5: ciliary body , aq humour & IOP(copy)
1/69
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
70 Terms
ciliary body
when viewed from the nterior eye, the ciliary body is a ring shaped structure
posterior area of ciliary body which terminates at the ora serrata, appears flat but anterior has lots of foolds that extends into the posterior chamber
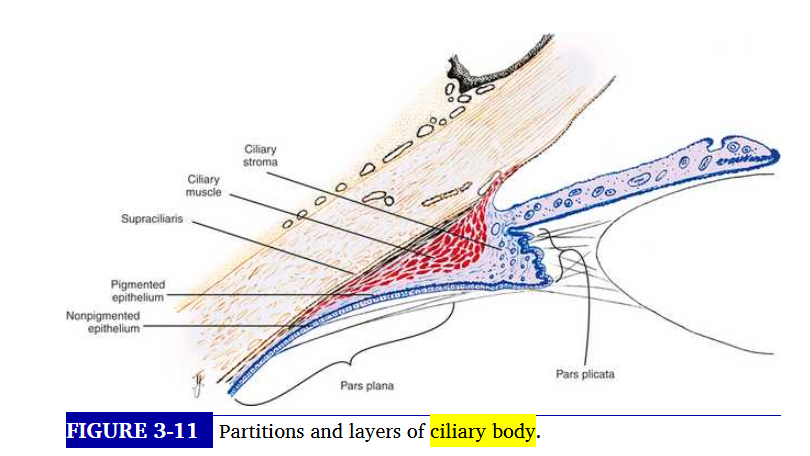
sagittal section of ciliary body
ciliary body has triangular shap
one corner lies at the scleral supr, the iris root extends from centre of base
outer side of triangle lies against the sclera and inner side lines the posterior chamber ad a small part of vitreous
apex located at ora serrata
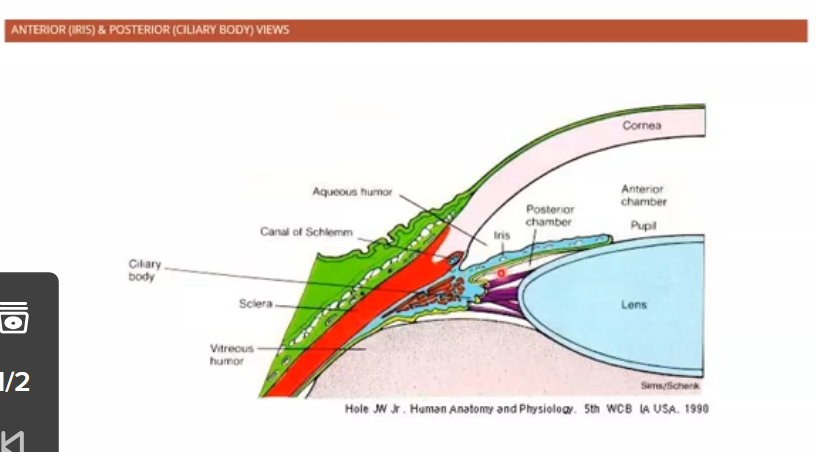
ciliary body is the light blue part
traingular as looking at one slice of it
it makes the aqueous humour that keeps the eye round and gives nourishment
passageway of aqueous humour
produced by non pigmented ciliary epithelium of ciliary processes
comes from posterior chamber to the pupil
pupil to theanterior chamber and the aqueous circulates:
warm iris → cool cornea → sets up convective current
then from anterior chamber angle it passes through trabecular meshwork and enters the schlemms canal
enters the episcleral veins or uveoscleral outlfow to to the supachoroidal space
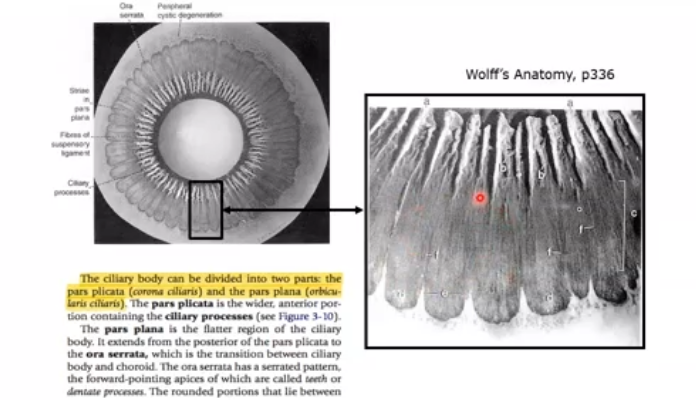
posterior view of ciliary body
pars plana is flatter
plicata are the ciliry processes that allow constricion of eye
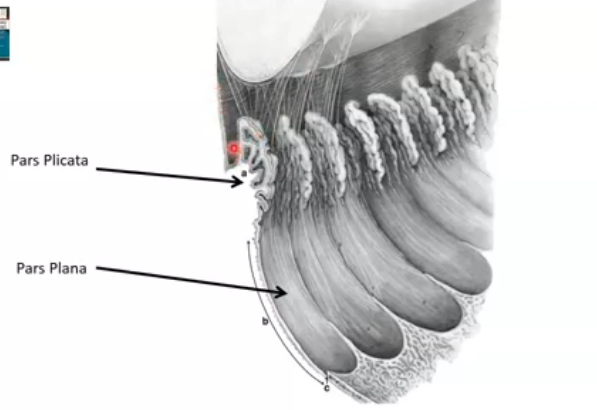
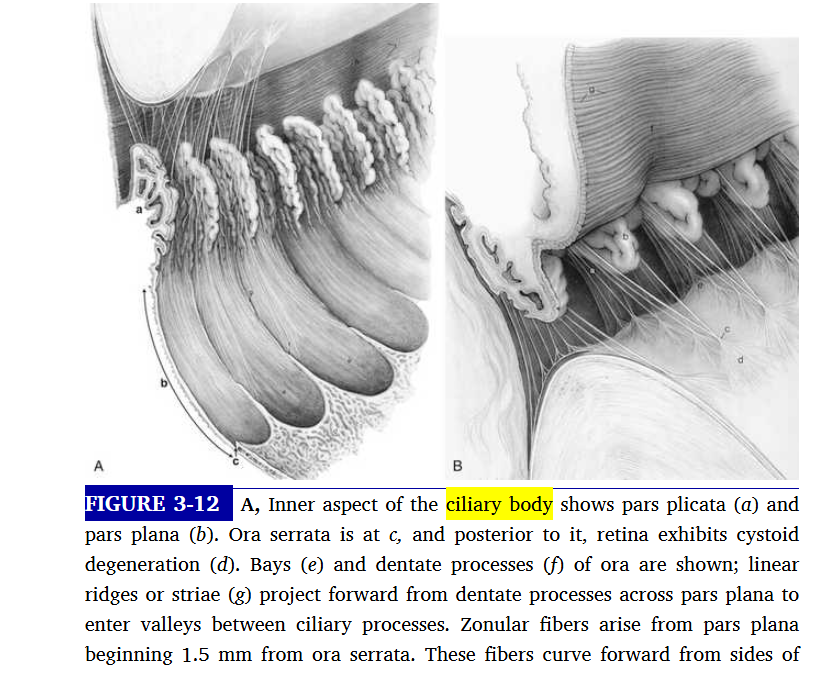
what is the ciliary body divided into
pars plicata
pars plana

pars plicata
wider , anterior portion containing ciliary processes
cilliary processes extend into posterior chamber and the regions between them are called valleys of kuhnt
pars plana
flatter region of the ciliary body, extends from the posterior [art of the pars plicata to the ora serrata, which is the transition between ciliary body and choroid
ora serrata has serrated pattern,called teeth, and rounded portions that lie between teeth are oral bays
dentate processes
elongations of retinal tissue into the region of the pars plana
what fibres course from the cilary body
zonule fibres course from ciliary body to the lens. some of these fibres instert into the internal limiting membrane of pars plana region and travel forward through valleys between ciliary processes
what is ciliary body attached to
vitreous base, which extends forward over the posterior pars plana
ciliary muscles
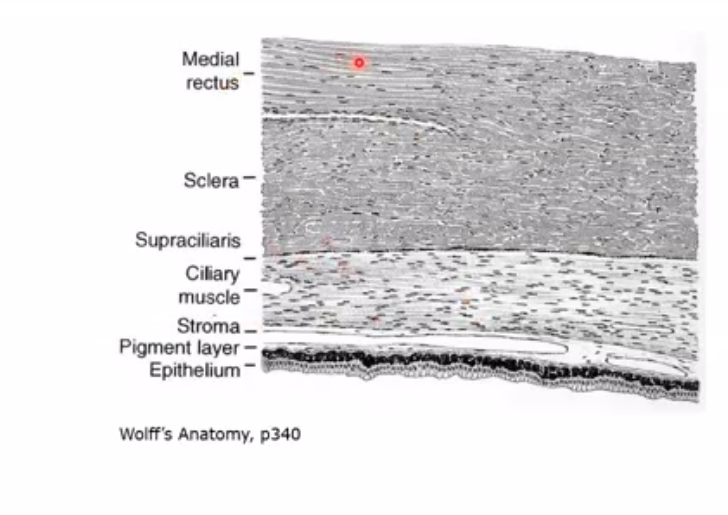
light section on picture on right is stroma
black outline is pigmented epithelium
shaded area around black line is non pigmented epithelium
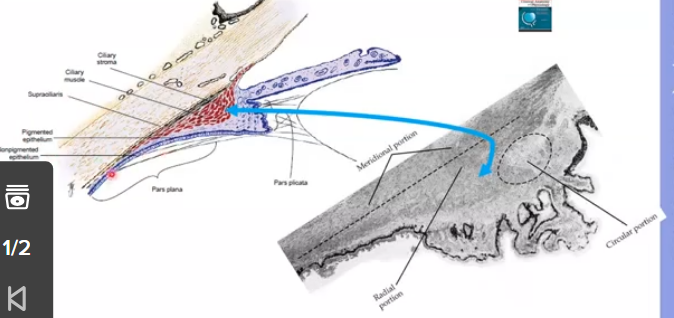
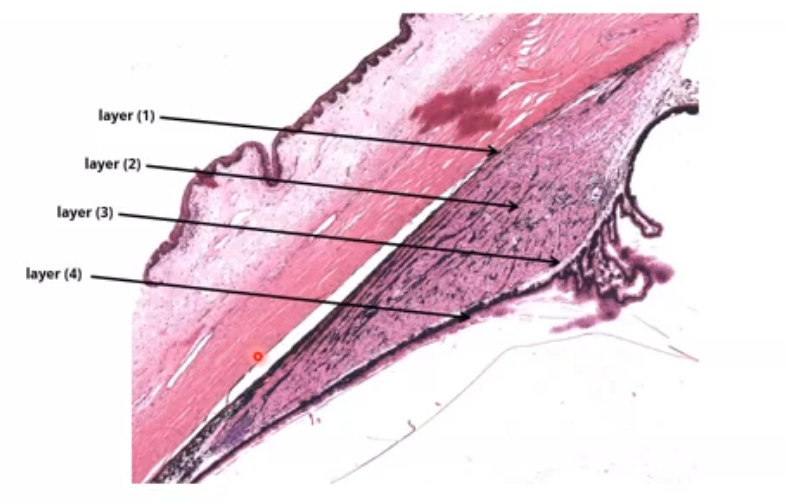
layers of the ciliary body
1.supraciliary layer - outermost
2.ciliary muscle
3.stroma
4.epithelial layers: outer basement membrane, pigmented epithelium, non pigmented epithelium, inner basement membrane
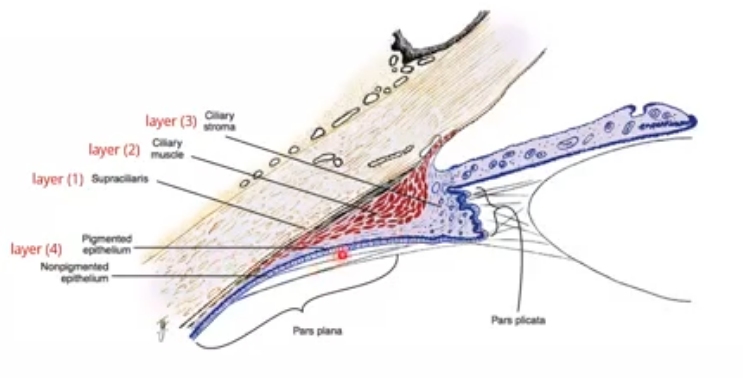
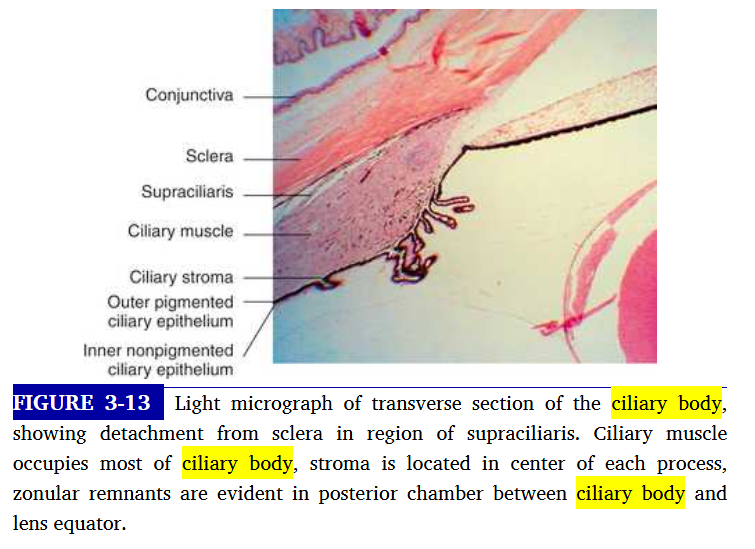
supraciliaris layer of ciliary body
outermost layer of ciliary body adjacent to sclera.
loose connective tissue arranged in ribbonlike layers containing pigmented melanocytes, fibroblasts and collagen bands
arrangement allows ciliary boody to slide against the sclera without detaching from or stretching the tissue
arrangement also allows accumulation of fluid within its spaces which may cause displacement of ciliary body from sclera.
damage to this laye caused by trauma may result in ciliary body detachment
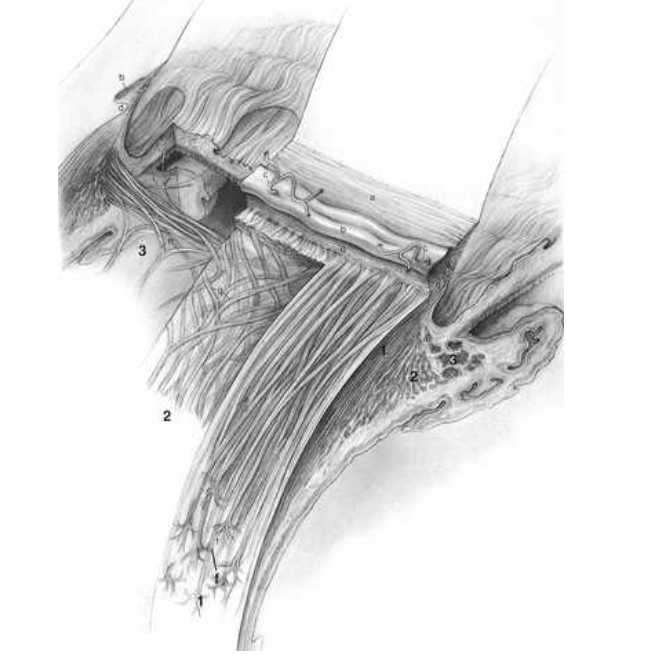
ciliary muscle
smooth muscle tissue
function is controlling accomodation
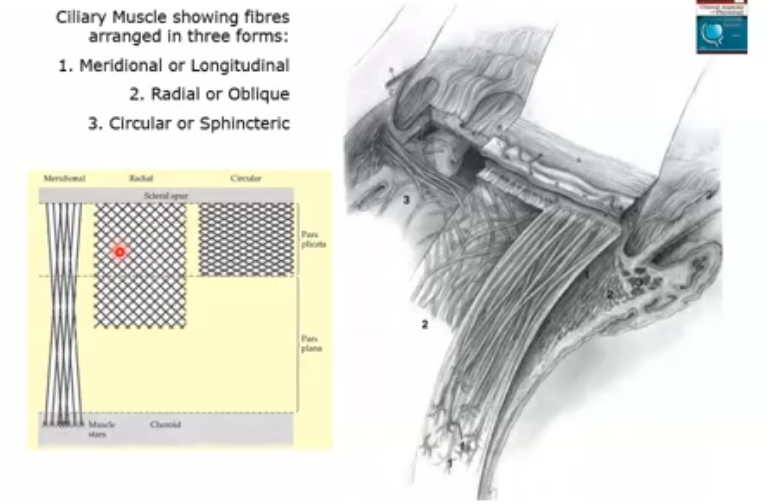
long radial and circular directions
longitudinal muscle fibres lie adjacent to supraciliaris and parallel to sclera
radial fibres form wider shorter Vsthat originate at the scleral spur and insert into connective tissue near base of ciliary proceses
innermost region of ciliary muscle , annular muscle is formed of cicular muscle bundles with a sphincter type of action. located near major circle of iris .

what is ciliary muscle innervated by
autonomic nervous system. parasympathetic stimulation activates muscle for contraction whereas sympatheic innervation has inhibitory effect that is a function of level of parasymp activity
ciliary stroma
connective loose tissue
function is supporting framework for muscle and blood vessels
lies between muscle and epithelial layers and forms the core of each of the ciliary processes
separated bundles of ciliary muscle
stroma thins in pars plana where it continues as choroidal stroma
major arterial circle of iris
located in the ciliary stroma to ciliary muscle and near the iris root
ciliary epithelium
2 layers of epitheliumpositioned apex to apex , cover the ciliary bpdy and line psterior chamger and part of vitreous chamber
intercellular junctions, desmosomes and tight junctions connect the two layers
gap junctions between apical surfaces provide a mans of cellular communication between the layers and are important in formatin of aqueous
both layers involved in secretion
outer layer of the ciliary epithelium
pigmented and cuboidal and simple
function is light absorption in posterior cavity
cells joined by desmosomes and gap junctions
anteriorly, its continous with ant iris epithelium
posteriorly, its continours with retil pigment epithelium to stroma
basement membrane attaches pigment epithelium to the stroma
unpigmented simple epithelium of ciliary
composed of columnar cells in the pars plana and cuboidal in the pars plicata
lateral walls of the cells contain extensive interdigitations and are joined, near their apices by desmosomes , gap junctions and zonula occludens whcih form one sitte of blood aqueous barrier
function is secretion of aq humour,and serve as a barrier between blood and aqueous
metabolically active, have large number of mitochondria than pigmented cellls and thus a higher degree fof metabolic activity
baswment membrane of non pigmented epithelium
line posterior chamber and extends into invaginations and is continous wih internal limiting membrane of reitna
what is the attachment site for zonular fibres fibres
the internal limiting membrane also the attachment for fibres of the vitrous base
structure in the pars plana
looking at the left eye
ciliary muscle organisation
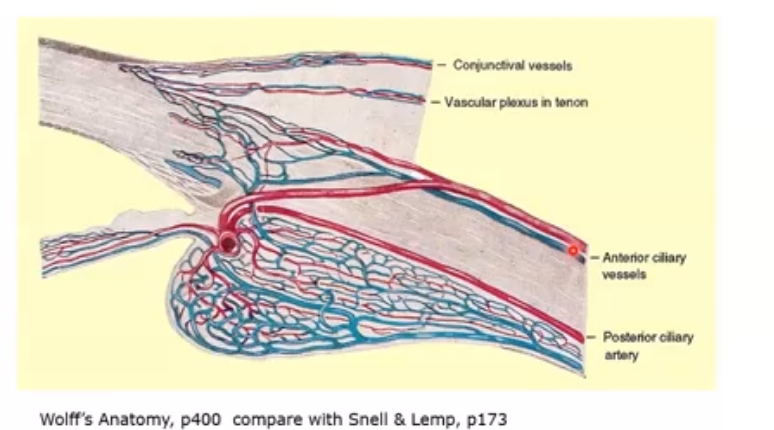
blood vessels of the anterior eye
major circle of iris supplies blood to the iris
then the capillaires go into the ciliary body
those then secrete liquids into the pigmented and non pigmnted epithelium
then secrete through pupil, and anterior chamber it exits out canal of schlemm
canall connected to anterior ciliary artery os goes through here
exits out the anterior ciliary vein
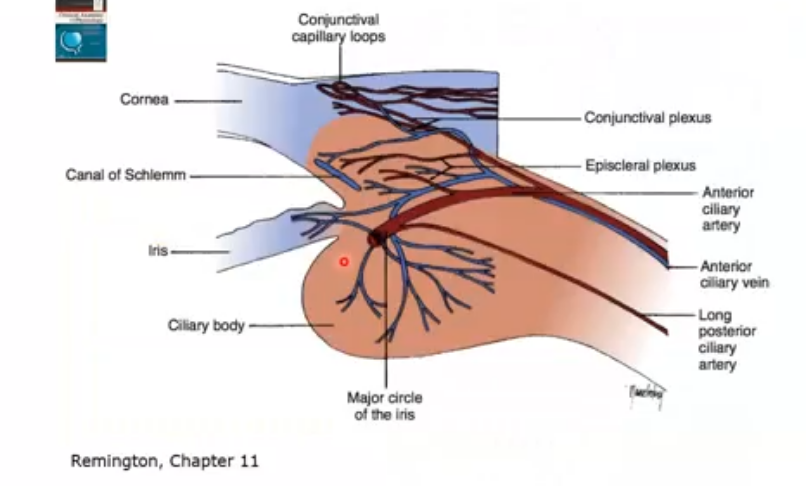
ciliary body- structure of the ciliary processes
ciliary processes are lined by 2 layers of epithelium: outer pigmented and inner pigmented
lots of folds to increase surface area
outer surface will have un pigmented cells
what are ciliary processes
folds or ridges on the inner surface of ciliary body, arranged in crcular pattern behind the iris
inside posterior chamber
each process has a core of connective tissue and capillaries covered by 2 layers of epithelium; pigmentated and no pigmented
produces aq humour
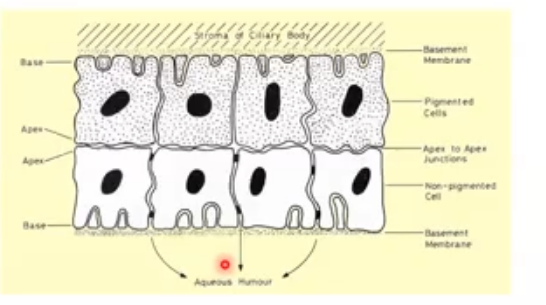
how is aqueous humour produced
produced from blood in the capillaries of the ciliary processes and transported to anterior chamber via the ciliary epithelium
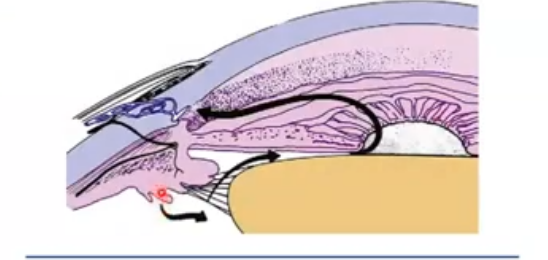
flow of aqueous humour
aq is formed in ciliary processes, moves out around the crystalline lens and through pupil, and flows out of anterior chamber through trabecular meshwork into the schlemms canal and then to episcleral veins
what is trabecular meshwork
encircles the circumference of anterior chamber occupying most of the inner aspect of the internal scleral sulcus. cross section- has a triangular shape
flattened perforated sheets
open latticework with branches interlacing
canal of schlemm
circular vessel and a venous channel
contains aq humor rather than blood
tight junctions of the inner wall restrict blood flow into the canal between the lateral walls of the cells
what is the unconventional outflow of aqueous
an an=venue by which aqueuous exits the anterior chamber
passes through spaces within the uveal meshwork
fluid then passes into the connective tissue spaces surrounding ciliary muscle bundles , moves into suprachoroidal space and absorbed into and through the sclera
where does remainder of aq follow: conventional outflow pathway
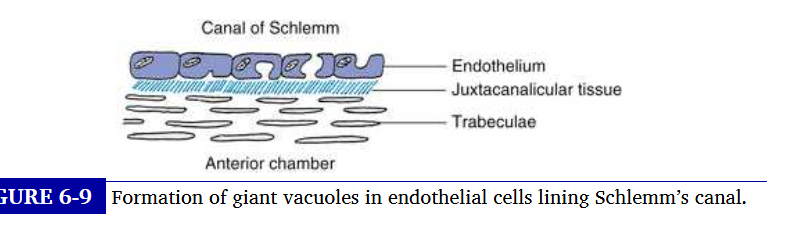
moves through the meshwork and into the narrower pores of the corneascleral meshwork and through the juxtacanicular tissue and the endothelial lining into schlemms canal
internal wall of schlemms canal
contains number of evaginatinos or blind pouches that extend into the juxtacanicular tissue toward the meshwork
these internal collector channels can be long and branching, and serve to increase surface area of canal
endothelial cells lining external wall of schelmms canal
the endothelial cells lining wall are joined by zonula occludens and contain no vacuoles
external collector channels re distributed around outer wall of schlemms canal and branch from it to empty into either deep scleral plexus or intrascelral plexus ov veins . which in turn drain into episcleral veins
what 3 mechanims contriute to production and secretion of aqueous humor
diffusion, ultrafilteration and active secretion
diffusion
passive
movement from high to low concentration
small molecules like h20, 02 and c02 can diffuse across membrane
lipid soluble substances ie cell membrane
ultrafilteration
passive
movement from high to low pressure
involves hydrostatic pressure
secretion
active
high energy bod (ATP) and diffusing it into ADP, and producing energy
energy used to secrete something
non depenent on the concentration gradient
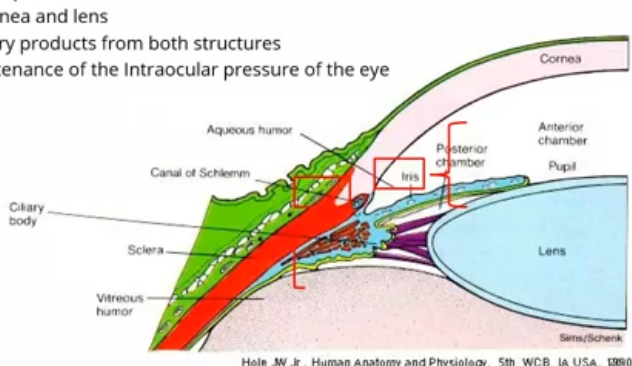
what is aqueous humor
a clear fluid in anterior and posterior chamber of eye
produced by eptihelial cells of ciliary body
provifed nutrition to cornea and lens
removes excretory products from both structures
conributes to maintenance of the intraocular pressure of the eye
structure of cell membrane
lipids form most of surface area and about 425 i wieght. generally hydrophobic
proteins account for 55% of weight, many functions like anchoring and transport of substances by channel or carrier activity
carbohydrates account for 3% of weight - functions include lubrication and protection, anchoring and locomotion
hydrophobic tails and hydrophillic heads - lipid bilayer
cholesterol moelcules in cell membrane
found in the central fatty acid portion decrease the membranes permeability to water soluble molecules
lysosomes in cell membrane
digestiive systems containing enzymes take up bacteria and break down into molecules that are reused or reabsorbed into the cytoplasm to be transported to cell membrane and out of the cell
channel proteins
create water filled passages linking the intracellular and extracellular spaces
facillitate ion movement across lipid bilayer and move ions
carrier proteins in facillitated diffusion
carrier proteins bind to substrates that they carry across the membrane , molecule slike glucose and amino acids move through this way
osmosis
aqueous humor is mostly water so most of water moves across ciliary eptihelium via osmosis
goes from low to high concentration volume of water
net diffusion of water
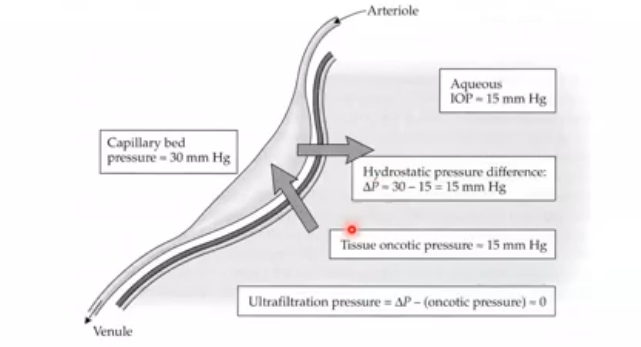
ultrafilteration- pressure
high to low pressure
net effect is that ultrafilteration plays little part in production of aq humor
pressure in capillaries of ciliary body is offset by oncotic pressure in tissue of ciliary processes which result from protein leakage through fenestrated capillaries
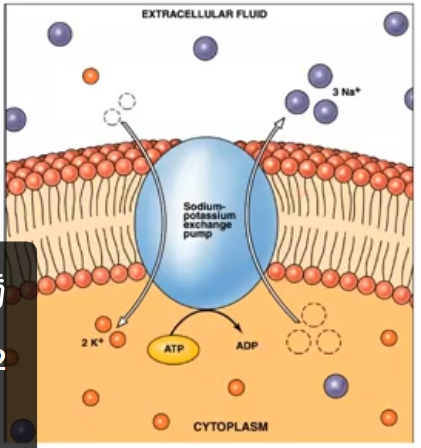
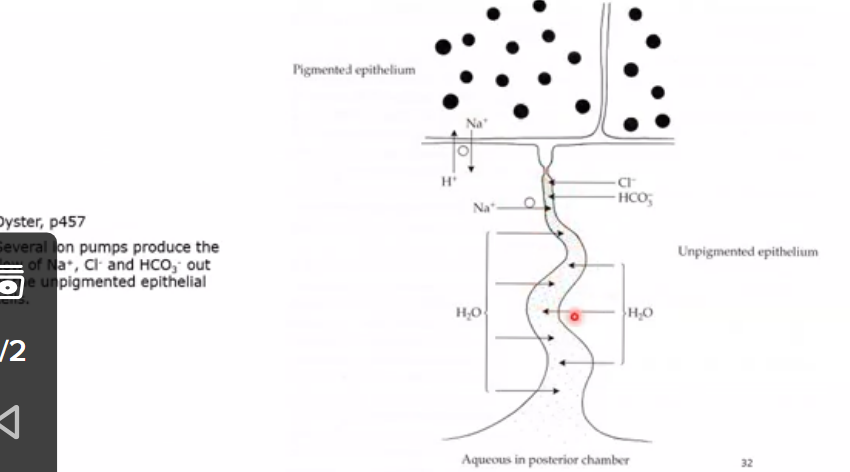
secretion by active transport
done through sodium potassium exchange pump
sodium-potassium activated ATPase is an enzyme in the cell membrane
role is to break down ATP to ADP releasing phosphate which supplies energy for sodium potassium exchange
mechanism exchanges 3 intracellular Na ions in the ciliary epithelium for 2 extracellular K ions
the 3 positive charges leave making inside more negative
net movement of sodium ions to posterior chamber produces a conc gradient which causes water to flow into the chamber by osmosis
water drawn out of cell and into tight junction area that is then released.
what is iop
intraocular pressure is the fluid pressure inside the eye
prodcution of aqueous humor
drainage of the fluid through trabecular meshwork
supports refractive structures and intraocular contents
nutrients to avascular structures
IOP relies on what?
Relies on the balance between the secretion of aq humor from ciliary body and the outflow resistance in the trabecular meshwork
angle structures
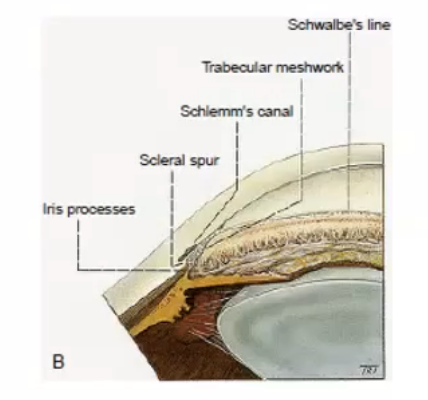
what is the health range of IOP
11-21mmHg
the eye requires a constant volume of aqueous to be present in the eye to give a constant pressure
production=outflow
IOP errors
increased outflow= low IOP : retinal detachment/ odema risk
normal outflow- rasied IOP= raised IOP : rare cause of glaucoma
production> outflow- raised IOP : glaucoma
increased outflow of fluid = lower IOP
means the aqueous humor is draining faster than normal through the eyes drinage pathways
eye is losinf fluid faster than its being produced, reducing the pressure inside the eye
decreases stress on the optic nerve
can cause blurred vison, corneal swelling and retinal problems
decrease in outflow
fluid inside the eye isnt draining properly, whilst aq is still being produced
fluid accumulates which raises IOP
puts stress on optic nerve which can lead to glaucoma
can be due to blocked trabecular meshwork
closure of the angle between cornea and iris
how is IOP measured
measured using tonometry
goldmann machine
or pulsair which is non contact tonometry
what is IOP affected by
balance of secretion and drainage of aqueous fluid
produced by ciliary body at 2-3 microlitres per minute
drains through tabecular meshwokr or via uveoscleral route
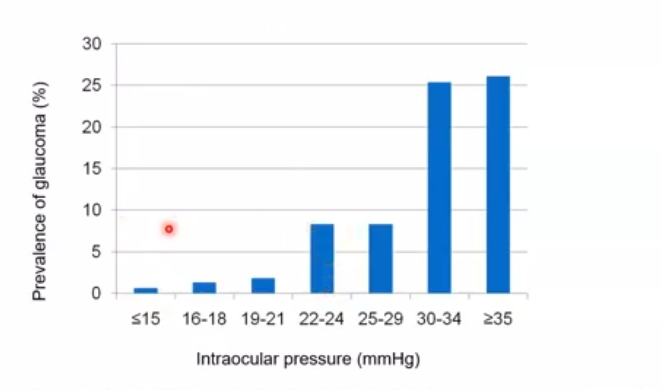
variations of IOP
iop can change every day
its highest in the morning and lowest at night
average ocular pressure barely changes throughout life
important systemic factors of IOP
systolic blood pressure
diabetes
BMI
ethnicity in factors affecting iop
higher mean in poeple of african descent
increased age increment
also have thinner corneas
lower mean in poeple of east african descent
iop shown to decrease with age
family history in factors affecting iop
higher iop with a family history of OHT or glaucoma
artefactual changes affecting iop
depends of pulse
standing lower than reclining; if lying down it increases
after immersing hand in cold water
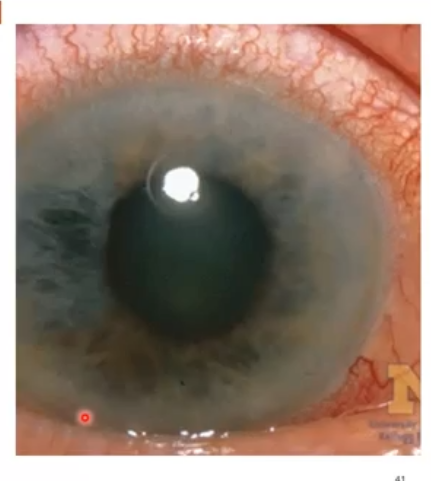
very high iop
acute closed angle glaucoma
pupil blocks drainage
retinal or choroidal detachment
leakage of ocular fluid after penerating injuries or surgery
intraocular inflammation
what are iop measuremnts affected by
corneal thickness
curvature
hydration - too much liquid increases pressure; odema
biochemical behaviour
variations
dinural
disease
age
racial background
short term factors affecting iop measurement
breath holding- when doing pulsair can increase pressure
lid sqeezing increases pressure
opening eyes wide- increases iop
ocular pulse can increase or decrease value
accomodation - increases as lens taking up more curvature space
eye movement- increase when moving a lot
tight clothing around the neck +1-3mmHg
recent contact lens removal increases value
eye rubbing - increases when rub then decrease after
medium term effects of measuring iop
diurnal variation of IOP 3-5 mmHg up to 10mmHg in glaucoma
posture changes - lying down increases pressure
repeated iop measurements- reduces pressure of iop -5mmHg
recent alcohol consumption - decreases value
recent exercise - incrases during, decreases after
recent consumption of fluids increase
prescribed or recreational medication - increase or decrease
long term factors affecting iop measurement
age- increases in caucasian and decrease in east asian
seasons +1-2mmHg in winter
smoking increases iop value
caffeine +2mmHg
diabetes, blood pressure and BMI: increase value of iop
drugs affecting iop
drugs that inhibit production act on the ciliary epithelia, either by interfereing with neural pathways or by inhibiting intracellular enzymes that maintain the ionic transport mechanisms in the formation of aq
beta blockers decrease aq production
certain prostaglandin may increase trabecular meshwork outlfow
aging changes in anterior chamber
with age the anterior chamber angle width narrows and volume decreases
due to decrease in aq production , a decrease in denisty and size of vacuoles , an accumulation of extracellular matrix plaques in the juxtacanalicular tissue and the inner wall of schlemms canal