13 Respiratory System
1/26
Earn XP
Description and Tags
13.3
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
27 Terms
functions
__ of respiratory system
provides oxygen
eliminates CO2
regulates H+ conc. (pH) with kidneys
speech
defends against inhaled microbes
influences arterial concentrations of chemical messengers
traps/dissolves blood clots from systemic veins
alveoli
site of gas exchange with blood
Airways
Tubes where air flows from external environment to the alveoli and back
Structures that make up the __ are:
nose
nasal cavity
pharynx →common to both air + food
branches into the esophagus (digestive system) and the larynx
larynx →houses the vocal cords
trachea →branches into two bronchi
bronchi (singular: bronchus)
bronchioles →first airway branches that no longer contain cartilage
branches into terminal bronchioles → respiratory bronchioles
alveoli →first appears in respiratory bronchioles
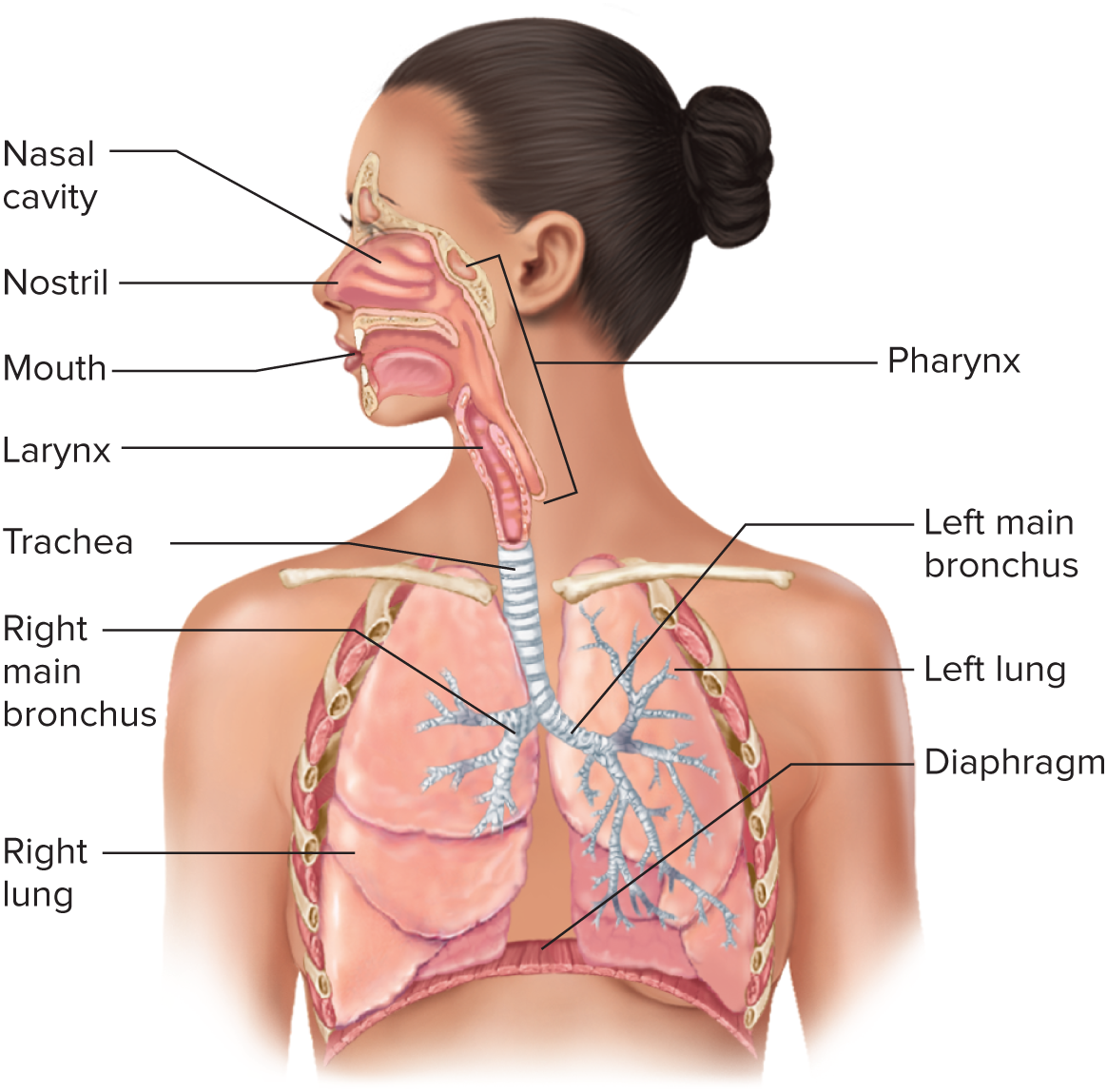
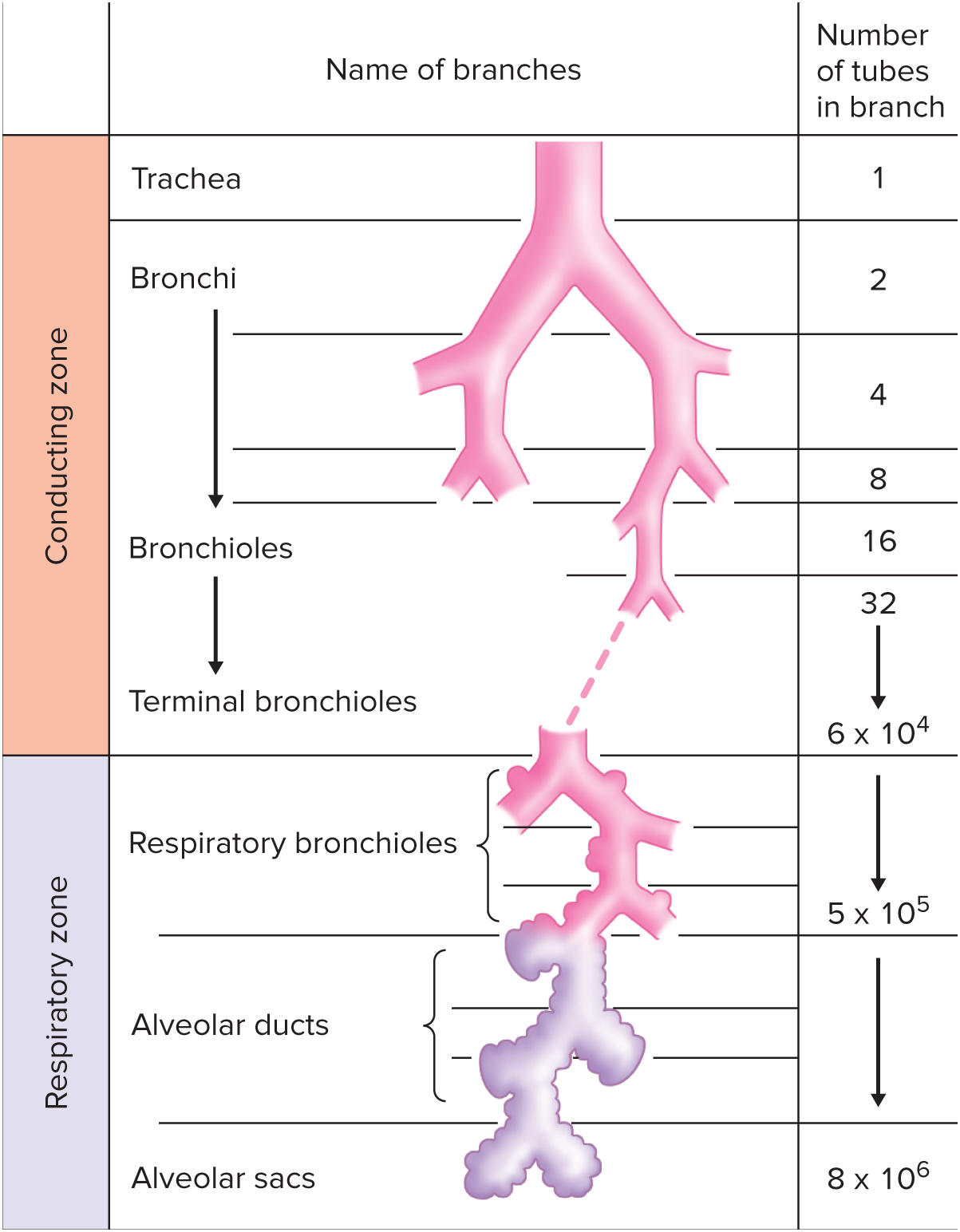
Conducting zone
Airways beyond the larynx can be subdivided into (1/2) zones
__ extends from top of trachea to end of terminal bronchioles. Contains no alveoli.
The __ provides low-resistance pathway for airflow
resistance regulated by:
bronchiolar smooth muscle. constricts to prevent further particulate matters/irritants from entering site of gas exchange
physical forces acting upon airways
Defends against microbes, toxic chemicals, and other foreign matter
cilia, mucus, macrophages
Warms and moistens air
& Participates in sound production
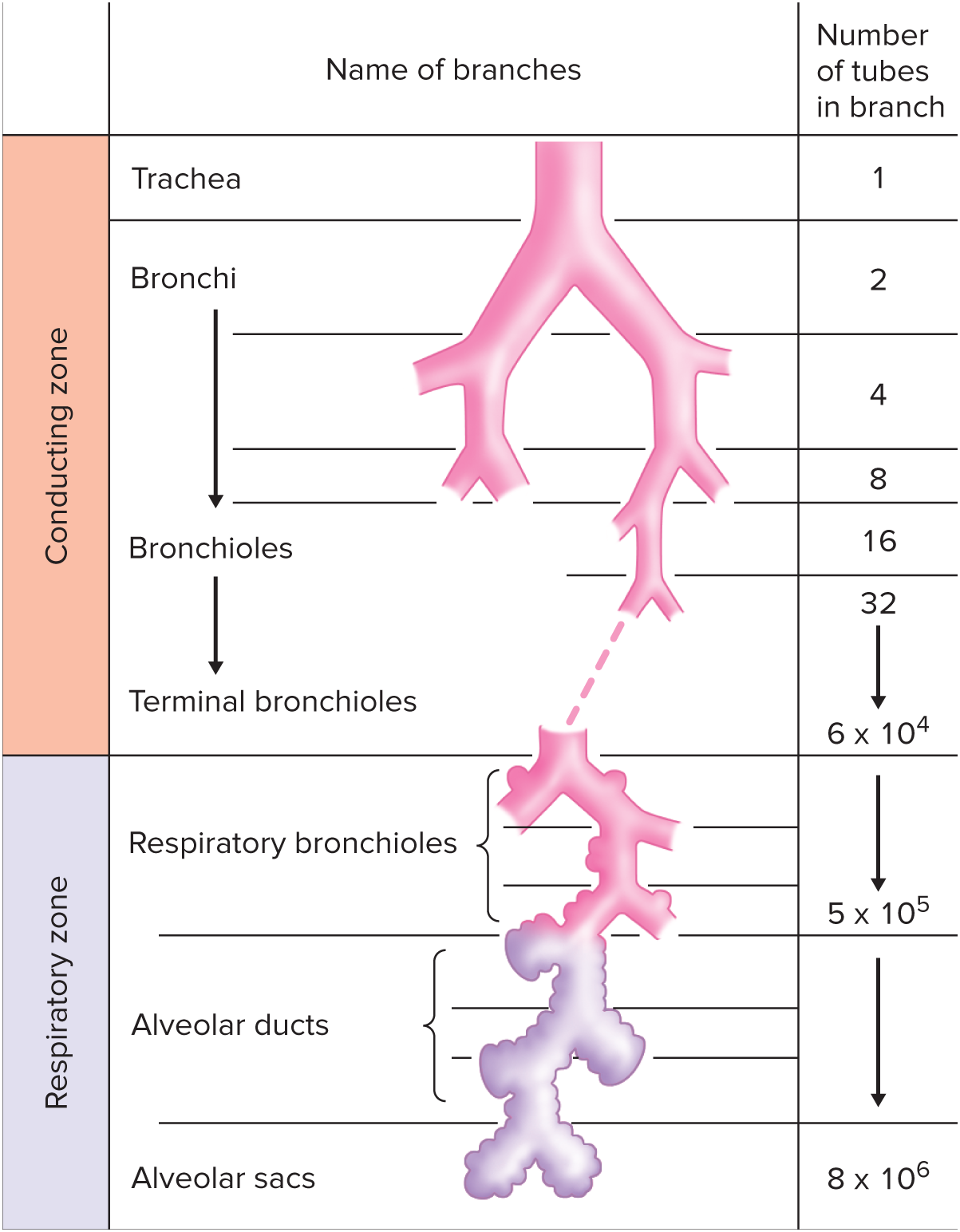
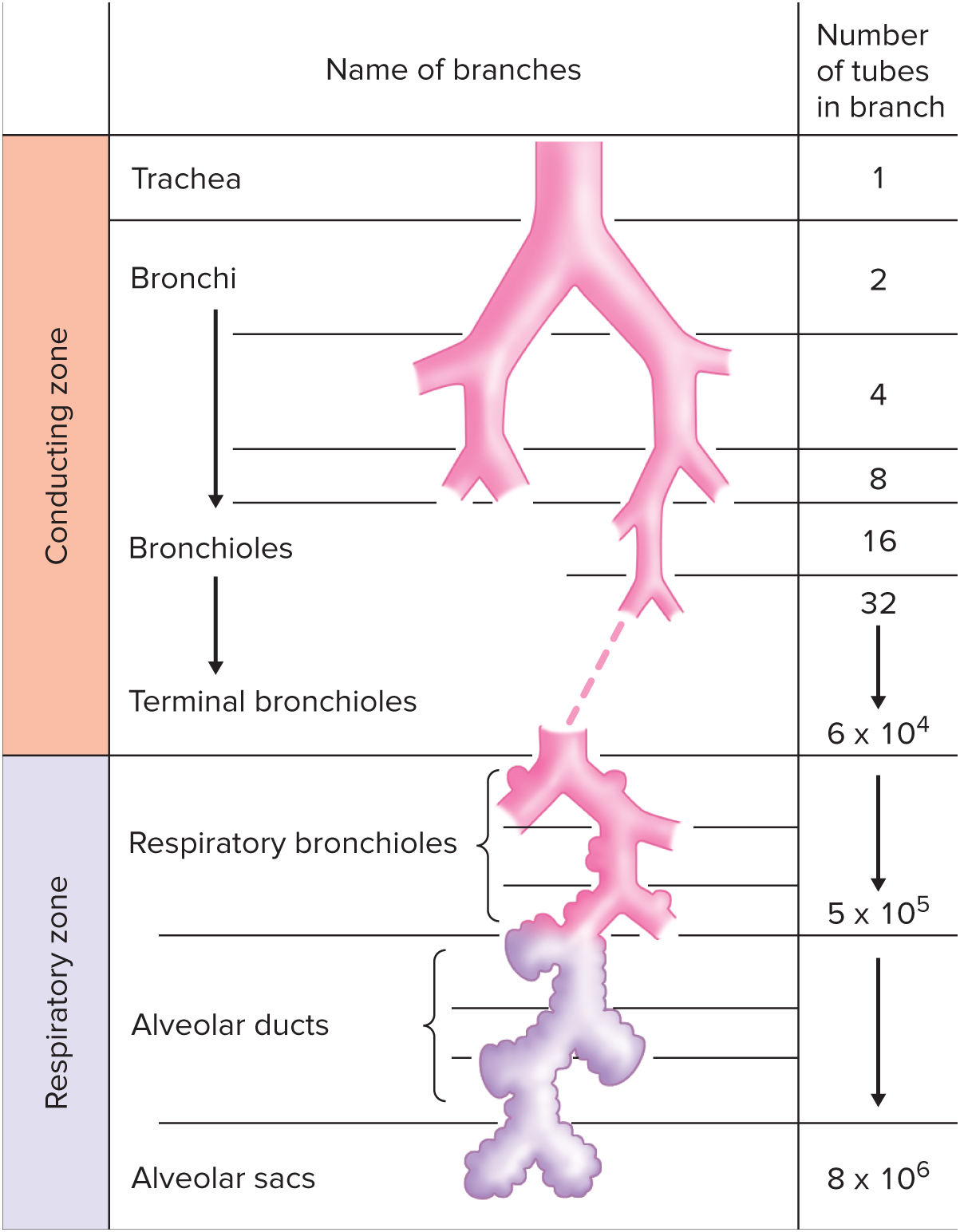
Respiratory zone
Airways beyond the larynx can be subdivided into (1/2) zones
__ extends from respiratory bronchioles and down.
Where alveoli exchange gases with the blood.
Ciliary Mucuous escalator
Refers to the cilia (present from the airways to the end of the respiratory bronchioles) that constantly beat upward towards the pharynx
mucous secreting glands + epithelial cells are present in oral and nasal cavities
particulate matter gets stuck in mucus; gets moved towards the pharynx by a “__” = Keeps lungs clear of matter and bacteria
macrophages → phagocytize inhaled pathogens
A/N: Cilia is killed by noxious agents like tobacco smoke → smokers often cough up mucus
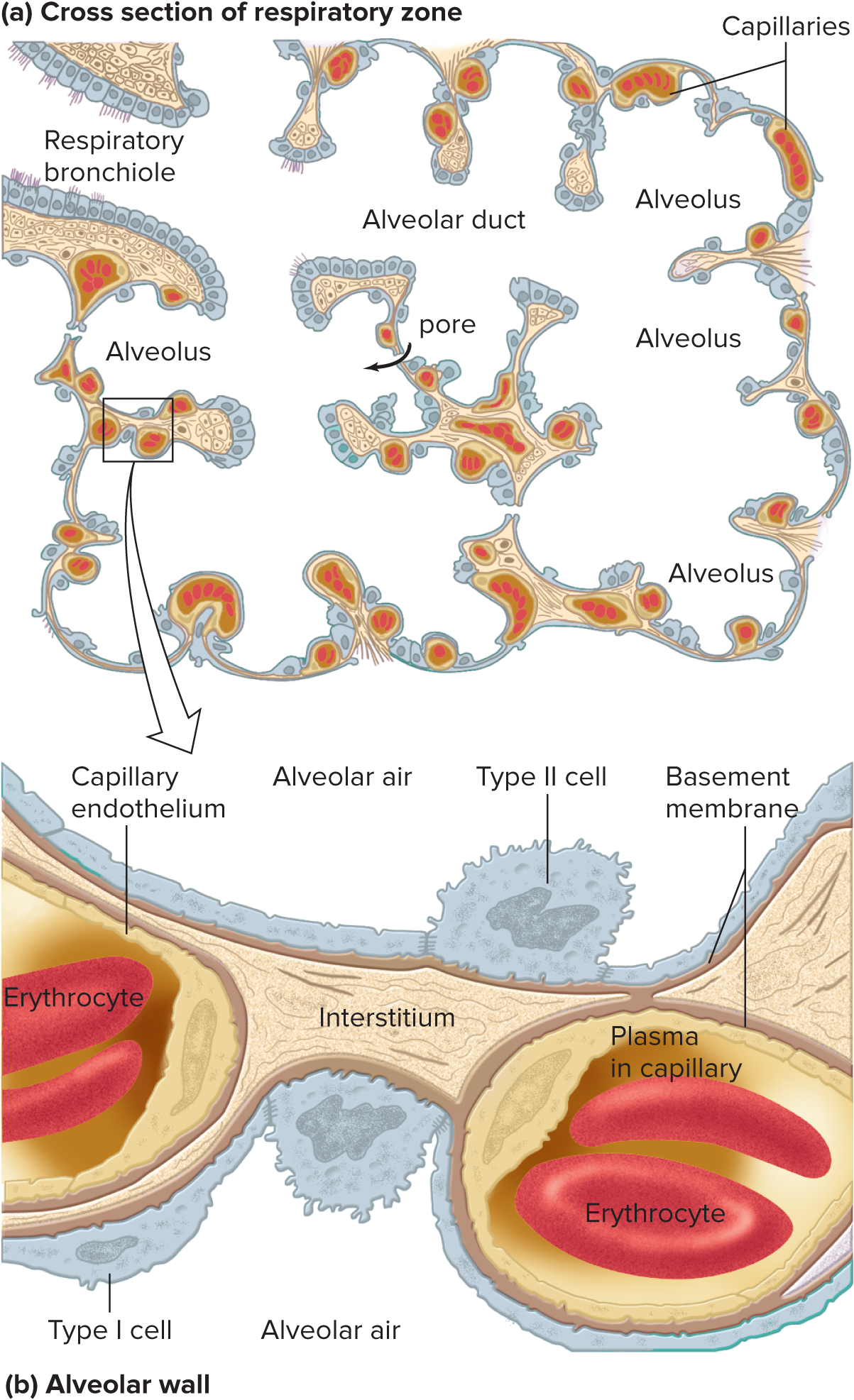
Alveoli
Tiny, hollow sacs whose open ends are continuous with the airways
Type 1 alveolar cells: thick, flat epithelium. Lines the air-facing surface of alveolar wall
Type 2 alveolar cells: specialized cells (produces a detergent-like surfactant: important for preventing collapse of alveoli) interspersed between the epithelial cells.
The following leads to a rapid oxygen-CO2 exchange by diffusion in the __:
Large SA of __ and capillary contact
as large as a tennis court
Thin interstitial space
sometimes absent altogether between capillary and __
Additionally, pores permit flow between adjacent __
pleura
Each individual lung is surrounded by a completely closed sac known as the pleural sac; it is made up of sheet cells known as __
Visceral [__]: portion coating the surface of lung
Parietal [__]: portion enclosing the (thoracic) cavity around lung
has thin layer of intrapleural fluid in between → surrounds lungs and lubricates pleural surfaces to slide over each other during breathing
Respiratory cycle
constituted by a single
inspiration: inhalation, movement of air from external environment to alveoli during breathing
expiration: exhalation, movement of air from alveoli towards external environment
During the entirety of a __:
4L of air enters and leaves alveoli per minute
inc. 20 fold during heavy exercise
5L of blood (cardiac output) flows through pulmonary capillaries
inc. 5-6 fold
Respiration
__ has 4 steps:
1⃣ Pulmonary ventilation: exchange of air between atmosphere and alveoli by bulk flow
2⃣ Exchange of O2 and CO2 between alveoli and capillaries by diffusion → packaging of oxygen in pulmonary circulation
3⃣ Transport of O2 and CO2 thru pulmonary & systemic circulation by bulk flow
4⃣ Exchange of O2 and CO2 between capillaries and tissue cells by diffusion → drop off of oxygen in systemic circulation
760
All pressures in respiratory system are given relative to atmospheric pressure, which is __ mmHg at sea level
eg. when Palv= 0 mmHg, Palv = Patm
Patm = atmospheric pressure
pressure surrounding body.
decreases as altitude increases
Pip= intrapleural pressure
pressure outside lungs / intrapleural fluid surrounding lungs
Palv= alveolar pressure
pressure inside lungs / alveoli
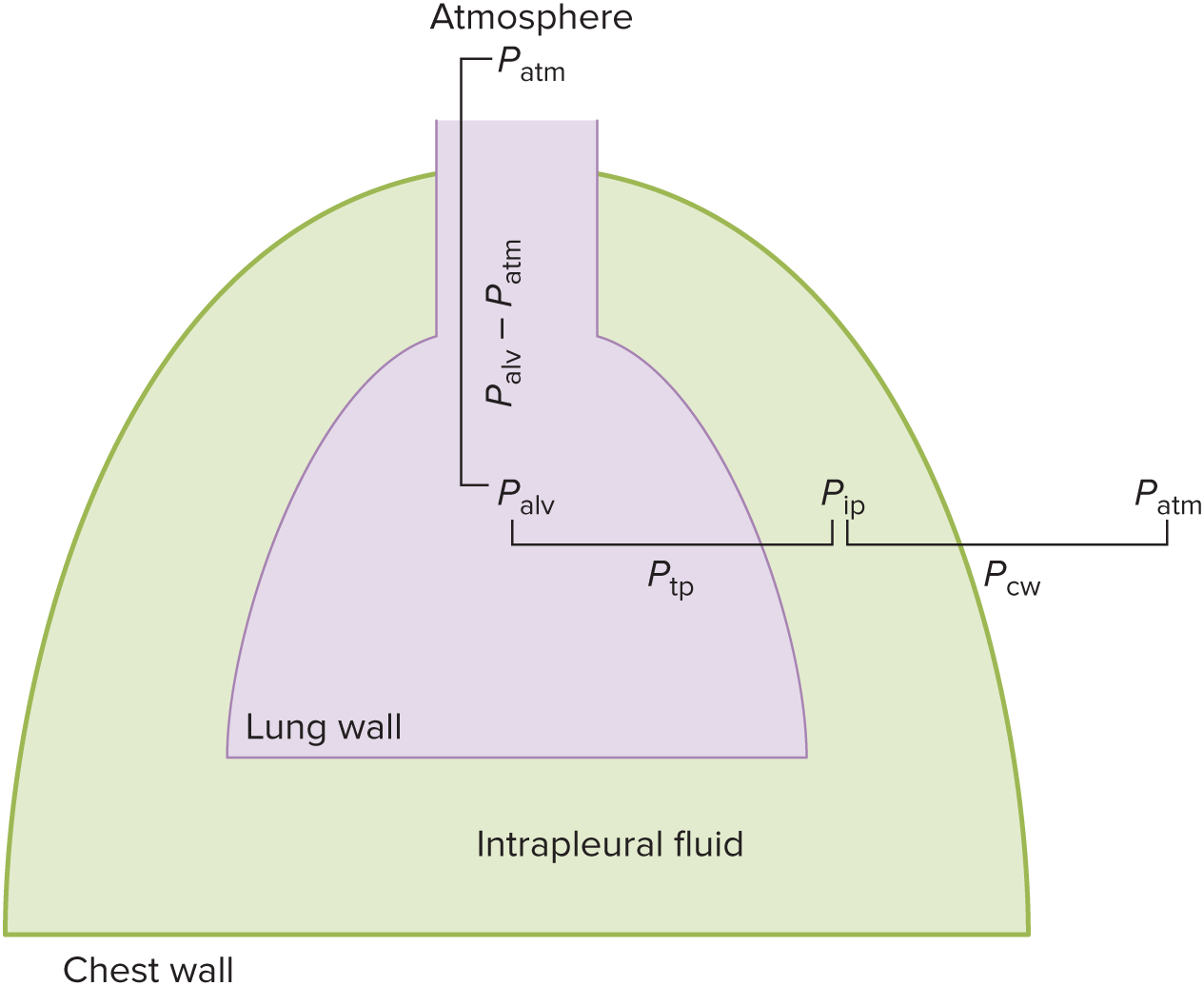
flow
__ is directly proportional to pressure difference and inversely proportional to airway resistance
F = ( Palv - P atm) / R
A/N: equations comparing pressures follow pattern of Pinner- Pouter
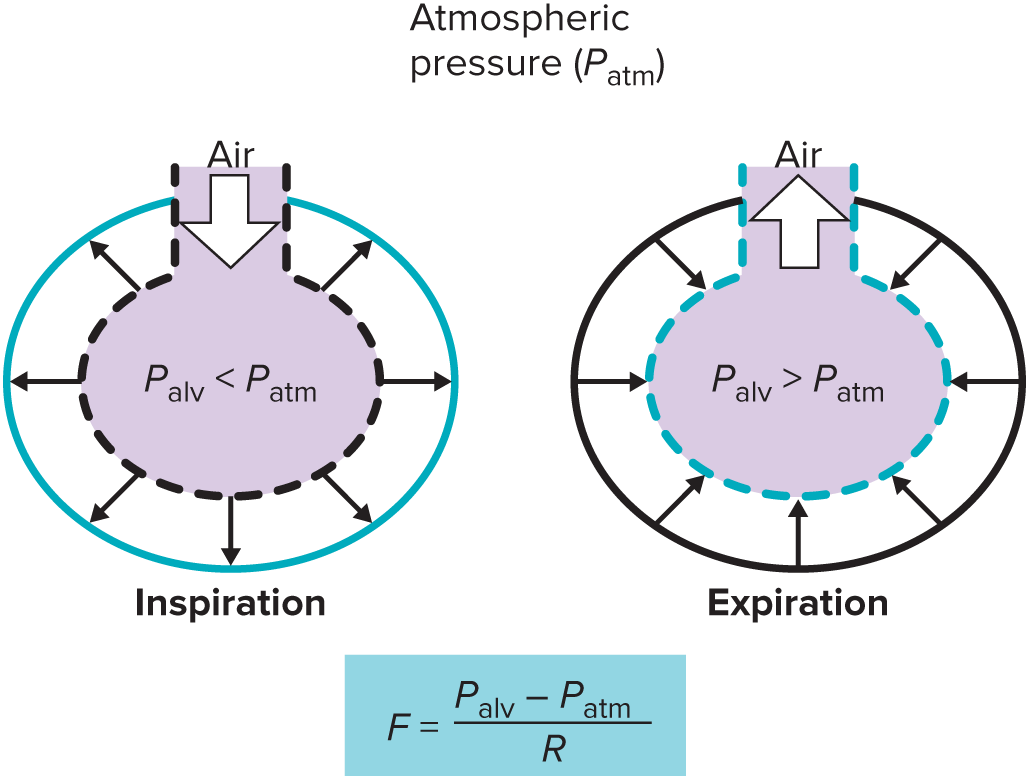
negative value (Palv< Patm) → inward flow (into) → inspiration
for transmural: inward pressure direction across lung/thorax (not into) = depression
positive value (Palv > Patm) → outward flow (out of) → expiration
for transmural: outward pressure direction across lung/thorax = expansion
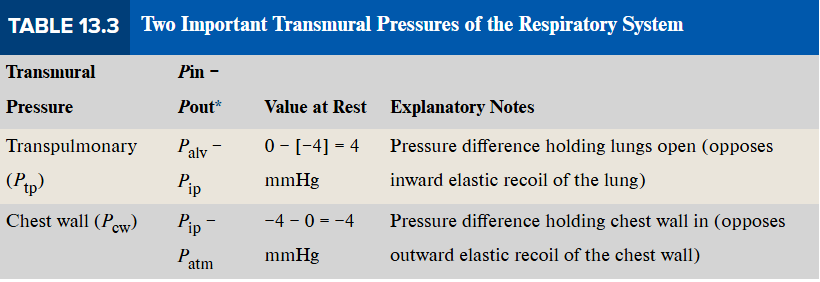
Transmural
Differences in pressures “across a wall” refer to “__” pressures.
Ptp: transpulmonary pressure = Palv - Pip
__ pressure acting upon lung, opposing intrinsic collapsing of lung
positive at rest → expansion of lungs. Normal (Ptp= -4 mmHg)
negative → depression of lungs
Pcw: chest wall pressure = Pip - Patm
__ pressure acting upon chest wall. opposing intrinsic expansion of thorax
positive → expansion of thorax.
negative at rest → depression of thorax. Normal (Pcw = 4 mmHg)
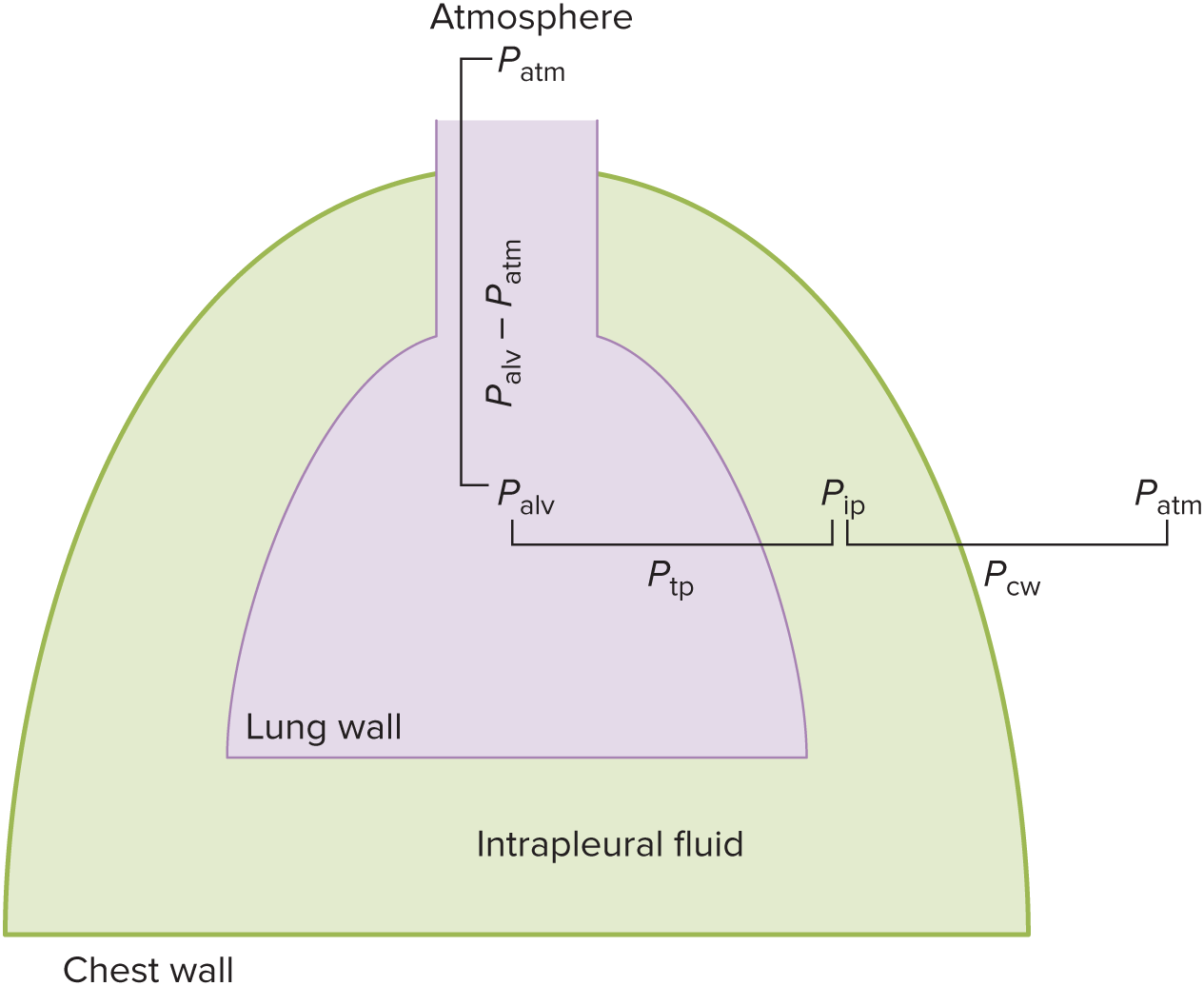
Intrapleural Pressure
__ (Pip), or hydrostatic pressure of the intrapleural fluid causes lungs and thorax to move in and out together during normal breathing
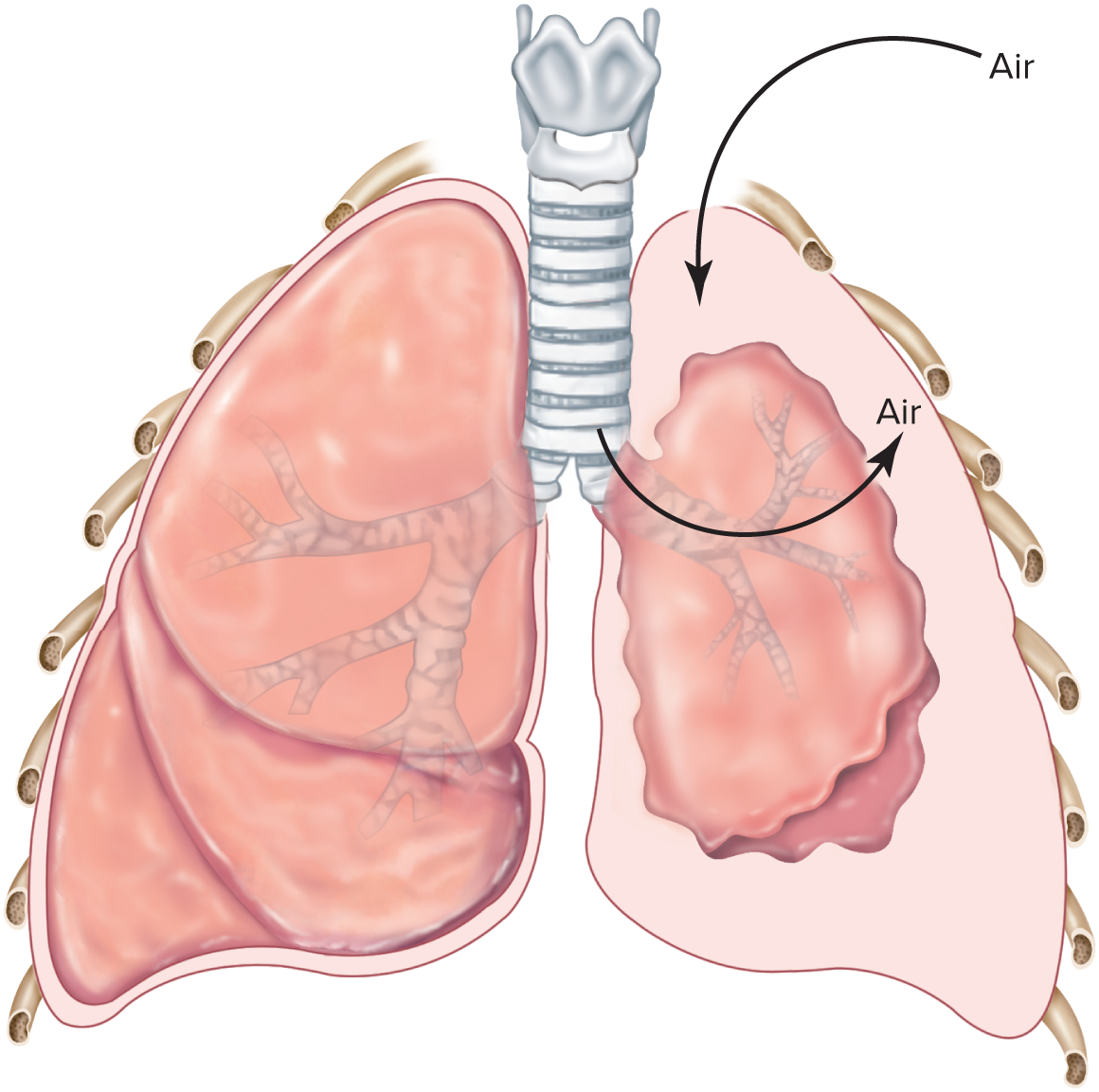
Pneumotharx
Collapsing of lungs that occurs during surgery or trauma when chest wall is pierced without damaging lung and atmospheric air enters intrapleural space (Pip= -4 mmHg → 0 mmHg)
i.e. Pip = Patm or Pip becomes positive/higher pressure than Palv
→ Ptp = Palv - Pip = + -(+) = 0 (eliminated)
→ moves across wall towards lower pressure (Palv) → collapsing of lungs
elastic recoil
Defined as the tendency of an elastic structure to oppose stretching or distortion.
Why:
lungs at rest/stretch tend to collapse.
chest wall at rest/compression tends to expand
Tendencies of collapsing/expanding causes enlargement of intrapleural space between lung & chest wall
Maintained Pip= -4 mmHg counteracts their tendency to collapse/expand
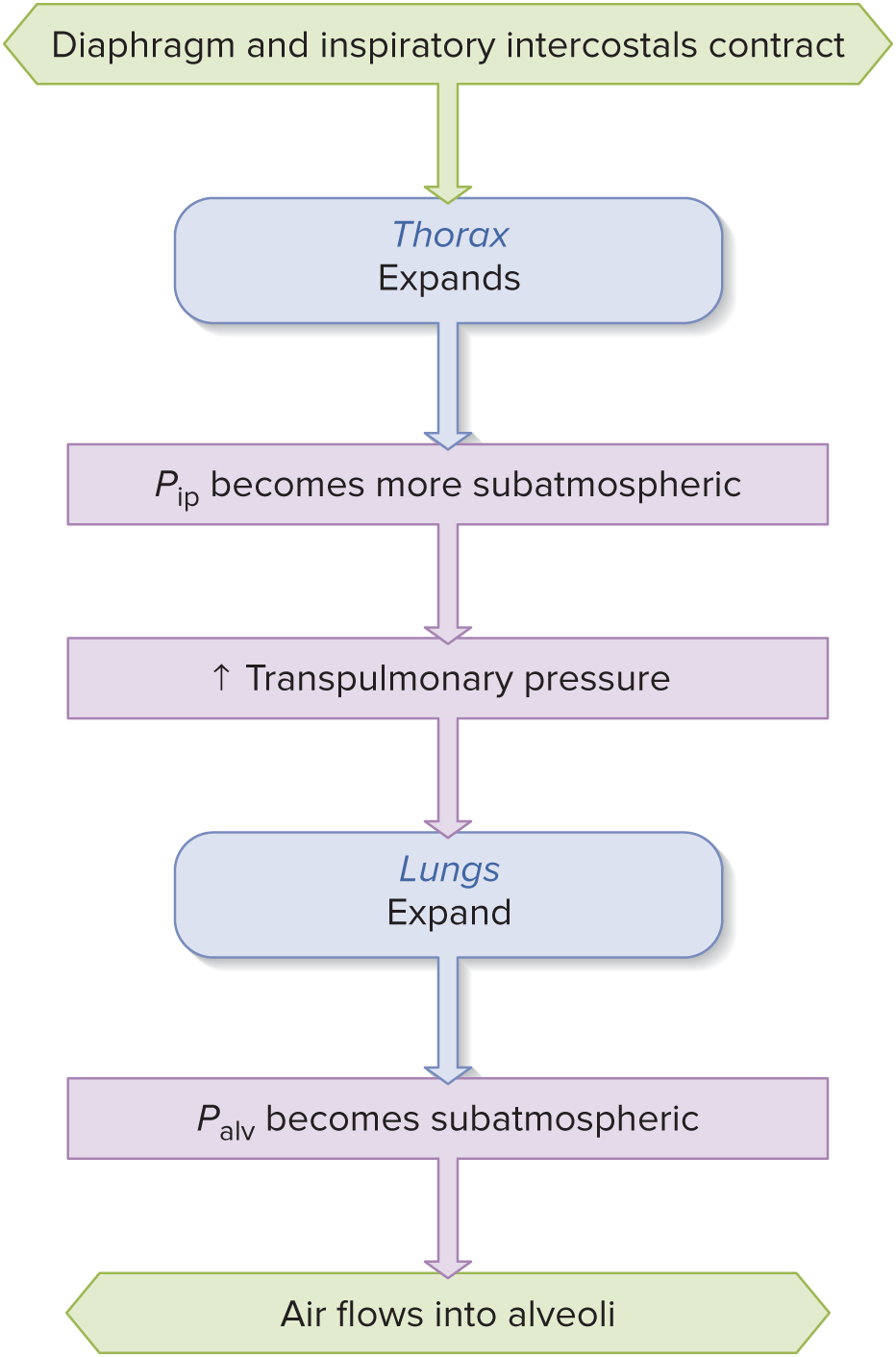
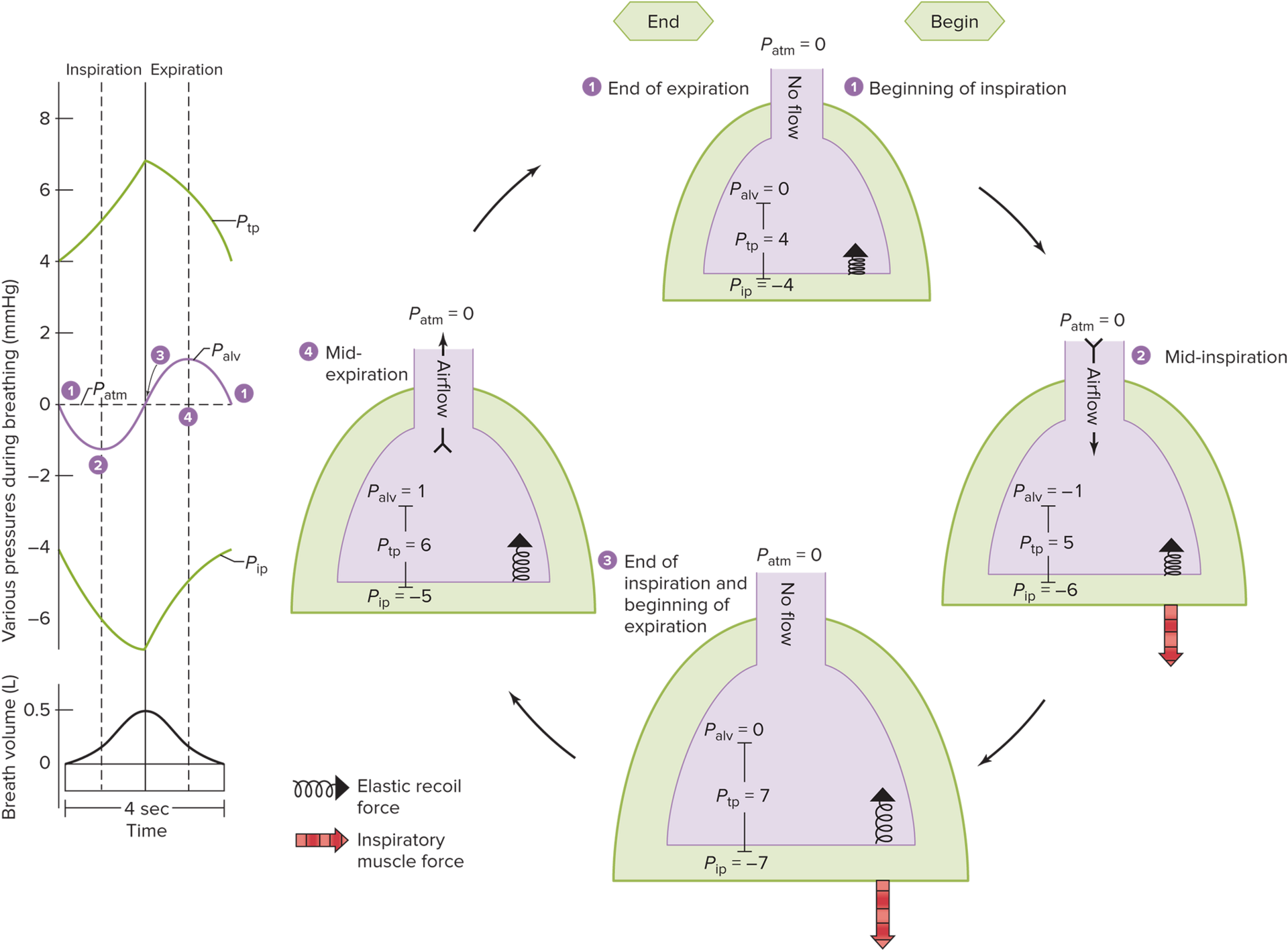
Inspiration
__ is initiated by contraction of diaphragm (phrenic nerve) and external intercostal muscles (motor neurons)
Enlargement of thorax
Pip decreases due to Boyle’s law
Ptp = Palv -( -Pip) = more positive/inc.
Lungs expand
Palv decreases
Air flows into lungs (as Palv < Patm )
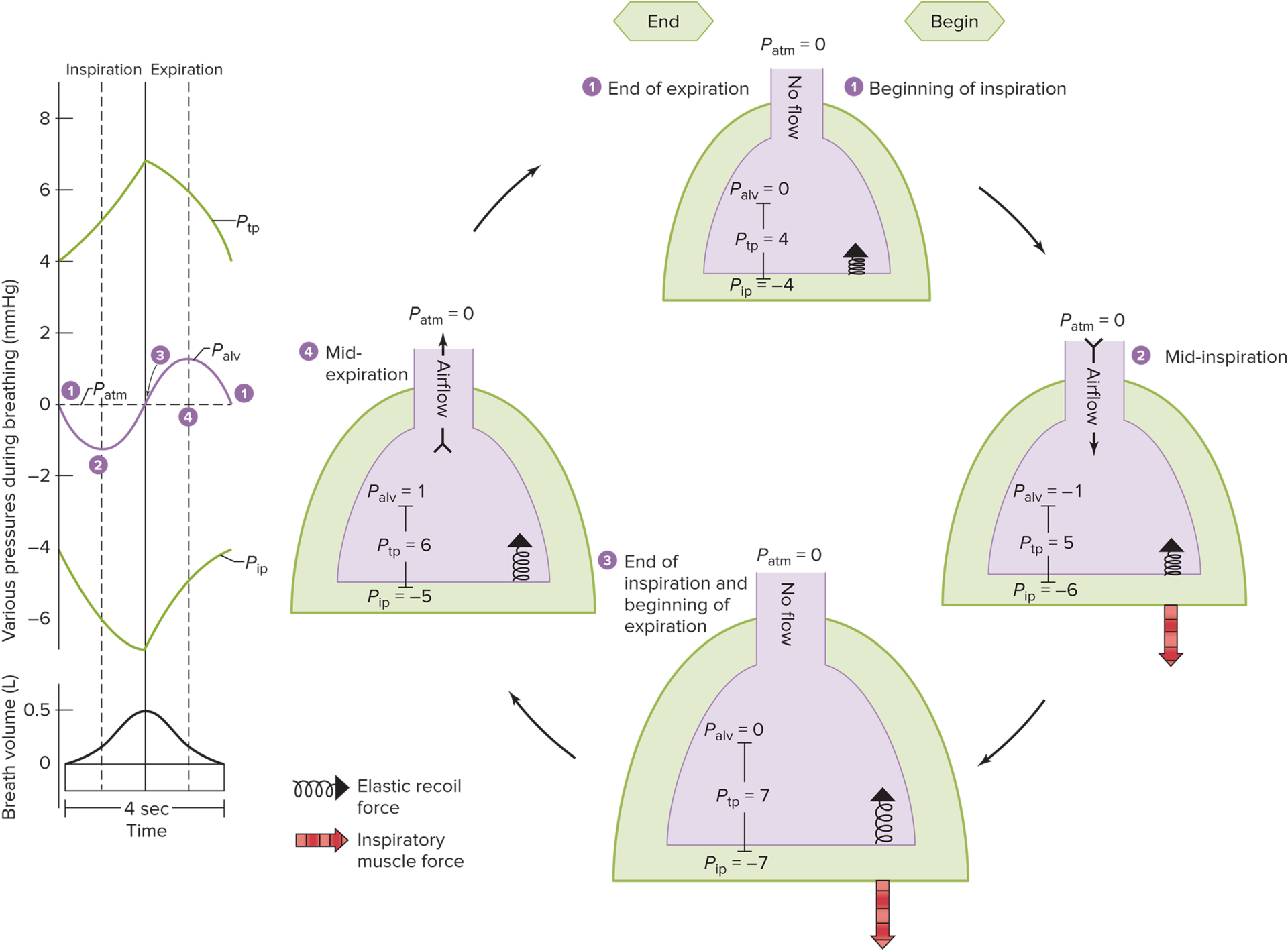
Ceases __ when:
Palv = P atm (equilibrium; no more pressure change needed for flow)
Ptp= elastic recoil opposing it (can no longer expand lungs)
Expiration
__ is initiated by relaxation of diaphragm and external intercostal muscles (decreased firing of motor neurons)
Shrinking of thorax and diaphragm
Pip increases
Ptp = Palv -( + Pip) = more negative/dec.
Lungs shrink as Ptp < elastic recoil of lungs
Palv increases
Air moves out (as Palv > Patm)
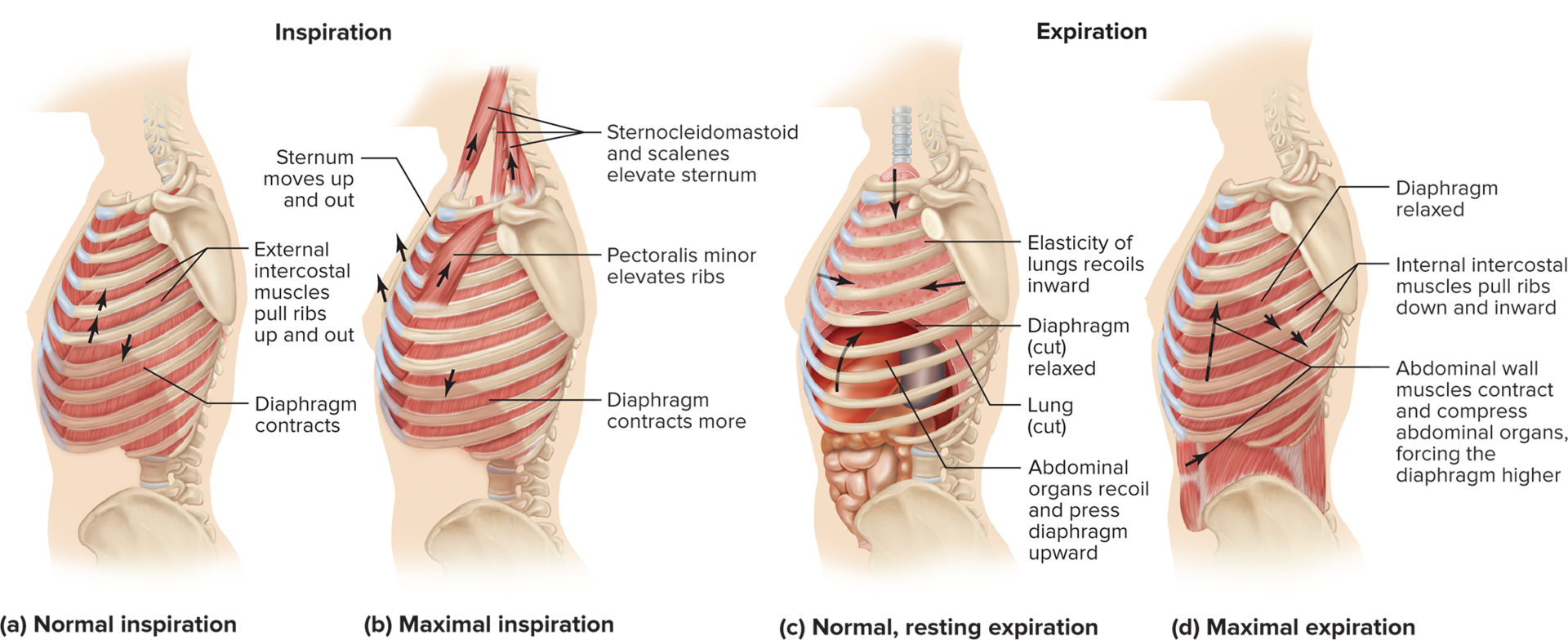
Abdominal
During inspiration:
diaphragm contracts down
external intercostals (+pectoralis minor) pull ribs upwards and out
Sternum is elevated by sternocleidomastoid and scalenes
During exhalation:
diaphragm is relaxed and __ organs/wall/muscles press against diaphragm
internal intercostals pull ribs downwards and inwards
elasticity of lungs causes inward recoil
passive
Lungs are __ elastic structures and their volume depends on:
transpulmonary pressure Ptp: difference in pressure inside and outside lung
Lung compliance: how stretchable lungs are, determining how much they expand for given change in Ptp. proportional to Ptp
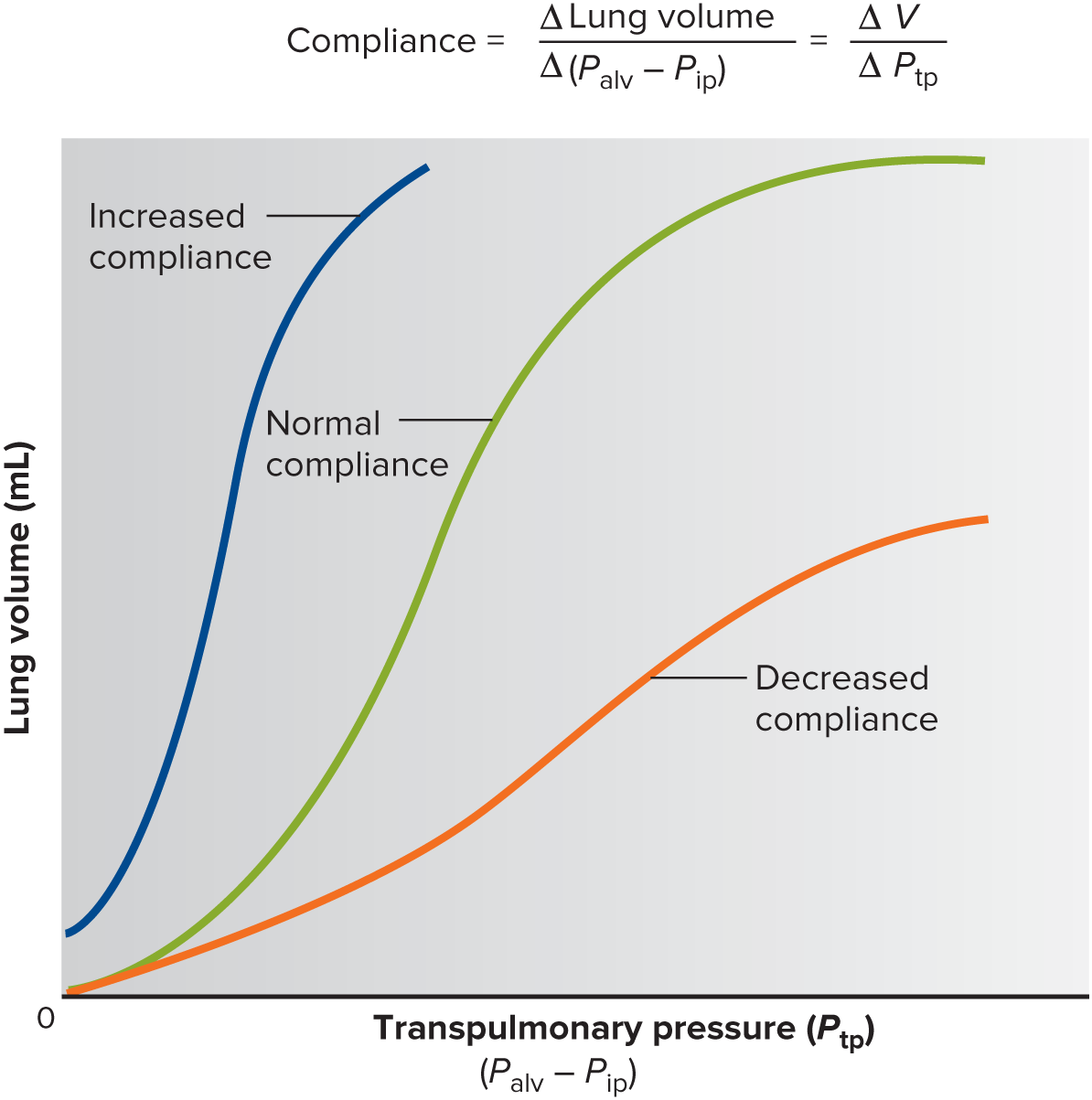
Lung Compliance
CL and or __: magnitude of change in lung volume produced by given change in transpulmonary pressure.
Impacted by:
(1) stretchability of lung tissue
(2) surface tension of air-water interfaces in alveoli
the greater the __, the easier it is to expand the lungs
→ more change in vol. with lesser pressure change (lungs not fully expanded)
the lower the __, the harder (stiffer) it is for lung expansion
→ less change in vol. with greater Ptp (lungs already expanded from high Ptp)
need more subatmospheric/smaller Pip to make lung move overall
→ i.e,, it needs a smaller intrapleural pressure to cause the movement needed for further expansion (greater Ptp = Palv -(-Pip) = more expansion)
→ does NOT mean that it will make compliance higher (again, increased denominator makes lung less compliant because it is fully expanded!)
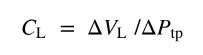
surface tension
inner alveolar cells’ moist water molecules attraction to each other.
adds on additional force lungs have to overcome in order to stretch.
Surfactant (produced by Alveolar Type 2 Cells): detergent-like substance that lowers the __ → increases lung compliance
mixture of lipids and proteins
deep breaths stretch type II cells → increased surfactant secretion
production occurs in late gestation in the fetal lung. stim. by increase of cortisol (glucocorticoid)
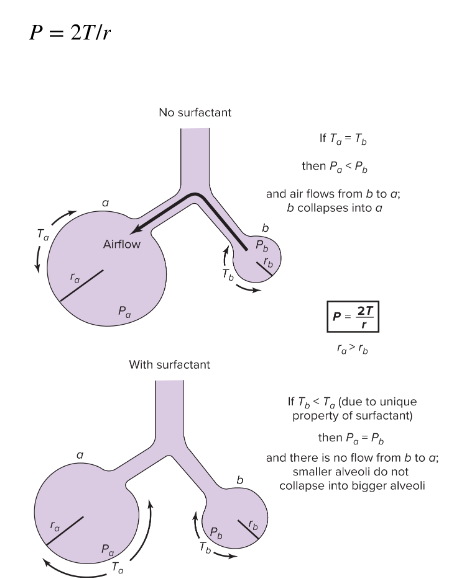
Law of Laplace
This law describes the relationship between:
r = alveolus radius
decreased r → increased pressure
P = pressure
T= surface tension
affected by presence of surfactant or not. more effective in small alveoli
with surfactant: no air flow. surfactant reduced T in smaller alveoli (b) such that Tb < Ta & small alveoli matches larger radius alveoli pressures (a)
without surfactant: air flow goes from high pressure (b) to low (a); small alveoli would be unstable and collapse
Respiratory distress syndrome of the newborn
Surfactant deficient disease when newborn is premature
lacks developed Type 2 alveolar cells → can’t breath without strenous efforts
Leading cause of death in premature infants
Asthma
Disease characterized by intermittent episodes of contracted smooth airway muscles from inflammation causing hyperresponsiveness → inc. airway resistance
Therapy for __ aims to:
reduce inflammation with anti-inflammatory drugs (leukotriene inhibitors + glucocorticoids)
reduce excessive muscle contraction with bronchodilator drugs
one class mimics epinephrine action on B-2 adrenergic receptor
another class blocks muscarinic cholinergic receptors → bronchoconstriction
chronic obstructive pulmonary disease
COPD. refers to either the following, or a combination of the two:
emphysema: destruction and collapse of smaller airways
when there’s too much compliance, a decrease in Ptp can lead to lungs to collapse
chronic bronchitis: excessive mucus production in bronchi; inflammation in airways → blockage by accumulation of mucus in airways; thickening of airways
last left off of 13.3 / L29