?
Simple squamous epithelium
What is the function of type 1 alveolar cells?
Gas exchange
What is the function of type 2 alveolar cells?
Secrete alveolar fluid - reduces likelihood of alveolar collapse by reducing surface tension within alveoli
What are the four layers of the respiratory membrane?
Alveolar wall (type 1 and 2 cells)
Epithelial basement membrane
Capillary basement membrane
Capillary endothelium
What is the rate of removal of carbon dioxide by the lungs?
200ml/min
What is the histology of the terminal bronchioles?
Non-ciliated simple cuboidal epithelium
How is ventilation calculated?
Respiratory rate (/min) x tidal volume (l)
What is FVC?
Forced vital capacity
What is FEV1?
Forced expiratory volume in 1 second
What is the ideal gas law?
P V = n R T
P = pressure (Pa)
V = volume (m3)
n = number of moles
R = gas constant (8.314 J K-1 mol-1)
T = temperature (K)
What is Dalton’s law of partial pressures?
The total pressure of a mixture of gases is equal to the sum of the partial pressures of each gas
What shifts the oxygen dissociation curve to the right?
Reduced pH
Increased PO2
Increased temperature
Increased DPG
What does a shift of the oxygen dissociation curve to the left represent?
Increased affinity of haemoglobin for oxygen
How can carbon dioxide be transported?
Dissolved in plasma (7%)
As carbamino compounds (23%)
As bicarbonate (70%)
What are the metabolic consequences of a drop in blood pH?
Diabetic ketoacidosis (DKA)
Renal failure
What is the smallest contractile unit of muscle?
Sarcomere
Which two proteins are the units of muscle fibres?
Actin - thin filament
Myosin - thick filament
What protein inhibits actin and myosin coupling?
Troponin I
What initiates the contraction of heart muscle?
Sinoatrial (SA) node
What is inotropy?
Increase in the force of contraction
What is the normal duration of the cardiac cycle?
0.8 s
What are the five stages of the cardiac cycle?
Atrial systole
Isometric ventricular contraction
Ejection phase
Isometric ventricular relaxation
Slow filling
What happens during atrial systole?
P wave
Mitral valve open
Aortic valve closed
What happens during isometric ventricular contraction?
QRS
All valves closed
First heart sound - closure of valves
What is the ejection phase?
ST segment
Aortic valve opens
Blood ejected from heart
Valves open when pressure in heart is higher than in the aorta
What happens in isometric ventricular relaxation?
T wave
All chambers in diastole
All valves closed
What happens during slow filling?
V wave on atrial trace
Passive filling of atria and ventricle
AV valves open
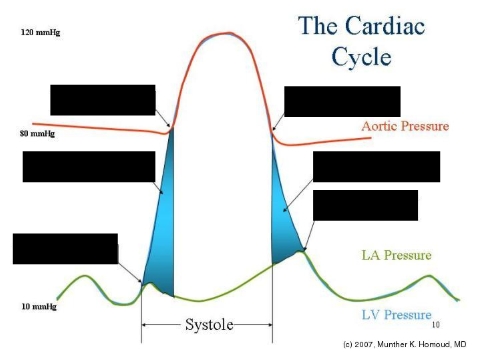
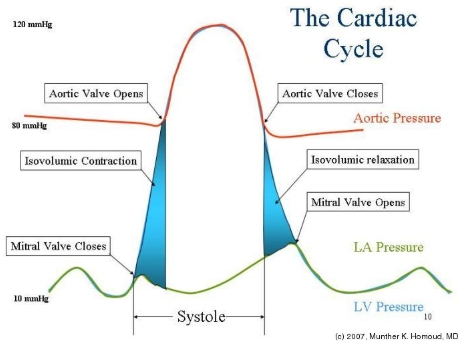
Mitral valve closes
Isovolumetric contraction
Aortic valve opens
Aortic valve closes
Isovolumic relaxation
Mitral valve opens
How is cardiac output calculated?
Stroke volume x heart rate
During exercise, what is the main way to increase cardiac output?
By raising heart rate
What is the Frank-Starling effect?
Increasing fibre length → increased velocity of contraction
Increased end diastolic volume → increased stroke volume
What is unique about cardiac muscle?
It is myogenic
Which ion initiates an action potential in pacemaker cells?
Ca2+
Which two membranes cover the heart?
Fibrous pericardium
Serous pericardium
What does blood flow through from the right atria into the right ventricle?
Right atrioventricular orifice
How many papillary muscles are there in the right ventricle?
3
What attaches each papillary muscle to a cusp of a valve?
Chordae tendinae
What type of valve are the pulmonary and aortic vaves??
Semilunar
What causes the closure of the pulmonary and aortic valves?
Recoil of blood into the sinuses
What embryologically allows the flow of blood between the two atria?
Fossa ovale
What is the embryological origin of the cardiovascular system?
Cardiogenic mesoderm
What supplies blood to the right atrium and ventricle?
Right coronary artery
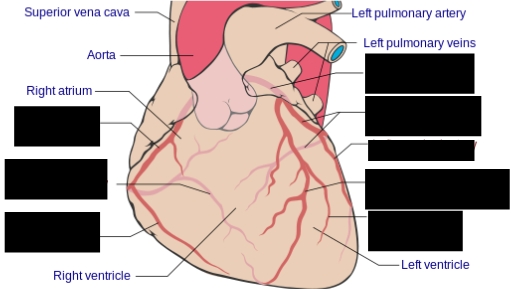
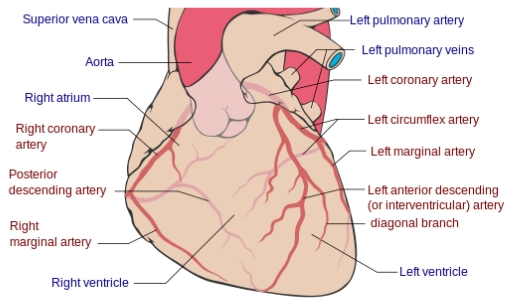
Right coronary artery
Posterior descending artery
Right marginal artery
Left coronary artery
Left circumflex artery
Left marginal artery
Left anterior descending (interventricular) artery
Diagonal branch
What are the three cardiac veins?
Great
Middle
Small
Where do all the cardiac veins drain into?
Coronary sinus
Then into the right atrium
What nerve provides parasympathetic innervation to the heart?
Vagus nerve
What are the three types of cell found in the heart?
Pacemaker - SA & AV nodes
Purkinje fibres
Muscle cells
What is automaticity?
Even at resting potential some cells have a flux of ions that increase transmembrane potential
Can be enough to trigger further depolarisation
Generates normal heart rhythm