Week 7 - Health and mortality
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
What is health?
A state of complete physical, mental and social well-being and not merely the absence of disease or infirmity.
What determines health at the population level?
Determined by:
Conditions of birth
Environment of upbringing
Work and housing conditions
Ageing context
Genetics matter at the individual level
Population health largely shaped by social, economic and cultural factors
Measurements of Population health - Life expectancy (LE)?
most used population health indicator
The average number of years a person is expected to live based on current mortality rates (period measure, not a real cohort prediction).
Measurements of Population health - Healthy life expectancy (HLE)?
The average number of years lived in good health, combining mortality and morbidity.
KEY distinction between LE and HLE: living longer does not equal living healthier
3 Theories of Population Health Change (how we will spend the end of our lives healthy or sick as we live longer)
Compression of morbidity (James F. Fries, 1983): HLE increases, resulting in a short, intense period of chronic disease immediately before death. (occurs when HLE increases faster than LE). Assumes:
Successful prevention of chronic diseases
Removal of major risk factors e.g. eliminating major risks—like smoking, obesity, and physical inactivity
Expansion of morbidity (Ernest Gruenberg, 1977): longer life = the more time spent with chronic illness so increase LE DNE increase HLE
Dynamic equilibrium (Kenneth Manton, 1985): while we are living longer with chronic diseases, the severity of those diseases is decreasing
What is the epidemiologic transition?
The shift from infectious to chronic diseases as main causes of death during development (Abdel Omran, 1971).
What are the three stages of the epidemiologic transition?
Pestilence & famine — high mortality, low life expectancy
Receding pandemics — declining infectious disease
Degenerative diseases — chronic illness dominates (modern UK stage)
What is McKeown’s thesis?
Mortality decline was mainly due to social improvements (nutrition, sanitation, economic growth), not medical advances (Thomas McKeown). Evidence: TB declined before antibiotics.
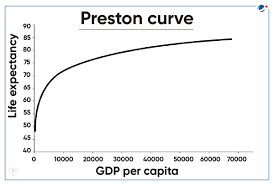
What does the Preston Curve show?
The relationship between national income and life expectancy (Samuel H. Preston, 1975).
Initially, as developing countries’s national income rises, life expectancy increases significantly
eventual plateau → diminishing returns (further wealth yields smaller gains in longeitvity as human life span cannot stretch indefinitely)
Fundamental Cause and Primary Mechanism of health - Socioeconomic Position (SEP)
It determines an individual's position on the societal hierarchy Defined by:
Income
Wealth
Education
Occupational class
Housing tenure
→ directly dictates their exposure to all other Social Determinants (like housing and stress) and their risk of Mortality and Morbidity.
higher SEP correlates with higher life expectancy, lower mortality and lower morbidity
What are social determinants of health?
Non-medical factors shaping health: income, education, housing, work, environment.
The actual conditions (Housing, Environment, Stress) that SEP controls. High SEP buys you a better environment; low SEP exposes you to chronic stress.
Key insight: most health improvements occur outside healthcare systems.
What are health inequalities?
Systematic, avoidable, and unjust differences in health outcomes between social groups → strongly linked to socioeconomic position (SEP).
What are the four main explanations for health inequalities?
Cultural–behavioural: unhealthy lifestyles more common in lower SEP
Materialist: unequal access to resources and living conditions
Psychosocial: inequality → stress → worse health (Richard Wilkinson & Kate Pickett, 2009)
Health selection: poor health leads to downward mobility e.g. if you are chronically ill or disabled, you might lose your job, drop out of school, or have high medical costs.
What did major UK reports conclude about health inequality?
Black Report: inequalities persist due to economic inequality
Marmot Review (Michael Marmot): health follows a social gradient (“Fair Society, Healthy Lives”)
What do UK vs USA comparisons show about health inequality?
The USA has worse average health and greater inequality → wider gap between rich and poor; in some cases, richest USA ≈ poorest UK.
What did COVID-19 reveal about population health?
It exposed and intensified existing structural inequalities, showing health outcomes are strongly shaped by SEP, age, and life-course conditions. e.g. Low-income and informal workers (e.g., in retail, transport, or cleaning) often faced a choice between risking infection or losing their livelihood.