Geriatric Questions from Class (lecture and kahoot)
1/57
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
58 Terms
Which of the following is a normal change in the aging skin that predisposes individuals to pressure injuries?
A. Increased elastin
B. Increased vascularity
C. Increased dermal-epidermal turnover
D. Loss of subcutaneous fat
D. Loss of subcutaneous fat
Which PI stage is described as full thickness skin loss with damage to muscle, bone, or supporting structures.
A. Stage I
B. Stage II
C. Stage III
D. Stage IV
D. Stage IV
Which PI stage is described as intact skin with a localized area of non-blanchable erythema?
A. Stage I
B. Stage II
C. Stage III
D. Stage IV
A. Stage I
Which PI stage is described as a localized area of tissue necrosis covered with slough or eschar?
A. Stage III
B. Stage IV
C. Unstageable
D. Deep Tissue Pressure Injury
C. Unstageable
Which word best describes moist avascular tissue that adheres to the wound bed; can be white, yellow, tan or green?
A. Eschar
B. Granulation
C. Epithelium
D. Slough
D. Slough
Which type of exudate is thin, pale red to pink, and watery in presentation?
A. Serous
B. Serosanguinous
C. Purulent
D. Seropurulent
B. Serosanguinous
Which stage of pressure injuries heal by tissue regeneration?
A. Stage IV
B. Unstageable
C. Deep Tissue Pressure Injuries
D. Stage II
D. Stage II
Which stage of healing is considered the scarring period?
A. Hemostasis
B. Inflammatory
C. Proliferation
D. Maturation
D. Maturation
Which nutritional plan should be encouraged to optimize wound healing as long as there are no medical contraindications?
A. Encourage high fat, calorie-dense foods and fluids
B. Encourage high protein, calorie-dense foods and fluids
C. Encourage high carbohydrate, calorie-dense foods and fluids
D. Diet has no effect on wound healing, keep wound clean and avoid pressure
B. Encourage high protein, calorie-dense foods and fluids
What is the recommended solution to cleanse and optimize pressure injury wound environment?
A. Saline
B. Betadine
C. Hydrogen Peroxide
D. Chlorhexidine
A. Saline
Which form of dizziness is best described as a rotational sensation?
A. Disequilibrium
B. Pre-syncope
C. Lightheadedness
D. Vertigo
D. Vertigo
Which below is the most common cause of vertigo?
A. Ototoxic medications
B. Benign paroxysmal positional vertigo (BPPV)
C. Acoustic neuromas
D. Meniere's disease
B. Benign paroxysmal positional vertigo (BPPV)
Muffled hearing loss, tinnitus, a feeling of pressure in the ear, and dizziness is associated with which condition?
A. Benign paroxysmal positional vertigo (BPPV)
B. Acoustic neuromas
C. Perilymph fistulas
D. Meniere's disease
D. Meniere's disease
Which test is most useful for the diagnosis of Benign paroxysmal positional vertigo (BPPV)?
A. Epley’s maneuver
B. CT of the brain
C. Dix-Hallpike maneuver
D. Tilt-table test
C. Dix-Hallpike maneuver
What is a recommended initial treatment for Meniere's disease?
A. Epley’s maneuver
B. Low dose aspirin
C. Vitamin B12
D. Diuretics
D. Diuretics
Which class of medications are most commonly inplicated with dizziness?
A. Antihypertensive medications
B. Antihistamine medications
C. Antibiotic medications
D. Antiemetic medications
A. Antihypertensive medications
A drop in systolic BP > 20mmHg occuring 1-2 hours after eating is associated with which condition?
A. Orthostatic hypotension
B. Neurally mediated hypotension
C. Geriatric hypotension
D. Post-prandial hypotension
D. Post-prandial hypotension
Which of the following is associated with normal aging and makes the elderly more prone to syncope?
A. Increased baroreflex control of heart rate
B. Decreased sensitivity to dehydration
C. Decreased baroreflex control of arterial vasoconstriction
D. Decrease sensitivity to vasodilator drugs
C. Decreased baroreflex control of arterial vasoconstriction
What is the most common treatment used for bradyarrhythmia induced syncope?
A. Pacemaker
B. Electrophysiology ablation
C. Implanted defibrillator
D. Medical therapy
A. Pacemaker
Cataracts and macular degeneration are most associated with which type of dizziness?
A. Disequilibrium
B. Pre-syncope
C. Vertigo
D. Lightheadedness
A. Disequilibrium
Which type of urinary incontinence is described as the leakage of urine along with or before the need to void?
A. Stress
B. Urge
C. Overflow
D. Functional
B. Urge
Which is the best initial treatment for a patient that is experiencing urge incontinence?
A. Bladder training
B. Indwelling urinary catheter
C. Adult diapers
D. Prescribe an antimuscarinic agent
A. Bladder training
Which type of UI is described as leakage of urine with intra- abdominal pressure in the absence of bladder contraction?
A. Urge
B. Overflow
C. Stress
D. Functional
C. Stress
Which type of UI would most likely present in men that complain of nocturia, hesitancy and a weakened urinary stream?
A. Stress
B. Urge
C. Functional
D. Overflow
D. Overflow
Physically unable to timely toilet themself despite intact storage and emptying function is assoc with which type of UI?
A. Urge
B. Stress
C. Functional
D. Overflow
C. Functional
Which post void residual is associated with inadequate emptying?
A. > 25 ml
B. > 50 ml
C. > 100 ml
D. > 200ml
D. > 200ml
What type of behavioral bladder training is best for indiviuals with cognitive impairment?
A. Prompted voiding
B. Pelvic muscle exercises
C. Urgency suppression
D. Biofeedback-assisted training
A. Prompted voiding
Which of the following is true about antimuscarinic agents used for urge urinary incontinence?
A. Sialorrhea is a common side effect
B. Increase functional bladder volume
C. Increase micturition frequency
D. Efficacy varies greatly across agents
B. Increase functional bladder volume
Indwelling catheters should be reserved for which situation?
A. Short term decompression of acute urinary retention
B. Surgically remediable urinary retention
C. Patients with constipation
D. Individuals with stress incontinence that have failed pelvic floor training
A. Short term decompression of acute urinary retention
What survival prognosis is required to be hospice eligible?
A. < 12 months
B. < 6 months
C. < 3 months
D. < 9 months
B. < 6 months
Which protocol provides a framework for presenting distressing information to a patient?
A. SORRY
B. SPURS
C. SPIKES
D. SUDDEN
C. SPIKES
Which answer below best describes the palliative care model?
A. Patient-primary care provider centered care
B. Patient-community centered care
C. Patient-spiritual centered care
D. Patient-family centered care
D. Patient-family centered care
Which of the following is an appropriate diagnosis for hospice care?
A. Class II NYHA congested heart failure
B. HIV diagnosis with an undetectable viral load
C. Advanced alcoholic cirrhosis
D. BMI < 20
C. Advanced alcoholic cirrhosis
Which medication would most likely be recommended for a hospice patient in moderate/severe pain?
A. Tramadol
B. Acetaminophen
C. Ibuprofen
D. Morphine
D. Morphine
Which medication would best manage nausea and vomiting in the palliative care patient?
A. Zantac
B. Senna
C. Zofran
D. Metamucil
C. Zofran
Which medication can contribute to developing a bowel obstruction in patients taking opioids?
A. Metamucil
B. Lactulose
C. Bisacodyl
D. Dulcolax
A. Metamucil
Which end of life trajectory is most commonly seen in an individual with organ failure?
A. Dwindling decline
B. Rapid decline following a high level of function
C. Fluctuating decline
D. No observed decline before death
C. Fluctuating decline
The FAST score helps follow the progression of which disease process?
A. Liver disease
B. Alzheimer’s disease
C. Congested heart failure
D. Chronic obstructive pulmonary disease
B. Alzheimer's disease
Which of the following provides the best method for establishing a diagnosis of delirium in a post operative patient?
A. Confusion Assessment Method
B. Depression Scale Screening Test
C. Toxicology Screen
D. Metabolic screen
A. Confusion Assessment Method
Antalgic gait is best described as which of the following?
A. Outward swing of leg in a semicircle from the hip
B. An acceleration of gait
C. Hyperextension of the knee
D. Pain-induced limp with shortened phase of gait on painful side
D. Pain-induced limp with shortened phase of gait on painful side
Dental caries are commonly associated with medications that cause which side effect?
A. Nausea and vomiting
B. Dizziness
C. Xerostomia
D. Dysphagia
C. Xerostomia
After removal of dentures, palate cobblestoning and erythema is seen. These findings are consistent with which below?
A. Denture stomatitis
B. Dental abscess
C. Angular cheilitis
D. Squamous Cell Carcinoma
A. Denture stomatitis
Denture stomatitis is commonly associated with which organism below?
A. Staphlococcus aureus
B. Streptococcus pneumoniae
C. Pseudomonas aeruginosa
D. Candida albicans
D. Candida albicans
Oral care protocols led to a reduction in ventilator associated pneumonias. What percent reduction was documented?
A. 50%
B. 70%
C. 30%
D. 90%
D. 90%
What is the best recommendation for managing xerostomia?
A. Frequently suck on hard mints and candies
B. Drink small sips of water during the day and with meals
C. Drink small sips of apple juice during the day and with meals
D. Drink small sips of tea during the day and with meals
B. Drink small sips of water during the day and with meals
72 year old female patient w/ worsening UI, brought on by coughing, sneezing, or bearing down.
Had been using light pad & recently switched to thicker.
what is the best first step in treatment?
pelvic floor training (Kegels) & Behavioral therapy
Patient w/ Parkinson's disease, nursing home, w/ worsening urinary incontinence.
She is using incontinence pads & is developing several yeast infections in the groin.
What is the most appropriate recommendations? (only proven effective in Cognitively impaired)
Prompted voiding.
83 year old man comes to clinic d/t urinary incontinence.
urine leaks when he coughs or bends, has uncomfortable urgency.
Difficulty w/ starting to void, stopping & restarting midstream, weak stream, frequency, & urgency. (&nocturia). C/o Abdominal fullness & suprapubic discomfort.
not been ill or started new medications. Portable US shows 600mL urine.
What is the most appropriate next step?
Insert foley catheter, if bladder volume confirmed, leave catheter & refer further evaluation.
3 multiple choice options
76 year old woman returns to clinic 1m after starting treatment for stress incontinence.
symptoms mostly unchanged after trial of estradiol ring, & Kegels from a booklet.
Currently taking HCTZ for HTN.
What is the most appropriate next step?
Refer for biofeedback-assisted training pelvic floor muscle.
3 multiple choice options
78 yr old woman comes to office for sx of mixed stress & urinary incontinence. She is most bothered by the urge incontinence.
Generally healthy & cognitively intact. Does not drink caffeinated beverages or take diuretics.
Patient is interested in NON-Pharm therapy and will not consider surgery.
Which of the following is true about combing urge suppression strategies w/ pelvic floor exercises.
Antimuscarinic drug therapy can enhance the effectiveness of behavioural therapy in some patients.
3 multiple choice options
68 year old woman brought to the ED b/c she woke up from an afternoon nap w/ udden onset of rotational vertigo & clumsiness of right arm. She feels world is tilting toward the right.
Unable to walk w/o assistance & has a HA.
hx of HTN, T2DM-insulin dependent, currently on lisinopril, metformin, aspirin.
Direction-changing nystagmus & head thrust are negative.
Difficulty w/ rapid alternating movements right arm, and toe tapping/ heel to shin on right leg.
Which of the following is the most likely diagnosis?
Cerebellar infarct
1 multiple choice option
70 year old man w/ difficulty walking, especially in dark, unable to read street signs during car rides because environment seems to be jumping up & down.
Hx DM, peripheral neuropathy, renal insufficiency.
Recently discharged from hospital for cellulitis, received IV gentamicin & nafcillin.
Reported continuous sense imbalance w/o vertigo. No tinnitus, aural fullness or hearing loss.
Examination normal except wide based gait & + Rombergs.
Which of the following is the most likely cause of patients imbalance?
Aminoglycoside ototoxicity
3 multiple choice options
Which of the following is an age related physiological change that predisposes older adults to syncope?
Reduced baroreflex control of heart rate
3 multiple choice options
75 year old woman comes to office d/t repeat episodes of profound dizziness & syncope, along w/ 2 episodes found on the floor but unaware how she fell.
episodes preceded by prodrome during which she feels warm & diaphoretic & progressively light headed. They are more likely to occur when she has been standing for a long time, such as church services.
HX htn- takes HCTZ.
BP 142/84 supine, 110/70 upright.
HR: 76bpm supine & 80 bpm upright.
no JVD, carotid bruits, lungs clear, delayed carotid upstroke, II/VI murmur @ base. no gallop.
Which of the following is the most appropriate next step?
stop Hydrochlorothiazide
3 multiple choice options
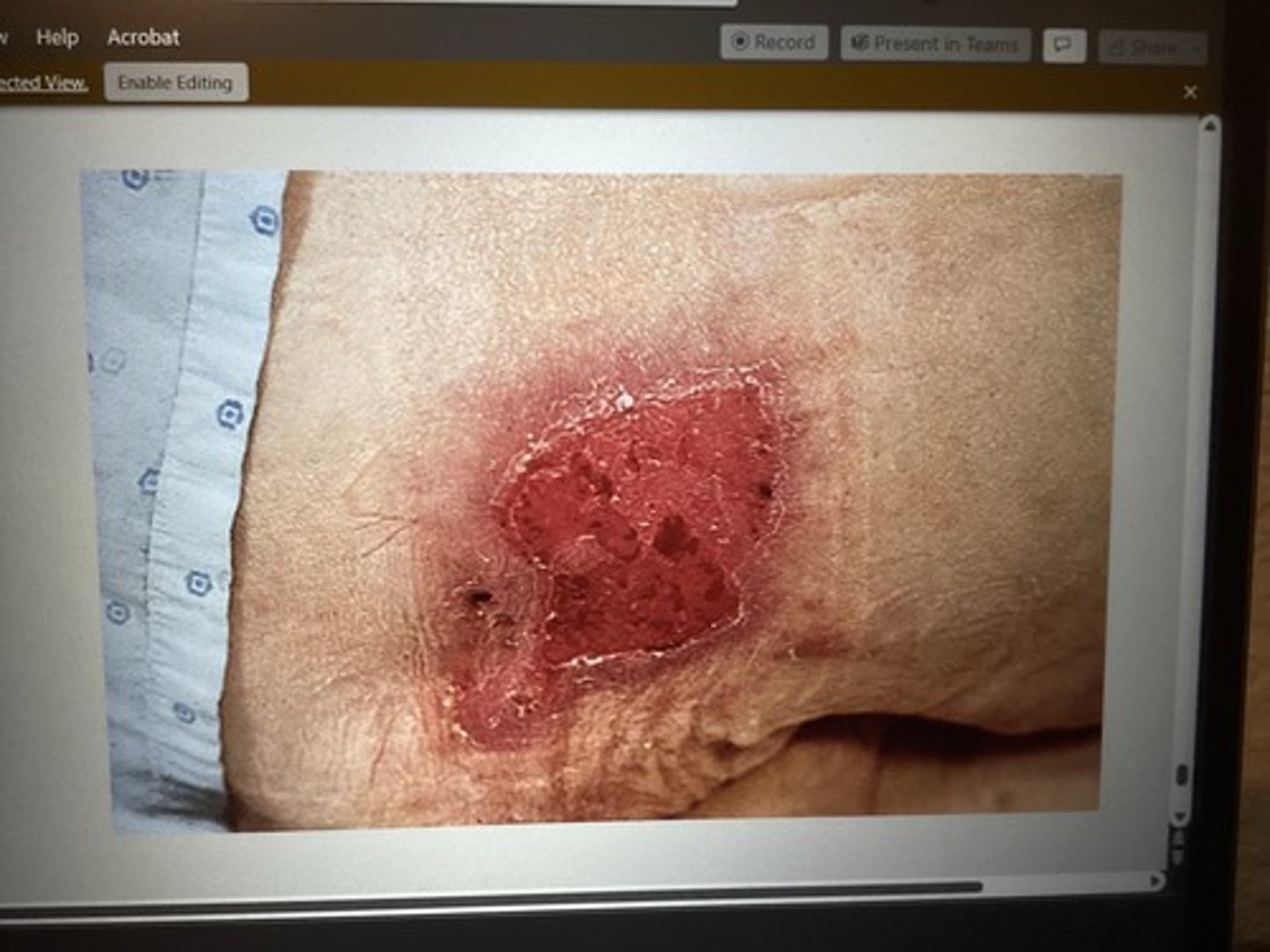
What stage is this pressure ulcer & what will your treatment plan include?
intact skin w/ non blanchable redness of a localized area.
stage 1
Encourage adequate perfusion & protect from further tissue damage & friction.
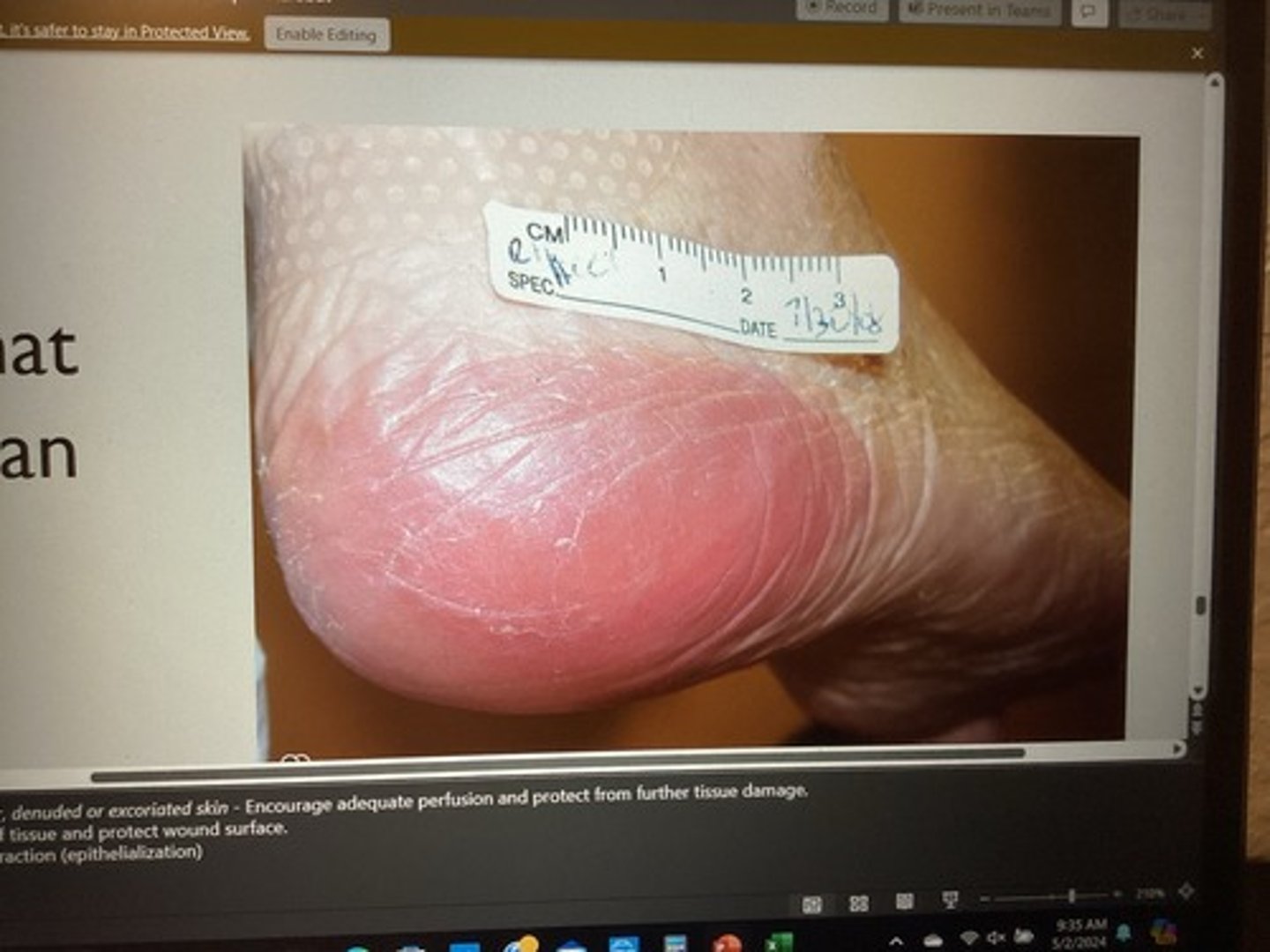
What stage is this pressure ulcer & what will your treatment plan include?
Full thickness skin loss. Subcutaneous fat visible, NO bone, tendon or muscle exposed.
stage 3
Debridement can promote granulation & contraction. (Epithelialization)
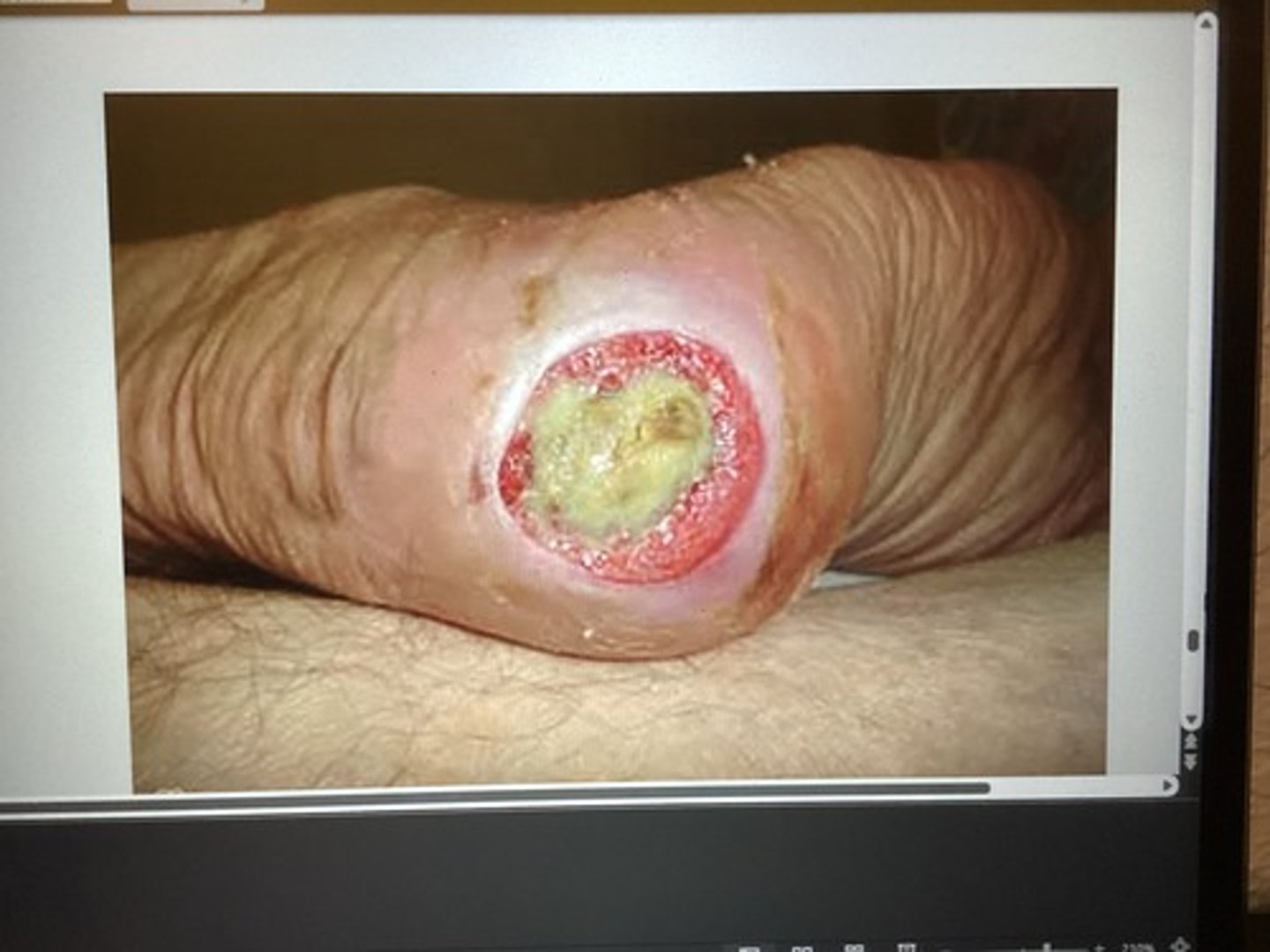
What stage is this pressure ulcer & what will your treatment plan include?
Full thickness skin loss w/ exposed bone, tendon, muscle.
stage 4
More aggressive debridement (surgical) to promote granulation & contraction.
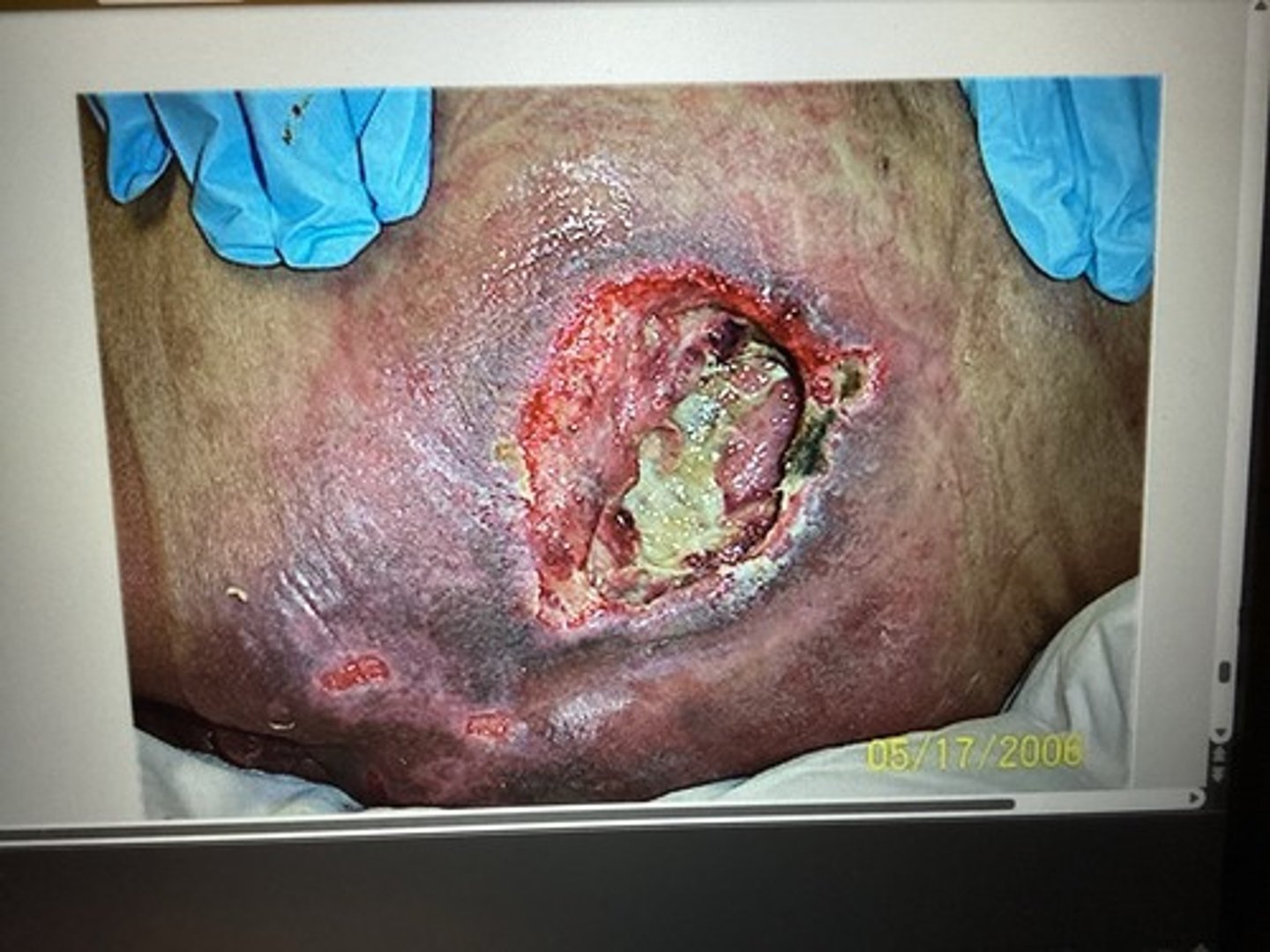
What stage is this pressure ulcer & what will your treatment plan include?
Partial thickness loss of dermis. Presenting as shallow open ulcer w/ red/pink wound base, w/o slough.
stage 2
Encourage regeneration of tissue & protect wound surface.