Anxiety Disorders 🫨
1/42
Earn XP
Description and Tags
Anxiety is a spectrum of experience – not always pathological.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
State anxiety
Transient experience with a temporarily increased sympathetic nervous system response and feelings of intense tension, worry and apprehension. Short term
Trait anxiety
Personality trait. Stable across time and situations – people have a predisposition to respond in an anxious way.
Long term - shapes way process and make decisions
Brain area for state anxiety
Anterior cingulate gyrus, precuneous cortex
Brain area for trait anxiety
Superior frontal gyrus
Anxiety is clinically relevant when…
Disproportionate
Severe/enduring
Linked with functioning impairments
Anxiety sensitivity
Fear of experiencing anxiety-related sensations and symptoms, based on the idea that you perceive them as psychologically/socially/physically harmful.
Linked to onset of anxiety disorders.
GAD Criteria A
Excessive anxiety/worry on more days than not for >6 months, about several events or activities.
GAD Criteria B
Difficult to control the worry.
GAD Criteria C
Anxiety/worry linked with >3 symptoms. At least some present for more days than not, for at least 6 months.
i. Restless/keyed-up or on edge
ii. Easily fatigued
iii. Difficulty/concentrating/mind going blank
iv. Irritable
v. Muscle tension
vi. Sleep disturbance
GAD Criteria D
Clinically significant distress or functional impairment.
20% have more severe impairments.
Panic attacks
Sudden and intense episodes of extreme fear/discomfort – 20% of people with GAD experience panic attacks.
Last 5-20 minutes, de-esculate themselves - in the moment, they genuinely think something catastrophic is happening.
1/3 of us will experience at least 1 panic attack in our lives
PD Criteria A
Recurrent, unexpected panic attacks = abrupt surge of intense fear/discomfort that peaks within minutes.
PD Criteria B
At least one attack has been followed by >1 month of:
i. Persistent concern about additional panic attacks or their consequences.
And/or
ii. Sig maladaptive behaviour change related to the attacks e.g. avoidance of situations, activities that believe triggered PD, performing safety behaviours (things think will stop another one happening).
How many people with anxiety fulfil criteria for 2+ disorders.
40-70%
Kessler et al. (2005)
Tetrachoric correlations show relationships between conditions for past 12 months (highest GAD-MDD, PD-dysthymia)
Remes et al. (2016)
Review. Anxiety range 3.8-25%, most estimates 4-11%
Rates higher in women, young adults, people with chronic diseases, LGB, been/currently pregnant
Millet et al. (2016)
Review anxiety prevalence in trans - 17-68%, higher in trans men
Javaid et al. (2023)
Total number of people worldwide with an anxiety disorder increased 1990-2019. BUT after adjusting for changes in underlying population age structure, prevalence rates over the same time period appeared to be relatively stable.
Baxter et al. (2013)
Review in 44 countries. Prevalence in Euro-Anglo cultures, non-western appear to have lower rates.
Women with anxiety disorder are…
More likely to be diagnosed with MDD or BN over lifetime
Less likely to be diagnosed with a substance use disorder, ADHD or intermittent explosive disorder.
Sig higher proportion of women (44.8%) with a lifetime incidence of anxiety disorder met criteria for an additional anxiety disorder than men (34.2).
Women/men internalising/externalising co-morbid disorders
· Women more likely to have co-morbid internalising disorders – symptoms focused on self e.g. depression, ED.
· Men more likely to have co-morbid externalising disorders – symptoms more outward focused e.g. aggression, impulsivity, substance-use.
De Lijster et al. (2017)
14 studies. Mean age of onset is 21 years, similar for all genders.
Bruce et al. (2005)
Followed MH people over 12 years. PD has higher remission than GAD. PD and GAD have similar recurrence rates until 8 years since recovery, where PD has increase in recurrence rates.
Penninx et al. (2011)
Followed anxiety for 2 years. Median duration of illness 16 months.
42% showed chronic course
7% switched to depression
16% developed co-morbid depression
Presence of anxiety and longer duration episodes predicted by:
a) Severity and duration of baseline episode
b) Co-morbid depression-anxiety
c) Earlier age of onset
d) Older age overall
Meier and Deckert (2019)
If have a first degree relative with an anxiety disorder, are 4-6x more likely to get one.
Heritability 30-50%
Lawrence et al. (2019)
People whose parents have an anxiety disorder are more likely to have anxiety, depressive disorders (greater for anxiety).
If have a family member with anxiety disorder, not at risk for that specific disorder, but for an anxiety disorder in general.
Ohi et al. (2020)
Shared genetic risk between anxiety disorders and Sz, ADHD and depressive disorders.
Temperament in anxiety disorders
Behavioural inhibition = temperament style characterised by shyness, fear and avoidance of novel stimuli/situations. Longitudinally predicts anxiety disorders.
Sandstrom et al. (2020)
Review. Odds ratio of developing any anxiety disorder from behavioural inhibition 2.8
Psychosocial risk factors in early life
Prenatal stressors, childhood maltreatment, socioeconomic deprivation, stressful life events early childhood
Zimmerman et al. (2020)
Review.
Identified risks:
Cig smoking frequency
Alcohol use
Cannabis use
Negative appraisals of life events
Avoidance
Occupational factors
Identified protective factors:
Social support
Adaptive coping skills
Physical activity
HPA axis in anxiety
Increased sympathetic tone and decreased parasympathetic activity from anxiety disorders = increases inflammation.
Dysregulation of HPA axis leads to chronic, low-level inflammation, which creates neurotoxic effects on the brain.
Brain circuits in anxiety
Mixed evidence - these are the most consistent:
Increased volume and hyperactivation of amygdala, anterior cingulate cortex, postcentral gyrus.
Decreased volume and hypoactivity of dorsolateral PFC.
Impaired communication between limbic areas and PFC.
Cognitive processes
Perceived lack of control
Intolerance of uncertainty
Positive and negative beliefs about worry
Cognitive biases
NICE recommendation for GAD and PD
Stepped-care approach, using low intensity treatment possible to match severity.
Recommends treatment switching if 1 doesn’t work
Slee et al. (2019)
Review of meds vs placebo in GAD.
Small to moderate effects sizes for:
SNRIs and SSRIs e.g. escitalopram (first choice drug treatment for GAD, start at lower dose than depression then titrate above depression)
Anticonvulsants e.g. pregabalin (treat neuropathic pain)
Antipsychotics (for severe)
Side effects, risks and acceptability vary
Long term effectiveness rates we’re not so sure about
Drugs in PD
Many meds appear effective for PD as GAD - remission less likely following treatment (Chawla et al., 2022).
Psychological treatment for PD
‘Formulation’ = clinical psychologists do at beginning of treatment to create an individualised treatment course for an individual.
5 Ps:
1. Presenting: What is problem itself e.g. functional impairment?
2. Predisposing factors: What made patient vulnerable in first place?
3. Precipitating factors: What triggered the current episode / escalation of symptoms?
4. Perpetuating factors: What keeps the symptoms going?
5. Protective factors: What protective factors are in place?
Cognitive Model of Panic (Clark, 1986)
People that experience recurrent panic attacks do so because misinterpret benign bodily sensations as symptoms of an “immediately impending physical or mental catastrophe”.
Avoidance/safety behaviours - reduce anxiety, prevent person from discovering that their fears are groundless. Negatively reinforces them and catastrophic misinterpretation.
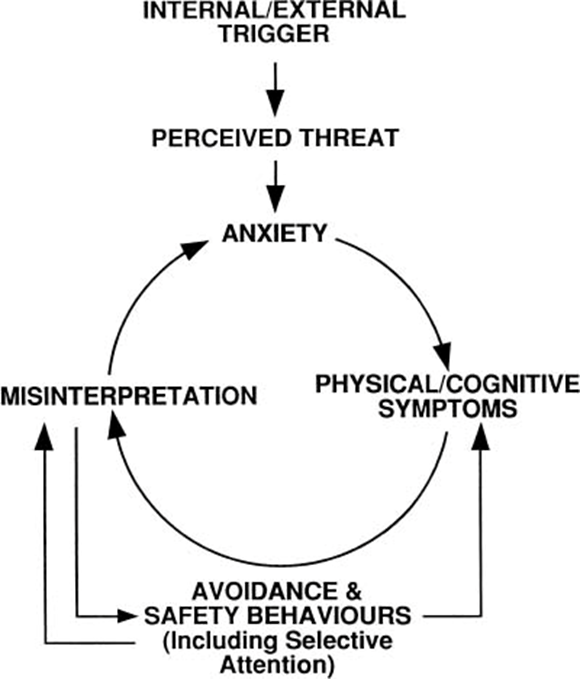
Stages that CBT can work on (in Clark, 1986’s model)
Triggers - Identify anxiety triggers
Perceived threat - Reduce anxiety-driven biases that lead to ambiguous stimuli being interpreted as threatening
Avoidance and safety behaviours - Replace them
Cuijpers et al. (2016)
Large positive effect for CBT for GAD
Cuijpers et al. (2019)
Large positive effect for CBT for PD (better than GAD)
Cuijpers et al. (2014)
Meta-analysis. Combined therapies (CBT and meds) sig reduce symptoms.