NR507 Advanced Pathophysiology With 100% correct answers + rationales 2026
1/97
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
98 Terms
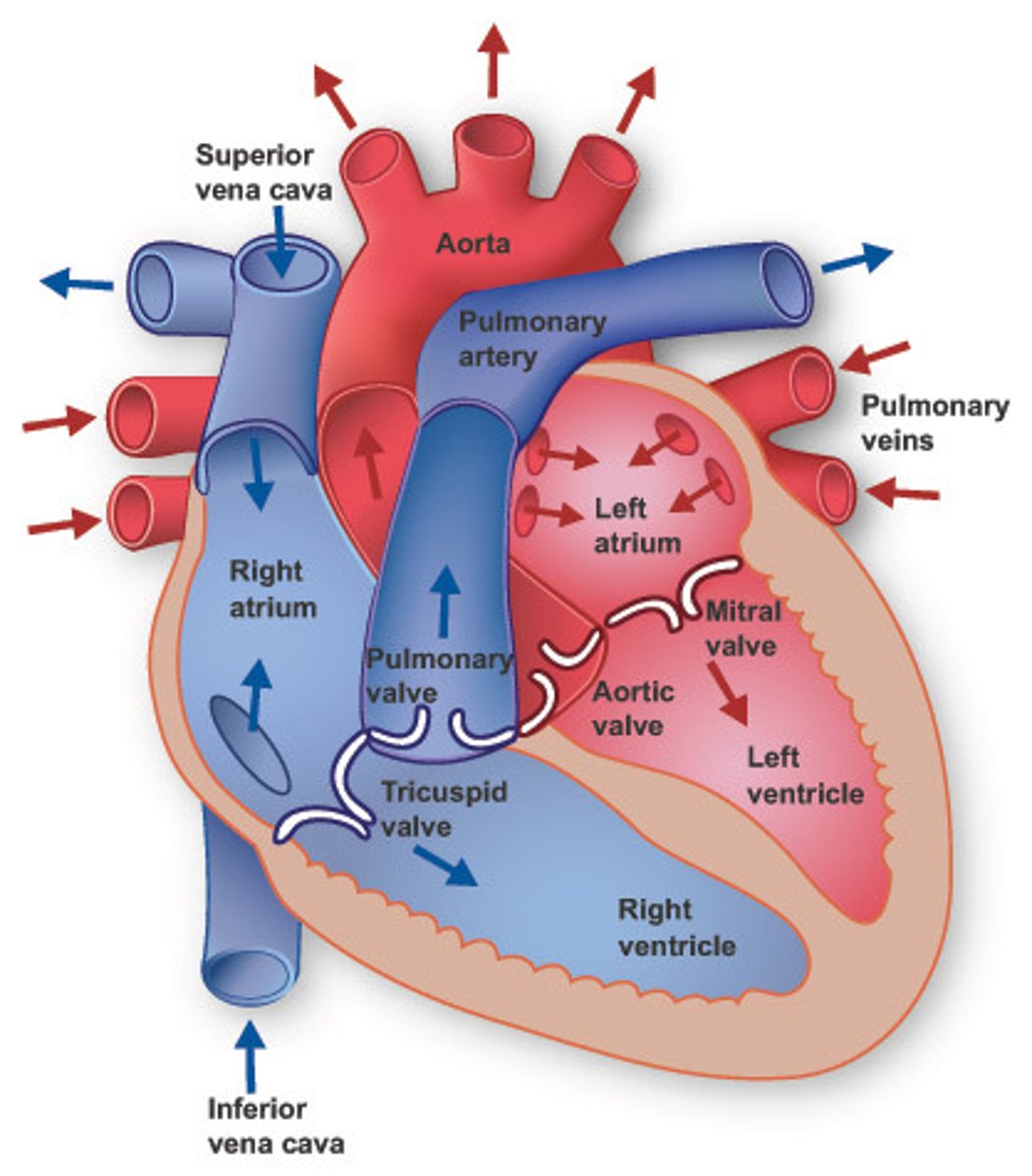
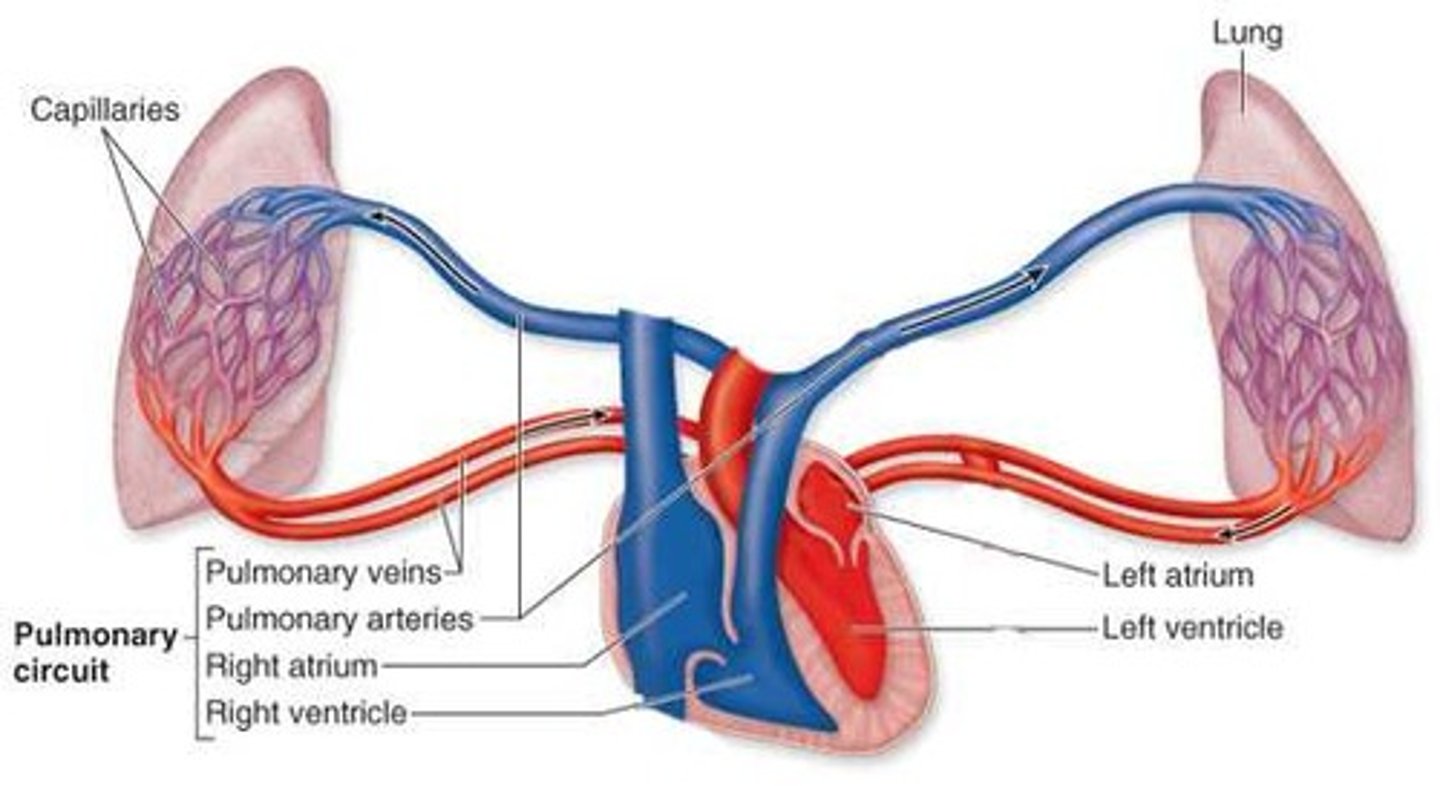
How does blood flow through the heart?
Deoxygenated venous blood → Sup. Vena Cava → Right Atrium →Tricuspid (AV) →Empties into R. Ventricle (& it contracts) → Blood ejected through Pulmonary Valve → Pulmonary Artery → Lungs to be Oxygenated → Pulmonary Veins → L. Atrium → Mitral (AV) → L. Ventricle (pumps with each contraction) → Aortic Valve → Aorta → Body
What is systole?
Contraction of the heart which pumps blood
Diastole
Relaxation of the heart
What produces S1 and S2 sound?
closing of the heart valves
What produces S1?
The mitral and tricuspid valves which close in systole
What produces S2 sound?
The closing of the aortic and pulmonic valves in diastole
What is cardiac output?
the volume of blood pumped out by each ventricle per minute
What is stroke volume?
amount of blood pumped out by each ventricle with contraction
What determines cardiac output?
stroke volume and heart rate
What is preload?
the degree of stretch on the heart before it contracts, related to ventricular filling, end diastolic pressure, amount of blood entering the ventricle during diastole
What is afterload?
resistance left ventricle must overcome to circulate blood
What is contractility?
Normal ability of muscle to contract at a given force for a given stretch. It is independent of preload/afterload
Will sustained tachycardia result in increased or decreased stroke volume?
Decreased
What conditions can result in decreased contractility?
Ischemia, acidosis, cardiomyopathy
What can cause increase afterload?
HTN, pulmonary disease, damage to the aortic valve
What has the most immediate effect on afterload?
HTN
Why would hemorrhaging cause decreased afterload?
Decreased volume of blood creates less resistance
What does increased preload do to stroke volume?
Increases stroke volume, over time the body will be unable to compensate however
What can cause a decreased preload?
Hemorrhage, dehydration...anything that causes reduced blood volume
What side of the heart is affected by cor-pulmonale?
Right (AKA Right sided HF)
What is cor-pulmonale?
is defined as right ventricular hypertrophy with eventual RV failure resulting from pulmonary HTN, secondary to pulmonary disease. Causes dilation (stretching) of the right ventricle causes a back up of blood flow, and hypertrophy of cardiac cells
What conditions could cause cor pulmonale?
COPD, PE, Pulmonary fibrosis, sleep apnea, myasthenia gravis, polio
What are causes of heart failure?
CAD, HTN, Cardiomyopathy, faulty heart valves
Explain how systemic HTN can lead to heart failure?
HTN causes increased LV preload which increases LA preload causing pulmonary edema

What makes up the pulmonary anatomy?
nose->pharynx->larynx->trachea->bronchi->bronchioles-->alveoli
What is ventilation?
The action of inhaling and exhaling
What is perfusion?
the ability of the lungs to perform gas exchange at the alveolar-capillary level moving blood into and out of the capillary cells
What causes intrinsic asthma?
Something internal, non-allergic factors (anxiety, chemicals, airborne irritants, exercise, GERD, obesity
What causes extrinsic asthma?
Triggered by chronic allergic reaction (mold, pollen, dust mites, pet dander)
What are signs and symptoms of asthma?
wheezing, shortness of breath, chest tightness, and coughing
What are treatment options for asthma?
Beta2-agonists and anticholinergics which block acetylcholine binding to promote bronchodilation
What are signs and symptoms of chronic bronchitis?
Productive cough, copious sputum, dyspnea, wheezing, rhonchi, cyanosis of skin and membranes, persists for at least three months consecutively for two successive years
Where does the damage occur for chronic bronchitis?
the airways (not alveoli)
What causes chronic bronchitis?
inflammatory cells activated in the bronchioles d/t irritants such as chronic smoke inhalation. The lamina propria which is a thin layer of connective tissue lining mucous membranes becomes inflamed and causes mucus secretion.
What are long term effects of obstructive pulmonary disease?
Secondary polycythemia, alveolar hyperinflation
What is secondary polycythemia?
A condition in which RBC numbers increase in response to hypoxic conditions: living at higher altitudes, smoking, chronic low O2 conditions like COPD (a lung disorder). This can lead to a blood clot
What is alveolar hyperinflation?
Due to decreased ability to exhale excess air becomes trapped in alveoli which causes an expanded thorax resulting in barrel chest and flat diaphragm
What medications are used to treat chronic bronchitis?
Antitussives, expectorants, bronchodilators, systemic corticosteroids, antibiotics, ensure proper immunizations
What is a nephron?
functional unit of the kidney for filtration
What components make up a nephron?
Bowman's capsule (Glomerular capsule) and tubule system consisting of proximal convoluted tubule, Loop of Henle, distal convoluted tubule and collecting duct
What four processes occur in the nephron during the formation of urine?
filtration, reabsorption, secretion and excretion
Describe glomerular filtration
blood pressure forces water and dissolved plasma components through the glomerulus and Bowman's capsule into the renal tubule system
Describe tubular reabsorption
selectively returns 99% of substances from filtrate to blood in renal tubules and collecting ducts
What is essential for renal filtration to occur?
blood (hydrostatic) pressure
What is reabsorption in relation to the renal system?
the back movement of content from the glomerular filtrate into the blood
What is excretion in relation to the renal system?
Elimination from the body (i.e. drugs)
What is secretion in relation to the renal system?
tubular secretion is the movement of material (urea, H+,) FROM the bloodstream of the peritubular capillaries INTO the filtrate of the nephron tubule system
What are the three types of acute renal failure?
Pre-renal
Intra-renal
Post-renal
What is glomerulonephritis?
-loss of kidney function, causes elevated BUN/creatinine levels d/t decreased GFR
What is pre-renal failure?
-Most common form of renal failure
-Damage occurs BEFORE kidneys d/t reduced blood flow
-less blood flow to the glomerulus
-Decreased GFR causes decreased blood flow
What are some causes of pre-renal failure?
-Volume depletion (too much diuretic)
-Polyuria s/t DM
-Vomiting/diarrhea
-skin loss of fluid s/t burn or hemorrhage
What is one of the bodies first responses to decreased GFR in regards to pre-renal failure?
Activation of the renin-angiotensin-aldosterone system
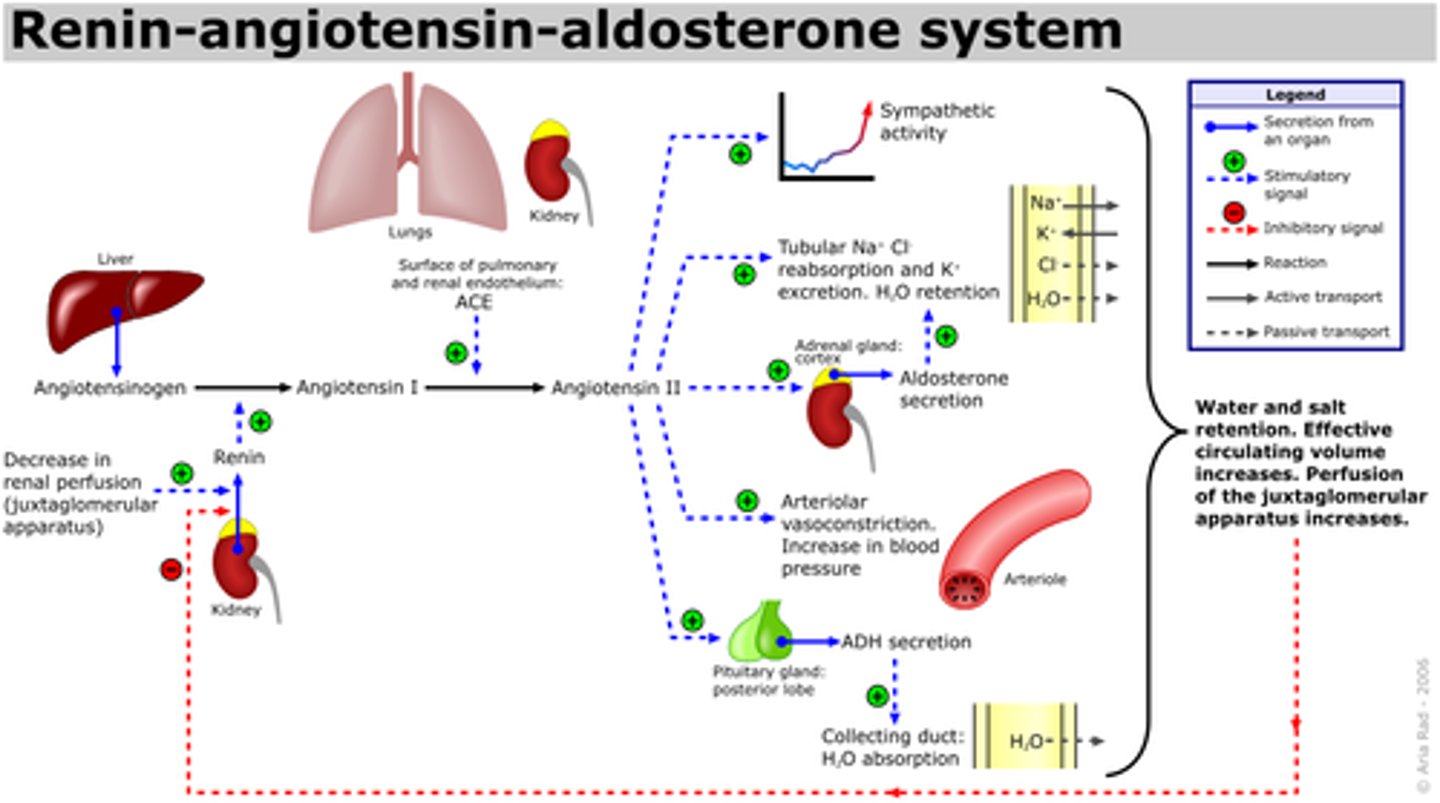
How does the renin-angiotensin aldosterone system increase blood volume?
Causes sodium and water to be reabsorbed as aldosterone acts in the distal tubule to take up more sodium and water to maintain pressure
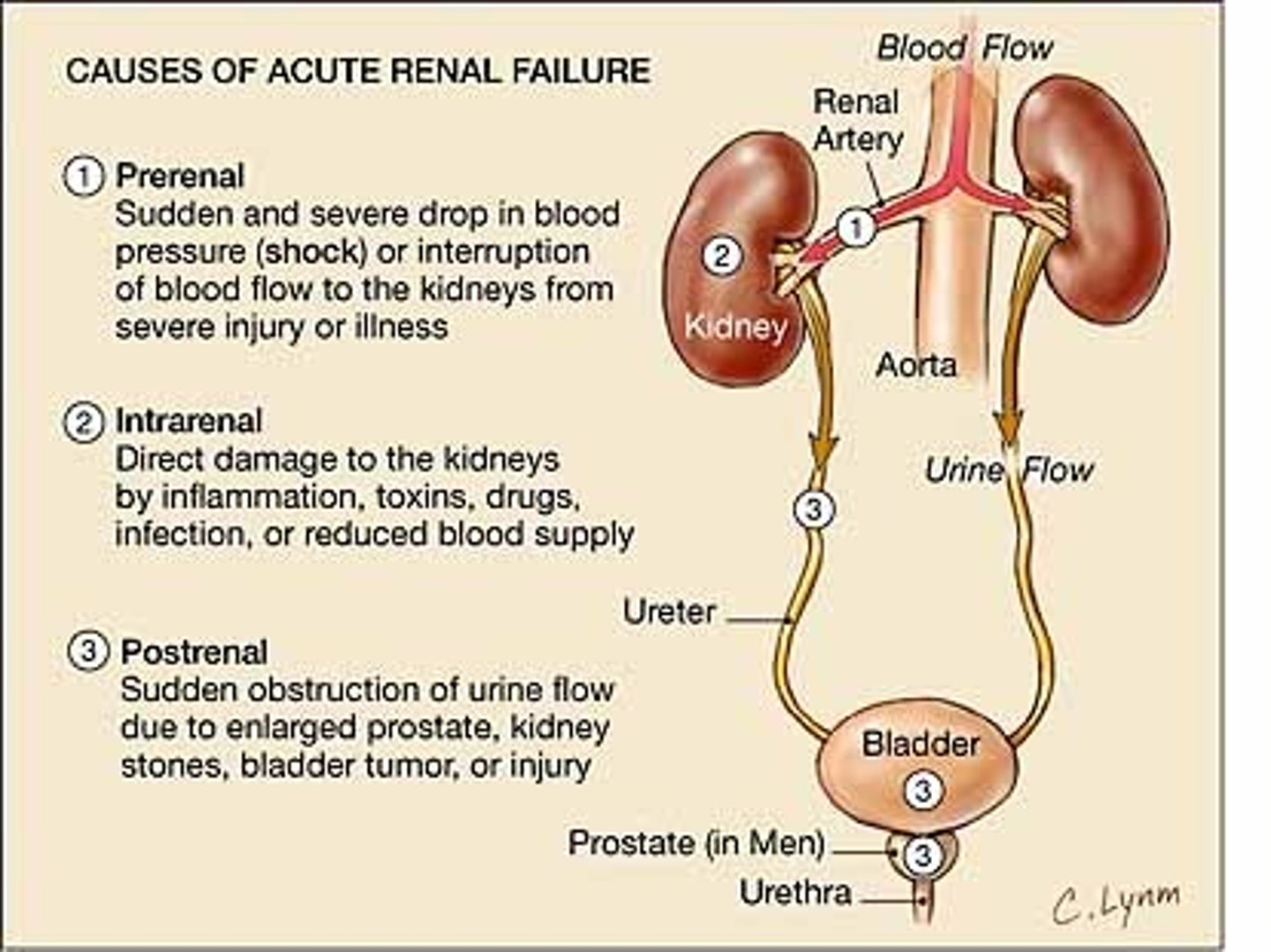
What is intra-renal kidney failure?
damage which occurs IN the kidney d/t some type of damage to the glomerulus, renal tubules, renal interstitium, or renal vasculature
If intra-renal failure occurs at the tubules what is a result?
Since one of the functions of the tubules is to reabsorb sodium and water, their would be increase loss of sodium and water loss in the urine
What is post-renal failure?
Damage in the collecting ducts, ureter, bladder, or urethra d/t some type of obstruction
What is contrast-induced nephropathy?
A complication from angiographic procedures result from contrast
Who is most at risk for experiencing contrast-induced nephropathy?
Those with DM as they are more likely to already have CKD
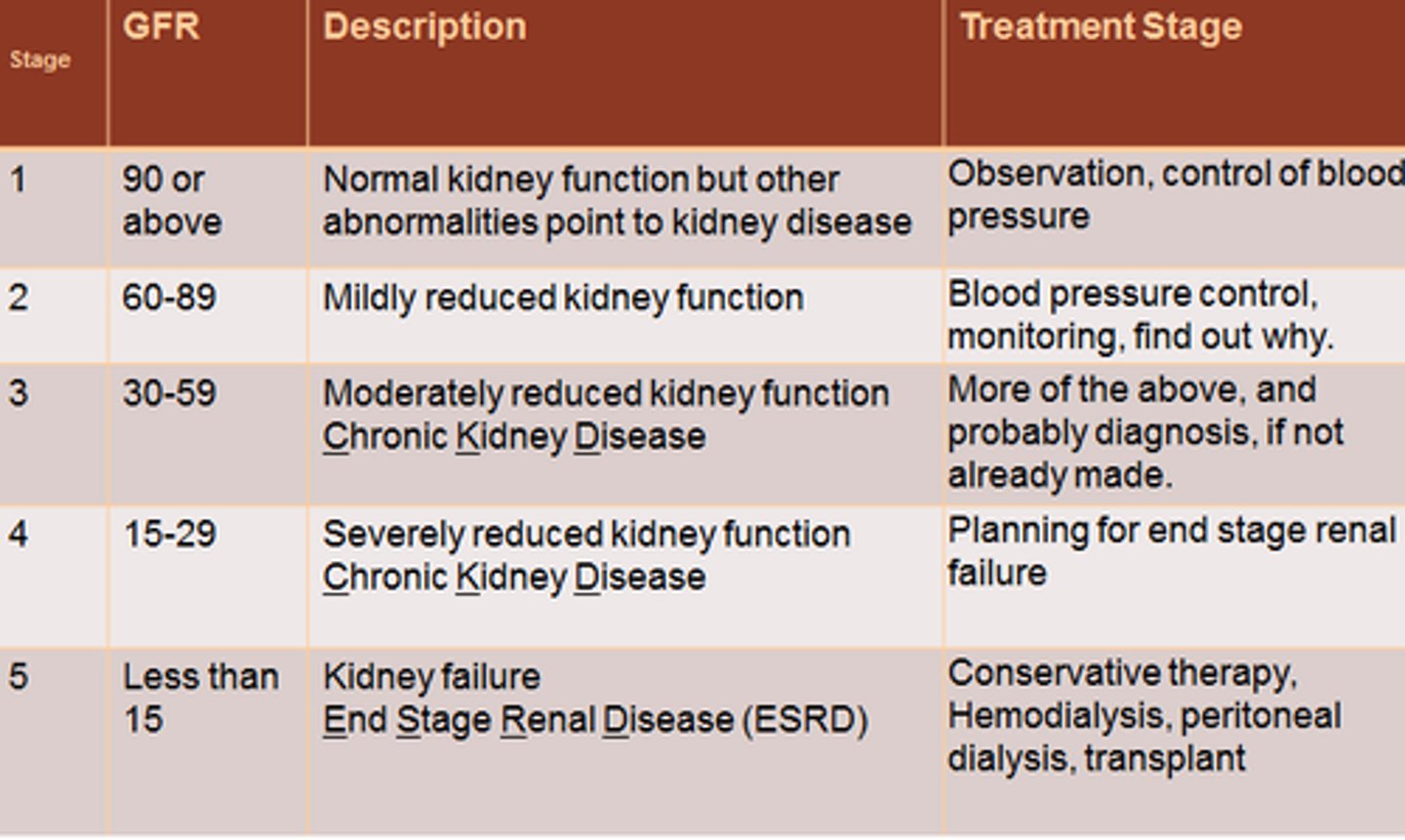
What is chronic kidney disease?
long term, permanent decline of renal function
What is end stage renal disease?
-the final stage of CKD
-number one cause is DM combined with HTN
-pt. completely dependent on dialysis
What is vesicoureteral reflux?
retrograde projection of urine from bladder to the ureters and kidneys
caused by insufficient tunneling of the ureters into submucosal bladder tissue, leading to ineffective restriction of retrograde urine flow during bladder contraction
may also be due to posterior urethral valves, urethral or meatal stenosis, or a neurogenic bladder
What is the average lifespan of RBC?
120 days (4 months)
What two ways can anemias be classified?
By size of RBC and color of RBC
How would you describe the cells of microcytic anemia?
Smaller than normal (MCV<80fl)
How would you describe cells of macrocytic anemia?
Larger than normal (MCV>100fl)
How would you describe cells of normocytic anemia?
Normal in size (MCV 80-99)
What are symptoms of anemia?
-severe fatigue
-pallor
-weakness
-dyspnea
-dizziness
How would you describe a hypochromic RBC?
-less Hb than normal
-pale in color (MCHC low)
How would you describe a hyperchromic RBC?
-More Hb than normal
-Cell has a dark hue or more red than normal
-MCHC high
How would you describe a normochromic RBC?
-RBC has normal amount of Hb
-RBC is normal in color (MCHC normal)
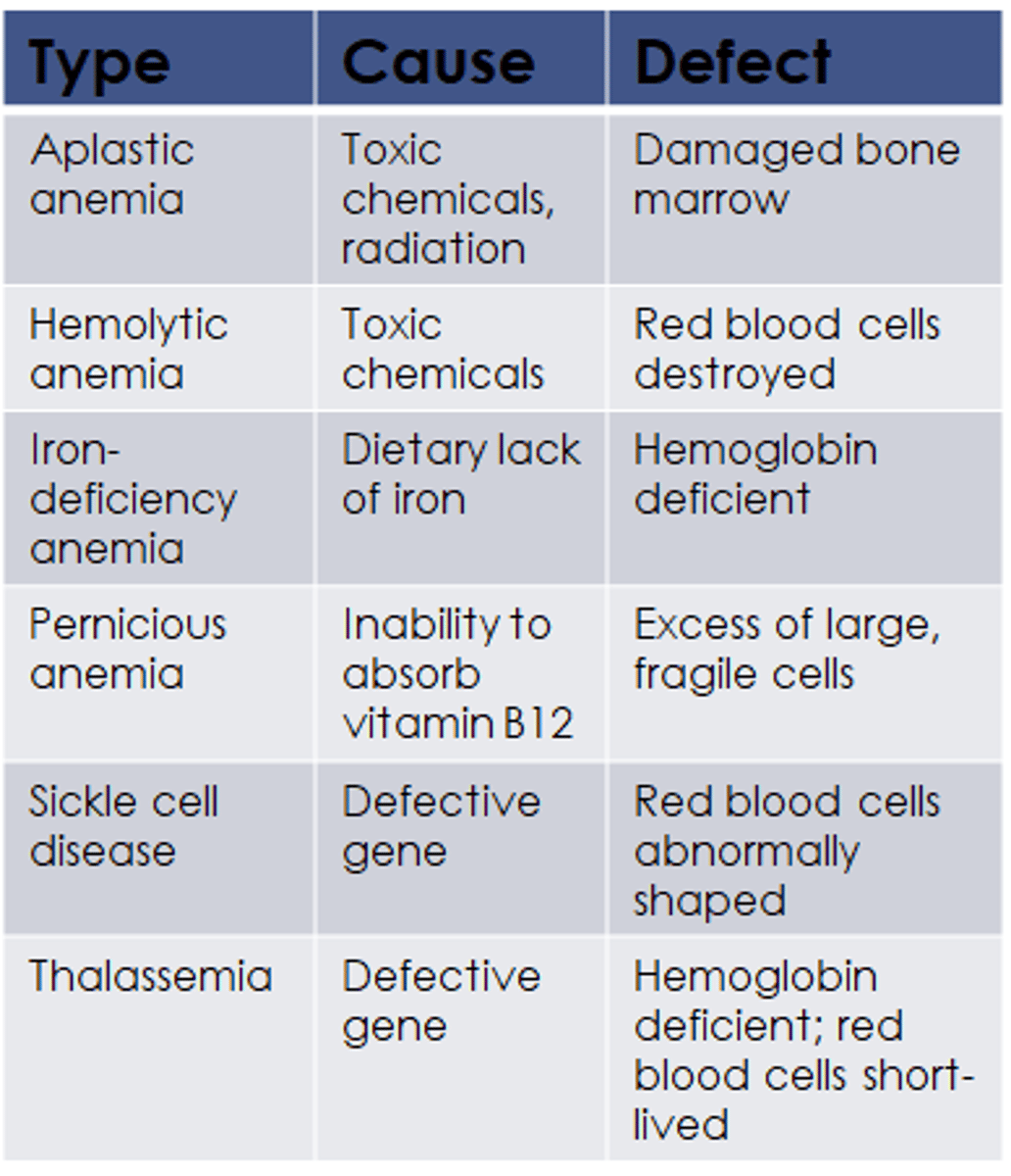
What type of anemia is iron deficiency anemia?
microcytic hypochromic anemia
What causes iron deficiency anemia?
-caused by Hb synthesis disorders
-Fe deficiency
-decreased dietary intake of iron
-occult bleeding (post-partum, colitis, cirrhosis, GI ulcers)
What would an NP order to know the body's total iron stores?
Ferritin level
What does a low ferritin level mean?
anemia
What causes pernicious anemia?
Vitamin B12 deficiency
What is a sign of pernicious anemia?
-Peripheral neuropathy *
-fatigue
-dyspnea
What are risk factors of pernicious anemia?
-Older adults
-H. Pylori infection
-Affects Vit. B-12 absorption
What is hemolytic anemia?
when the RBC have a short life span and there is increased destruction of the RBC
What causes hemolytic anemia?
-mismatched blood transfusion
-autoantibodies against erythrocytes that the immune system perceives as an antigen and then the body attacks it
-allergic reaction to a drug which causes drug-induced hemolytic anemia
What is thalassemia?
a form of inherited autosomal recessive blood disorder characterized by abnormal formation of hemoglobin. The abnormal hemoglobin formed results in improper oxygen transport and destruction of red blood cells.
What is sickle cell anemia?
A mutation in a gene causes a problem making the hemoglobin of the red blood cells., A genetic disorder causing red blood cells to be rod/sickle shaped. This causes them to get stuck in capillaries and the bodies cells become deprived of oxygen
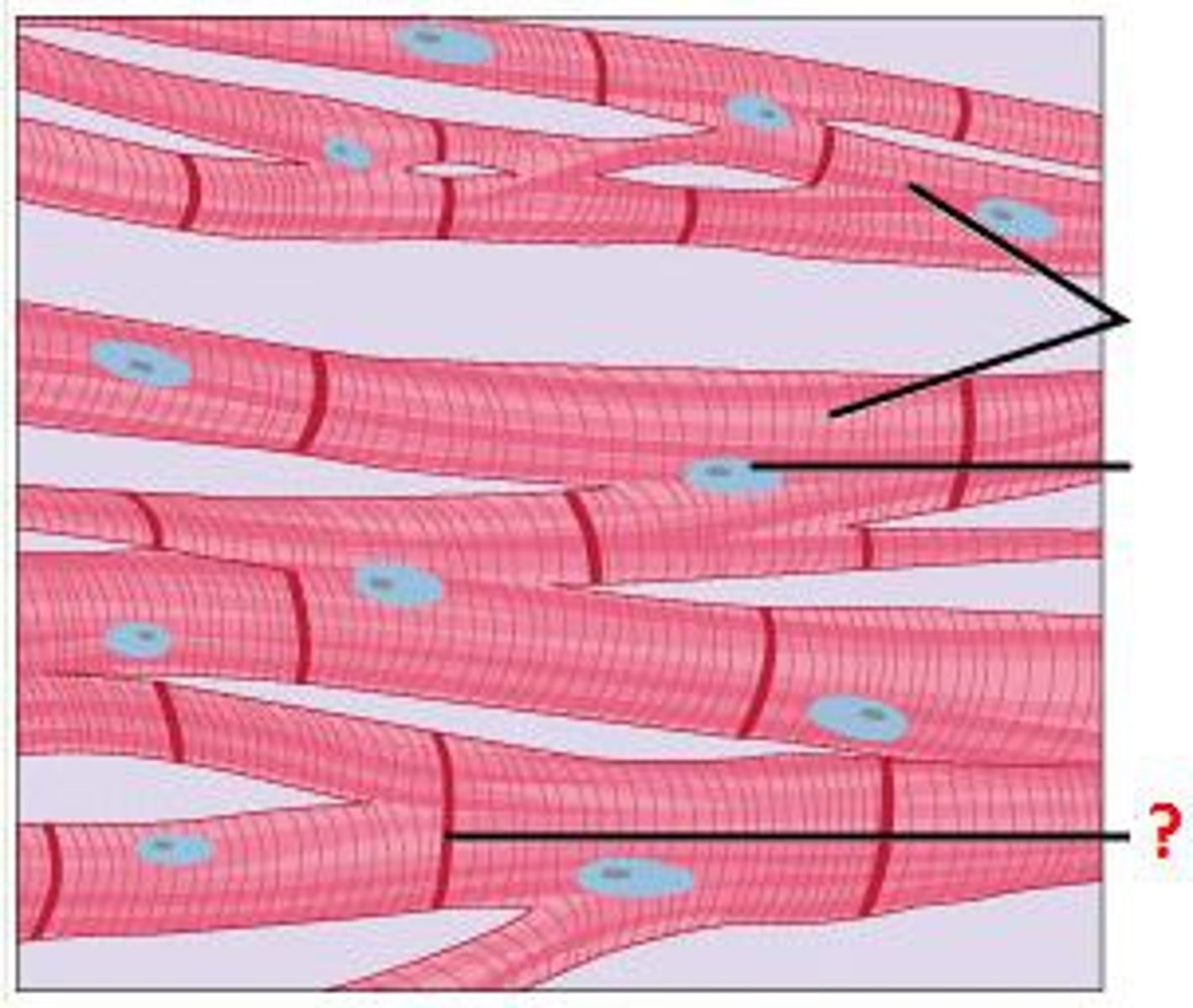
How are muscle cells linked together?
Intercalated disks which are a latticework of channels that allow the cells to function as a single unit (syncytium)
What proteins are arranged in contractile units of the heart muscles called sarcomeres?
actin and myosin
What is the sliding filament theory?
theory that actin filaments slide toward each other during muscle contraction, while the myosin filaments are still
What is end diastolic volume (EDV)?
The amount of blood in the ventricles before contraction (systole)
What is end-systolic volume (ESV)?
Amount of blood left in ventricle after systole (contraction)
What is ejection fraction?
-stroke volume divided by end diastolic volume
-expressed as percentage to signify how much blood is pumped out by left ventricle with contraction
How would you find CO?
SVxHR=CO
What type of relationship does HR and stroke volume have?
Inverse
-decrease in HR-> longer fill time->increase stroke volume
-increase in HR->shorter fill time->decreased stroke volume
What is the Frank-Starling Law?
The greater the stretch on the myocardial fibers, the greater the force with which they will contract. (ex. stretching a rubber band).
What is Laplace's law?
When the heart muscle is weak, ventricles are hypertrophied and/or pulmonary or systemic blood pressure is high