Anaemia and Bone Marrow Overview - Week 8
1/133
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
134 Terms
Anaemia
Condition characterized by insufficient red blood cells.
Erythropoietin (EPO)
Hormone controlling red blood cell production. Produced primarily in kidney by Type-1 fibroblastoid cells and partially in liver. Stimulates Erythropoiesis and reduces apoptosis.
Primary site for RBC production
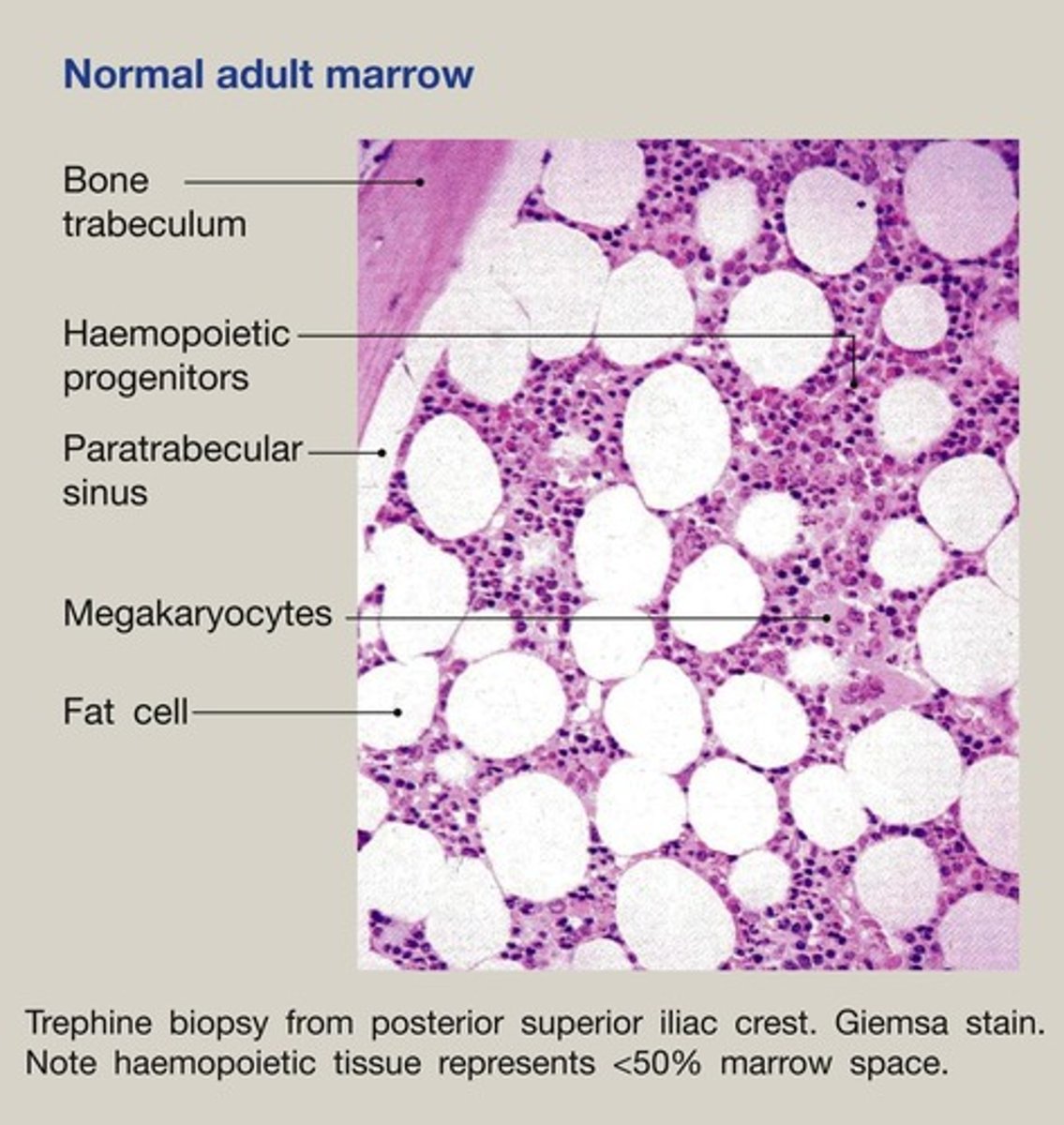
Bone Marrow
Vitamin B12
Essential for red blood cell formation and DNA synthesis
Folate
Vitamin crucial for DNA synthesis in cells.
Haematocrit
Percentage of blood volume occupied by red cells.
Spherocytes
Abnormal red blood cells lacking a pale center.
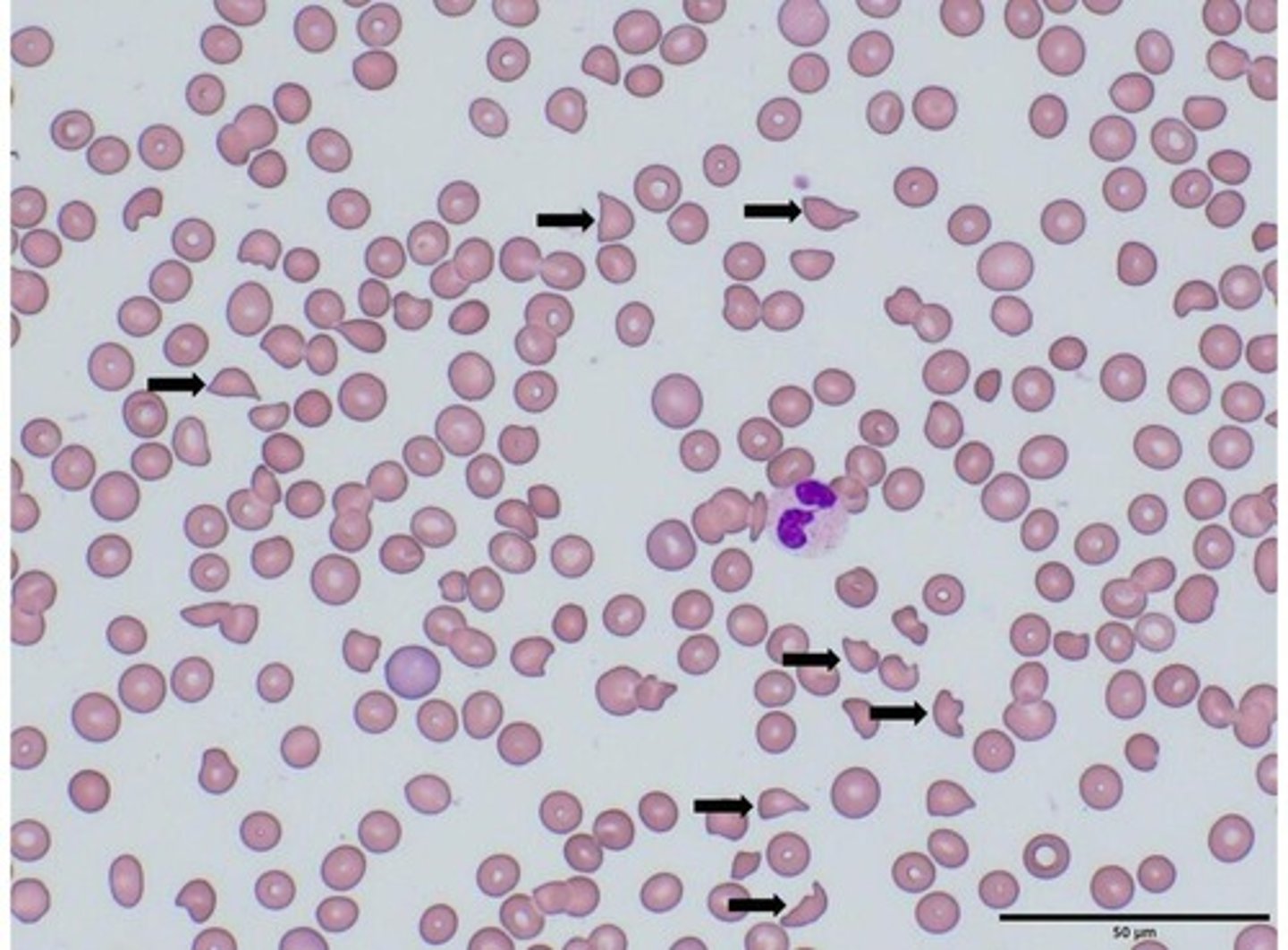
Schistocytes
Fragmented red blood cells indicating damage.
Granulocytes
Type of white blood cells with granules.
Lymphocytes
White blood cells crucial for immune response.
Thrombocytes
Another term for platelets, involved in clotting.
Chronic Anaemia
Long-term condition with compensatory erythropoietin production.
MCV
Mean corpuscular volume, measures red cell size.
Microcytic: <80 fL, Normocytic: 80-100 fL, Macrocytic: >100 fL.
MCHC
Mean corpuscular hemoglobin concentration, measures hemoglobin per cell.
RDW
Red cell distribution width, indicates size variation.
Sickle Cells
Abnormal red blood cells in sickle cell anemia.
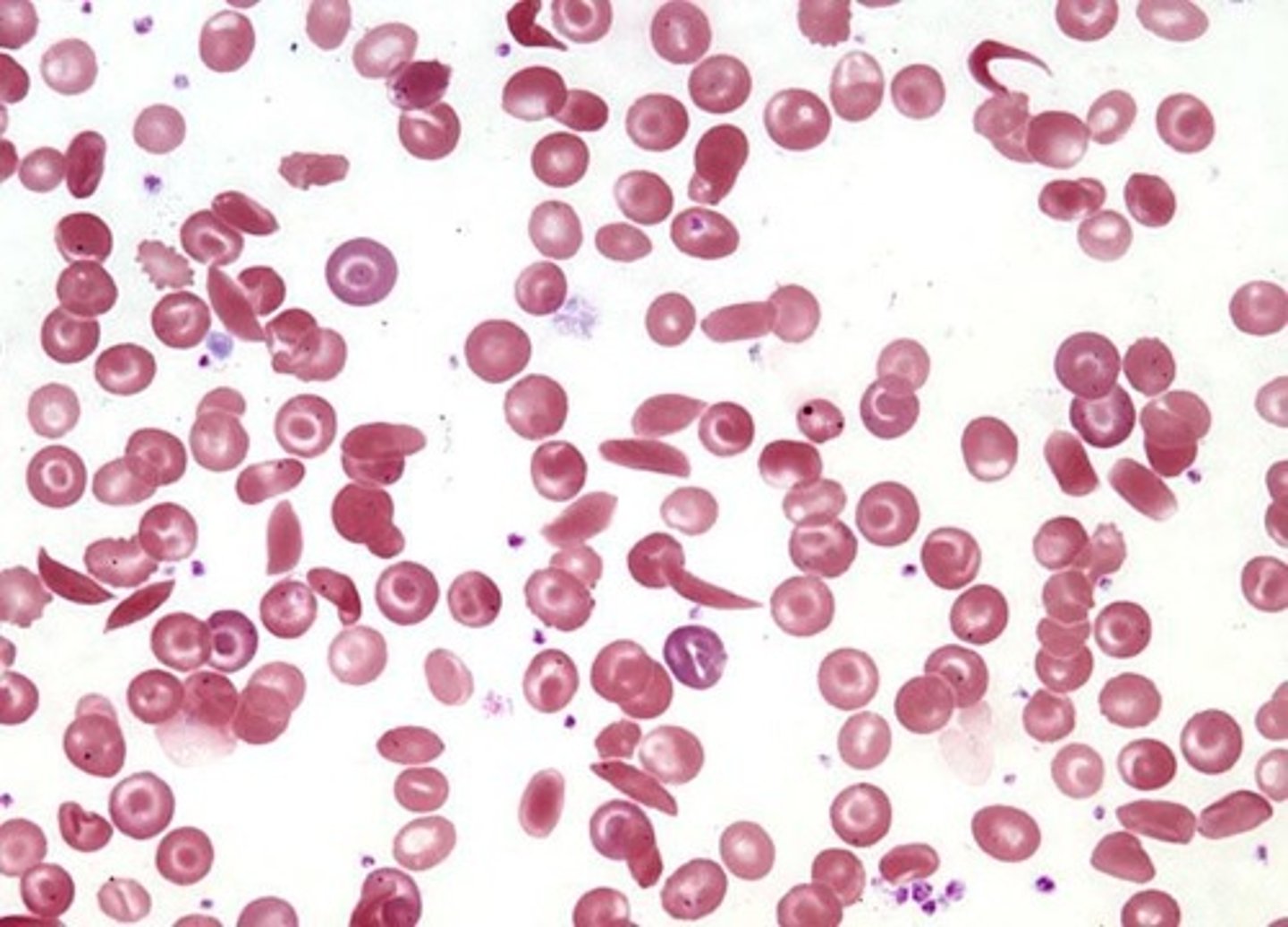
Target Cells
Red blood cells with a bull's-eye appearance.
Howell-Jolly Bodies
Nuclear remnants in red blood cells.
Bite Cells
Red blood cells with membrane loss.
Agranulocytes
Leukocytes without granules in cytoplasm.
B-cells
Lymphocytes that produce antibodies.
T-Cells
Lymphocytes that regulate immune responses.
Natural Killer Cells
Lymphocytes that attack infected or cancerous cells.
Haematopoietic Stem Cells
Stem cells that differentiate into blood cell types.
Common Myeloid Progenitor
Gives rise to various blood cell lineages.
Common Lymphoid Progenitor
Gives rise to lymphocytes and NK cells.
Erythrocytes
Red blood cells, derived from myeloid progenitors.
Megakaryocytes
Precursor cells that produce platelets.
Extramedullary Haematopoiesis
Blood cell production outside bone marrow.
Bone Marrow Stroma
Supportive tissue for blood cell development.
Erythropoiesis
Process of red blood cell development.
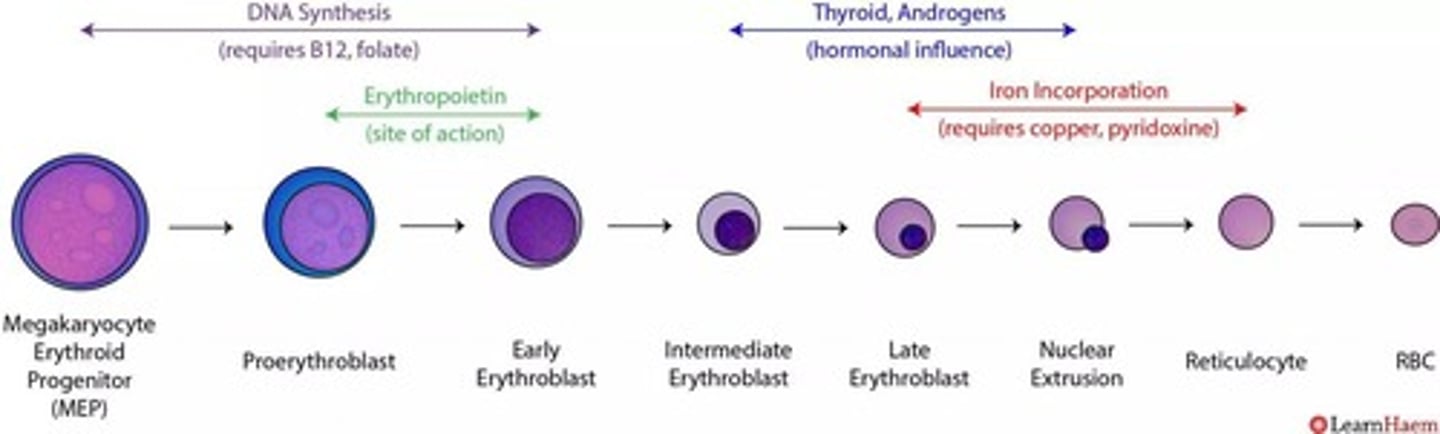
Duration of Haematopoiesis
Takes approximately 7 days for blood cell formation.
Increased Hb
More eosinophilic hemoglobin in erythrocytes.
Nuclear extrusion
Nucleus is expelled during erythroblast stage.
Organelle loss
Mitochondria are lost in erythrocyte maturation.
RBC cell size over time
Erythrocytes decrease in size during maturation.
Myeloid stem cell
Precursor cell for erythrocyte lineage.
Megakaryocyte-erythroid precursor
Common precursor for platelets and erythrocytes.
BFU-E
Burst-forming unit; develops EPO receptors.
CFU-E
Colony-forming unit; dependent on EPO.
Pro-erythroblast
Initial stage before erythroblast formation.
Erythroblast
Normoblast; stops dividing, nucleus extruded.
Erythrocyte destruction
Occurs mainly in the spleen.
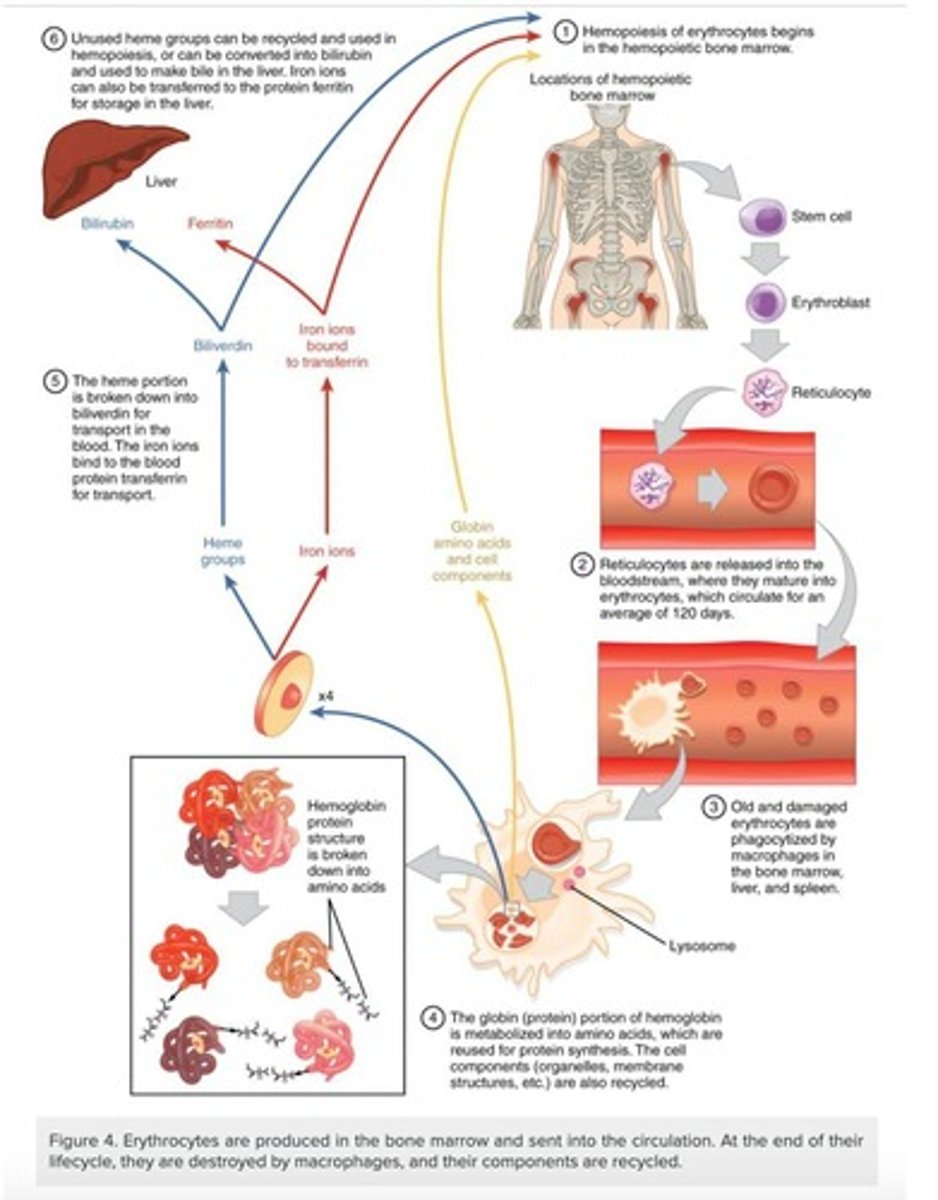
RBC lifespan
Approximately 120 days before destruction.
Phagocytosis of RBC
Macrophages engulf old RBCs for breakdown.
Bilirubin
Product of heme breakdown, excreted.
Colony Stimulating Factors
Cytokines promoting blood cell production.
Iron requirements
Men need 8 mg, women 18 mg.
Iron Absorption Process
Involves heme dissociation and transporter HCP1.
Heme Iron
Iron from hemoglobin, absorbed in the duodenum.
Inorganic Iron Forms
Includes ferrous (Fe2+) and ferric (Fe3+) iron.
Ferrireductase Enzyme
Converts ferric iron to ferrous form in duodenum.
DMT1 Transporter
Transports ferrous iron into enterocytes.
Ferroportin
Transporter that releases iron from enterocytes.
Hepcidin Function
Regulates iron levels by degrading ferroportin.
Transferrin
Protein that transports ferric iron in plasma.
Iron Storage Forms
Stored as ferritin (soluble) or haemosiderin (insoluble).
Vitamin B12 Sources
Found in meat, liver, fish, and dairy.
Vitamin B12 Requirement
Minimum adult requirement is 2ug/day.
Intrinsic Factor
Protein necessary for B12 absorption in ileum.
Methionine Synthase
Enzyme requiring B12 for DNA synthesis pathway.
Methylmalonyl CoA Conversion
B12 converts it to succinyl CoA, a TCA intermediate.
Vitamin B12 Deficiency Causes
Includes vegan diet and malabsorptive conditions.
Folate Sources
Found in greens, liver, and yeast.
Folate Absorption
Occurs in duodenum and jejunum as 5-methyl THF.
Folate Function
Essential for purine DNA precursor synthesis.
Folate Deficiency Causes
Includes nutritional reasons and malabsorptive conditions.
B12 Deficiency
Causes neurological symptoms via methylmalonyl-CoA buildup.
Ineffective Erythropoiesis
Qualitative defect in red blood cell production.
Megaloblastic Anaemia
Caused by low B12 or folate levels.
Thalassaemia
Genetic disorder affecting hemoglobin production.
Sideroblastic Anaemia
Ineffective erythropoiesis due to iron metabolism issues.
Myelodysplastic Syndrome
Disorder caused by poorly formed or dysfunctional blood cells.
Insufficient Erythropoiesis
Quantitative lack of erythrocyte precursors.
Renal Failure
Leads to decreased erythropoietin production.
Iron Deficiency
Common cause of insufficient red blood cell production.
Anaemia of Chronic Disease
Associated with chronic inflammatory conditions.
Aplastic Anaemia
Failure of blood cell production in bone marrow.
Bone Marrow Replacement
Displacement of normal marrow by abnormal cells.
Haemorrhage
Loss of blood leading to decreased RBCs.
Haemolysis
Destruction of red blood cells.
Intravascular Haemolysis
Destruction of RBCs within blood vessels.
Extravascular Haemolysis
Destruction of RBCs in the spleen.
Koilonychia
Thin, spoon-shaped nails associated with anaemia.
Angular Stomatitis
Ulcers at the edges of the lips.
Atrophic Glossitis
Smooth, inflamed tongue due to anaemia.
Compensatory Mechanisms
Body's response to maintain oxygen delivery during anaemia.
Chronic Anaemia Symptoms
Includes pallor, fatigue, dyspnoea, and tachycardia.
2,3-Diphosphoglycerate (2,3 DPG)
Regulatory molecule enhancing oxygen release from hemoglobin.
O2 extraction
Increased oxygen uptake by tissues from hemoglobin.
HbO2 curve shift
Rightward shift indicates decreased hemoglobin affinity for O2.
Cardiac Output (CO)
Volume of blood pumped by heart per minute.
Afterload
Resistance the heart must overcome to eject blood.
Vasodilatation
Widening of blood vessels, reducing vascular resistance.
HIF-1
Oxygen sensor regulating EPO production in kidneys.
Hydroxylation
Chemical modification affecting HIF-1 stability.
Ubiquitination
Process marking proteins for degradation.
Bone marrow suppression
Reduced production of blood cells in the marrow.
O2 dissociation from Hb
Release of oxygen from hemoglobin to tissues.
Hb
Measure of haemoglobin concentration in blood.