NCM 109: Acquired Heart Disease and Inflammatory Disorders
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
45 Terms
Congestive Heart Failure (Definition)
The failure of the heart to efficiently pump, leading to excessive blood or fluids in the lungs, the body, or both.
- Common Pediatric Emergency
- Results from structural or functional cardiac disorders that impair the ability of the ventricles to fillwith and/or eject blood.
- Clinical condition in which the heart fails to meet the metabolic and circulatory demands of the body.
- CHF is most apt to occur in children under 1 year of age.
Congestive Heart Failure (Etiology)
-either left or right ventricles or both may be sources of inadequate pumping
- Various forms of congenital heart disease such as ventricular septal defect (VSD), patent ductus arteriosus (PDA) or common AV canal
- Heart valve disease caused by Rheumatic fever or other infections
Infections of the heart valves and/or heart muscle (endocarditis)
- Cardiac arrhythmias (irregular heartbeats)
- Cardiomyopathy or another primary disease of the heart muscle
- Coronary artery disease
Inflammation of heart muscle (myocarditis)
- Complication of CHD, rheumatic fever, Kawasaki disease, etc.
Congestive Heart Failure (S/S)
- Tachycardia: Early sign
- Tachypnea
- Right heart failure
- Left heart failure:
In infants: Breathless, Tires easily, Difficulty feeding, Diaphoresis, Generalized edema
*left heart failure causes right heart failure
Signs of left sided heart failure
Dyspenea, Orthopenea, Cough, Rales, Tachycardia
(pulmonary flow)
Signs of right sided heart failure
edema, jugular vein distension, peripheral edema, ascites, hepatomegaly
(systemic flow)
Compensatory systems of the heart in cases of dec. cardiac output
RAAS System = fluid retention, vasoconstriction (may cause congestion such as in CHF)
Inc. Heart Rate = to increase cardiac output, may fatigue the heart
Congestive Heart Failure (Management)
Pharmacologic Treatment
Diuretics: Furosemide
Inotropic Agent: Digoxin
Vasodilator: Hydralazine
ACE Inhibitor: Captopril
Calcium Channel Blocker: Nifedipine
- Provide for rest periods.
- Put the patent in a semi-fowler’s position (to alleviate LHF symptoms)
- Sedation with morphine
- Provide oxygen as necessary
- Maintain proper nutrition
- Diet should be planned with low salt for sodium restriction and to be given in small amounts frequently
Congestive Heart Failure (HOPE)
H: Head of Bed (Semi Fowler's)
O: Oxygen
P: Push Morphine
E: End Sodium, LOF
Kawasaki Disease (Other name)
mucocutaneous lymph node syndrome
Kawasaki Disease (Definition)
- an acute systemic vasculitis or the inflammation of the blood vessels of unknown origin
- usually occurs in children less than 5 years of age.
- a febrile, multisystem disorder that occurs almost exclusively in children before the age of puberty.
- It has replaced rheumatic fever as the most likely cause of acquired heart disease in children.
= The peak incidence is in boys under 4 years of age.
After infection, altered immune function occurs and an increase in antibody production which creates circulating immune complexes that bind to the vascular endothelium and cause inflammation.
Kawasaki Disease (Acute Phase)
-Onset of fever greater than 38.9 (102) lasting 5 days to 2 weeks, no response to antiphyretics
-RED eyes without drainage
-Bright RED, chapped lips
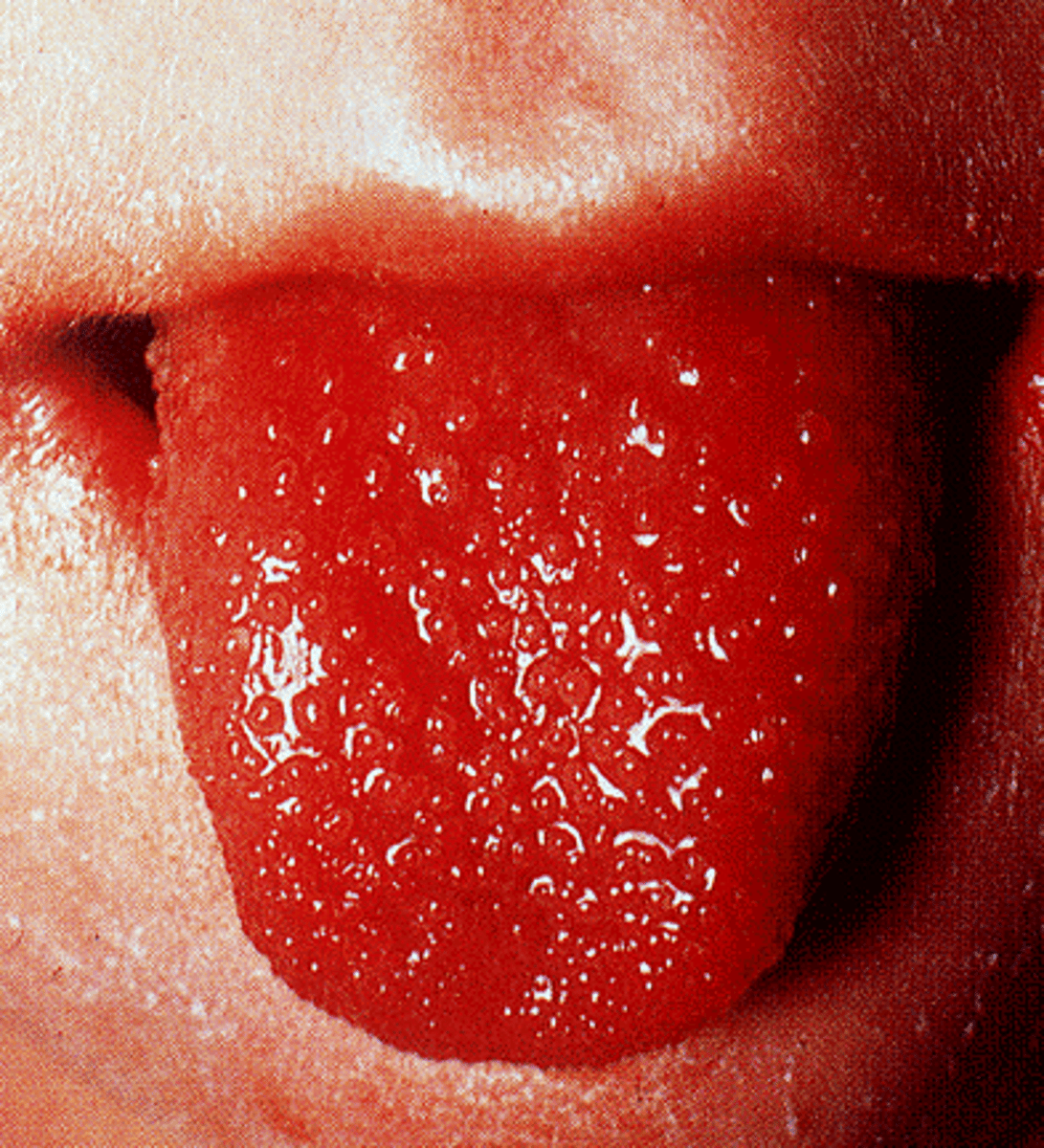
-Strawberry tongue with white coating or RED bumps on the posterior aspect
-RED oral mucous membranes with inflammation
-Swelling of hand and feet with RED palms and soles
- Cervical lymph nodes become enlarged.
- Children may develop abdominal pain, anorexia, and diarrhea.
- Joints may swell and redden, simulating an arthritic process.
Kawasaki Disease (Subacute Phase)
10 days after onset
- Skin: desquamates, particularly on the palms and soles.
- Platelet count rises; this increases the possibility of clotting, which could result in necrosis of distant body cells, particularly the fingertips, if they no longer receive adequate blood.
- Aneurysms may form in coronary arteries, compromising heart activity.
- Sudden death from accumulating thrombi or rupture of an aneurysm may occur (most dangerous phase)
Kawasaki Disease (Convalescent Phase)
complete resolution of symptoms until all signs of inflammation have disappeared after 8 weeks
Kawasaki Disease (Criteria for Diagnosis)
- Fever >5 days + 4/5:
- bilateral nonexudative conjuctival injection
- changes in lips, tongue or oral mucosa (drying, fissuring, red strawberry tongue)
- changes in the peripheral extremities (edema, erythema, desquamation)
- Polymorphous truncal exanthem
- Cervical lymphadenopathy
Kawasaki Disease (Management)
Acetylsalicylic acid (aspirin) or Ibuprofen:
- decreases inflammation and blocks platelet aggregation.
Abciximab:
- platelet receptor inhibitor specific for Kawasaki disease.
IV immune globulin (IVIG):
- to reduce the immune response
- Caution: patients should not receive routine immunizations while taking IVIG or the immunization will be ineffective.
Steroids:
- may increase aneurysm formation; arecontraindicated.
Coronary artery bypass surgery:
- if the child is left withcoronary artery disease from stenosis of the coronary arteries
Rheumatic Heart Disease (Definition)
- It is an inflammatory disease that can develop as a complication of inadequately treated streptococcus infection.
- Common in children 6 to 15 years of age with a peak incidence at 8 years. It is most seen in a poor crowded urban area
- Children appear well again in 1 to 3 weeks. However if the child is not treated, the rheumatic fever’s symptoms can begin.
- It occurs in a late reaction of its response to infection.
- The name takes after “Rheumatism”
Caused by abnormal immune response against M protein = causes inflammation of the heart
Rheumatic Heart Disease (Causative Agent)
group A beta hemolytic streptococcus.
Rheumatic Heart Disease (S/S)
Fever
Sydenham’s Chorea
Chest pain
Erythema marginatum
- A subcutaneous rash that does not itch and forms rings that spread out overtime.
Carditis
Bacterial vegetations on tricuspid valve
Wrist inflammation
Rheumatism
- Inflammation occurs in the joints making it painful to move.
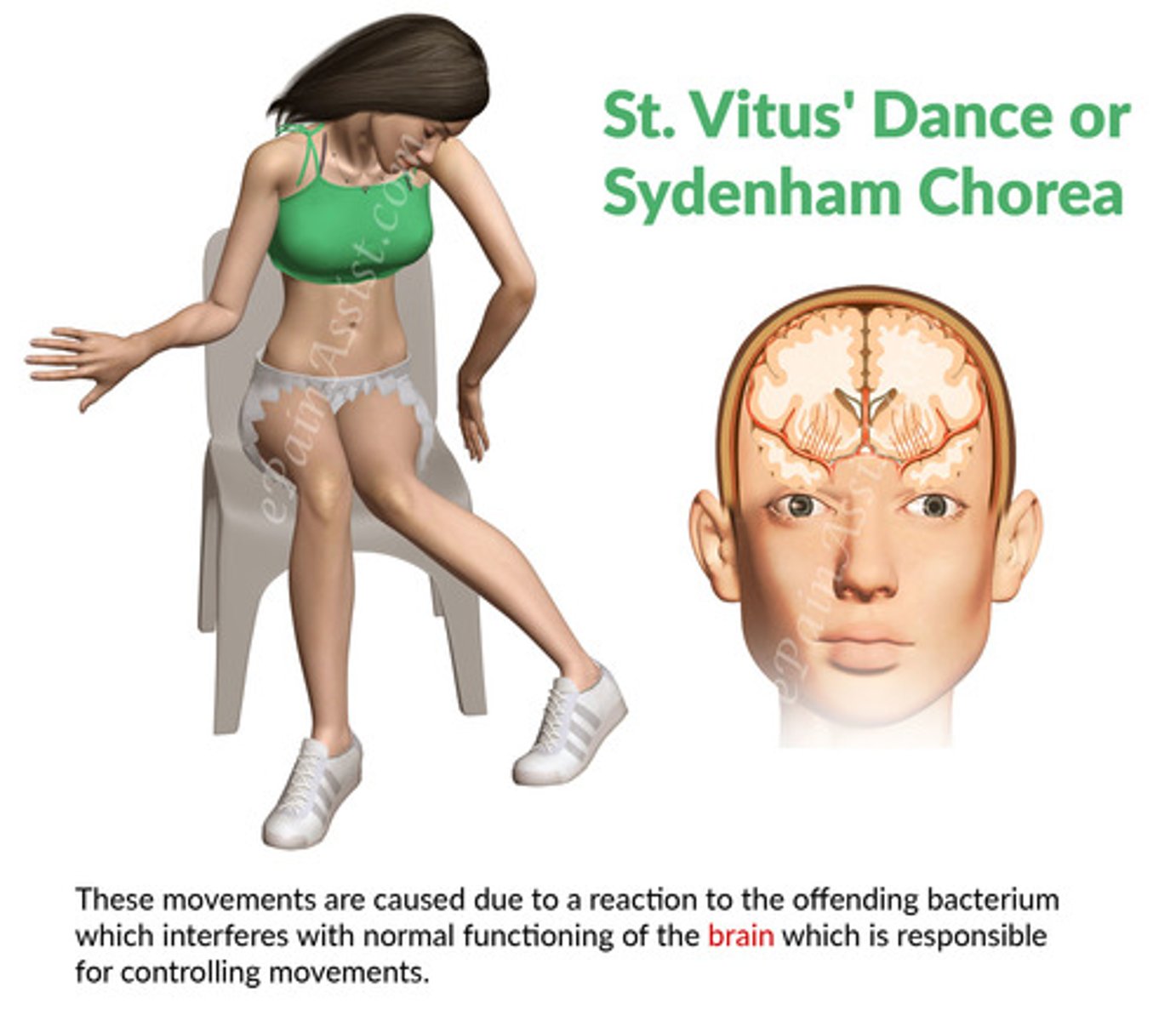
Sydenham Chorea
jerky, uncontrollable and purposeless movements of the hands, arms, shoulder, face, legs, and trunk. These movements look like twitches, and disappear during sleep
This is known as chorea or St. Vitus’ dance.
Rheumatic Heart Disease (JONES)
Joint pain
🫀Carditis
Nodules [Subcutaneous]
Erythema Marginatum
Sydenham’s Chorea
Rheumatic Heart Disease (CAFEPAL)
C-reactive protein ↑ [>3 mg/dL]
Arthralgia
Fever
Erythrocyte sedimentation rate [>60 mm/h]
Prolonged PR interval
Anamnesis Suggestive of Rheumatism
Leukocytosis
Rheumatic Heart Disease (Diagnostic Tests)
ECG: blocks
Chest X-ray: congestion/cardiomegaly
Echocardiogram: effusion/any valvular dysfuntion
Throat Culture: usually negative
Serology
- Anti streptolysin O
- Anti deoxyribonuclease B
Rheumatic Heart Disease (Nursing Management)
Encourage bedrest and decrease oxygen demands
Monitor vital signs during the acute phase.
Rheumatic Heart Disease (Pharmacological Management)
Penicillin therapy: Benzathine penicillin
Oral Ibuprofen: ↓ inflammation and joint pain
Corticosteroid: ↓ inflammation on children who are not responding to ibuprofen therapy
Phenobarbital and Diazepam: ↓ the purpose less movement of the chorea
Digoxin and Diuretics: ↓ heart failure
Pericarditis (Definition)
Is an inflammation of the pericardial membrane with or without accumulation of excess pericardial fluid.
Pericarditis (Causative Agent)
The most common causes of pericarditis in North America and Europe are viral or post viral in origin.
Pericarditis (Complications)
pericardial effusion and cardiac tamponade
Cardiac Tamponade
acute compression of the heart caused by fluid accumulation in the pericardial cavity
Pericarditis (S/S)
Chest pain, which can be sharp, precordial, radiating, and is worse with inspiration or cough.
It is characteristically positional
Fever is also common.
Weakness,
Trouble breathing and coughing.
Palpitations
Pericarditis (Treatment)
Anti-inflammatory Agents (NSAIDS): Ibuprofen
Corticosteroids
Myocarditis (Definition)
inflammation of the myocardium (muscle layer)
- This inflammation can weaken the heart muscle, affect its function, and in severe cases, lead to heart failure, arrhythmias, or sudden cardiac death.
Myocarditis (Causative Agent)
viral agents such as adenovirus, parvovirus, COVID-19, bacterial infections, autoimmune diseases, toxins, or allergic reactions.
Myocarditis (S/S)
Chest pain: This is one of the hallmark symptoms of myocarditis.
Shortness of breath (dyspnea)
Fatigue and weakness
Palpitations
Edema (swelling)
Flu-like symptoms
Arrhythmias
Myocarditis (Treatments)
- Depends on the underlying cause and severity of the condition.
- The use of steroids or immunosuppressants is NOT well established but has been shown to be beneficial with certain types of myocarditis.
- For fulminant myocarditis , the use of mechanical circulatory devices, like - VAD and ECMO may be necessary as a bridge to transplant or recovery.
Bacterial Endocarditis (Definition)
- It is the inflammation and infection of the endocardium or the valves in the heart.
- The incidence of infective endocarditis in children is increasing due to the increased survival of children with chronic heart disease.
Bacterial Endocarditis (Causative Agent)
- typically caused by bacteria, but fungi or other microorganisms can also be responsible.
- The condition usually occurs when bacteria or other germs from another part of the body, such as the mouth, skin, or urinary tract, enter the bloodstream and attach to damaged areas of the heart.
Ex. during dental surgery, impetigo, or UTI
- Staphylococcus aureus or Streptococcus viridans
Bacterial Endocarditis (S/S)
Fever: Persistent or recurrent fever is a hallmark symptom of infective endocarditis.
Chills
Fatigue and weakness
Heart murmurs
Petechiae
Bacterial Endocarditis (Treatment)
Antibiotic therapy until complete eradication achieved
IV therapy
Arrhythmia (Definition)
Abnormal heart rhythm
Sinus arrhythmia is commonly found in children.
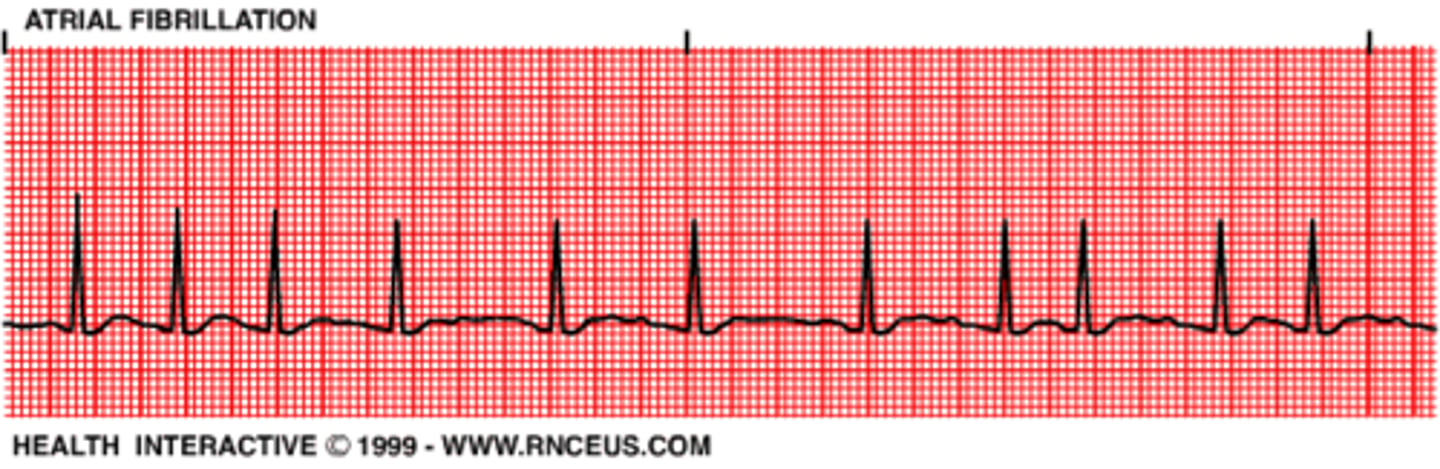
Atrial Fibrillation
occurs when the normal rhythmic contractions of the atria are replaced by rapid irregular twitching of the muscular heart wall
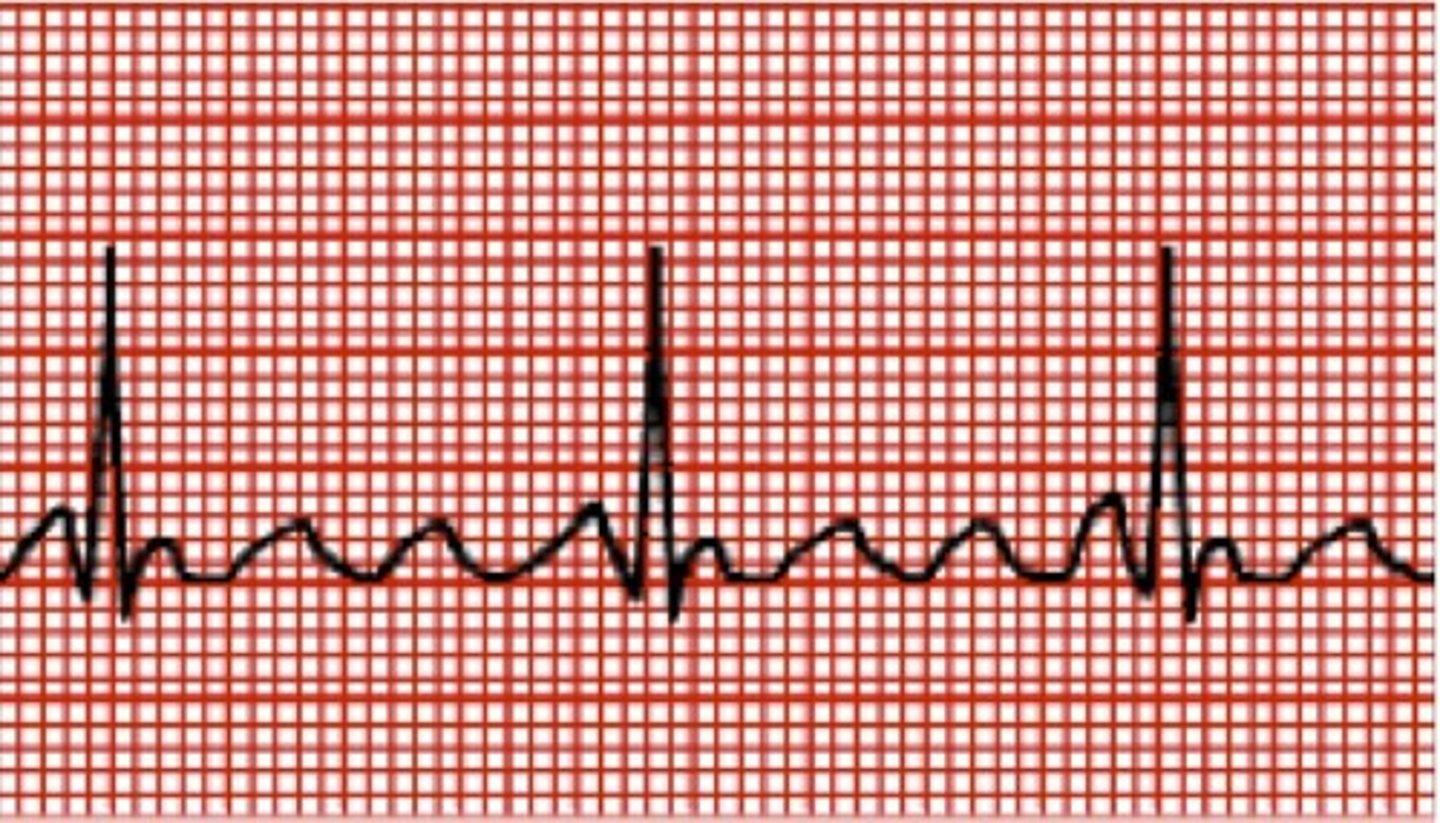
Atrial flutter
irregular beating of the atria; often described as "a-flutter with 2 to 1 block or 3 to 1 block"
ventricular fibrillation
the rapid, irregular, and useless contractions of the ventricles
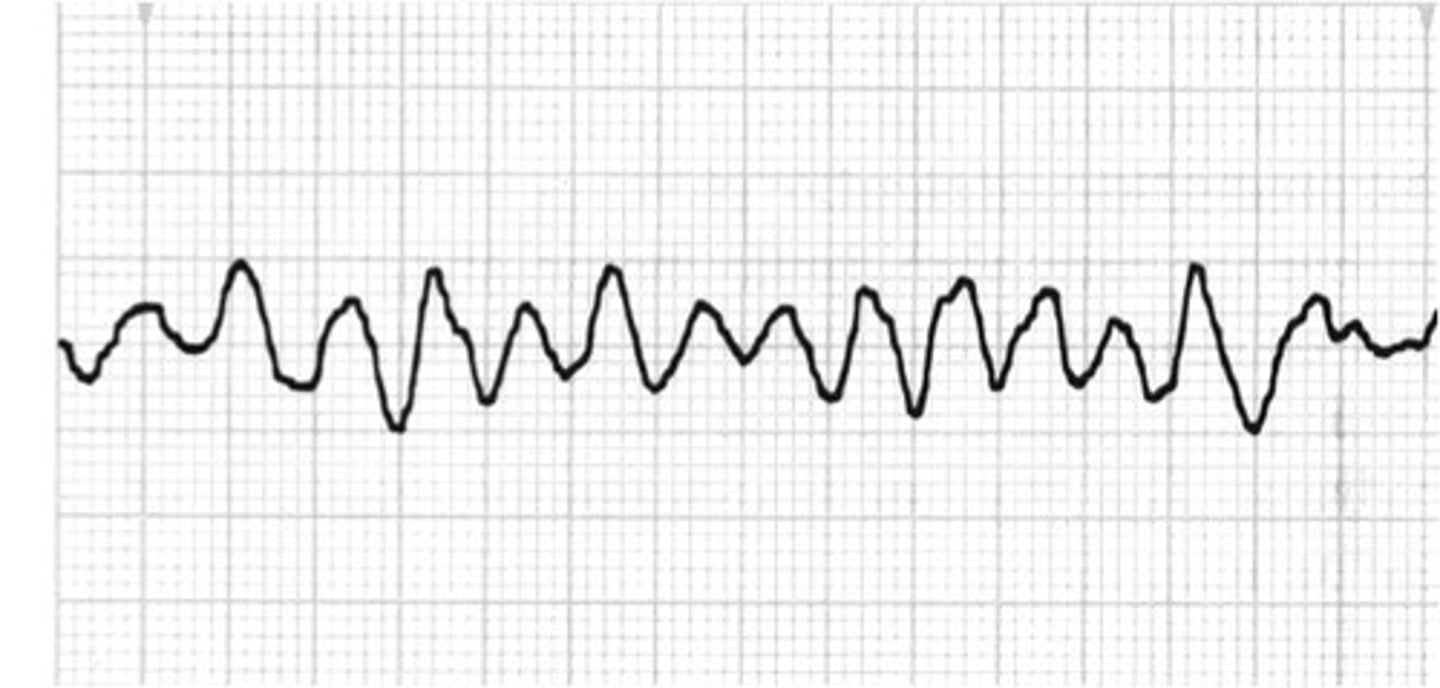
Arrhythmia (Management)
■ Atropine: To counteract the vagal stimulation
■ Digoxin: Decreases and strengthens heart rate
■ Pacemaker: To maintain a steady heart rhythm
Normal digoxin levels
0.5-2 ng/mL
Potassium and Digoxin relationship
Potassium ions compete with Digoxin for binding to receptors
When potassium levels are low, binding of digoxin to receptors increases
Can produce toxicity of Dig
When potassium levels are high, Digoxin affinity to receptors is low
Thus blocks therapeutic response of Digoxin
ACE Inhibitors can increase potassium levels