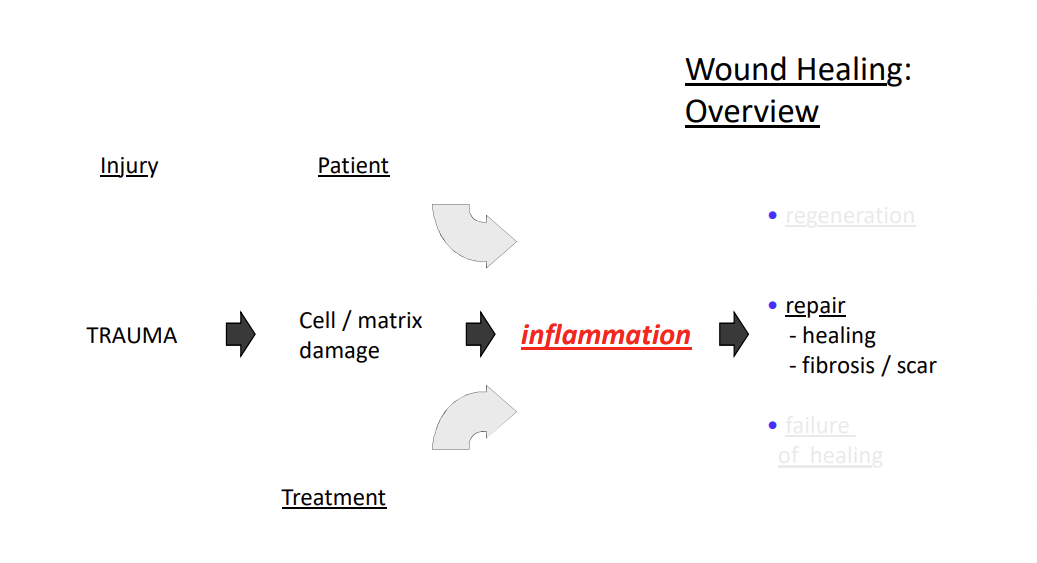
wound healing
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
why study wound healing?
most dental procedures involve wound healing - incising the gingiva, extracting teeth
some medications impact wound healing
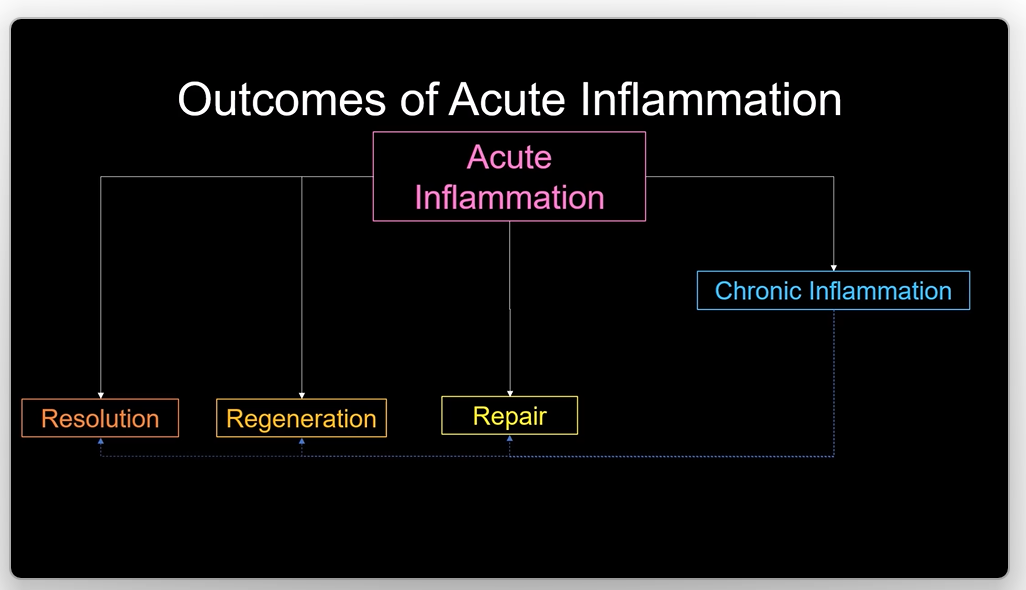
outcomes of acute inflammation - recap
resolution - wound healing
regeneration - wound healing
repair - wound healing
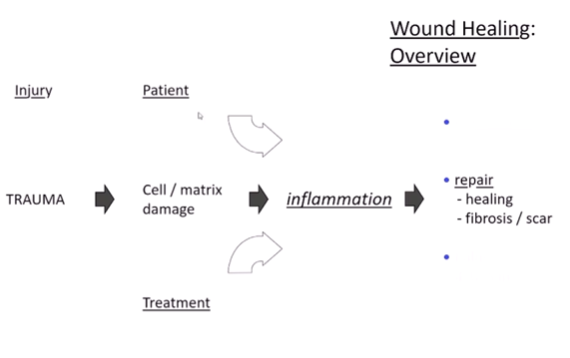
wound repair - overview
what is regeneration?
regeneration is the replacement of lost or damaged tissue by that of a similar type derived from the the proliferation of the surrounding undamaged cells
humans have latent capacity of regeneration

notable disscussion points for regeneration
liver cells have a high propensity for regeneration
teeth - developing research
what is repair?
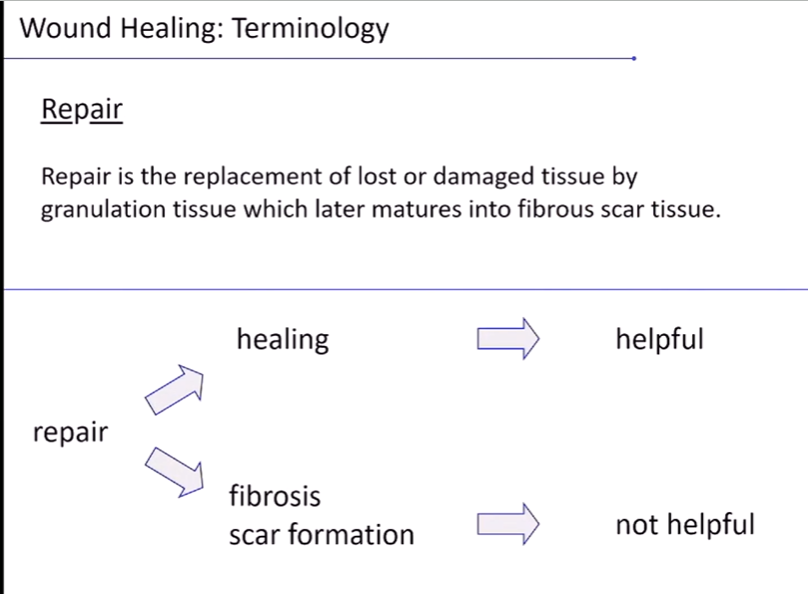
repair is the replacement of lost or damaged tissue by granulation tissue NOT GRANULOMA which later matures into fibrous scar tissue
repair can mean 2 things
healing - which is helpful
fibrosis scar formation - which is not helpful
apicectomy - root canal via the other end - cutting the gums
TB lesion has fibrous lesion , but if it was healing we’d call it healing
wound healing - scope
the process of healing and repair is similar in many tissues
healing is usually described with refence to a smaller skin wound
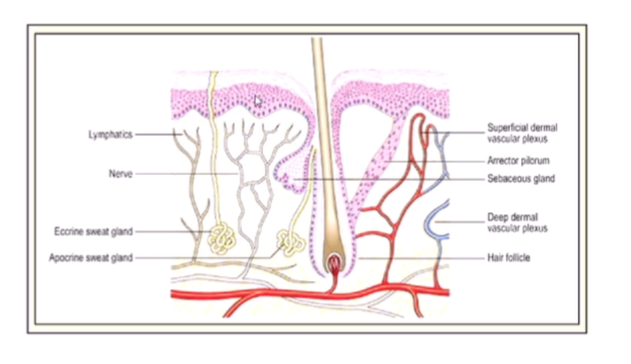
wound healing - skin/mucosa recap
parallels between skin and the mucosa
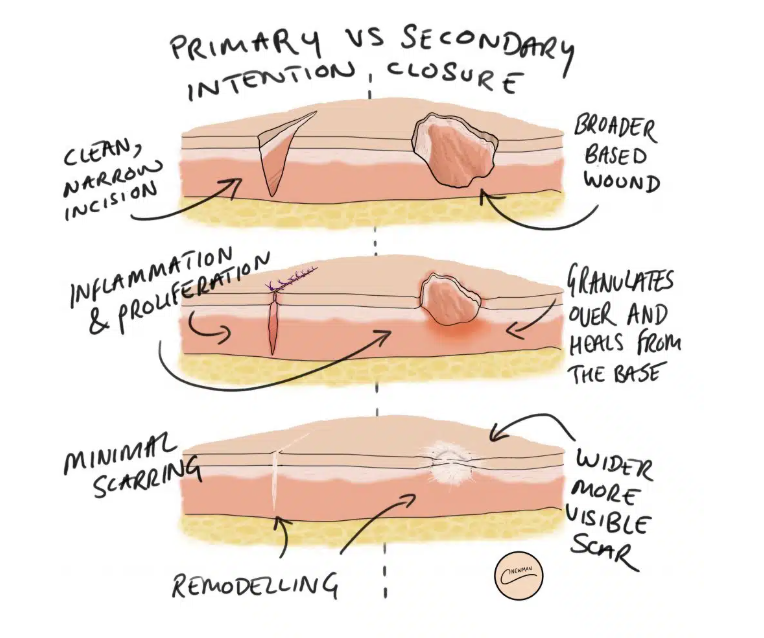
primary vs secondary intention wounds
healing by primary intentions - the wound edges are in close apposition , reepithelization dominates healing
healing by secondary intention - the wound is more extensive and the wound edges are widely separated,
healing by primary intention
reepithelization dominates healing
healing by secondary intention
wound more extensive
granulation tissue covers wound
wound area reduced by contraction of epithelial cells
reepithelization from the wound edges and the residual appendages (hair follicles etc)
Healing of a small skin wound - summary

healing of a small skin wound - 1st hour
connective tissue and epithelium:
Haemostasis
platelet plug formation
fibrin clot formation
Note → Factors which inhibit the formation of the platelet plug and fibrin clot inhibit wound healing. Examples: Asprin; Warfarin; factor VIII deficiency
Healing of a small skin wound - 48 hours
connective tissue and epithelium
inflammation - inflammatory cells migrating into the area and cleaning up the area
macrophage infiltration
debridement - the medical removal of dead, damaged, or infected tissue—such as necrotic tissue, slough, scabs, and foreign bodies—from a wound to promote healing
Healing of a small skin wound - 1 to 3 days
epithelium
Re-epithelialisation
Proliferation of basal epithelial cells adjacent to the wound
Migration of basal epithelial cells across wound-bed under fibrin scab to restore epithelial continuity
Epithelial cells differentiate and stratified squamous structures re-form
Healing of a small skin wound - 2 to 5 days
connective tissue
Granulation tissue formation
endothelial cell and fibroblast proliferation these give rise to new blood vessels
new blood vessels migrate from the wound edges
small blood vessels are accompanied by fibroblasts and inflammatory cells
collagen extra-cellular matrix
what is granulation tissue?
a loose, cellular connective tissue with many plump, synthetic fibroblasts, dilated, irregular blood vessels and inflammatory cells
Healing of a small skin wound - over > 5 days
connective tissue
Maturation → scar becomes less red
decreased cellularity
decreased vascularity
remodelling of collagen matrix
(collagen remodelling involves involves MMP’s 1 and other proteases)
collagen cross linking
1 matrix metalloproteinases

final result due to maturation may take months to fully complete
image - punch biopsy
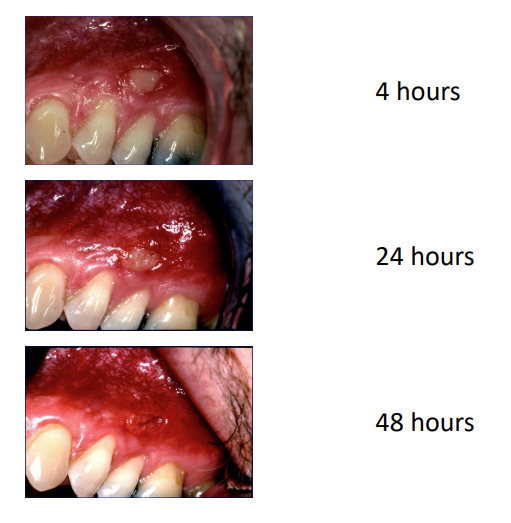
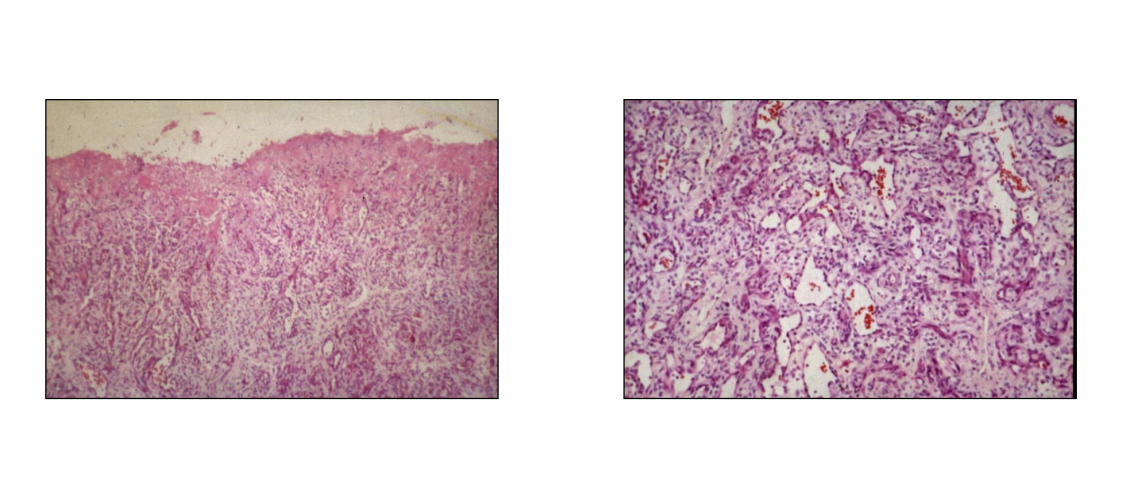
granulation tissue - you can see cellular tissue - irregular dilated spaces - erythrocyte filled
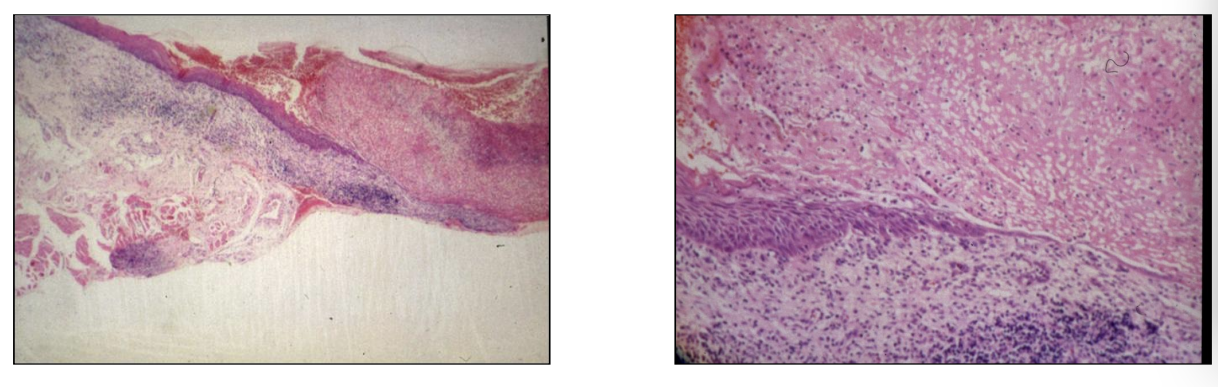
epithelium is proliferating under the scab - over connective tissue bed
WHAT FACTORS ARE IMPORTANT IN CONTROLLING WOUND HEALING ? 3
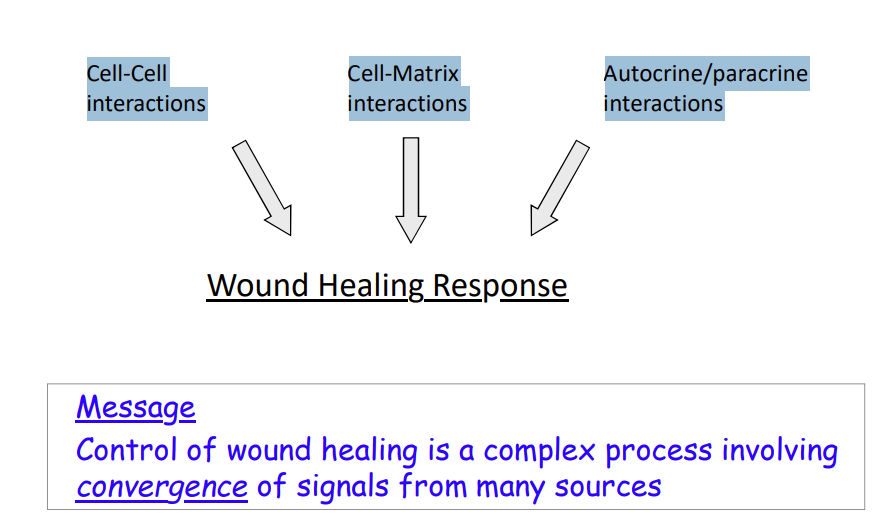
Control of wound healing is a complex process involving convergence of signals from many sources
Cell-Cell interactions
Cell-Matrix interactions
Autocrine/paracrine interactions
redundancy system, - if something doesn’t work, some things may work
macrophages in wound healing - Mononuclear (macrophage precursor) depletion in guinea pigs dramatically impaired wound healing
Traditional functions of the macrophage
Phagocytosis
Protease synthesis
Regulation of immune cell function
macrophages are more than that though, they can produce growth factors, such as…/// these are regulators of other cell processes
Growth factors – FGF a/b – TGF-b – PDGF – VEGF – Other bioactive molecules
see image
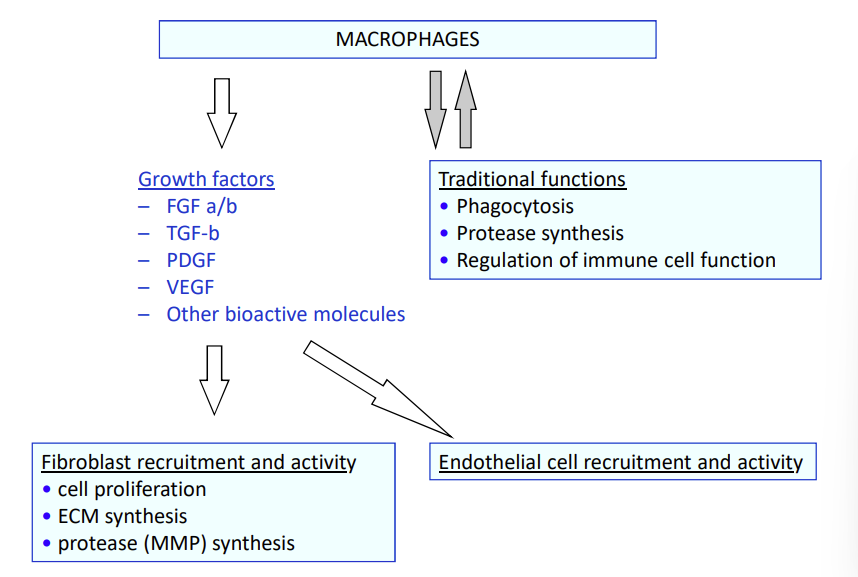
FGF is good for
Fibroblast recruitment and activity
cell proliferation
ECM synthesis
protease (MMP) synthesis
VEGF is good for…
vascular endothelial growth factor
Endothelial cell recruitment and activity
Factors Important in Wound Healing - Local 7
Blood supply - WBCs, nutrients compromised, susceptible to infection
Infection
Persistent irritation
Poor wound stability
Poor apposition of wound edges
Skin wounds: direction of incision -Langers lines - lines of tension
Ionising radiation - radiotherapy - avascular
Factors Important in Wound Healing - Systemic 4
Age - fit elderly people heal well, concurrent elderly ppl with illness → reduced healing
Nutritional status (e.g. protein deficiency; vitamin-C deficiency; scurvy others) MMPs - metal ion cofactors zinc ions
Iatrogenic (e.g. glucocorticoids)
Pre-existing medical conditions (e.g. diabetes)
Complications of Wound Healing 6
Wound dehiscence - breakdown of the wound
Contractures - pattern of wound contraction changes afterwards - problems post surgery
Keloid / hypertrophic scar formation
Weak scars (incisional hernia)
Pigmentation
Neoplastic changes (Marjolins ulcer) - not a feature of oral wounds
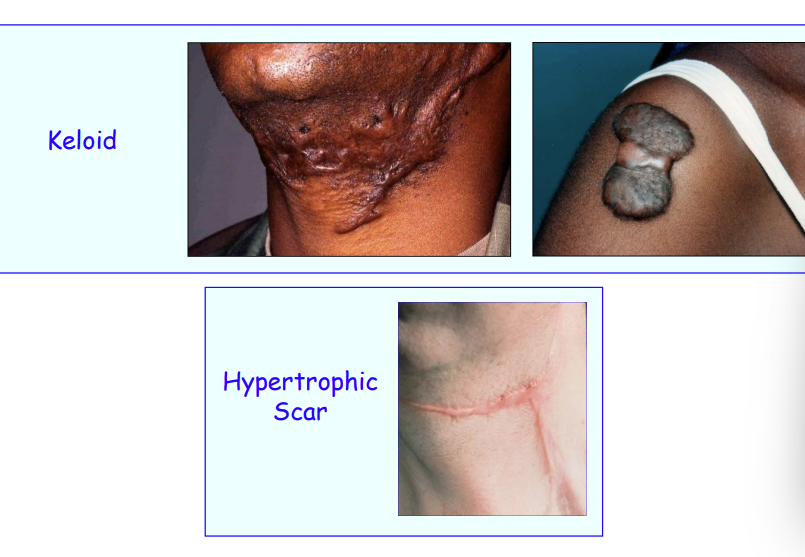
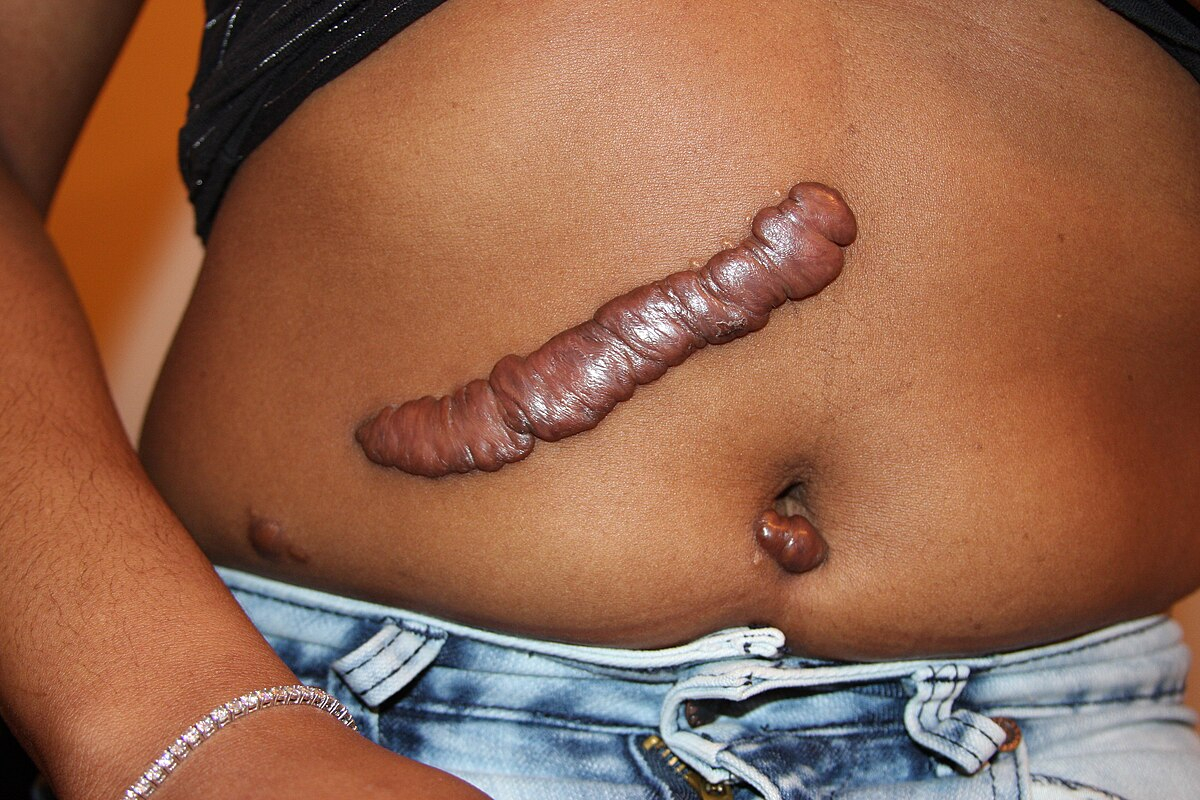
complications of wound healing - keloid
A sharply elevated, progressively enlarging scar characterised by the formation of excessive amounts of collagen in the dermis during connective tissue repair.
It may spread beyond the margins of the original wound
Characteristically found in Afro-Carribean populations
Seen on the face but does not affect the oral mucosa
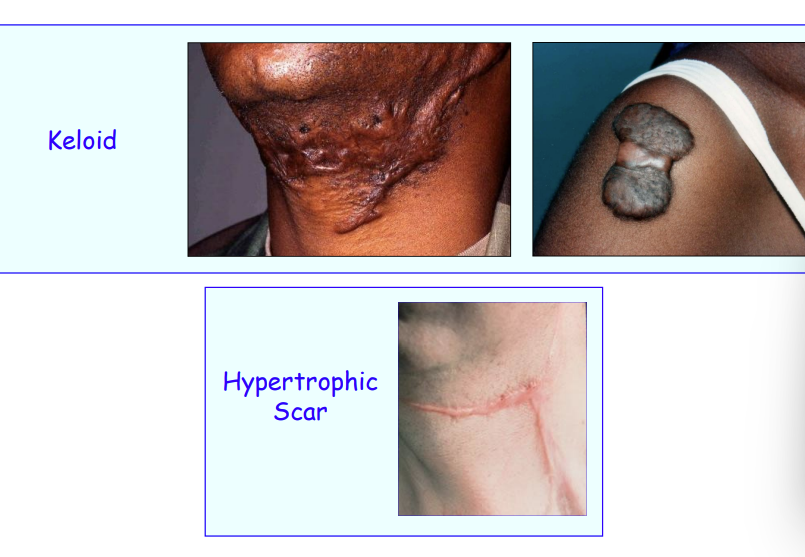
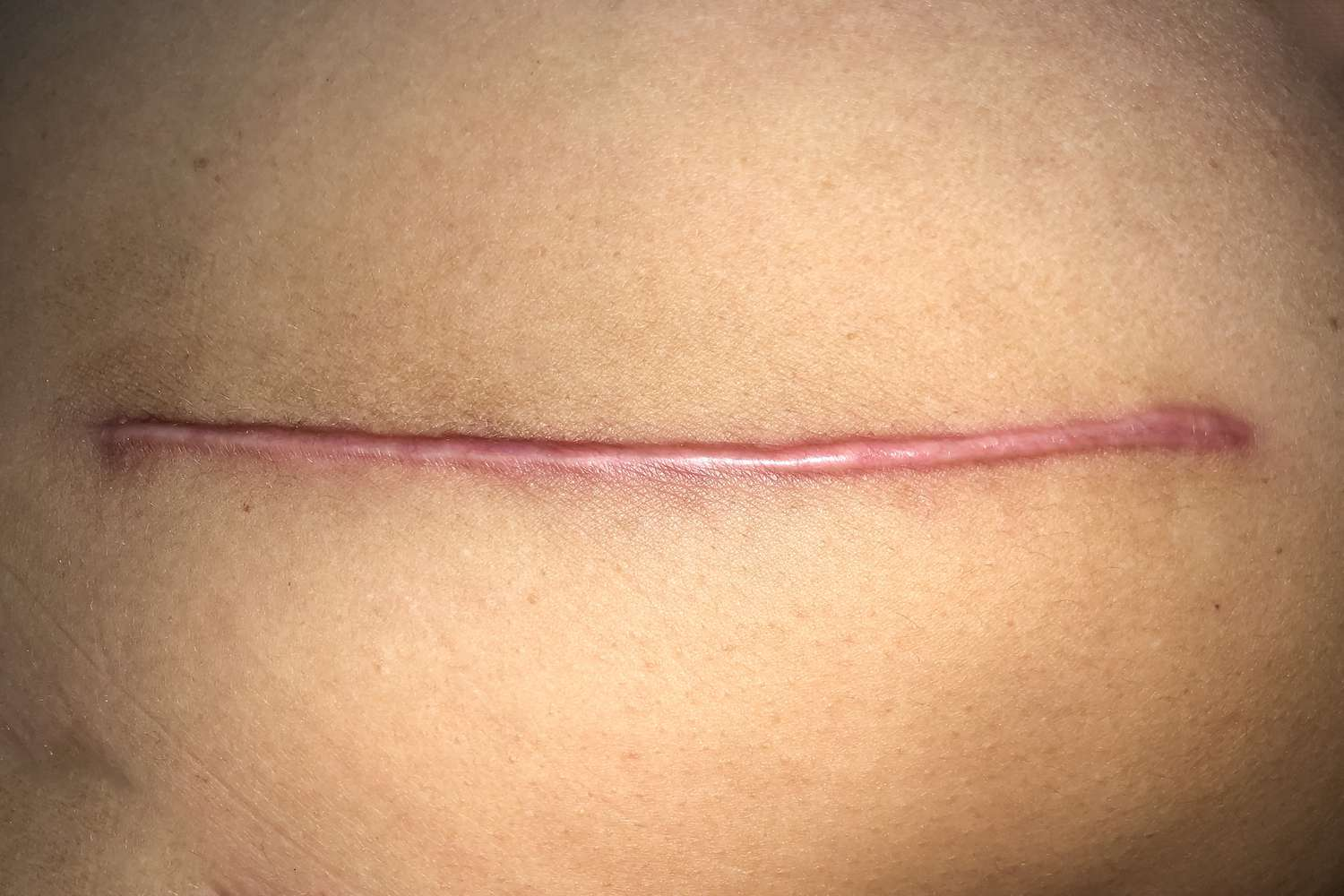
complications from wound healing - hypertrophic scar formation
Similar to keloid but does not spread beyond the wound margins
Will affect varied population groups
Seen on the face but does not affect the oral mucosa
Situations of special relevance to us
Embryonic wound healing - early/midgestational wounds heal without scarring. however, this is not understood, perhaps because the immune system is not fully formed. Intrauterine surgeries for cleft lip/palate??
Oral mucosal wound healing - there is scarring, but less of an issue in the skin, no keloid/hypertrophic scarring. unknown reason why, nature of inflammatory response?