APK2105C Chapter 13 - The Cardiovascular System - Hauge UF
1/105
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
106 Terms
What is the primary function of the cardiovascular system?
To transport materials to and from cells in the body.
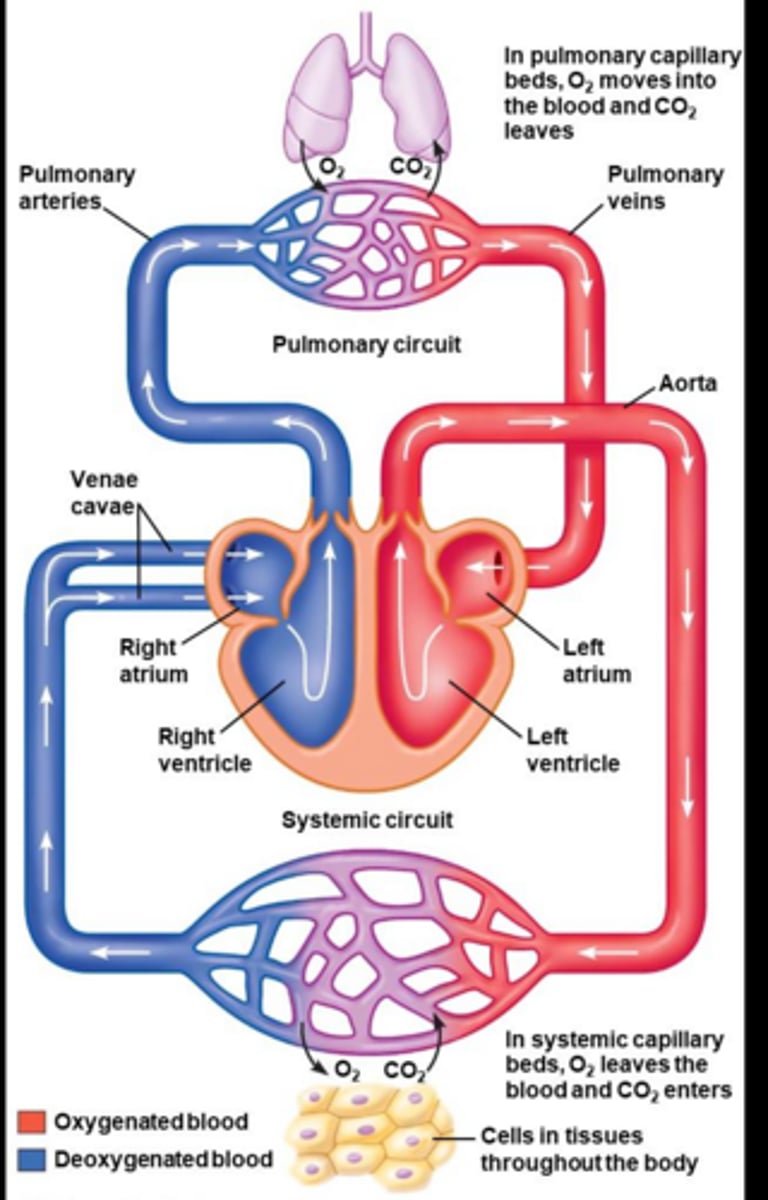
What are the major components of the cardiovascular system?
Heart, blood vessels, and blood.
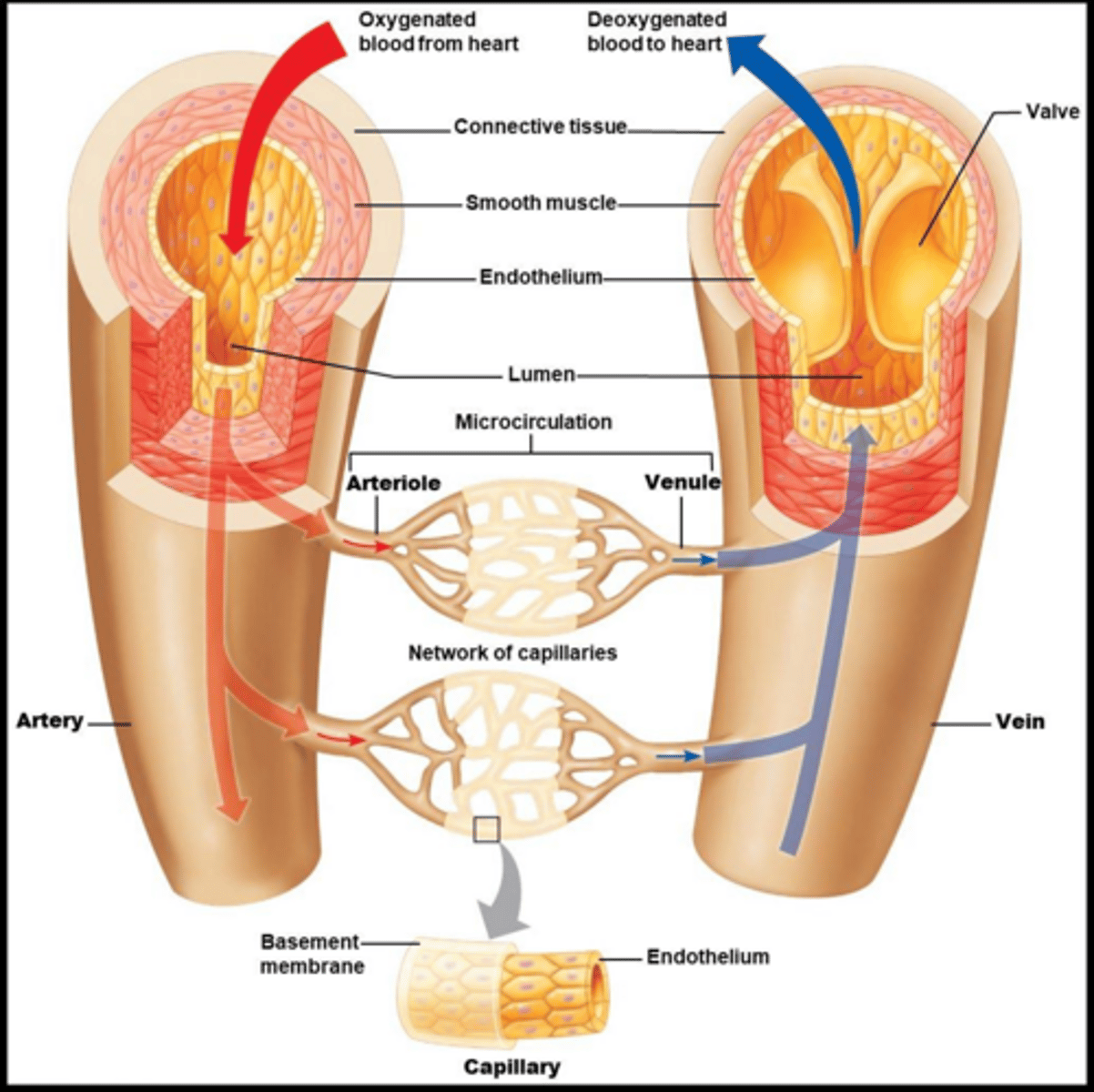
What is the role of the heart in the cardiovascular system?
To pump blood through the vessels.
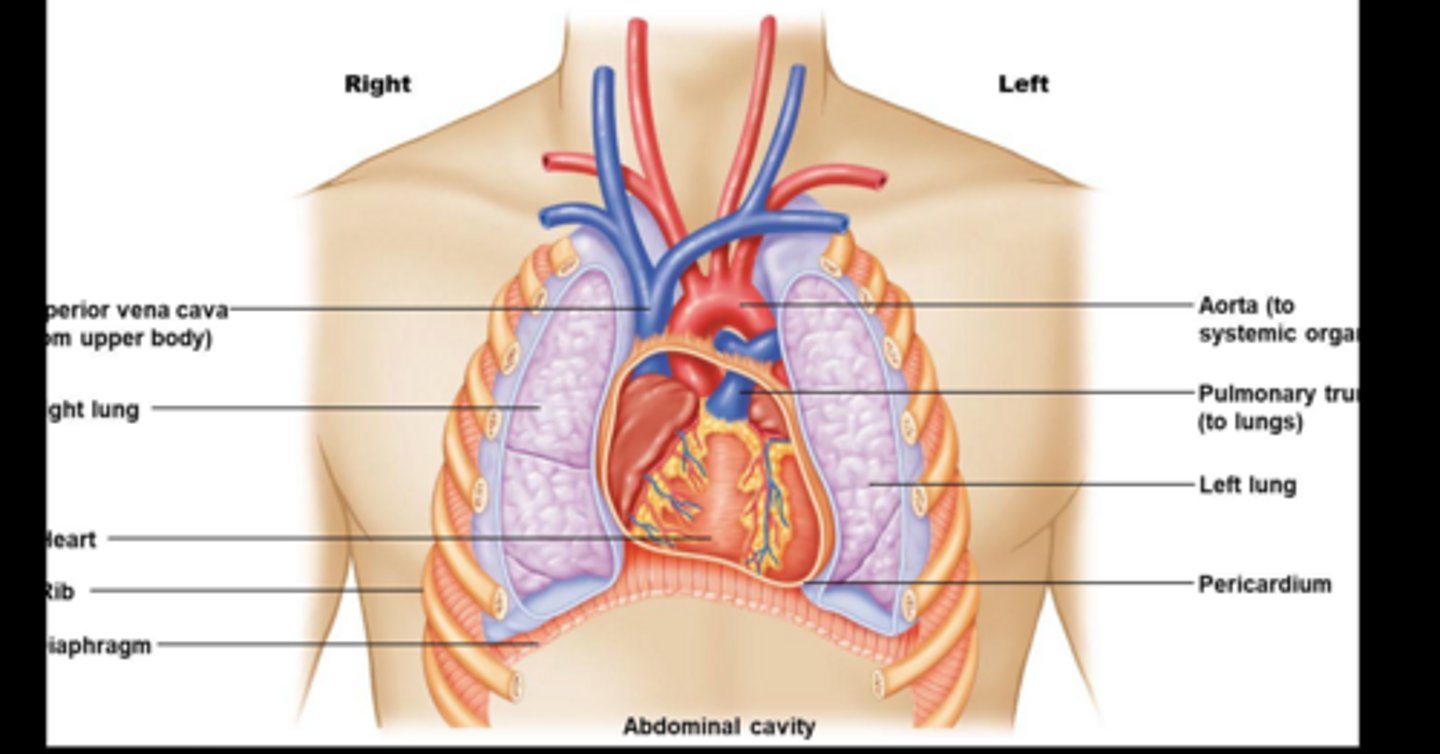
What is the role of the blood vessels in CV system?
Tubular conduit system for the blood
What is the role of blood in the CV system?
Carries material to/from cells
What brings blood to the heart?
Vena Cava
What brings blood away from the heart?
Aorta
What prevents the backflow of blood in the heart?
Valves
What is the deepest layer of the pericardium? Another name?
Visceral layer; Epicardium
Name the layers of the heart wall in order
Fibrous pericardium
Parietal Layer of Pericardium
Pericardial cavity (serous fluid for friction reduction)
Visceral layer of pericardium/epicardium
Myocardium
Endocardium
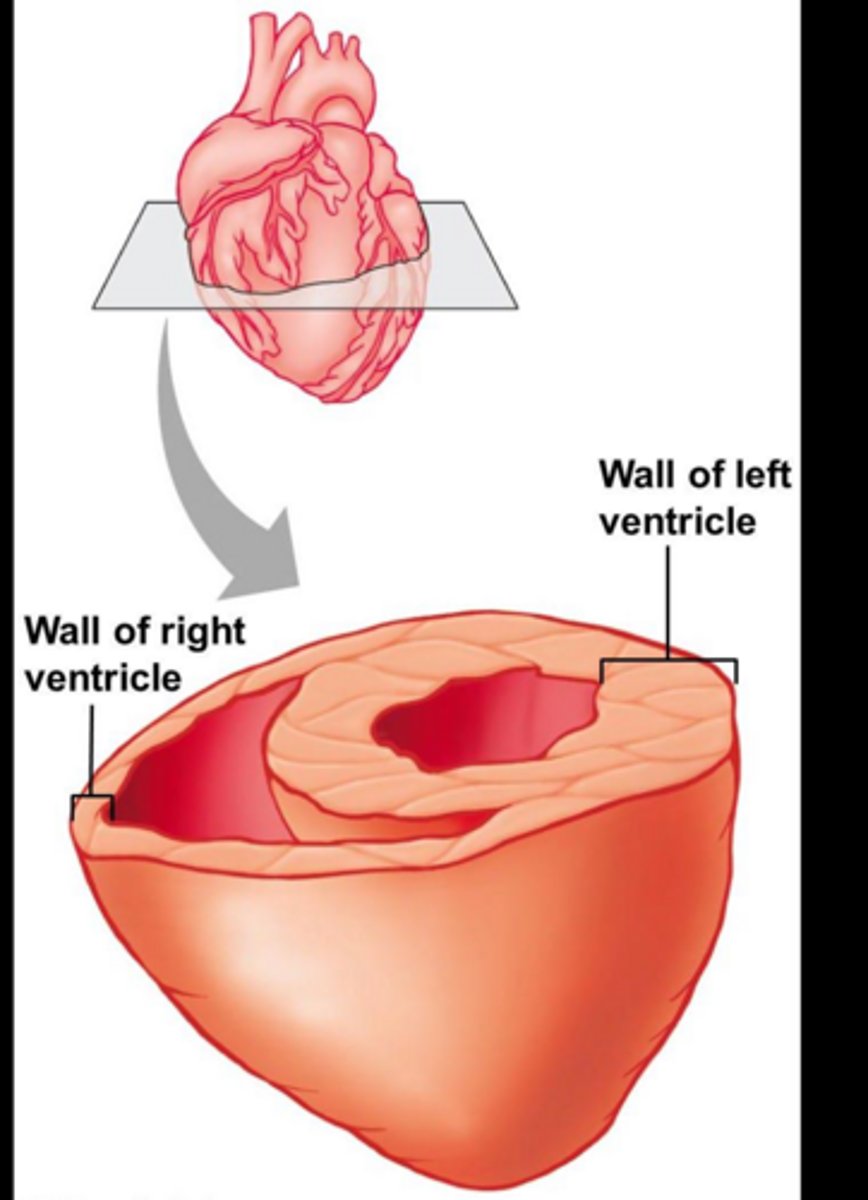
Do ventricles or atriums have thicker walls? Why?
Ventricles because they need to be able to generate force via muscle fibers
Why is the left ventricle wall thicker than the right?
The left ventricle has to pump blood to the entire body, whereas the right ventricle pumps to the nearby lungs
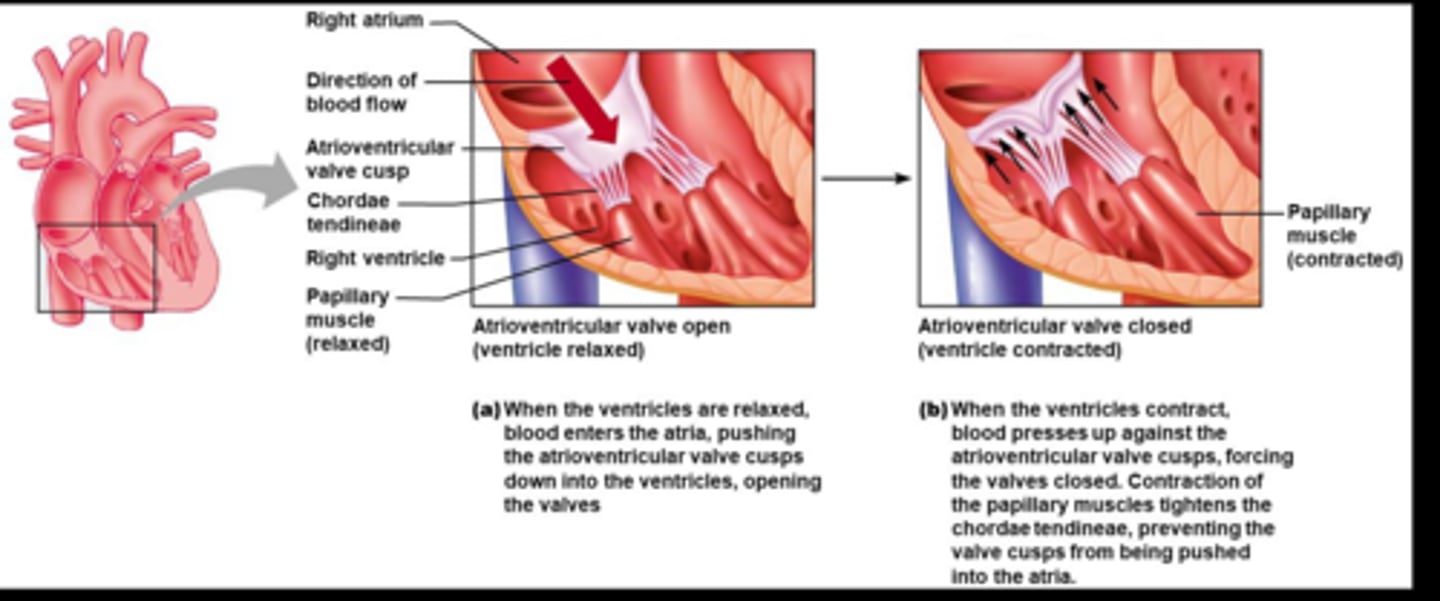
What factors prevent the backflow of blood via closing AV valves?
Pressure of blood
Papillary muscles tighten chordae tendineae
What factor prevent the backflow of blood via closing semilunar valves?
Pressure of blood in aorta forces valves shut
What kind of muscle allows vessels to constrict/dilate?
Smooth muscle
In what body part might you find valves in the veins? Why?
The limbs because the blood is working against gravity to travel back to the heart
What characteristics do erythrocytes (RBCs) get from being biconcave discs?
Flexibility and increased surface area
Where does blood go immediately after leaving the right ventricle? Destination?
The pulmonary arteries; lungs
Where does blood go immediately after leaving the lungs?
The pulmonary veins
Where does blood go immediately after leaving the left ventricle? Destination?
The aorta; entire body
What is the difference between parallel and series blood flow?
Parallel flow delivers the same blood to all organs simultaneously, Series flow directs blood through a sequence of organs.
What are the primary organs that have series flow? Why?
GI tract, liver, and kidneys because of the filtration these organs perform
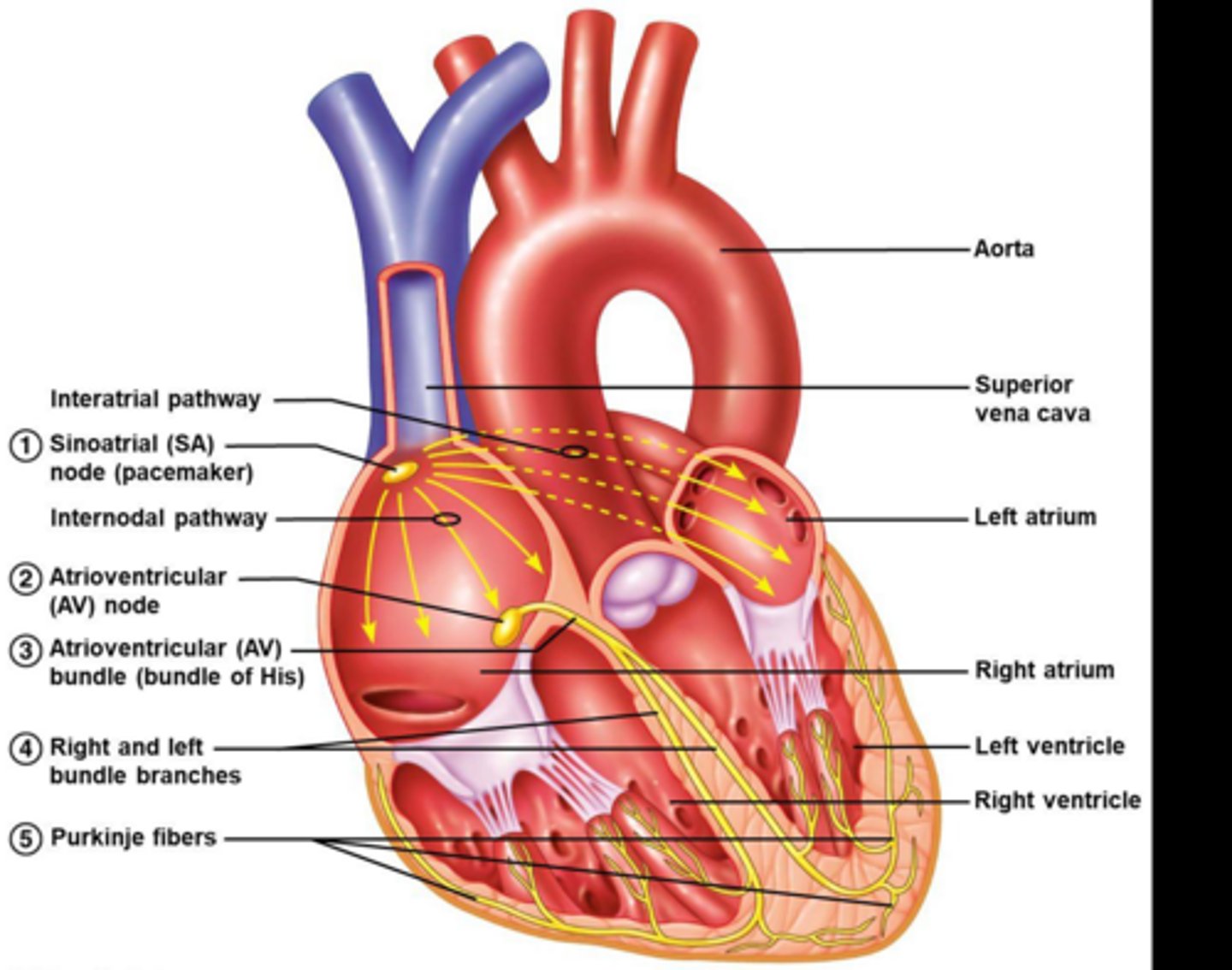
What coordinates the highly synchronized nature of contractions?
The conduction system in the myocardium
The myocardium can keep its own beat, also known as
Myogenic
What are autorhythmic cells?
Specialized cardiac myocytes
What do pacemaker cells do?
Spontaneously generate action potentials and establish the heart rhythm
Where are pacemaker cells found? Which site of the two can generate action potentials more quickly?
SA node and AV node; sinoatrial node
What are conduction fibers?
Large diameter cardiac myocytes that transmit action potentials
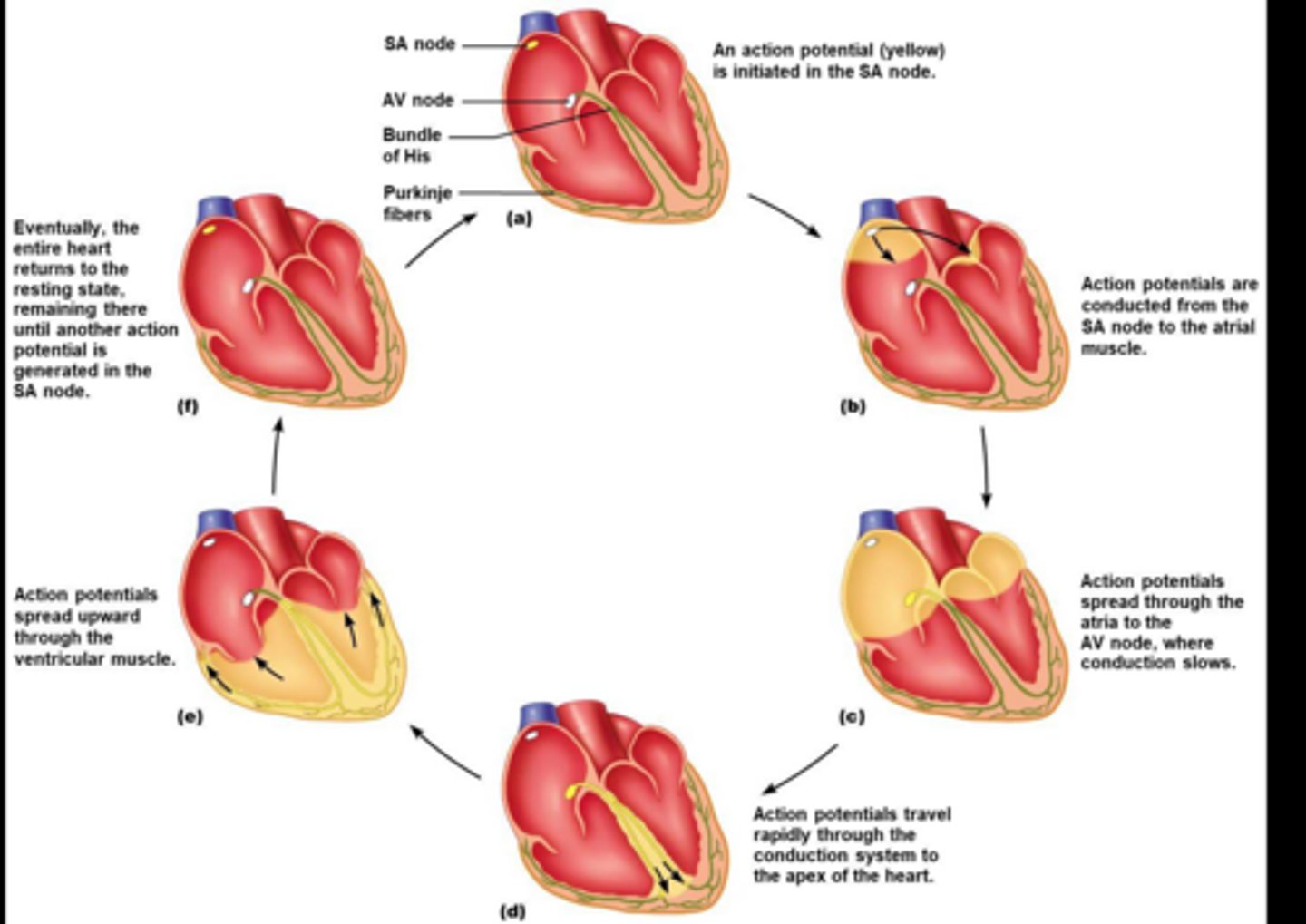
What sends the electrical signal for contraction (from SA node)
Purkinje fibers
After an action potential is initiated in the SA node, where does it go next? What happens to conduction?
Atrioventricular node; slows
After moving through the AV node, where does the AP travel? How quickly is it traveling here?
Apex of heart/Pukinje fibers; rapidly
What is the purpose of an electrocardiogram (ECG)?
To record the electrical activity of the heart.
What does the P-wave represent in an ECG?
Atrial depolarization (atriums contract)
What does the QRS complex represent in an ECG?
Ventricular depolarization (ventricles contract)
What does the T-wave represent in an ECG?
Ventricular repolarization (ventricles relax)
What is the cardiac cycle?
The sequence of events in one heartbeat, including systole and diastole.
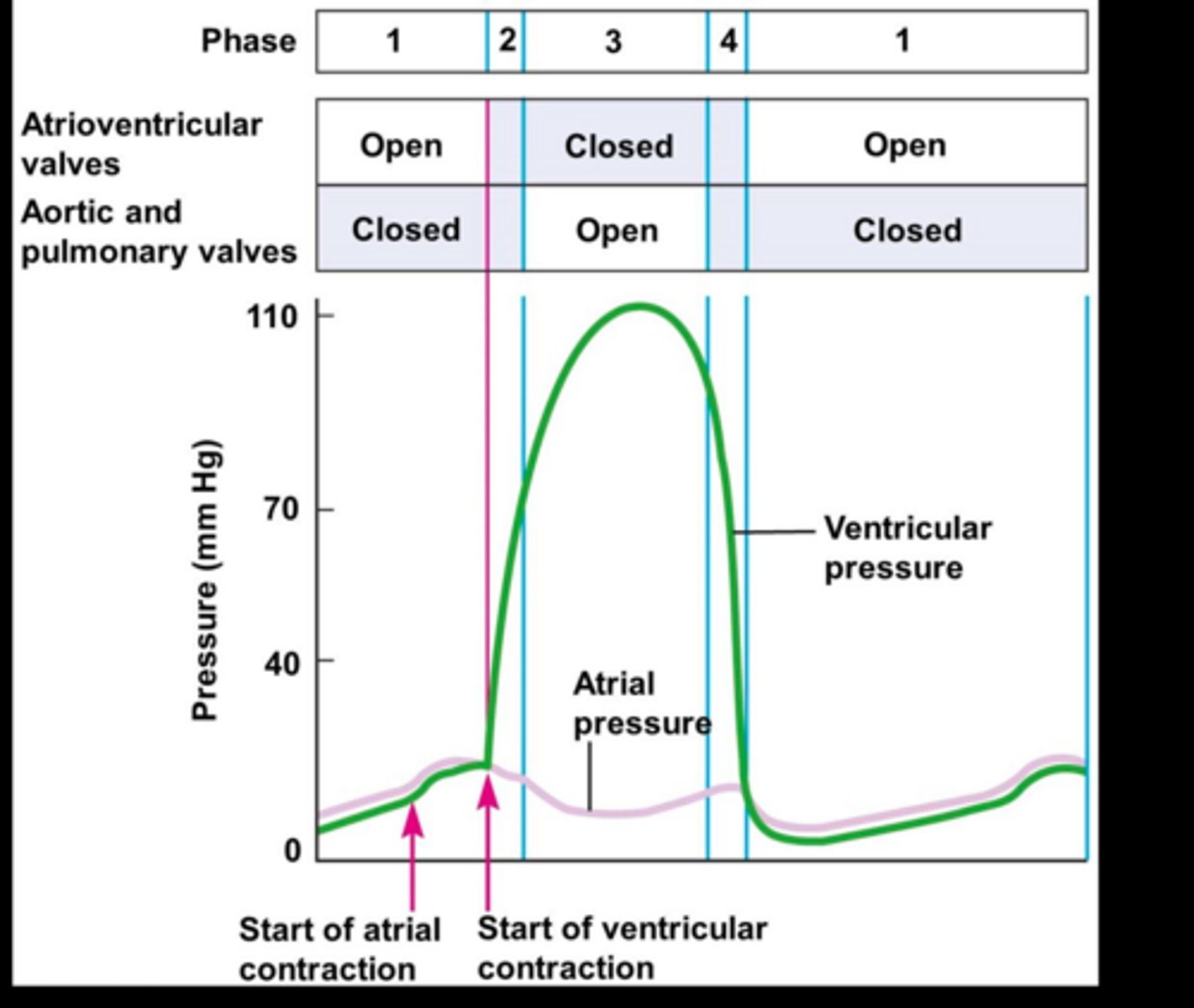
What happens during mid-to-late diastole?
- Ventricle fills with blood from venous return
- Pressure from atria pushes on AV valves into right ventricle, semilunar valves close
What happens during systole?
-Contraction phase
-Build up of pressure in ventricles
-Isovolumetric (both valves closed , no blood movement to build pressure)
-Ejection = blood goes into aorta via opening of semilunar valves
What happens during early diastole?
-Some blood leftover (still some pressure)
-Valves are closed until pressure drops enough and AV valves open, allowing the cycle to restart
All pressures are relative to atmospheric:
760 mmHg
T/F: Start of contraction means blood moves immediately due to rapid increase in pressure
False, there is a rapid increase in pressure, but the blood does not move immediately
When ventricular pressure drops, isovolumetric _______ occurs
Relaxation
______ pressure gets superimposed by _______ pressure
aortic; ventricular
What is the dicrotic notch?
Closing of the semilunar valves and start of diastole (following dramatic increase in ventricular pressure)
What are the main roles of the atria and ventricles?
Atria receive blood; ventricles pump blood out.
What are the functions of the valves in the heart?
To prevent backflow of blood.
What is the function of the pericardium?
To stabilize the heart and reduce friction.
What is the difference between arteries and veins?
Arteries carry blood away from the heart, while veins carry blood to the heart.
What is the significance of capillaries in the cardiovascular system?
They are the site of gas exchange between blood and tissues.
What is autorhythmicity in the myocardium?
The ability of the heart muscle to generate its own rhythm.
What are Purkinje fibers responsible for?
Conducting electrical signals for contraction in the heart.
What is the role of the sympathetic nervous system in heart function?
Increases heart rate (through AP control) and contractions (SV) via cardiac accelerator nerves
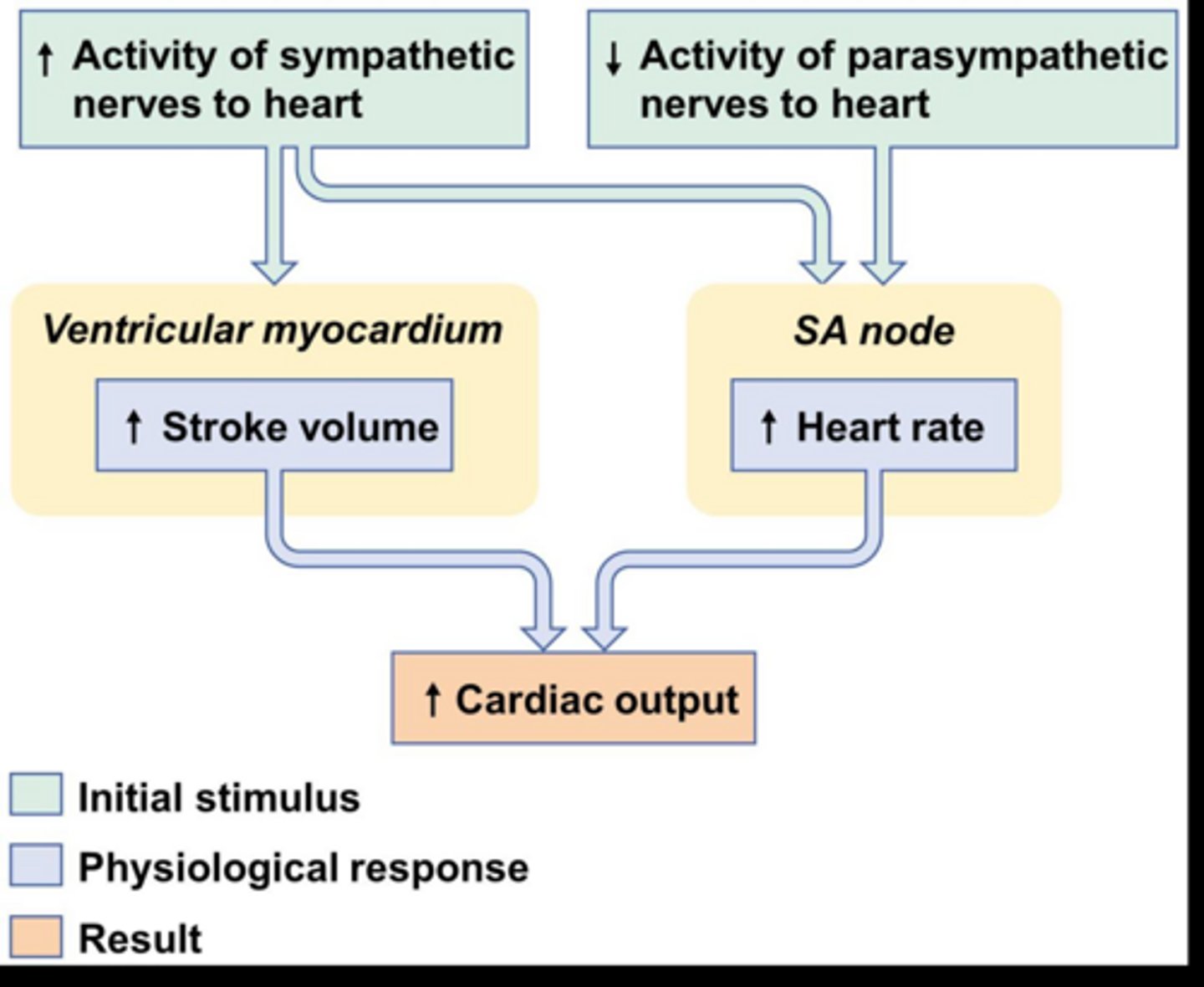
Vagus nerves in the parasympathetic system are crucial for what cells in the heart?
Pacemaker cells
At rest, the heart has a ____ (higher/lower) vagal tone
Higher
The myocardium is part of the ________ nervous system
Sympathetic
What is the role of the parasympathetic nervous system in heart function?
It decreases heart rate via vagus nerves
What is preload in cardiac function?
The degree of stretch of the heart muscle before contraction.
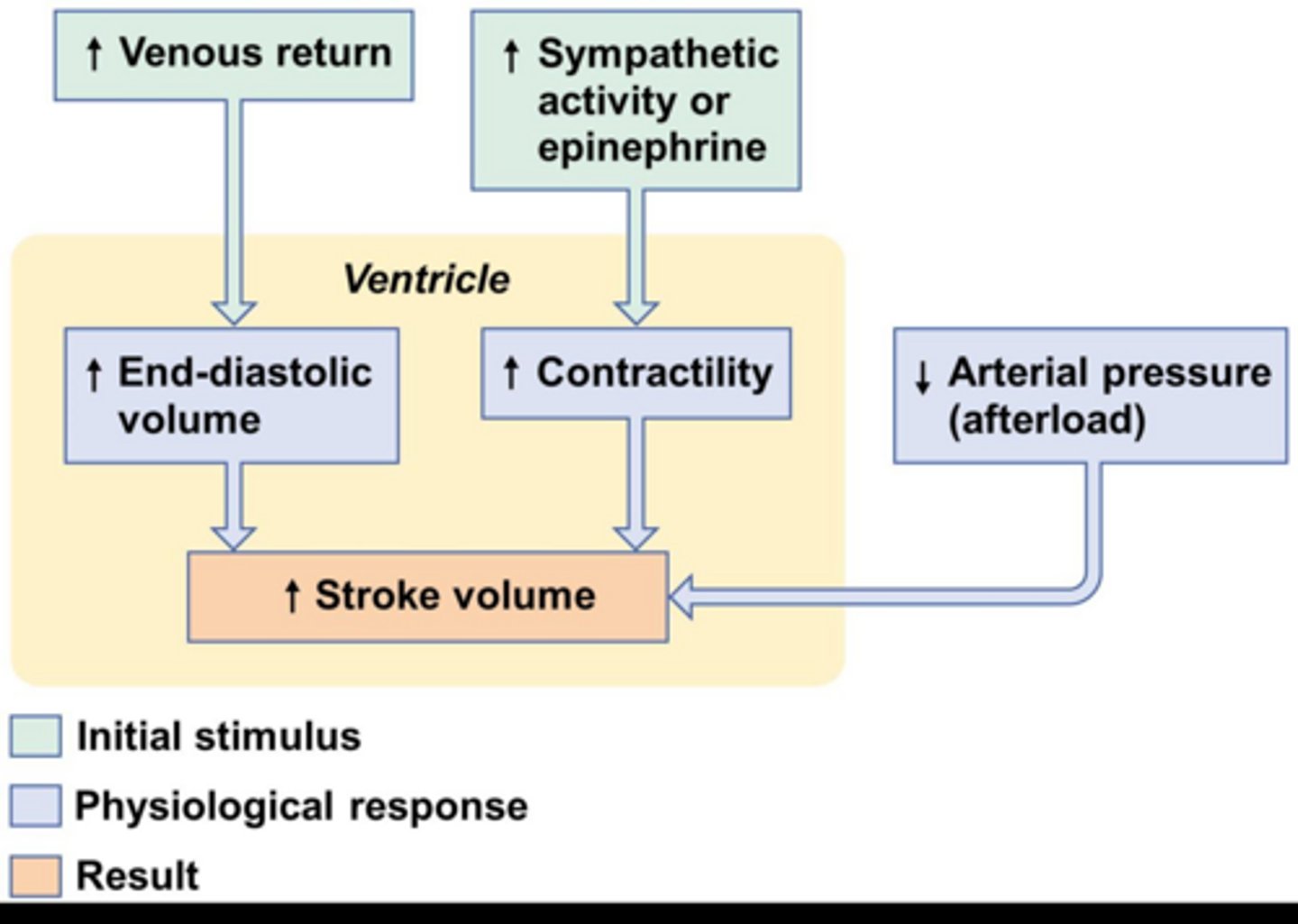
What is afterload in cardiac function?
The pressure the heart must work against to eject blood.
What is the significance of circulating epinephrine on cardiac function?
It increases heart rate and contractility.
What is cardiac output (CO)?
The rate at which a single ventricle pumps blood
CO = HR x SV
How does ventricular contractility affect cardiac output?
Increased contractility enhances the heart's ability to pump blood.
What is the function of the aorta?
To carry oxygen-rich blood away from the heart to the body.
What is the function of the vena cava?
To bring oxygen-poor blood back to the heart.
What does an upward deflection on the ECG indicate?
Electrical activity traveling toward the positive electrode.
What are the two phases of the cardiac cycle?
Systole (ventricular contraction) and Diastole (ventricular relaxation).
What occurs during isovolumetric contraction?
Both valves are closed, and no blood movement occurs to build pressure.
What impacts stroke volume?
EDV, ventricular contractility, afterload
Ventricular contractile force is under extrinsic control via
SNS innervation and circulating epinephrine
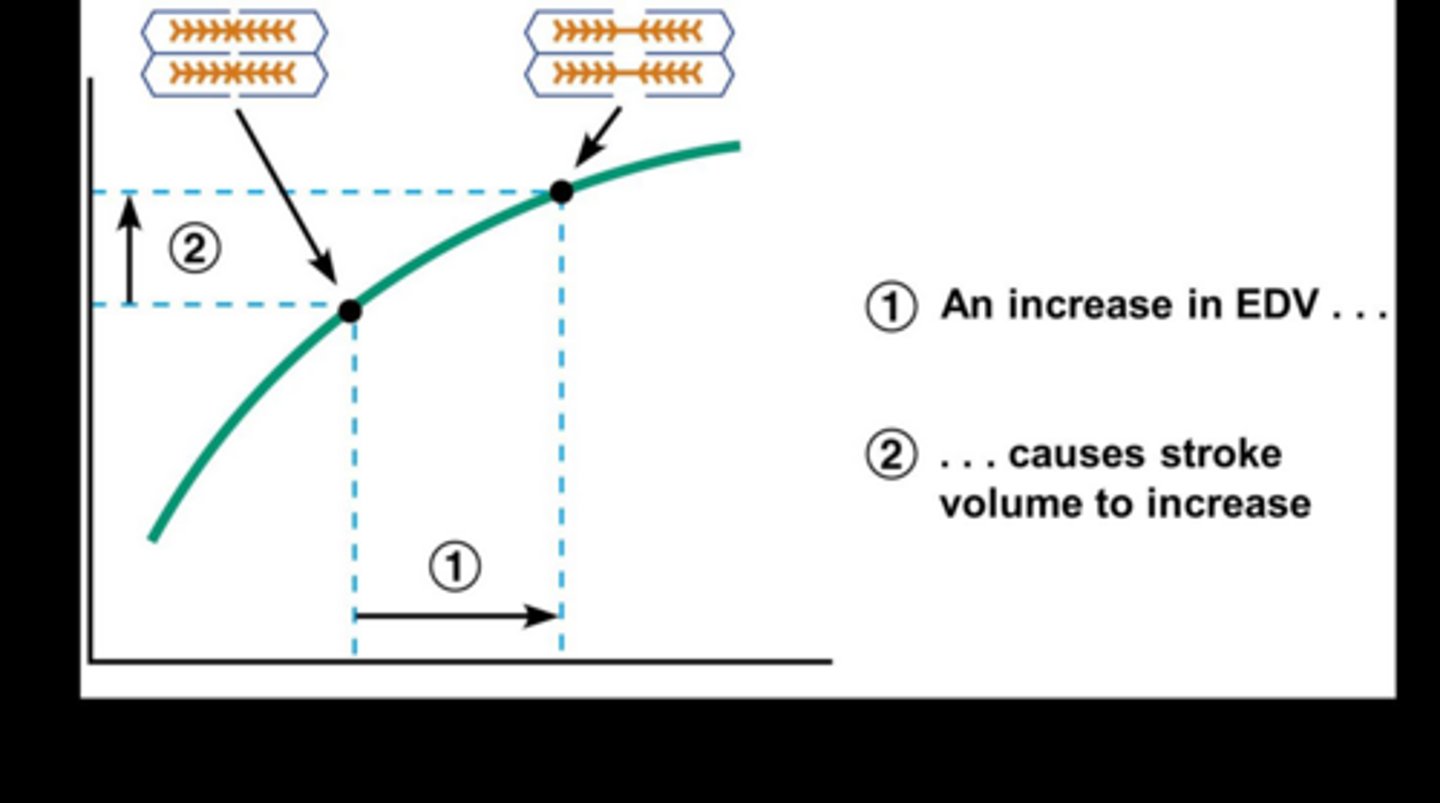
Ventricular contractile force is under intrinsic control via
Increasing EDV to stretch the myocardium, putting the sarcomere at an ideal length
Why would a better length of a sarcomere generate more force?
At the ideal length, more crossbridges can be formed
End diastolic pressure is also known as
Preload
What is the major factor affecting EDV?
Preload
What will happen to EDV if venous return increases?
EDP will increase, expanding the ventricle and increasing EDV
How does HR affect preload?
An increase in HR means the heart has less time for filling, decreasing preload and EDV
How does atrial pressure affect preload?
More venous return = increased atrial pressure = increased atrial contractility = increased ventricular filling = increased preload
Contractility refers to
the increased force at any given EDV
How does ventricular contractility affect SV?
Increased pumping is a result of Sterling's law, the heart matches the output with the imput via ventricular contraction
Starling's law is an __trinsic mechansim to increase SV
intrinsic
How is contractility regulated extrinsically?
SNS and epinephrine circulation:
•Catecholamines bind to B1 adrenergic receptors →
increased myocardial cAMP:
•Enhanced Ca++ presence
•Increased rate of crossbridge cycling
Increased sympathetic activity has the same amount of blood, but a ______ blood volume ejection
Higher
Increased sympathetic activity has the same amount of blood, but a ______ blood volume ejection
Lower
What is end-diastolic volume (EDV)?
The volume of blood in the ventricle at the end of filling, before contraction.
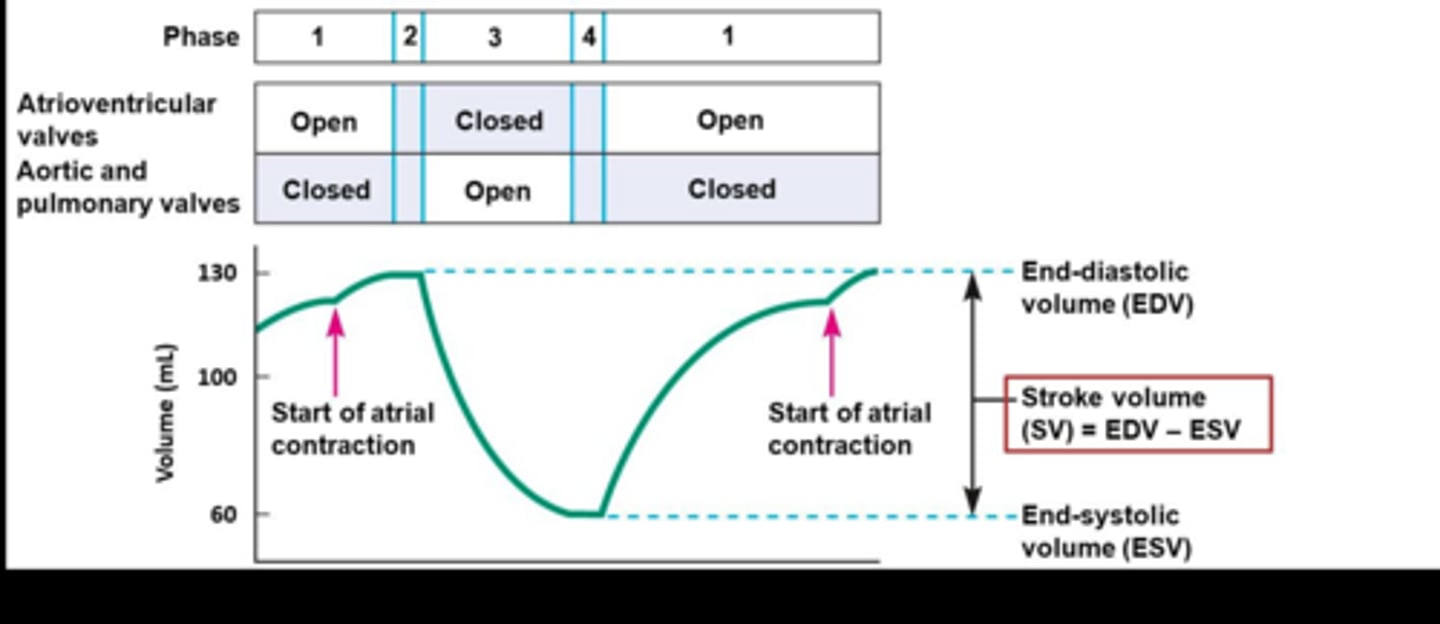
What is end-systolic volume (ESV)?
The volume of blood remaining in the ventricle after contraction.
How is stroke volume (SV) calculated?
SV = EDV - ESV.
What is ejection fraction?
The percentage of EDV ejected from the heart during one cardiac cycle.
What is systolic blood pressure (SBP)?
The maximal aortic pressure occurring during systole (Blood enters aorta from left ventricle)
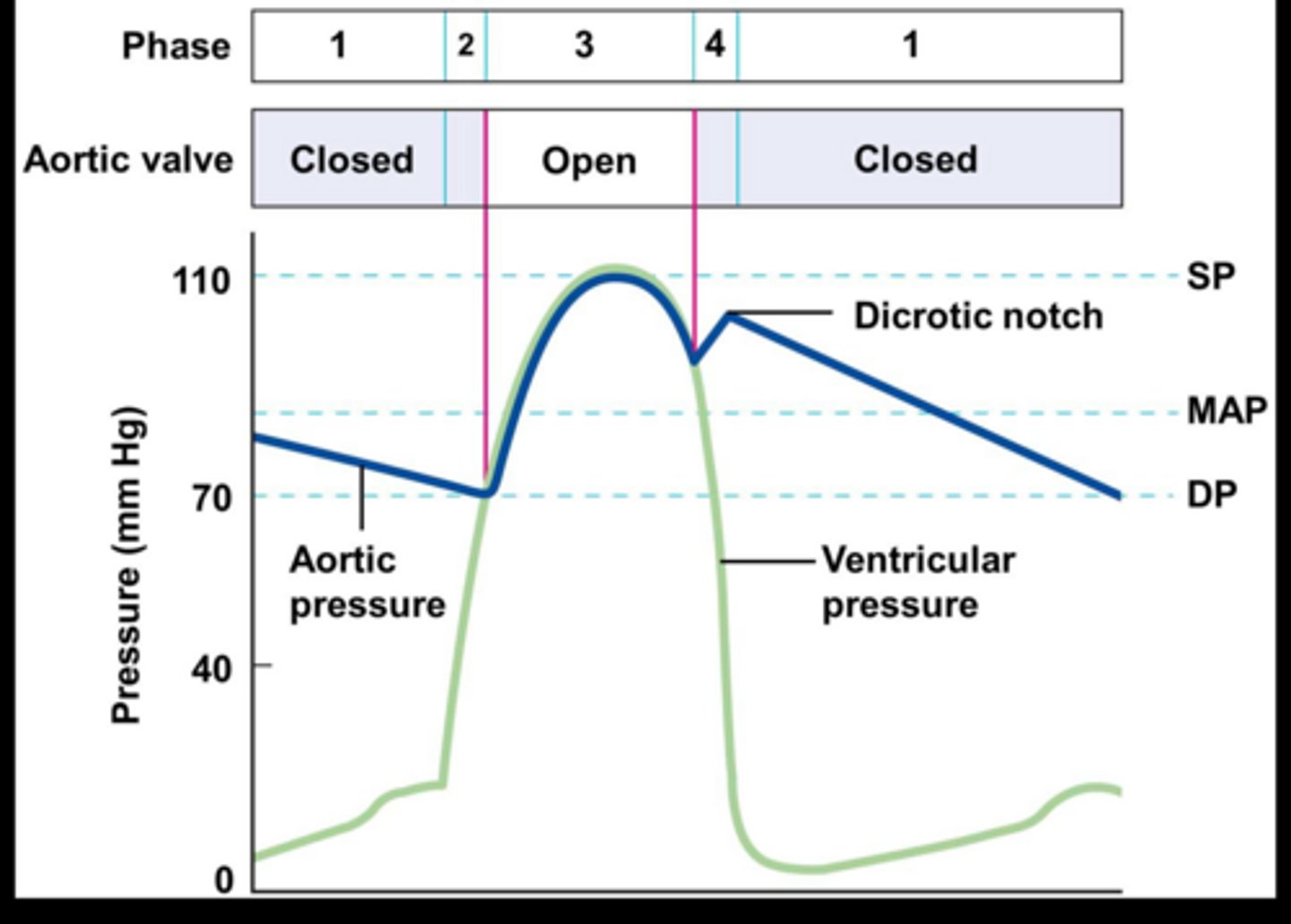
What is diastolic blood pressure (DBP)?
The minimum aortic pressure occurring during diastole (Blood leaving aorta from closed semilunar valves)
What is mean arterial pressure (MAP)?
The average aortic pressure during a cardiac cycle. This is the OVERALL DRIVING FORCE for blood to reach organs
What is the relationship between right and left heart cardiac output?
They must match to prevent complications like pulmonary edema (because of in-series blood flow)
What are examples of extrinsic control mechanisms?
Nervous system and epinephrine
What is an example of intrinsic control mechanisms?
Autoregulation (the heart itself)
Heart rate regulation is strictly __trinsic (ex/in)
extrinsic
What is intrinsic rate? How is this achieved?
100-110 BPM; By decreasing vagal tone
Afterload increases as ____ increases
MAP
What factors affect heart rate (HR)?
Neural control (sympathetic and parasympathetic) and hormonal control (e.g., epinephrine).
What is Starling's Law of the Heart?
The heart automatically adjusts its output to match the inflow of blood.
What is preload?
The load on the myocardium before contraction, determined by end-diastolic pressure (EDP).
What factors affect preload?
Atrial pressure, filling time, and venous return.
What is afterload?
amount of resistance (pressure from the arteries) the heart must pump against when ejecting blood
How does increased mean arterial pressure (MAP) affect afterload?
Increased MAP leads to increased afterload.