Micro Bio- Ch. 15
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
72 Terms
Signs
Changes in body measured or observes because of a disease
Symptoms
changes in body function, felt by a patient
Syndrome
specific group of signs and symptoms with a disease
Asymptomatic, subclinical
no signs or symptoms
Infectious disease
caused by direct effect of pathogen
Contagious
easily and rapidly spread from one host to another
Communicable disease
spread from person to person through direct/ indirect mechanisms
Iatrogenic diseases
contracted as the result of medical procedure/ treatment
Nosocomial diseases
acquired in hospital setting
Zoonitic disease
animals to humans
noncommunicable disease
disease that is not transmitted from one host to another
Noninfectious disease
noncommunicable infectious diseases not caused by pathogens
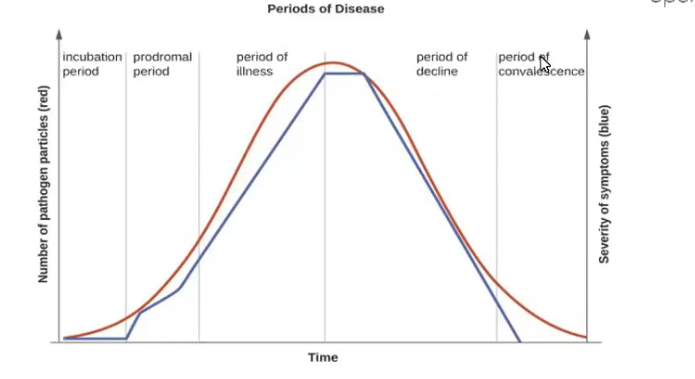
Periods of disease: incubation period
interval between initial infection and first signs and symptoms, pathogens begin multiplying
Periods of disease: Prodromal period
short period after incubation, early, mild symptoms, pathogen continues multiplying, host will react
Periods of disease: Period of illness
disease is most severe
Periods of disease: period of decline
signs and symptoms subside, # of pathogens decrease
secondary diseases possible
Periods of disease: period of convalescence
body returns to prediseased state, no pathogen
Acute disease
symptoms develope rapidly
disease lasts for short time
Ex. influenza
Chronic disease
symptoms develop slowly
pathologic changes occur over loner time spans
Latent disease
casual pathogen goes dormant for periods of time
no active replication, but then activates and produces symptoms
Pathogenicity
ability of a microbial agent to cause disease
Virulence
degree to which an organism is pathogenic
Avirulent
not harmful
Less virulent pathogens
more likely to result in mild signs and symptoms/asymptomatic
Highly virulent pathogens
almost always lead to a disease state, some may cause multi organ and body system failure
dependent on route of transmission
Median infectious dose (ID50)
number of pathogens required to cause active infection in 50% of inoculated populations
Median lethal dose (LD50)
number of pathogens or amount of toxin required to kill 50% of inoculated populations
infective does for individual varies
route of entry
age
health
immune status
Bacillus anthracis
Portal of Entry (ID50)
Skin: 10-50 endospores
Inhalation: 10,000-20,000 endospores
Ingestion: 250,000-1,000,000 endospores
For steps of pathogens
exposure (contact)
adhesion (colonization)
invasion
infection
portals of entry
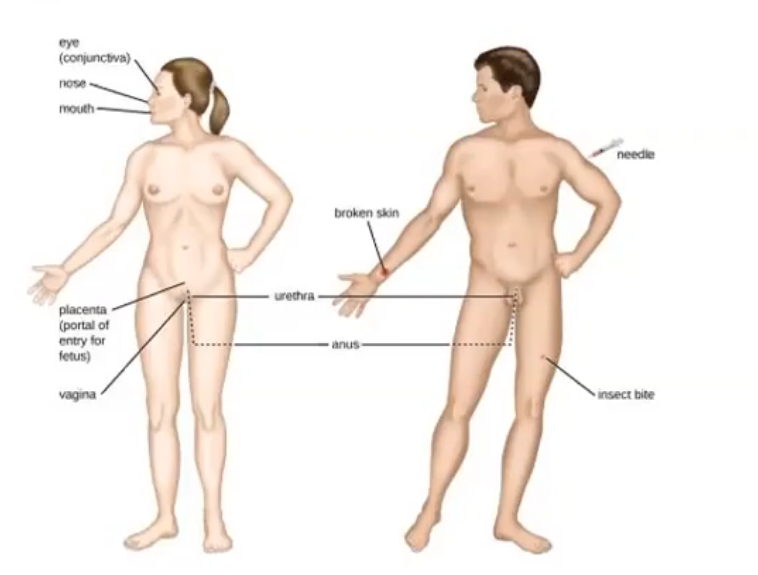
portals of entry: Mucous membranes
lining respiratory tract, gastrointestinal tract, genitourinary tract and conjunctiva -most accessible
portals of entry: skin
impenetrable by most microorganisms
portals of entry: parenteral route
cut on skin
directly into tissues when barriers are penetrated
Streptococci portals of entry
inhaled: pneumonia
ingested: no signs/symptoms
Adhesion
capability to microorganism to attach to host
capsules
slime layers
biofilms
Invasion
dissemination of a pathogen throughout local tissues or the body
different factors: virulence factors
exoenzymes: used to combat
toxins
Coagulase
coagulates (clot) fibrinogen:
fibrin clot may protect bacterium from phagocytosis
Kinases
digest fibrin clots formed by the body to isolate the infection
Hyaluronidase
digests polysaccharides that hold cells together, spreading infection
Collagenase
degrades collagen in connective tissue to promote spreading
IgA proteases
destroys IgA antibodies (critical in mucosal immunity)
Infection: local
limited to small area of the body
Infection: focal
localized pathogen or toxins it produces can spread to a secondary location
Infection: Systemic
infection disseminated throughout the body
Primary infection
acute infection that causes initial illness
Secondary infection
opportunistic infections after a primary infection
Bacteremia
bacteria in blood
toxemia
toxin in the blood
viremia
viruses in blood
Septicemia
bacteria present and multiplying in the blood
Septic
patients with septicemia
Shock
life threatening decrease in blood pressure that prevent cells and organs from receiving enough oxygen and nutrients
some bacteria release toxins which can lead to low blood pressure
Portal of exit: respiratory tract
coughing, sneezing
tuberculosis, pneumonia, smallpox and influenza
Portal of exit: Gastrointestinal tract
feces
salmonellosis, cholera, typhoid fever, shigellosis, amebic dysentary
saliva
rabies
Portal of exit: genitourinary tract
urine and vaginal secretions
STD
portal of exit: skin
ringworm, herpes simplex and warts
portal of exit: blood
arthropods that bite
yellow fever, plague, tularemia and malaria
portal of exit: needles or syringes
aids
Hep B
Toxin
poisonous substances produced by microorganisms that assist in their ability to invade and cause damage to tissue
toxigenicity
ability of a microorganism to produce a toxin to cause damage to host cells
Toxemia
presence of toxin in hosts blood
Intoxications
presence of toxin without microbial growth
Exotoxins and Endotoxins
based on mode of action
neurotoxin
cytotoxin
enterotoxin
Endotoxins
produced by gram negative
apart of outer membrane
Lipid A (lipopolysaccharides)
fever: yes
Neutralized by antitoxin: no
LD 50: relatively large
Test to detect endotoxins
Limulus ameobocyte lystate (LAL)
blood cells (ameobocytes) of horseshoe crab (limulus polyphemus) mixed with patients serum
ameobocytes react with endotoxin
observed through chromoenically (color) or coagulation (clotting)
Enzyme linked immunosorbent assay (ELISA) uses antibodies to detect endotoxin
Exotoxin
mostly gram positive
by product of growing cell
made of protein
no fever
can be neutralized by antitoxin
small LD50
types of exotoxins
intracellular targeting
membrane disrupting toxins
superantigens
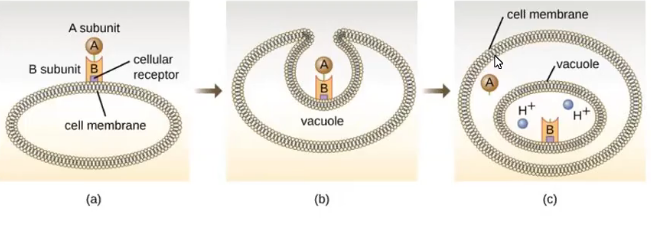
Intracellular targeting toxin
targets host cell
A-B toxin
B subunit binds to cell membrane
A unit connects
enters cell through endocytosis
units separate
A→ cytoplasm
Membrane disrupting toxin
lyses host cells by
making protein channels in plasma membrane
Leukocidins- kills White Blood Cells
Hemolysins- kills Red Blood Cells
Streptolysins- Hemolysin produced by streptococcus
disrupts phospholipid bilayer
Superantigens
causes intense immune response due to release of cytokines from host cells
overstimulation of host immune system: distracts body from pathogen
excessive cytokines in blood causes: fever, nausea, vomiting, diarrhea, shock, death