Unit 4: Newborn
1/94
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
95 Terms
neonatal period
from birth to day 28 of life
newborn physiologic taksks to extrauterine life involve
establishing & maintaining respirations
adjusting to circulatory changes
regulating temp
ingesting, retaining and digesting nutrients
eliminating waste
regulating weight
establishing & maintaining respirations
# 1 priority
bag and mask respirations if needed or mouth to mouth (over mouth and nose)
babies usually will never need compressions
adjusting to circulatory changes
ductus venous, foramen ovale, and ducts arteriosus close after birth
may stay open for 24 hours & heard as a murmur - normal
unless accompanied by other s/s (poor feeding, aepnic periods over 20 seconds, cyanosis , pallor)
regulating temp
#2 priority after breathing
a cold baby has low sugar - causes issues with the brain
naked under radiant warmer OR skin to skin with mom if he’s healthy (with hat & blanket)
eliminating waste
babies need to void and stool at least once in 24 hours after birth (may not happen if baby is nit eating well)
After day 4, six to eight voidings per day of pale straw-colored urine indicate adequate fluid intake.
regulating weight
babies will lose up to 10% of weight in the first 3 days, should return in 10-14 days
assess if he’s eating well
weigh babies the at the same time, same way each time according to policy (naked or just diaper)
blanket on the scale to avoid heat loss
newborn behavioral tasks to adjust to extrauterine life
establishing a regulated behavioral tempo independent of mom, involving regulations self arousal, self monitoring changes in state and patterning sleep
processing,storing and organizing multiple stimuli
establishing relationships with caregiver/ environment
predictable series of events 6-8 hours after birth
involve sympathetic NS
changes in HR, Respirations, temp, GI function
baby is very vulnerable - watch closely!
first period of reactivity
how long?
HR, RR LOC of baby?
Bowel sounds? movement?
lasts for 30 minutes after birth
1st stage of transition
baby is awake - great time for feeding if baby can go straight to mom
HR - increases to 160-180 bpm but will gradually decrease
RR - may be irregular, can be as high as 60-80
Bowel sounds can be heard, may pass meconium
can have startle tremors, movement , good tone
if we hear abnormal lung sounds/ see abnormal breathing in the first period of reactivity?
fine crackles, audible grunts
nasal flaring, retractions
give him time to resolve (about 1 hr), baby is still expelling fluid but watch closely
get him to cry - expels fluid and opens lung
how do we elicit cries
dry him off after birth for heat conservation - it bothers him
back rub
flick feet
wash face with warm water
period of decreased responsiveness
LOC? RR? Bowel sounds/?
60 -100 minutes
very sleepy
marked decrease in motor activity
skin should stay pink
RR - rapid, up to 60, shallow and unlabored
Bowel sound present
2nd period of reactivity
2-8 hours post birth
can last from 10 minutes to many hours
common to pass mec
improved skin color
mucous production
increased muscle tine
very preterm - will not have this stage
once baby is out
cut cord in between 2 clamps to avoid bleeding, cause rise in BP & lung perfusion
most important is establishing effective respirations
prxtermers may have difficulty
chemical factors of breathing initiation
it is thought that from cutting the cord, prostoglandins drop
helps with the initiation of breathing
mechanical factors of breathing initiation
pressure of baby coming out vaginal Canal expels fluid out of the lungs
crying opens alveoli
thermal factors of breathing initiation
colder outside the uterus
stimulates breathing
sensory factors of breathing initiation
suctioning with bulb syringe right when head is out
suction mouth before nose (1 side of mouth, then each nostril)
dry baby off to get all the fluid off and to warm him
environment around him stimulates baby
if fluid is retained
interferes with baby’s ability to maintain respiration & oxygen
transient tachypnea
if baby has aspirated on meconium in utero, it will affect his breathing
transient tachypnea
respiratory distress up to 2 hrs post brith,
may go up to 100bpm
goes to NICU
will need supplemental O2
will resolve on 48-27 hrs
Normal respirations
shallow
30-60 normal range (but may go up if he’s crying a lot)
may have aepnic periods up to 20 seconds - anything longer abnormal
s/s of respiratory distress
nasal flaring
intercostal or subcostal retractions
grunting
what can case abnormal apnea
hyper or hypothermia
hypoglycemia
sepsis - babies will usually present with a low temp if septic
tachypnea
comes form inadequate clearing of fluid
may be first sign of illness
can be result if respiratory distress syndrome (generally in premature babies or babies of diabetic moms, bc of lack of surfactant)
acrocyanosis
normal finding in the first 24 hours
blue on hands and feet
central cyanosis
blueness of lips, mucous membranes (circumoral)
abnormal
significant hypoxia
late sign of distress, inadequate oxygenation, poor tissue perfusion, cardiac dysfunction
signs of respiratory distress
nasal flaring , retractions, grunting
RR under 30 or over 60 - needs evaluation!
apnea
hyper or hypothermia
hypoglycemia
sepsis
tachypnea
color changes
cardiovascular system adaptations
CO duoubles
blood flow increases to lungs , kidney , heart , GI
pulmonary artery pressure drops
normal HR 120-160, can drop if baby is sleeping, can go up if baby is crying
umbilical cord becomes ligament
foramen ovale closure
increase in pulmonary blood flow from the left slide of the lungs to close foramen ovale
crying - can reverse the closure of the Forman ovale
ductus arteriosus closure
functionally closes within 24 hours
permanently closes within 2-3 months, turns into a ligament
may reopen if O2 levels are low as a protective measure - detected as murmur
pallor can indicate
anemia or bleeding
jaundice
can either be from hyperbillirubinemia
tx: phototherapy
may also be from Rh factor or ABO incompatibility with mom
delayed cord clamping
delayed cord clamping (3min) increases blood volume and clamping
also decreases risk of intro ventricular hemorrhage
decreases risk of necrotizing enterocolitis
both preemie problems
ma cause hyperbillirubinemia
increase in blood volume
can happen from delayed cord clamping
can cause polycythemia - high RBC and H&H
Thermogenic system
#2 most important after respiratory
thermoregulation: the
convection
the flow of heat from the body surface to cooler ambient air
babies need to swaddled in crib and with hat to prevent heat loss by convection
keep babies away from windows and open doors
radiation
loss of heat from the body surface to a cooler solid surface not in direct contact but in relative proximity.
keep babies away from windows and open doors to prevent heat loss by radiation
Evaporation
the loss of heat that occurs when a liquid is converted to a vapor
keep babies dry! sponge baths in sections & dry after birth with clean, dry linens each time
conduction
the loss of heat from the body surface to cooler surfaces in direct contact
scale, circumsicion restraint board, cold hands , cold stethoscopes
pre warm the radiant warmer
blanket on the scale
skin to skin reduces which heat loss
conduction and radiation
thermogenesis
baby trying to produce their own heat - non shivering
uses stores of brown fat - less in preterm babies
hypothermia and cold stress effects
vessels vasoconstrict
makes extremities cool
imposes physiologic and respiratory demands
RR increases
O2 and energy diverted away form normal brain and cardiac function
hypoglycemia
hyperthermia
temp of 99.5 or more
caused by too hot of a warmer, or swaddled in the warmer
can cause neurologic issues, seizures, death from heat stroke
an infant who has not voided by 24 hours should be assessed for
adequacy if fluid intake
bladder distention
restlessness / s/s of discomfort
renal problmems
s/s: lack of steady stream , can indicate:
hypospadias - the urethral opening forms on the underside of the penis rather than the tip
epispadias - the urethral opening forms on the upper side of the penis rather than the tip, or between clitoris and labia in girls
feeding behavior is related to
gestational age
neuromuscular maturity
maternal medications
type of initial feeding
Meconium
First stool: composed of amniotic fluid and its constituents, intestinal secretions, shed mucosal cells, and possibly blood (ingested maternal blood or minor bleeding of alimentary tract vessels).
Dark, olive green in color; viscous and sticky (like tar), almost odorless.
Passage of meconium should occur within the first 24–48 h, although it can be delayed up to 7 days in very low-birth–weight infants.
Passage of meconium can occur in utero and can be a sign of fetal distress
back stools after meconium has passed
sign of upper GI bleed - not good
red blood - lower GI blood
Transitional Stools
• Usually appear by third day after initiation of feeding.
• Greenish brown to yellowish brown; thin and less sticky than meconium; can contain some milk curds
Milk Stool
• Usually appears by the fourth day.
• Breastmilk: yellow to golden, pasty in consistency; resemble a mixture of mustard and cottage cheese, with an odor similar to sour milk.
• Commercial infant formula: stools pale yellow to light brown, firmer consistency, stronger odor than breast milk stools.
GI problems
non-patent anus
stool coming from anywhere but the rectum can indicate fistula
risks for hyperbillirubinemia
• Preterm
• Breastfeeding: especially if exclusively breastfeeding and weight loss is excessive
• Rh or ABO incompatibility or other known hemolytic disease (e.g., G6PD deficiency)
• Polycythemia
• Asian or Native American race
• Bruising related to birth trauma
• Previous sibling who received phototherapy for hyperbillirubinemia
Vitamin K
1 IM shot @ birth for coag synthesis
do no develop for 9 months
all newborns at risk for bleeding until coags have developed
all circumcised babies - at risk for bleeding
Immune system
immune response is decreased @ birth & immunoglobulins are low
makes babies succeptible to pathogens
breastmilk - passes immnunoglobuin A
s/s of infection in newborns
temp instability - usually hypothermic
lethargy
irritability
poor feeder
vomiting (not spit up)
diarrhea (not normal soft stools)
decreased reflexes
pallor / mottled skin (red and patchy)
discharge from eyes , nose, mouth
some rashes
dyspnea if respiratory infection
desquamation
skin peeling
leave the vernix to protect skin
milia
Distended, small, white sebaceous (sweat) glands noticeable on the newborn face
babies do not sweat for 24 hours
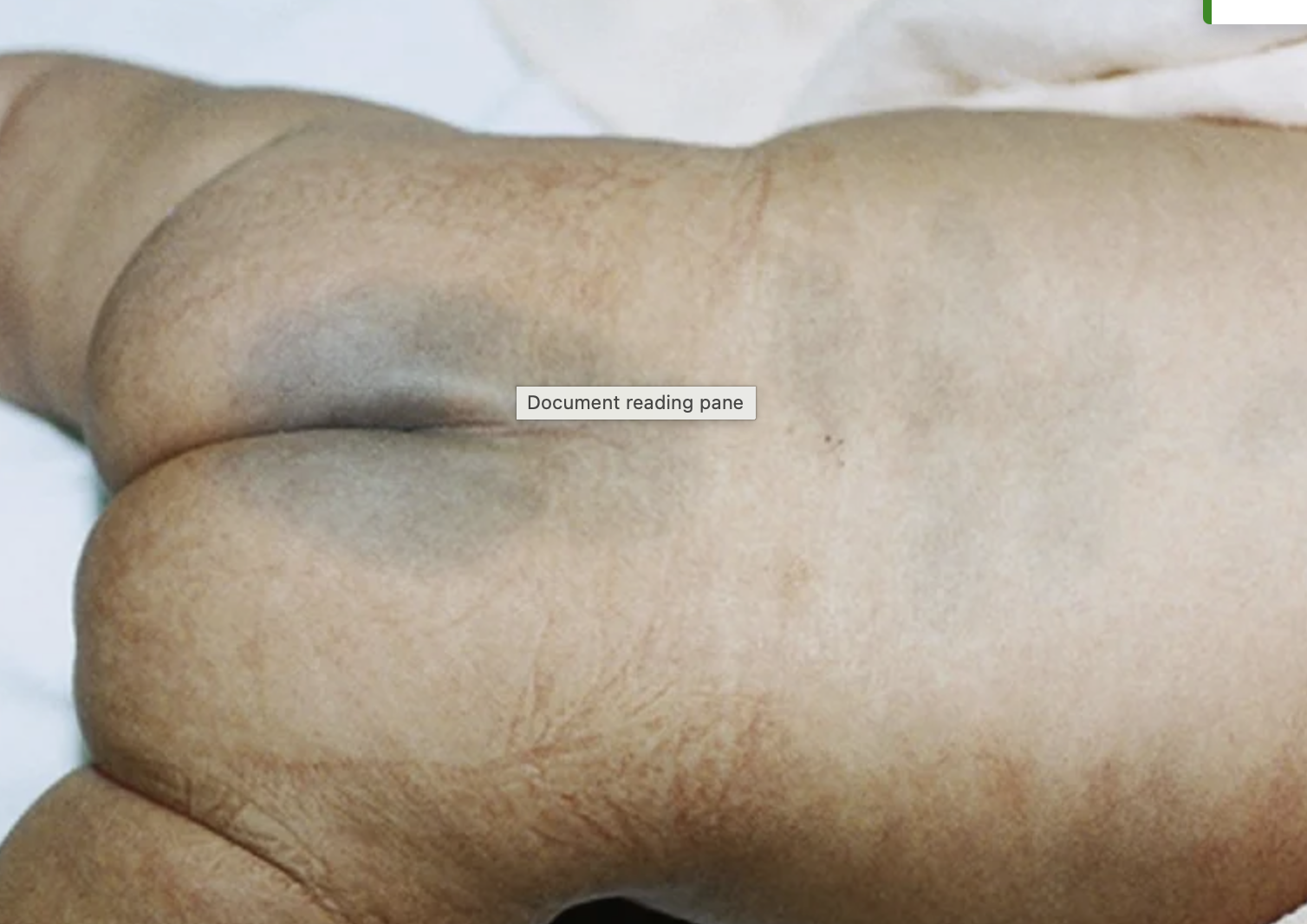
slate gray nevi
aka mongolian spot
blue/black area - not a bruise
more common on dark skin
may takes months or years to fade
usually seen on buttocks area but can be seen on arms and legs
nevi simplex
seen in 80% of newborns
superficial capillary defect
aka stork bite
usually small, flat, and pink and are easily blanch-able
common sites are the upper eyelids, nose, upper lip, and nape of the neck.
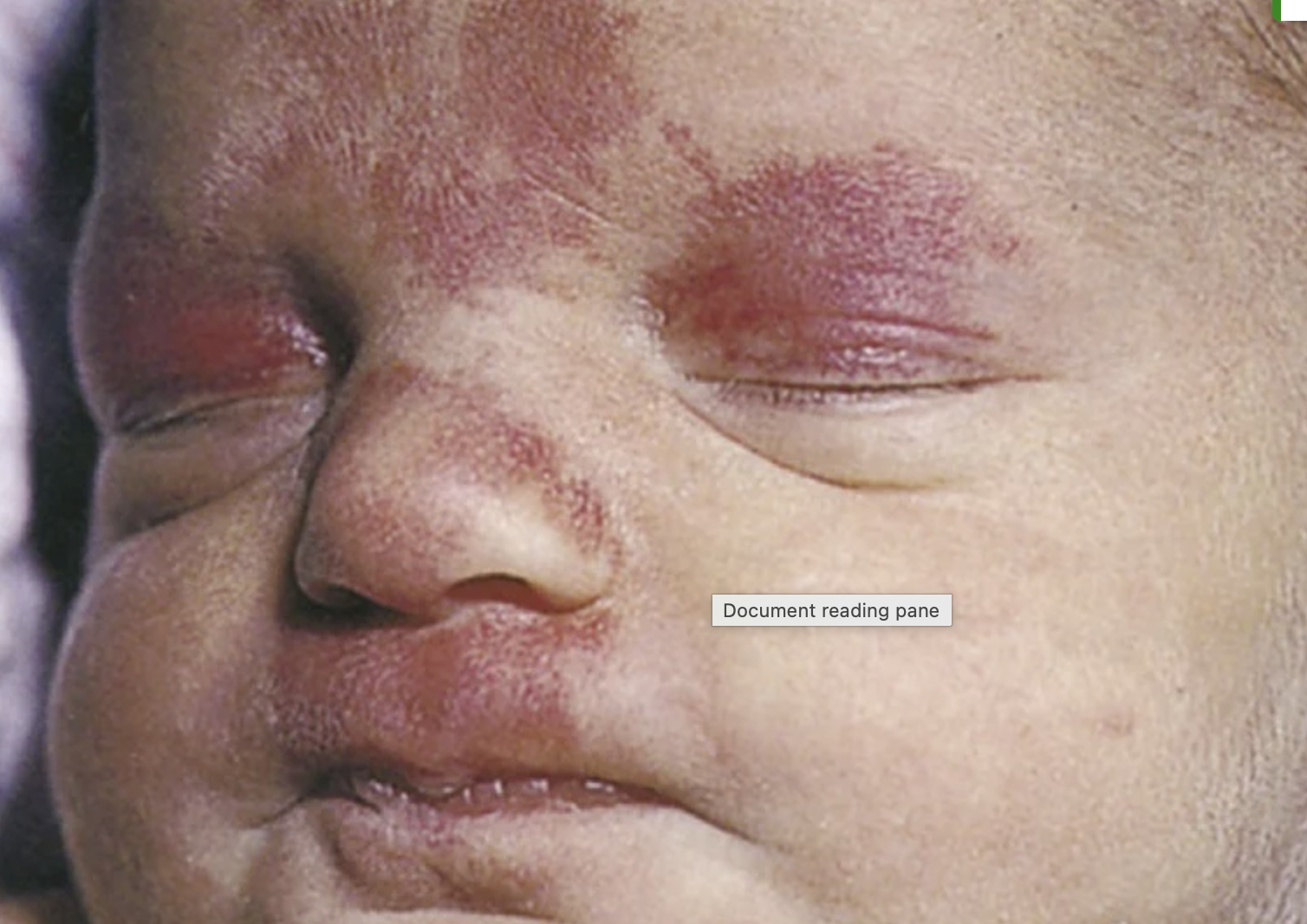
nevus flammeus
aka port wine stain
doesn't blanch
darkens over time - purple color
Infantile hemangiomas
newly formed capillaries that are dilated
come from dermal and subdermal layers
may be present at birth or come after
raised red bumps, rough to touch
goes away in 5-10 years
Erythema toxicum
transient newborn rash - comes and goes and moves around the body
appears in term neonates during the first 24 to 72 hours after birth and can last until up to 3 weeks of age.
no need to Treat
s/s of integumentary problems
pallor
petechia - not significant in first 24 hours
cyanosis
birth injuries
female reproductive system
genitalia usually edematous
vaginal tags common
leave vernix between the labia if any to not aggravate
stool - remove with warm washcloth
male reproductive system
foreskin should completely cover glans penis
urethra should be @ tip (abnormal - hypospadias or epiespadas)
if he has hypospadias, he will not be circumcised in the hospital (needs to be repaired and the foreskin is used in that)
palpate testes to make sure they are descended
asses for rugae - lines on scrotum sac
Hydrocele
caused by an accumulation of fluid around the testes, can be present.
Hydroceles can be easily transilluminated with a light (pen light shines through )
usually resolve without treatment
how do moms hormones affect baby
both boy and girls may have swelling int he breast tissue from moms hormones
may cause psuedomenses in girls - not a period
ambiguous genitalia
cannot tell if the baby is male or female
usually needs continuing care past postpartum stay
may get surgery in the future
Caput succedaneum
considered birth injury
generalized edematous area of scalp
most often on occiput
extends across suture line
resolves in 3-4 days
Cephalhematoma
considered birth injury
collection of blood between skull and periosteum
does not cross suture line
resolves in 2-8 weeks
raises risk for hyperbillurubinemia (hemolysis of RBCs)
Subgaleal hemorrhage
bleeding into subgaleal compartment
associated with difficult operative births (vaccum)
scalp is pulled away from bone, vessels torn and blood collects
blood loss can be severe → hypovolemic shock
may result in Disseminated intravascular coagulation (DIC) - severe bleeding, life threatening
early detection is vital - continue to measure head circumference
feels boggy to touch
tachycardia, pallor, increase bilirubin level, may need transfusion of blood or clotting factors
spine
straight, symmetrical and easily flexible
no opening or pilonidal dimple - checking for spina bifida
polydactyl and oligodactlyl
polydactyl - more than 10 finger
oligodactyl - less than 10 fingers
hip dysplasia s/s
instability or dislocation of the hip joint caused by a shallow socket
asymmetric gluteal and thing fold
uneven knees
neuromuscular system
almost completely developed @ birth
brain requires glucose to grow rapidly
sutures allow for that growth
tremors can be normal
jitteriness of upper extremities - hypoglycemia
what would cause hypoglycemia
not eating
cold
stress
illness
baby of a diabetic mom
rooting
do it before feedings, bc they won’t if they are not hungry
sleep-wake states
Variations in the state of consciousness of infants
The six states form a continuum from deep sleep to extreme irritability
the ability to make smooth transitions between states is called state modulation
habituation
ability to respond to and then inhibit responding to discrete stimulus (e.g., light, rattle, bell, pinprick) while asleep
baby wakes up less and less to the same stimuli bc he has processes that information
Orientation
quality of alert states and ability to attend to visual and auditory stimuli while alert
Motor performance
quality of movement and tone
Range of state
measure of general arousal level or arousability of infant
Regulation of state
how infant responds when aroused
Autonomic stability
signs of stress (e.g., tremors, startles, skin color) related to homeostatic (self-regulator) adjustment of the nervous system
immediate care after birth
respirations - only 10% of babies need extra help (O2 usually )
warmth - skin to skin with hat & blanket
Apgar scores include
heart rate
respiratory rate
muscle tone
reflex irritatabiltiy
generalized skin color
made @ 1 minute and at 5 minutes
sometimes @ 10 minutes
most babies will not get a full 10 because ?
they lose points due to skin color
a baby will no go to the warmer if
it is a preterm baby
has poor muscle tone
baby is not breathing
how can you asses the heart rate
stethoscope
palpating umbilical cord
baby with Apgar score 7-10
baby has no difficulty transitioning
baby with Apgar score 4-6
baby is having moderate difficulty transitioning
baby with Apgar score 0-3
severe difficulty transitioning
newborn vitals usually include
temp, hr and respirations
usually not a BP or SpO2