21- Non ST segment elevation Acute Coronary Syndrome I. Etiology, manifestations, diagnosis.
1/31
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
32 Terms
what is acute coronary syndrome
inbalance of O2 supply + demand
what are the types of ACS without ST elevation
unstable angina
NSTEMI
what is the cause of NSTEMI
partial coronary occlusion
usually not complete occlusion
what are the characteristics of NSTEMI
more freqent than STEMI
most common indication for coronography
patients are usually older than in STEMI
more comorbidities in patients
equal or wosrse prognosis than STEMI
what are the causes of O2 supply decrease
acute coronary perfusion deficit
acute cardiac but not coronary origin
extracardiac origin
severe anaemia
what are the causes of acute coronary perfusion deficits
C plaque rupture → partial or total occlusion
C a. stenosis
C a. spasm
prinzmetal angina, cocaine, takotsubi
C embolisation
what are the causes of acute cardiac but not coronary origin
severe aortic stenosis
cardiac decompensation
what are the causes of O2 demand increase
heavy exercise
hyperthyrosis
shock
sepsis
describe prinzmetal angina
temporary partial or total coronary occlusion due to coronary spasm
mainly:
at dawn
in smoker, middle age women
can lead to malignant arrhythmia- VF
urgent coronography
prognosis is different
with coronary stenosis w/o revascualrisation poor, with is good
w/o coronary stenosis with medical treatment is good
what are the risk factors for ACS
family history
smoking
HT
hypercholesterinemia
DM
what are the complaints in ACS
pain
shortness of breath
sweating
dizziness
fear from death
what is visible upon inspection of ACS pts
pallor, anaemia
cyanosis
shortness of breath, orthopnea, periodic (cheyne stokes) respiration
distention of collar veins
what are the laboratory tests performed
biomarker release
troponin T and I
CK- MB
what is the Wash out phenomenon
rapidly and higher peak of cardiac marker after successful reperfusion therapy
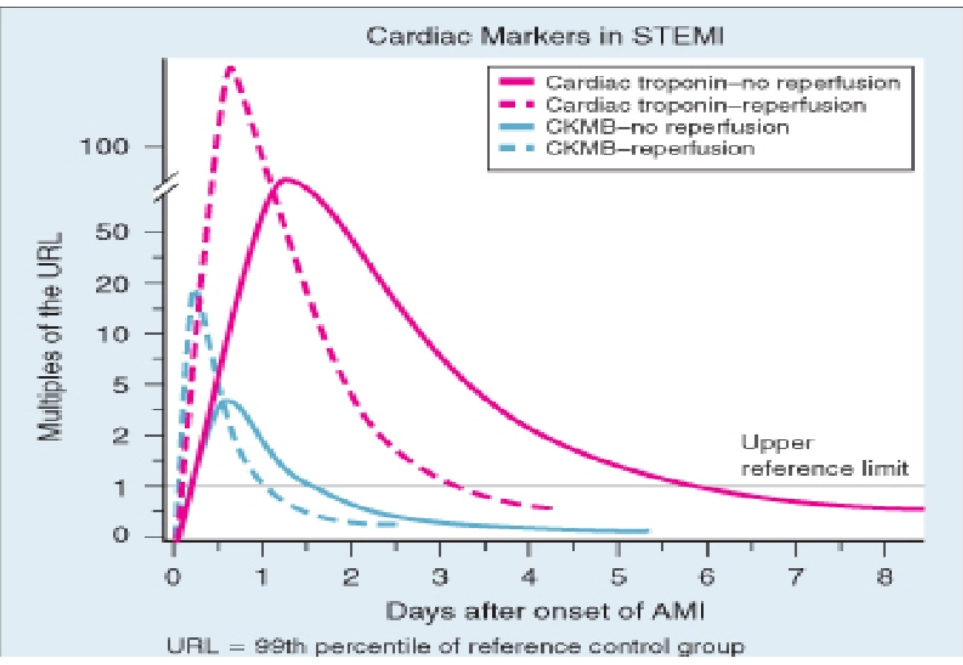
what are the ECG findings
must be made within 10 min of first contact
ST segment depression
T wave inversions
what are some other diseases that mimic the same ECG findings
ischemia
CVA
apical HCM
what is the Dx
PE
acute aortic syndrome
haematoma, penetrating atherosclerotic ulcer, aortic dissection
other
pleuritis
gastro oesophageal disease
myositis
gastric or duodenal ulcer
gallbladder pain
what is the risk stratification
calculation of acute and long term prognosis
what is the risk stratification based on
clinical condition
co morbidity
suggests high probability of CHD
GRACE score
what is the clinical condition in risk stratification
ongoing chest pain
haemodynamic status
HF, cardiogenic shock, resuscitation
complication- arrhythmia, mechanical complication
what is NSTE
NSTEMI → subendocardial infarction → due to partial occlusion of coronary artery
more common than STEMI
most common indication of coronary angiography
what is the cause of NSTE ACS
subendocarial ischemia
what is NSTEMI
subendocardial necrosis → irreversible injury/ death
increased cardiac biomarkers
ST depression + T inversion
what are the comorbidities in NSTE
DM
impaired LV function
previous myocardial infarction
previous coronary revascularisation- PCI, CABG
what is the GRACE score
risk model that takes different factors into account
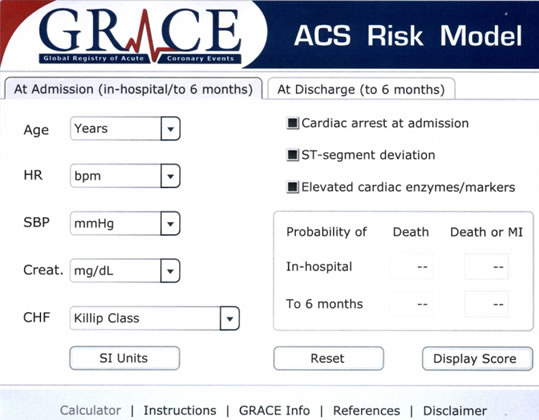

()
when is ACS NSTEMI very high risk
needs immediate invasive strategy
refractory/ recurrent angina despite intense antianginal treatment
deep ST depression >2mm in V1-4
HF or shock
life threatening arrhythmias
resuscitation
other complications
when is ACS NSTEMI high risk
early invasive needed <24h
GRACE score ≥140
elevated troponin
dyanmic ST-T changes
DM
renal failure
depressed LV function EF<40%
early post MI angina
PCI within 6 months
previous CABG
intermediate or high risk according to risk score
what are the complications of ACS
arrhythmias
HF- LV mass loss >40%
mechanic complications
what are the life threatening arrhythmias in ACS
ventricular tachycardia/ ventricular fibrillation
II-III degree AV block
describe the HF in ACS
pulmonary congestion
cardiogenic shock
RV failure- impaired filling pressure
describe the mechanical complications in ACS
mitral papillar rupture- acute mitral regurgitation
ventricular septal rupture
free wall rupture- pericardial tamponad