Abdomen: organs
1/197
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
198 Terms
2 incisors, 1 canine, 2 molars
Deciduous set of teeth includes
2 incisors, 1 canine, 2 premolars, 3 molars (3rd is the wisdom tooth)
Deciduous set of teeth are replaced by adult teeth containing
Enamel
Cementin
Dentin
-acellular, mineralized tissues that are fairly resistant
Specialized minerals that contribute to the teeth
Outer layer of crown
Enamel
Lines the alveolar bone (tooth sockets, aka ligament for the tooth)
Cementum
Found deep to enamel and cementum. Makes up bulk of tooth.
Dentin
Occur when prolonged exposure to bacterial enzymes demineralize the enamel, cementum, and dentin, creating carries
Typically, the gingiva (gums) cover the tooth below the crown. If the gingiva pulls away it exposes the dentin, which is softer than the enamel and is eroded more quickly
Cavities
Skeletal
Keratinized stratified squamous
The tongue consists of ____ muscles covered by ____ epithelium that resists abrasion during chewing
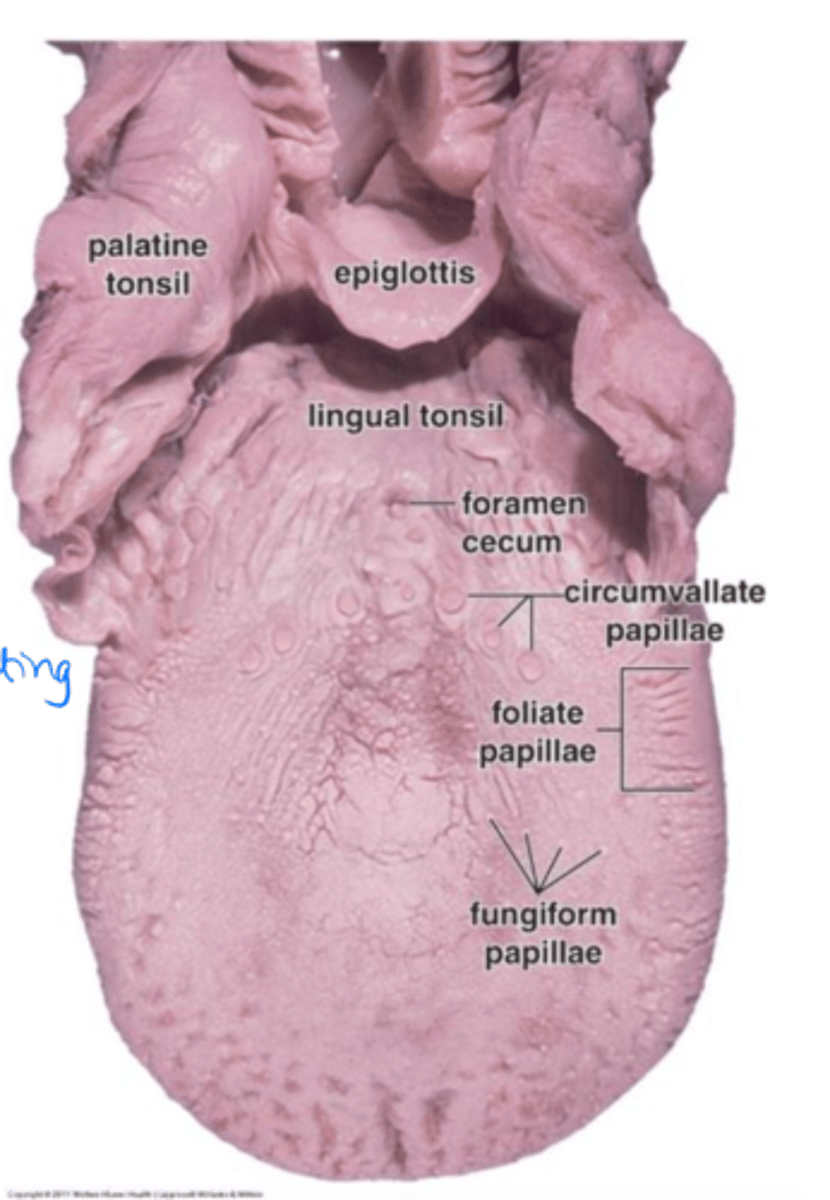
Specialized structures on the tongue surface
-filiform
-fungiform
-circumvalate
-foliate
Papillae
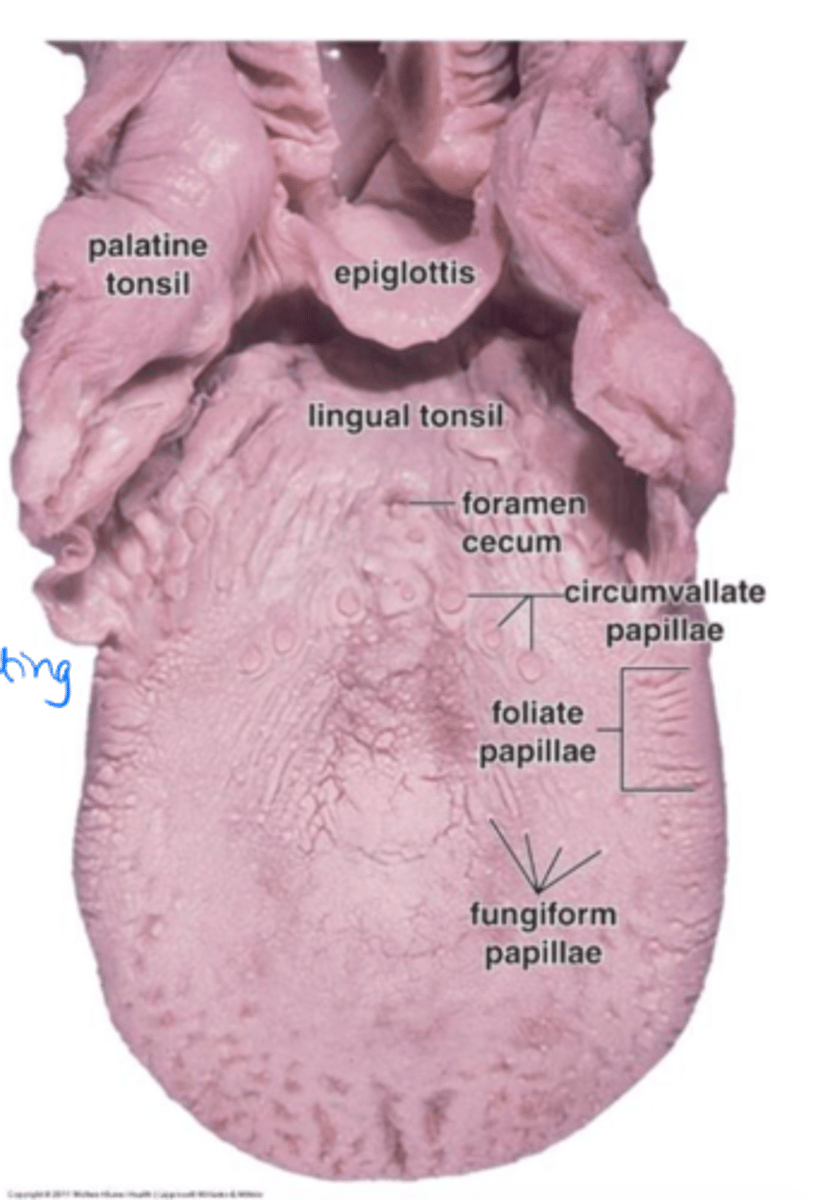
Sharp extensions that cover most of the tongue. NO TASTE BUDS
Filiform papillae
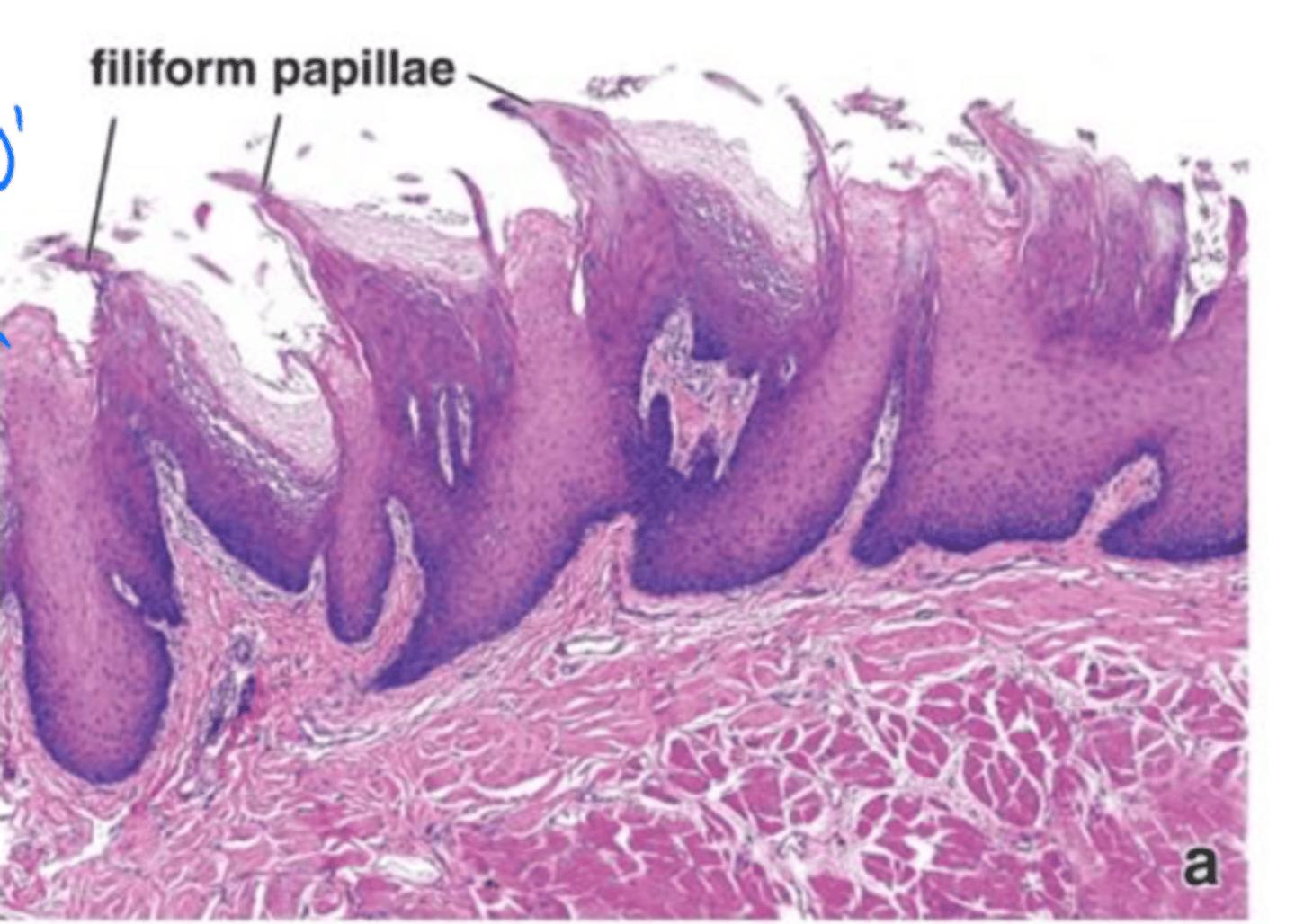
Little pale dots on the surface of the tongue that have taste buds.
Fungiform papillae
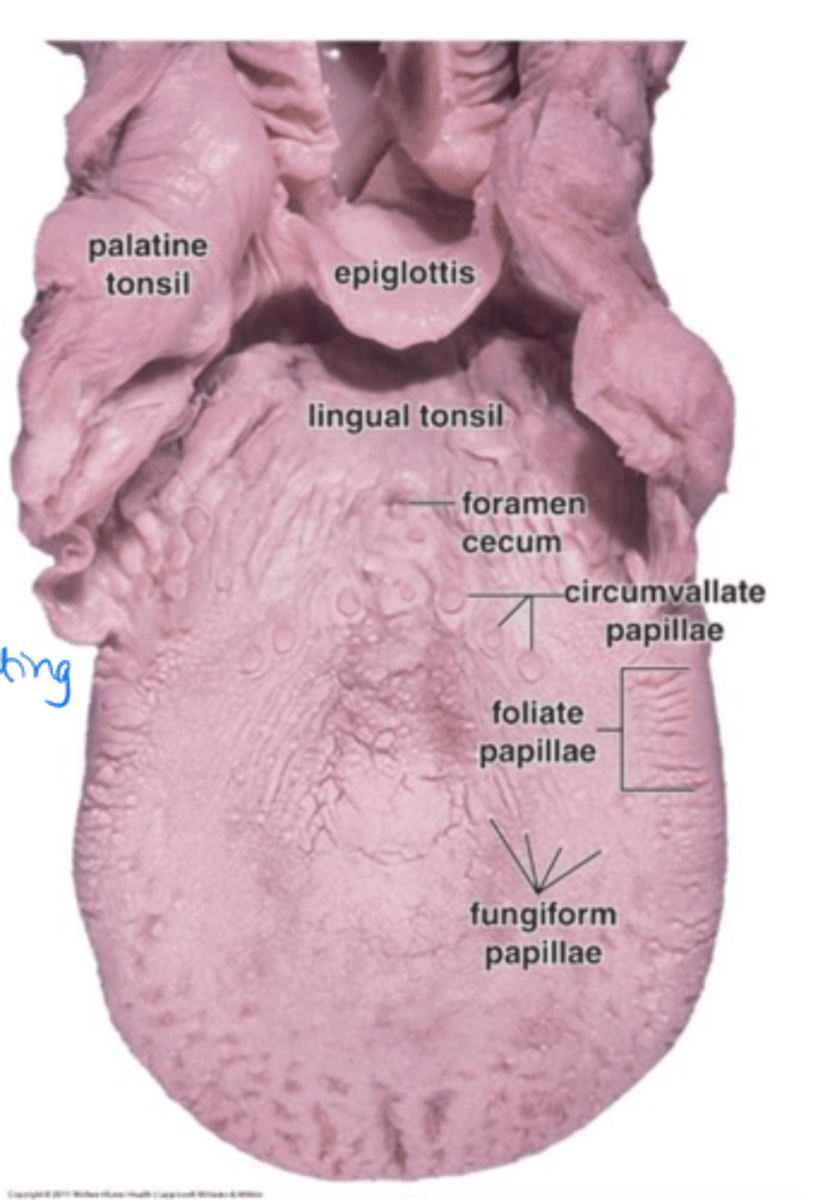
Large circular papillae near the posterior 1/3 of tongue. Have taste buds and secretory glands.
Much larger than other papillae, marks where the anterior and posterior tongue meets
Circumvalate papillae
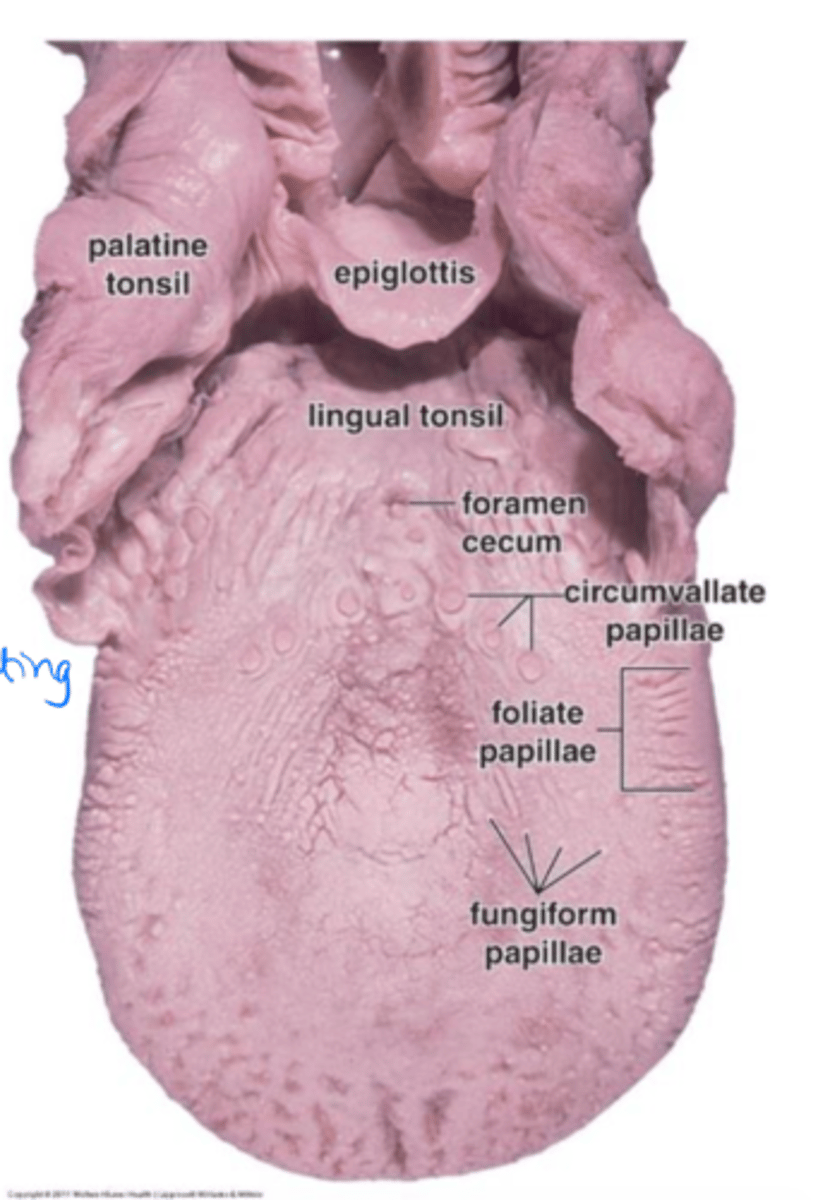
Longitudinal folds on the lateral aspect of the tongue. Have taste buds and secretory glands.
Foliate papillae
Have sensory cells that contact the outside environment through a small pore.
Sensory cells turn over after ~10 days. Nerve bundles are often visible coming from the taste buds
Taste buds
Epithelium
1
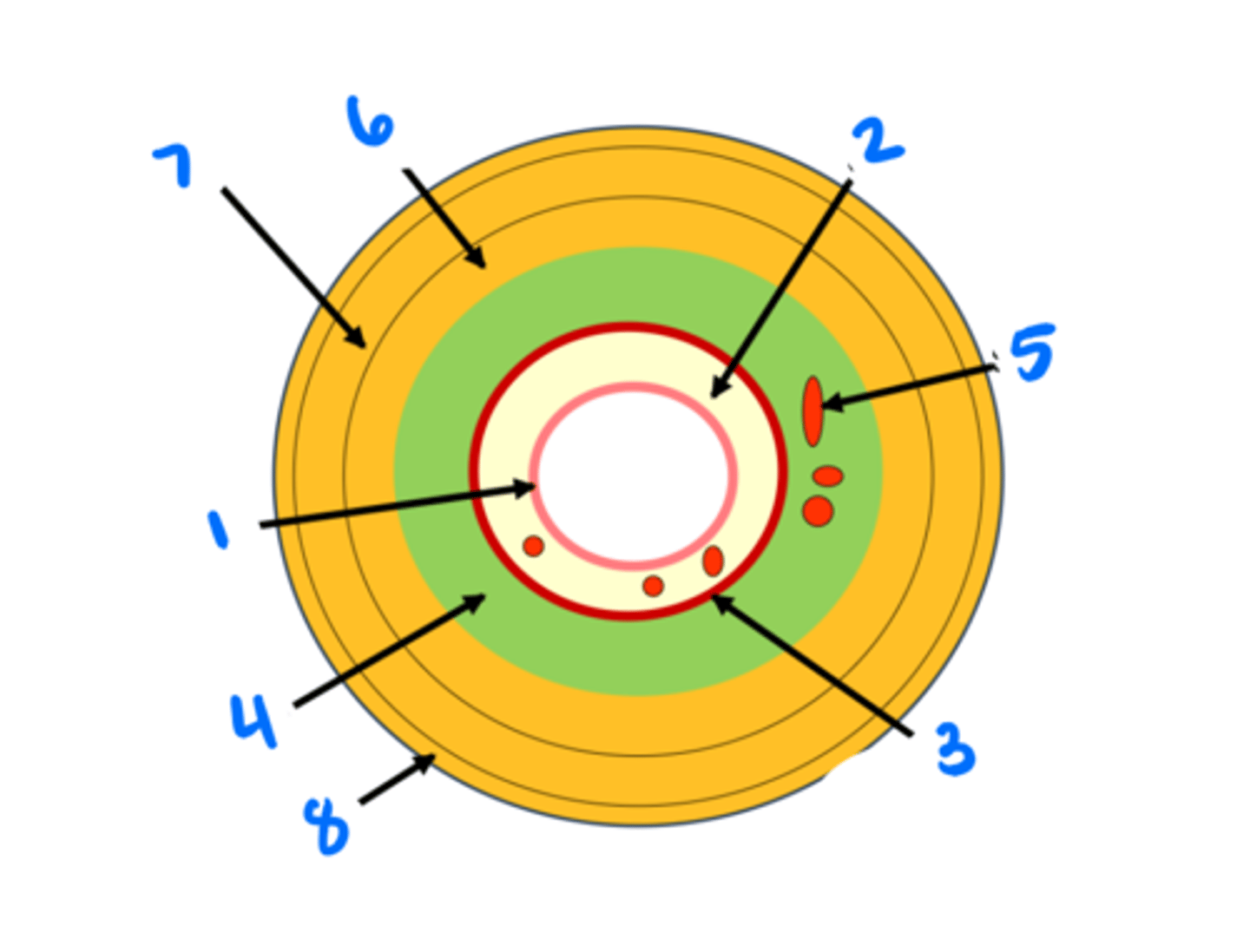
Lamina propria
2
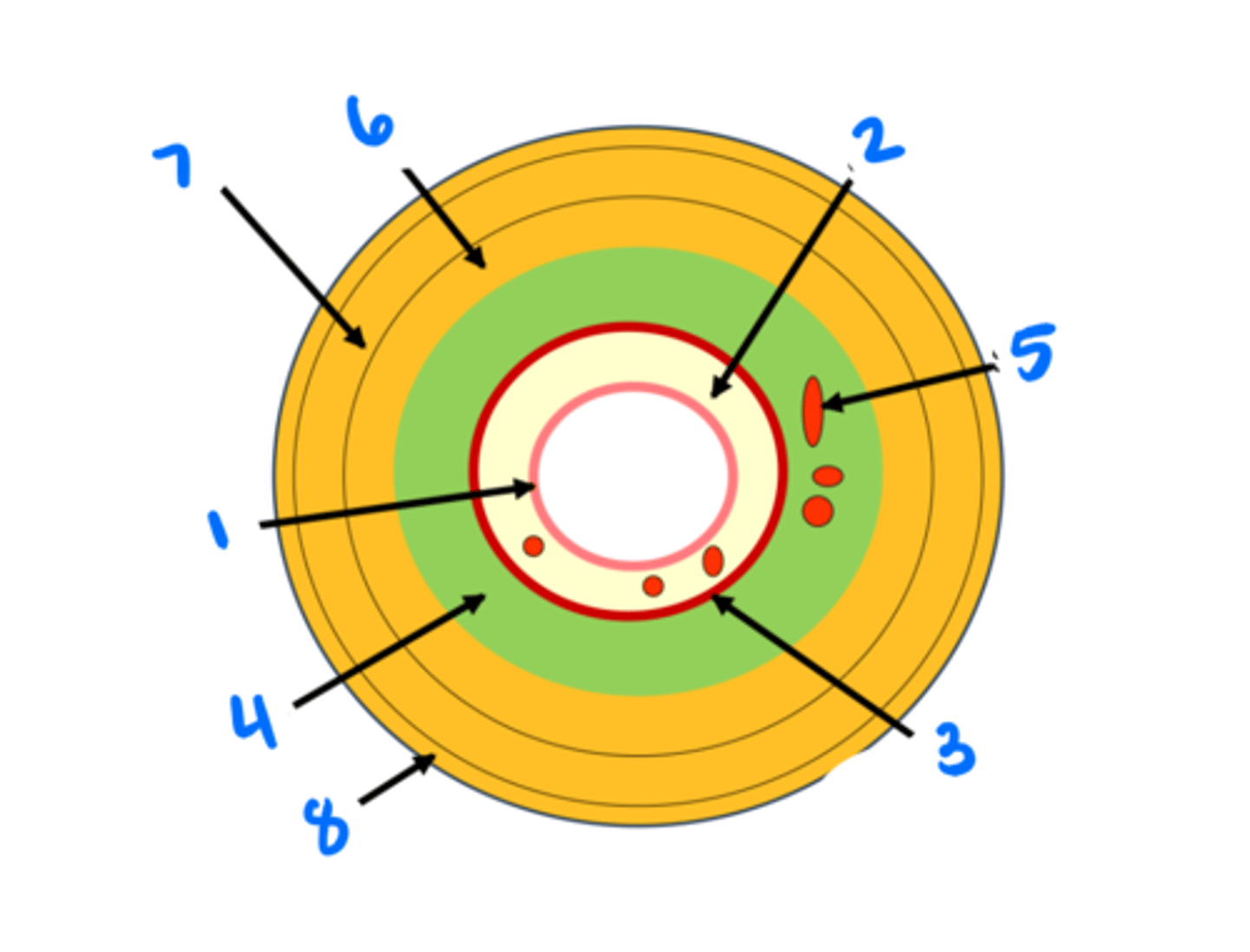
Muscularis mucosae
3
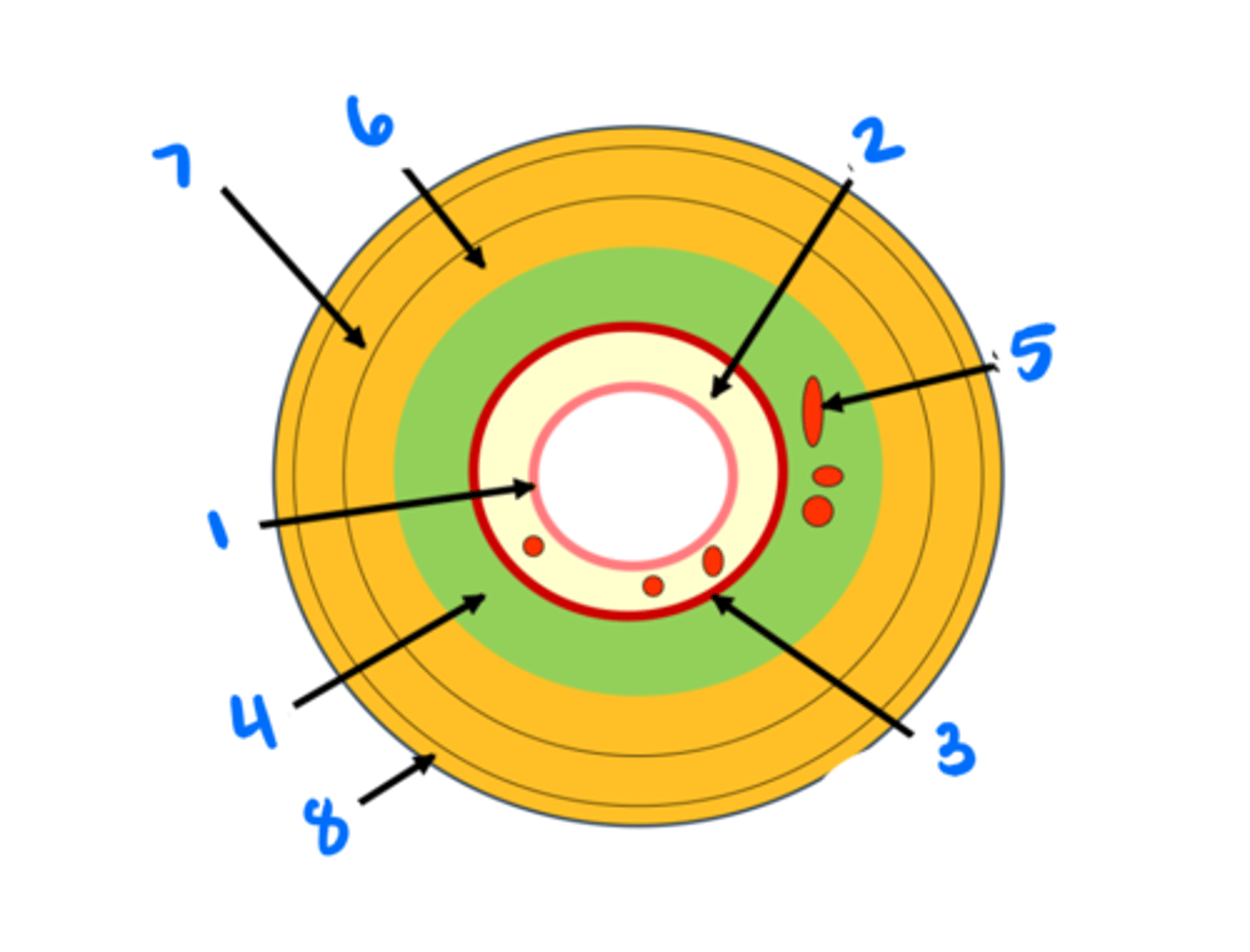
Submucosa
4
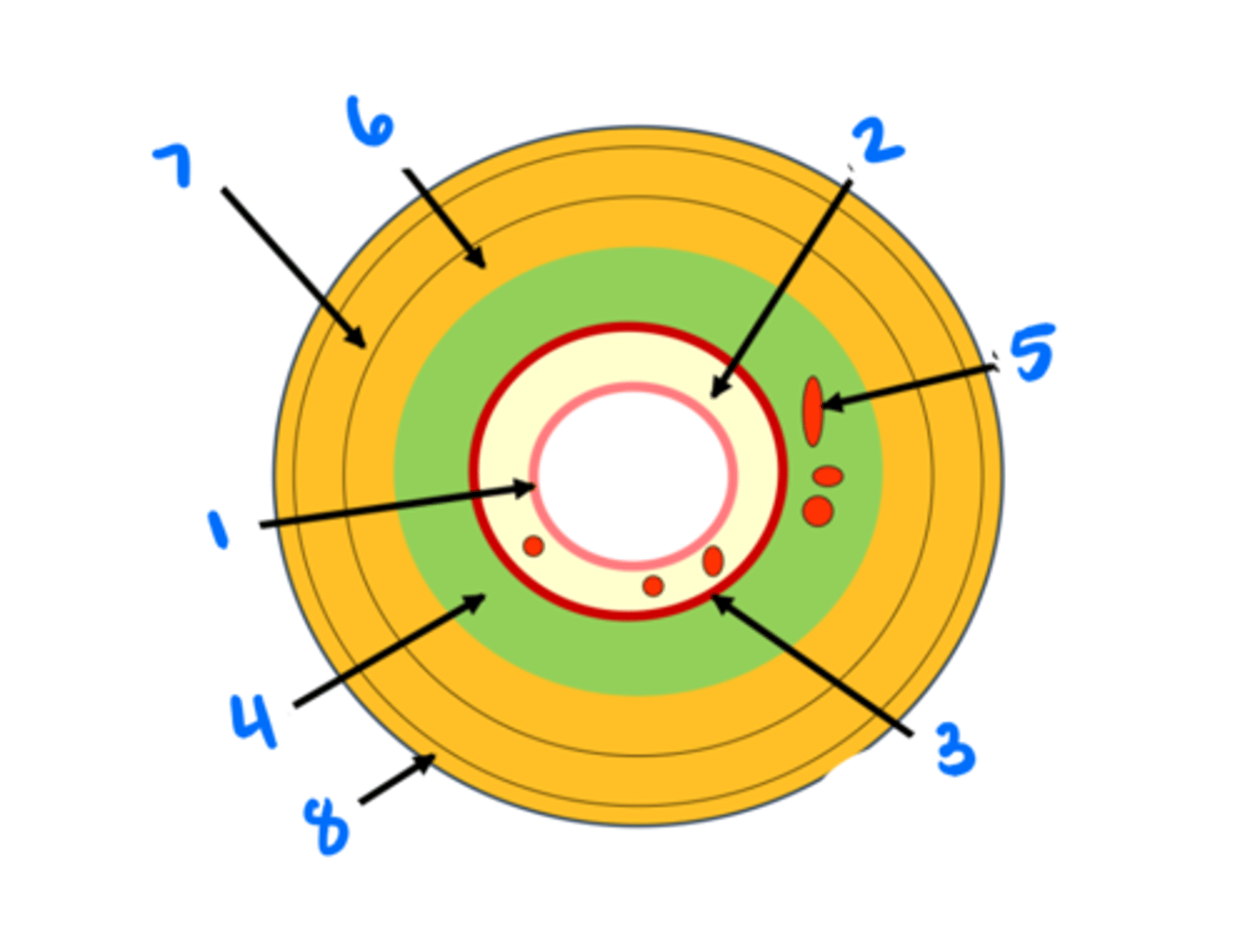
Submucosal glands
5
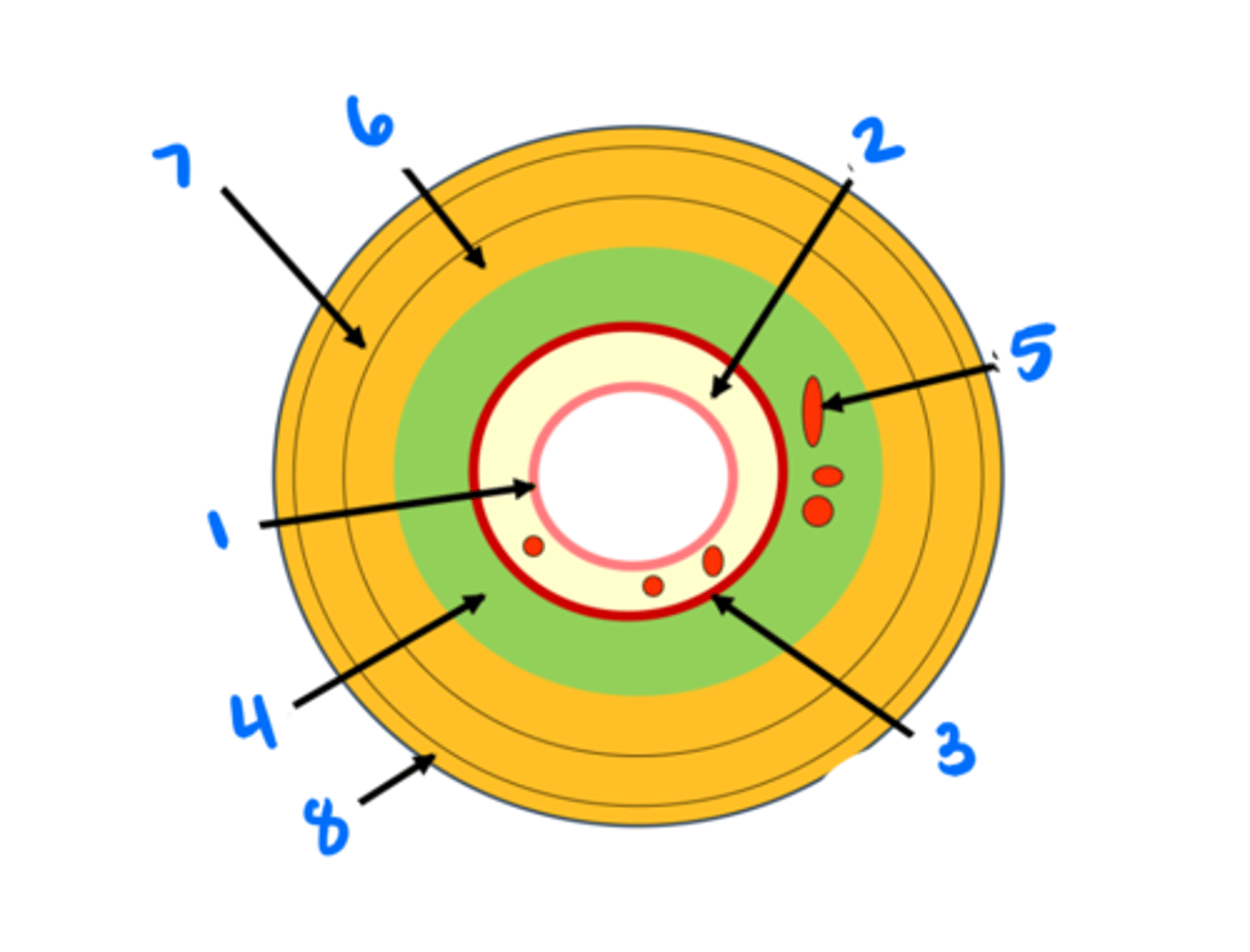
Circular muscularis externa
6
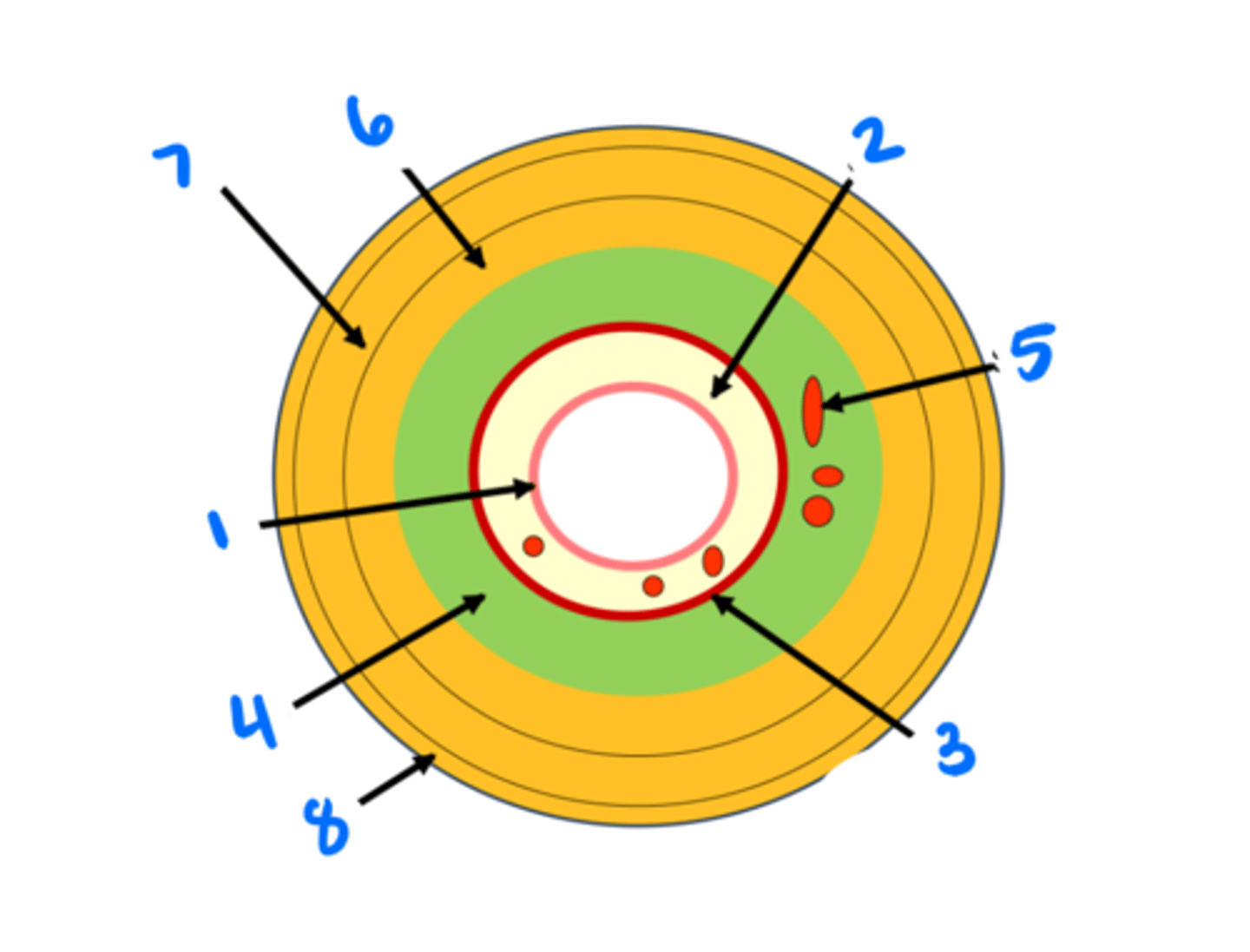
Longitudinal muscularis externa
7
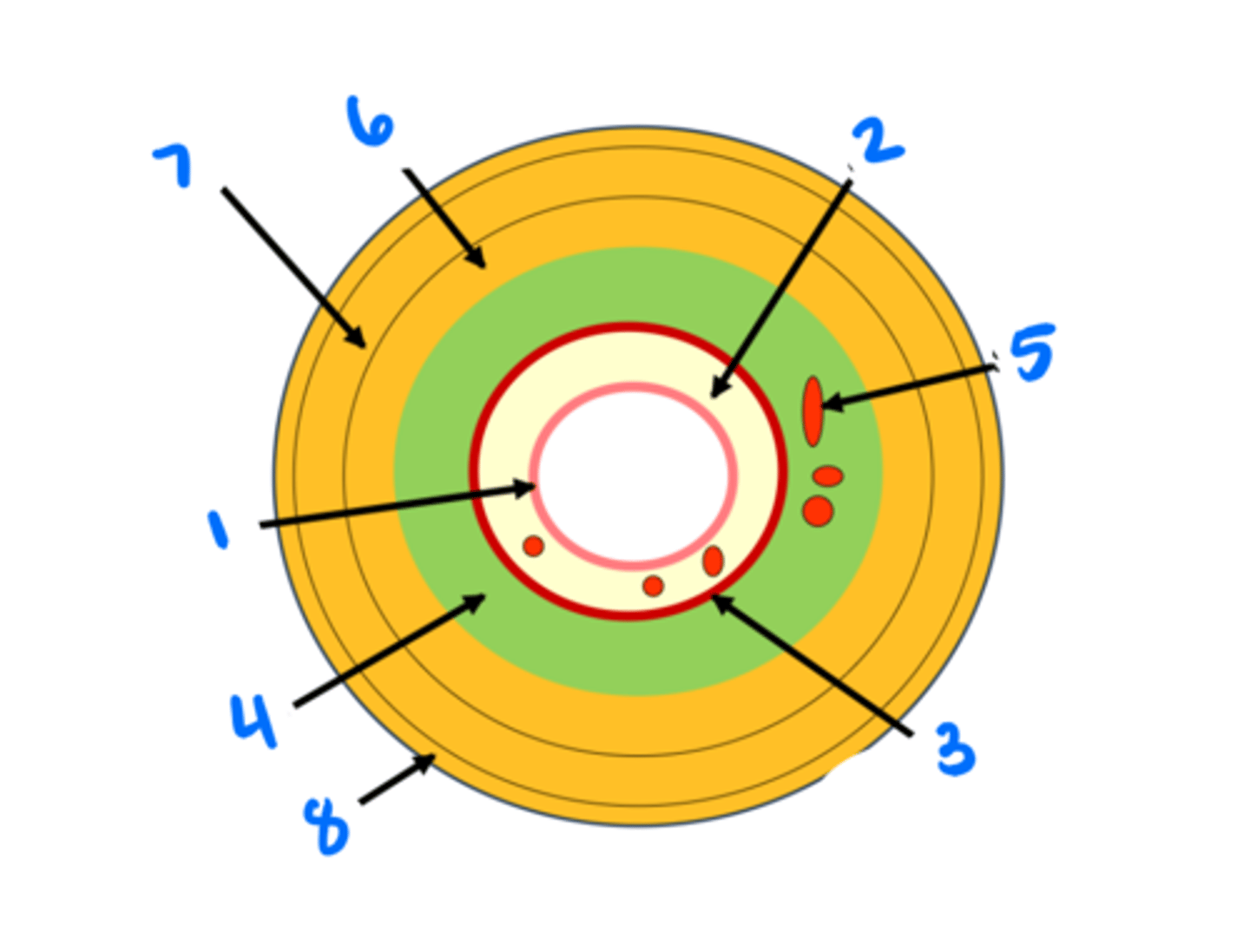
Adventitia/serosa
8
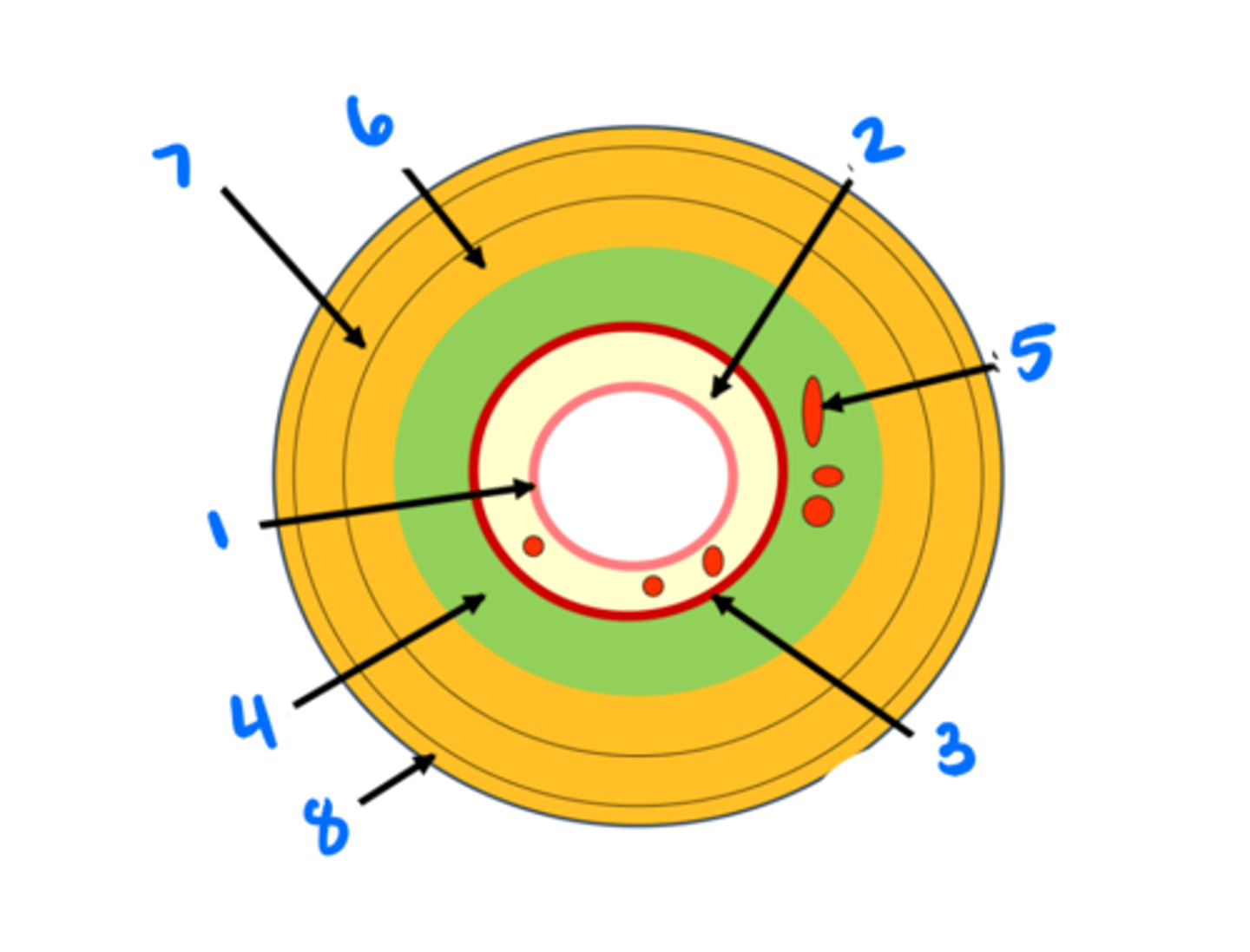
Portion of gut tube in contact with the external environment (innermost layer of generic gut tube).
-Extracts nutrients from food
-protects the body from pathogens.
Mucosa
epithelium (1) - stratified squamous or simple columnar (absorbs food and moves it to LP)
lamina propria (2) - loose connective tissue (WBC screen for pathogens here)
muscularis mucosae (3) - smooth muscle (does some work, but not as much as muscularis externa)
3 layers of the mucosa
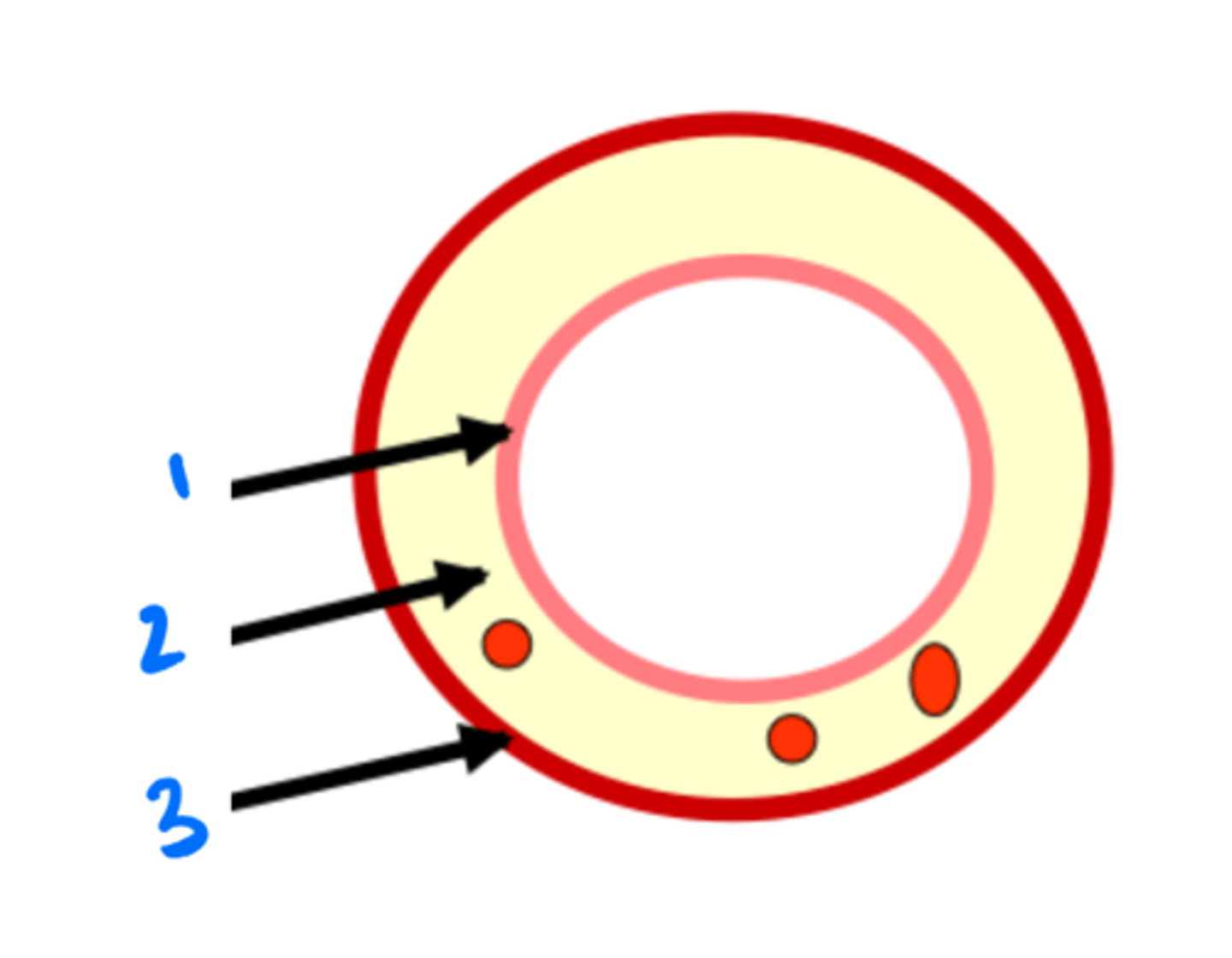
Portion of the gut tube superficial to the muscularis mucosae. Contains:
-large vessels (arteries, veins, lymph)
-submucosal ganglia: nerve cells
-submucosal glands
-large lymph nodules.
Submucosa
Contains two layers of smooth muscle that move contents in the gut tube. Most important for doing work
-inner circular layer
-myenteric ganglia: nerve cells
-outer longitudinal layer.
Muscularis externa
Outermost layer of gut tube.
Adventitia is loose connective tissue that anchors gut to nearby tissues.
Serosa is thin connective tissue with simple squamous epithelium that secretes fluid to lubricate the gut tube and other structures in the abdominopelvic cavity, which keeps bowel mobile and prevents irritation that could lead to adhesions
Adventitia/serosa
esophagus, upper esophageal sphincter
Bolus of food passes from the pharynx to the _____ through the ____ which keeps it closed.
Mucosa: nonkeratinized startified squamous epithelium, lamina propria, muscularis mucosa
Submucosa
Muscularis externa: inner circular layer, outer longitudinal layer, transition from skeletal (upper 1/3) to smooth muscle (lower 1/3)
Layers of the esophagus
lower esophageal sphincter
keep acidic gastric contents out of the esophagus
gastroesophageal reflux disease (GERD).
After the bolus passes through the esophagus it reaches the _______, which functions to ______. Dysfunction can lead to ______
The lower esophageal sphincter is compressed by muscles of the diaphragm
As the esophagus enters the abdomen...
There is a stark shift between stratified squamous epithelium of the esophagus and the simple columnar (but highly folded) epithelium of the stomach
Gastroesophageal junction
Due to prolonged GERD, causes metaplasia of the esophagus: mucosa of the esophagus takes on the appearance and function of the cardiac region of the stomach (esophagus becomes columnar epi).
It also leads to increased risk of adenocarcinoma, a type of esophageal cancer
Barrett's esophagus
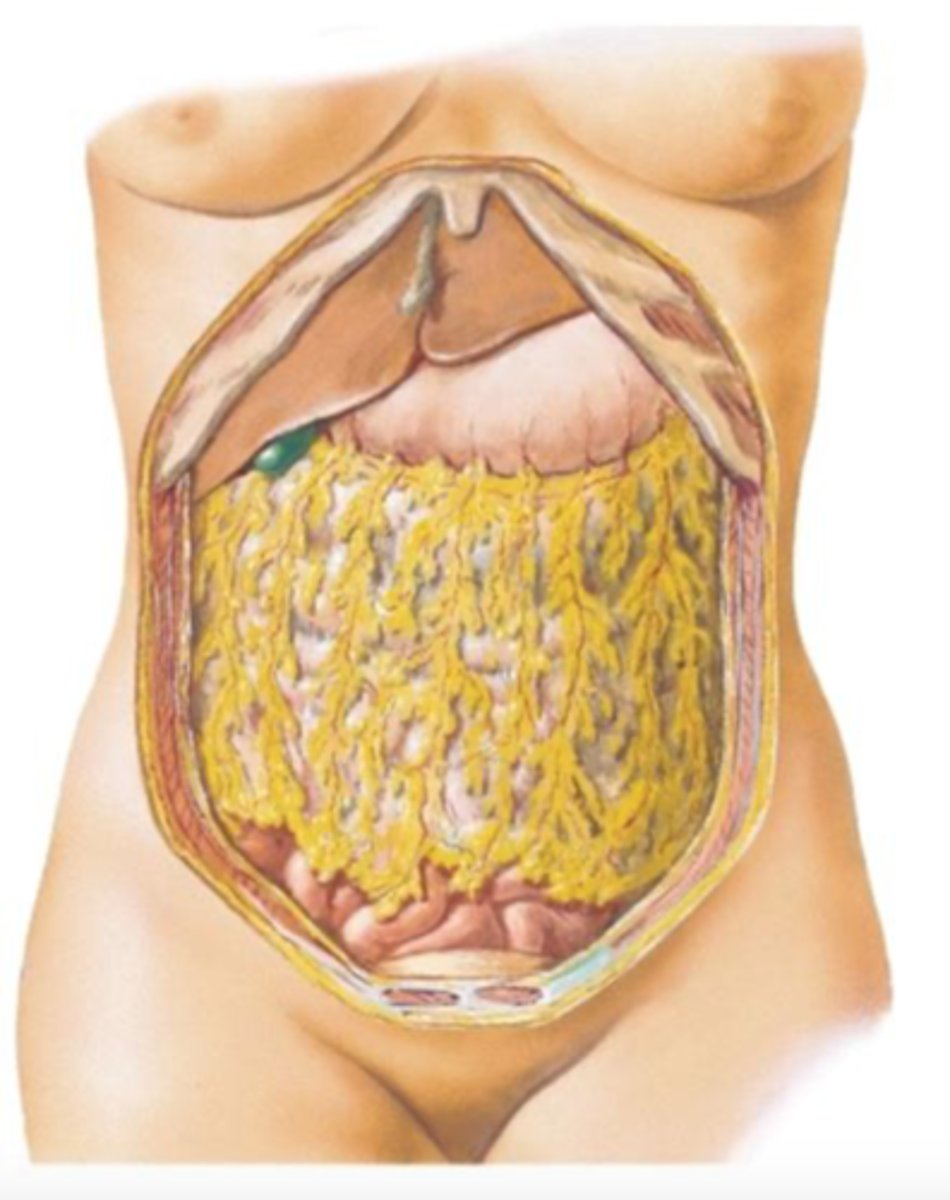
part of the peritoneum attached to the greater curvature of the stomach and down covering the intestines
mobile and will migrate around the abdomen to wall off areas of inflammation or infection. It will sometimes leave adhesions between itself and the abdominal wall
greater omentum
muscularis externa, hydrochloric acid
The stomach digests food mechanically using the ______ and chemically with ______.
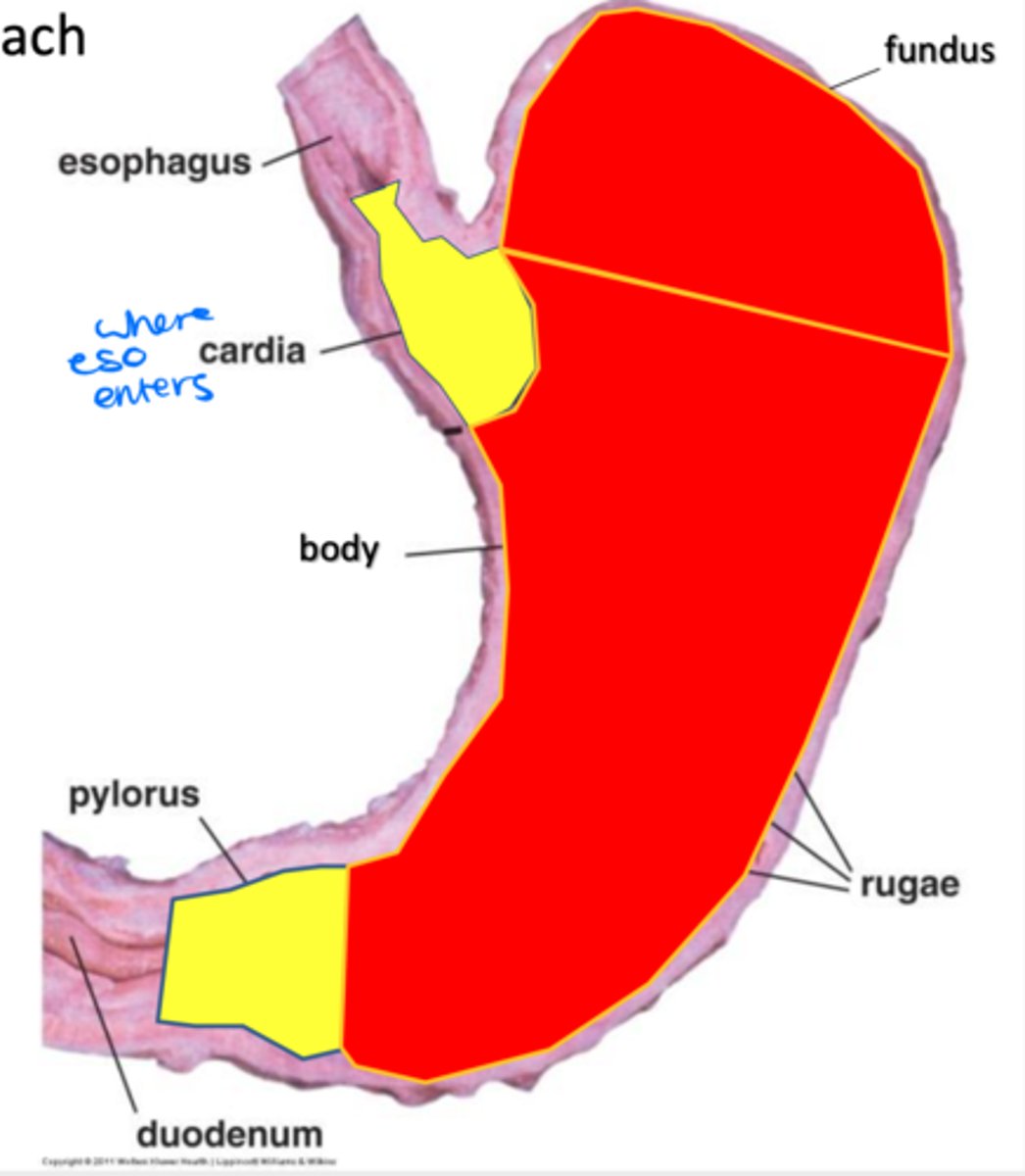
Folds in the stomach wall that facilitate it's expansion
Rugae
Cardia, fundus, body, pyloris
Four regions of the stomach
Parts of the stomach that create mucus to protect the stomach from the low pH
Cardia and pyloris function
Digestive
Fundus and body function
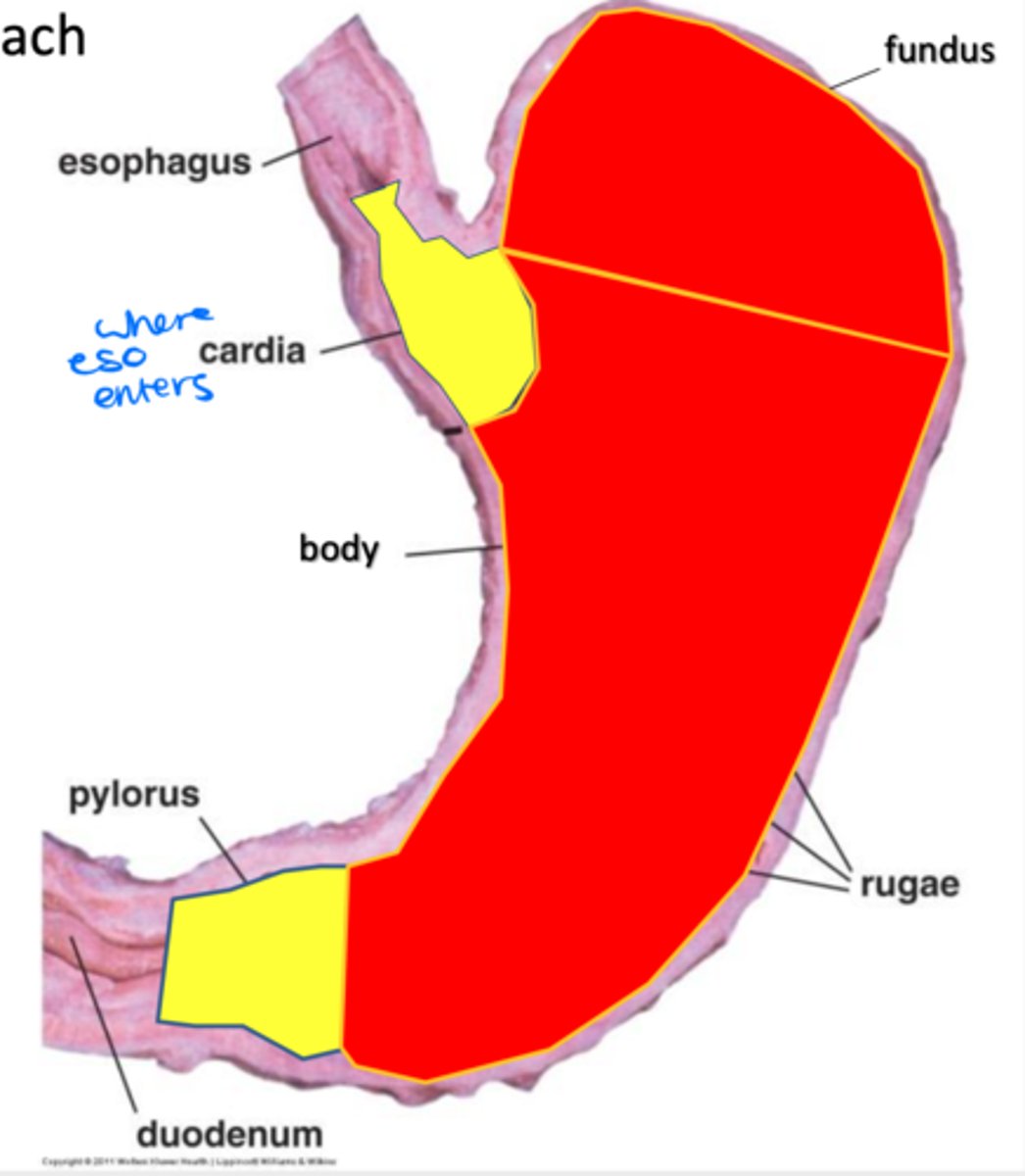
Outermost protective layer of the stomach, covering 3 layers of smooth muscle
-outermost is longitudinal (greater and lesser curvature)
-middle is circular
-innermost is oblique
Tunica serosa
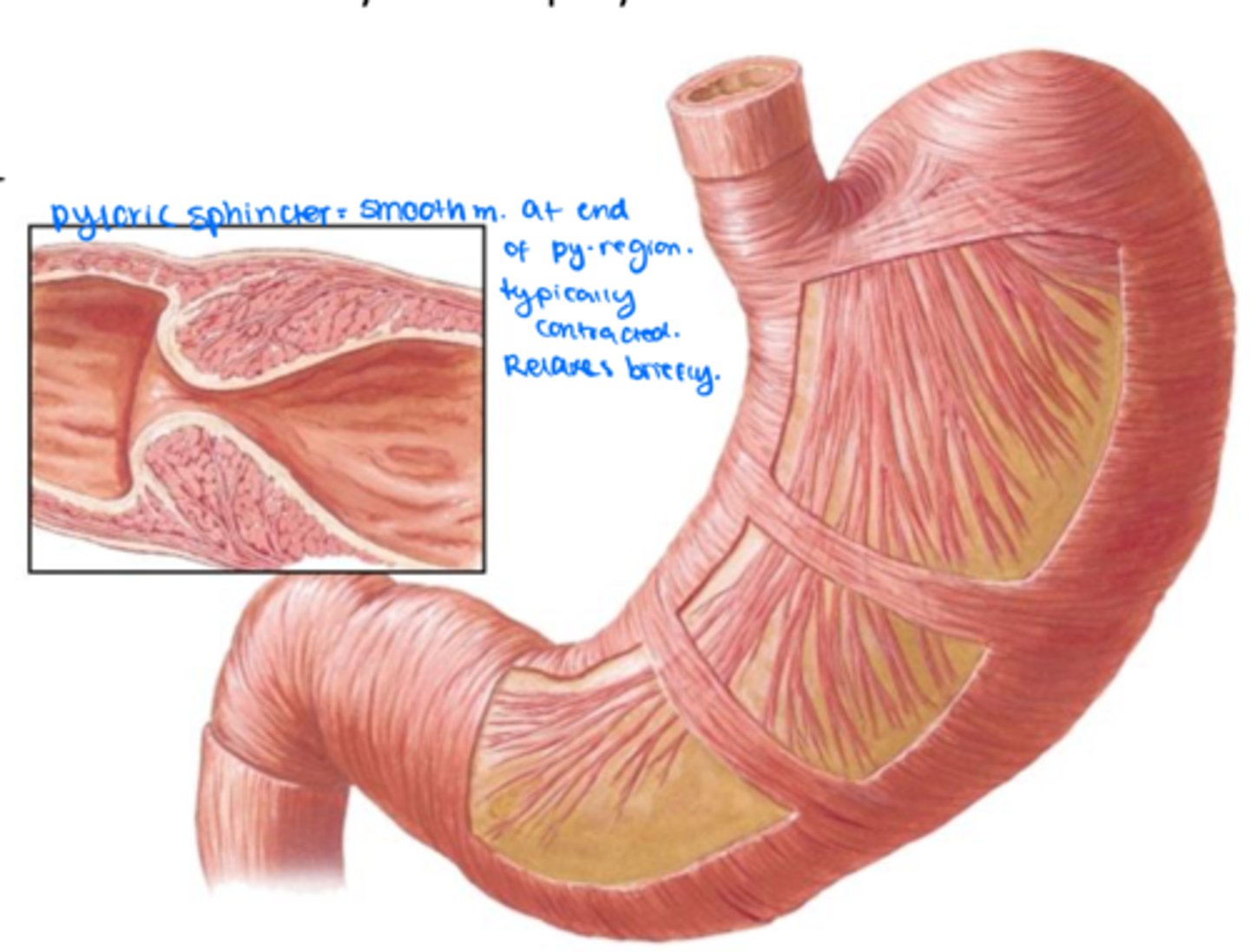
circular, pyloric sphincter
The middle layer of the stomach is ______ and thickens considerably at the pyloric region to form the ______ which regulates release of food into the duodenum.
Chief cells
Parietal cells
Cells found only in the stomach (in body/fundus)
mucous-producing goblet cells surrounding gastric pits to protect the stomach
Cells found in the simple columnar epithelium of the cardia and pylorus
Cells of the stomach that produce HCl to make the stomach acidic. They also release intrinsic factor which helps absorb Vitamin B12 (in ilium) - assist in digestion
Parietal cells
Cells of the stomach that release precursors of digestive enzymes pepsin, renin, and lipase.
Chief cells
Caused by increased secretion of HCl that erodes the stomach's mucosa, submucosa, and even muscularis externa. Causes:
-over production of gastrin causing excessive HCl secretion
-long term NSAID use
-infection with H. pylori which can survive acidic environment and destroy epithelial lining
Gastric ulcers
-raises the pH of food as it exits the pyloric sphincter.
-adds bile from the liver and digestive enzymes from the pancreas
-absorbs nutrients.
Roughly 6-7 meters long.
Function of small intestine
Duodenum (20-25cm)
jejunum (2/5 of length)
ileum (3/5 of length)
3 parts of the small intestine
Surface area
Macroscopic Plicae circularis (circular folds)
Microscopic villi
Super microscopic microvilli
To insure that nutrients are absorbed efficiently, there is a tremendous increase of _____ in the small intestine via _____, _____, and ______
Folds in the lumen of the small intestine
Pilcae circularis
Folds of mucosa with a lymphatic duct in the core called a lacteal
On the pilcae circularis
Villi
Seen on the surface of the actual absorptive cells of the small intestine
Microvilli
A disease in which the body mounts an immune response to a protein in gluten. Inflammation damages villi leading to blunt, shortened villi with a large infiltration of lymphocytes in the mucosa. Can lead to malabsorption.
Celiac disease
First part of the small intestine that receives gastric contents and neutralizes their acidity and also controls the release of pancreatic enzymes and bile into the digestive tract.
Function of duodenum
Part of the submucosa in the duodenum that secretes mucus and bicarbonate to raise the pH to protect the remaining digestive tract and activate pancreatic enzymes.
Duodenal glands (Brunner's glands)
pyloric
duodenum
The _____ region of the stomach releases gastric content into the first part of the small intestine, the _____.
superior, descending, inferior, ascending
4 sections of the duodenum
Portion of the duodenum that receives gastric content (blue)
Superior duodenum
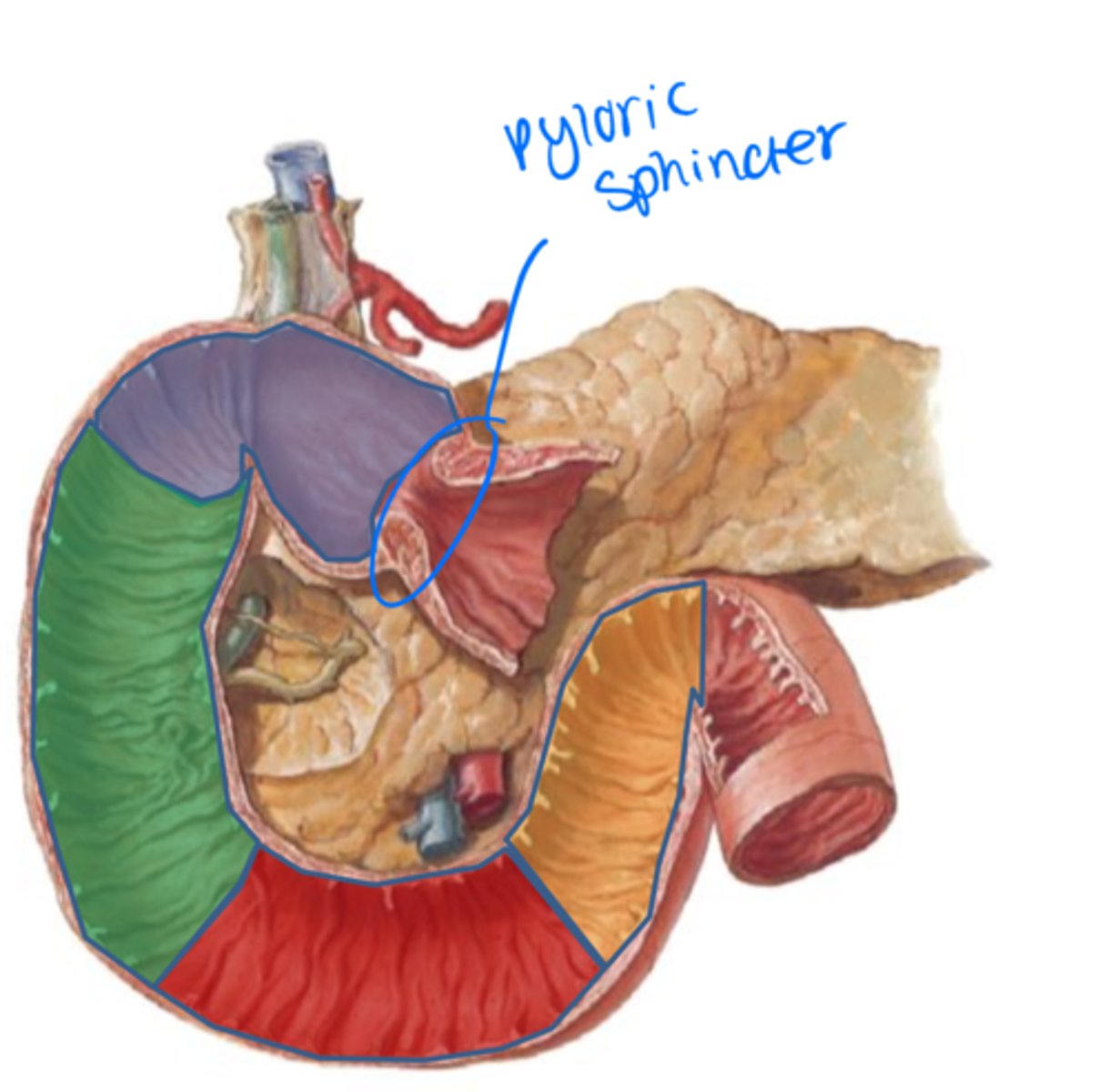
Portion of the duodenum that receives common bile duct from the liver and pancreas - hepatopancreatic ampulla!! (green)
Descending duodenum
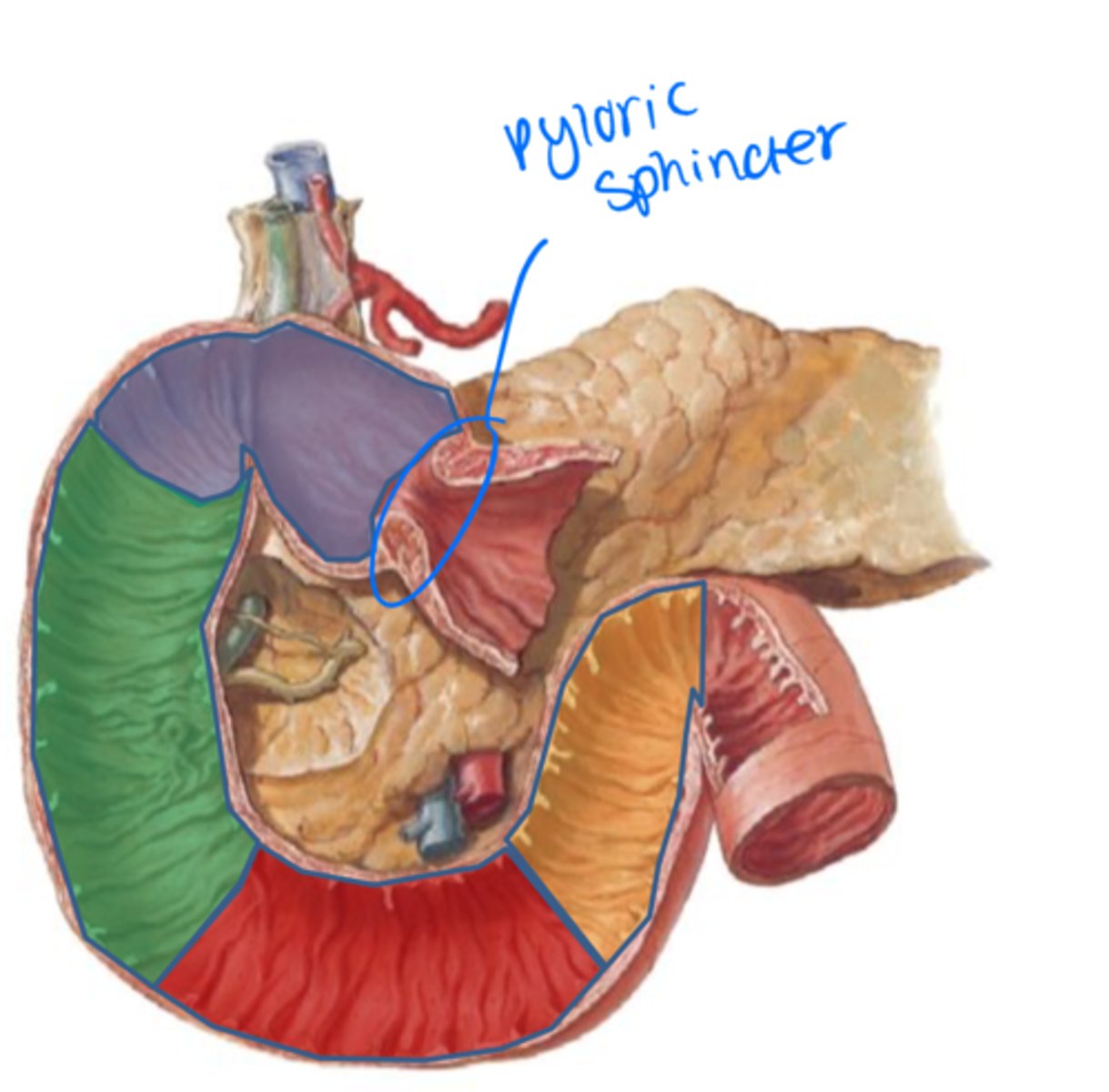
Portion of the duodenum that passes posterior to the superior mesenteric vessels (red)
Inferior duodenum
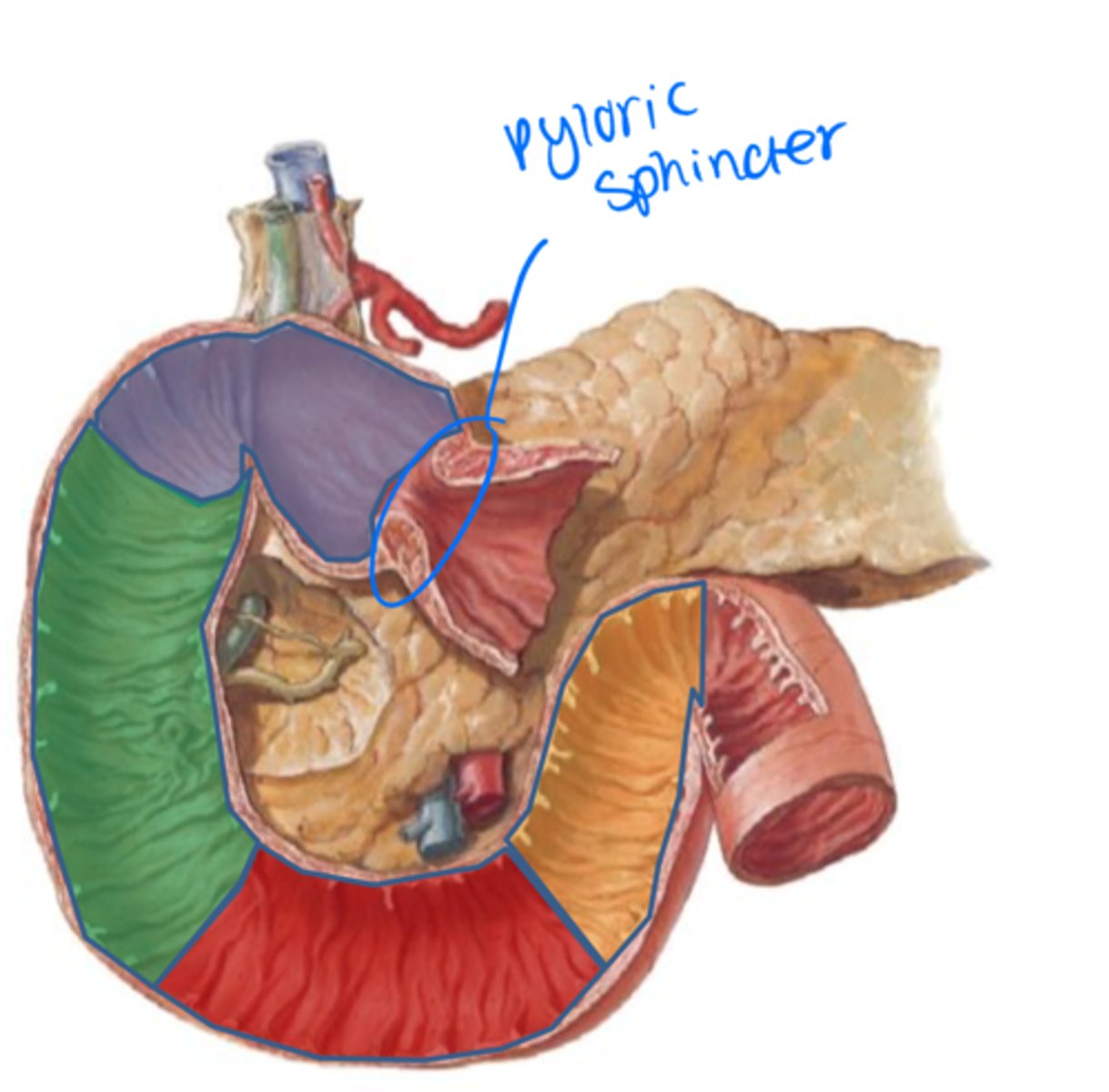
Portion of the duodenum anchored by suspensory ligament and becomes the jejunum there after (yellow)
Ascending duodenum
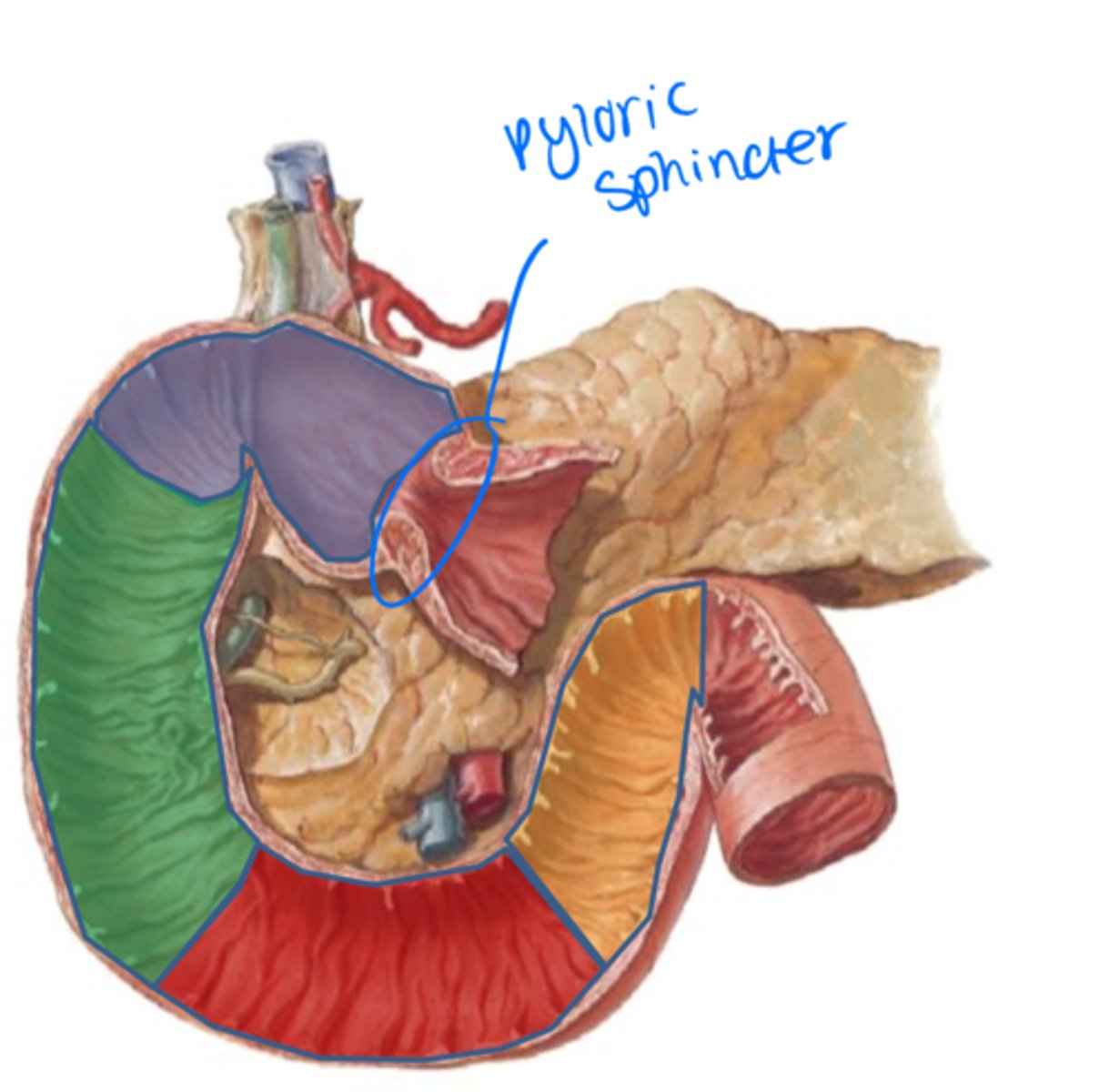
Extension of the right diaphragmatic crura and is and important surgical landmark. Thereafter continues as the jejunum.
suspensory ligament (ligament of the duodenum/Trietz)
Jejunum
1
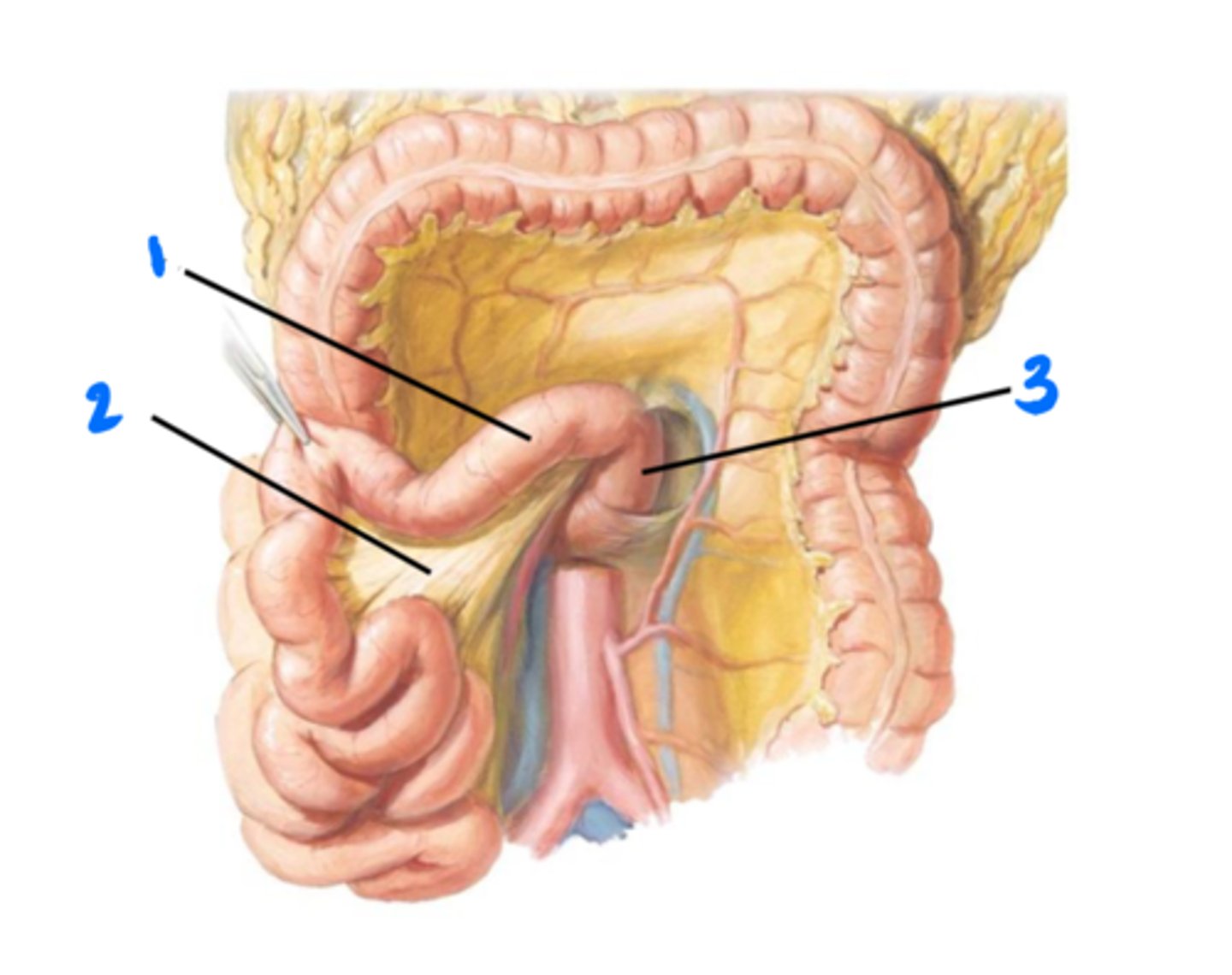
Mesentery of small intestine
2
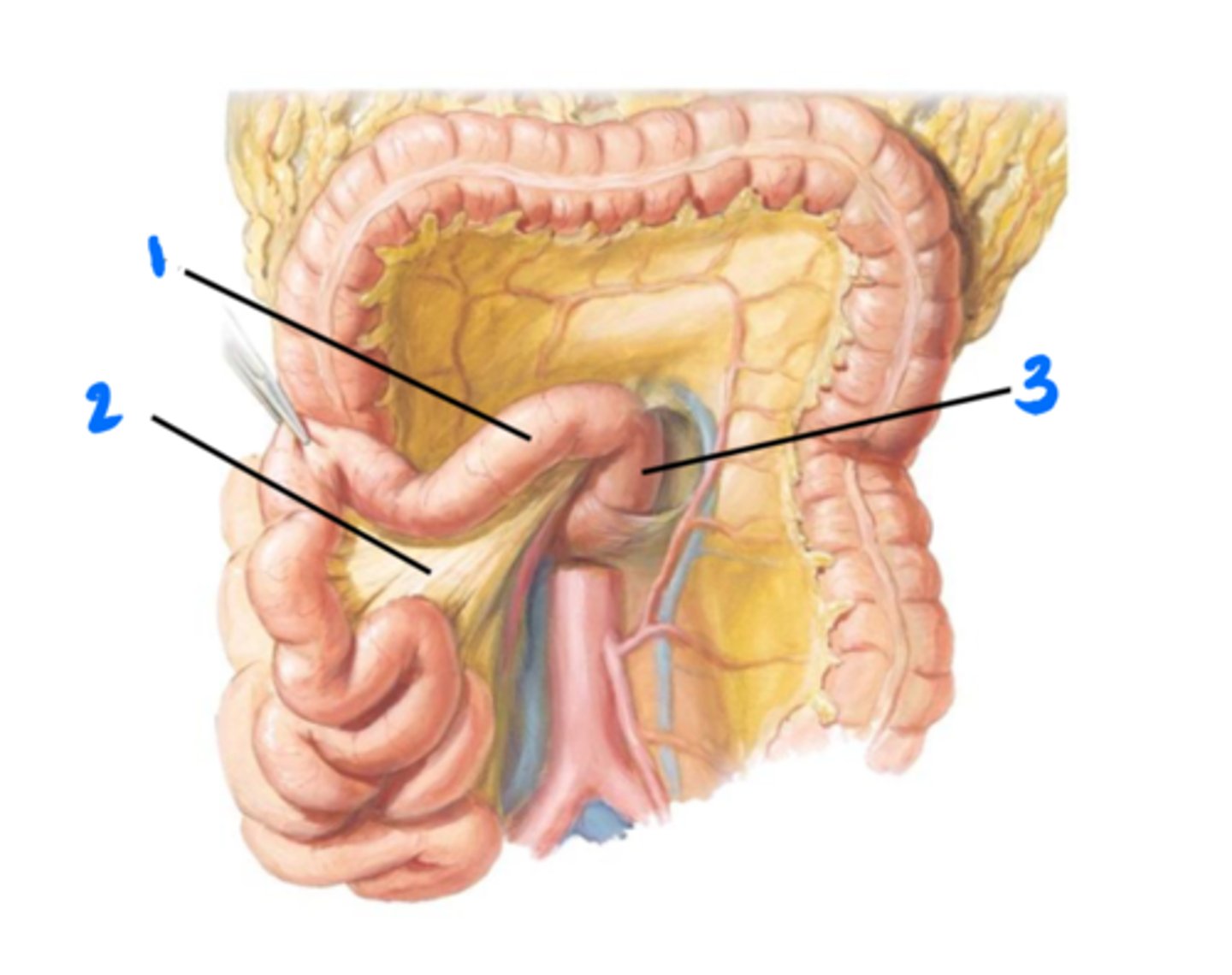
4th part of duodenum
3
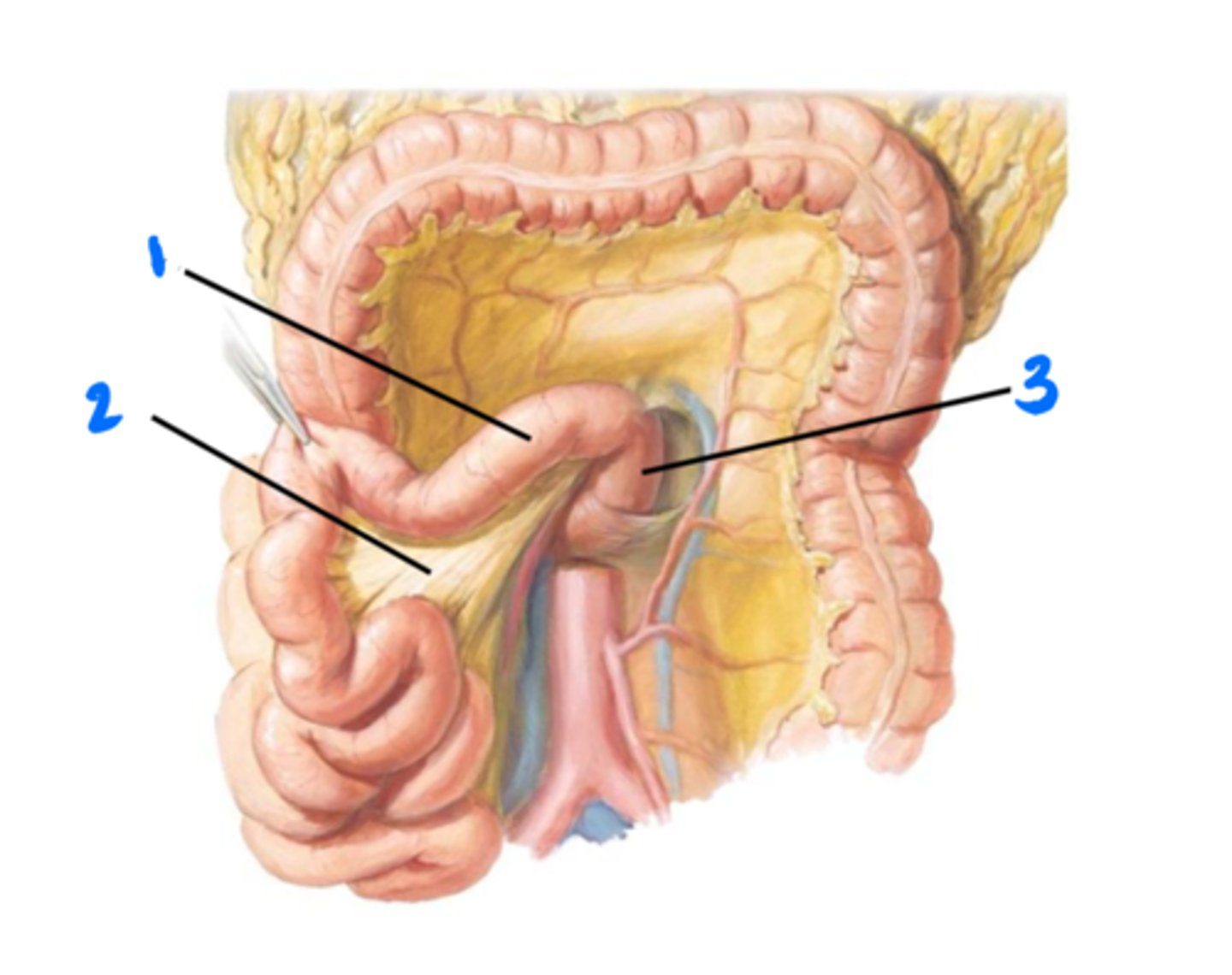
Left upper quadrant, under the greater omentum
Jejunum is located in the
Right lower quadrant, under the greater omentum
Ileum is located in the
Branches of the superior mesenteric artery
Jejunal artery: less complex arcades (loops), long vasa recta
Ileal artery: complex arcades, short vasa recta
Jejunum/ileum blood supply
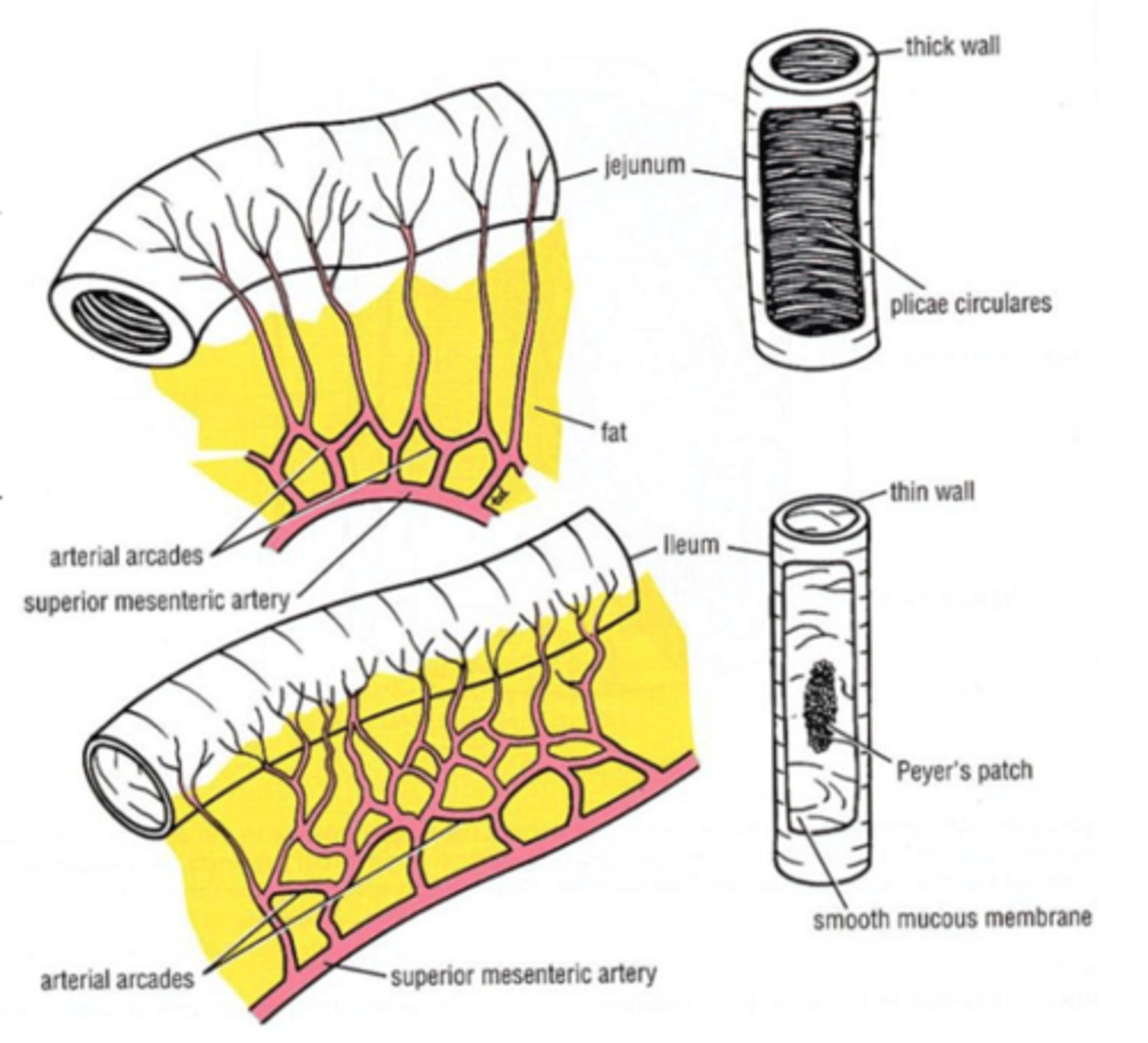
-second portion of the small intestine, 2/5th length-
"typical" small intestine
-Villi are broad and often have a visible lacteal.
Unlike the duodenum (duodenal glands) and ileum (peyer's patches), there are no special structures in the submucosa
Jejunum function
Intestinal veins
Proteins and carbohydrates generally travel through ______ and are then transported to the liver.
lacteals
lymphatic ducts
left subclavian vein
Fatty molecules tend to get absorbed by ______ which transport them through _____ bypassing the liver until they reach the _____.
-third portion of the small intestine, 3/5 of its length
-similar to the jejunum except that it contains large lymph nodules in the lamina propria - peyer's patches.
Ileum function
-large lymph nodules in the lamina propria (submucosa) of the ileum
-major component of our immune maintenance over the normaflora of the gut and response to infection
Peyer's patches
-needed for proper red blood cell production
-parietal cells (stomach) secrete intrinsic factor, which allows VB12 to get absorbed in ileum
Vitamin B12
Vitamin B12 deficency
Pernicious anemia
Careless removal of the stomach or ileum can result in ______ deficiency, which can then lead to ______
At terminal end of the ileum is a thickening (not a true sphincter) of the muscularis externa
Prevents release of the food bolus into the large intestine unless relaxed
-can have a papillary form or labial form
Ileocecal valve
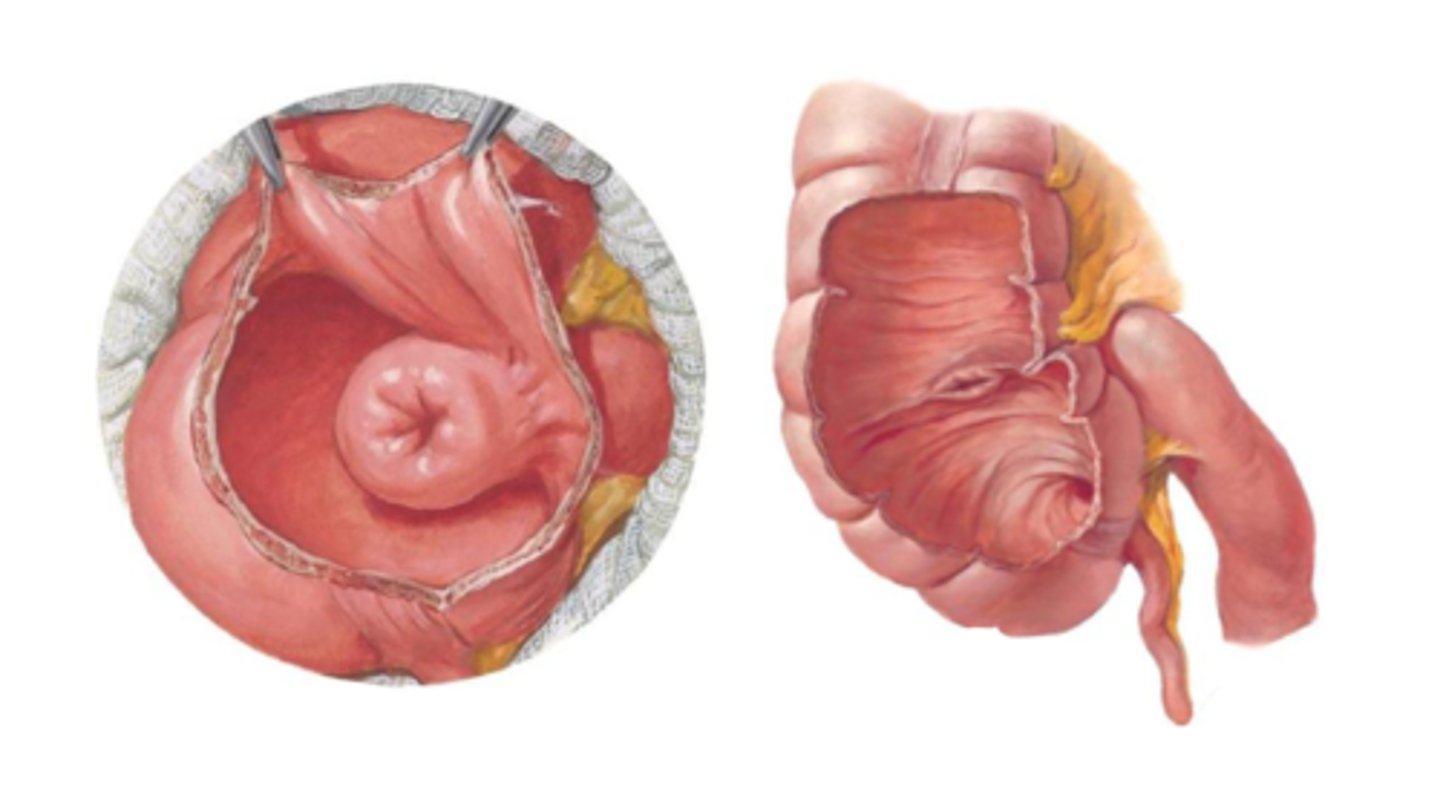
May result in the ileum folding into the colon (cecum) - intussusception
Ileocecal valve dysfunction
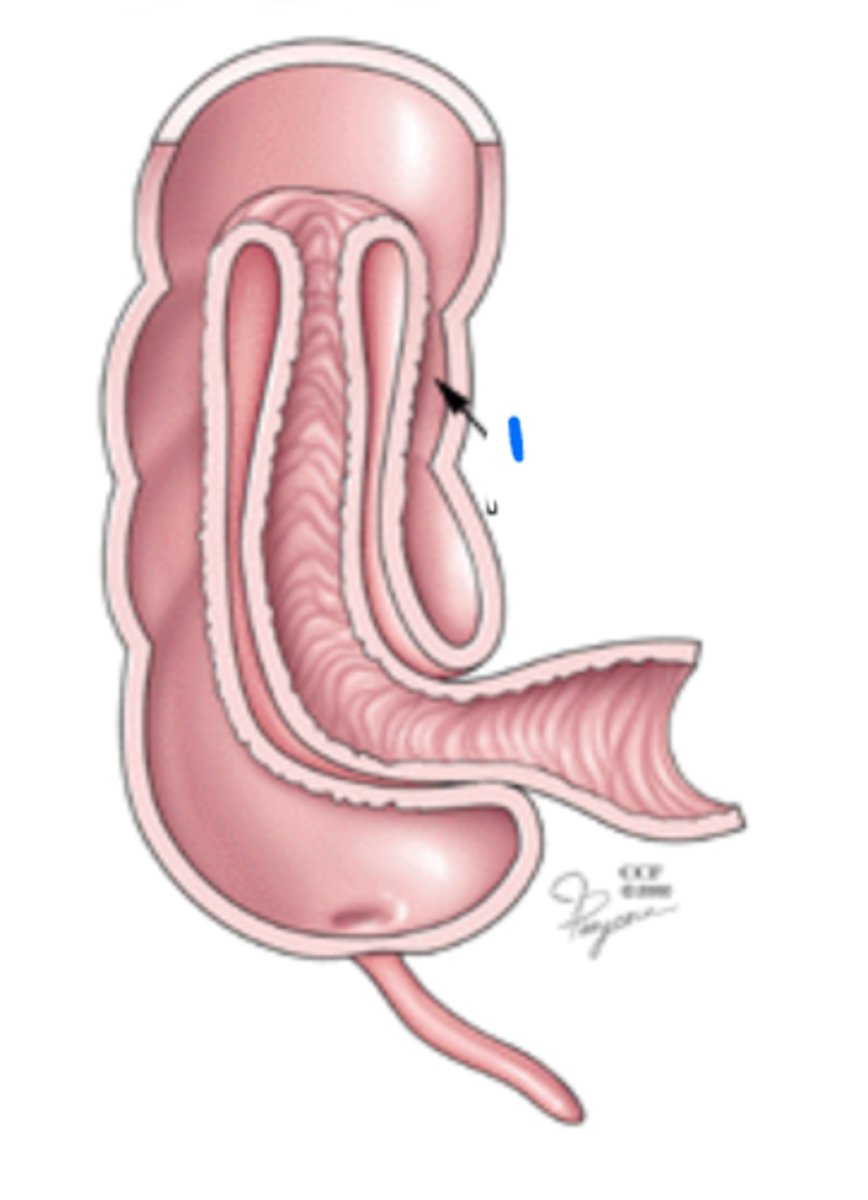
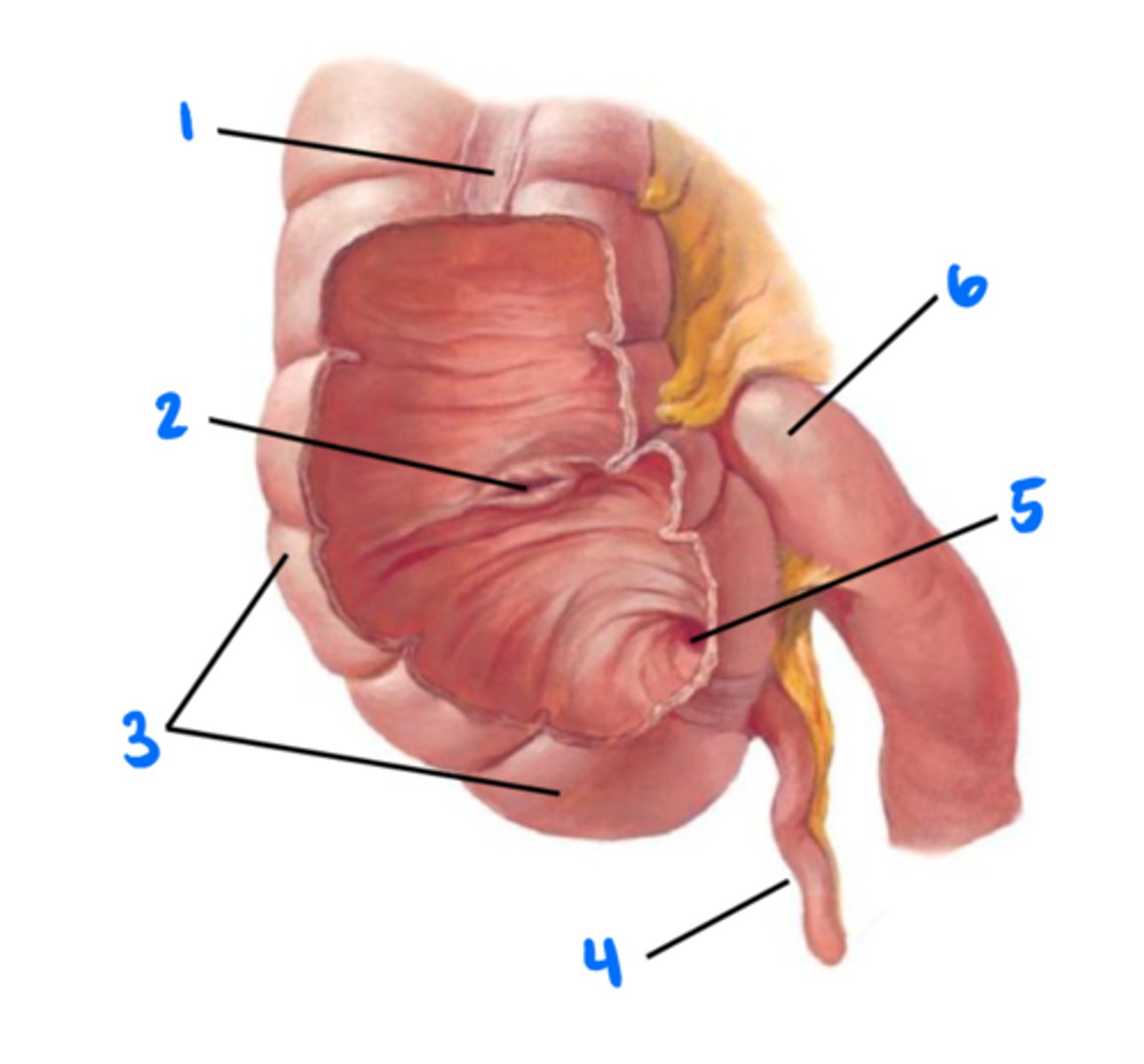
Tenia coli (longitudinal muscles of colon)
1
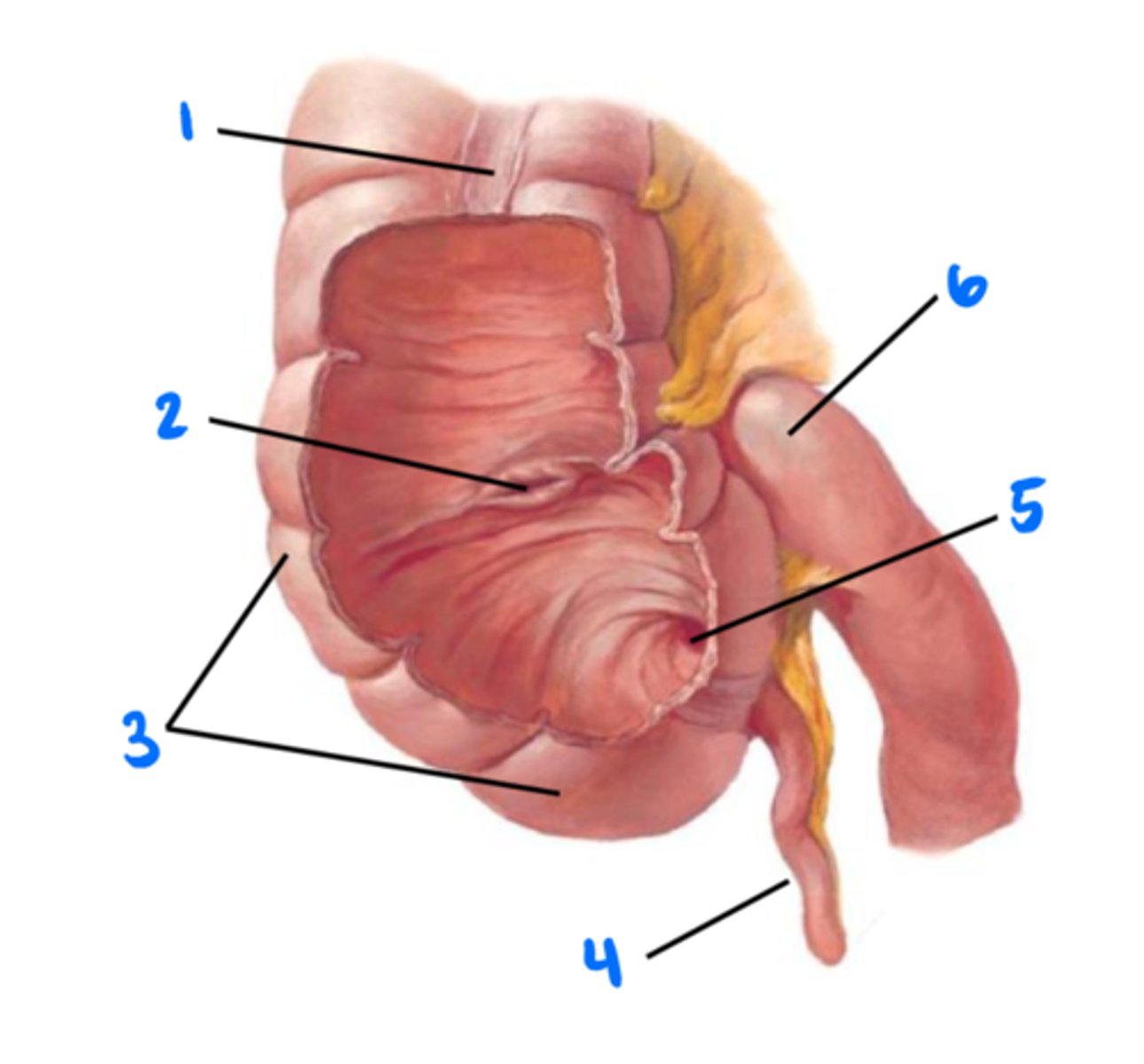
Ileocecal valve
2
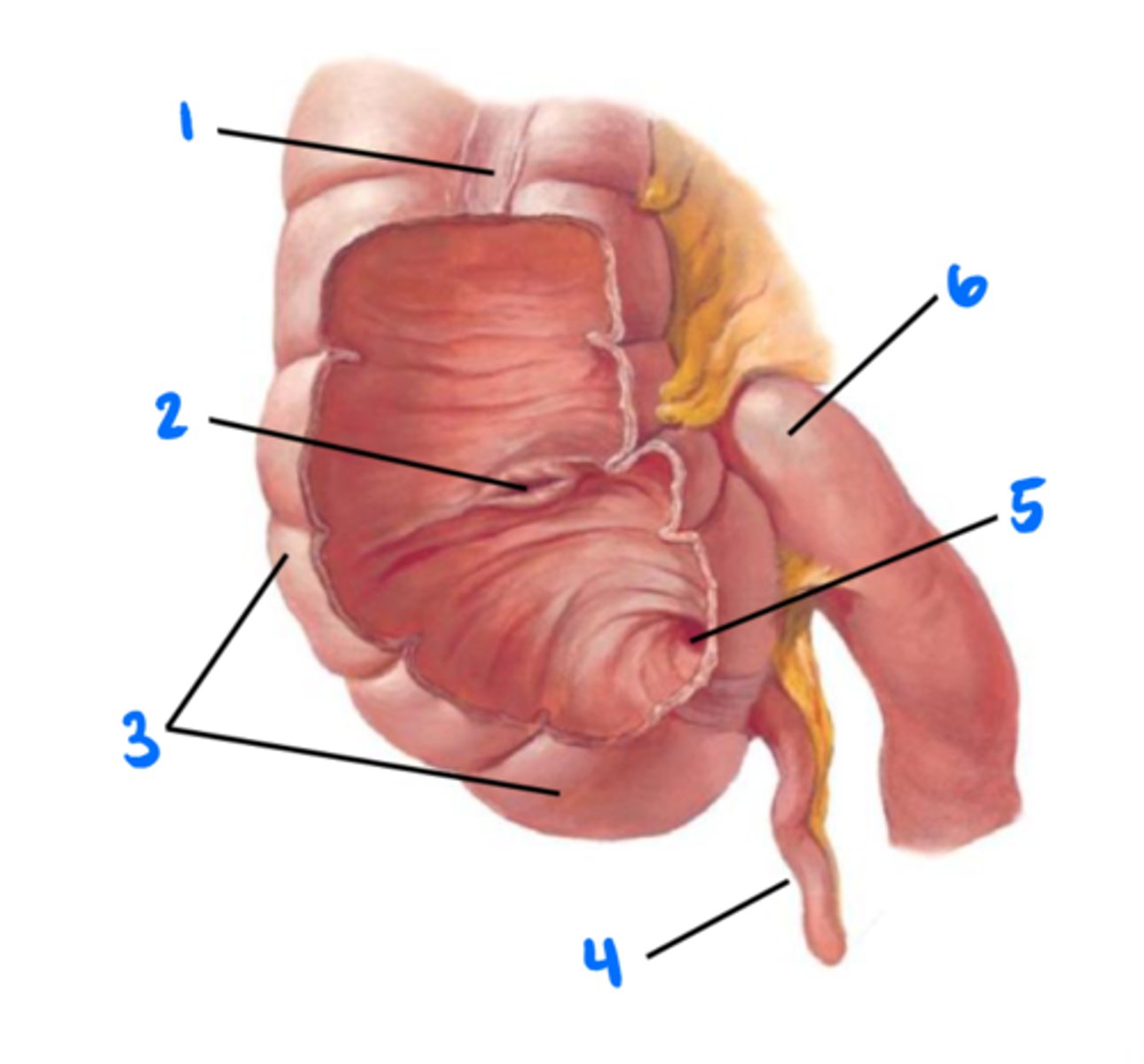
Cecum
3
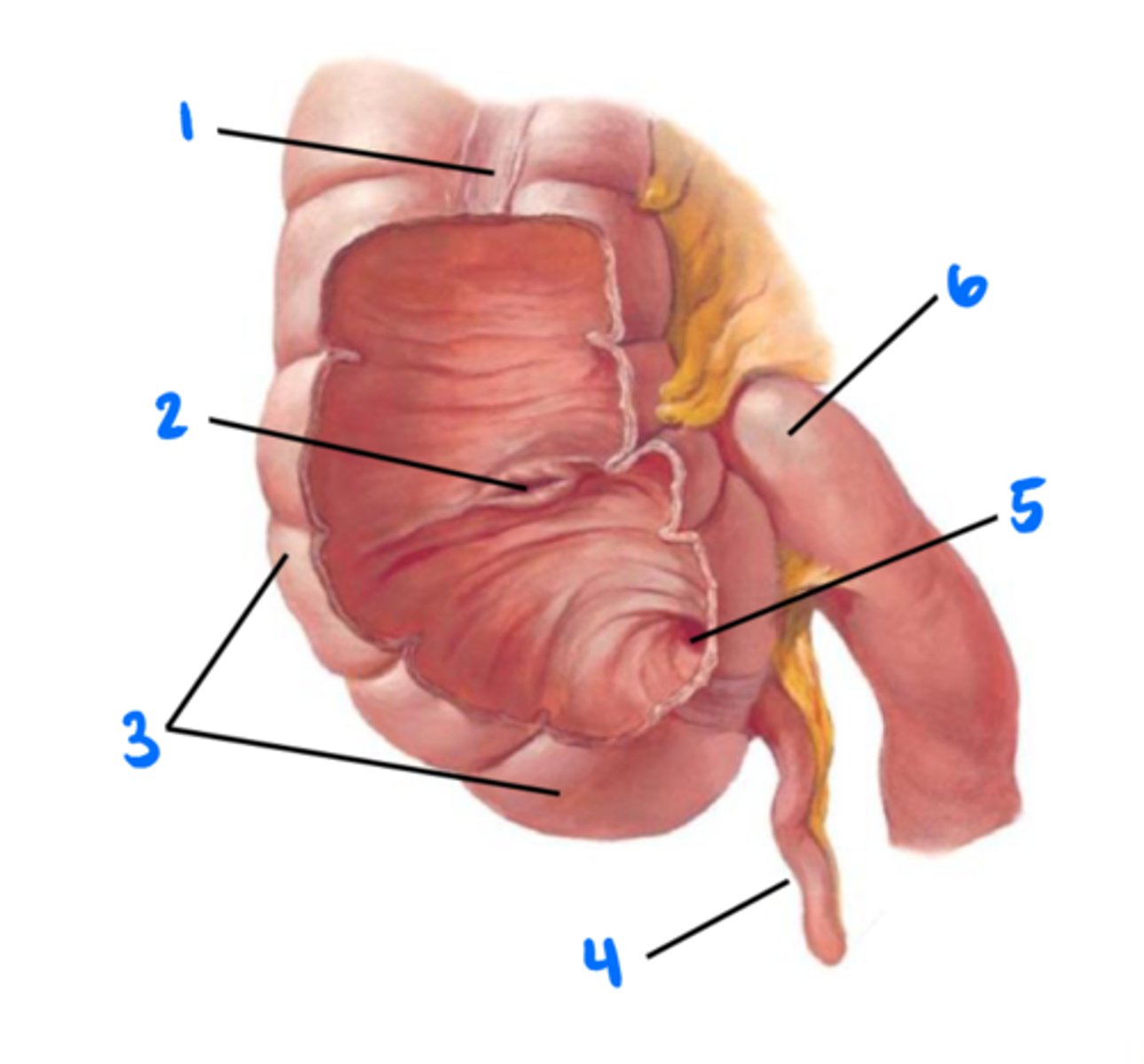
Vermiform appendix
4
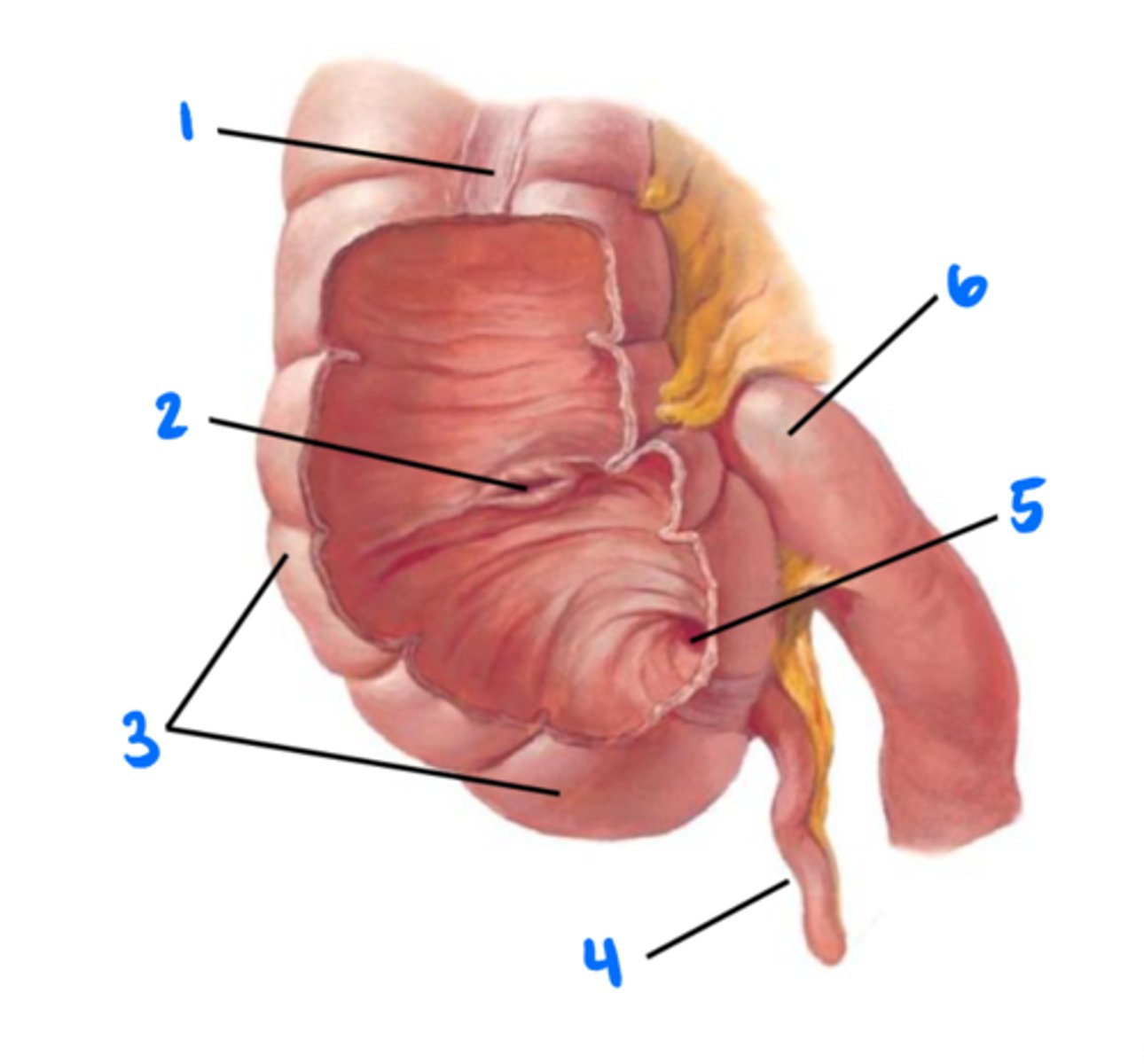
Orifice of vermiform appendix
5
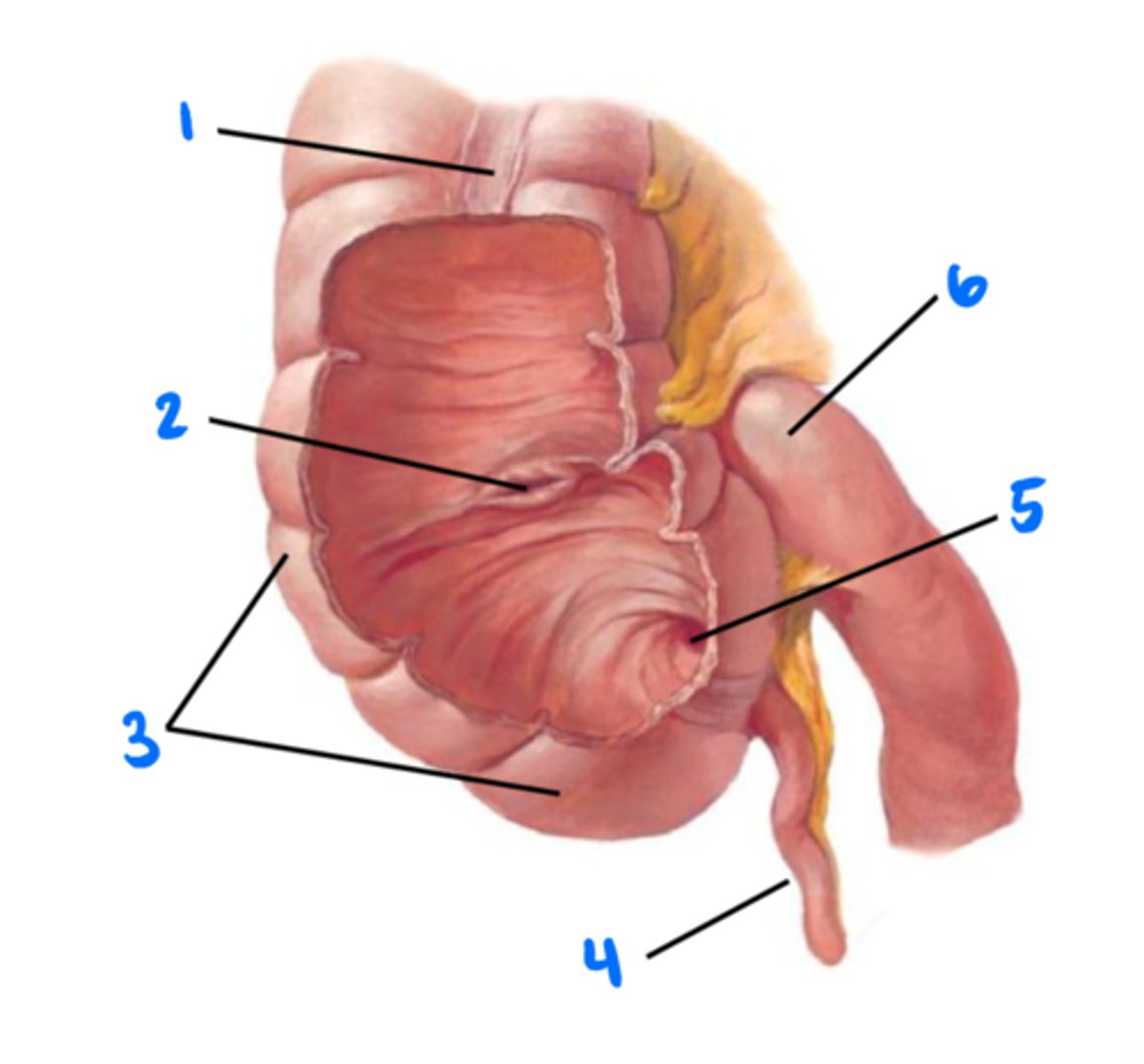
Ileum
6
Receives the bolus from the ileum and and recovers water and electrolytes from it. Feces then passes through the anal canal.
Large intestine
Cecum (with appendix), colon, rectum, anorectal junction, anal canal
Portions of the large intestine
Extension of the cecum. Has a narrow lumen and a large number of lymphatic nodules.
If the opening is blocked by feces or lymphatics it will become inflamed, rupture will cause GI contents being released into peritoneal cavity
May function as a reservoir to replenish intestinal normaflora
-suspended by a tiny mesentery that carries it's blood supply
-many variations in location
Appendix
ileum
cecum
ascending colon
The _____ is suspended by a mesentery but the _____ and _____ are not.
Pain in RLQ with appendicitis caused by swelling or infection of the appendix, which irritates the parietal peritoneum nearby.
This turns the dull and diffuse abdominal pain to become sharp and well-localized pain
McBurney's point
right lower quadrant
The cecum is located in the
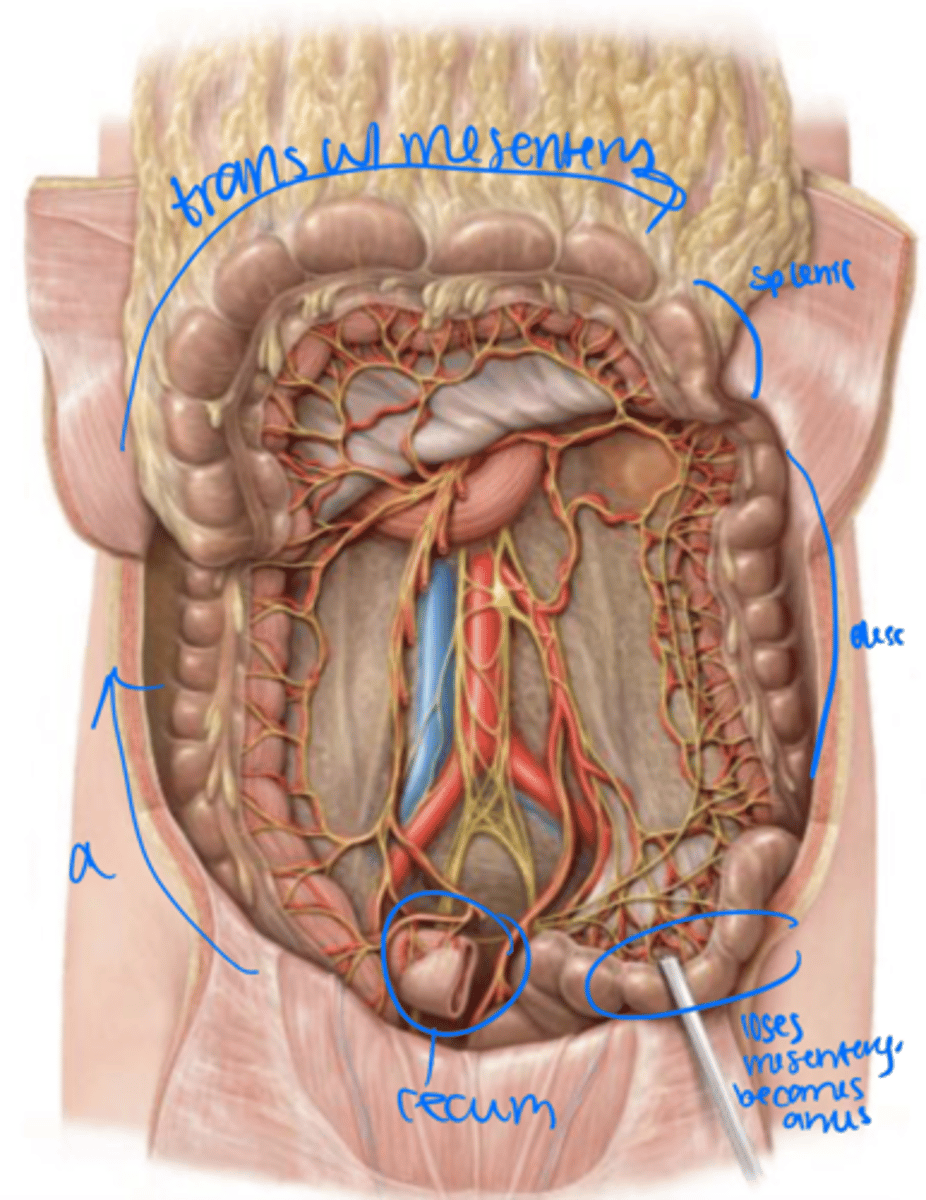
right upper quadrant
The ascending colon ascends to the
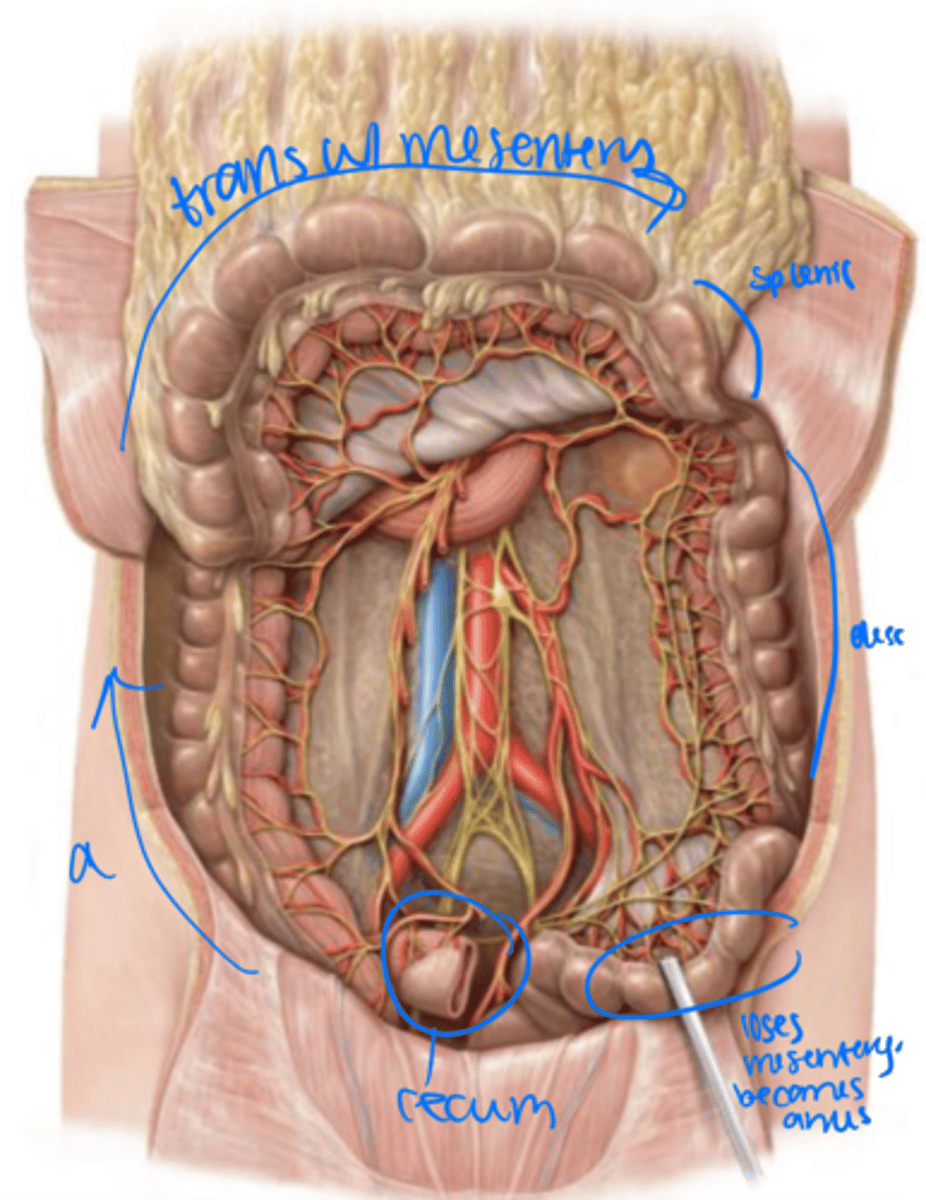
Transverse colon
right colic (hepatic) flexture
The ascending colon becomes the _____ at the ______.
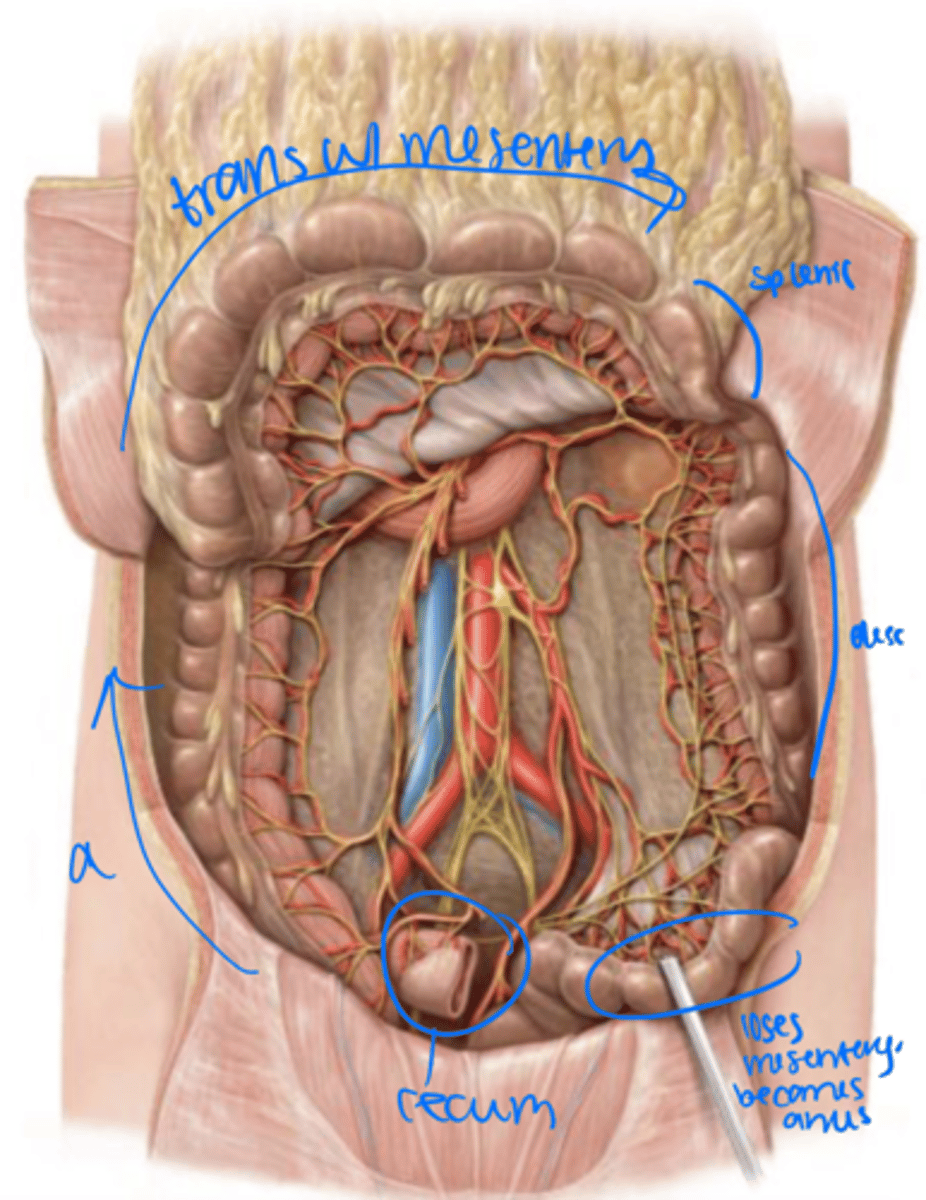
mesentery
left upper quadrant
The transverse colon has a _____ and stretches across to the _____
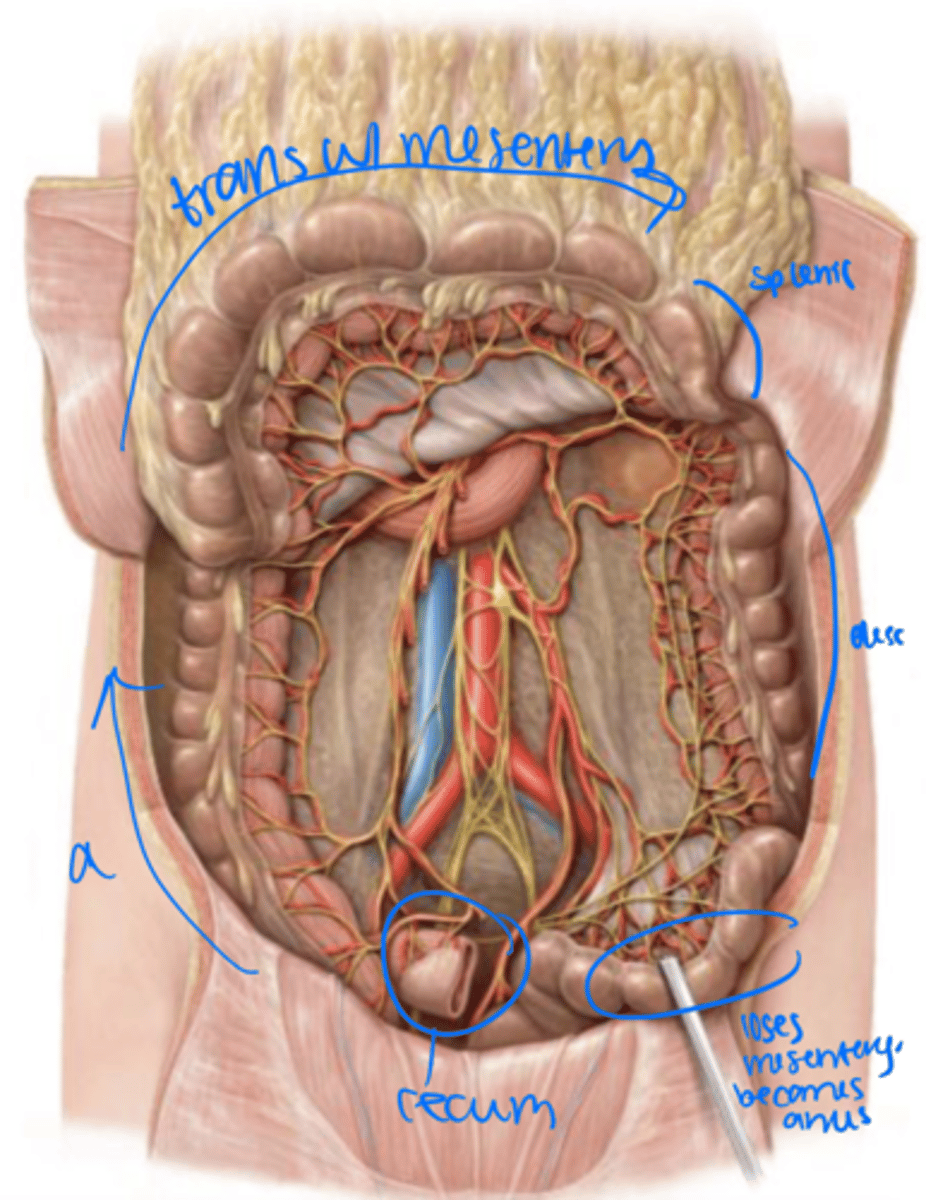
descending colon
left colic (splenic) flexture
The transverse colon turns into the _______ at the _________
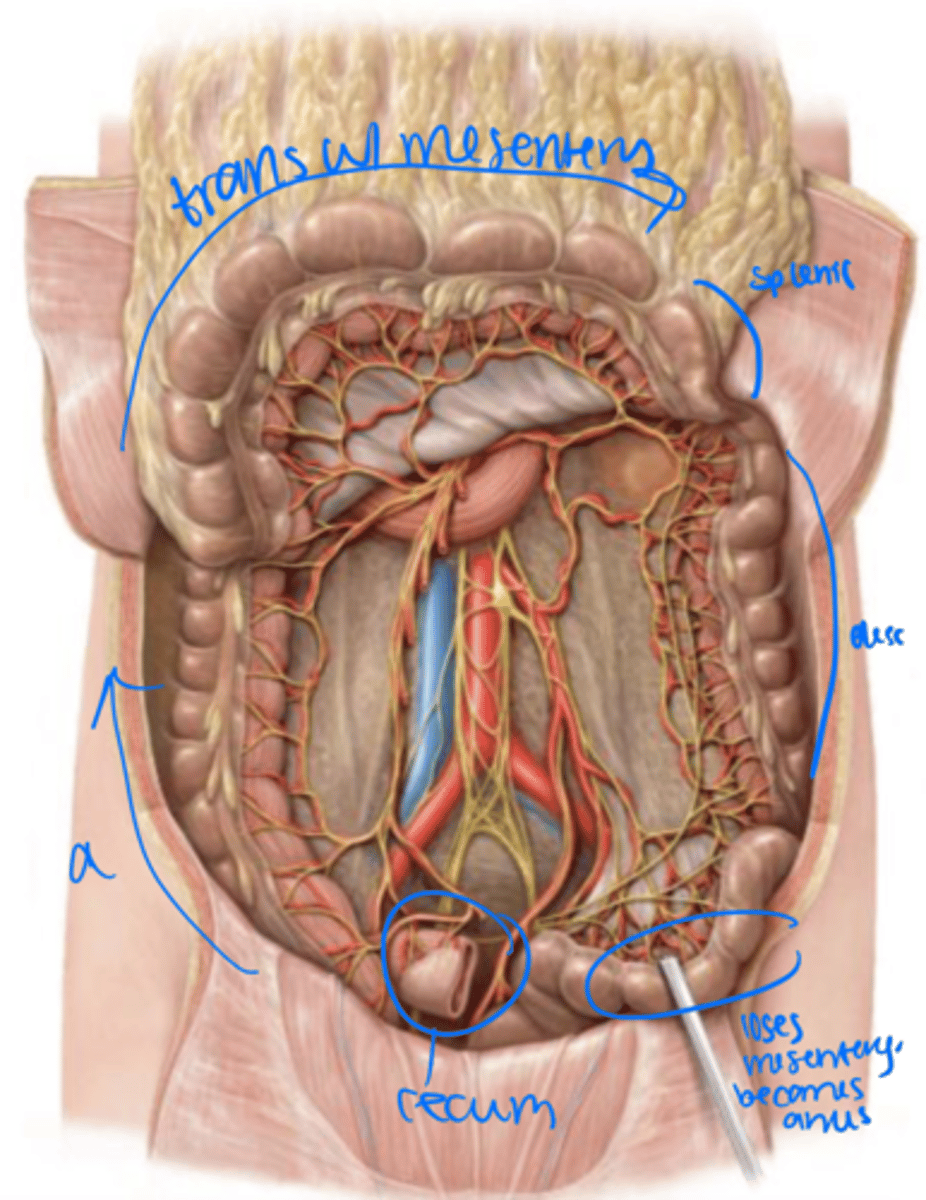
Left lower quadrant
sigmoid colon
The descending colon moves into the _______ and becomes the _______
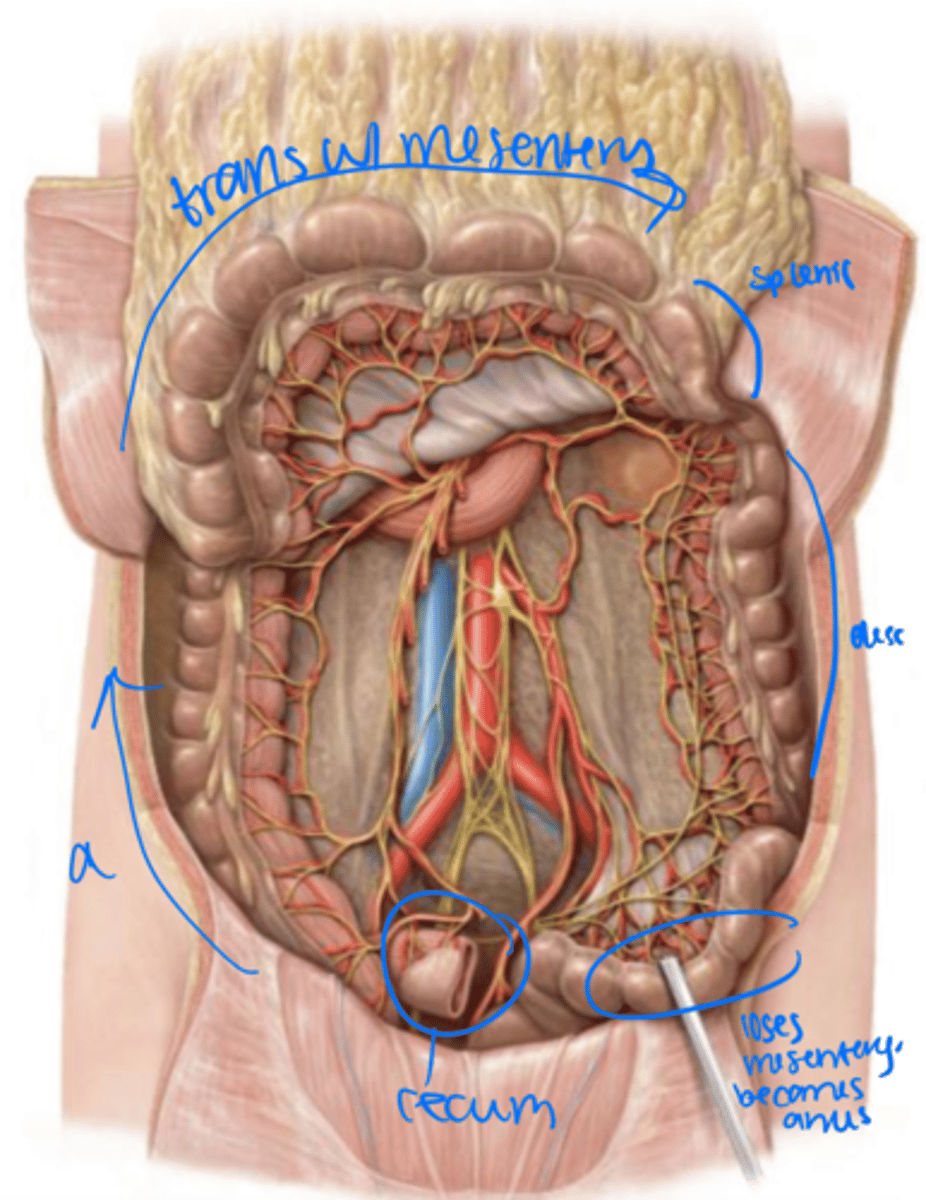
mesentery
left lower quadrant
The sigmoid colon has a _____ but tends to stay in the ______
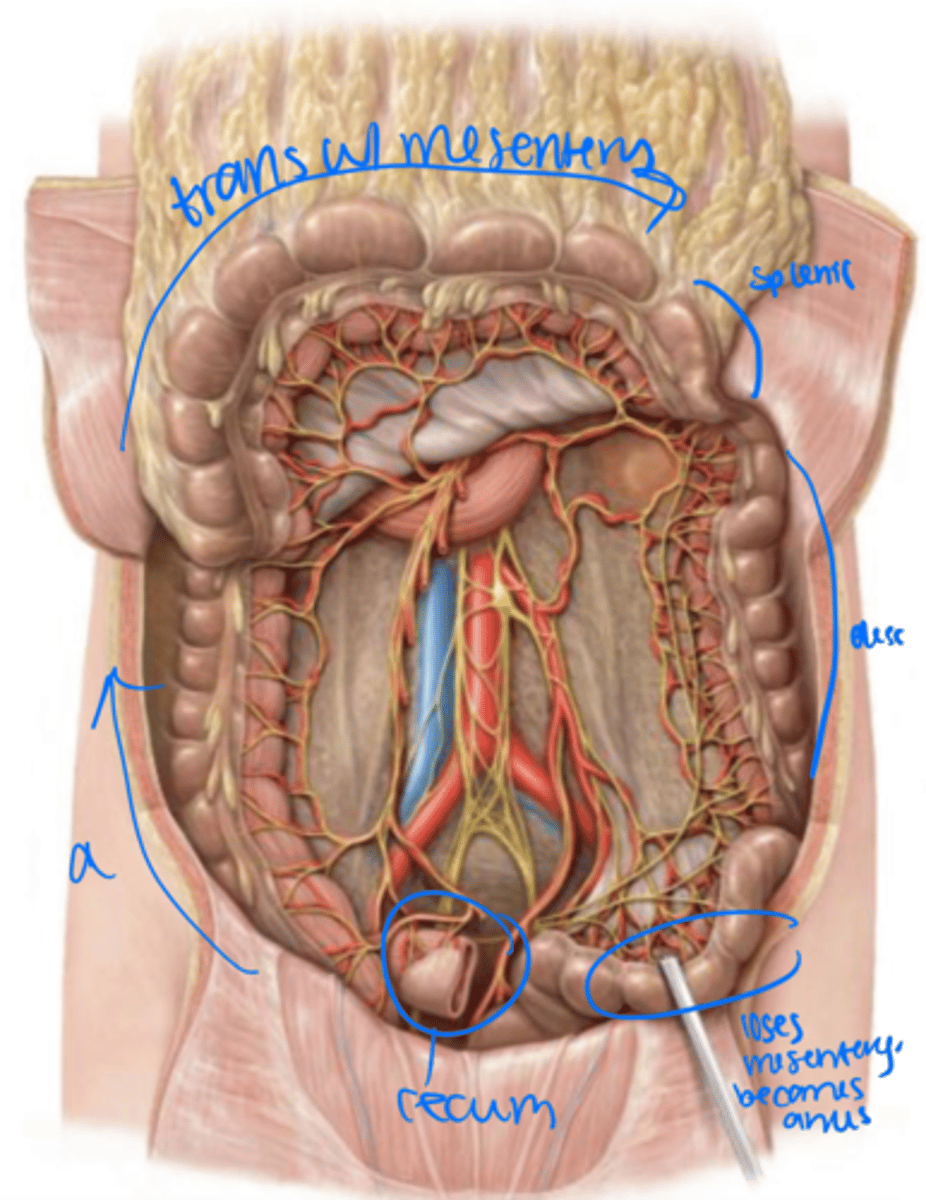
rectum
The sigmoid colon loses its mesentery as it becomes the _______ within the pelvis.
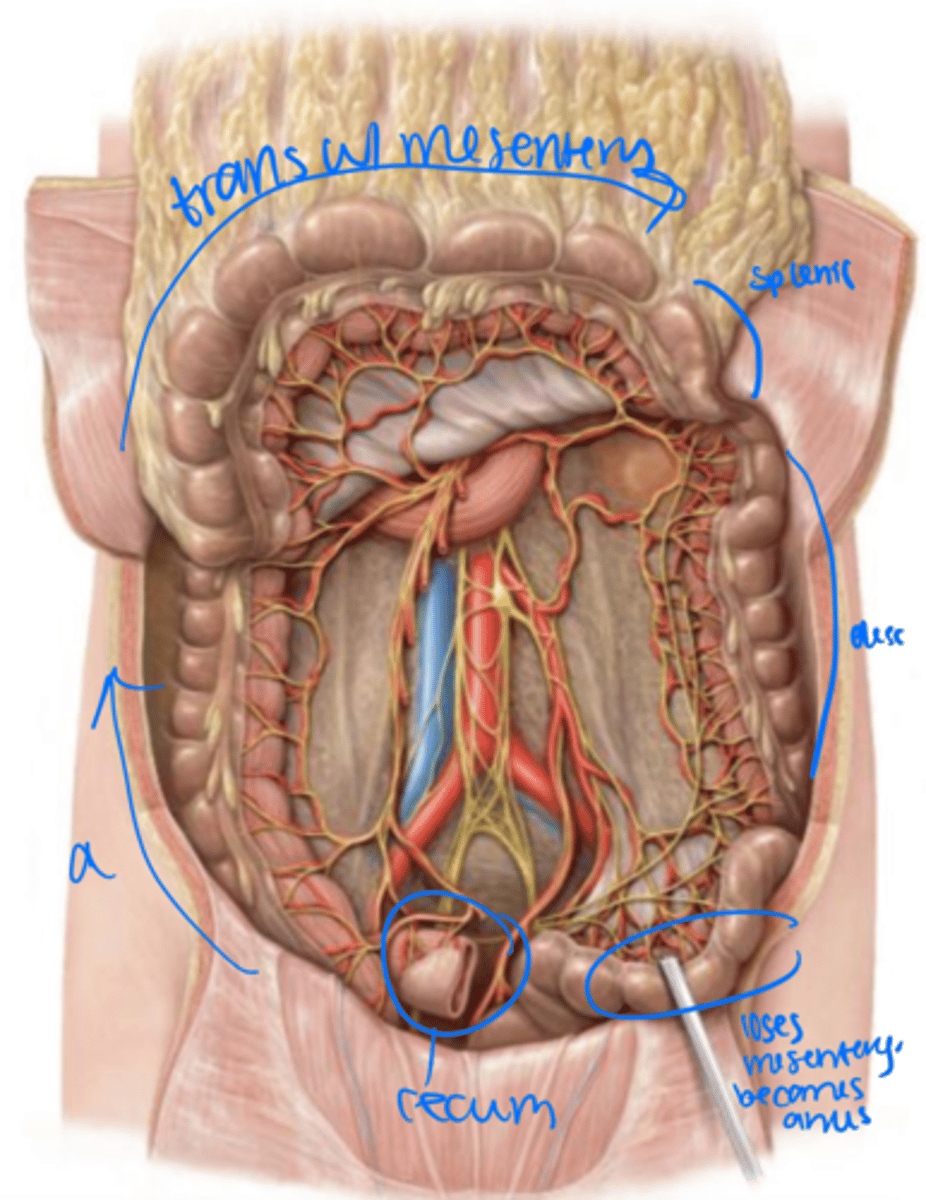
3 longitudinal muscles that move food through the colon and pinch off sacs, haustra, that can be seen macroscopically
Tenia coli
peristaltic activity of the circular and longitudinal muscles creates visible compartments, haustra, in the length of the large intestine. As the feces moves along, it passes into the rectum where it is stored prior to defecation
Movement of feces through large intestine
Abnormal side pockets in the intestinal wall due to weak spots in lumen of large intestine. Can become inflamed.
Diverticula
Occur when proliferating masses grow into lumen of the large intestine
Polyps