Cardio/Renal 25 - Glomerular Filtration and Clearance I (Dr. Olgun)
1/71
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
72 Terms
Kidneys regulate the composition and volume of the...
plasma and extracellular fluid

a nephron consists of a glomerulus and a ________________
tubule
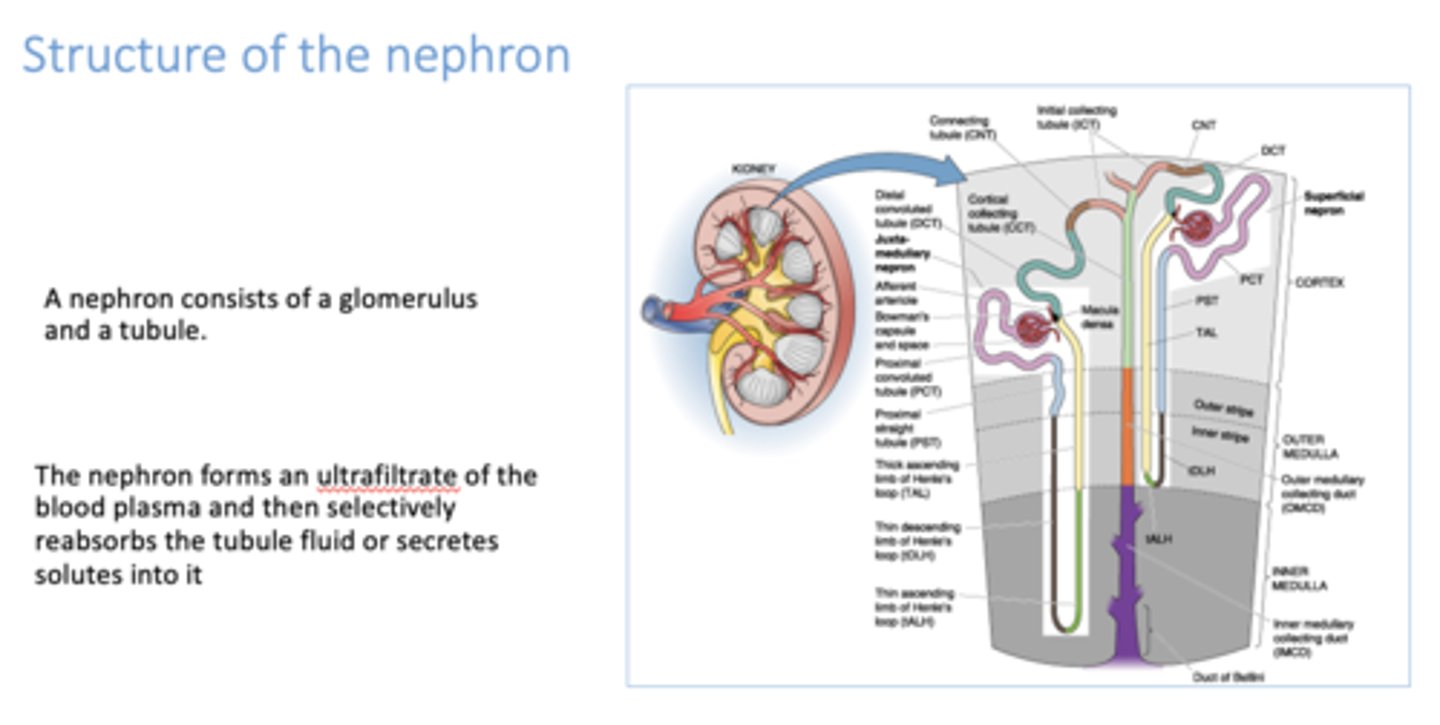
The ___________ forms an ultrafiltrate of the blood plasma and then selectively reabsorbs the tubule fluid or secretes solutes into it
nephron
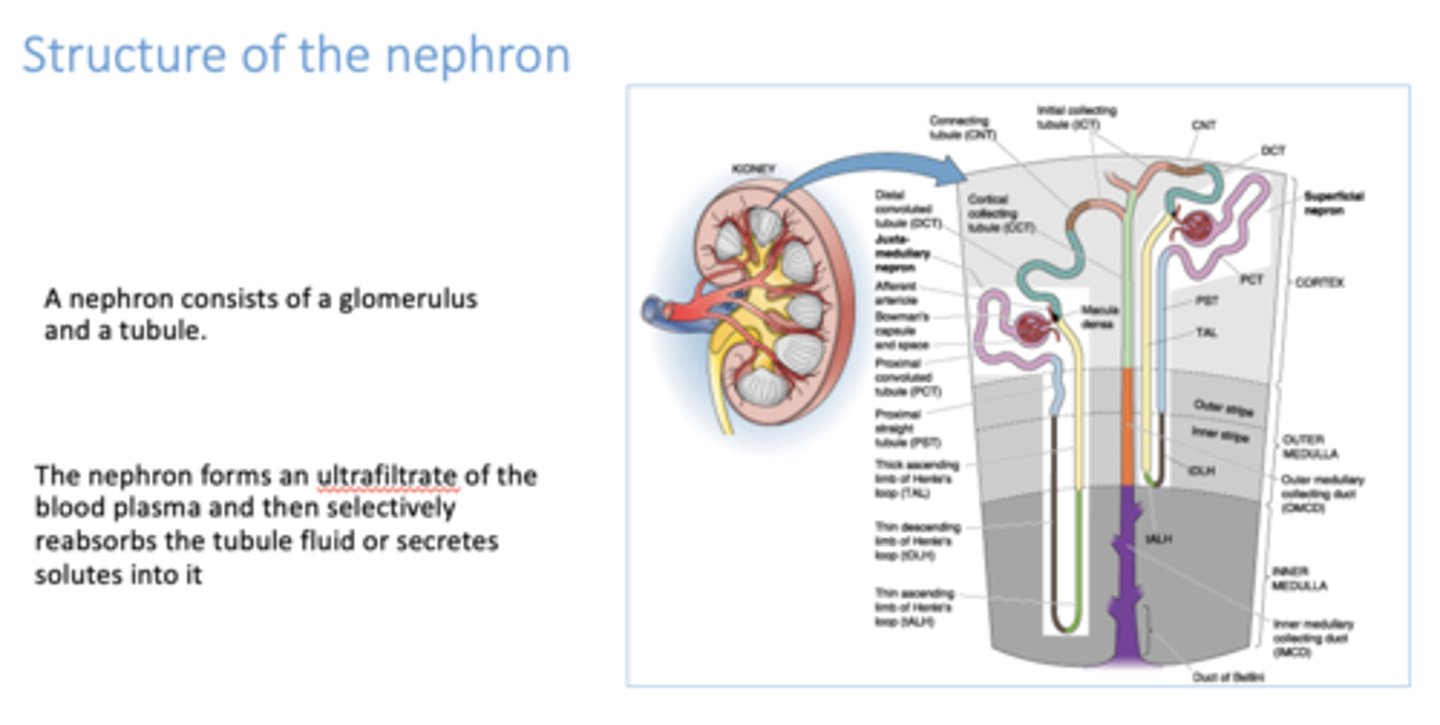
4 things the kidneys do to regulate the composition and volume of plasma and ECF:
- Filtration
- Reabsorption
- Secretion
- Excretion

______________ is the site of formation of the glomerular filtrate
renal corpuscle
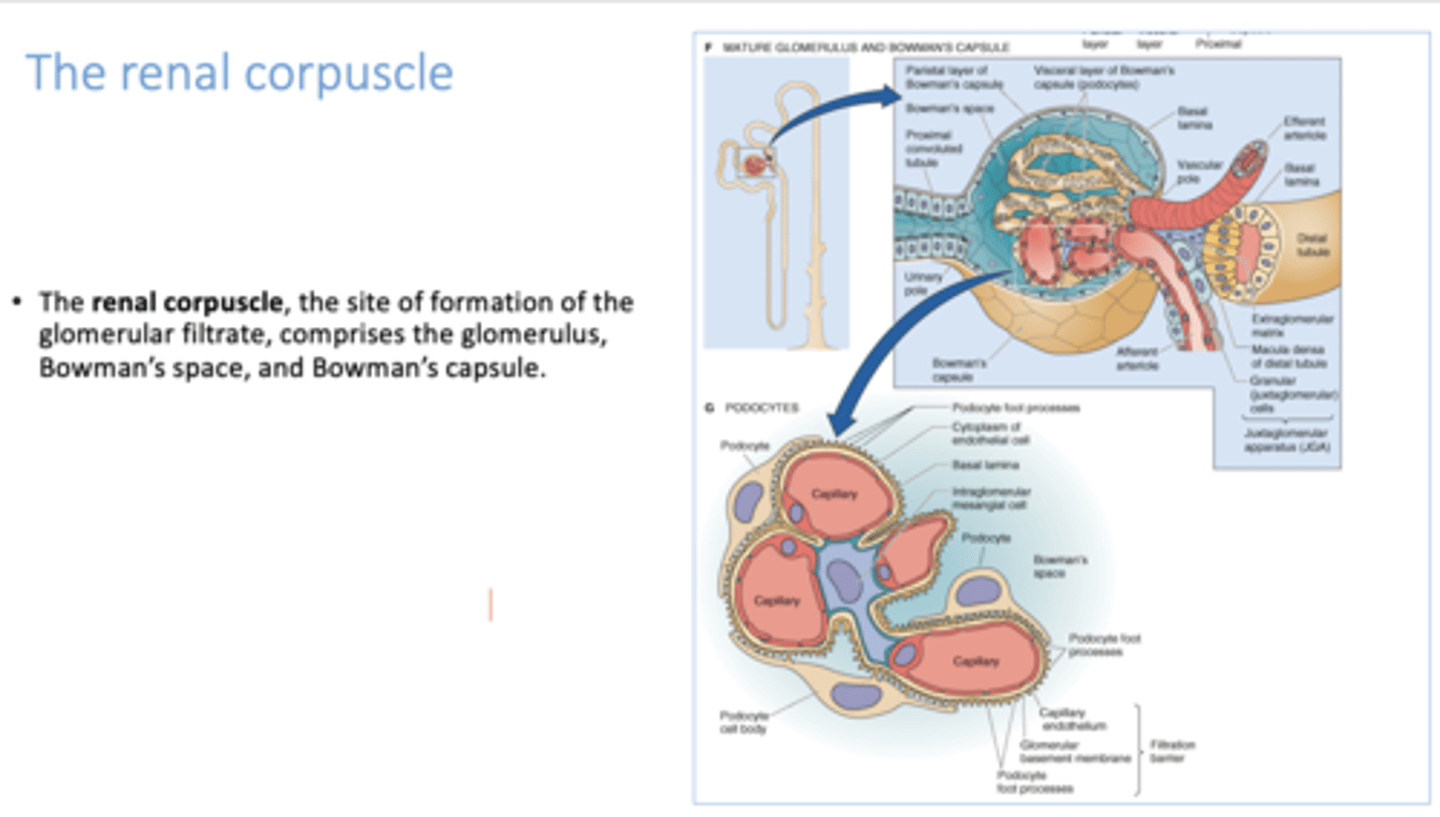
______________ comprises the glomerulus, bowman's space and bowman's capsule
renal corpuscle
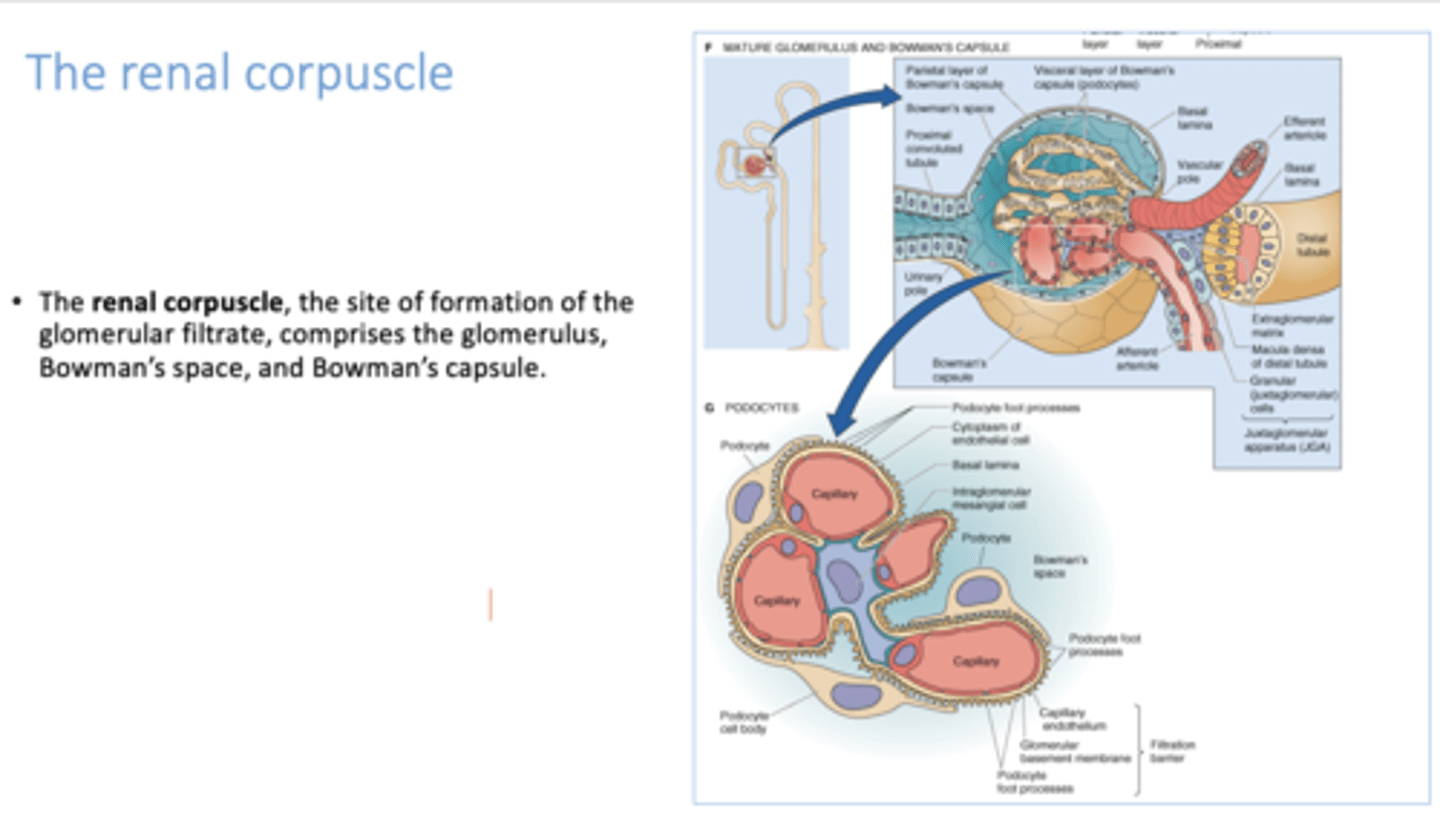
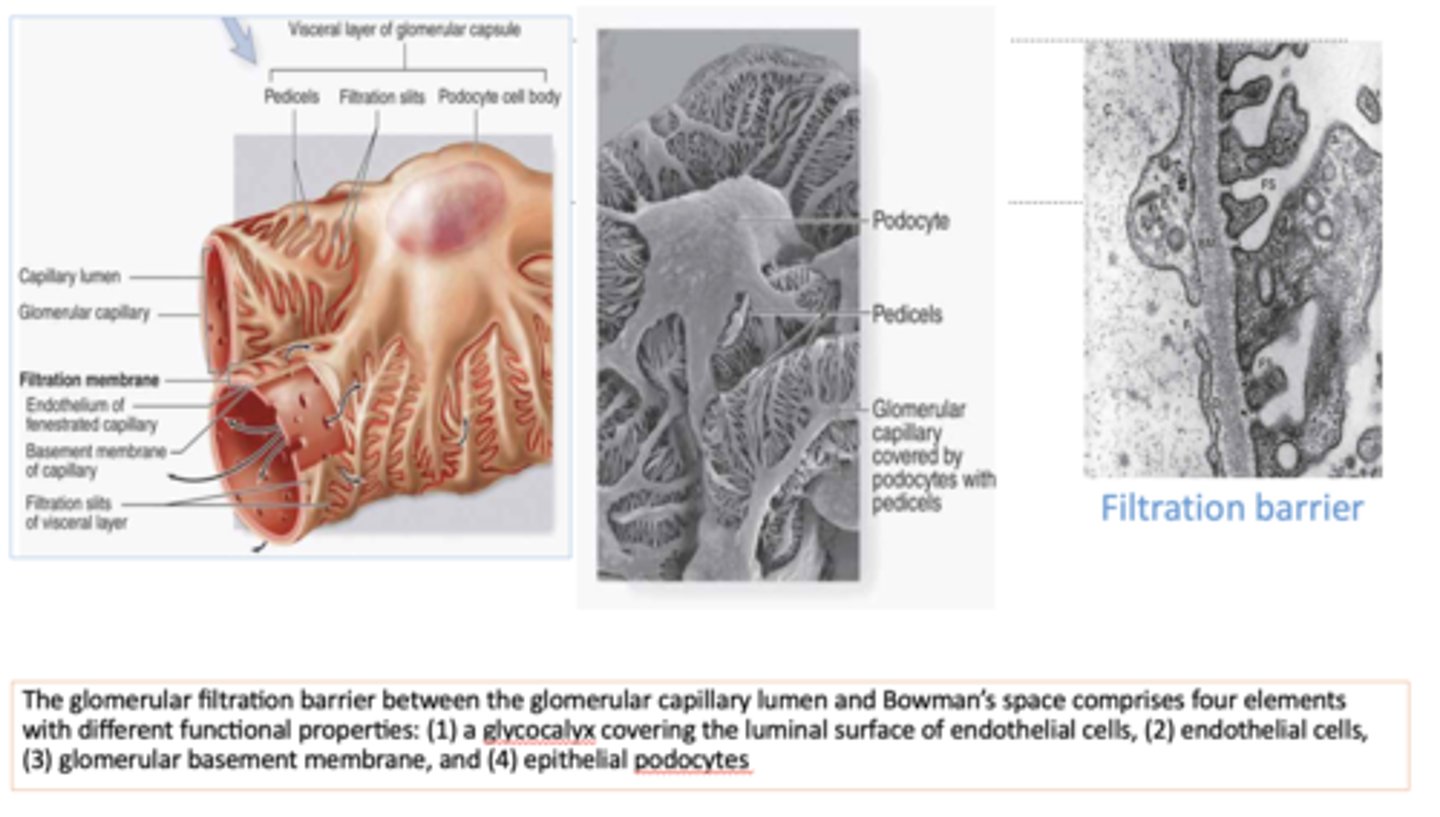
What four elements comprise the glomerular filtration barrier?
- Glycocalyx
- Endothelial cells
- Glomerular basement membrane
- Epithelial podocytes
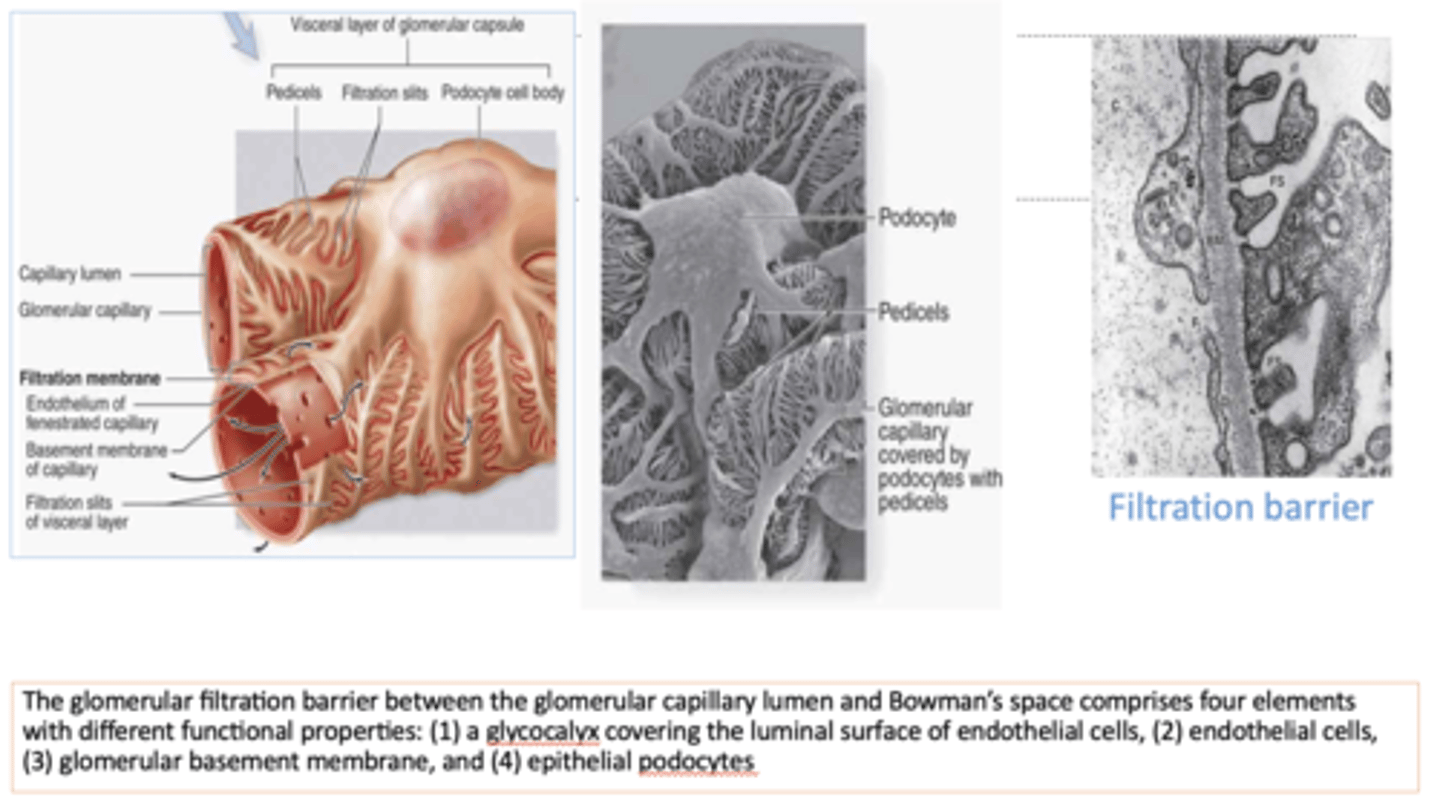
Why does the basement membrane in the glomerular filtration have a negative charge?
Repel proteins from filtration
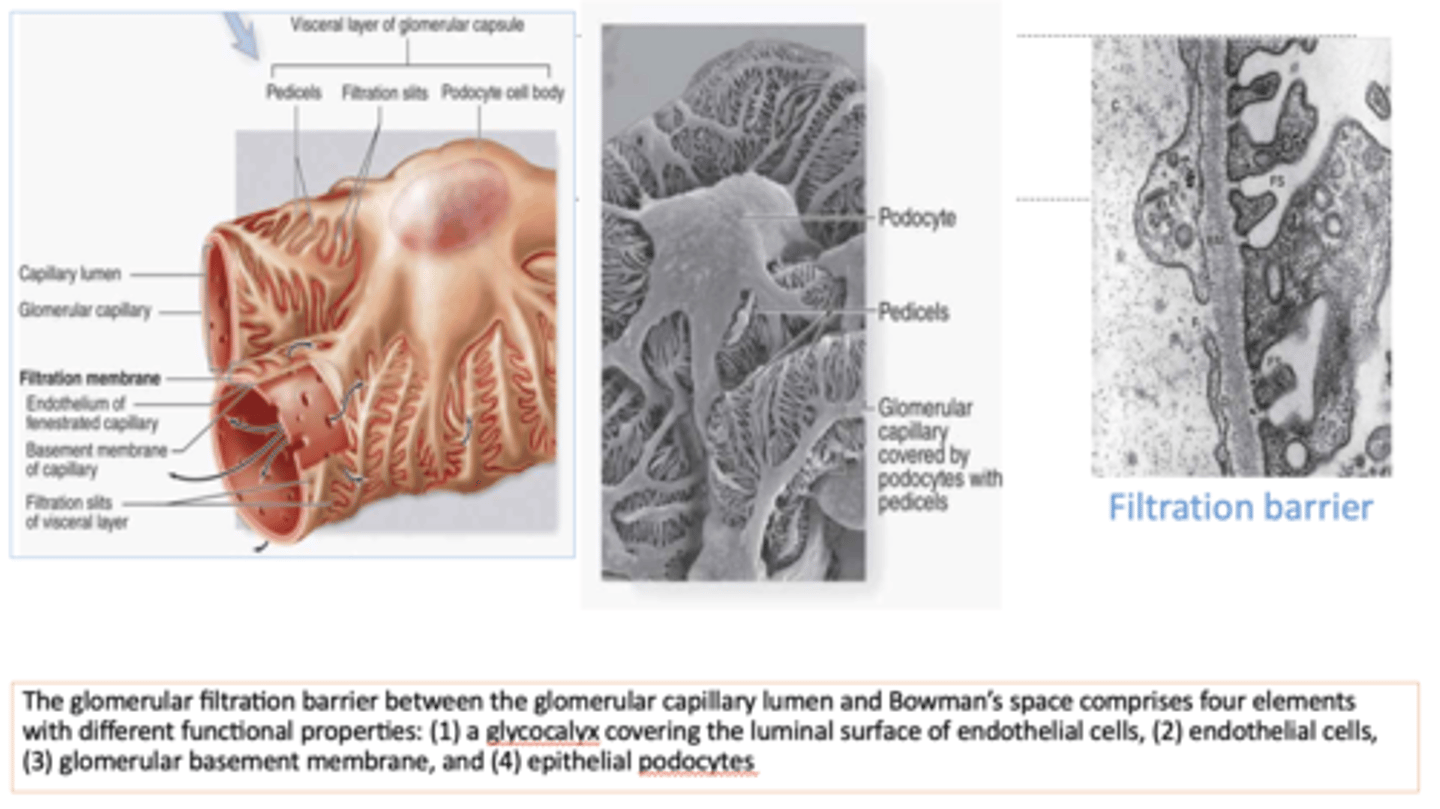
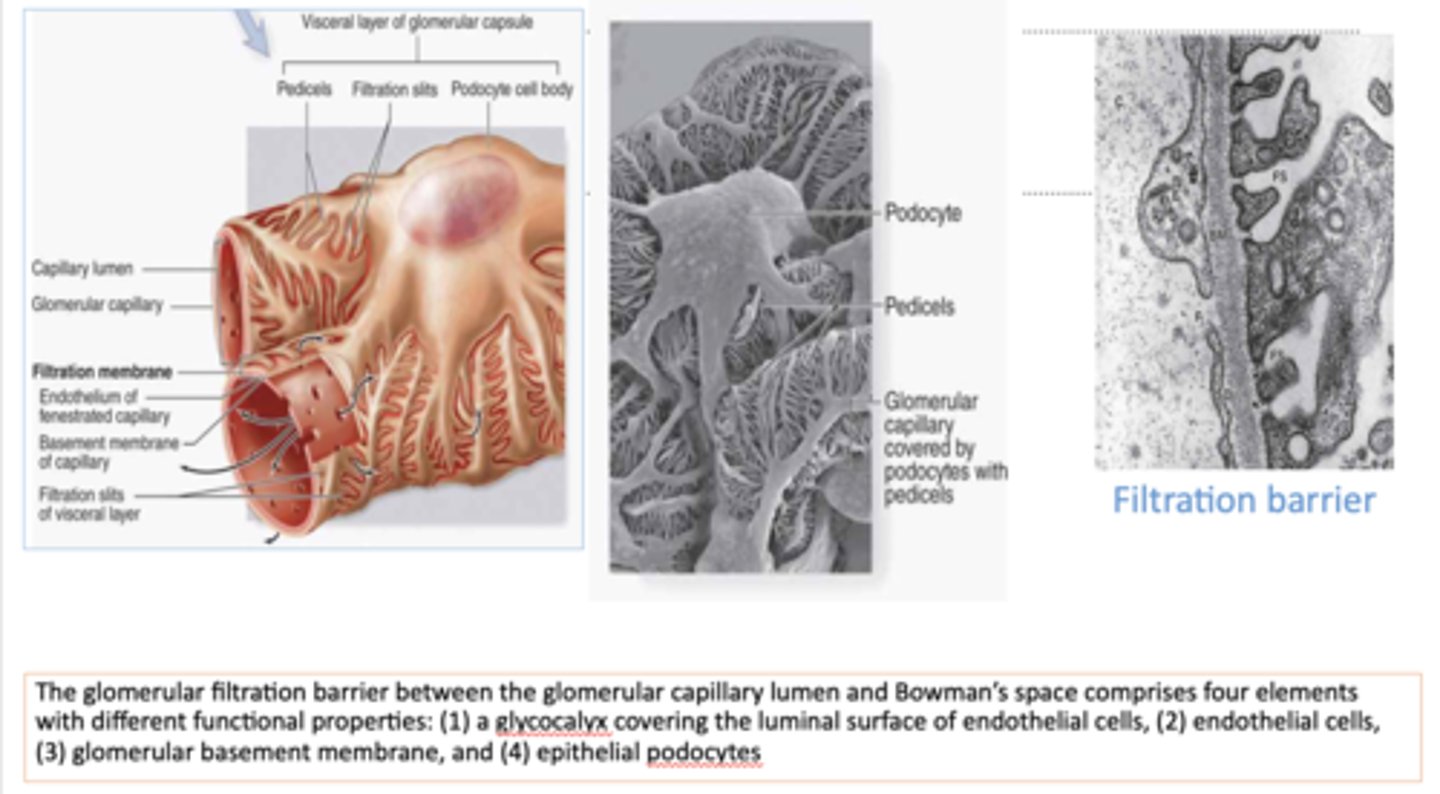
what structures cover the glomerular capillaries and represent the visceral layer of Bowman's capsule?
podocytes
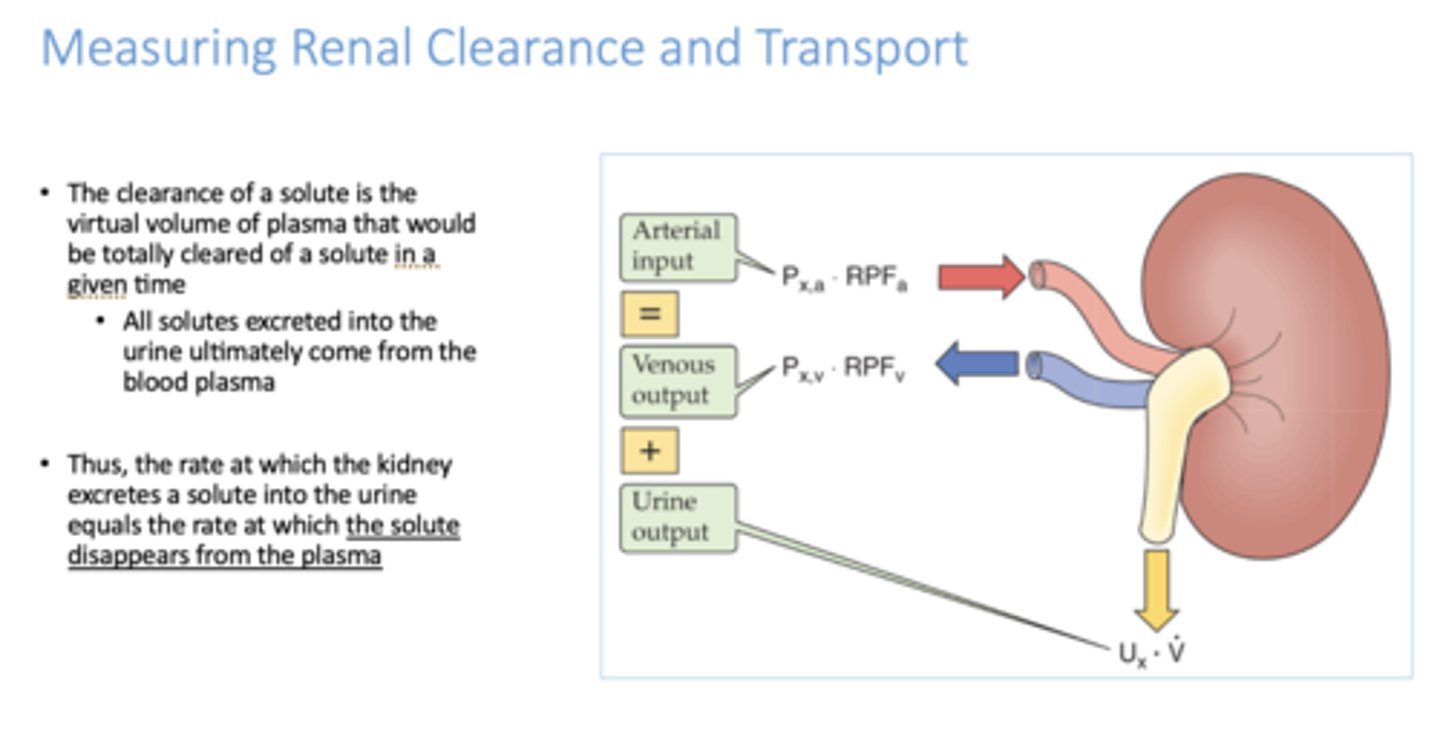
All solutes excreted into the urine ultimately come from the _____________
blood plasma
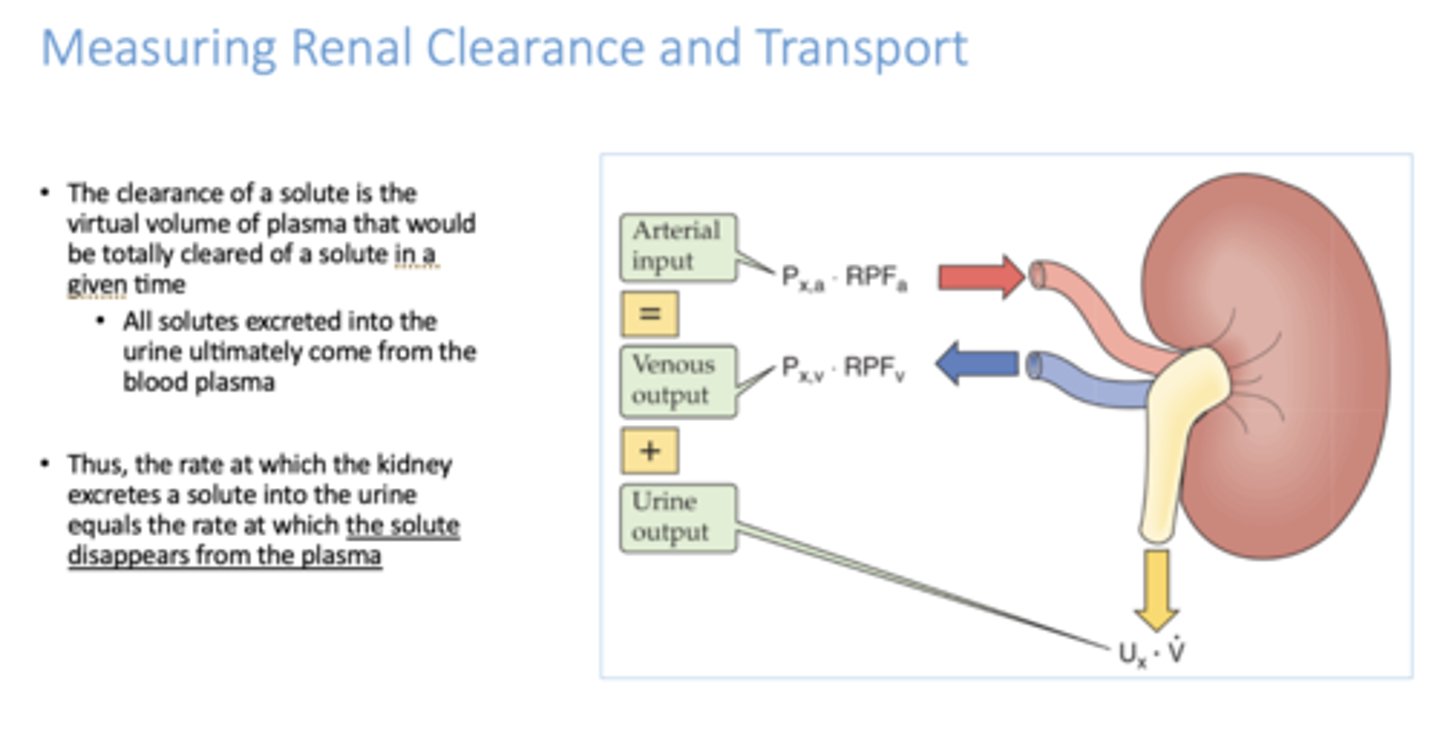
The _________ of a solute is the virtual volume of plasma that would be totally cleared of a solute in a given time
clearance
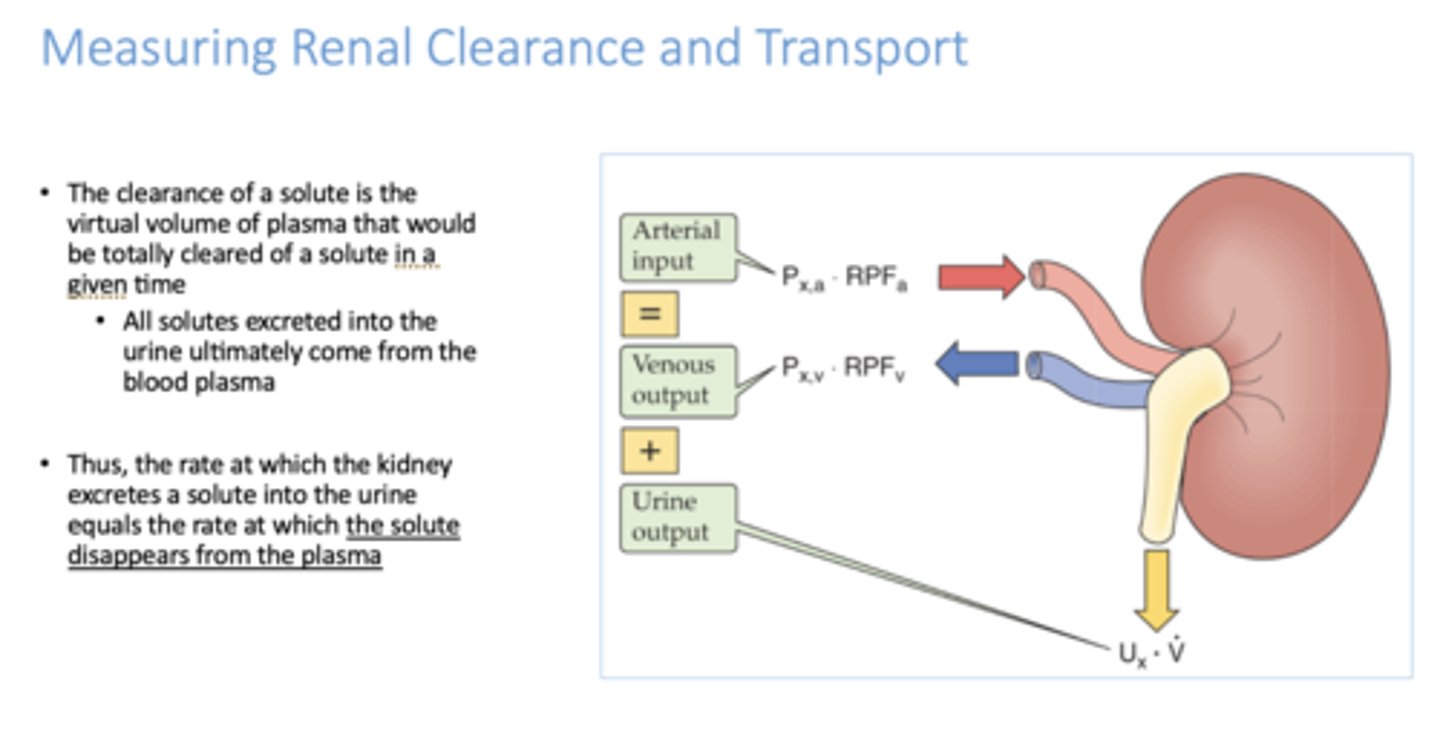
t/f: the rate at which the kidney secretes a solute into the urine = the rate at which the solute disappears from plasma
True
These are the 3 basic functions of the _____:
- Glomerular filtration
- Tubular reabsoprtion
- Tubular secretion
kidney

The ______ consists of negatively charged glycosaminoglycans that may play a role in preventing leakage of large negatively charged macromolecules.
glycocalyx
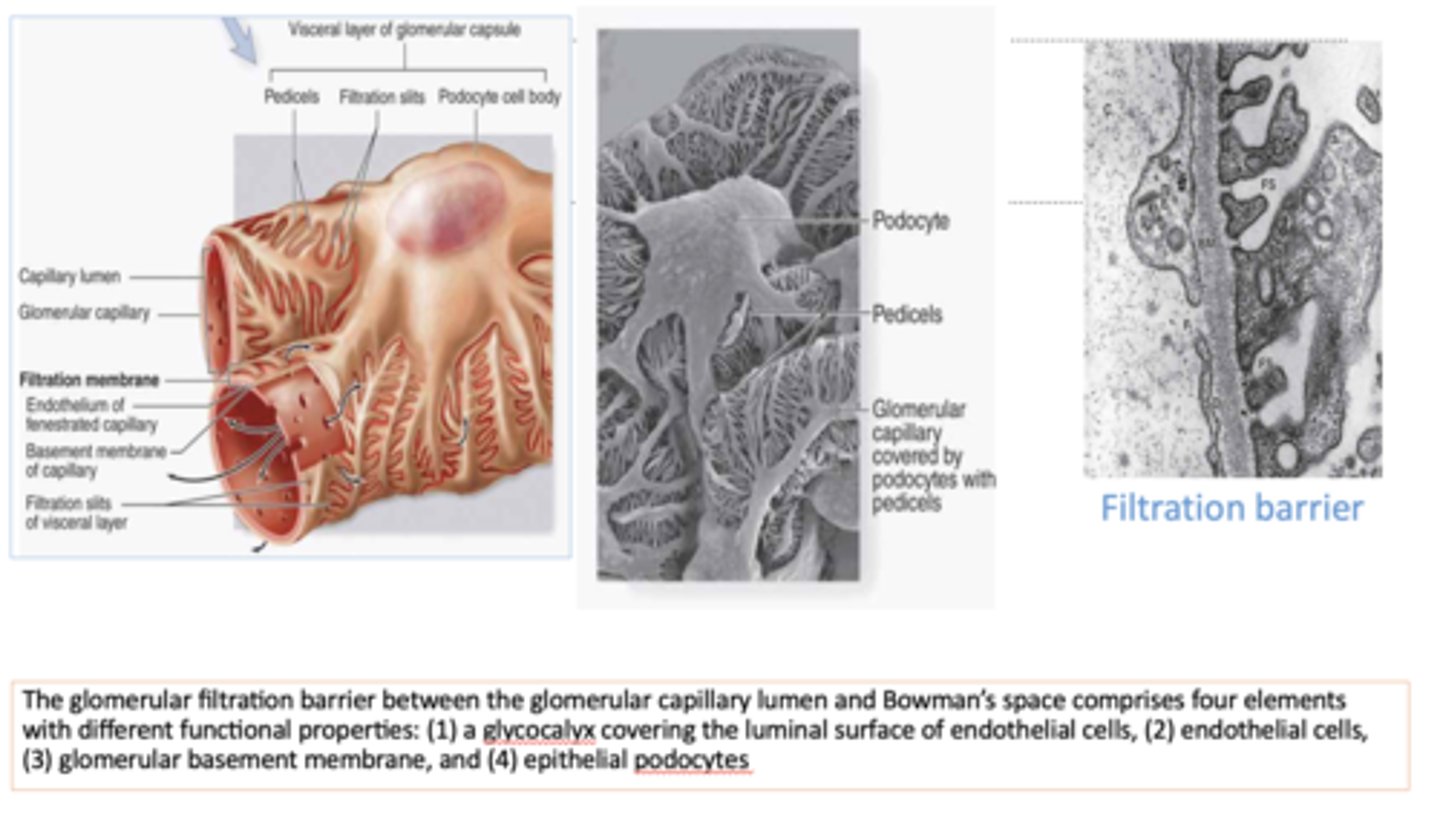
what is located between endothelial cells and podocyte foot processes?
basement membrane
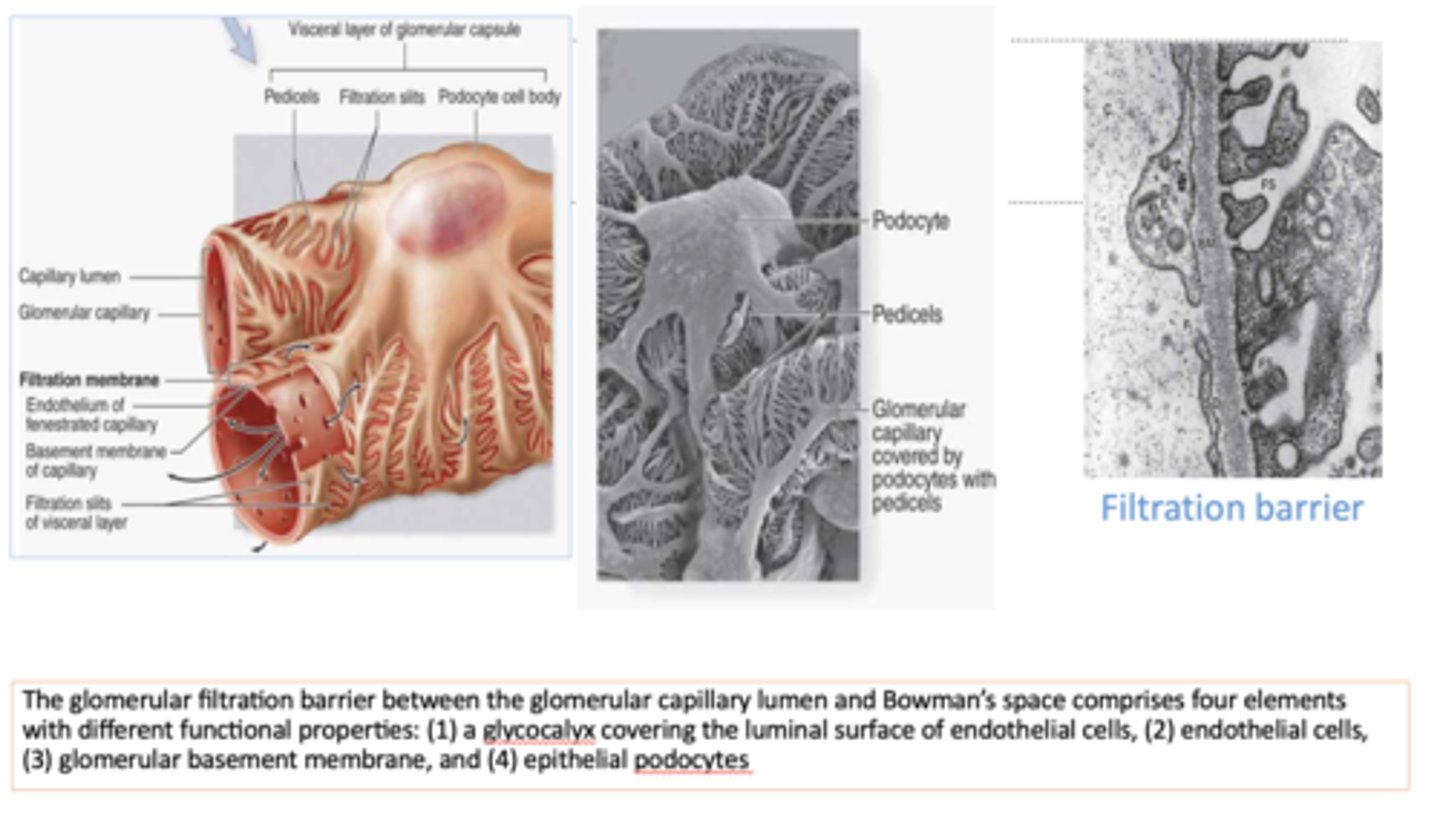
The __________ makes an important contribution to the permeability characteristics of the filtration barrier by restricting intermediate-sized to large solutes
basement membrane
this molecule is used as a diagnostic agent in the measurement of renal plasma flow (RPF):
p-aminohippurate (PAH)

if you use p-aminohippurate (PAH) clearance, you can calculate:
renal plasma flow

if you use inulin or creatinine clearance, you can calculate:
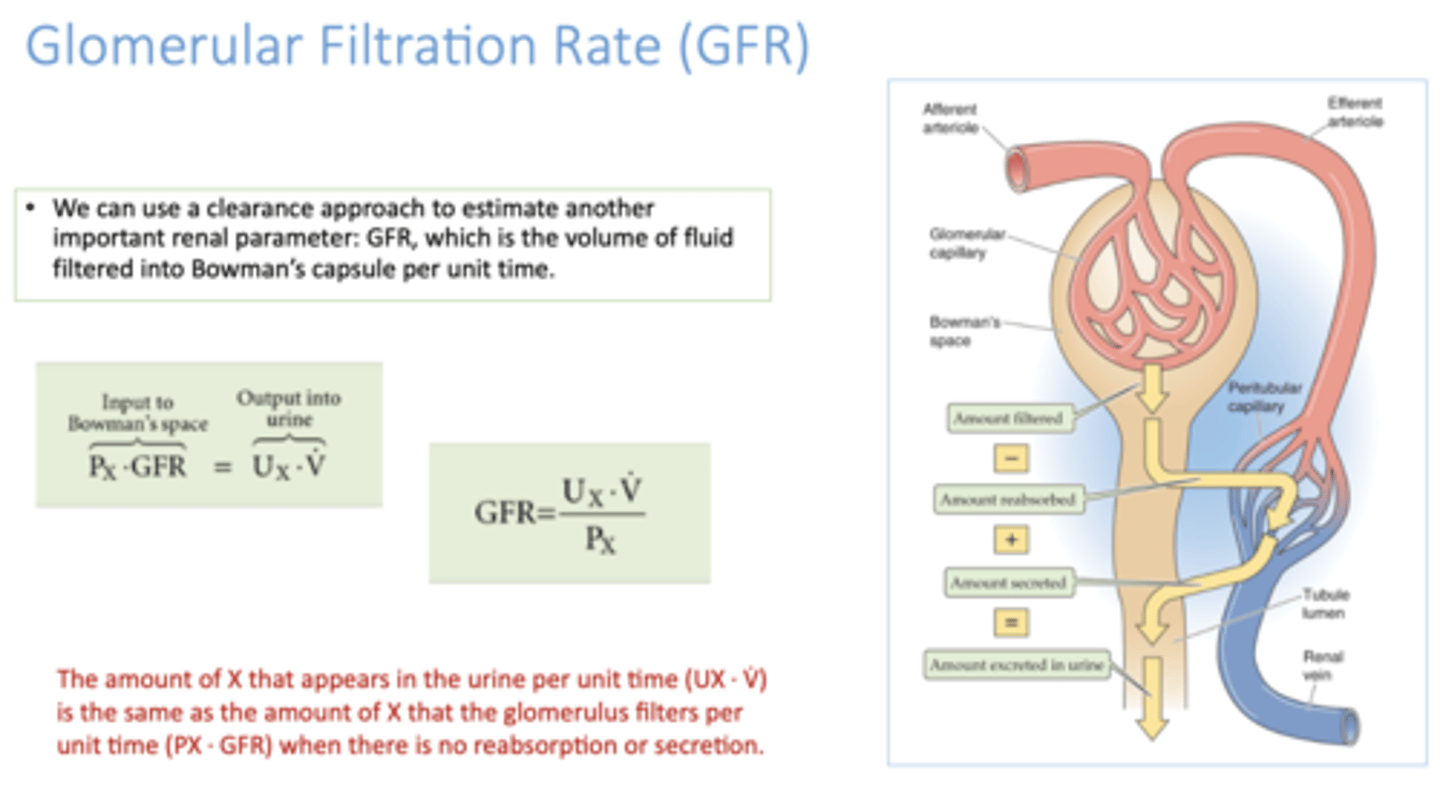
Glomerular Filtration Rate (GFR)
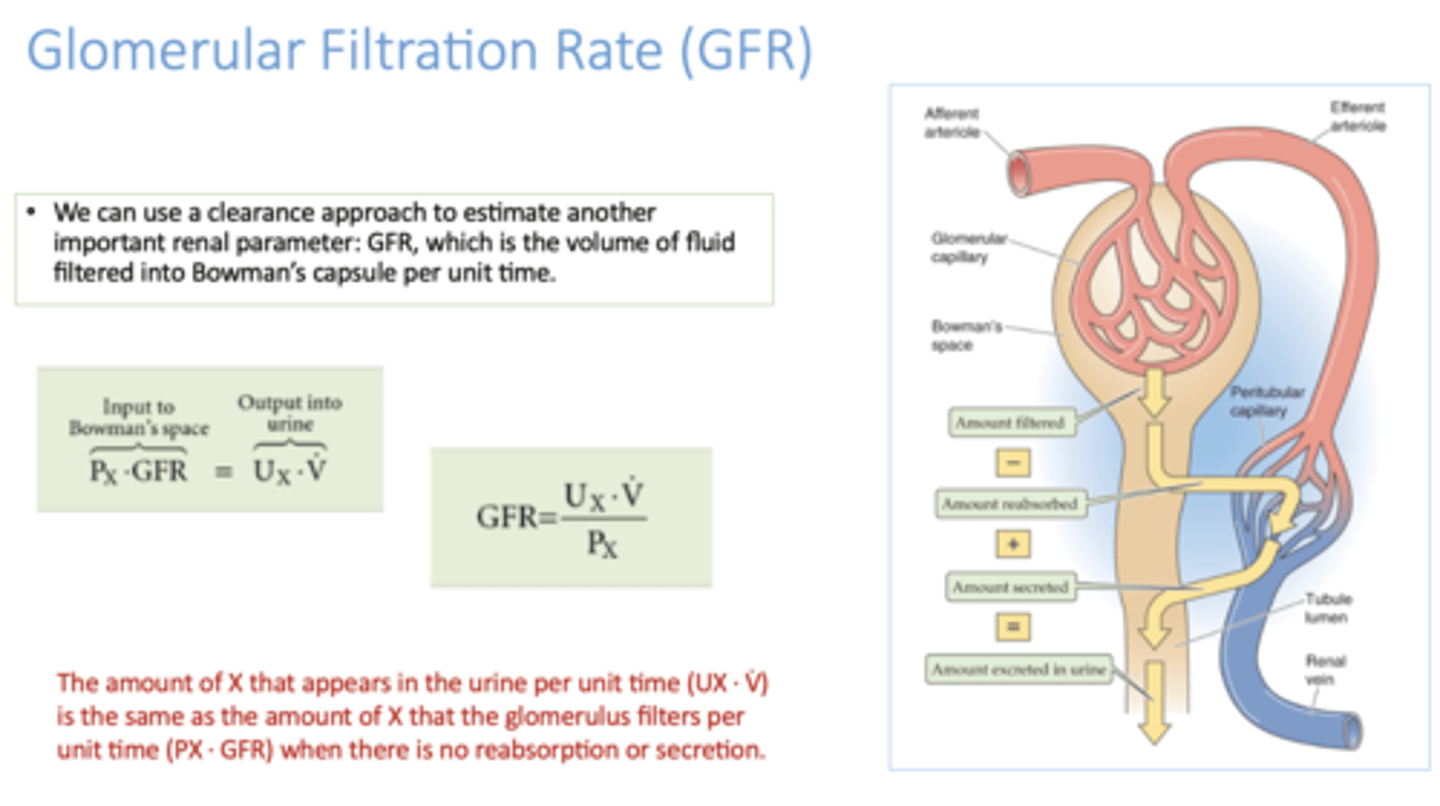
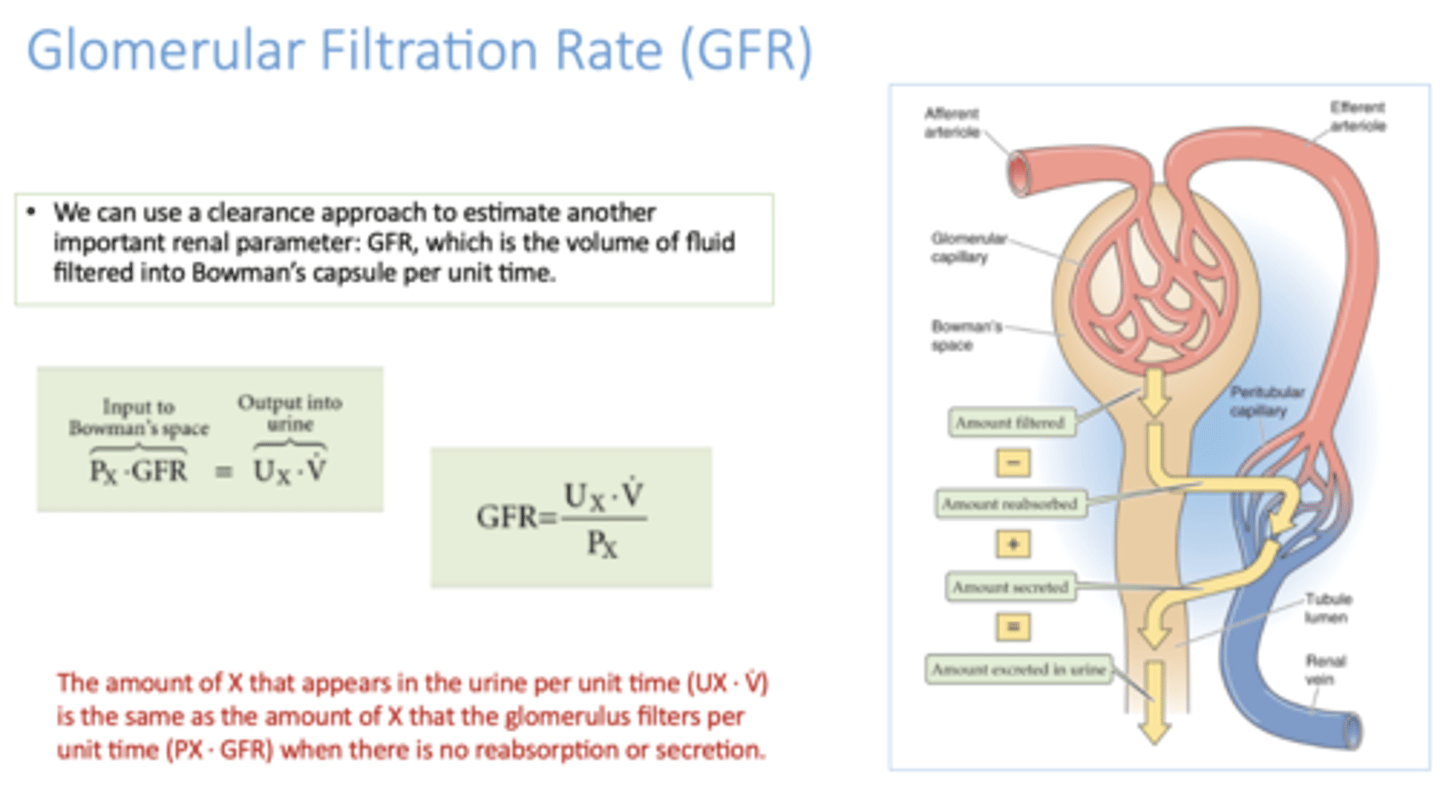
Define the following:
Volume of fluid filtered into Bowman's capsule per unit of time
Glomerular Filtration Rate (GFR)
What is the Clearance equation?
C= [U]*V/[P]
![<p>C= [U]*V/[P]</p>](https://knowt-user-attachments.s3.amazonaws.com/9eb67882-660a-473b-9741-845aac0df276.jpg)
The following tests were obtained on a specimens
- Urine urea: 220 mmol/liter
- Urine flow rate: 2.0 ml/min
- Plasma urea: 5 mmol/liter
What is the clearance of urea for this patient?
A. 44 ml/min
B. 88 mmol/min
C. 44 mmol/min
D. 88 ml/min
E. 444 ml/min
D. 88 ml/min

A ___________ GFR is essential for maintaining stable and optimal extracellular levels of solutes and water
high

________ levels of GFR would cause the excretion of material to be delayed
Low

Define the following:
Fluid moving from peritubular capillaries into tubule system
secretion
Define the following:
Fluid moving from tubule system into peritubular capillaries
Reabsorption
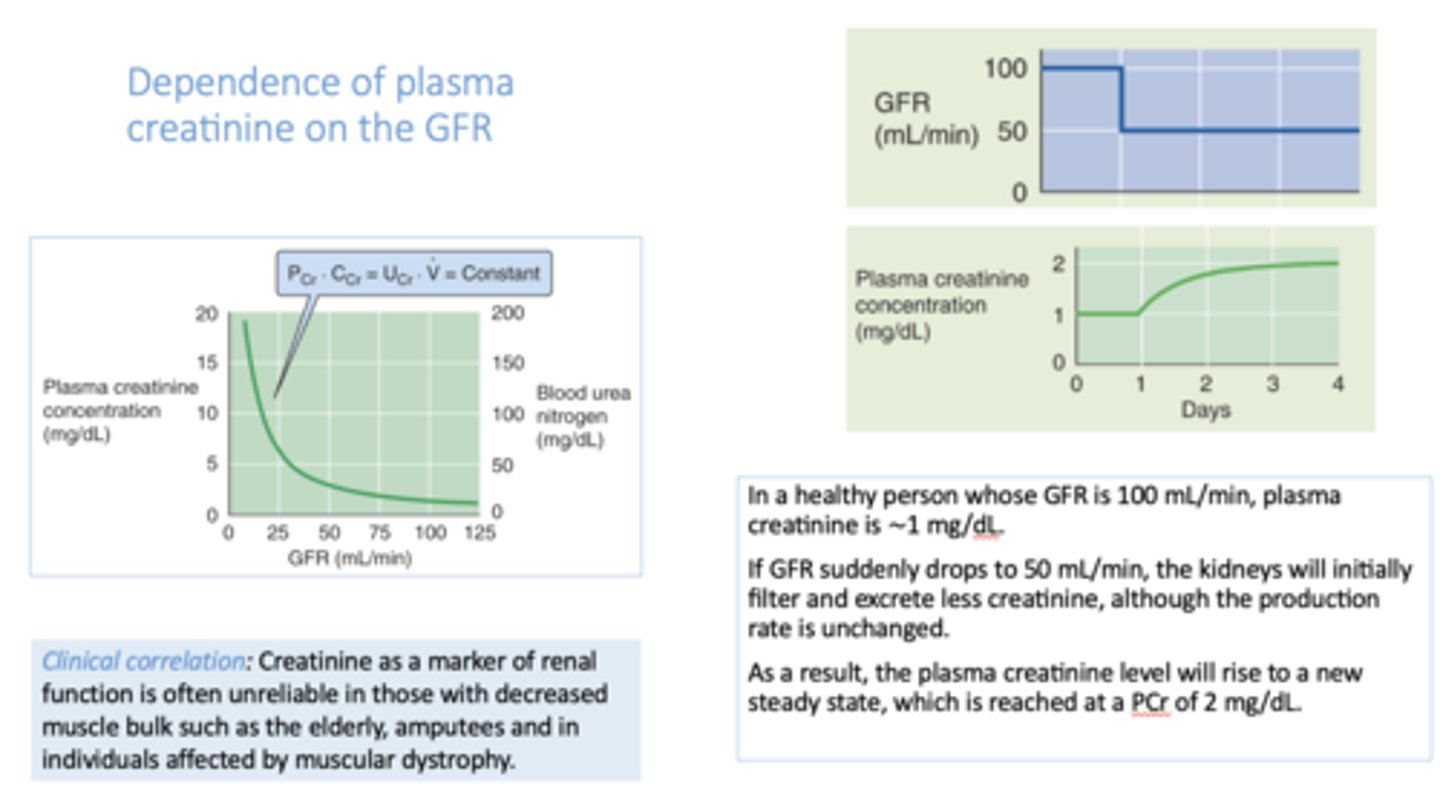
_________ as a marker of renal function is often unreliable in those with decreased muscle bulk such as the elderly, amputees and in individuals affected by muscular dystrophy.
Creatinine
if 100 mL was filtered into the PCT and 120mL was passed as urine, what occurred?
secretion
if 100 mL was filtered into the PCT and 80mL was passed as urine, what occurred?
Reabsorption
a protein that is filtered but does not experience secretion or absorption can be used to calculate:
Glomerular Filtration Rate (GFR)
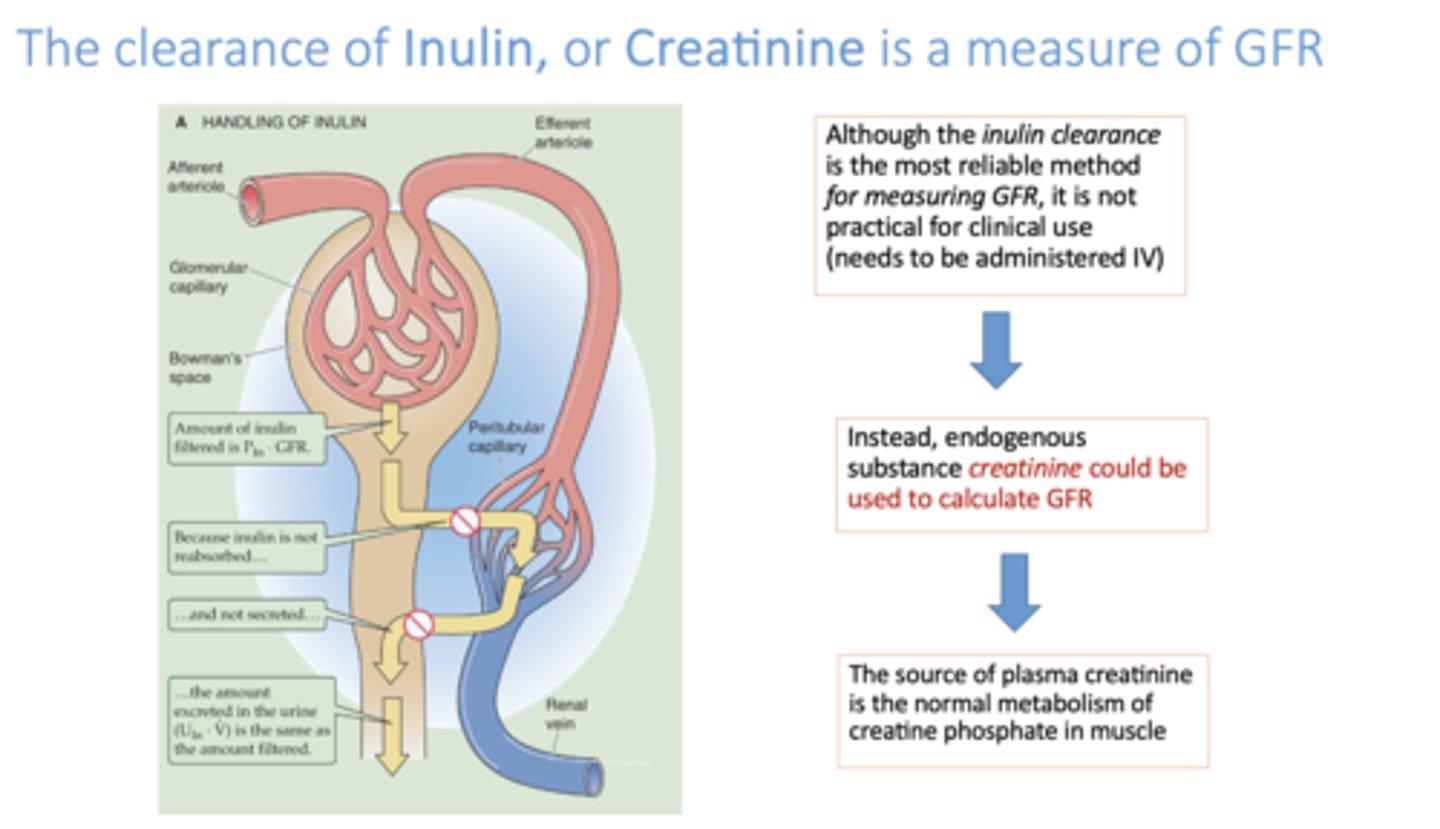
what two proteins are used to calculate Glomerular Filtration Rate (GFR)?
inulin and creatinine
what is Ux in the renal clearance formula?
urine concentration of a solute

What is V in the renal clearance formula?
Urine volume

what is Px in the renal clearance formula?
plasma concentration of a solute

Under normal conditions, the GFR of the two kidneys is:
125 mL/min or 180 L/day

Low levels of GFR would _______ the plasma level of a toxic material
increase
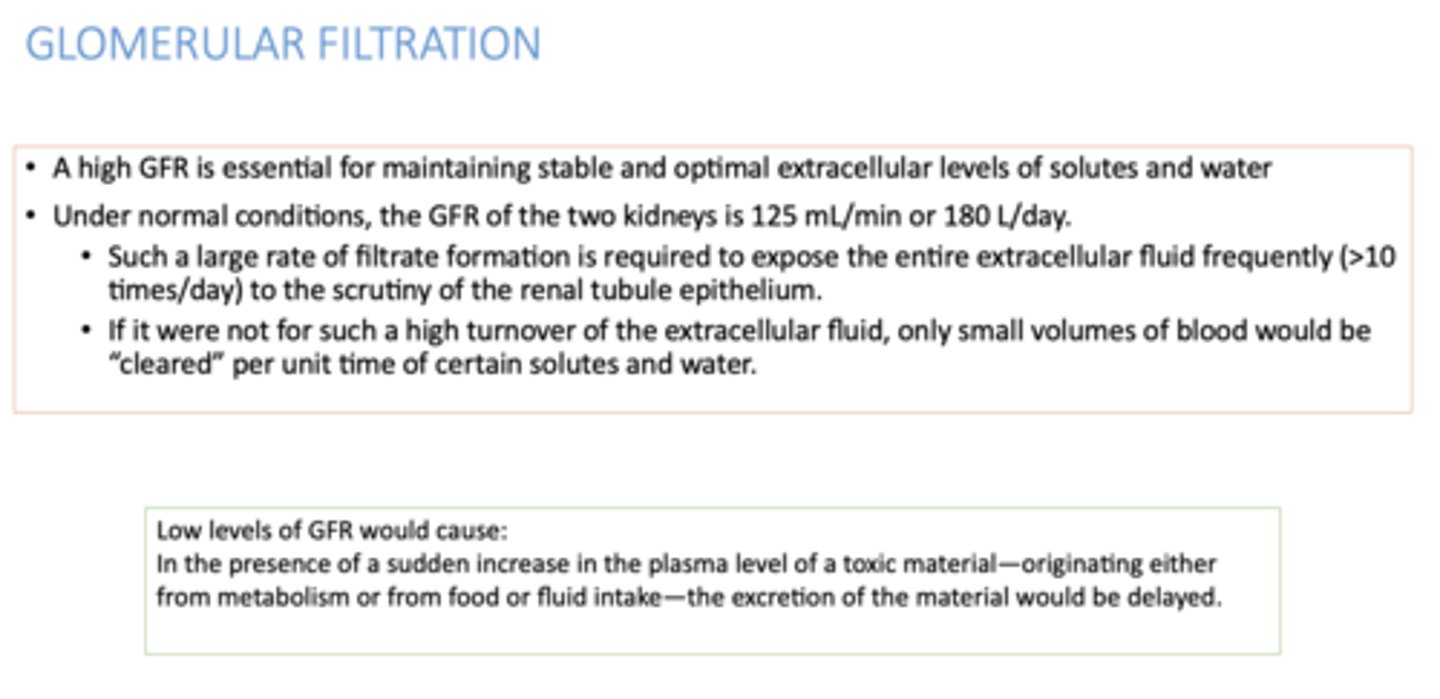
Low levels of GFR would _______ the steady-state plasma levels
increase

clinically, what protein is used to calculate glomerular filtration rate (GFR)?
creatinine
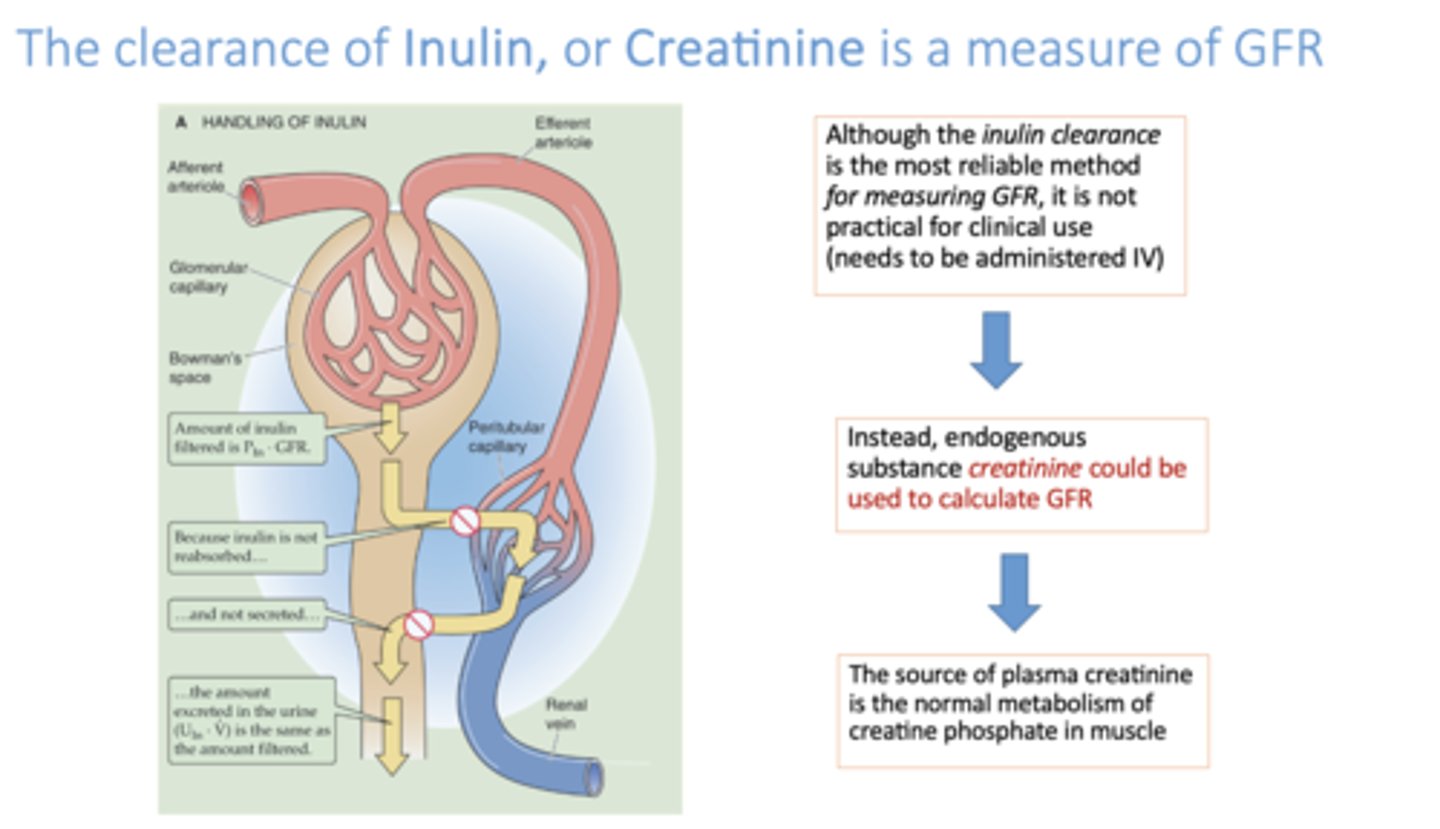
what is the source of creatinine?
muscles
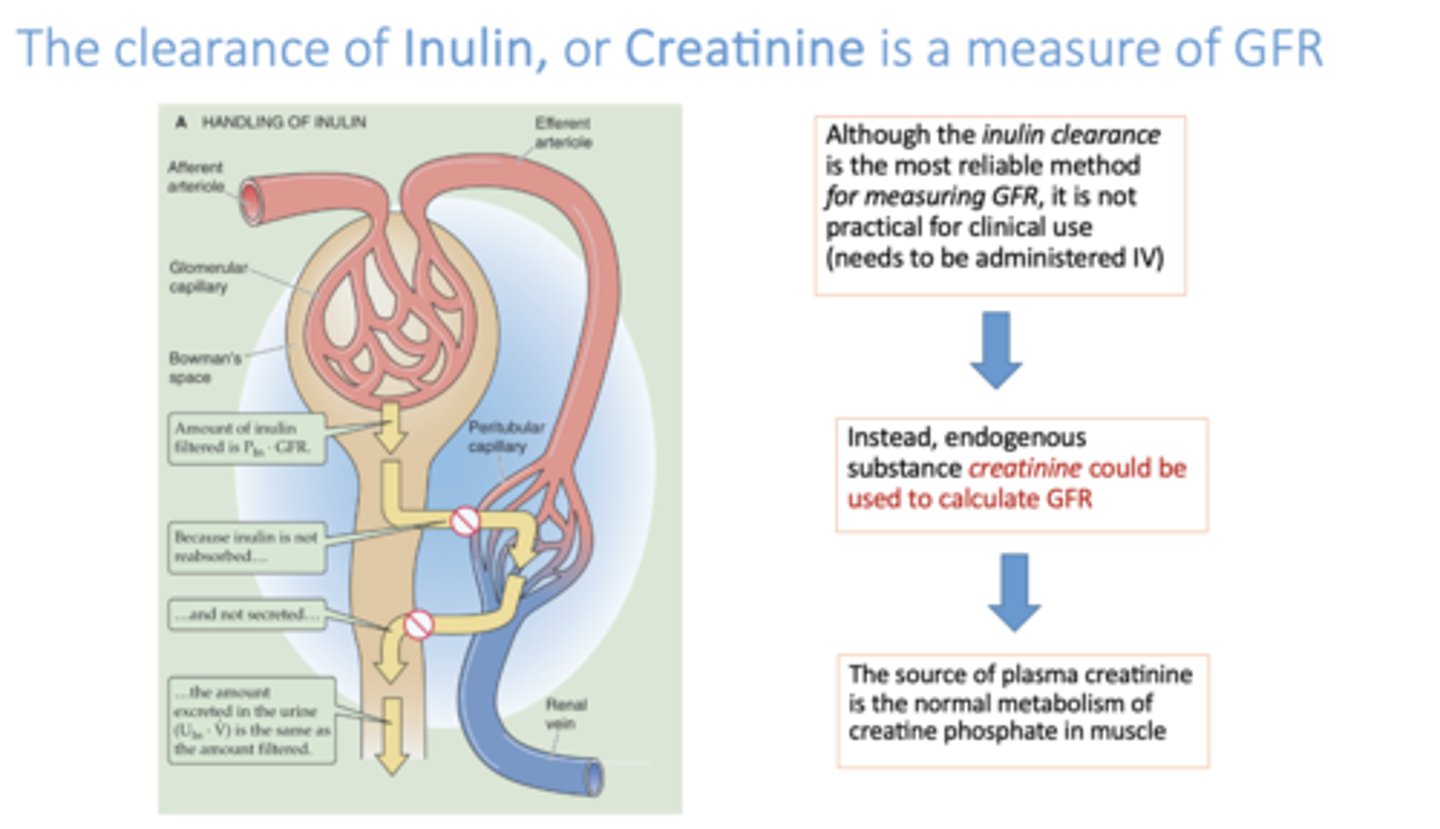
in a healthy patient, there is a ______ relationship between creatinine levels and excretion of creatinine
direct
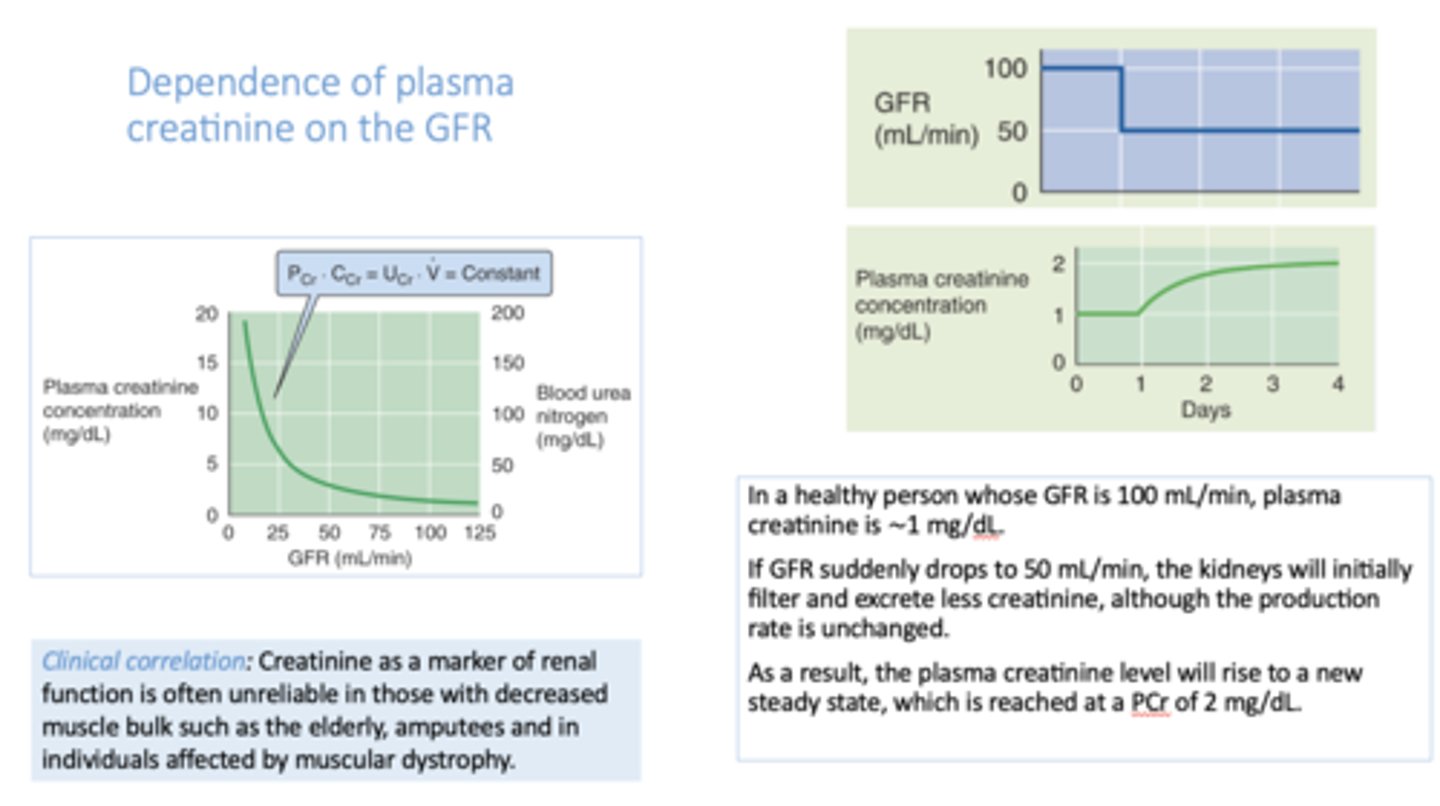
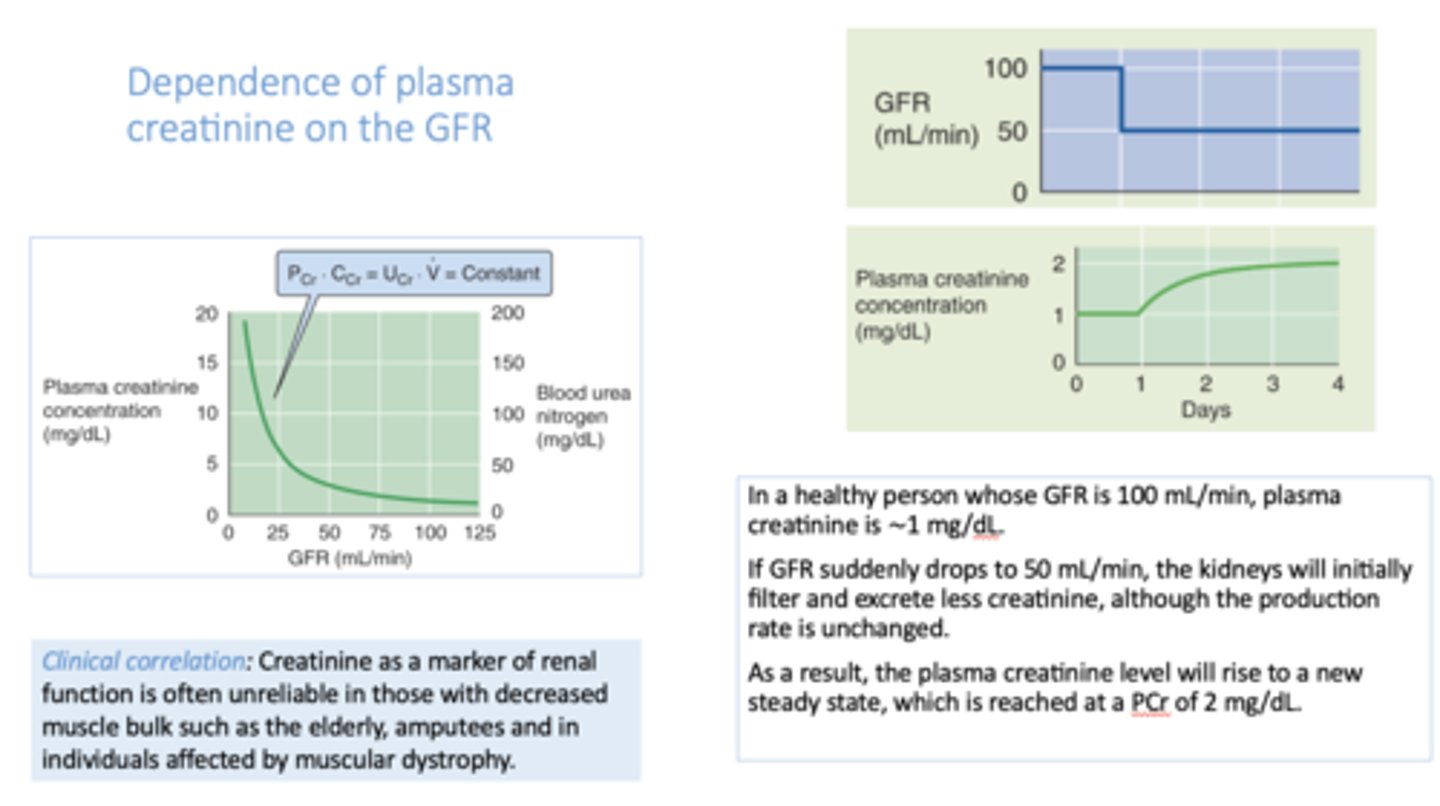
there is a _________ relationship between glomerular filtration rate (GFR) and plasma creatinine concentration
inverse
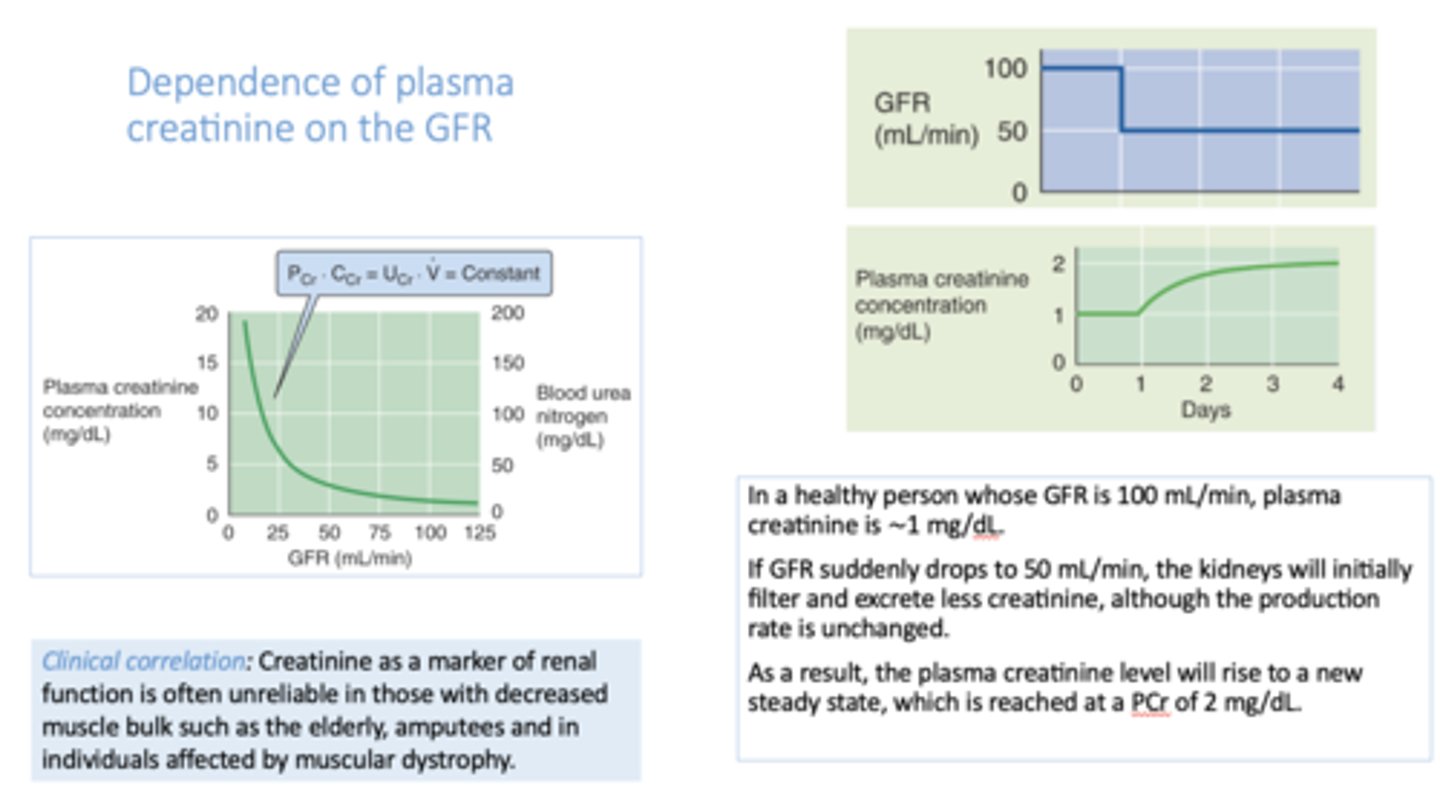
if GFR increases, plasma [creatinine] will ________
decrease
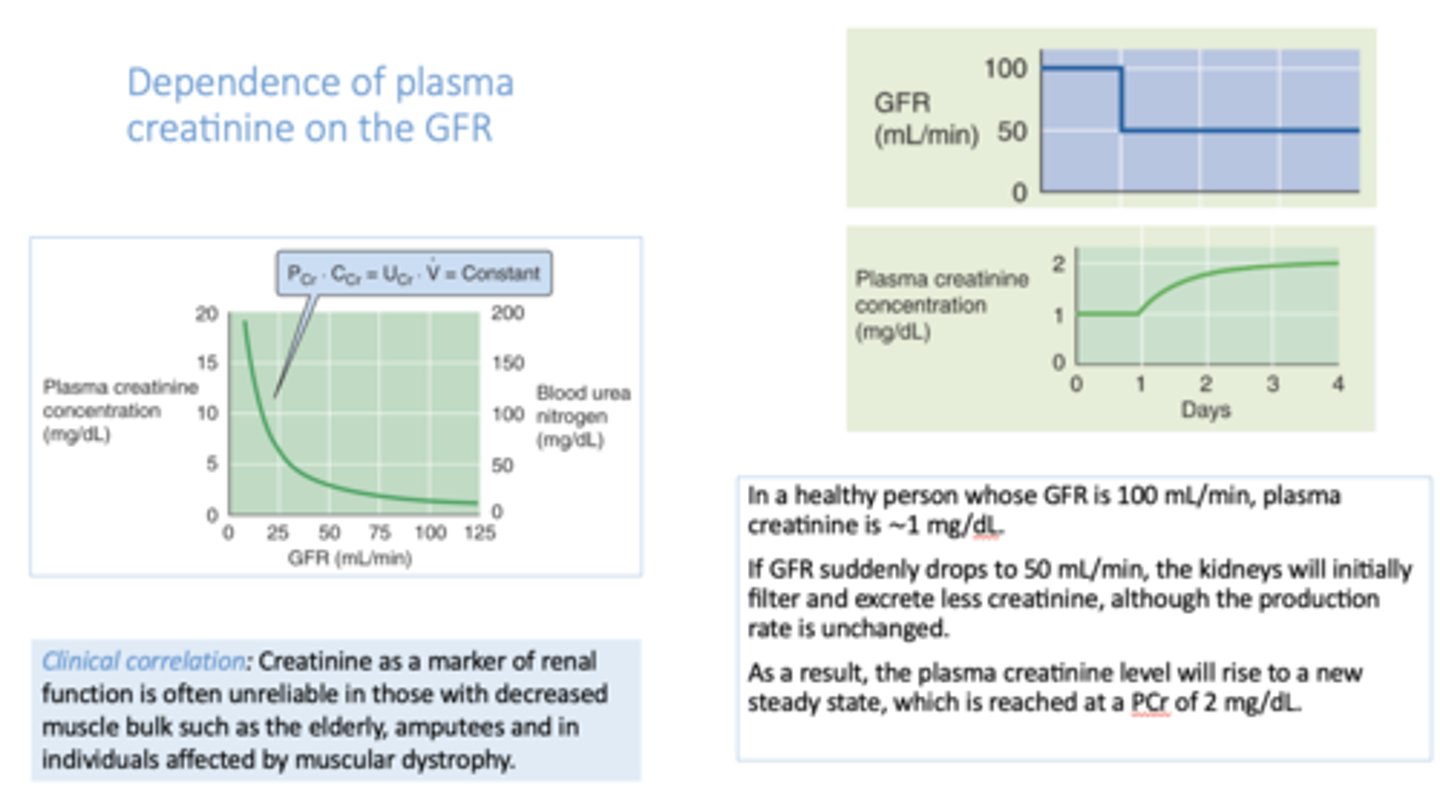
if GFR decreases, plasma [creatinine] will ________
increase
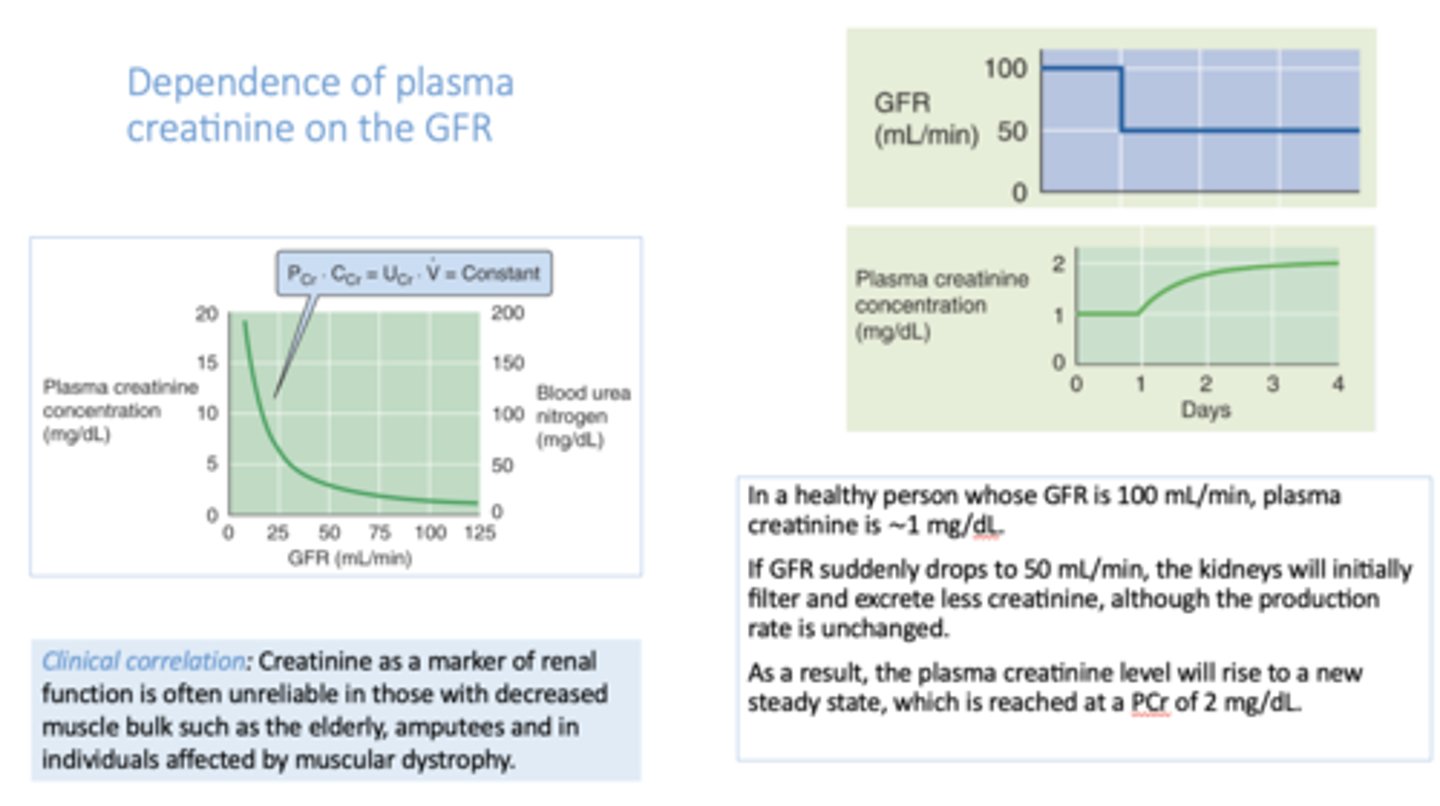
if GFR decreases by 50%, plasma [creatinine] will
double
The sieving coefficient for the solute X, depends on:
molecular weight and radius
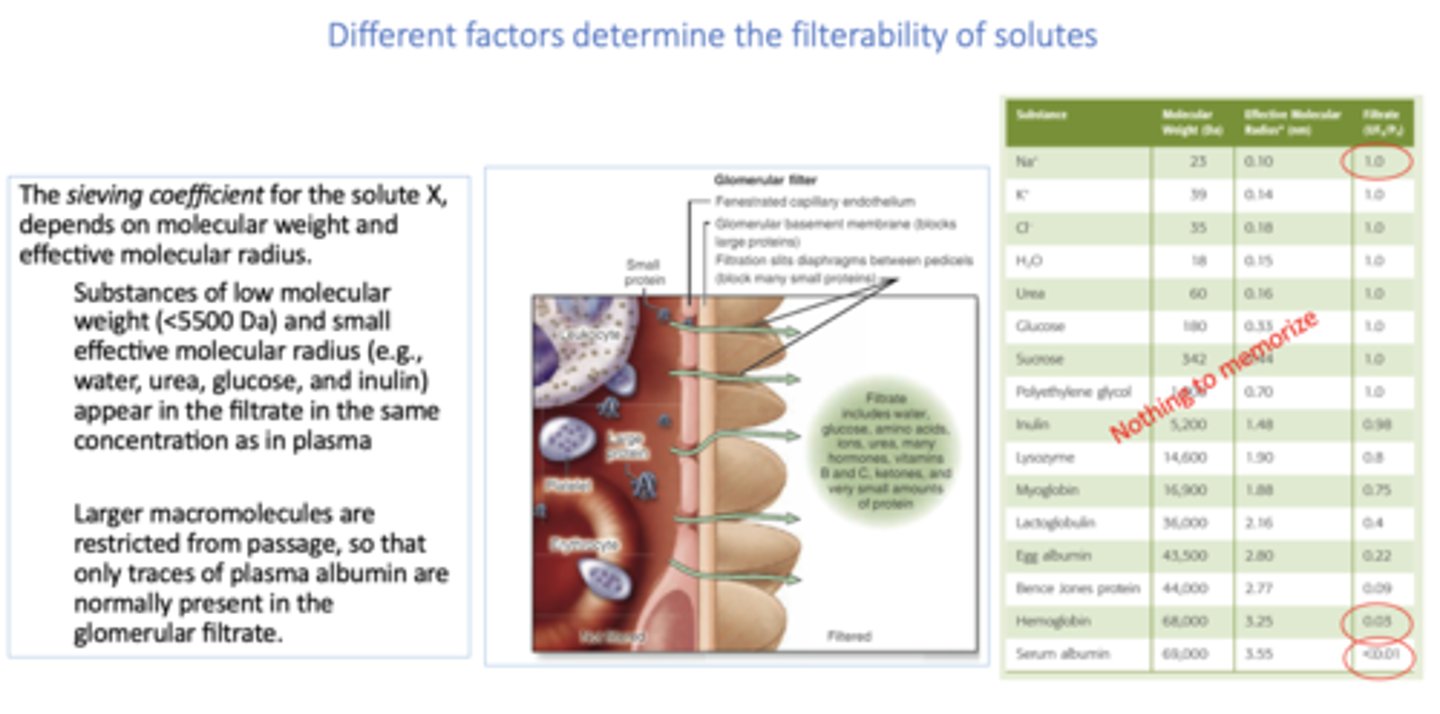
T/F: Substances of low molecular weight (<5500 Da) and small effective molecular radius (e.g., water, urea, glucose, and inulin) appear in the filtrate in the same concentration as in plasma
True
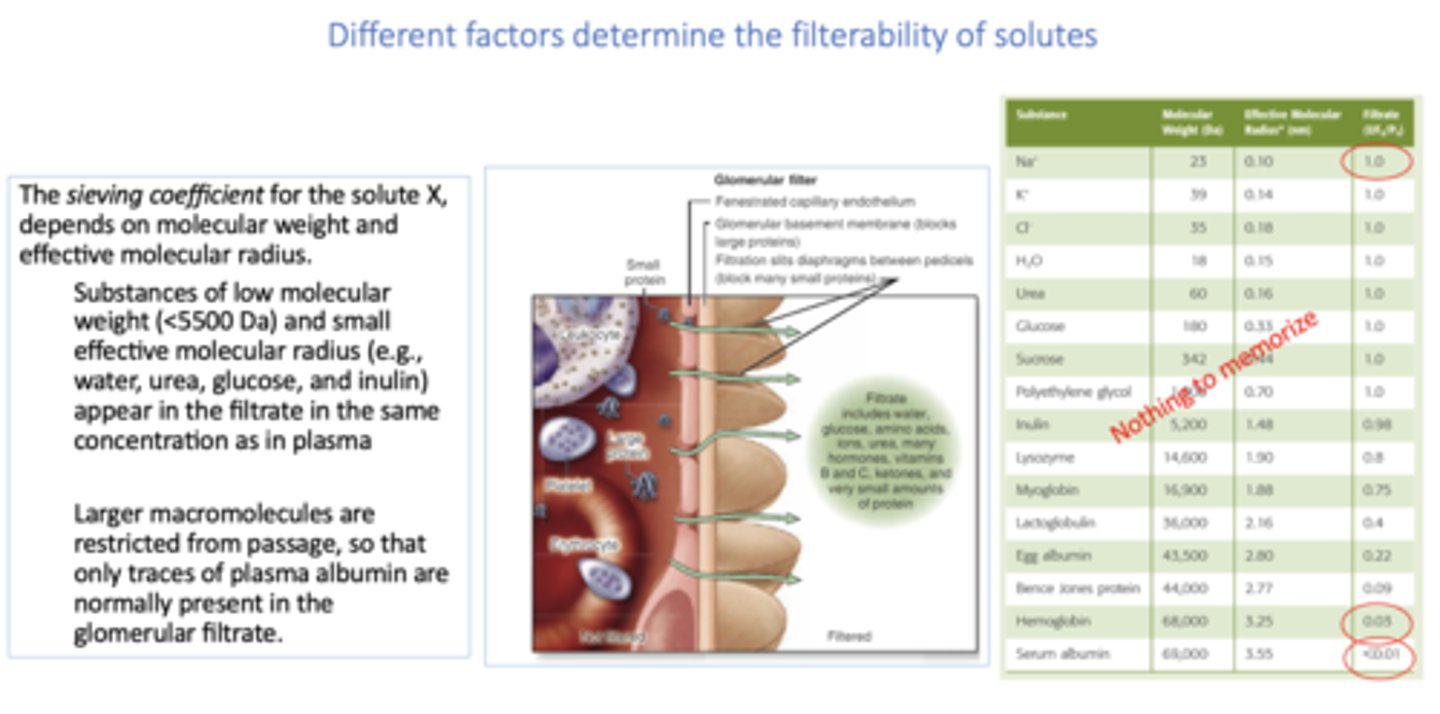
T/F: Larger macromolecules are restricted from passage, so that only traces of plasma albumin are normally present in the glomerular filtrate.
True
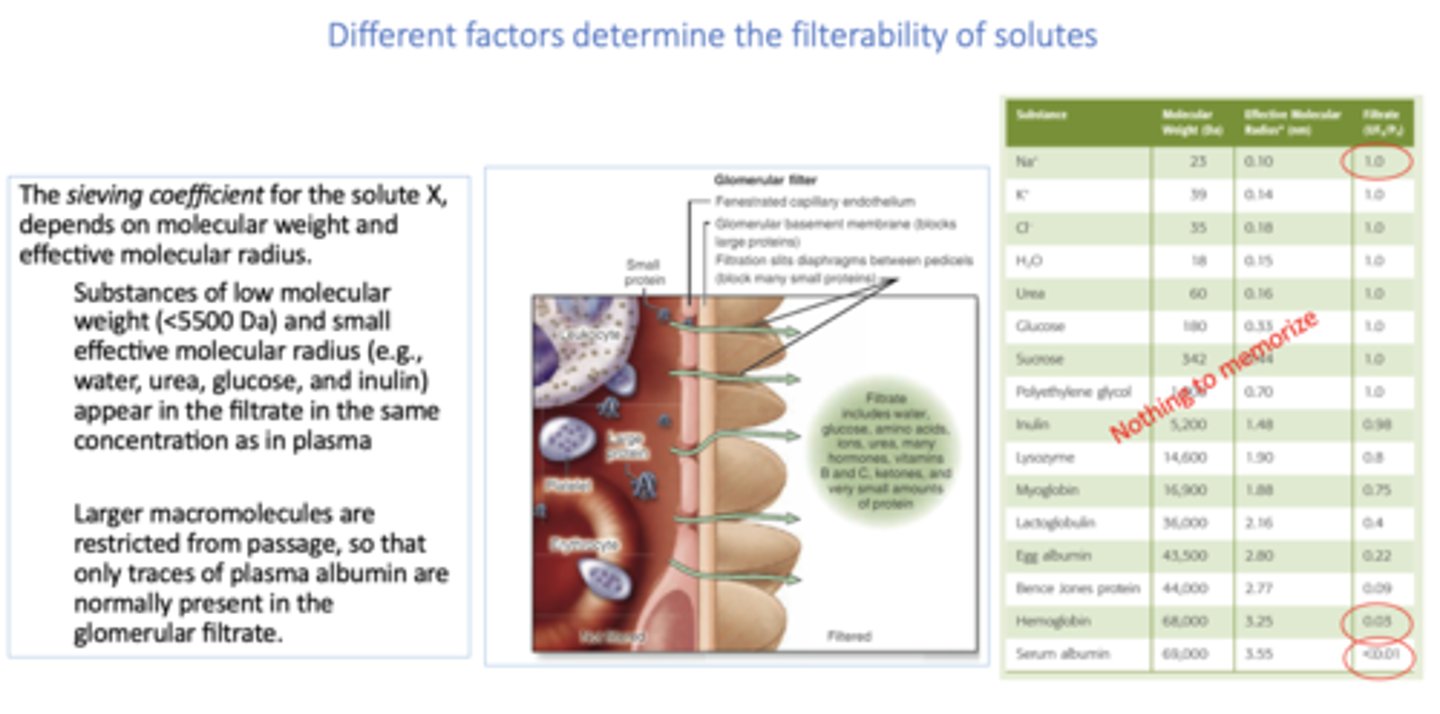
all of the following are present in glomerular filtrate except:
- water
- albumin
- Na+
- glucose
- urea
albumin
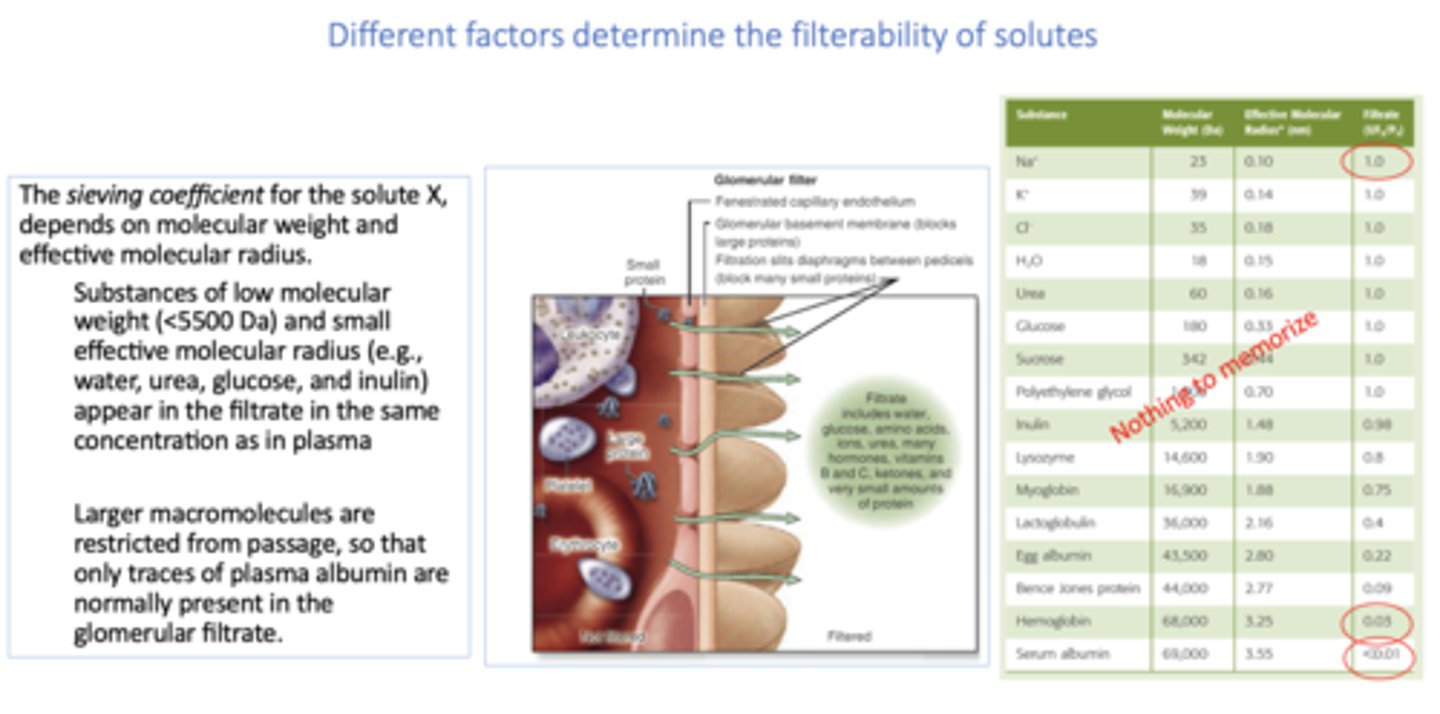
all of the following are present in glomerular filtrate except:
- Cl
- hemoglobin
- K+
- glucose
- urea
hemoglobin
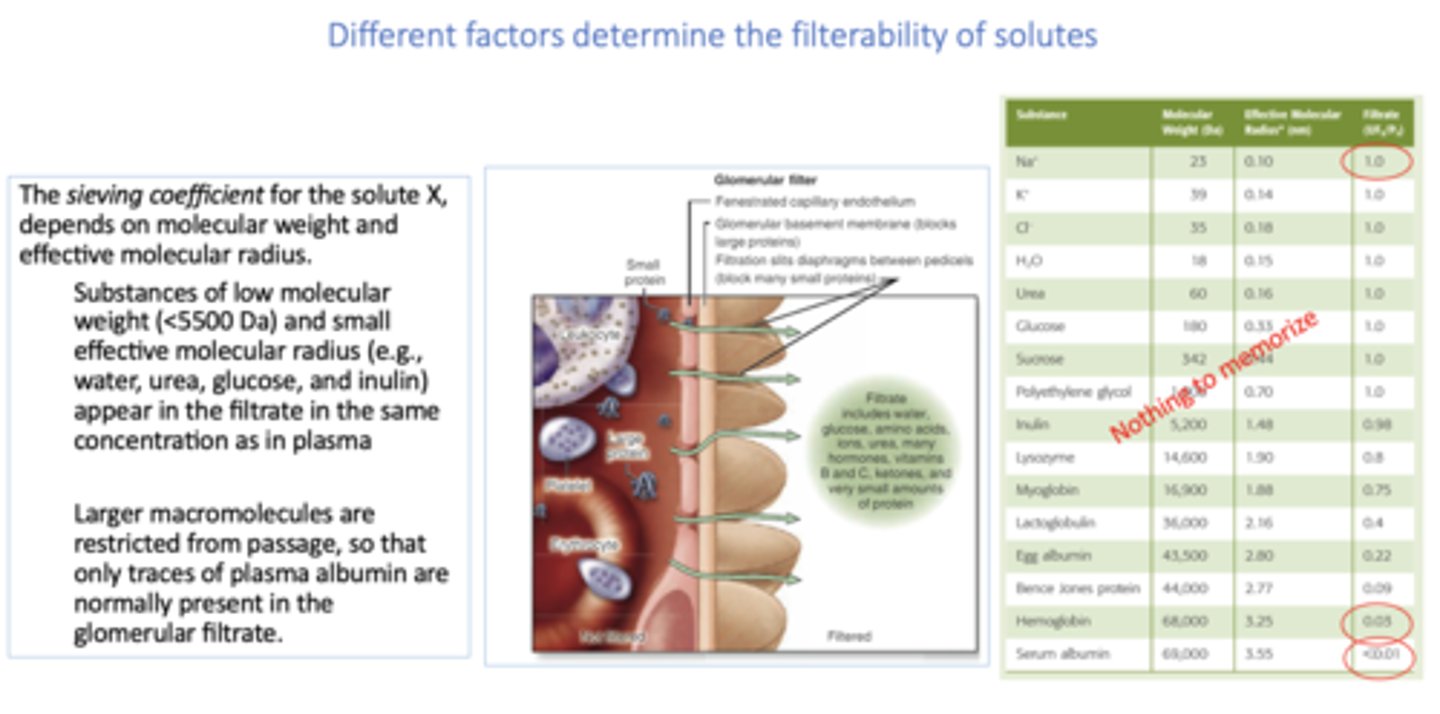
What determines the filterability of solutes across the glomerular filtration barrier?
Molecular size, charge, and shape

_________ dextrans are restricted from filtration
anionic

_________ dextrans pass more readily into the filtrate
cationic

________ dextrans with an effective molecular radius <2nm pass readily across the glomerular barrier
Neutral

In cases of _________________, glomerular barrier loses its negative charge, the permeability of the barrier to negatively charged macromolecules is enhanced. Proteins leak into ultrafiltrate, may appear in the urine
glomerulonephritis

In cases of glomerulonephritis, glomerular barrier loses its _________ resulting in proteinuria (proteins in urine) b/c the permeability to negatively charged macromolecules is enhanced
negative charge

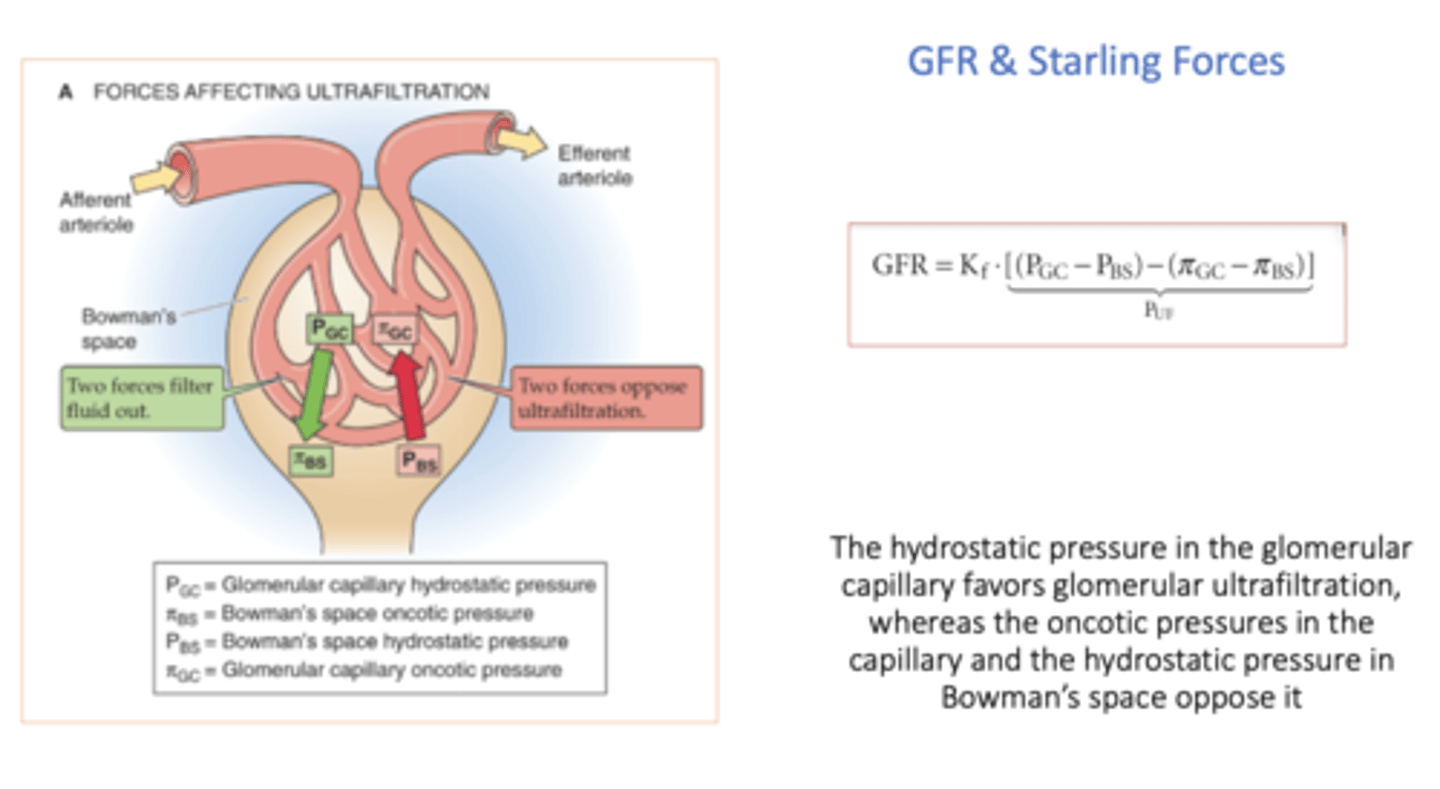
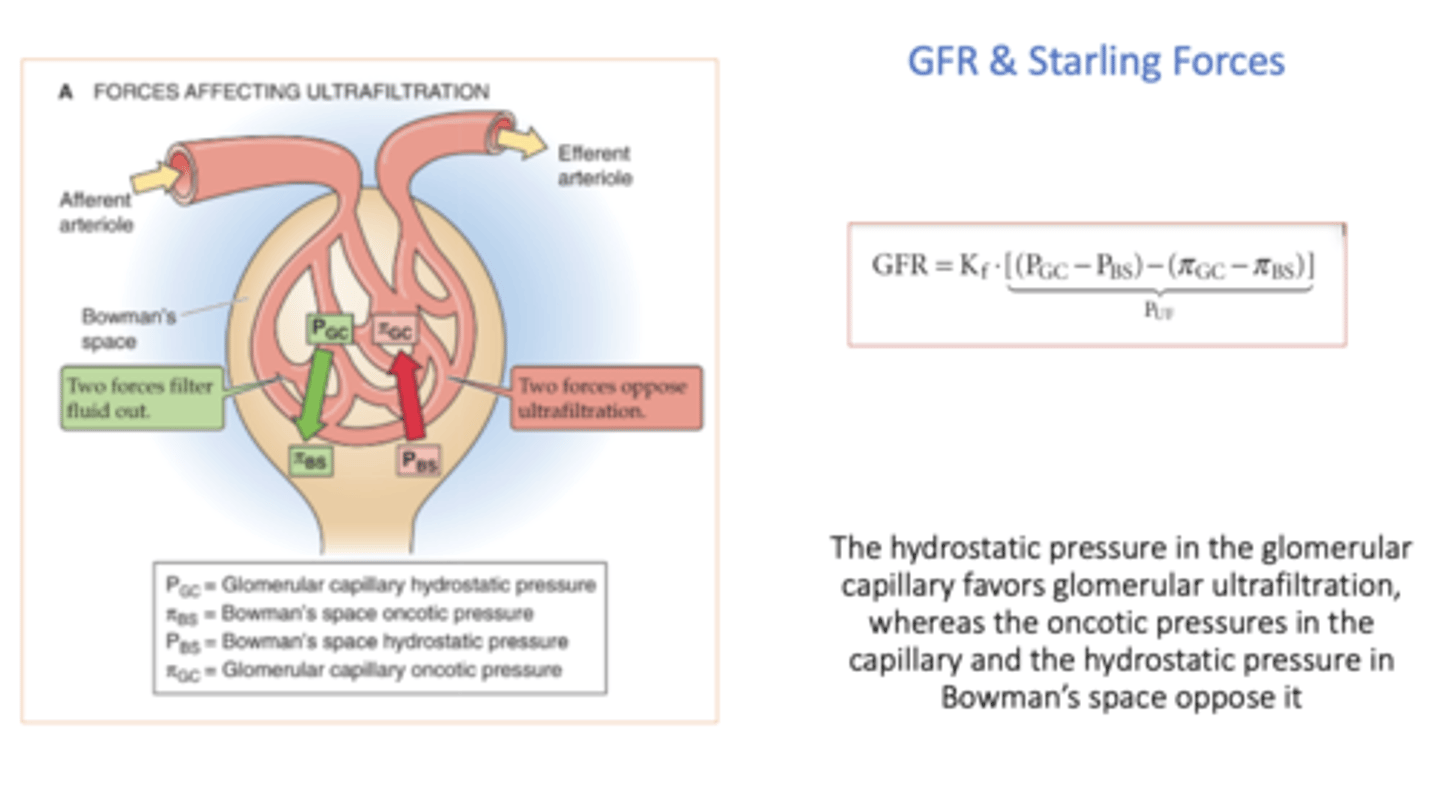
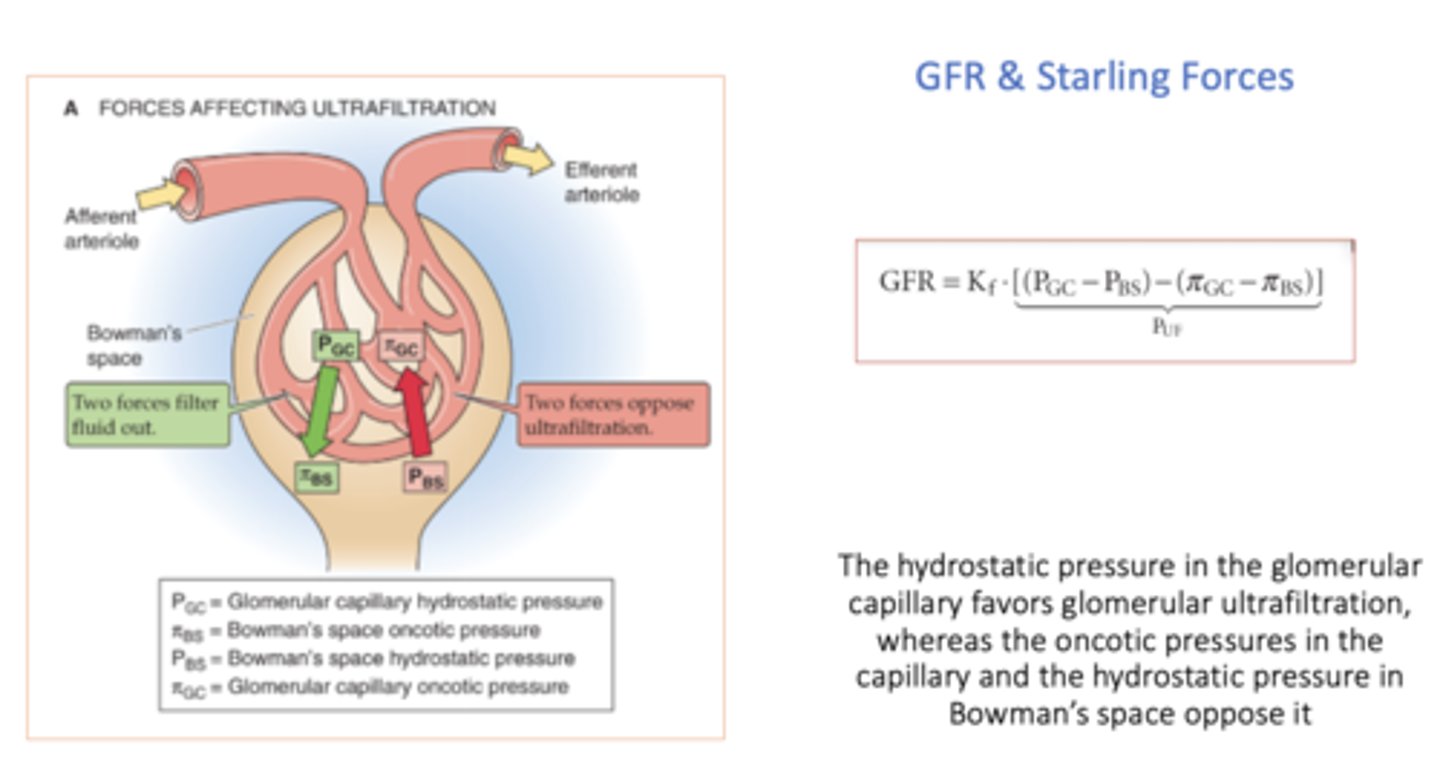
hydrostatic pressure in the glomerular capillary _______ (favor or oppose?) glomerular ultrafiltration
favors
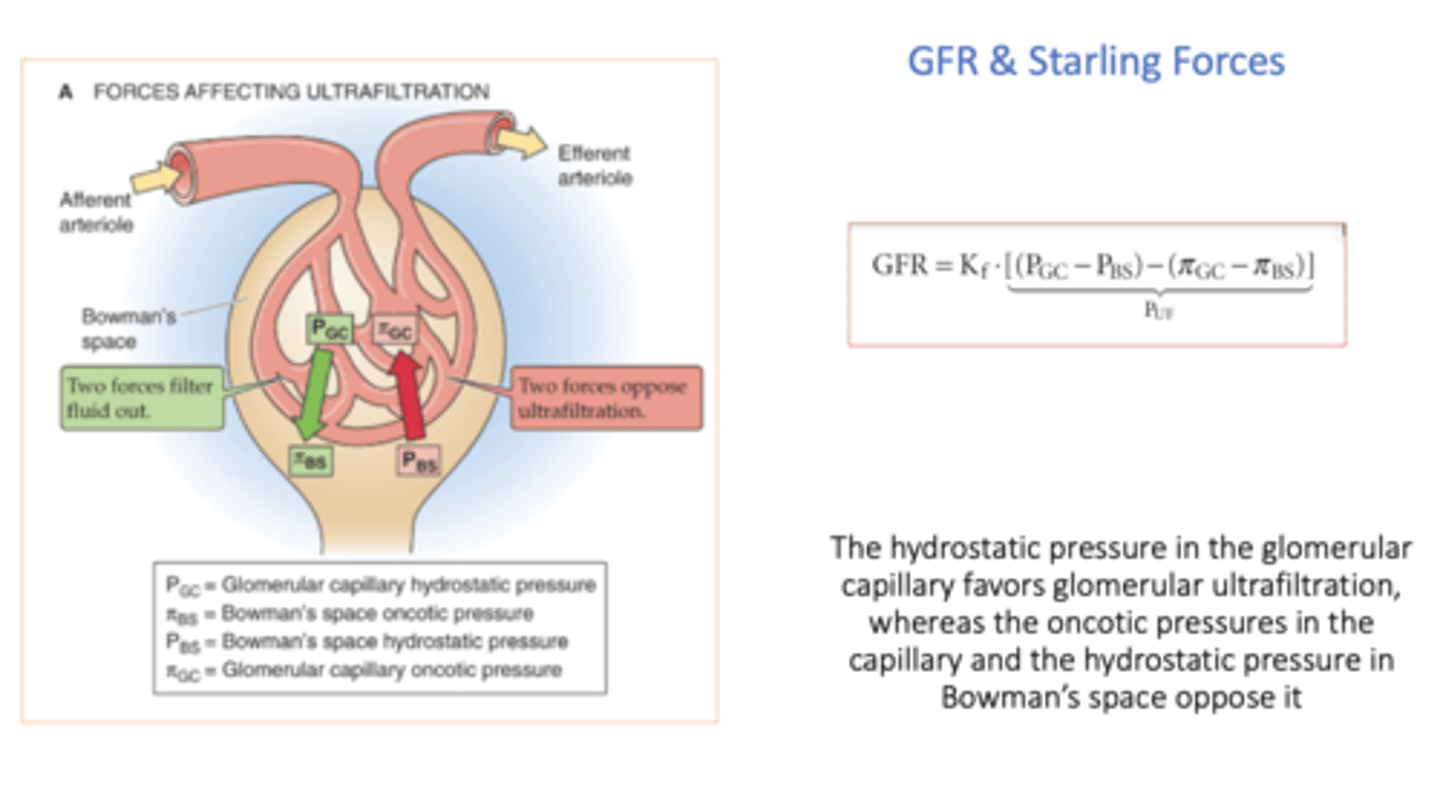
oncotic pressure in Bowman's space _______ (favor or oppose?) glomerular ultrafiltration
favor (but it is usually 0)
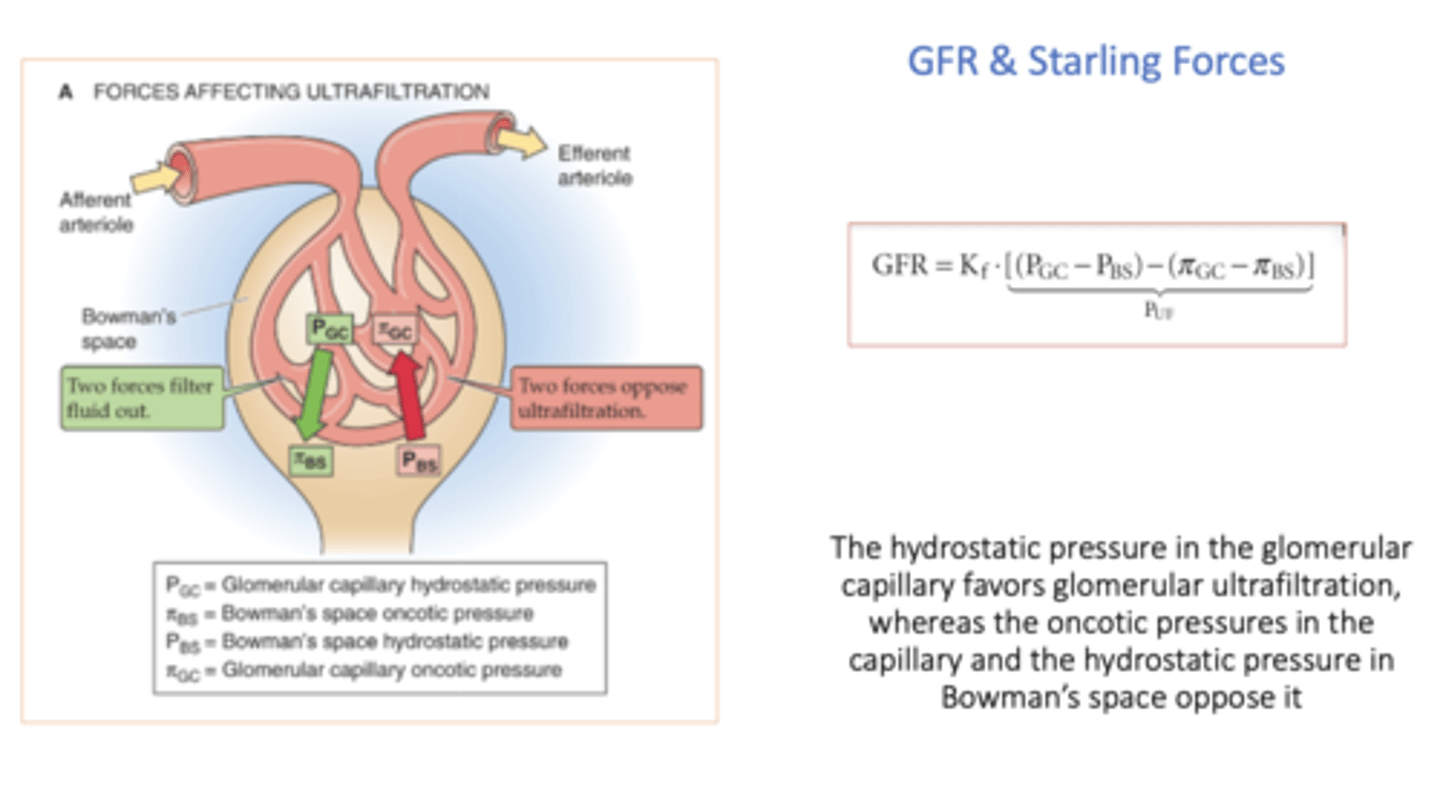
oncotic pressures in the capillary _______ (favor or oppose?) glomerular ultrafiltration
opposes
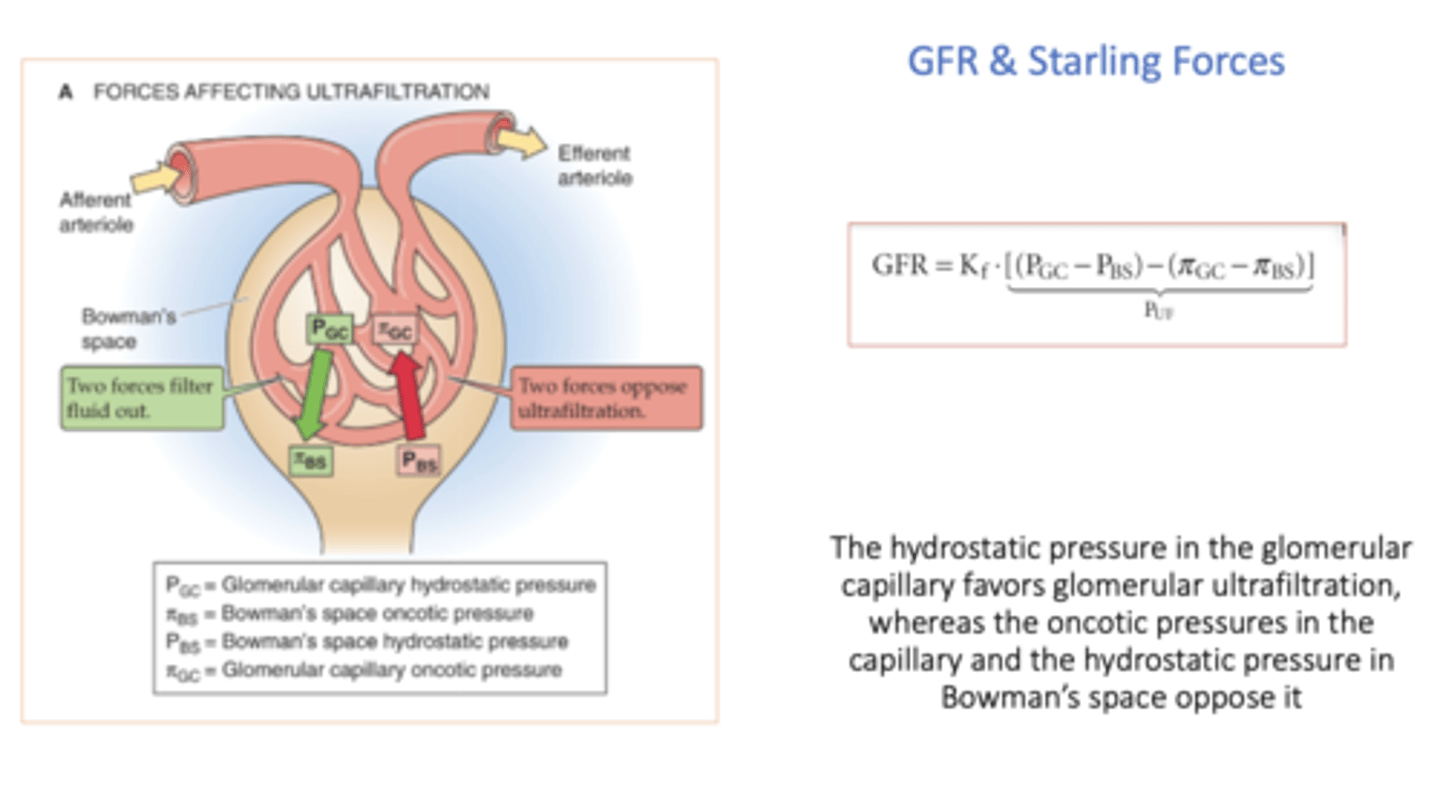
hydrostatic pressure in Bowman's space _______ (favor or oppose?) glomerular ultrafiltration
opposes
Increased glomerular plasma flow leads to a __________ in glomerular filtration rate
increase
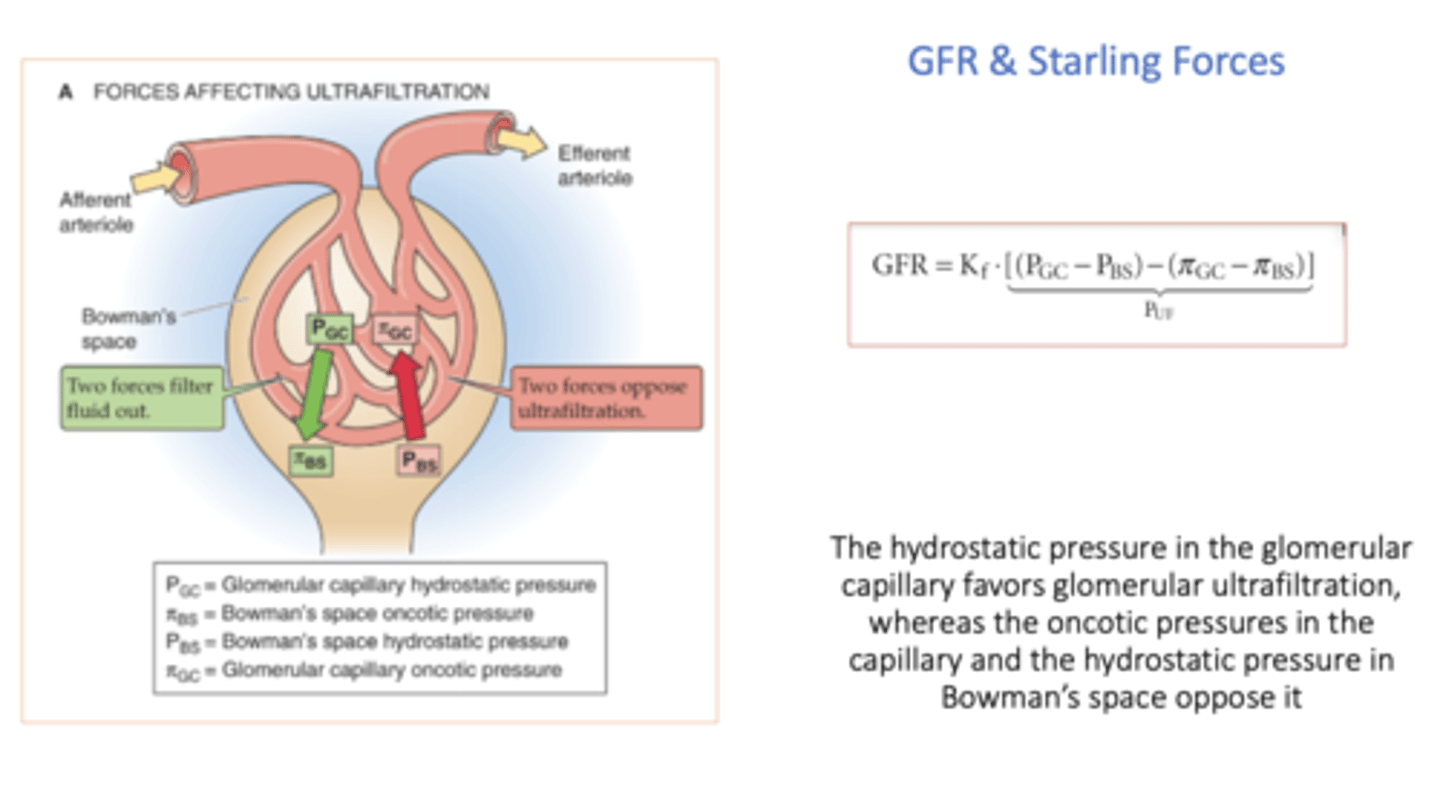
What is the normal oncotic pressure in the Bowman's space?
0
To approximate human net filtration pressure, several animal subjects were instrumented with Milar pressure transducers. Blood pressure averages 120/80 mm Hg, with a glomerular capillary hydrostatic pressure of 60 mm Hg. Serum creatinine and albumin levels are normal. Blood and albumin are absent from the urine. On average, oncotic pressure in the glomerular capillary is 21 mm Hg and hydrostatic pressure in the Bowman's capsule is 15 mm Hg. Based on this data, what is the net filtration pressure?
a. 15 mm Hg
b. 21 mm Hg
c. 24 mm Hg
d. 54 mm Hg
c. 24 mm Hg (understand calculation w/ different numbers!!!!!!)

What is the "normal" renal plasma flow (RPF)?
600 mL/min

Renal blood flow (RBF) is ________ out of the total cardiac output of 5 L/min.
1 L/min

equation for Renal Blood Flow (RBF):
RPF/(1-Hct)

equation for Renal Plasma Flow (RBF):
(1-Hct) x RBF

T/F: Increased glomerular plasma flow leads to an increase in glomerular filtration rate.
True

equation for net plasma filtration pressure (Puf):
(Pgc - Pbs) - (πgc - πbs)
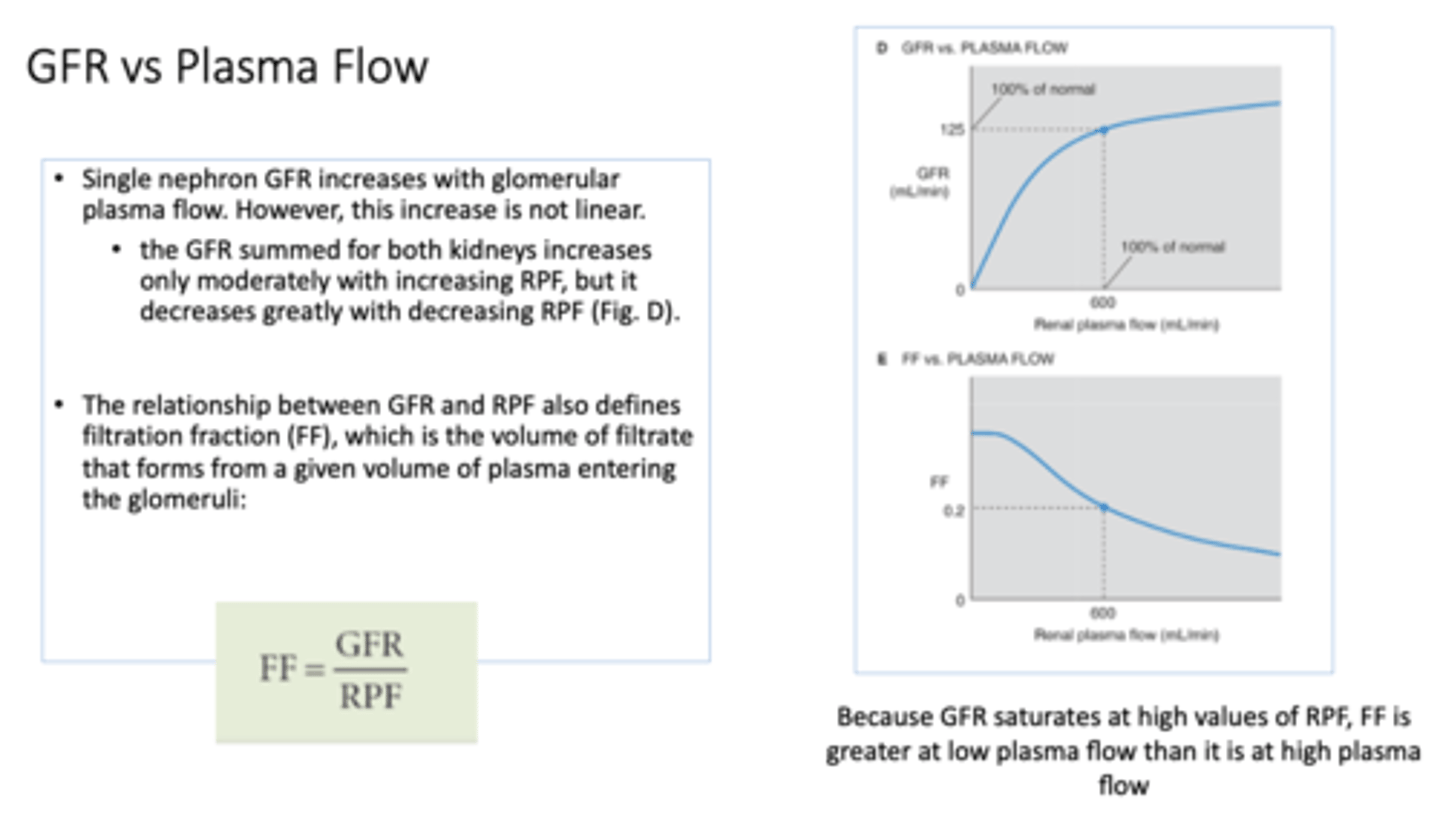
equation for filtration fraction:
GFR/RPF
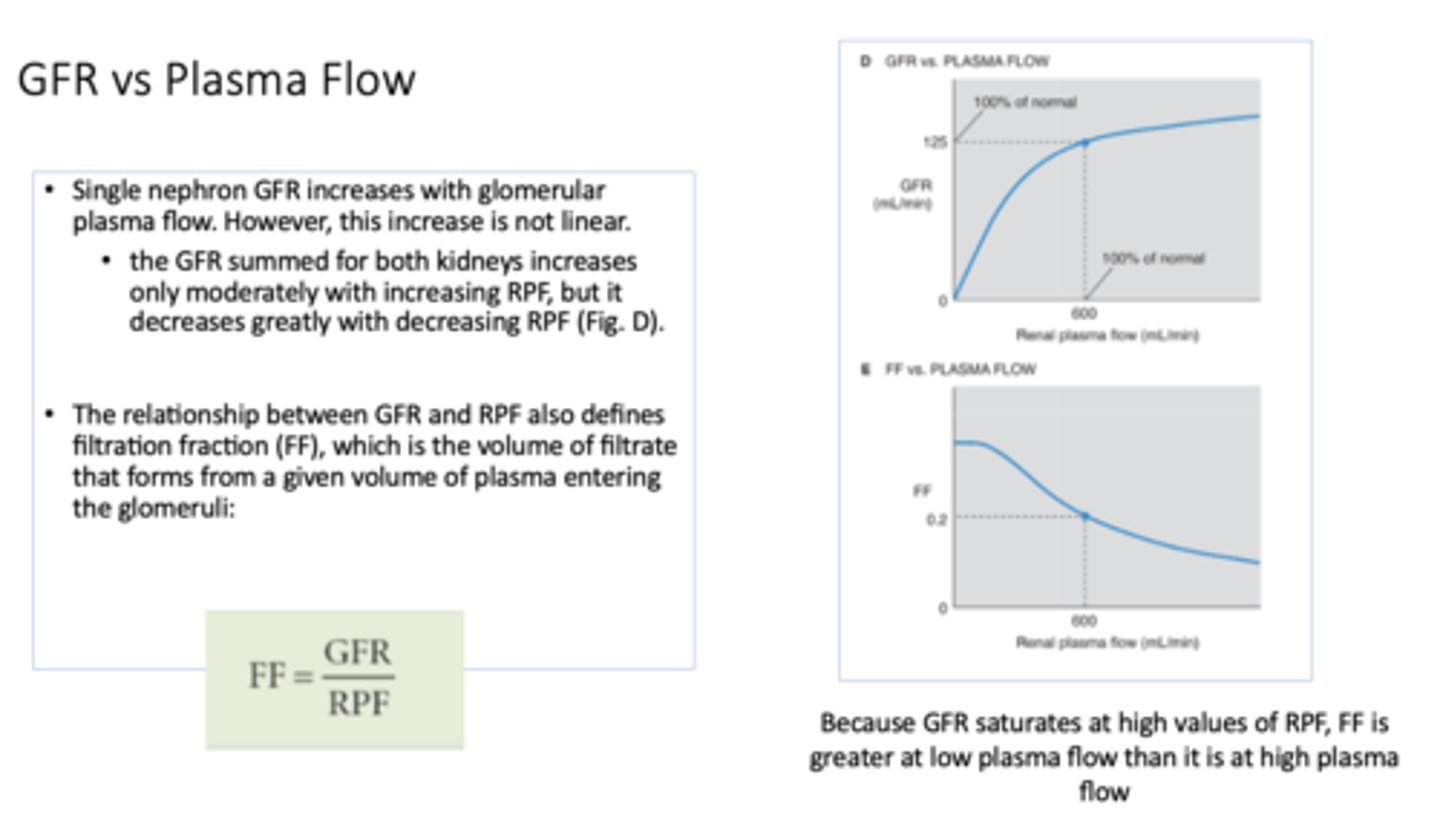
Define the following:
The volume of filtrate that forms from a given volume of plasma entering glomeruli
filtration fraction
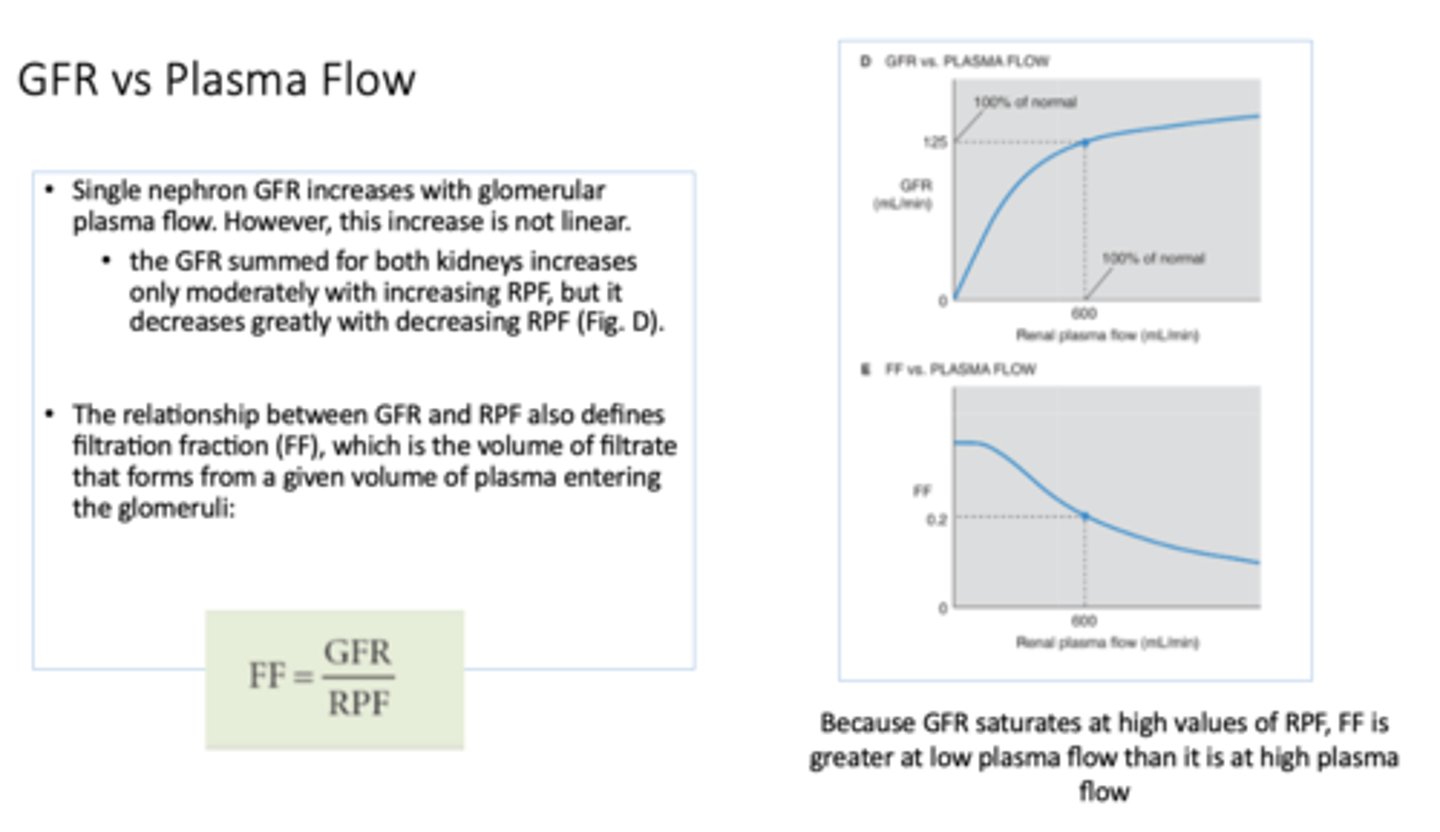
Because GFR saturates at __________ values of RPF, FF is greater at low plasma flow than it is at high plasma flow
High
_____________ govern the flow of fluid across the capillary walls in the glomerulus and result in net filtration
Starling forces