Lecture 8-appetite
1/63
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
64 Terms
homeostasis
•process by which the body maintains relatively constant internal milieu, within narrow limits
•Hormones are crucial to homeostasis and involve behaviour (e.g., drinking)
•Some are purely physiological, others more behaviour based (eating, drinking)
set point
•= optimal internal state in given environment
•If get away from setpoint there’s an internal system that regulates it (normally hormonally influenced)
•Narrow limits, can’t tolerate much deviation
•Doesn’t apply nicely to hunger and food intake
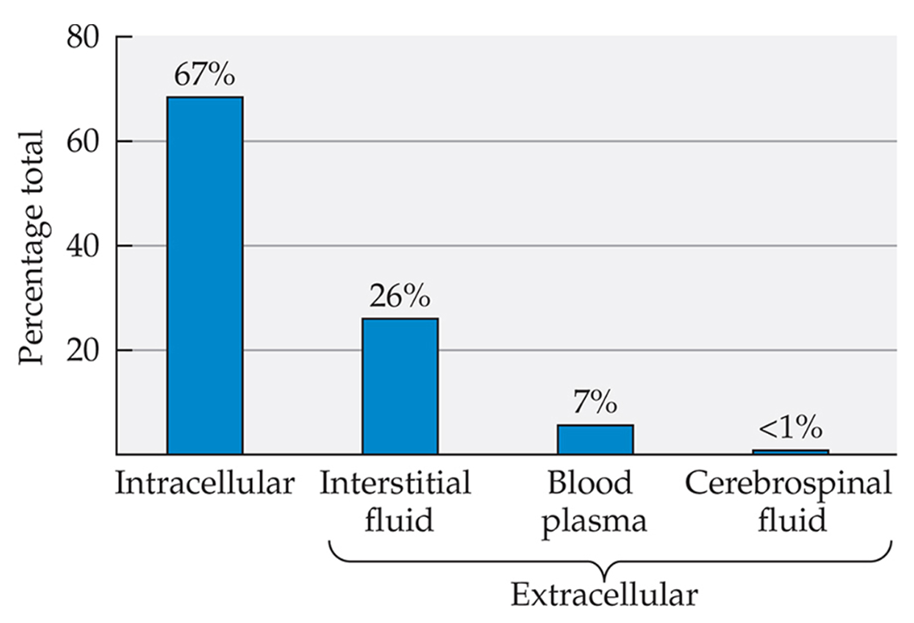
fluid balance
•Where water is stored in the body
•Dependent on the right concentration of salts to fluid, each of these have their own concentration
how do we keep salt and water concentrations stable?
•Barriers between compartments, is how we keep these concentrations stable
•Cell membranes
•Walls of blood vessels
osmosis
•Key homeostatic process in fluid balance
•Movement of water across a semipermeable membrane into more concentrated solution
Water can move across these membranes easily, it’s the salt that can’t easily move
thirst
motivation to seek and ingest water
1) hypovalemic
2) osmotic
hypovolemic thirst
•increased salt in extracellular fluid causes water loss from cells
•Volume, excess fluid loss, exercise, lost a lot of blood, losing both water and salt so replenish both
•Can stim both thirst and hunger
osmotic thirst
•increased salt in extracellular fluid causes water loss from cells
•Really salty foods and are thirsty, cells shrink and become dehydrated
key hormones for thirst
AVP and Aldosterone
AVP and thirst
•aka antidiuretic hormone (retains water)
•Filtration process in the kidney differs so less water
•Can go wrong in diabetes insipidus, lack vasopressin so constantly drink water and urinate, so are losing too much water
Aldosterone and thirst
•retains sodium in the kidney)
•Increases water loss, dehydration
key thirst mobilizers
osmoreceptors and baroreceptors
osmoreceptors
•in the organum vasculosum of the lamina terminalis (OVLT)
•specialized cells that signal to the brain when they shrink that we’re are thirsty and need more water, signal to the area where the ADH (hypothalamus) to retain water
baroreceptors
in blood vessels
•signal to our brain when blood volume is lost, stim ADH release from the hypothalamus
•Increasing our blood pressure in response to blood loss
energy balance
Not as tightly regulated as fluid balance
When more energy is consumed than needed, stored as fat, this can be beneficial for extreme environments of little access to food
Not same set point as homeostasis
We can tolerate a long range away from set point and be relatively “okay”
factors impacting feeding behaviours
•Redundant biological mechanisms
•Social factors- anticipation of food can impact food intake
•Learning
what is energy balance closely tied to?
reproductive function, if have enough energy stored signals we are able to reproduce
Leptin, signals satiety, has also been linked to increased sexual behaviours, tells your body you have a lot of energy so can stop worrying about survival and start reproducing, this is the opposite if you are extremely underweight because need to focus on survival
• some hormones that impact hunger also impact sex behaviour
what are the key processes for metabolism
1) catabolism
2) anabolism- the use of energy to build the body
how does metabolism shift?
based on when have recently ate or fasted
Set to program to defend for our “set point”, doesn’t like to get away from where we are
well fed metabolism
•2 post-feeding phases: postprandial phase and postabsorptive phase
•Insulin promotes uptake of energy into cells and the storage of excess energy
2 phases of insulin release: cephalic phase and gastrointestinal phase
postprandial
immediate phase after eating, when you have sugars, fatty acids, amino acids entering the bloodstream
postabsorptive phase
when body is trying to store excess energy
cephalic phase
first, anticipation of eating, before you even eat you get an increase in insulin, anticipation the energy will come, some people report getting hungrier when food is presented in front of them
gastrointestinal phase
storage of excess nutrients, energy into the cells
where is energy always prioritized for
the brain, will starve the rest of the body to feed the brain
-This is the only form of energy the brain can use
-
fasting metabolism
•Glucagon promotes breakdown of stored glucose in liver
•Use the stored energy from the 2nd phases
hunger
a strong motivation to seek out and ingest food
peripheral hormones and hunger
made outside the brain but impact brain and hunger
grehlin-peptide
leptin-peptide
insulin-peptide
glucagon-peptide
grehlin-peptide
•produced from stomach
•Peaks at onset of meal
•Increases hunger in experimental studies
leptin-peptide
•produced by adipose or fat cells, lvls of leptin proportional the fat stores in the body
•Levels proportional to total fat stores in body
•Satiety signal; reduces motivation to eat, lets brain know you have enough energy
insulin-peptide
•released from pancreas
•May signal satiety through both direct and indirect (i.e., metabolic) mechanisms
•Decrease blood sugar, metabolism effects
glucagon peptide
•released from the pancreas
•May signal end of meal/limit meal size
•Actually breaking down energy, activity is letting you know energy is coming
protein hormones that reduce food intake
Cholecystokinin (CCK)
•Corticotropin-releasing hormone (CRH)- HP axis, stress
•Glucagon-Like Peptide 1 (GLP-1)
•Peptide Tyrosine-Tyrosine (PYY)
•Cholecystokinin (CCK)
•Released from brainstem and hypothalamus during feeding to aid in digestion
•Decreases food intake in hungry animals by acting on vagus nerve
•Corticotropin-releasing hormone (CRH)- HP axis, stress
•Normally reduces food intake and body mass
•Stressors may motivate eating in some people, and CRH dysregulation may be important in this context
•Abnormal repsonse
•Glucagon-Like Peptide 1 (GLP-1)
•Released from gut following high fat/carb meals-limits overeating
•Inhibits further food intake via vagus nerve and hindbrain
•Peptide Tyrosine-Tyrosine (PYY)
•Produced from colon in response to food ingestion
•More food ingesting more of this hormone
•Decreases food intake
•Injecting can reduce food intake by 30%
central anabolic effectors
•Made in the brain and act within the brain
•In this context neurotransmitters
•Neuropeptide that increase food intake or building energy
central anabolic effectors types
neuropeptide y
agouti-related protein, AgRP
Melanin-concentrating hormone
orexin
Neuropeptide Y
•Increases food motivation (e.g., food seeking)- to get food
Decreases amount of food consumed passively (e.g., food already on the plate)
Agouti-related Protein, AgRP
potent stimulator of food intake
Melanin-concentrating homrone
signals food intake and reduction of metabolic intake
orexin
induced feeding behaviour and metabolism
central catabolic effectors
decrease food intake
pancreatic polypeptide (PP)
melanocortins
cocaine and amphetamine regulated transcript (CART)
pancreatic polypeptide (PP)
•Increases in response to food intake
Infusions of PP reduces calories consumed in humans-nearly a day, so more long term effects
Melanocortins
•including α-MSH, β-MSH, and adrenocorticotropic hormone
•Inhibit food intake
•Mutations in these receptors have been found to be linked to obesity in humans
Cocaine- and Amphetamine-regulated Transcript (CART)
•Works in concert with leptin, and insulin to decrease food intake
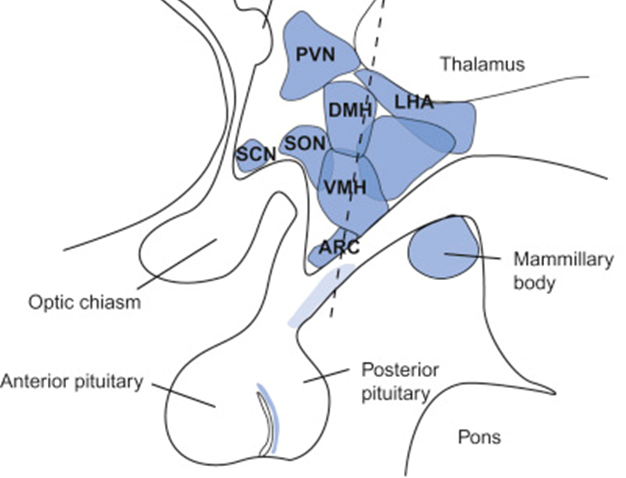
role of hypothalamus and hunger
•Key areas of the hypothalamus include the arcuate nucleus (ARC), lateral hypothalamus area (LHA), and paraventricular nucleus (PVN)
•Peripheral hormones act on the brain the increase food intake and hunger
•Neuropeptied also do this and all happens in then hypothalamus
paraventricular nucleus
•Satiety centre
•Activation reduces feeding
•Primary integrator of info, hormonal, nutrition, etc
•When you suppress you get more food intake
arcuate nucleus
2 circuits- stimulatory circuit (more food) and inhibitory
Main stuff is happening here
Both of these circuits feed info to the PVN and other nuclei in the hypothalamus
Insulin, leptin, ghrelin receptors
- So peripheral hormones can act here to change food intake
stimulatory circuit of arcuate nucleus
•Cells produce NPY and AgRP
•Activated by ghrelin
•NPY and AgRP inhibit neurons in the PVN
inhibitory circuit of arcuate nucleus
•Cells produce CART and α-MSH
•Activated by leptin
•CART and α-MSH activate neurons in PVN and LHA
lateral hypothalamus
•Produces Melanin-Concentrating Hormone and Orexin
•Food palatability
•Receives input related to gustatory information (taste and smell of food)
•Neurons in nucleus accumbens that express dopamine receptors project to this area
•Inhibited during food consumption
pica
•Persistent eating of non-food substances (e.g., soap, paper, chalk)
•May be related to vitamin or mineral deficiencies-homeostatic mechanism gone wrong, this is a minority of cases
anorexia nervosa
•Restricted eating, significantly low weight, body image concerns, fear of gaining weight
•Elevated ghrelin and low leptin, but may be resistant to ghrelin effects
•Elevated CCK and PYY when gaining weight
binge eating disorder
•Binges = eating a very large amount of food; lack of control; emotional distress
•Ghrelin not uniformly higher, but may be higher in pre-absorptive phase
•Blunted GLP-1 after a mealm
most research for eating disorders is?
correlational
type 1 diabetes
•immune system destroys the cells of the pancreas that produces insulin, so can’t develop
type 2 diabetes
•more so insensitivity to inuslin, it’s there but you aren’t responding
•This makes it so you can’t get energy into cells, so increased food intake
prader-wilii syndrome
very high insatiable hunger, hyperphagia, never get full always want to eat, condition that impacts the hypothalamus, high ghrelin,
obesity
•BMI of 30 or greater
bio mechanisms that contribute to obesity
•Obesity genes”
•Leptin resistance
•Changes in “set point” and metabolic rate
•Dysregulated HPA-axis
•Psychosocial mechanisms of overeating also make lifestyle changes difficult
guilt and shame
emotional eating
biggest loser video take aways
Some research has shown activation in the reward system, not the same as we see in addictive substances such as drugs and alcohol
Metabolism slows down when you lose a lot of weight quickly or gain a lot quickly