micro bio lecture test 3
1/167
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
168 Terms
CFU
colony forming unit
sterilization
removing and destorying all microbial life
commerical sterilization
killing c. botulinum endospores from canned goods
disinfection
destroying harmful microorganisms (kills 99.9 of bacterica and viruses)
antispsis
destroying harmful microorganisms from living tissue (mouth wash)
degerming
the mechanical removal or microbes from a limited area
sanitation
lowering microbial counts on eating utensils
sepsis
refers to bacterial contamination
asepsis
absence of significant contamination
biocide (germicide) treatments
kill microbes but not necessarily endospores
bacteriostatic and fungistatic
inhibit microbial and fungal growth
biological safety levels (BSLs)
CDC and NIH made 4 classification levels based on risks associased with specific pathogens
BSL- 1
used in lab/ minimal risk
BSL- 2
moderate risk to workers and environment
BSL- 3
cause serious or potential lethal diseases thru respiratory transmission
BSL-4
high risk and fatal without treatment or vaccines
BSL determined by
agents infectivity
ease or transmission, potential disease severity
type of work being done with agent
dry heat
kills by oxidation
moist heat
denatures enzymes and proteins
combination of heat and pressue
autoclave
high pressure
denatures protein, endospores may resist
desiccation
addition of solute creating a hypertonic environment, drawing water out of cells
radiation
causes the formation of thymine dimers in DNA, leading to lethal mutation in the exposed microes
food irradiation
exposed to gamma radiation by passage on a conveyor belt thru a radiation chamber
filtration
passage of liquids and air thru a screenlike material
used for heat sensitive materials
joseph lister
began using carbolic acid, phenol, as disinfectant for the treatment of surgical wounds
most common halogens
iodine, chlorine, fluorine
iodine
works by oxidizing cellular components, including sulfur-containing amino acids, nucleotides, amino acids
heavy metals
kill microbes by binding to proteins, thus inhibiting enzymatic activity
conditions influencing effectiveness of antimicroial agent
population size/ composition
concentration or intensity of an antimicrobial agent
duration of exposure
temperature
local environment
disk diffusion
method to evaluate the efficacy of chemical agents
surfactants
surface active agents, a group of chemical compounds that lower the surface tension of water
chemotherapy
the use of chemicals to treat a disease
selective toxicity
selectively finding and destorying pathogens without damaging the host
antibiotic
substance produced by a microbe that, in small amounts, inhibits another microbe
antimicrobial drugs
synthetic substances that interfere with the growth of microbes
salvarsan
arscenic containing compounds, Ehrlich and Hata discovered
penicillin
Fleming discovered
Prontosil
red dye, used for strep and staphylococcal infections
prontosil
Klarer, Mietzsch, and Domagk discovered
natural antibiotics
compounds isolated from organisms
natural antibiotics
mold, fungi, bacteria
semisynthetic antimicrobials
chemically modified derivative of a natural antibiotic
synthetic antimicrobial
developed from a chemical not found in nature
narrow spectrum of microbial activity
drugs that affect a narrow range of microbial types
broad spectrum antibiotics
affect a broad range of gram postive or gram negative bacteria
dosage
amount of medication given during a certain time interval
orally
pros- patients can more conveniently take drugs at home
cons- some drugs are not easily absorbed by GI tract into blood stream
parenteral ( intravenous or intramuscular injection)
pros- short time to reach high concentration in plasma
cons- typically preformed in health-care settings
half life of drug
rate at which 50% of a drug is eliminated from the plasma (doses/day X toxicity)
toxicity
side effects caused by the drug
selective toxicity
selectively kills or inhibits the growth of microbial targets while causing minimal or no harm to the host
synergism
two antibacterial drugs may be administered together to improve efficacy
atagonism
can occur between two antimicrobials or between antimicrobials and non antimicrobials being used to treat other conditions
inhibition of cell wall synthesis
B- lactam ring prevents the synthesis of peptidoglycan
gram postive
thick cell wall
gram negative
thin cell wall
natural penicillins
extracted from penicillium cultures
narrow spectrum of activity
susceptible to penicillinases (B- lactamseses)
semisynthetic penicillins
contain chemically added side chains, making them resistant to penicillinases
Which of the following might make a disinfectant less effective?
Using a low concentration
Applying the disinfectant for a short amount of time
Presence of biofilms
All of the above
All of the above
Which of the following does not kill or inhibit bacteria but can mechanically remove bacteria from a surface?
Soaps
____________ is a physical method of microbial control.
Ionizing radiation
Which of the following is FALSE regarding specialized transduction?
Phages pick up bacterial DNA during exsicion and can transfer it to a new host
It occurs when random host DNA is packaged during the lytic cycle
It can change the genetic properties of a bacterium
All are correct
It occurs when random host DNA is packaged during the lytic cycle
Reverse transcriptase is an enzyme that some viruses use to make ______ using ______ as a template.
DNA; DNA
DNA; RNA
RNA; RNA
RNA; DNA
DNA; RNA
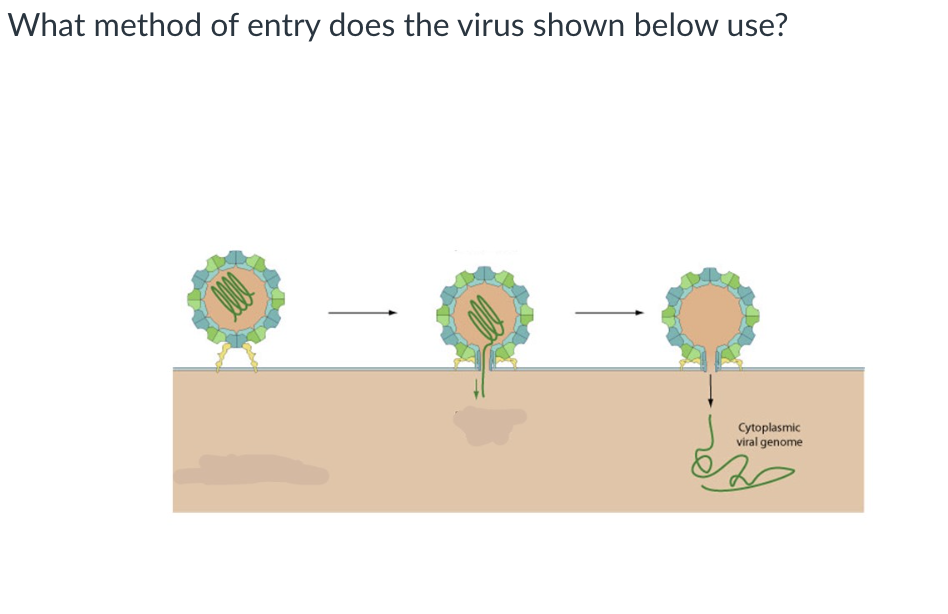
injection
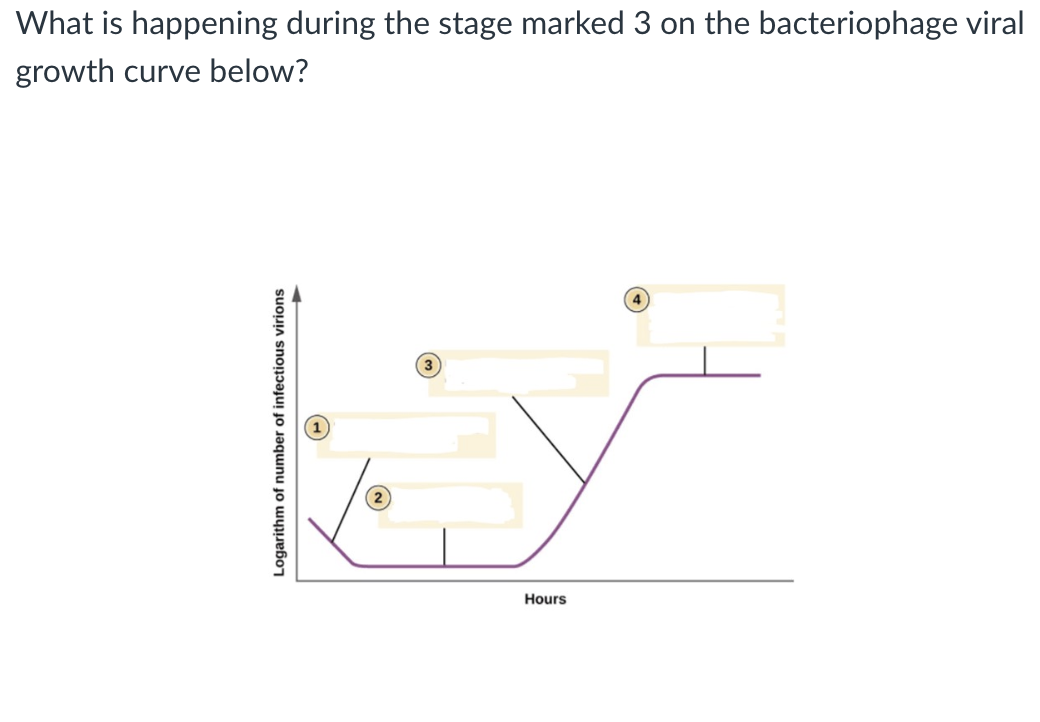
Viruses are released by lysing the bacteria
Chemotherapeutic agents that are natural products of microorganisms are most specifically referred to as __________.
antibiotic
Selective toxicity __________
harms the microbes without significantly harming the host.
Chemotherapeutic agents that are chemically modified natural products of microorganisms are most specifically referred to as __________.
semisynthetic drugs
When a chemotherapeutic agent is effective against many different pathogens, it is said to be a __________ antibiotic.
broad- spectrum
pathogenicity
the abilty of a microoorganism to cause disease or damage in a host organism
pathogenicity is often viewed as ?
binary, qualitative trait - microbe is either pathogenic or not
disease
any condition in which the normal structure or functions of the body are damaged or impaired
infection
sucessful colonization of a host by a microorganism (pathogen)
symptoms of disease are
subjective and felt or experianced
signs of disease are
objective and measurable
morbidity
number of cases of a disease
mortality
number of deaths due to a disease
infectious disease
caused by the direct effect of a pathogen
non-communicable
infectious disease that are not spead from one person to another
latrogenic
diseased contracted as the result of a medical procedures (wounds/ flesh eating clostridium)
nosocomial
diseases are acquired in hospital settings (MRSA)
zoonotic
diseased that can be transmitted form animals to humans (rabies, yellow fever, flu)
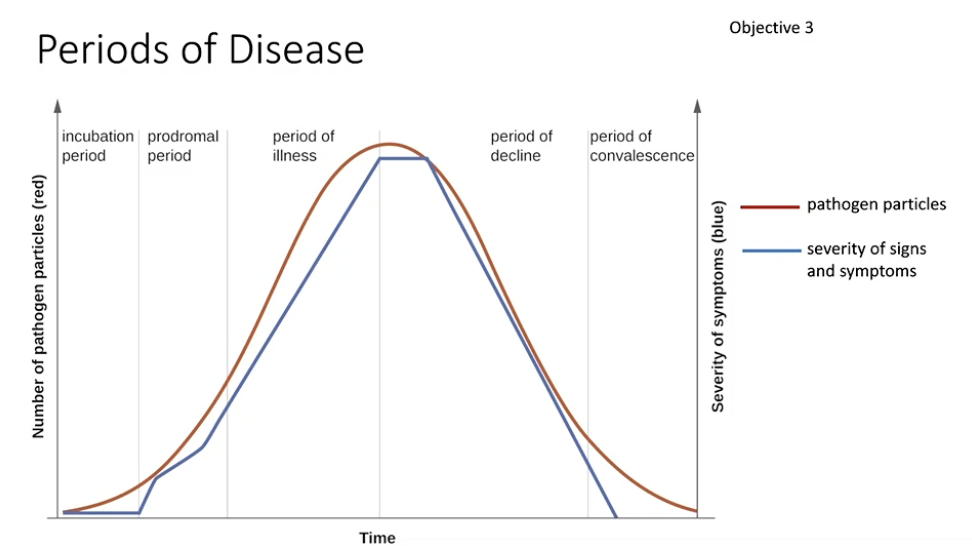
know whats going on
acute disease
short time ( hours, days, few weeks) and involve a rapid onset of disease conditions
chronic disease
longer time spans ( months, years, lifetimes)
molecular koch postulates
in 1988 stanley falkow proposed an updated version of koch postulates
looks for specific genes that make an organism cause disease
pathogenicity
the potential ability to cause disease, qualitative term
virulence
the diesase producing power of an organism or the degree of pathogenicity when compared within a group
median infectious dose
number of pathogen cells or viruons required to cause active infection in 50% of innoculated animals
median lethal dose
number of pathogenic cells, virons, or amount of toxin required to kill 50% of infected animals
primary pathogen
cause disease in a host regardless of the hosts resident microbiota or immune system
opportunistic pathogen
only cause disease in situatiosn that compromise the hosts defenses such as the bodys protective barriers, immune system or normal microbiota
mucosal surfaces
are most important portls of entry for microbes
adhesion
capabilty of pathogenic microbes to attach to the cells of the body using adhesion factors
invasion
dissemination of a pathogen throughout local tissues of the body pathogens may produce exoenzymes or toxins
infection
sucessful multiplication of the pathogen
local infection
confined to a small area of the body typically near portal of entry
focal infection
localized pathogen, or the toxins it produces can spread to a secondary location
systemic infection
infection becomes disseminated throughout the body