3. Gastrointestinal Disease III: Abomasal Disease
1/91
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
92 Terms
What are the sources of rumen fluid collection for transfaunation?
C
A
O
cannulated cow
animal at slaughter
oral collection (pass a tube)
When should collected rumen fluid be used?
as soon as possible
Can collected rumen fluid be stored? What happens if this occurs?
yes, for ~1 day; decreased microbial viability
True or false: The transfaunation of as little as 1 L of rumen fluid caused significant improvement in the activity of rumen flora in cows with indigestion.
true
Abomsasal displacements are a ________ etiology.
multifactorial
What are some etiologies behind abomasal displacements?
H
P
D
K
hypomotility or atony of the abomasum
possible concurrent diseases (mastitis, metritis, etc)
deficiencies in nutrition or management
ketotic cattle (days 3-5 post calving)
With abomasal displacements, ________ sided disorders are more common than ________ sided disorders, but ________ sided disorders have more complications.
left; right; right
What is the presentation for a displaced abomasum?
C
D
S
D
O
U
T
complete or partial anorexia (tucked up)
dehydrated
scanty’pasty feces
decreased milk production
off-feed (not just grain)
usually ketotic
TPR may be normal or elevated
When do most displaced abomasum occur?
shortly after calving
Displaced abomasums are much more common in ________ than ________ cattle.
dairy; beef
In what age range of cattle are displaced abomasums more common?
older (> 2 years)
What is thought to contribute to displaced abomasums?
stress and nutrition
What are displaced abomasums commonly associated with?
mastitis or metritis
Left displaced abomasum is a disorder of ________ ________, about ____ ________ in ________.
early lactation; <30 days; milk
What are the clinical signs of a left displaced abomasum?
A
M
F
R
appetite decreased
milk production decreased
fecal output decreased
rumination possibly decreased
With a left displaced abomasum, there are variable levels of ________. A ________ can identify gas under pressure in an area of suspicion.
ketosis; ping
How do you diagnose left displaced abomasum?
A
B
P
ausculatation (ping the abdomen)
bloodwork
pH of aspirated fluid (<4.5)
Where should you listen for pings with a left displaced abomasum?
mid thorax from the point of the elbow to the hip
Where can you hear pings from the rumen? What might it indicate?
the rumen gas cap (dorsal area over the last few ribs, paralumbar fossa, and hip); tympany (bloat) or empty (void)
Why else might you hear pings?
F
U
C
free gas in the abdomen (pneumoperitoneum)
uterine gas (physometra)
cecal dilation/displacement
With a left displaced abomasum, what is sequestered in the abomasum?
chloride (HCl)
What are serum chemistry findings associated with displaced abomasum?
H
H
M
P
hypochloremia
hypokalemia (±)
metabolic alkalosis
possible hypophosphatemia
What are the treatments for left displaced abomasum?
P
A
pexy (return the abomasum to normal anatomic location)
address metabolic disorders
What are the types of pexy procedures that can be done in left displaced abomasum?
R
R
L
V
R
L
right abomasopexy
right ometopexy (COMMON)
left ometopexy (more difficult)
ventral paramedian abomasopexy (more secure but more involved)
roll and tack/toggle
laparoscopic correction
What is one of the more common pexy techniques in treating left displaced abomasum?
right ometopexy
A right displaced abomasum can be ________ or ________(________).
simple; complex (volvulus)
A right displaced abomasum is ________ frequent than a left displaced abomasum.
less
What are the clinical signs associated with right displaced abomasum?
S
P
similar to left displaced abomasum
potentially palpable on rectal examination
True or false: A right displaced abomasum is an emergency.
true
What are the differentials for right sided pings?
R
A
C
P
S
R
P
right displaced abomasum
abomasal volvulus
cecal distention (can have a torsion component)
physometra
spiral colon gas
rectal gas (after rectal palpation)
pneumoperitopneum
Where do you hear pings if due to right displaced abomasum?
usually cranial to 8th rib and more cranial than left displaced abomasum ping
What is the initial presentation of right abomasum torsion/volvulus similar to?
right displaced abomasum
On further exam of right abomasum torsion, how are the clinical signs? What are they?
T
D
M
A
P
clinical presentation is more severe
tachycardia (100+ bpm)
decreased/absent rumen motility
minimal to no fecal output
advanced cases can have a ping with an arched dorsal border
possible splashes with succession behind last rib
What are the differential diagnoses when it comes to right abomasum torsion?
I
T
C
intestinal obstruction
torsion of the mesenteric root
cecal torsion
What can help differentiate right abomasum torsion?
rectal palpation
What is seen on clinical pathology with right displaced abomasum?
D
H
H
M
P
P
dehydration/hypovolemia can lead to hemoconcentration
hypochloremia
hypokalemia (±)
metabolic alkalosis
possible hypophosphatemia
paradoxic aciduria
What can develop in right displaced abomasum? Why? What type of prognosis does this cause?
metabolic acidosis; reduced perfusion; poor
What is an important component of the clinical pathology seen with right displaced abomasum? What is it?
paradoxic aciduria; conservation of Na, Cl, and K results in excretion of H+ to maintain electroneutrality
Why do cattle become alkalotic with displaced abomasums?
F
E
D
E
first sequestration of Cl- (little leaves the abomasum to distal GI tract where it is absorbed)
elevated pH and elevated HCO3
dehydration leads to renal retention of Na
excessive H+ ion loss via kidney (paradoxic aciduria)
What is the pathophysiology behind right displaced abomasum leading to torsion/volvulus?
C
D
A
counterclockwise torsion of abomasum and omasum from right to rear
duodenum pulled medially to the body of the omasum
abomasal blood vessels and ventral vagal trunk compromised (torsion near site where duodenum wraps around omasum causing functional pyloric stenosis/failure of abomasal outflow)
Where is the most common twist associated with right displaced abomasum torsion?
between the omasum and the abomasum
What is the treatment for right displaced abomasum/torsion?
S
T
P
N
surgical correction (right sided or ventral paramedian)
treat underlying metabolic deficiencies (hypokalemia, hypochloremia, alkalosis, and dehydration)
possible antibiotics
NSAIDs
What is the prognosis for right displaced abomasum? When is the prognosis poor?
good if simple, guarded with volvulus; if HR > 100 and if dark discoloration, severely distended, necrosis, and thrombosis of the gastric veins
What is the main prevention of displaced abomasum?
reducing forestomach atony caused by high concentrate diets
How can you reduce forestomach atony caused by high concentrate diets?
S
I
M
P
slow introduction of concentrates
increasing fiber length and particle size (check with particle separator)
maintain serum calcium levels
prevent ketosis
True or false: Displaced abomasums are not just seen in dairy cattle, but also in beef calves, sheep, goats, and girraffes.
true
An abdominal fistula is most commonly a ________ from a ________ ________. It can also be a result from ________ ________.
complication; ventral abomasopexy; other surgeries
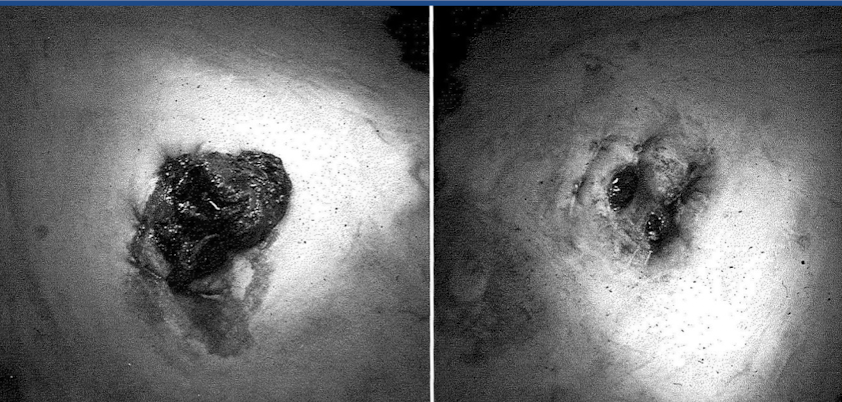
What is this showing?
abdominal fistula
What are abdominal ulcers caused by?
stress and high starch diets
What are the 4 types of abomasal ulcers?
N
N
P
P
non-perforating
non-perforating and bleeding
perforating with localized peritonitis
perforating with diffuse peritonitis
What is a type I ulcer?
erosion or ulcer without hemorrhage
What is a type II ulcer?
hemorrhage
What is a type III ulcer?
perforation with acute localized peritonitis
What is a type IV ulcer?
perforated with acute diffuse peritonitis
What is a type V ulcer?
perforated with peritonitis within the omental bursa
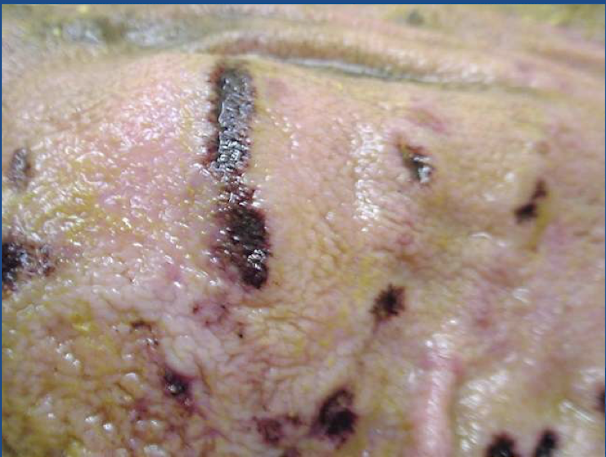
What type of ulcer is this?
type I
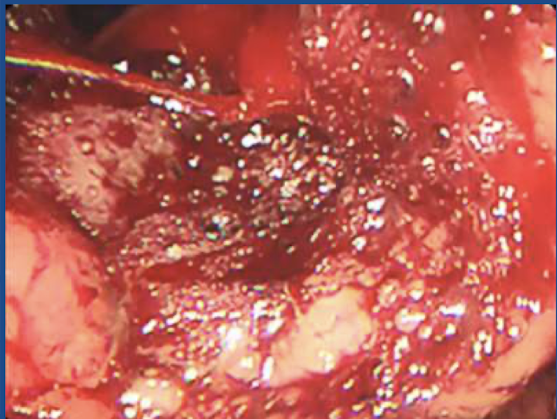
What type of ulcer is this?
type II
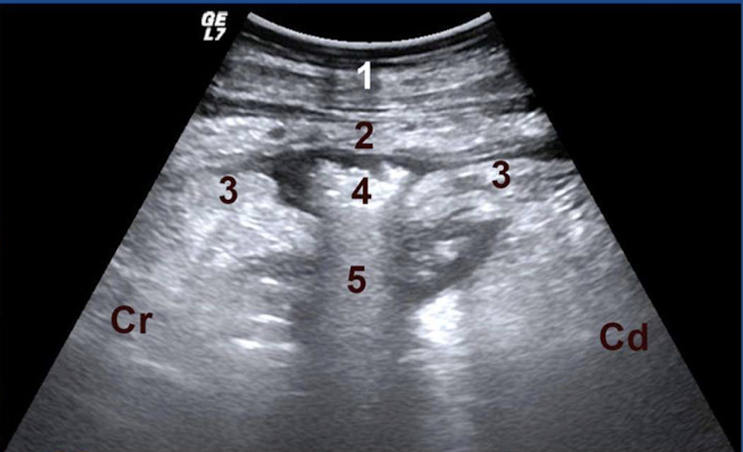
What type of ulcer is this?
type III
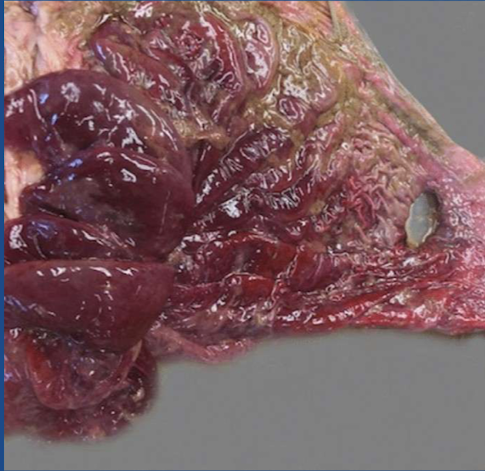
What type of ulcer is this?
type IV
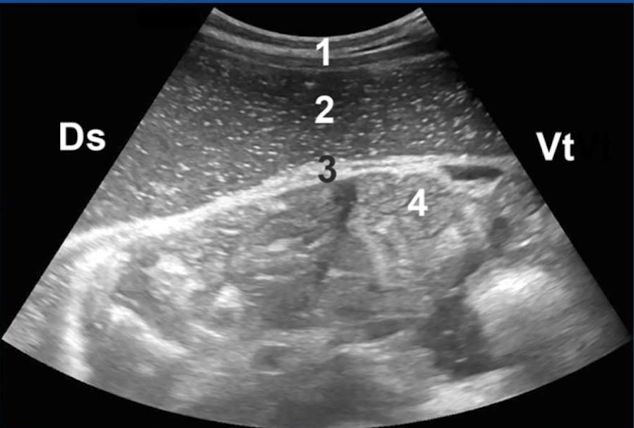
What type of ulcer is this?
type IV
How do you diagnose abomasal ulcers?
P
F
U
A
B
physical exam (bruxxism)
fecal occult blood (looking for digested blood in the feces)
ultrasound
abdominocentesis
bloodwork
What are the clinical signs associated with abomasal ulcers?
V
I
B
D
S
P
vague
inappetence
bruxxism
dietary preference (will sort out forage instead of grain)
salivation (excessive)
poor thrift
What are the causes of abomasal ulcers in calves?
A
B
N
B
S
N
abrasion theory
bacterial and fungal agents
NSAIDs
BVD or IBR
stress
nutritional deficiencies (copper and selenium-vitamin E)
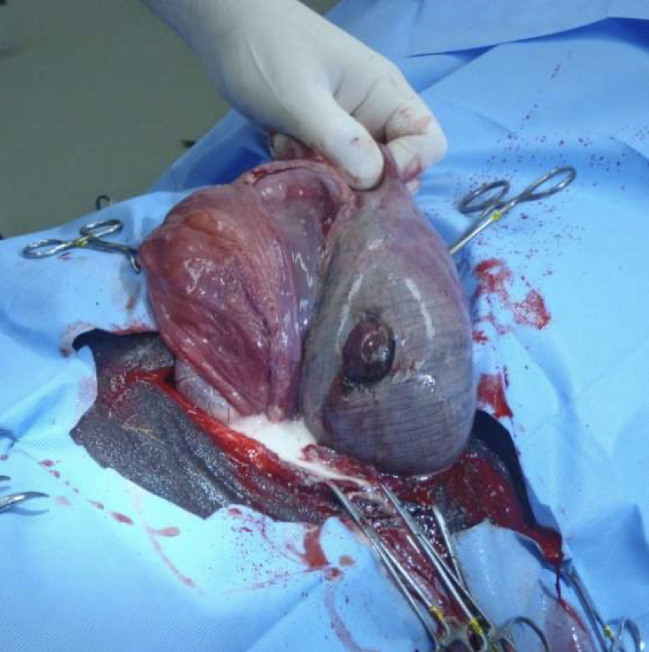
What is this showing?
abomasal ulcer
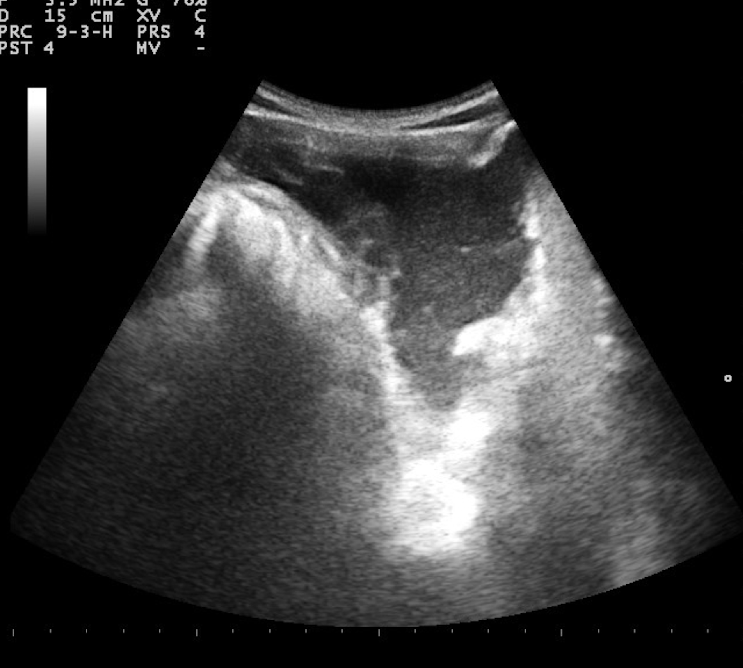
What is this showing?
abomasal ulcer
What is the treatment for abomasal ulcers?
R
B
A
M
remove starch (rapidly fermentable and ground carbohydrates → grain)
blood transfusion possible
antibiotics possible
mucosal protectants
What are the several different classes of gastroprotectant therapies for ruminants?
C
S
A
S
H
P
coating agents
sucralfate
alkalinizing agents
synthetic prostaglandins
H2 antagonists
proton pump inhibitors
There are limited gastroprotectant therapies for ________ ruminants.
adult
What are local agent gastroprotectants?
B
S
A
bismuth subsalicylate
sucralfate
aloe vera juice
True or false: Bismuth subsalicylate is GRAS and needs frequent administration. Sucralfate has multiple mechanisms of action and is deactivated by rumen flora. Aloe vera juice is described in organic references and comparative human data.
true
What group of gastroprotectants are effective acid suppressing agents? How do they work?
H2 antagonists; work far upstream
What are examples of H2 antagonists?
F
R
famotidine
ranitidine
How is the efficacy of H2 antagonists described in ruminants?
limited to no oral efficacy in ruminants
What are the adverse effects associated with H2 antagonists?
E
D
electrolyte disorders
drug interactions
What is the most effective group of acid suppressors? How do they work?
proton pump inhibitors; directly on ATPase pump
What are examples of proton pump inhibitors?
O
P
omeprazole
pantoprazole
How is the efficacy of proton pump inhibitors described in ruminants?
limited to no oral efficacy in mature ruminants
What are the adverse effects of proton pump inhibitors in people?
N
E
A
H
neutropenia
electrolyte disorders
anaphylaxis
hepatotoxicity
When it comes to abomasal ulcers, do not forget about ________.
neoplasia
Abomasal impactions are usually a ________ cow problem.
beef
Surgery is usually ________ in abomasal impactions.
unrewarding
What is the treatment for abomasal impactions? What are specifics?
L
D
F
medical management
laxatives
detergents (DSS)
fluids
True or false: Abomasal impactions cab be more than just feed. They can be due to gravel, phytobezars, trochobezats, placenta, and sand.
true
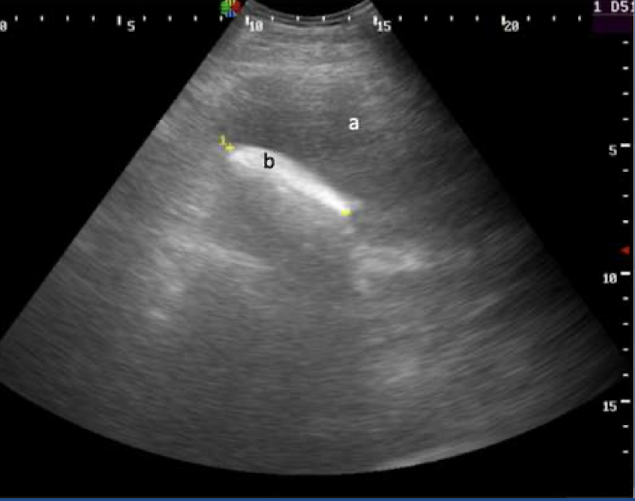
What is this showing?
abomasal impaction
What is a common neoplasia in cattle? What is it due to?
lymphoma; BLV
What does a BLV status indicate?
only indicates infection with the virus and does not mean they will have tumors
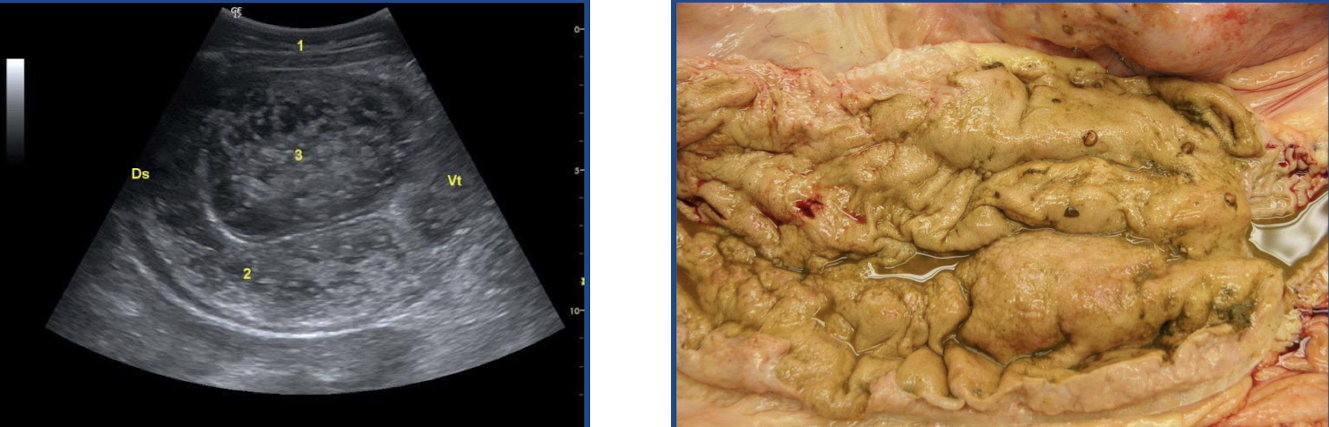
What is this showing?
lymphoma
Abomasal emptying disease is a recognized disease of what species only?
Suffolk sheep
Suffolk sheep can suffer from what disease?
abomasal emptying disease
What is the cause of abomasal emptying disease?
unknown but suspect dysautonomia
What are the clinical signs associated with abomasal emptying disease?
A
W
R
anorexia
wasting
right abdominal distention
Treatment for abomasal emptying disease is ________.
unrewarding