heart beat, contractility and conductivity
1/129
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
130 Terms
What sides of the heart hands venous and arterial blood ?
Right heart handles venous blood
Left heart handles arterial blood
What is the systemic and pulmonary blood flow route ?
RA → RV (pulmonary)
LA → LV (systemic)
What’s the difference between pulmonary and systemic?
Pulmonary:
low oxygenated blood
Returns highly oxygenated
Low resistance
Systemic:
highly oxygenated blood
Returns low oxygenated (plus Co2)
High resistance
What does resistance determine ?
Required pressure
Pressure determines wall thickness
What are the 3 layers of the heart wall?
pericardium
Myocardium
Endocardium
What is the pericardium/pericardial sac and what does it do?
tough dense connective tissue that protects the heart and maintains position (anchor within thorax)
Cavity provides lubricatin
Prevents excessive dilation + reduces friction
What is the epicardium?
Fibroelastic connective tissue
What is the myocardium?
Muscle tissue
What is the composition of the myocardium?
Composed of branching cardiac myocytes arraged in spirals
Spiral arrangement produces ringing contraction (twisting motion that increases efficacy of blood ejection)
What is the endothelium?
provides smooth endothelial surface
Minimises turbulence + clot formation
Describe the left ventricular musculature vs the right ventricular musculature
Left musculature:
systemic circulation
Much thicker
Overcome systemic resistance
High pressure
Right musculature:
pulmonary circulation
Reduced thickness
Lower pulmonary resistance
Lower pressure
Why is the left ventricular musculature much thicker?
As systemic vascular resistance higher than pulmonary resistance
To eject blood into systemic circulation, left ventricular pressure must exceed aortic pressure
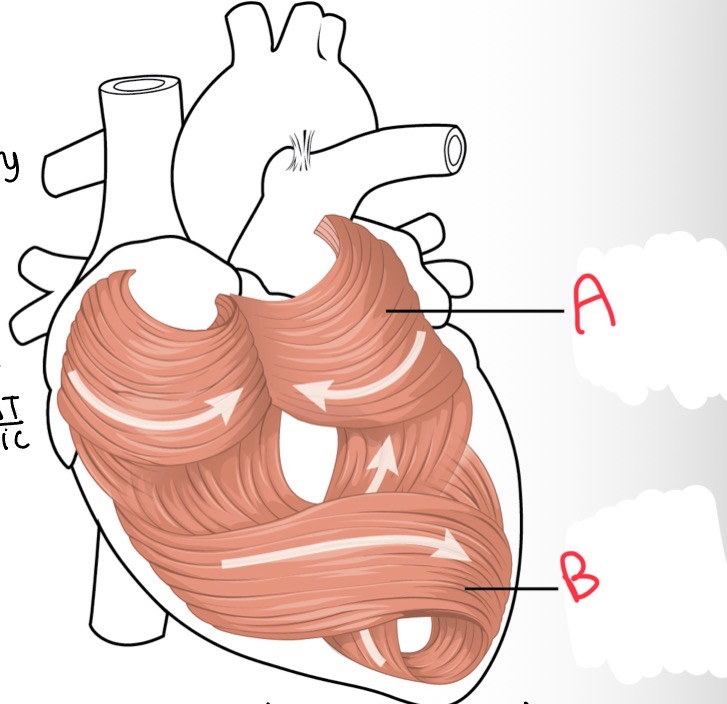
What’s A?
Atrial musculature
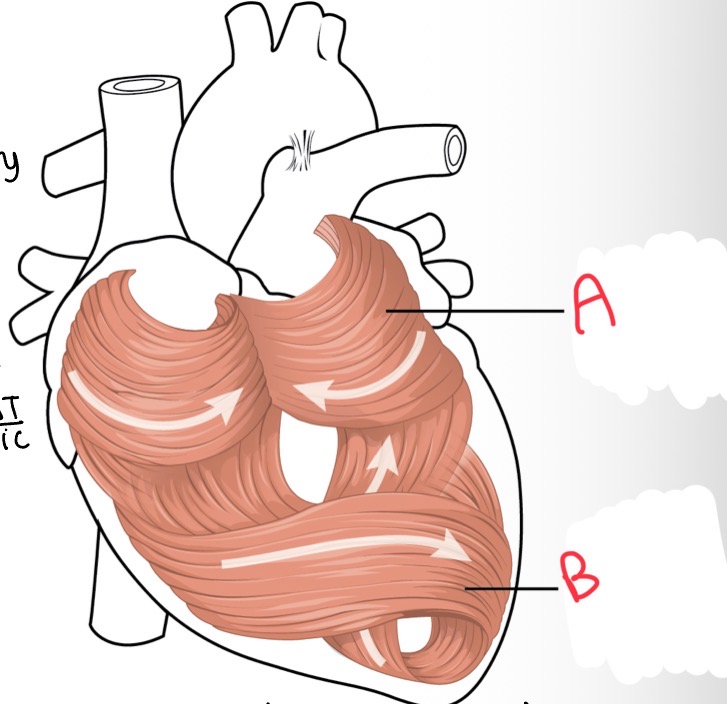
Whats B?
Ventricular musculature
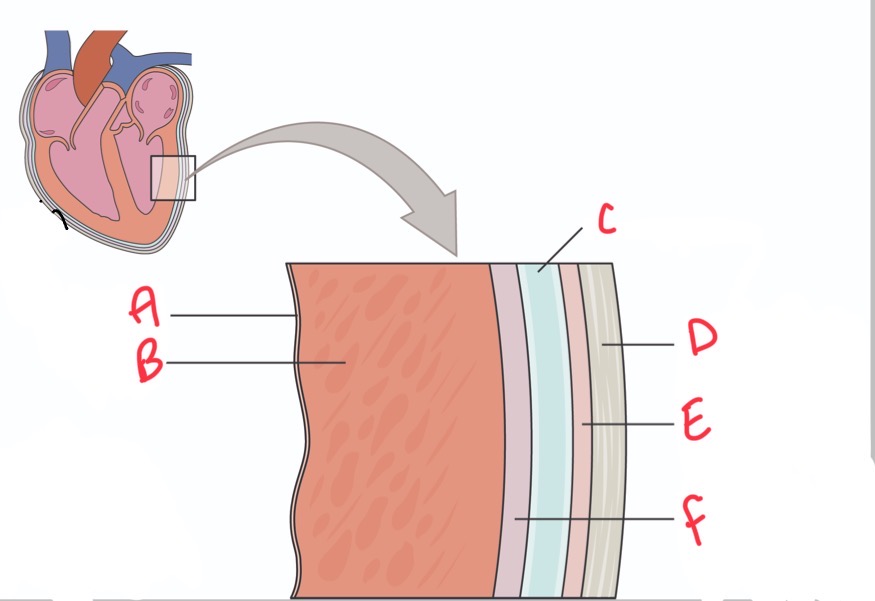
Whats A?
Endocardium
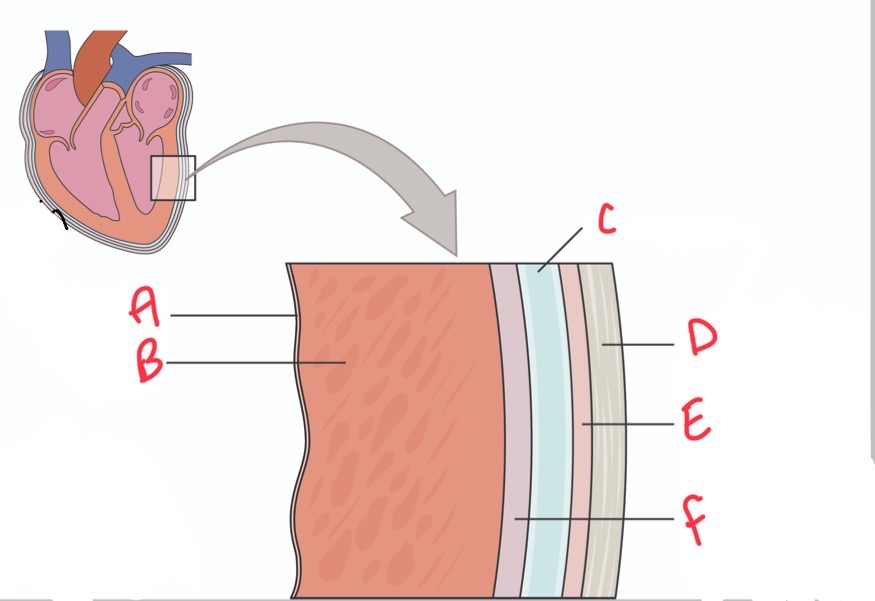
What is B?
Myocardium
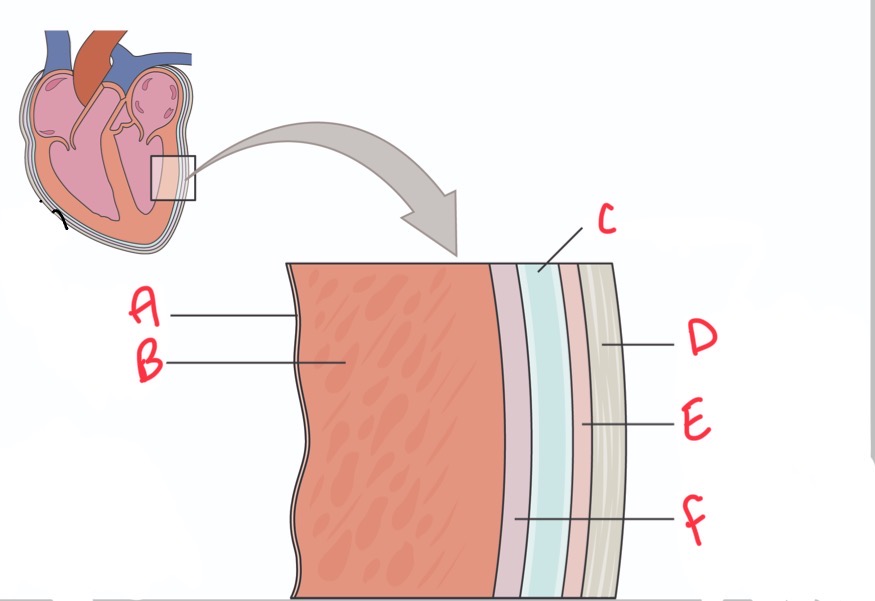
Whats C?
Pericardial activity
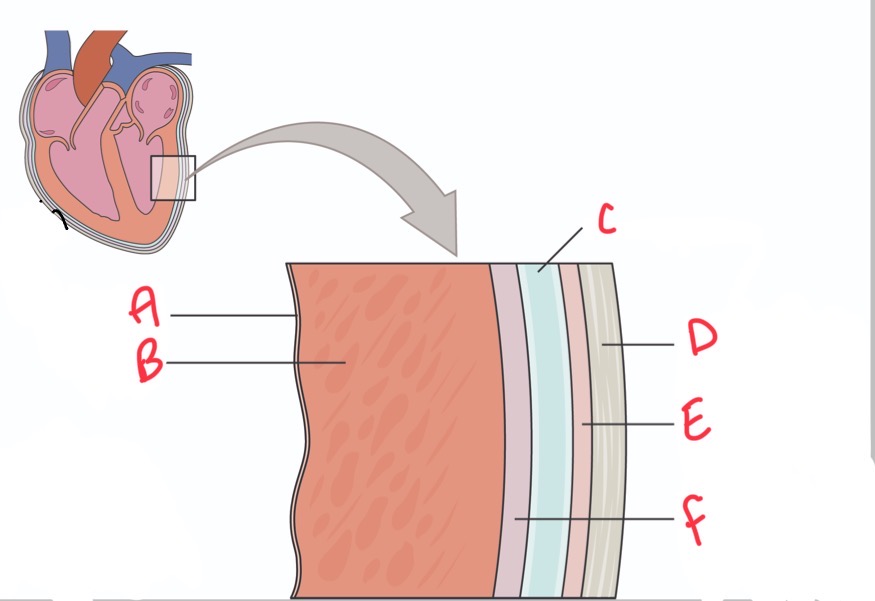
Whats D?
Fibrous pericardium
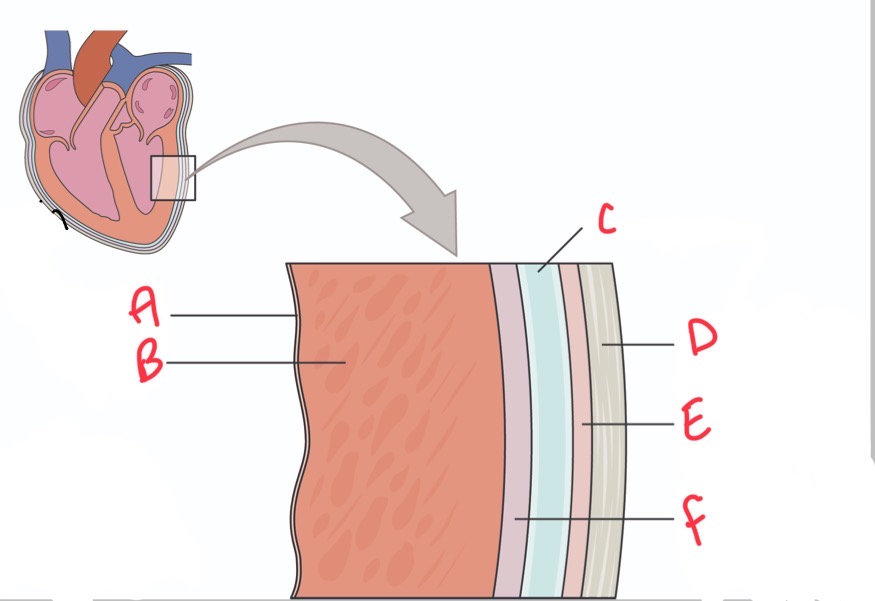
Whats E?
Parietal layer of serous pericardium
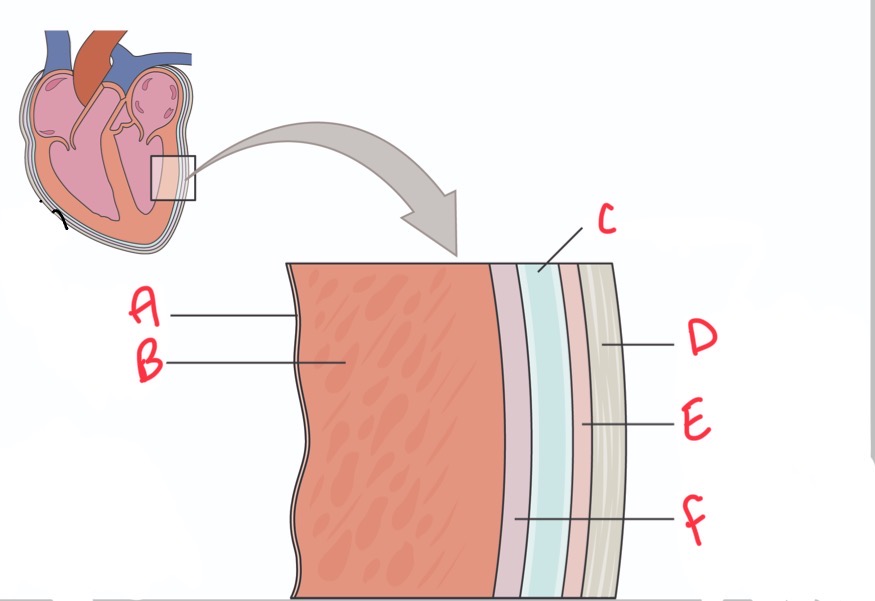
Whats F?
Epicardium (visceral layer of serous pericardium)
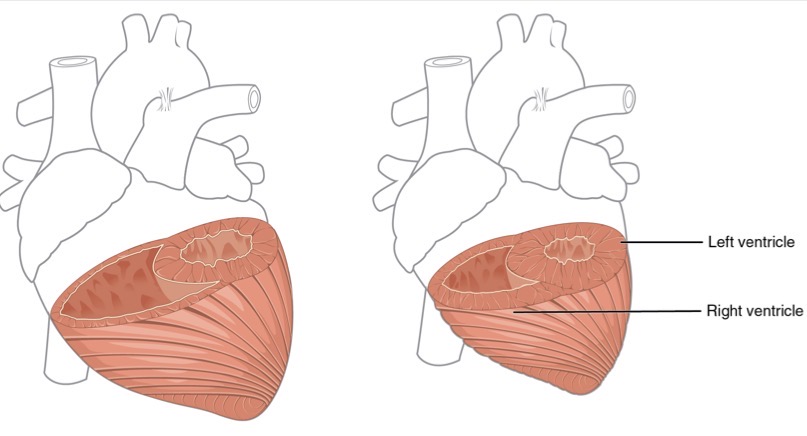
Which is contracted which is relaxed?
Relaxed - left
Contracted - right
What does wall thickness within heart reflect?
Laplaces’ law
What is wall stress proportional to?
(Pressure x radius) / wall thickness
What happens if the pressure increases
Thickness must increase to maintain wall stress
Explains hypertrophy in pressure overload situations
What is the role of the atrioventricular valves and what do they include?
link atria and ventricles
Bicuspid (mitral) LEFT
Tricuspid RIGHT
What is the role of the semilunar valves and what do they include?
link ventricles and aortic and pulmonary arteries
Aortic
Pulmonary
When do semilunar valves open?
When ventricular pressure exceeds arterial pressure
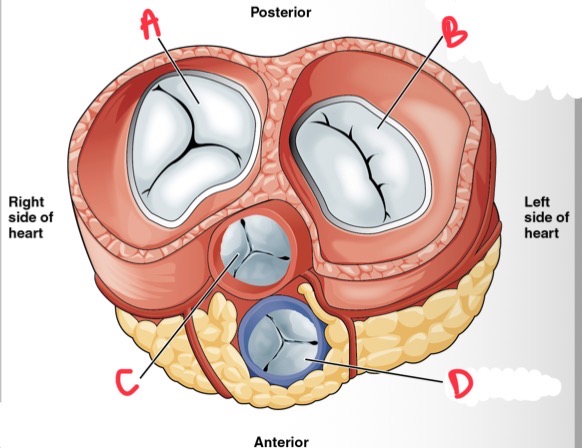
What is A?
Tricuspid valve
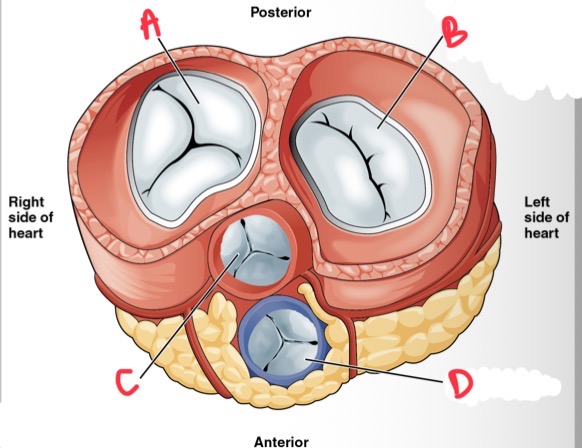
What is B?
Bicuspid (mitral) valve
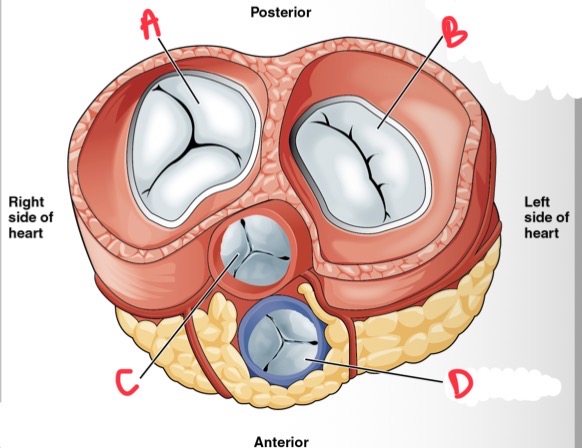
Whats C?
Aortic valve
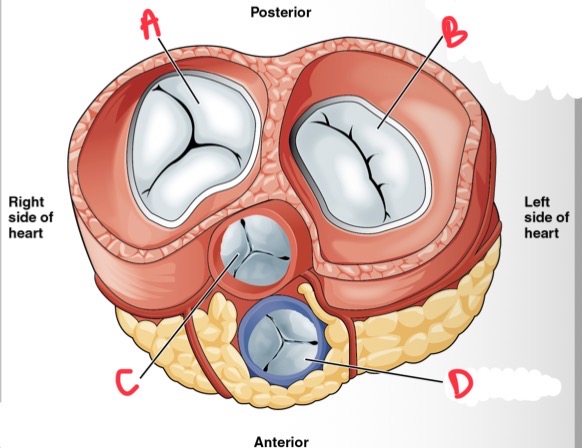
What is D?
Pulmonary valve
Cardiac valves are passive structures, they open and close due to pressure differences, what happens to AV valves when atrial pressure exceeds ventricular pressure?
AV valves open
Cardiac valves are passive structures, they open and close due to pressure differences, what happens to AV valves when Ventricular pressure exceeds atrial pressure?
AV valves close
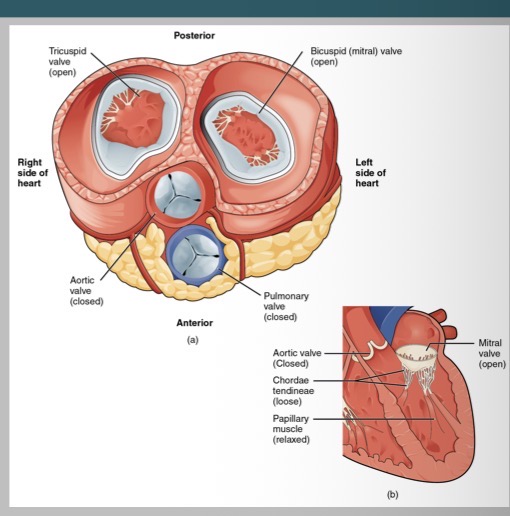
What follows the contraction of the atrial wall?
contraction of atrial wall
Relaxation of chordae tendinae
Enables downward force on valve flaps
Opening of valve
Blood drawn into ventricles from atria
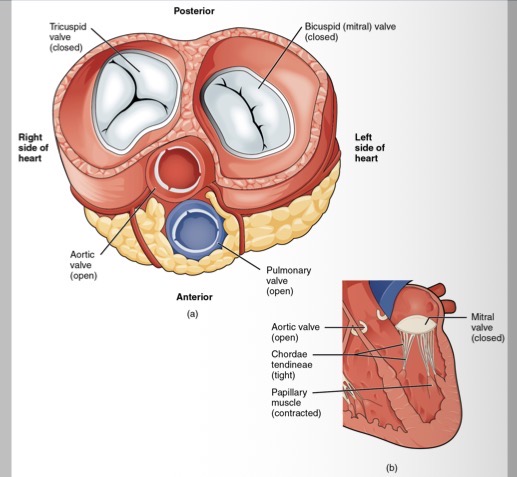
What follows the contraction of the ventricular wall?
contraction of ventricular wall
Stretch chordae tendineae
Mitral valves close
Pressure of blood on semilunar valves
Forces blood from ventricles into arteries
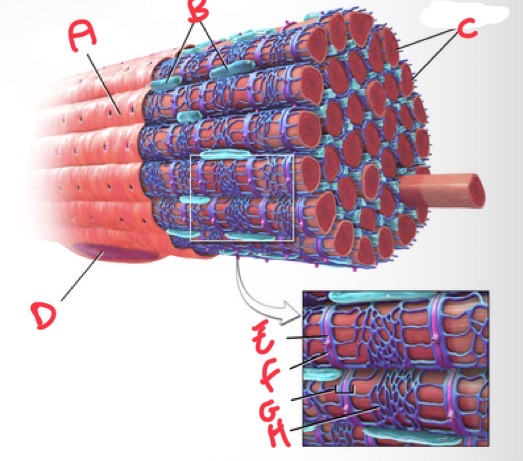
Whats A?
Sarolemma
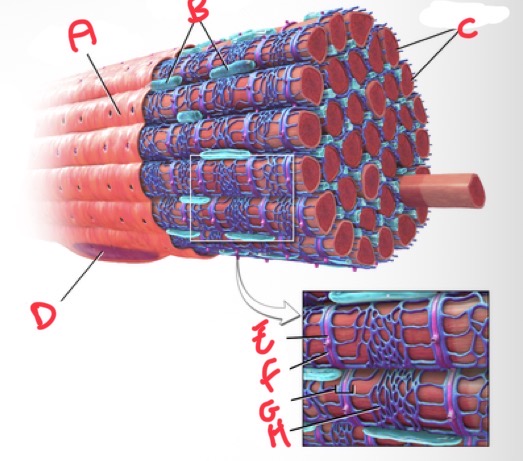
Whats B?
Mitochondria
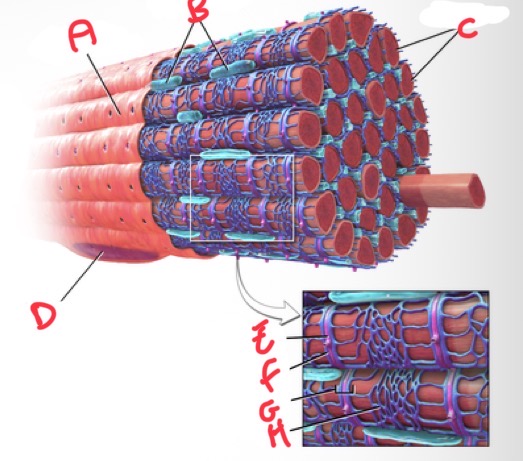
Whats C?
Myofibrils
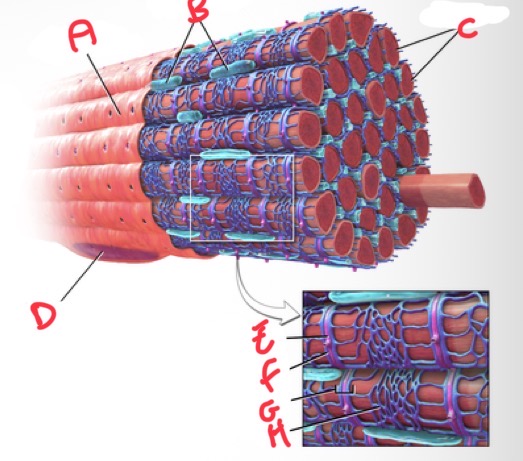
Whats D?
Nucleus
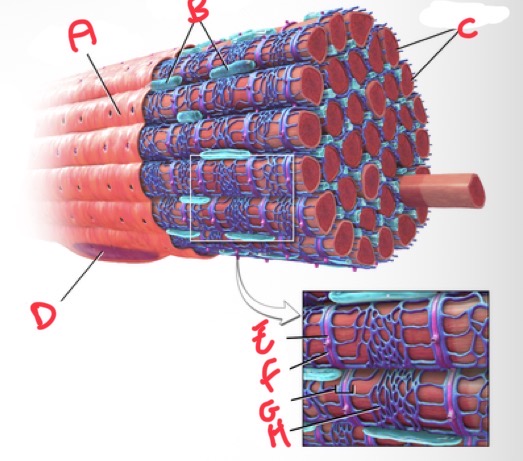
Whats E?
T tubule
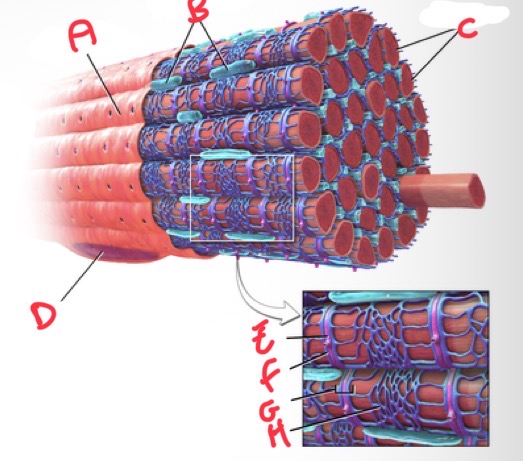
Whats F?
Terminal cisterna
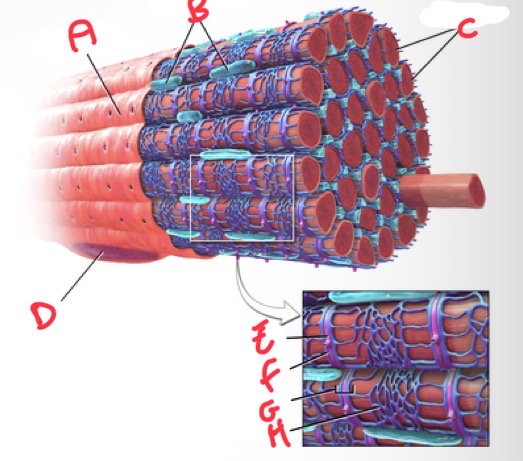
Whats G?
Triad
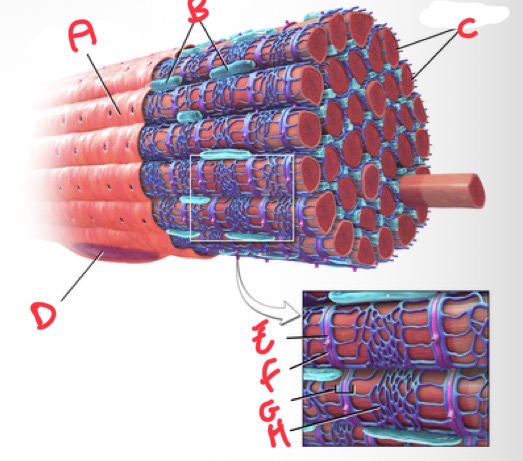
What’s H?
Sarcoplasmic reticulum
What is a muscle fibre ?
Individual unit made up of fibrils
What is an intercalated disc?
link between fibres
Contain desmosomes for mechanical strength and gap junctions for electrical coupling
intercalated disks contain gap junctions, what effect does this have?
Myocardium behaves as functional unit therefore depolarisation spreads rapidly between cells ensures coordinated contraction
What are T tubules?
Run through muscle to provide electrical and chemical link
What is the sarcoplasmic reticulum ?
Calcium store to aid contraction
Whats a sarcomere ?
Smallest unit of muscle contraction
What are thin filaments ?
Actin
Slide to provide muscle contraction
What are thick filaments ?
myosin
Provide the mechanical force
What happens during contraction?
Myosin heads bind to actin, ATP hydrolyses power stroke, filaments slide past each other and sarcomere shortens
Filaments do not shorten, they slide - generates force
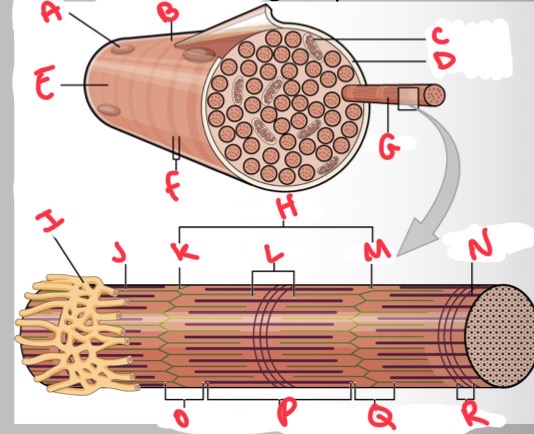
Whats A?
Nucleus
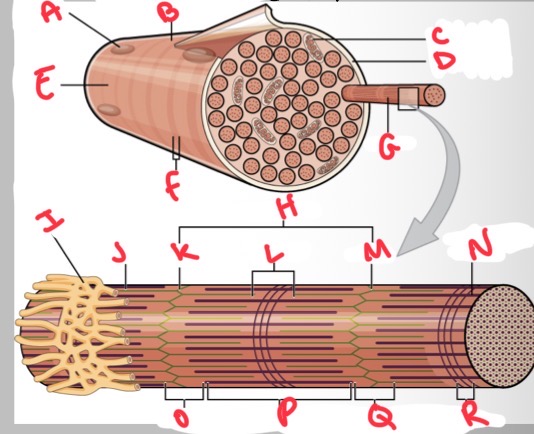
Whats B?
Muscle fibre
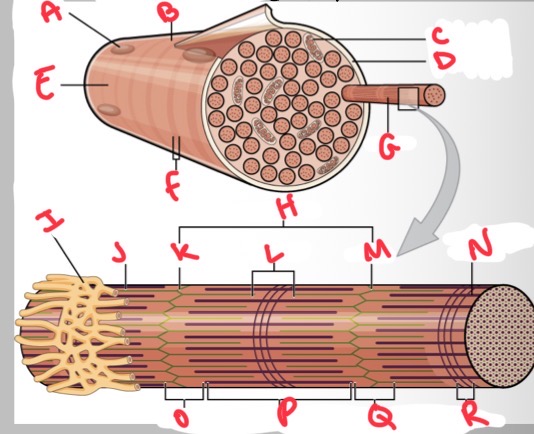
Whats C?
Mitochondria
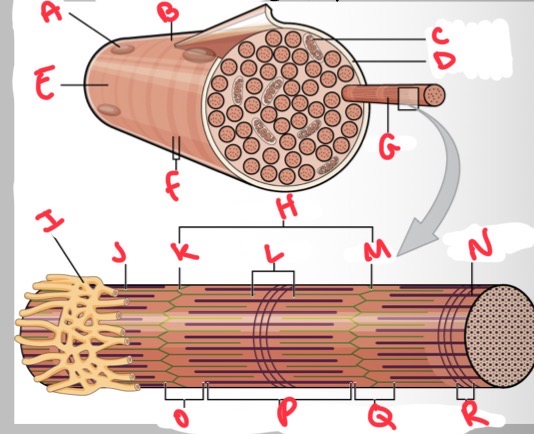
Whats D?
Sarcolemma
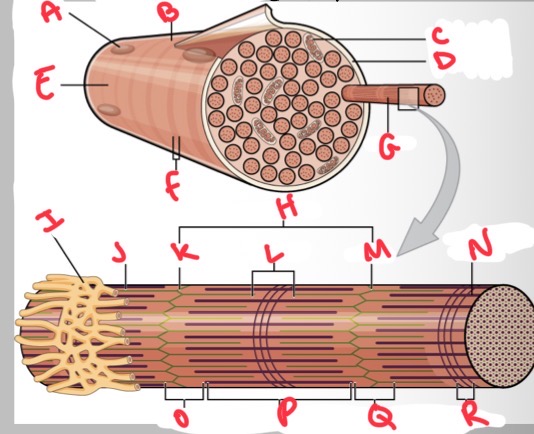
Whats E?
Light I band
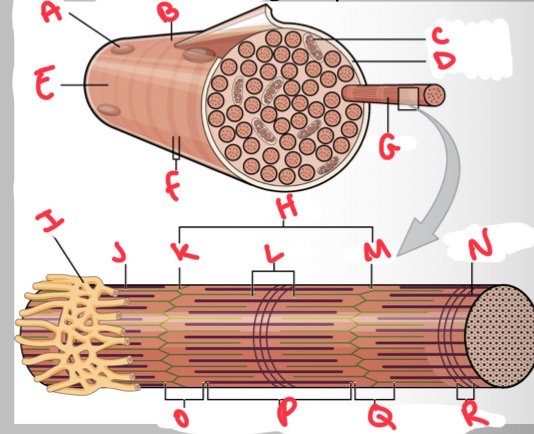
Whats F?
Dark A band
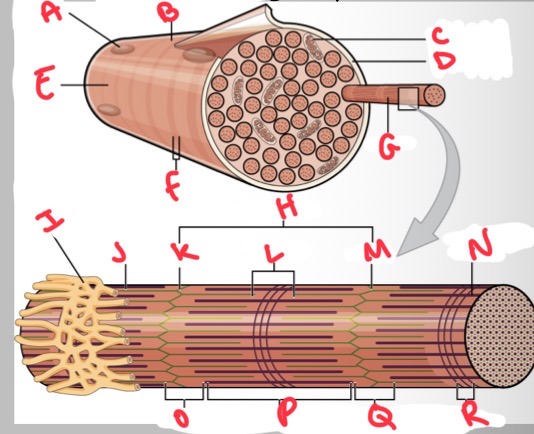
Whats G?
Myofibril
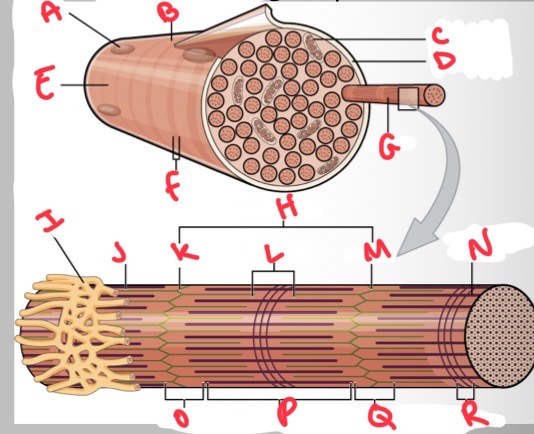
What’s H?
Sarcomere
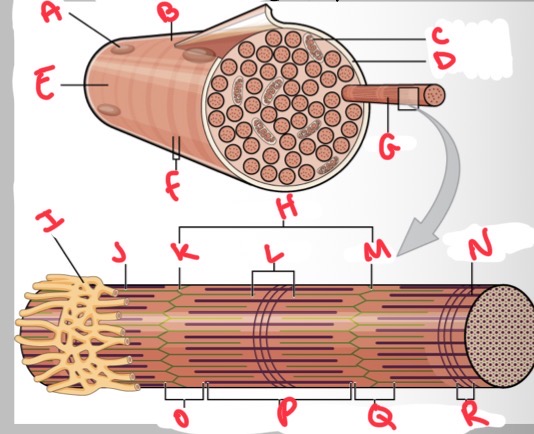
Whats I?
Sarcoplasmic reticulum
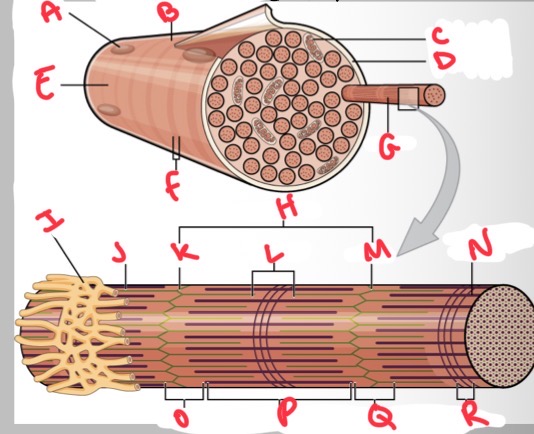
Whats J?
Thin (actin) filament
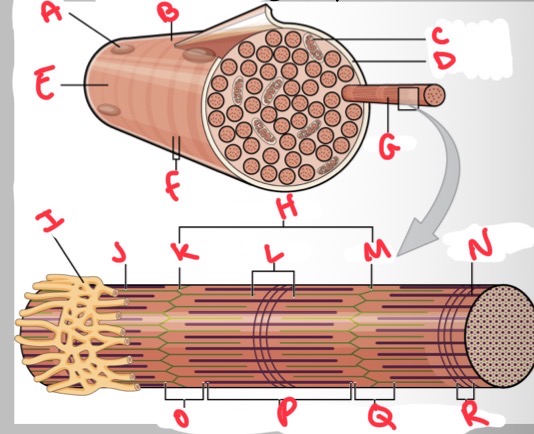
Whats K?
Z disc
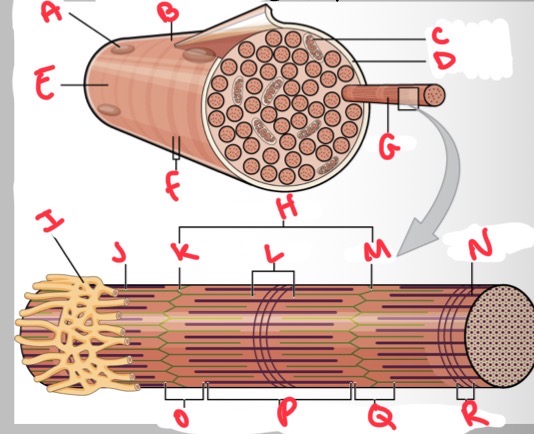
Whats L?
H zone
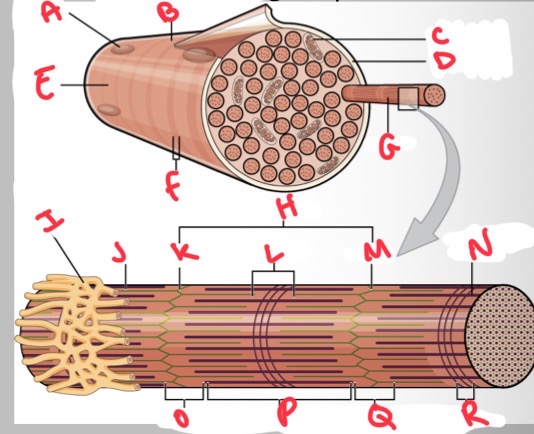
Whats M?
Z disc
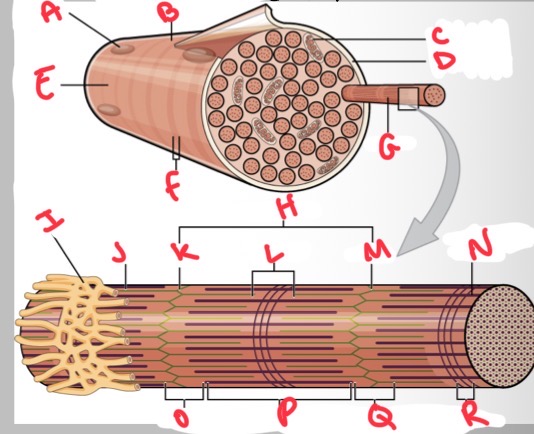
Whats N?
Thick (myosin) filament
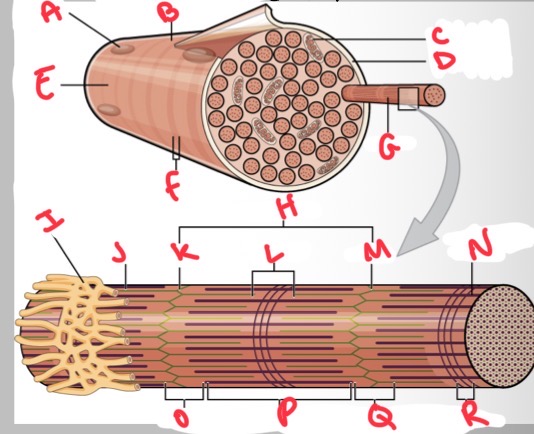
What’s O?
I band
Whats P?
A band
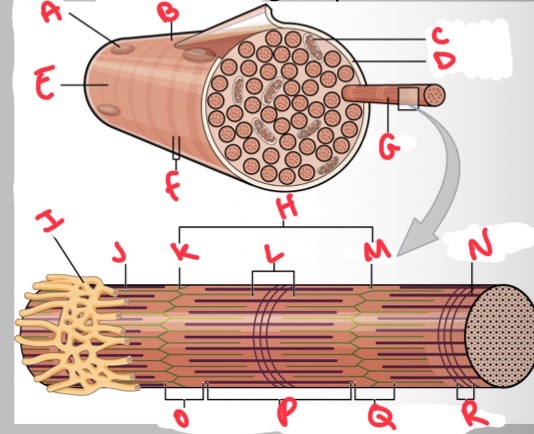
Whats Q?
I band
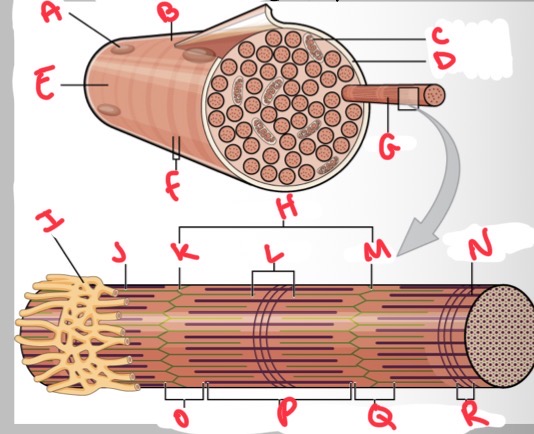
What’s R?
M line
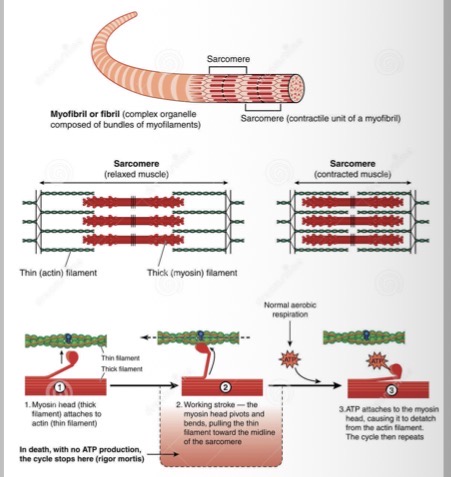
How does contraction occur (simple explanation)
myosin head on thick filament binds to actin
Myosin head pivots (power stroke)
Thin filaments pulled towards the midline
Myosin head detaches from the actin
Cycle repeats
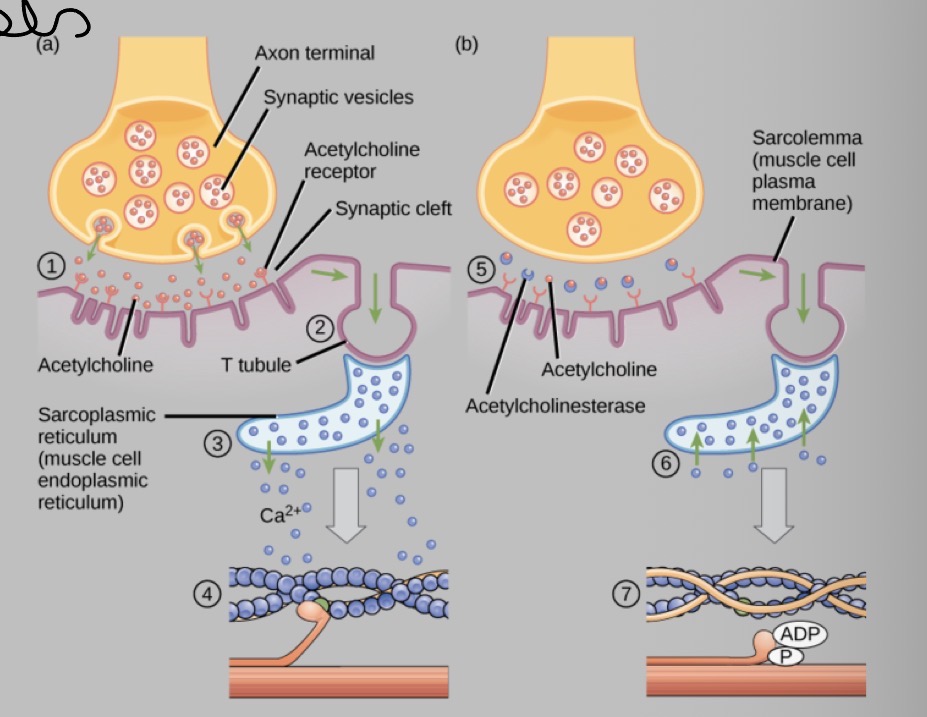
Describe the process of contraction using the diagram
1) acetylcholine released from the axon terminal binds to receptors on the sarcolemma
2) an AP is generated and travels down the T tubule
3) Ca2+ is released from the sarcoplasmic reticulum in response to the change in voltage
4) Ca2+ binds troponin. Cross-bridges form between actin and myosin
5) acetylcholinesterase removes acetylcholine from the synaptic cleft
6) Ca2+ is transported back into the sarcoplasmic reticulum
7) Tropomyosin binds active sites on actin causing the cross-bridge to detach
Acetylcholine stimulates post synaptic receptors on cardiac muscle, what follows this ?
Electrical depolarisation opens voltage gated Ca2+ channels
Membrane depolarisation spreads via the T Tubules
Small calcium influx triggers release of larger calcium fr sarcoplasmic reticulum
Calcium initiates myosin head binding and contraction
Cycstoic calcium binds to troponin C , what does this cause?
troponin changes confirmation
Tropomyosin moves
Myosin binding sites exposed
Cross-bridge cycling begins
Contraction occurs
Relaxation requires calcium removal. Why and how ?
reuptake to SR (sarcoplasmic reticulum)
Extrusion via sodium calcium exchanger
Without proper Ca2+ handling = contraction fails
What is sinoatrial (SA) node?
Primary pacemaker
What is bachmans bundle?
Links left and right atria
What is the atrioventricular (AV) node?
Secondary pacemaker
Whats the bundle of his ?
Links AV node to intraventricular septum
What is the right and left bundle branches?
Innervate ventricles
What is the role of the SA node?
Specialist cells that spontaneously depolarise to allow atrial contraction to complete before ventricular contraction begins
How does the SA node allow atrial contraction to complete before ventricular contraction begins ?
specialist cells that spontaneously depolarise
These impulses spread through atrial myocardium, reaches atrioventricular node, has a delay (approx 100milliseconds)
This delay allows atrial contraction to complete before ventricular contraction begins
Why is rapid coordinated activation important?
Ensuresheart has efficient ejection of blood
Where does the impulse travel after it allows atrial contraction to complete before ventricular contraction begins ?
Down bundle of his, left and right bundle branches + Purkinje fibres , distribute depolarisation rapidly through the ventricles
How long is the delay that lows atrial contraction to complete before ventricular contraction?
Approx 100 milliseconds
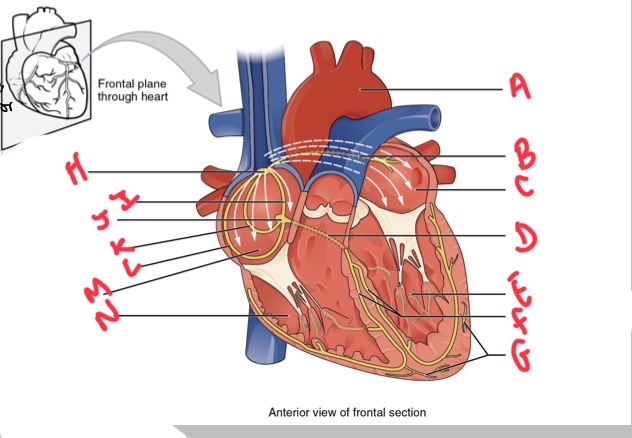
Whats A?
Arch of aorta
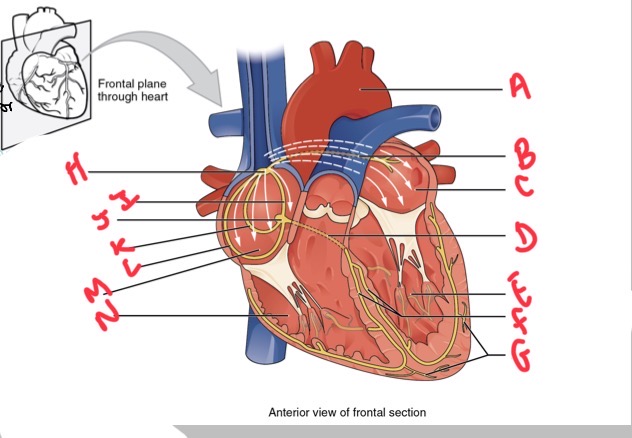
Whats B?
Bachmans bundle
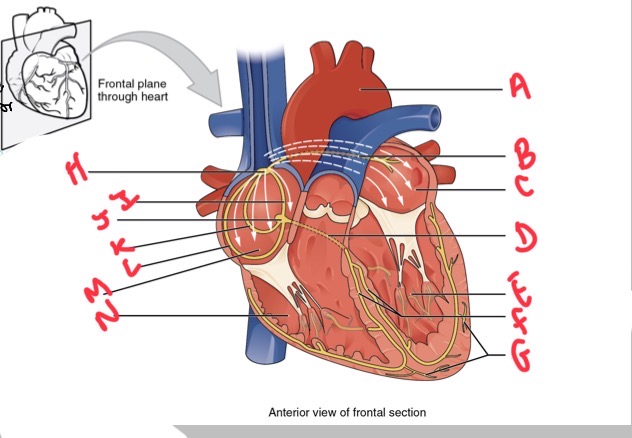
What’s C?
Left atrium
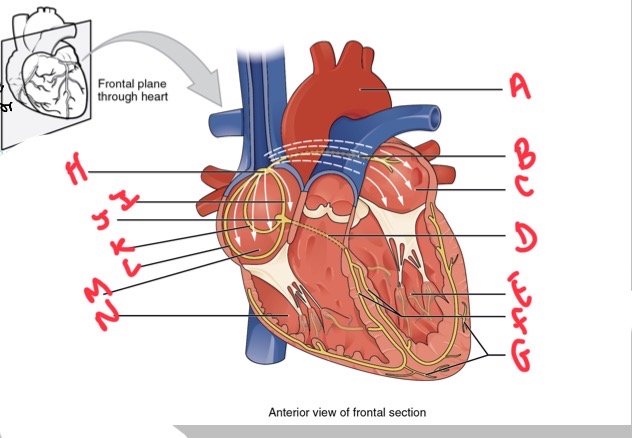
Whats D?
Atrioventricular (AV) bundle (bundle of his)
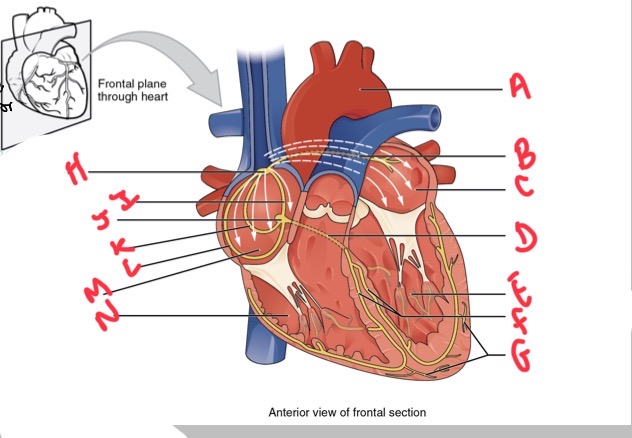
Whats E?
Left ventricle
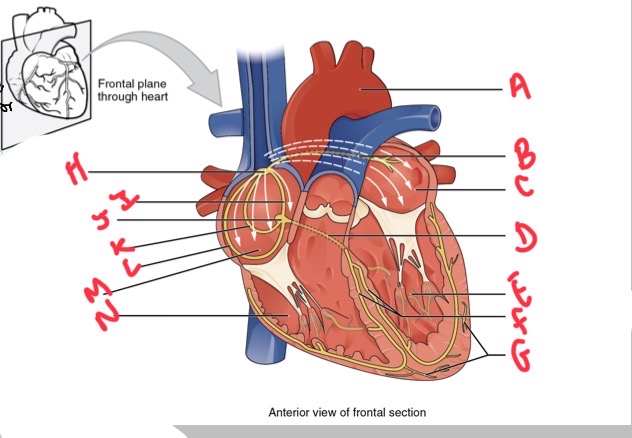
Whats F?
Right and left bundle branches
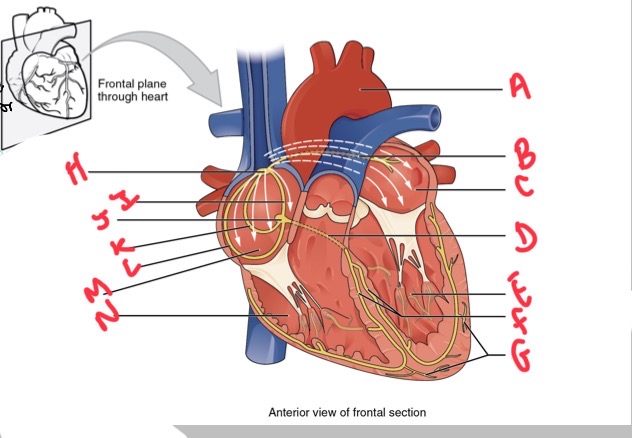
Whats G?
Purkinje fibres
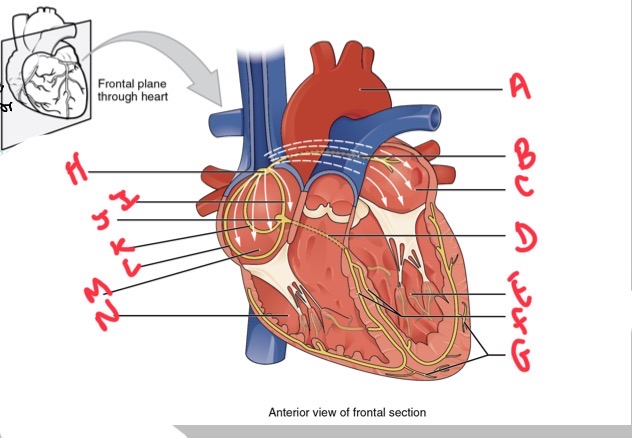
What’s H?
Sinoatrial (SA) node
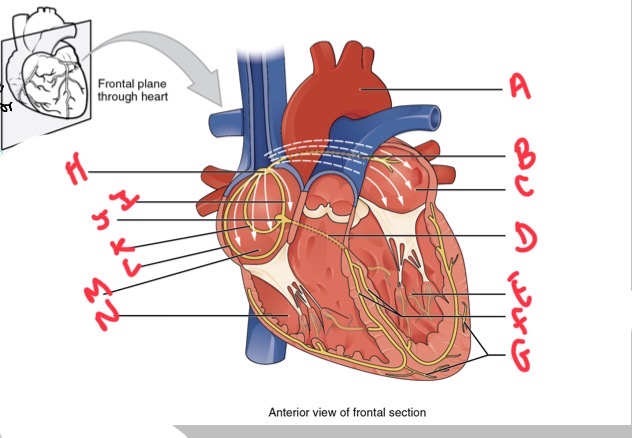
Whats I?
Anterior internodal
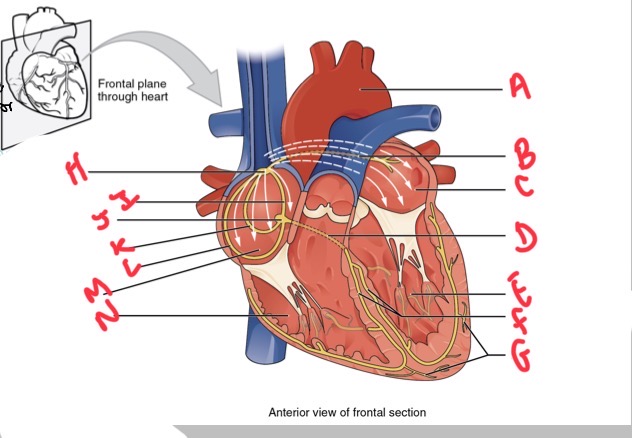
Whats J?
Atrioventricular (AV) node
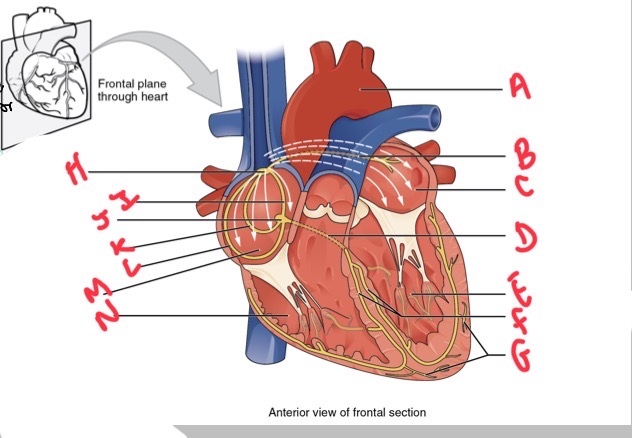
Whats K?
Middle internodal
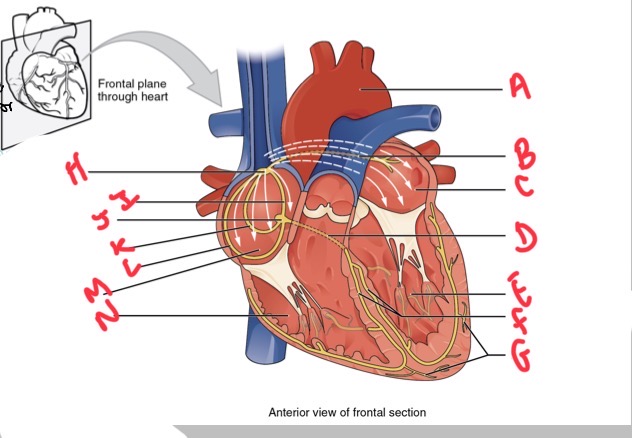
Whats L?
Posterior internodal
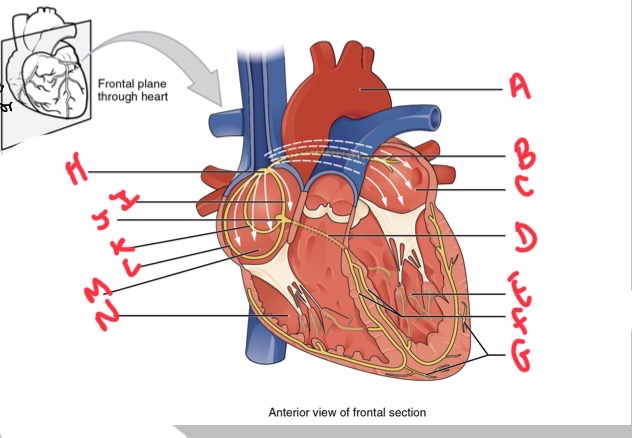
Whats M?
Right atrium
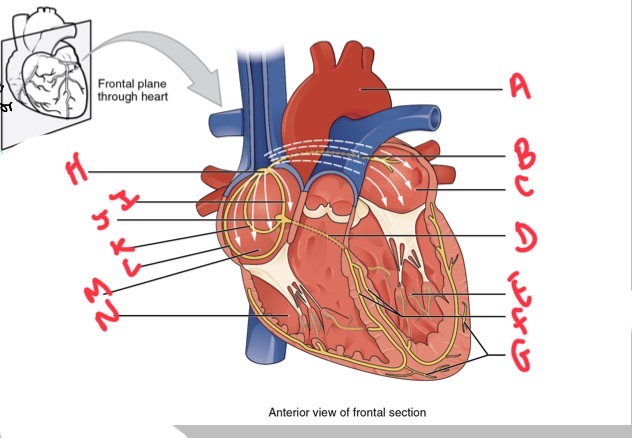
Whats N?
Right ventricle
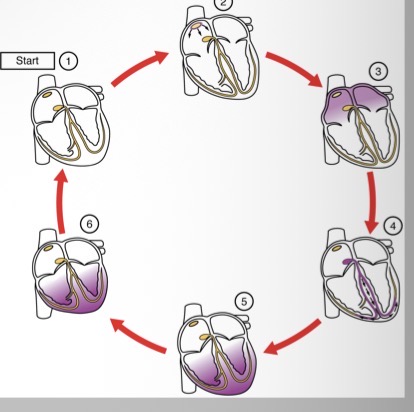
Describe how ventricular contraction begins
1) SA node and the remainder of the conduction system are at rest
2) SA node initiates the action potential which sweeps across the atria
3) after reaching the atrioventricular node, there is a delay of approximately 100ms that allows the atria to complete pumping blood before the impulse is transmitted to the atrioventricular bundle
4) the impulse travels through the atrioventricular bundle and bundle branches
5) the impulse spreads to the contractile fibres of the ventricle
6) ventricular contraction begins