Integumentary System: Aging, Conditions, and Treatment Strategies
1/90
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
91 Terms
What are the primary layers of the integumentary system?
Epidermis, Dermis, Hypodermis, Subcutaneous
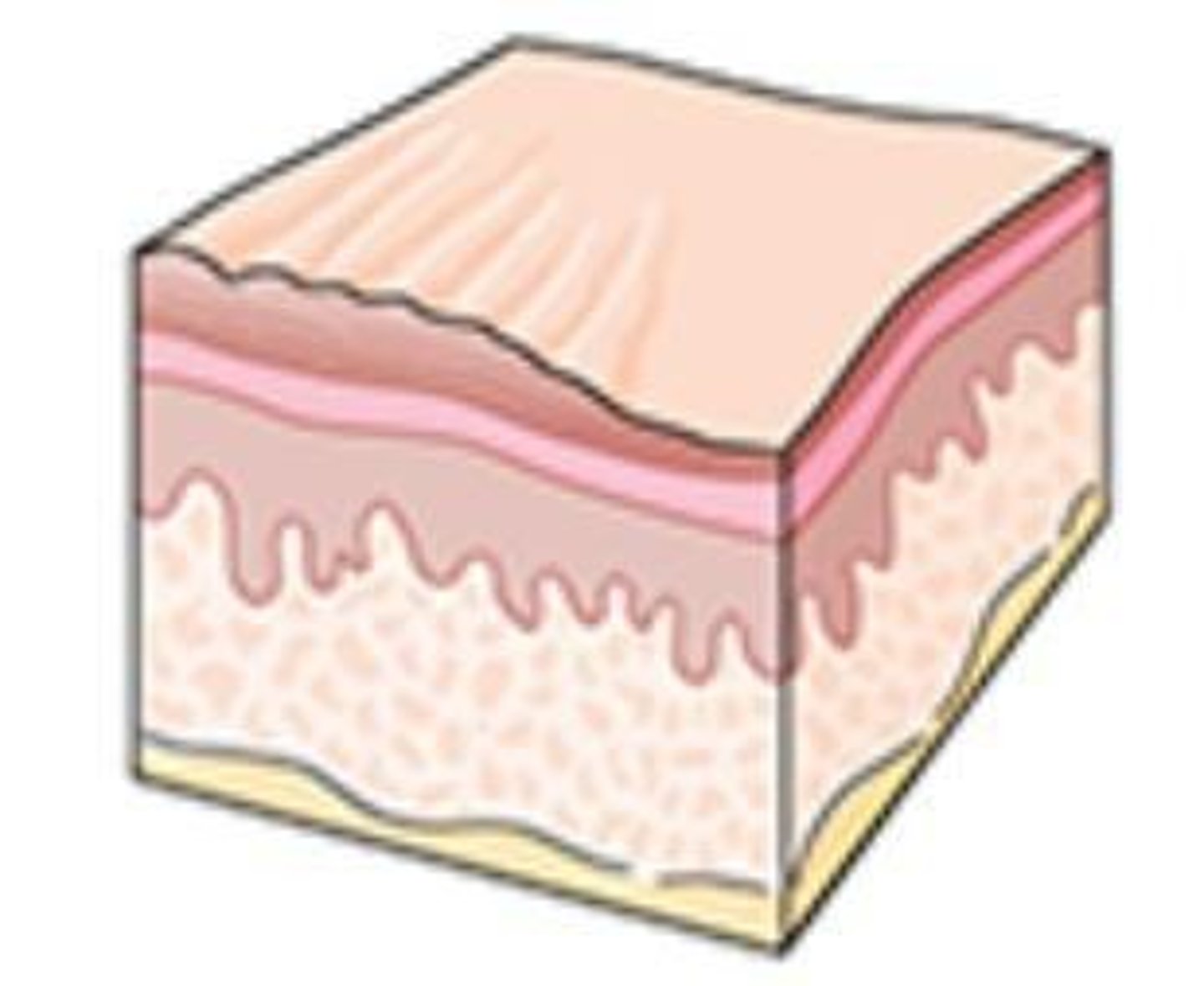
What is the main function of keratinocytes?
To provide a defensive role by protecting against invasion, preventing moisture and heat loss, and immunomodulation.
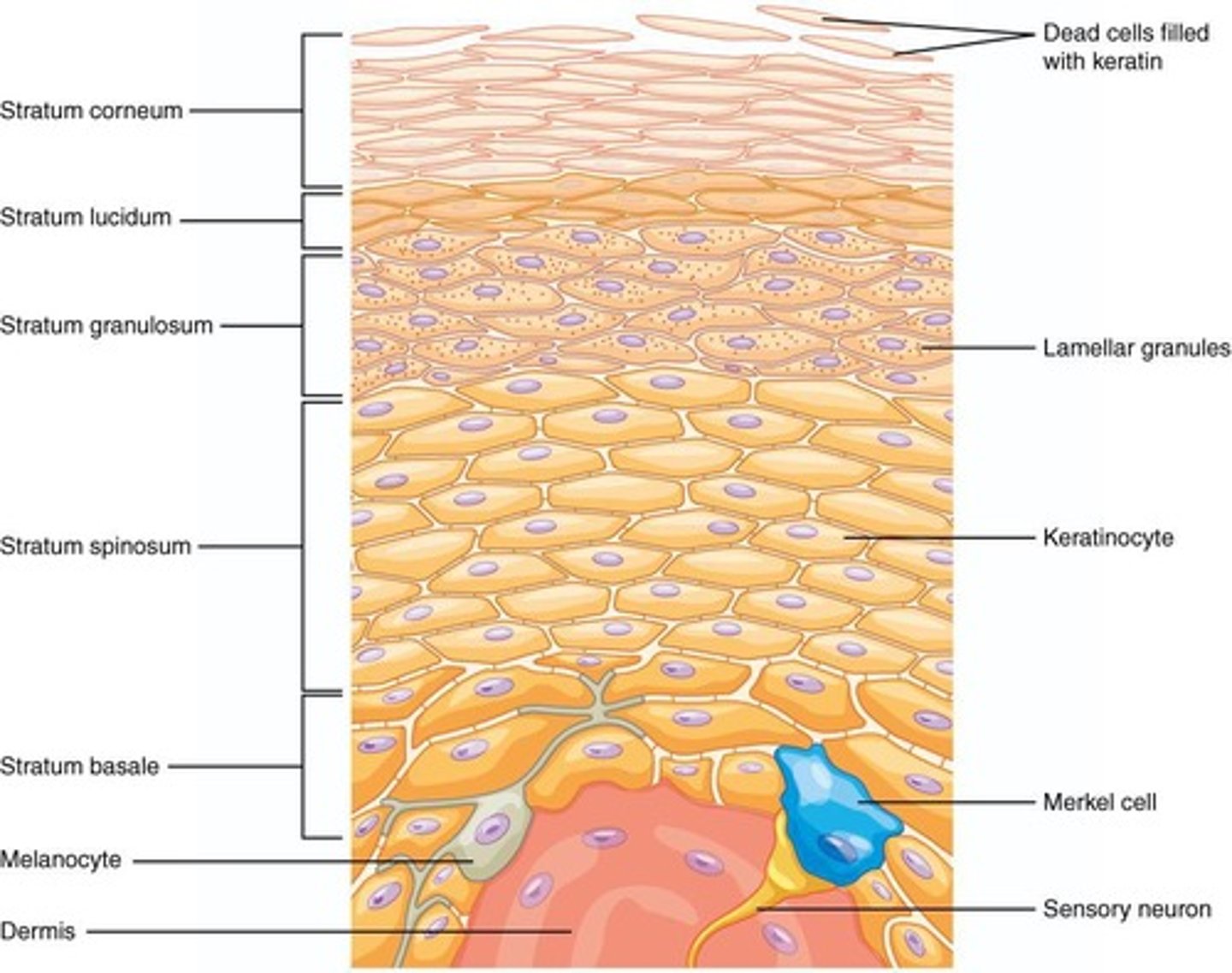
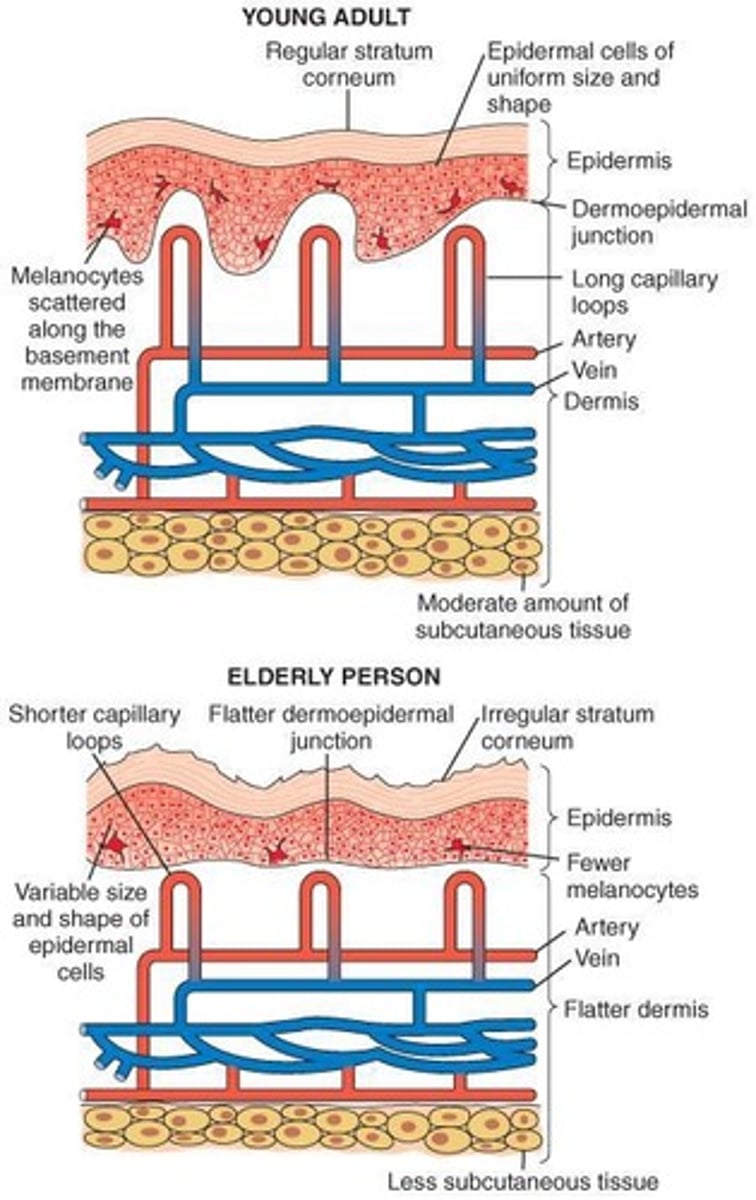
What age-related changes occur in the epidermis?
Epidermis thins, cells reproduce more slowly, and exposure to sunlight contributes to the development of aged skin.
How do sebaceous glands change with age?
They become less active, leading to dry skin and a predisposition to acne.
What are common hair changes associated with aging?
Progressive hair loss, greying of hair, and pattern baldness mediated by testosterone.
What happens to nails as a person ages?
Nails become brittle, hard, and thick, and there is a decrease in vascular supply to the nail bed.
What is senile purpura?
Aging purple spots that occur due to less vascular dermis.
What are primary lesions in the integumentary system?
Lesions that are present at the onset of a disease, such as macules, papules, nodules, and plaques.
What are secondary lesions?
Lesions that result from changes to primary lesions, such as crusts, scales, and ulcers.
What is the significance of the Woods Light test?
It helps identify certain fungal species that exhibit specific coloration under UV light.
What are common viral infections of the skin?
Herpes Simplex Virus (HSV), Human Papilloma Virus (HPV), and Herpes Zoster Virus.
What are the symptoms of Herpes Simplex Virus (HSV)?
Burning/tingling, erythema, vesicles, pustules, ulcers, and crusts.
What is the treatment for Herpes Simplex Virus?
Palliative care including pain relievers, cold compresses, and antiviral medications.
What are the characteristics of warts caused by Human Papilloma Virus (HPV)?
Common, benign growths that may appear on any body site.
What are the general rules for treating skin wounds?
Provide adequate pain control, ensure proper blood supply, and expect treatment to change over time.
What is the role of sensory nerves in the integumentary system?
They decline with age, causing decreased sensation and loss of effective vasoactivity.
What is the impact of aging on sweat glands?
Sweat glands decrease in size, number, and function, leading to reduced heat loss capabilities.
What is lichenification?
Epidermal thickening and roughening due to chronic irritation.
What is a keloid?
An augmentation of scar tissue that forms after injury.
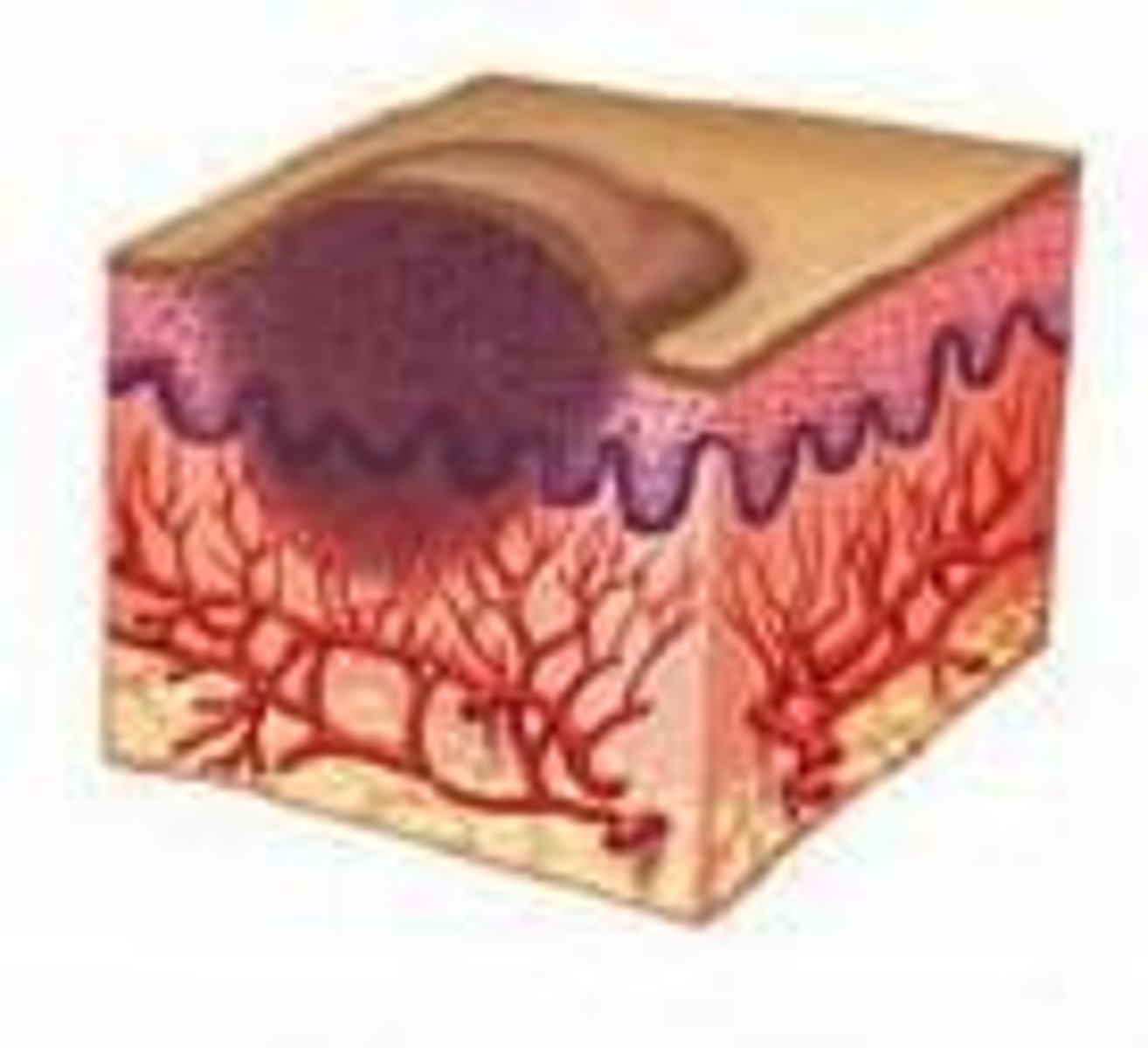
What is the significance of adequate blood supply in wound healing?
It is essential for healing to take place and for the removal of necrotic tissue.
What are the common etiologies of skin conditions?
Infection/infestation, genetics, trauma, and circulatory compromise.
What is the role of tissue biopsy in dermatology?
To confirm or establish a diagnosis, estimate prognosis, or follow the course of a disease.
What are the characteristics of a macule?
A flat change in color, less than 5mm in diameter.
What defines a papule?
A raised, palpable lesion that is less than 5mm in diameter.
What is a bulla?
An epidermal fluid collection greater than 5mm in diameter.
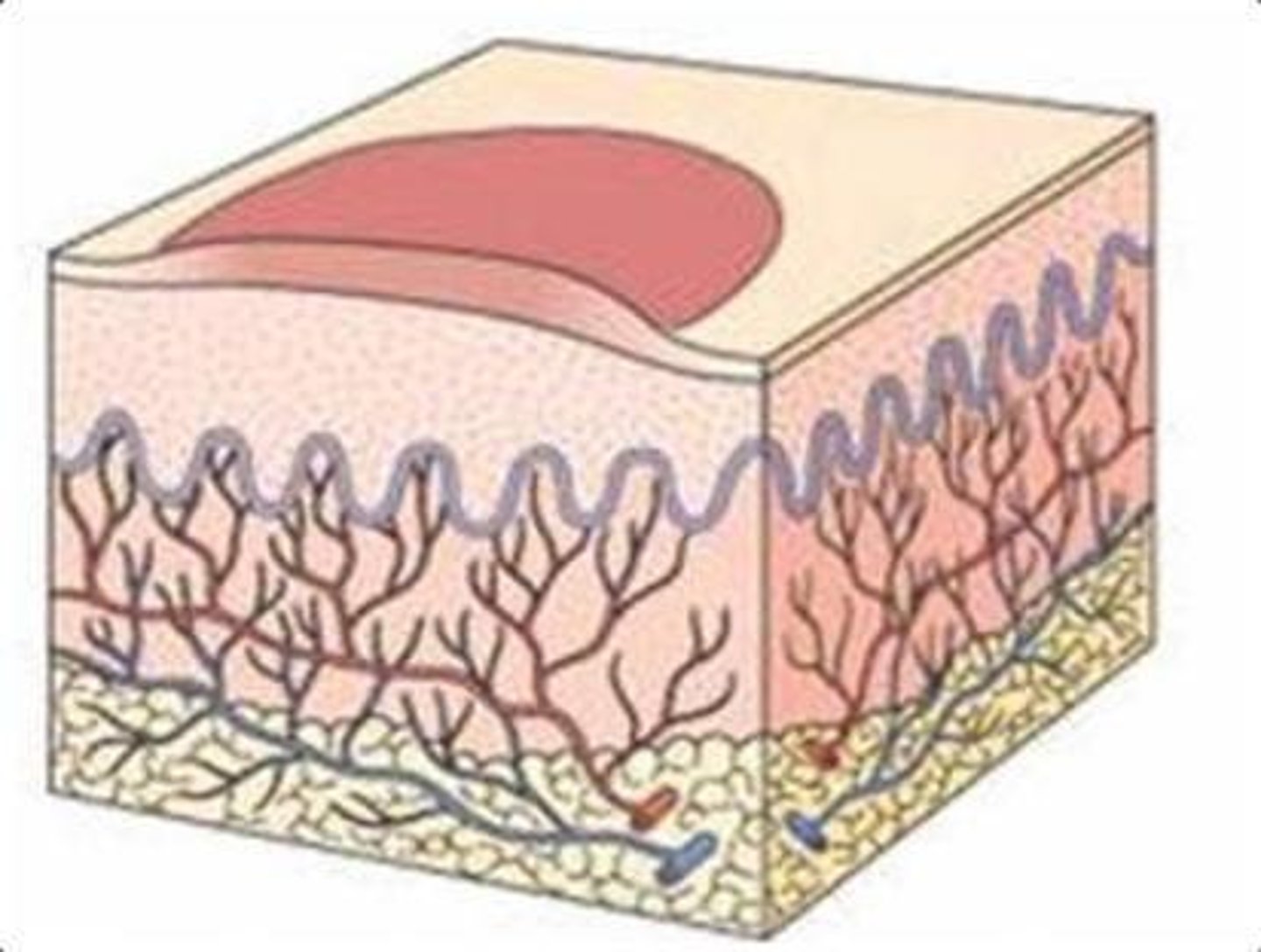
What is an ulcer in the context of skin lesions?
A loss of tissue through the epidermis.
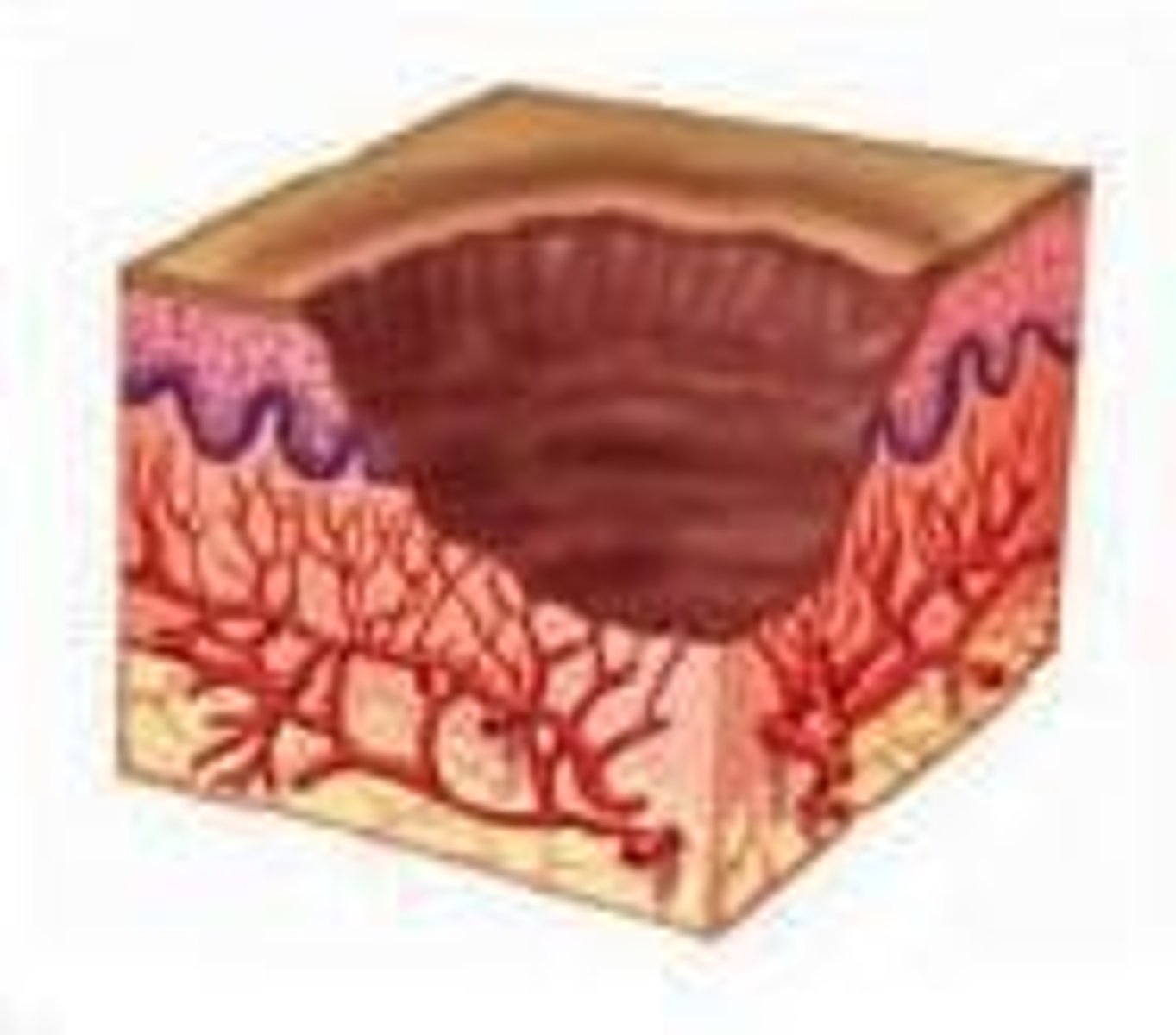
What is excoriation?
Loss of epidermis due to friction-related injury.
What virus causes Herpes Zoster (shingles)?
Reactivation of latent varicella zoster (chickenpox) virus along nerve ganglia.
What are the common symptoms of Herpes Zoster?
Vesicles grouped along dermatomes on trunk and face, painful.
What are the treatment options for Herpes Zoster?
Antiviral medication, local and systemic pain relievers, corticosteroids.
How can Herpes Zoster be prevented?
Vaccination.
What is Tinea?
A fungal infection commonly caused by species such as Microsporum, Trichophyton, and Epidermophyton.
What are the symptoms of Tinea?
Erythematous macules or plaques with peripheral scaling and central clearing, vesicular lesions.
What are the treatment options for Tinea?
Antifungal cream or powder, barrier ointment, keeping the area clean and dry.
What is Impetigo?
A contagious bacterial skin infection commonly caused by staph or strep species.
What are the symptoms of Impetigo?
Vesicles, pustules, yellowing crusts.
What are the treatment options for Impetigo?
Topical antibiotic ointment, oral antibiotics.
What is Necrotizing Fasciitis?
An aggressive skin/soft tissue infection that causes muscle fascia and subcutaneous tissue necrosis.
What are the common organisms causing Necrotizing Fasciitis?
Staphylococcus aureus and Group A Streptococcus.
What are the early signs and symptoms of Necrotizing Fasciitis?
Erythema and/or swollen area of skin that spreads quickly, severe pain, fever.
What are the later signs and symptoms of Necrotizing Fasciitis?
Changes in skin color, pus or oozing from the infected area, ulcers, blisters, or black spots on the skin.
What are the treatment options for Necrotizing Fasciitis?
IV antibiotics, removal of infected tissue, debridement of necrotic tissue.
What is the purpose of Negative Pressure Wound Therapy (NPWT)?
Promotes healing by removing excess fluid, debris, and infectious materials, reducing edema, and promoting granulation tissue formation.

What is Scabies?
A contagious skin disease transmitted by the itch mite (Sarcoptes scabiei).
What are the primary sites affected by Scabies?
Interdigital web spaces, wrists, axillary folds, periumbilical skin, pelvic girdle, penis, and ankles.
What are the symptoms of Scabies?
Intense pruritis (itching) especially at night, erythematous papules, excoriations, and occasionally vesicles.
What are the treatment options for Scabies?
Topical scabicides, topical sulfur.
What are Bed Bugs?
Nocturnal insects that feed on human and animal blood.
What is the Latin origin of the term 'Scabies'?
Latin 'scabere' meaning 'to scratch'.
What is the significance of vaccination in relation to skin infections?
Vaccination can prevent certain viral infections like Herpes Zoster.
What is the common treatment for skin infections caused by bacteria?
Topical or oral antibiotics.
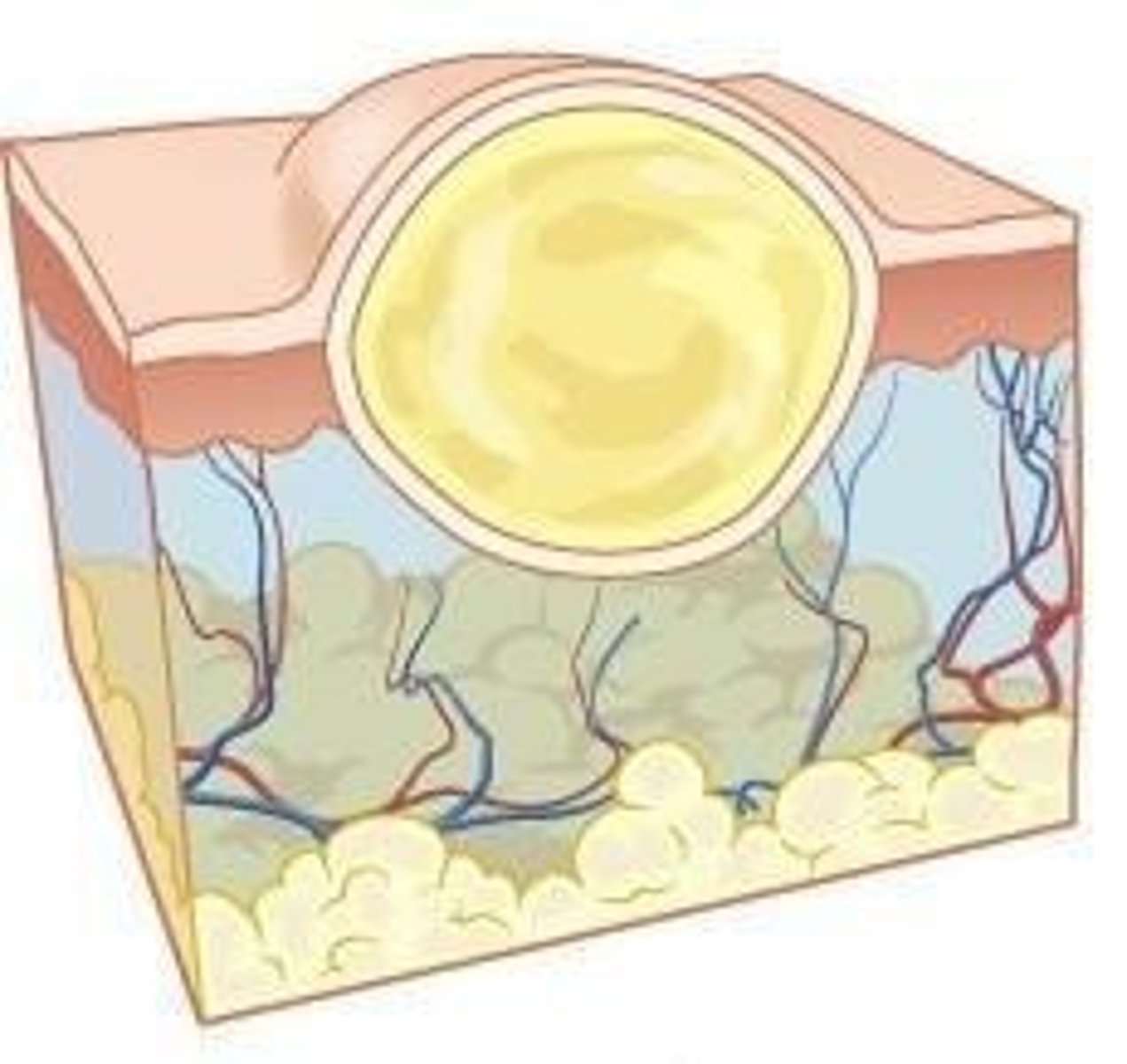
What is the role of granulation tissue in wound healing?
It fills the wound bed and is essential for the healing process.
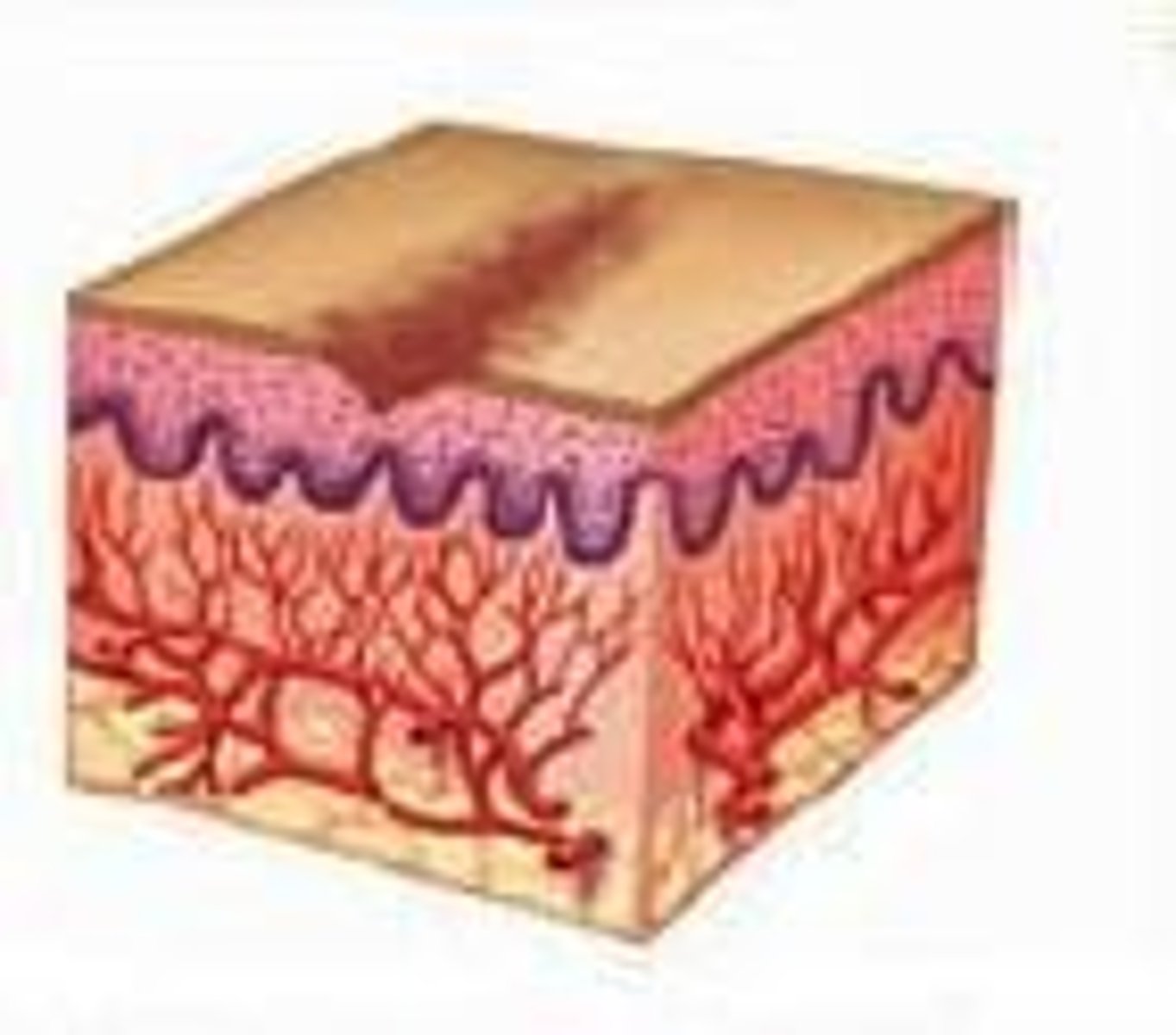
What are common primary sites for skin infestations?
Face, neck, hands, arms
What are the signs and symptoms of skin infestations?
Pruritis, oval or oblong wheals with puncture sites in centers, appearing in clusters or rows
What is a common treatment option for skin infestations?
Topical antipruritic
What is Rocky Mountain Spotted Fever caused by?
The carrier tick, specifically Rickettsia rickettsii
What are the signs and symptoms of Rocky Mountain Spotted Fever?
Papule or macule at original tick bite site, fever, headache, muscle aches, nausea, vomiting, macular or popular rash, edema, photophobia, lethargy, AMS
What is the treatment for Rocky Mountain Spotted Fever?
IV Antibiotics
What are prevention measures for Rocky Mountain Spotted Fever?
Insect repellent, remove attached tick immediately and completely
What causes Lyme Disease?
The carrier tick, specifically Borrelia burgdorferi
What are the stages of Lyme Disease?
Stage 1: erythemous papules (bullseye lesions), flu-like symptoms; Stages 2 & 3: more systemic, involve nervous system
What is the treatment for Lyme Disease?
IV Antibiotics and symptom management
What is Lupus Erythematosus?
An autoimmune disease with two common types: Systemic (SLE) and Cutaneous (CLE)
What are the signs of Cutaneous Lupus Erythematosus?
Scaly red disc-shaped plaques with scarring, butterfly-shaped erythema on cheeks and nose
What are treatment options for Lupus?
Topical corticosteroids and photoprotection
What is Psoriasis?
A chronic idiopathic skin condition that may be triggered by stress
What are the signs and symptoms of Psoriasis?
Pruritic erythemous macular clusters covered with silvery scales
What are treatment options for Psoriasis?
Topical corticosteroids, Vitamin D, ultraviolet light exposure, saltwater immersion
What characterizes Lichen Planus?
Severe pruritis, shiny, white-topped, purplish, polygonal papules on skin and mucous membranes
What are treatment options for Lichen Planus?
Discontinue all medications, topical corticosteroids, antipuritics, occlusive dressings
What is Scleroderma?
An idiopathic autoimmune disease causing sclerosis or scar-like changes to the skin
What are the signs of localized Scleroderma?
Firm, inelastic red or purple macules and plaques that slowly enlarge
What are treatment options for localized Scleroderma?
Palliative care including phototherapy, vitamin D, topical corticosteroids
What is Atopic Eczema?
A genetic deficiency in barrier function exacerbated by exogenous irritants
What are the signs and symptoms of Atopic Eczema?
Pruritis, papules, lichenification, scaling
What are treatment options for Atopic Eczema?
Moisturization, topical steroids, antihistamines, systemic antibiotics
What is Contact Dermatitis?
A hypersensitivity to specific irritants or allergens
What are the signs of Contact Dermatitis?
Pruritis, erythema, vesicles
What are treatment options for Contact Dermatitis?
Topical steroids, cooling agents to minimize pruritis
What is Vitiligo?
A chronic autoimmune disorder causing loss of color in patches due to melanocyte dysfunction
What is Albinism?
A genetic condition present at birth where melanocytes cannot produce melanin
What are the signs of Albinism?
White or very pale skin, hair, and eyes, light sensitivity, vision problems
What are the risk factors for pressure injuries?
Poor nutrition, aging, immobility, superficial sensory loss, bowel/bladder incontinence, medical devices
What is Stage 1 of pressure injuries?
Non-blanchable erythema of intact skin
What is Stage 2 of pressure injuries?
Partial thickness skin loss with exposed dermis
What is Stage 3 of pressure injuries?
Full thickness skin loss to subcutaneous layer, may have undermining or tunneling
What is Stage 4 of pressure injuries?
Full thickness skin and tissue loss to tendon, cartilage, or bone, with undermining or tunneling
What is an unstageable pressure injury?
Obscured full thickness skin and tissue loss, extent of damage cannot be confirmed
What is a Deep Tissue Pressure Injury?
Non-blanchable deep red, maroon, or purple discoloration, skin appears intact
What are prevention strategies for pressure injuries?
Educate patient & family, maintain nutrition and hydration, minimize moisture, frequent turning, keep devices off skin
What are treatment options for pressure injuries?
Keep area clean and dry, cover with non-adhesive dressing, irrigate as needed, debridement as indicated