Population Health Midterm
1/156
Earn XP
Description and Tags
spring 2026
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
157 Terms
What is the definition of population?
Groups of ppl who may/may not interact w each other but have common health concerns & needs
ppl experiencing eviction
ppl w the same occupation (nurses, migrant farmers, waiters)
ppl of same age
ppl living in the same county
ppl w disabilities
ppl of the same race/ethnicity
ppl w the same medical diagnosis (HIV, cancer, DM)
LGBTQ community
population examples
Aims of Healthy People 2030
Attain healthy, thriving lives and well-being free of preventable disease, disability, injury, and premature death.
Eliminate health disparities, achieve health equity, and attain health literacy to improve the health and well-being of all.
Create social, physical, and economic environments that promote attaining the full potential for health and well-being for all - “Vital Conditions”
What are the core functions of public health?
1.) Assessment
2.) Policy Development
3.) Assurance
Assessment
Monitoring health status, diagnosing and investigating health problems, & identifying community needs
Policy Development
Informing, educating, empowering ppl, mobilizing community partnerships, and developing policies & plans to support health
Assurance
Enforcing laws, linking ppl to services, ensuring a competent workforce, & evaluating services
What is health outcome?
Anything that might indicate health or well-being of a population
(could include measures of illness, aspects of health, quality of life, etc.)
CVD
HIV
Depression
Measles
Infant mortality
Childhood lead poisoning
Asthma
health outcome examples
Why are health outcomes important?
To know how to prevent, tx, or cure
Many populations are experiencing high burdens of diseases that are PREVENTABLE.
These are DISPARITIES!!
What is population health?
Focuses on the health needs of a specific group of ppl
Identifies and addresses societal factors that may hinder or enhance their access to health care
How do you assess a group of ppl for health needs?
affected by factors influencing individuals, families, neighborhoods, communities, & society at large
What does a pop-health nurse do?
Determine the need for advocacy & factors that prevent clients from acting on their own behalf
Determine the point at which advocacy will be most effective
Collect facts r/t the problem
Present case to appropriate decision makers
Empower clients to speak for themselves
Microaggression
Unintentional, daily, quick statements or actions of a discriminatory nature based on dominant culture ideology
Racial microaggression are daily commonplace insults & racial slights that cumulatively affect the psychological well-being of ppl of color
Can be directed at any marginalized group & be multi-layered
“You’re so smart, why didn’t you become a doctor?” (nursing student)
“Your hair looks so interesting. How do you keep it clean?” (black person)
“That’s so gay” (LGBTQ community)
microaggression example
Prejudice
Beliefs about groups of ppl based on specific characteristics or identities that make one group better than another
The groups have hierarchical differences that are measured or judged
“I assumed the older adult wouldn’t understand how to use a computer before I even assessed their baseline knowledge”
“I dismissed the patient’s pain because of their hx of substance use influenced my judgement”
“The staff assumed the pregnant teen was irresponsible w/o learning anything about her situation”
prejudice examples
Structural Racism
Focuses on institutions like education, housing, healthcare, and criminal justice.
Refers to how these institutions are built and maintained in ways that disadvantage certain racial groups.
Rooted in historical injustices that created long-term disparities.
Ex: segregated buses/schools for blacks vs whites
Slavery
Segregation
Jim Crow
redlining
Apartheid
Holocaust
structural racism examples
Systemic Racism
Encompasses the entire system of society, including cultural norms, beliefs, and behaviors.
It's broader than structural racism—it includes both institutional practices and societal attitudes that perpetuate inequality.
Think of it as the network of racism that runs through everything: laws, media, traditions, and even unconscious/implicit bias.
Discrimination
Actions taken (implicitly or explicitly) based on prejudiced beliefs that result in treating groups of ppl differently or creating systems that advantage certain groups over others
Individual (micro)
Institutional (macro)
“I provided less detailed explanations to the immigrant family because I know they wouldn’t understand anyway.”
“The nurse denied the learning disabled patient additional time to process instructions.”
“I offered fewer treatment options to the patient with Medicaid because I’m pretty sure they can’t afford the expensive ones.”
discrimination examples
Intersectionality
The ways that class, race, gender, ethnicity, sexual orientation, ability, status and other markers of difference intersect to inform individual realities and lived experiences
Brings attention to the ways that power operates in society to create marginalization of multiple groups, while maintaining power of other groups
“I assumed the Black woman was being ‘difficult’ when she questioned her treatment plan, instead of recognizing how her race and gender shaped her past experiences with healthcare.”
“I dismissed the concerns of the young Latino man because I unconsciously associated his race and gender with aggression.”
“The staff prioritized wealthier patients for specialized services while delaying care for those with disabilities and limited income.”
intersectionality examples
Strategies for addressing discrimination & reducing implicit bias in nursing
Counter-stereotypic imaging
Emotional regulation
Individualization
Mindfulness
Perspective-taking
Partnership building
Counter-stereotypic Imaging
Replace an image of a stereotypical group member with the image of someone who is in that group but does not fit that stereotype
Emotional Regulation
Recognize negative reactions (fear, anxiety, frustration) to patients from vulnerable groups and intentionally strive to be empathetic, patient and compassionate
Individuation
Mindfully seek to see the patient as an individual instead of as a member of the stigmatized group. Address any assumptions that are coming up about the group so they are not impacting care of the individual
Mindfulness
Calm our thoughts, take a deep breath, pause before speaking
Perspective-taking
Purposely and empathetically think about what the patient is thinking and feeling, stimulating feelings of caring and compassion. Put yourself in their shoes
Partnership Building
Intentionally frame the clinical encounter as one where the nurse and patient are equals, working collaboratively toward a shared goal
What is Epidemiology?
The study of causes, distribution, and control of diseases in a population
the distribution and determinants of disease or other health-related outcomes in human populations, and the application of that study to controlling health problems
Looking at cause and effect.
How does a disease/illness spread? Who gets sick? Why do they get sick?
SARS COV2 virus causing the disease we now call “COVID-19”
epidemiology example
Causality
1 event = result of another event
Links between contributing factors & resulting states of H&I
E.coli in the lettuce at work —> everyone eats the salad —> everyone ends up w GI s/s —> everyone ends up in the ED
causality example
Risk
Probability that a given individual will develop a specific condition
Risk may be absolute or relative
Absolute Risk
Probability that anyone in a given population will develop a particular condition
“Absolute risk of developing lung cancer in smokers is 3.5%.”
absolute risk example
Relative Risk
Probability that someone in a group of people with a particular characteristic will develop the condition when compared to people without that characteristic
“Smokers are 6-7 times more likely to develop lung cancer than nonsmokers.”
relative risk example
Rates of Occurrence
Statistical measures that indicate the extent of a health problem within a group
Allows comparison between groups of different sizes or divide the instances of an event by the population at risk
Multiply these proportions by 1,000 or 100,000 to make them easier to understand
Commonly used as morbidity & mortality rates
Morbidity
Another term for illness. A person can have several co-morbidities simultaneously. Morbidities are NOT deaths.
Measure of disease RISK (proportion of population who will get the disease)
Number of new cases of a particular condition in a specified time period
aka “disease-burden”
Mortality
Actual deaths that occur
Cause-specific death rate
Case Fatality
The number of people who develop a health problem and will die as a result of it
Shows how deadly a disease is
Ebola case fatality rate is very high
HIV/AIDS case fatality rate used to be very high and could’ve theoretically be zero if people had access to treatment
case fatality examples
What is surveillance in public health?
It’s DATA!!! Systemic collection, analysis, & interpretation of data in order to protect the public’s health AND the timely dissemination of the data to those who need to know (to protect public health)
Prevalence
Total number of people affected by a particular condition at a specific point in time
Impacted by incidence (how many ppl got the disease), duration (do ppl get cured or live w it forever), & deaths (how many ppl actually die of the disease)
tells you how many resources you’ll need to take care of ppl
tells you how well tx are working
need to determine causes of changes in prevalence (cures? deaths? lower incidence?)
Prevalence Rate
A statistical measure that tells you the proportion of a population that is affected by a particular condition at a specific point in time
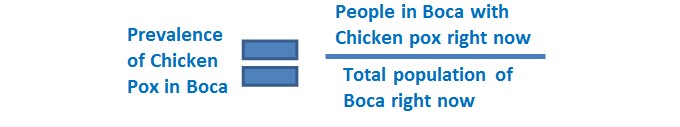
prevalence rate example
Incidence
Alerts you to change of how quickly something is spreading and how well you are doing at preventing a disease
Incidence Rate
The measure of how often new cases of a disease or condition occur in a specific population over a defined period.
Texas reported 803 new cases of measles in 2025
Divide by total population 31 million then multiply by 100,000 = 2.59
Wisconsin reported 23 new cases of measles in 2025
Divide by total population 5.9 million then multiply by 100,000 = 0.39
Let’s pretend Wisconsin had the same number of new cases as Texas did…
Incidence rate would be MUCH HIGHER because the population is MUCH LOWER – 13.61

incidence rate example
How do nurses use surveillance data?
Responsible for collecting and reporting on nationally notifiable diseases to public health officials (filling out a form, making a phone call, or completing information into an online database)
Monitor diseases in certain settings (hospital, community, population)
To track the point of origin of some diseases, manage an outbreak, or investigate disease patterns
To design and conduct population-level interventions (policy, environmental interventions) & to evaluate the effectiveness
Types of Immunity
Herd immunity
Natural immunity
Acquired immunity (active or passive)
Herd Immunity
Protection d/t the immunity of most community members, making exposure unlikely (previous infection / vaccination)
It is the level of disease resistance of a community or population
Natural Immunity (aka Innate)
ALWAYS PRESENT! READY TO FIGHT! RESPOND IMMEDIATELY!
First 2 hrs: Phagocytes (neutrophils & macrophages) release = Engulf bacteria phagocytosis
Inflammation 4 hrs: Mast cells release histamine, immune cells & fluid leak out of blood vessels into tissues —> Macrophages release cytokines (either attract more immune cells or active immune cells) = Fever & Swell
Antiviral Defense 6hrs: Natural killer cells (apoptosis)
Activate adaptive immunity
Adaptive Immunity
NOT ALWAYS PRESENT! TAKES 7-10 DAYS TO BE ACTIVATED! “SHARPSHOOTERS”
When pathogens bypass our innate immune system, the adaptive immune system will step in and fight those pathogens.
“Sharp shooters”: “more specialized,” making cells unique to specific pathogens in order to attack them. (Covid-19)
Remembers previously encountered pathogens to destroy them
Produces B-cells & T-cells
Naturally Active Immunity
natural exposure (ex: kids getting sick in school from contact) & then makes their own antibodies to never have the disease again (ex: chicken pox)
Artificial Active Immunity
Induced by vaccines
ex: after exposure to tetanus, botulinum, HBV, or rabies
Naturally Passive Immunity
Maternally passed down —> transfer of IgA antibodies found in breast milk
ex: mom to baby by feeding breast milk
Artificially Passive Immunity
Healthcare CREATED immunizations to prevent illness
ex: recovering serum/plasma from COVID-19 pts
Chain of Infection (ARPMPS)
agent —> reservoir —> portal of exit —> mode of transmission —> portal of entry —> susceptible host
Causative Agent (infectious)
A biological organism capable of being directly or indirectly transmitted from person to person, animal to animal, animal to person, or the environment (air, water, food etc) to person
bacteria
fungus
virus
parasite
How do we break causative agent part of the chain of infection?
Diagnosis and TX
Antimicrobial stewardship- is the systematic effort to educate and persuade prescribers of antimicrobials to follow evidence-based prescribing, in order to stem antimicrobial overuse, and thus antimicrobial resistance.
Resevoir
Hosts or environments where causative agent lives and reproduces
Dirty surfaces/equipment
Soil
Food
Water
People
Animals/Insects
How do we break reservoir part of the chain of infection?
Cleaning, disinfection and sterilization
Infection prevention policies
Pest control
Portal of Exit
Route that the agent takes to leave the reservoir
For humans, can include blood, respiratory secretions and anything exiting from the GI or GU tracts
How do we break portal of exit part of the chain of infection?
Hand Hygiene
PPE
Control of aerosols and splatter
Respiratory etiquette
Waste disposal
Mode of Transmission
How the causative agent makes it’s move
What are the modes of transmission?
Direct contact
Indirect contact
Droplet
Airborne
Vector-borne (mosquitoes (malaria, west nile, zika), ticks (lyme disease), fleas (plague))
Vehicle-borne (food, water, med, blood products (ex: salmonella from contaminated food))
How do we break mode of transmission part of the chain of infection?
Hand hygiene
PPE
Personal hygiene
First Aid
Removal of catheters and tubes
Susceptible Host
A person who is potentially vulnerable to that particular causative agent
Host factors that influence the outcome of an exposure include:
the presence or absence of natural barriers
the functional state of the immune system
the presence or absence of an invasive device.
How do we break susceptible host part of the chain of infection?
Immunizations
TX of underlying disease
Health Insurance
Patient Education
What is a communicable disease?
A disease that can spread from one person or animal to another in several ways: directly, through physical contact with bodily fluids or secretions; indirectly, through contaminated items like drinking glasses, toys, or water; or via vectors such as flies, mosquitoes, ticks, and other insects.
Stages of Infection (IPIC)
1.) Incubation Period
2.) Prodromal Stage
3.) Illness Stage
4.) Convalescent Stage
Incubation Period
Pathogen begins replication but does not yet cause symptoms
Prodromal Stage
Symptoms begin to appear but can be non-specific
Illness Stage
Pathogen reproduces and disseminates rapidly causing s/s
Convalescent Stage
Affected tissues are repaired & manifestations resolve
Level of Spread (communicable diseases)
Endemic
Epidemic
Pandemic
Endemic
Moderate ongoing occurrence in a given location
Chicken pox that occurred at a predictable rate among school age children before we had the varicella vaccine.
Malaria, which is endemic to Africa, Asia, Latin America, and the Middle East.
COVID-19 now that it is past the acute phase.
endemic examples
Epidemic
Infectious disease that spreads rapidly, or the rate of disease is exceeding the usual endemic level
Measles– currently spreading in the US beyond recent endemic levels.
epidemic example
Pandemic
Spreads beyond continents, across the entire globe, & takes more lives & affects more ppl than an epidemic
COVID-19
HIV/AIDS
pandemic examples
Prevention & Control (communicable diseases)
Immunity
Vaccines
Surveillance
What are the steps for a community health assessment?
1.) Define the community
2.) Collect data
3.) Analyze data
4.) Establish community diagnoses
5.) Plan programs
6.) Implement programs
7.) Evaluate program interventions
Define the Community
What group will you be focusing on?
Can be broad or specific
Use data to help describe the population
Collect Data
Primary (you collect)
Secondary (others have collected)
Quantitative (measured & written w numbers)
Qualitative (info that describes something in character)
Analyze Data
Gather data
Assess completeness of data
Identify missing data
Synthesize data & identify themes
Identify community needs & problems
Identify community strengths & resources
Establish community diagnoses
Identify and prioritize needs of the community
Work with community members, local health professionals, administrators to develop priorities and establish outcomes
Consider:
Community awareness of the problem
Community readiness to acknowledge and address the problem
Available expertise/fiscal resources
Severity of problem - # of people, morbidity/mortality impacts
Amount of time needed for problem resolution
Plan programs
What are possible solutions to the diagnosed problem?
What resources are required for each possible solution?
Establish goals and objectives for the chosen solution
Include measurable objectives with a target date for achievement
Select strategies to achieve the objectives
Identify who is responsible to complete the strategy
Find funding
Plan for evaluation
Evaluate program interventions
Strengths and weaknesses
Did you achieve desired outcomes
Recommend any modifications to better meet community needs
Share findings with the community members and stakeholders
Ongoing evaluation is necessary
Sustainability plan
Helpful strategies for program interventions
Through assessment
Accurate interpretation of data
Collab w community partners
Effective outreach & communication patterns
Sufficient resources
Logical planning
Skilled leadership
Barriers for program interventions
Inadequate assessment
Inadequate/misconstrued data
No involvement w community partners
Impaired communication
Inadequate resources
Lack of planning
Poor leadership
Primary Data
Data that you collect yourself & are hearing directly from the interviewee
Secondary Data
Data that others have collected that you are not collecting yourself
you are gathering the data & reporting what OTHERS found
Quantitative Data
Info that can be measured & written w numbers (ex: temp, BP, pain score)
Qualitative Data
Info that describes something in character