Host-virus interaction
1/25
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
26 Terms
Host-virus interaction
Viral and host processes that occur during viral infection which enable both partners to respond to each other
Virulence
Degree of pathogenicity of a micro-organism and the severity of the caused disease
Opportunistic pathogen
Micro-organism that can become pathogenic in certain situations, particularly when the host’s defenses are disturbed
Latrogenic transmission
During medical procedures
Syringes, blood-derived drugs, transplants
HIV, HBV, HCV
Portals of entry for infection
Respiratory airway
Alimentary tract
Conjunctive
By inoculation (bires, IV injection)
Cutaneous route (with and without injury)
Urogenital tract (sexually transmitted)
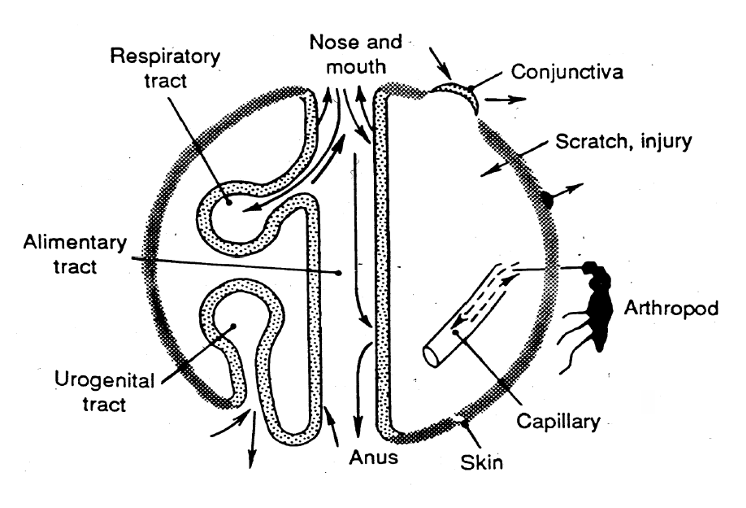
Release of the virus from the body
Saliva (EBV, CMV)
Respiratory secretions (flu)
Stool (rotavirus)
Urine (CMV)
Skin rash (VZV)
Blood (HIV, HBV)
Maternal milk (HIV)
Genital secretions (HIV)
Localized infection
Primary replication of the virus at a site near the entry site
Factors restraining localized infections
Temperature sensitivity of the virus
Lack of permissiveness of cells
Polarization of epithelial cells
Viremia
Passage through the lymphatic system, local lymph nodes and blood dissemination
Systemic infection
Reaching the target organ where multiplication leads to disease
Risk factors for viral infections
Extremes ages of life (newborns, elderly)
Pregnancy
Hormonal status
Innate or acquired immune deficiency
Undernutrition and malnutrition
Chronic pathologies
Genetic factors
Travel to endemic factors
Contact with animals
Acute infection
Virus replication
Elimination of the virus by the immune response
Symptomatic or asymptomatic
Persistent infection
Maintaining the viral genome in the cell, no elimination by the immune system
Invisible: no viral antigens, replication in immune cells
Escape to immune response: interference with APC, expression of MHC
Can be latent or chronic
Latent infection
Primary infection, latency, and reactivation
Mainly DNA viruses (CMV, HSV, EBV)
Possible transmission during reactivations
Latency in characteristic virus sites
Chronic infection
Continuous production of the virus, inadequate immune response (HBV, HCV)
Long periods
Persistence sites: organs, lymph nodes, blood
Innapropiate immune response
Transforming infection
Evolution toward cancer (HBV, EBV)
Host disease and infectiousness dynamics
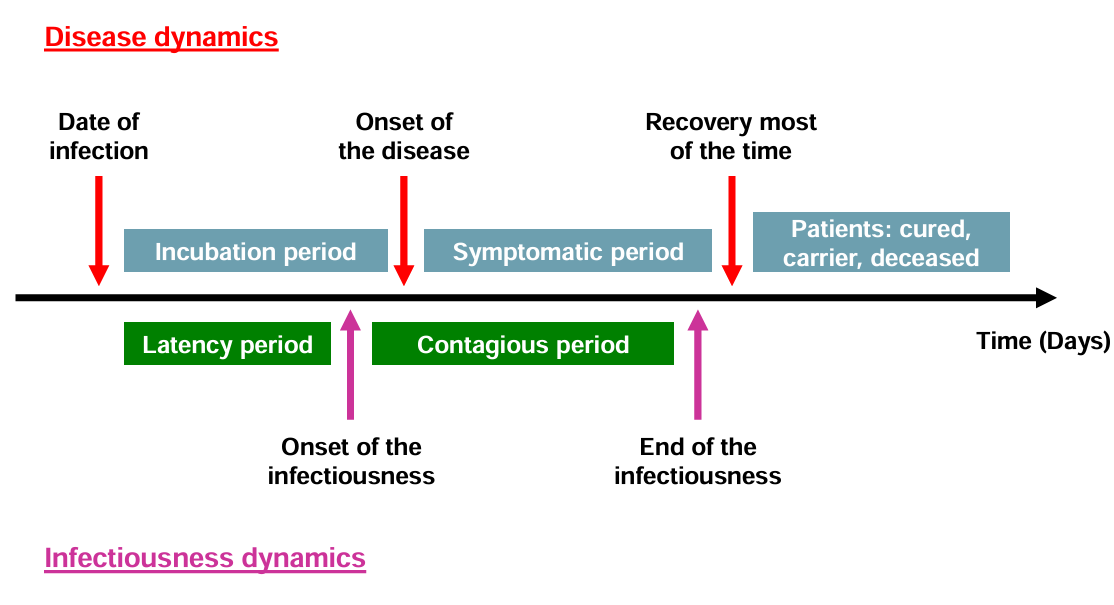
Antibody respone
Primary response: IgM, and slow IgG production, weak affinity
Secondary response: IgG, IgA, strong affinity, memory, somatic hypermutation
Cell- virus interactions
Virus is a parasite
Depend on the cell for the replication of their genome and the production of their components
Divert the functioning of the cell to their benefit
Promote the survival of the host cell
Cell and its antiviral defenses
Innate intracellular mechanisms: RNA interference, apoptosis, autophagy
Soluble immune system factors: interferons
→ stop translation
Adaptative mechanisms
Viral use of cellular machinery
Virus has mechanisms for recruiting, adapting, modifying or usurping cellular machinery
Survival of the virus in the host cell
Virus replication
Cell cycle blocking
Immortalization of cells
Modulation of cell gene expression
Blockage of splicing of the cell mRNA
Antiviral defense
Pattern Recognition Receptors (PRRs) detect viral components
Interferons production, immune cell activation or apoptosis
Viral modulation of the antiviral defense
Viruses produce proteins that act as saboteurs: blocking PRR sensing, halting interferon signaling, or overriding the cell's suicide commands
PKR Activation
Protein Kinase R (PKR) activation via stress or cytokines inducing:
Phosphorylation of eIF2α → translation inhibition
Activation of ADD/Caspase-8 pathway → apoptosis
Release of NF-kB → antiviral genes activation
Inhibition of PKR by many virus
Hiding of dsRNA via proteins (NS1 or σ3) → no PKR activation
US11 blockage
Mimic of eIF2α via K3L → no eIF2α phosphorilation