Acute Abdomen in Ruminants
1/69
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
70 Terms
1. Hemorrhagic bowel syndrome (HBS)
2. Duodenal outflow obstruction
3. Trichobezoar, phytobezoar, enterolith
4. Fat necrosis
What are examples of obstructive non-strangulating lesions of the small intestine in ruminants?
1. Intussusception
2. Segmental small intestinal volvulus
3. Torsion of mesenteric root
What are examples of strangulating lesions of the small intestine of ruminants?
Caudal right abdomen
Small intestinal fluid distention will ping where?
1. Root of mesentery
2. Jejunoileal flange
Torsion of small intestine commonly occurs where?
Mature dairy cattle
Hemorrhagic bowel syndrome is a disease of what?
A
T or F: HBS has a high case fatality rate
Hemorrhagic bowel syndrome (HBS)
Massive hemorrhage within lumen of jejunum, in dairy cattle
1. Clostridium perfringens type A
2. Hindgut acidosis, nutritional problem
What are speculated causes for HBS?
First 3 to 4 months
HBS occurs in lactating dairy cattle typically in the ________________ of lactation
1. Peracute death
2. Severe hemorrhage - down, hemorrhagic shock
3. Intraluminal obstruction - colic, weakness, abdominal distention
4. Melena (scant, tarry feces with casts/clots of blood)
5. Positive succussion right abdomen
6. +/- SI distention on rectal
What are clinical signs of HBS? (6)
1. Tachycardia
2. Tachypnea
3. Pale MM
4. Cool extremities
5. Down
What are the components of hemorrhagic shock? (5)
1. Dilated loops of SI
2. Clotted blood within lumen
3. Free abdominal fluid (effusion) and fibrin
What may you see on ultrasound to suggest HBS?
1. Intussusception
2. Small intestinal volvulus
3. Severe functional ileus
What are differentials for HBS?
Exploratory
How do you reach diagnosis of HBS?
1. Resection and anastomosis
2. Enterotomy
3. Manual massage
What are your options when surgically treating HBS with a standing right flank laparotomy?
1. Ration management
2. Transition health
3. C. perfringens Type A vaccine in problem herds
4. Feed supplements (mycotoxin binding agents)
How do you prevent HBS?
1. Foreign body
2. Ulceration and stricture
3. Iatrogenic (recent pyloropexy)
4. Extraluminal compression
What can cause a duodenal obstruction?
Sporadic and rare
Duodenal obstruction is a _____________________ condition
Surgical correction (FB - enterotomy & stricture - side to side anastomosis)
How do you treat duodenal obstructions?
1. Ectoparasites and shedding of hair coat
2. Low roughage diet
Why do trichobezoars occur?
1. Poor appetite, weight gain, vagal indigestion
2. Colic and abdominal distention, lack of manure
What are clinical signs of trichobezoars?
1. Rumenotomy
2. Abomasotomy
3. Enterotomy
How do you surgically remove trichobezoars?
Fescue toxicosis
________________ increases herd prevalence of fat necrosis
Fat necrosis
Necrosis of mesenteric, abdominal and retroperitoneal fat leading to intra- and extraluminal compression
Neoplasia and abscesses
What are DDx for fat necrosis?
1. Jejunum into jejunum or ileum
2. Ileum into cecum/colon
3. Cecum/colon
4. Colon into colon
What are the 4 types of intussusception?
Jejunum into jejunum or ileum
Which type of intussusception is most common?
Small intestine
Intussusception is most commonly involving the _____________ in cattle
1. Colic
2. Peritonitis, septic shock
3. Abdominal distention
4. Fecal production often zero beyond 24 hours
5. Passage of blood/mucus
What are clinical signs of intussusception? (5)
1. Abdominal ultrasound
2. Abdominocentesis
How do you diagnose intussusception?
Right
You should perform a (left or right) paralumbar fossa laparotomy for intussusception?
A
T or F: Manual reduction ("pulling it apart") is contraindicated for intussusceptions
Mass ligation
Fatty mesentery makes vasculature difficult to see for resection and anastomosis, for this reason you should perform _______________
End to end or side to side with suture (not stapling devices or ligasure electrocautery)
What is the best way to perform a resection and anastomosis?
Intestinal volvulus
Rotation of intestine about mesenteric attachment
Root of the mesentery
Volvulus of the ___________________ leads to the entire SI being involved
Cardiovascular shock
Intestinal volvulus of the root of the mesentery leads to ____________________
Acute obstruction
Intestinal volvulus of the jejunal flange leads to ___________________
Marked distention of SI
What will you feel on rectal for an intestinal volvulus?
Distended amotile loops (stacked Olympic rings)
What will you see on ultrasound for intestinal volvulus?
1. Immediate surgical correction
2. Standing right paralumbar fossa
3. Detorsion of twist (R&A if indicated)
How do you treat intestinal volvulus?
B
T or F: There is better survivability of root of mesentery intestinal volvulus compared to jejunal flange intestinal volvulus
Pelvis
The blind end (apex) or the cecum points towards the ____________
Proximal loop of ascending colon
Dorsally, the cecum is attached to the ______________________
Ileum
Ventrally, the cecum is attached to the _______________
1. Right paralumbar ping and positive succussion
2. Tense dome shaped hollow viscus in pelvic canal on rectal
What are important findings that suggest cecal dilation?
1. Tachycardia
2. Colic
3. Abdominal distention
4. Larger ping area
What are clinical signs of cecal volvulus?
1. Fluids, NSAIDs, off feed for ~24 hours
2. Surgery if deterioration
If there is only cecal dilation and the cow is still passing feces, what is the treatment?
1. Standing right flank laparotomy
2. Typhlotomy
How do you treat cecal dilation/volvulus?
A
T or F: Resection is NOT indicated for the first surgical procedure when correcting cecal dilation/volvulus
Axial
The normal anatomic position of the cecum is the spiral loop ascending colon is ____________ to the cecum and proximal loop of ascending colon
Salvage procedure
If there is atresia ani, what should be done?
Euthanasia
If there is atresia coli, what should be done?
A
T or F: Meconium impactions are NOT common in calves
1. Sedation and epidural
2. Abdominal pressure to find bulge
3. Remove skin (~quarter size where rectum should be)
4. Blunt dissection down to "balloon" and around to free up rectal pouch
5. Place stay sutures
6. Full thickness simple interrupted sutures
Describe the salvage procedure to atresia ani (6)
Vaginal prolapse
ID prolapse
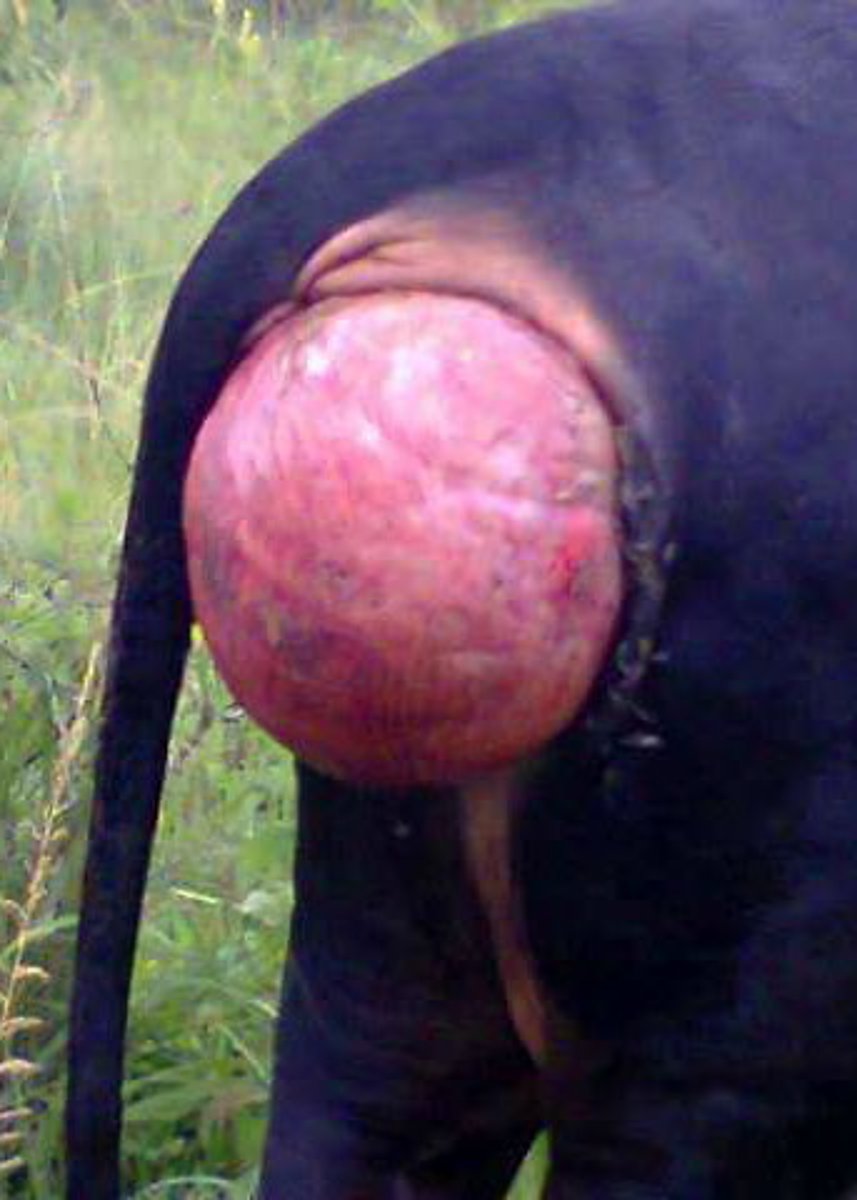
Cervical prolapse
ID prolapse
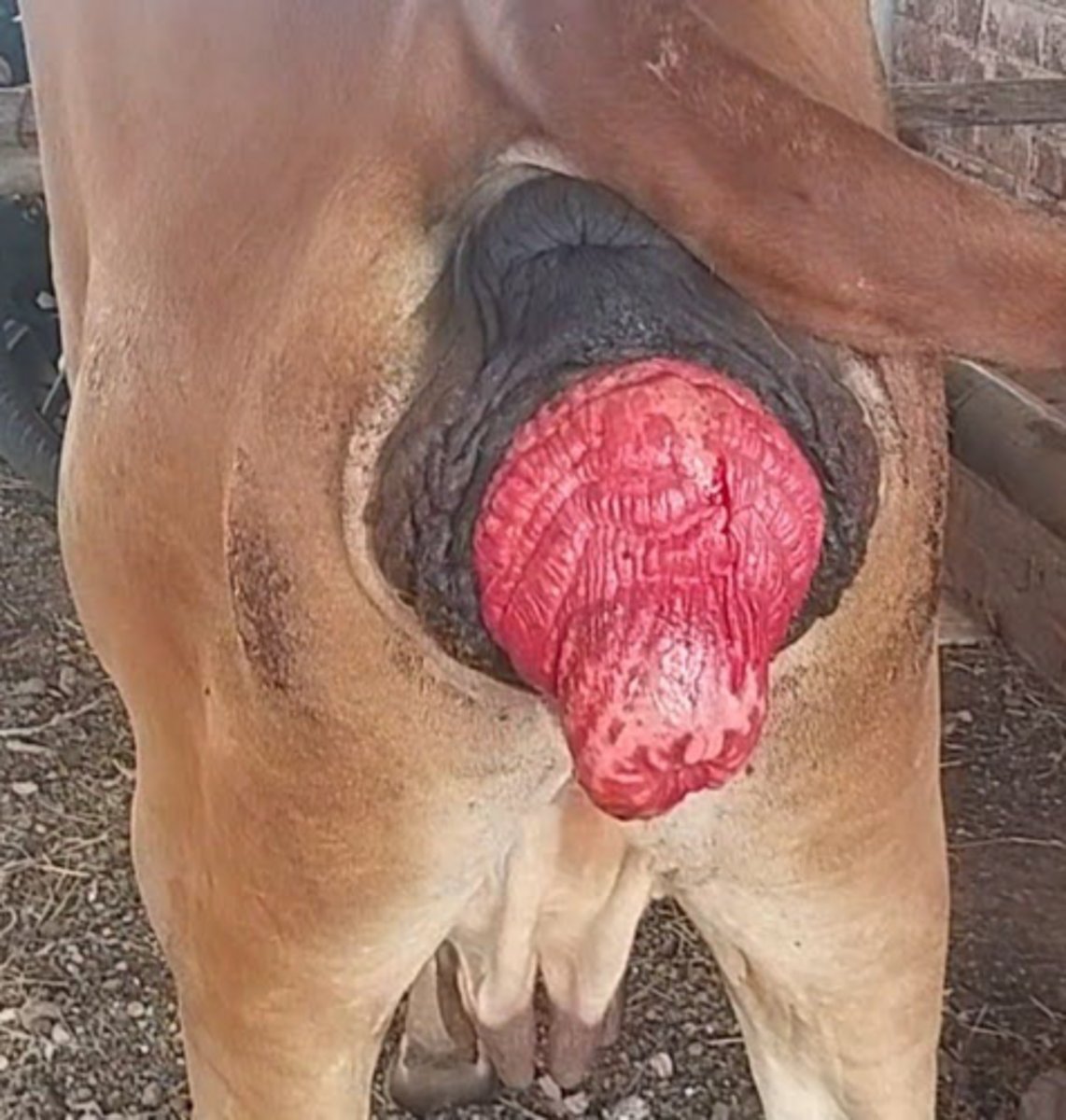
Uterine prolapse
ID prolapse
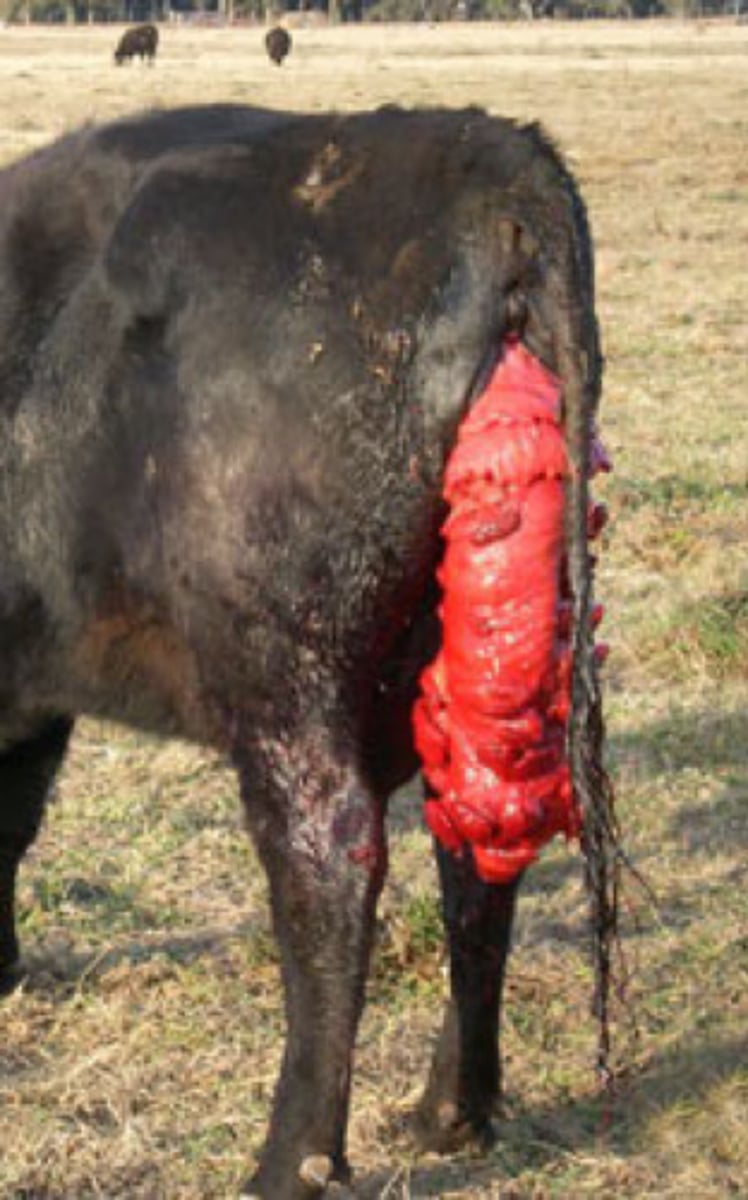
Rectal prolapse
ID prolapse
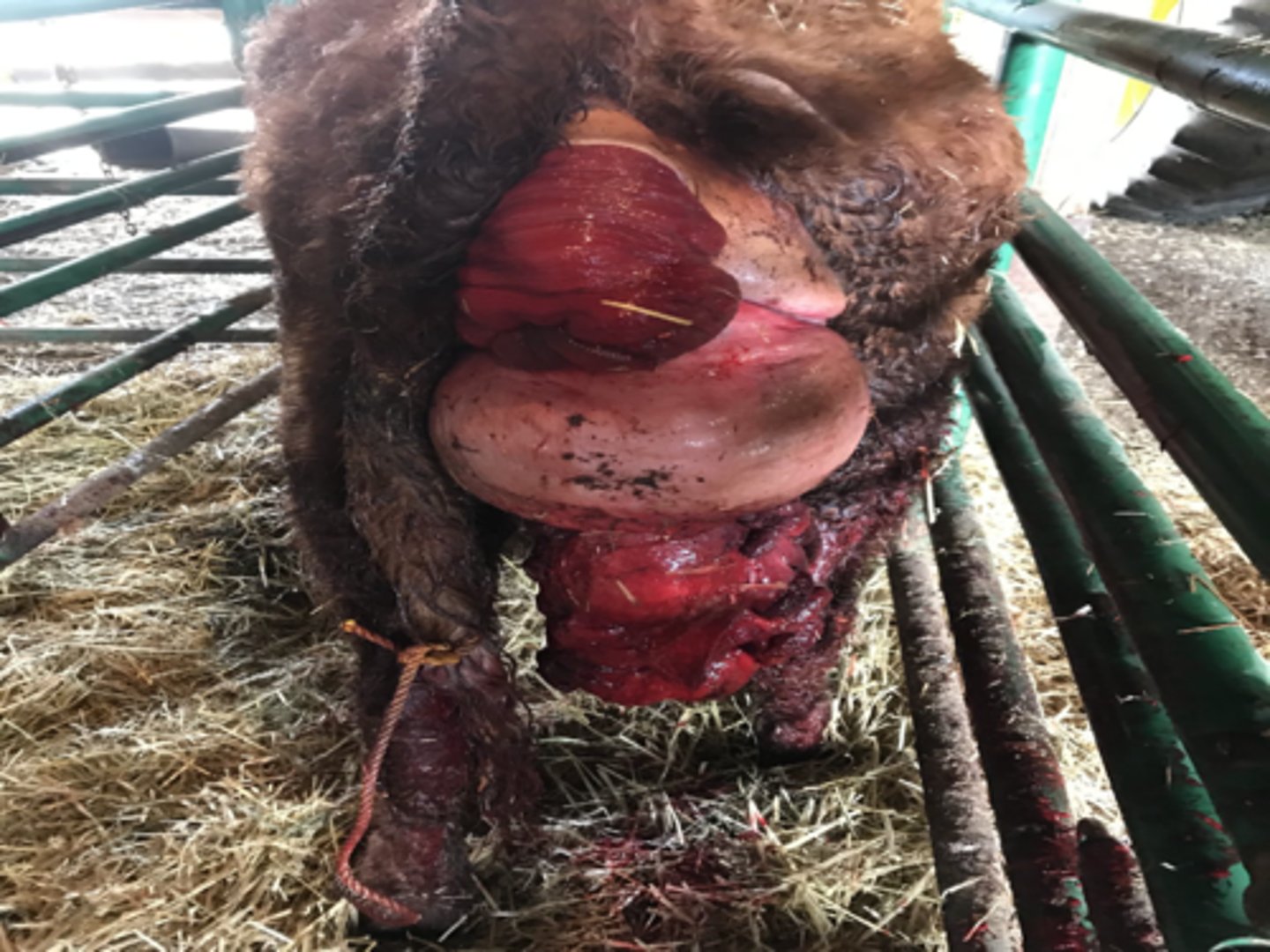
Increase in abdominal pressure or inadequate sphincter tone
Rectal prolapse occurs due to what?
1. Too short tail dockings
2. Enteritis
3. Chronic coughing
4. Straining from cystitis, dystocia
What are causes of rectal prolapse?
I
Anatomical classification of rectal prolapse: rectal mucosa only; small intermittent
II
Anatomical classification of rectal prolapse: all layers (mucosa to serosa) of rectum, variable length
III
Anatomical classification of rectal prolapse: all layers of rectum and prolapse of large colon
IV
Anatomical classification of rectal prolapse: sphincter intact with intussusception of colon and rectum through anus (palpable trench)
I
Extent of injury from rectal prolapse classification: mucosa and submucosa only
II
Extent of injury from rectal prolapse classification: disruption of muscular layers (diverticulum)
III
Extent of injury from rectal prolapse classification: serosa intact
IV
Extent of injury from rectal prolapse classification: al layers torn
1. Sugar
2. Hypertonic saline
3. Compression
What can be used to help correct rectal prolapse?