Final questions part 2
1/43
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
44 Terms
Risk factor of cardiac tamponade
Myocarditis and pericarditis
You suspect cardiac tamponade, your patient has a decrease of 10mm Hg or more in systolic BP during inspiration, this is known as?
Pulsus paradoxus
Cardiac Tamponade
Beck's Triad: hypotension, elevated
systemic venous pressure (jugular venous
distension), muffled heart sounds
Pulsus Paradoxus: a decrease of 10 mm
Hg or more in systolic BP during
inspiration, a physical exam finding
signaling pericardial effusion is causing
cardiac tamponade
ACTION: Notify provider, administer IV fluid for hydration and increasing BP, chest Xray or Echo, ECG, pericardiocentesis procedure to drain fluid, monitor hemodynamic pressures, heart rhythm,
and reoccurrence after removal of fluid.
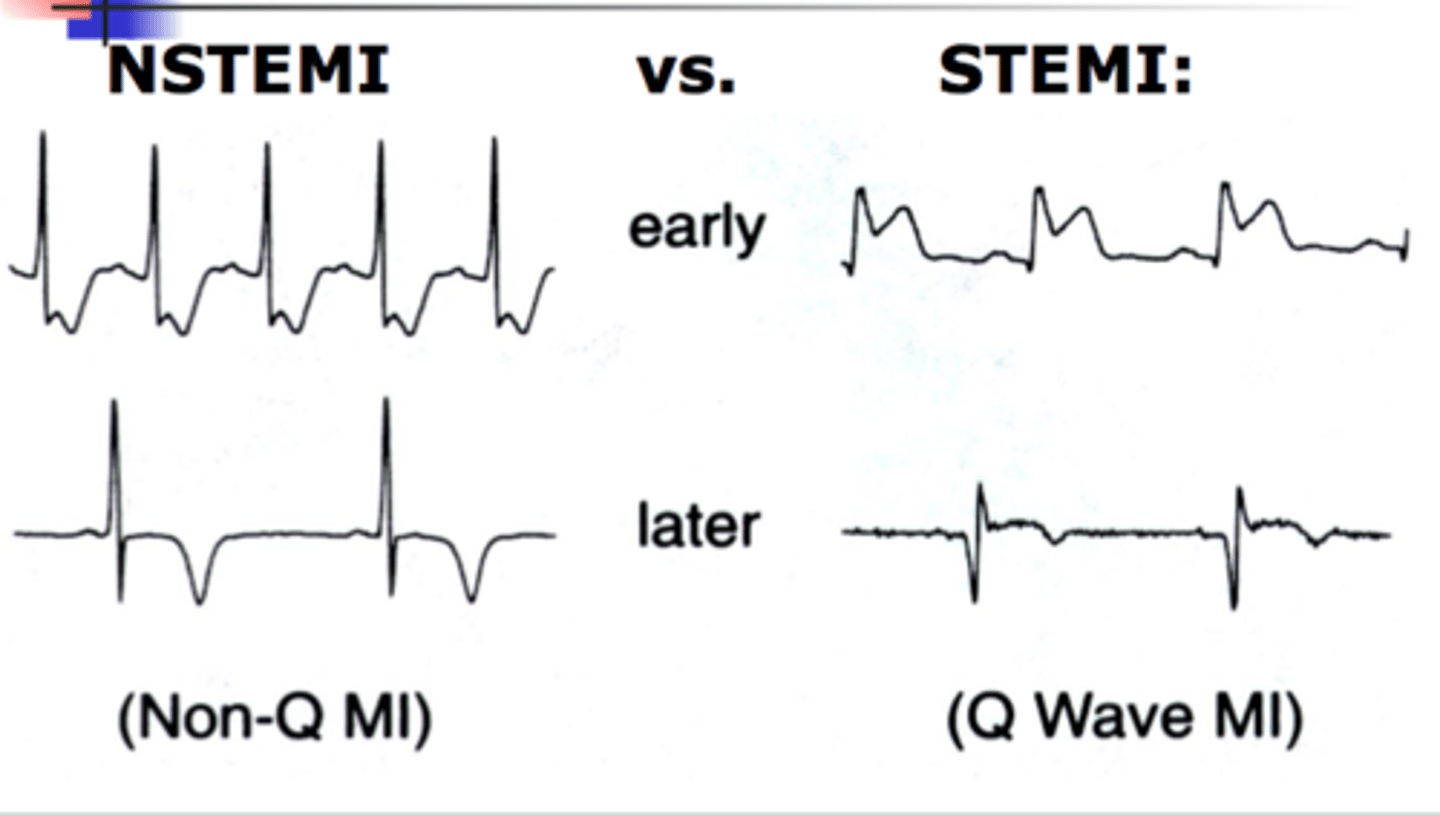
Widespread distribution of ST elevation often are related to?
Widespread, concave ST elevation across multiple leads is the hallmark sign of Acute Pericarditis.
Covid-19 increased the development of Myocarditis which leads to whatadditional complication?
COVID-19-induced Myocarditis (inflammation of the heart muscle) often leads to Heart Failure and Cardiogenic Shock
A decrease of 10mm Hg or more in systolic BP during inspiration indicates?
Pulsus Paradoxus.
What it Indicates: It is a classic sign of Cardiac Tamponad
To reduce risk for cardiac inflammatory disorders prevention includes?
Prophylactic Antibiotics: Especially before dental procedures for patients with a history of valve issues or previous endocarditis. 🦷💊
Prompt Treatment of Infections: Treating "Strep throat" or skin infections immediately to prevent the bacteria from traveling to the heart (Rheumatic Heart Disease).
Vaccinations: Staying up to date on vaccines (like the flu and COVID-19) to prevent viral infections that could trigger myocarditis.
Hand Hygiene and Wound Care: Preventing the entry of bacteria into the bloodstream (especially in patients with IV drug use history).
A nurse is caring for a patient with PAD after an arterial revascularization surgery. What would the nurse monitor for?What are signs that the blood flow has increased?
Bleeding and Hematoma: Check the incision site (often in the groin) for any firmness, swelling, or active bleeding.
Graft Occlusion (The #1 Emergency): Monitor for a sudden disappearance of pulses, increased pain, or coolness in the limb. If the graft clots off, the patient needs to go back to surgery immediately!
check Blood Pressure
Compartment Syndrome: Monitor for severe edema, "pain out of proportion" to the injury, and tenseness in the muscle.
What are signs ofa wound infection?
Localized induration
- Warmth
- Tenderness
- Erythema
- Edema
- Purulent drainage
- Elevated WBC
(Normal WBC: 4500-11000 per mm) Use sterile technique when providing wound care!
Think of 3 risk factors for VTE? Name one intervention for hospitalized patients to preventVTE? What are signs of VTE?
Risk factors: surgery, Immobility, Age
One Intervention: Early ambulation, SCDs (Sequential Compression Devices), Prophylactic Anticoagulants: Low-dose Heparin or Enoxaparin (Lovenox).
signs of VTE; Unilateral Swelling,
Warmth and Redness,
Pain or Tenderness
D-Dimer Lab Test
protein fragment that is made when blood clot dissolves in the body(fibrinolysis). A positive test indicates higher than normal levels and that a clotting conditionis present.
What is the one intervention you would NOT perform when caring for a patient with DVT?
Don't even think about massaging
Diet and warfarin - what types of food should youpatient avoid?
Patients should avoid (or be very consistent with) foods high in Vitamin K.
Specific Foods: Green leafy vegetables like spinach, kale, and broccoli.
List 3 risk factors for PE
Immobility/Post-Op Status
Long Bone Fractures
Obesity & Pregnancy
Use a calm, reassuring approach and do not leave the patient alone.
Name two clinical manifestations of PE?
Sudden Onset Dyspnea
Tachycardia & Hypotension
Bonus: Pleuritic Chest Pain (sharp pain when breathing in).
A nurse is caring for a client who has chronic venousinsufficiency and a prescription for thigh-highcompression stockings. Which of the following actionsshould the nurse take?
Apply the stockings in the morning upon awakeningand before getting out of bed
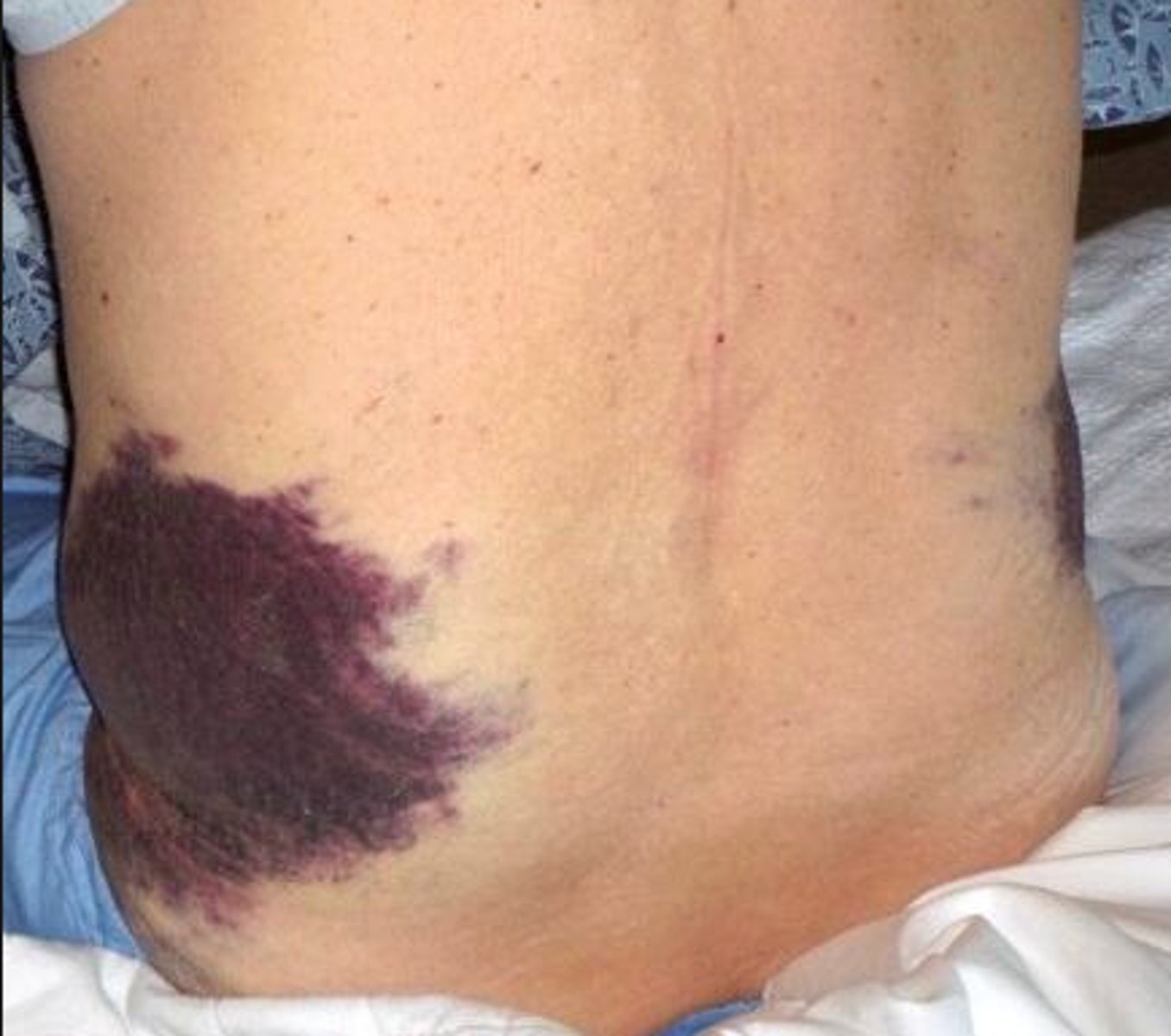
Clinical Manifestation of AAA? vs Discharge education for AAAw/graft
AAA manifestation: Petechiae on axilla
Educ- Strict BP control with set parameters
When should TEDS be applied? vs
- Most common complaint for
PAD
In am prior to getting OOB-
PAD complaint: Intermittent claudication
PVD s/s vs varicose veins
Burning sensation in thighs/calves,
itchy dry skin, moderate symmetrical
BLE swelling.
- Enlarged twisted superfiscal veins
mostly in legs
Two hours later, the patient is admitted to the medical unit where she is started on a continuous IV heparin weight-based protocol. Which finding indicates that the heparin infusion is therapeutic?
A. INR is less than 1.
B. INR is between 2 and 3.
C. aPTT is the same as the control.
D. aPTT is 1.5 to 2.5 times the control.
D
Who is at risk of hypovolemic shock
Trauma, Burns, DKA, Surgical fluid loss, OBGYN
angiodema
If tongue, lips mouth or throat swelling occur or dyspnea, seek emergency care...
• Life-threatening if swelling of tongue or throat blocks the airway
Treatment: Epinephrine for severe angioedema Antihistamines (
Sepsis guidelines
1) Measure lactate level.Measure
2) *Obtain blood cultures before administering antibiotics.
3) Administer broad-spectrum antibiotics.
4) Begin rapid administration of 30mL/kg crystalloid for hypotension or lactate ≥4 mmol/L.
5) Apply vasopressors if hypotensive during or after fluid resuscitation to maintain a mean arterial pressure ≥ 65 mm Hg.
*Remeasure lactate if initial lactate elevated (> 2 mmol/L).Remeasure
Quick Review of Shock Types
Hypovolemic: Not enough "fluid" (blood or water loss).
Cardiogenic: The "pump" (heart) is broken.
Distributive: The "pipes" (vessels) are too wide (includes Sepsis, Anaphylaxis, Neurogenic).
Obstructive: A physical "blockage" (like a PE or Tension Pneumothorax).
For anaphylactic shock what is the drug of choice? Route?
Epinephrine via IM (Intramuscular) injection (usually in the lateral thigh).
Manifestations of hemodynamic shock?
Tachycardia (Heart Rate > 100 bpm)
Hypotension (Low Blood Pressure)
Decreased Urine Output (Oliguria) 🚽
MODS is common with what type of shock? and septic shock is associated with what?
MODS (Multiple Organ Dysfunction Syndrome): This is most common with Septic Shock. When sepsis goes untreated, it triggers a body-wide inflammatory response that causes organs to fail.
Septic Shock Association: It is heavily associated with DIC (Disseminated Intravascular Coagulation), especially in the late or "refractory" stage where the patient starts bleeding from sites like IVs or catheters.
The nurse calls the health care provider to report the abnormal findings. The
provider orders
A. Tylenol 650 mg PO prn q6h for temp above 101º F
B. Blood cultures × 2, 5 minutes apart
C. C&S of abdominal wound drainage
D. Vancomycin 750 mg IVPB over 1 hour every 24 hour
In what order should the nurse implement these interventions?
C, B, D, A
Within 30 minutes of the patient's transfer to the ICU, his condition continues todeteriorate. His SaO2 continues to fall, RR is 36/min, and the ICU nurse notes thatthere is blood oozing around his IV catheter sites. A Foley catheter isplaced, and his urine output is minimal.What is the nurse's interpretation of these assessment findings?
The patient is going into severe sepsis.
The main manifestations are low
oxygen saturation, rapid respiratory rate, decreased to absent urine output,
and changes in cognition. He is at risk for septic shock. The blood oozing
around his IV catheters may indicate the presence of DIC.
When assessing a patient for shock, the nurse knows that which symptom is
the earliest manifestation of shock?
A. Anuria
B. Increased heart rate
C. A decrease in respiratory rate and depth
D. A change in both systolic and diastolic blood
pressure
B. Increased heart rate
A 37-year-old male is admitted with a severely abscessed tooth, BP 90/42, HR 136, RR 28, SpO2 90% on room air, temperature 38.7º C. The nurse suspects that the patient has developed sepsis.
What is the priority nursing intervention?
A. Insert an indwelling urinary catheter.
B. Initiate intravenous fluid resuscitation.
C. Obtain a complete chemistry for laboratory analysis.
D. Administer prescribed antibiotics prior to blood cultures.
K
B. Initiate IV fluid ressuscitation
ABGs
ABG Measure Expected Ref Range
pH 7.35-7.45 (low pH= acidosis, high pH =alkalosis)
PAO2 80-100 mm Hg
PACO2 35-45 mm Hg
HCO3 21-28 mEq/L
SAO2 95%-100%
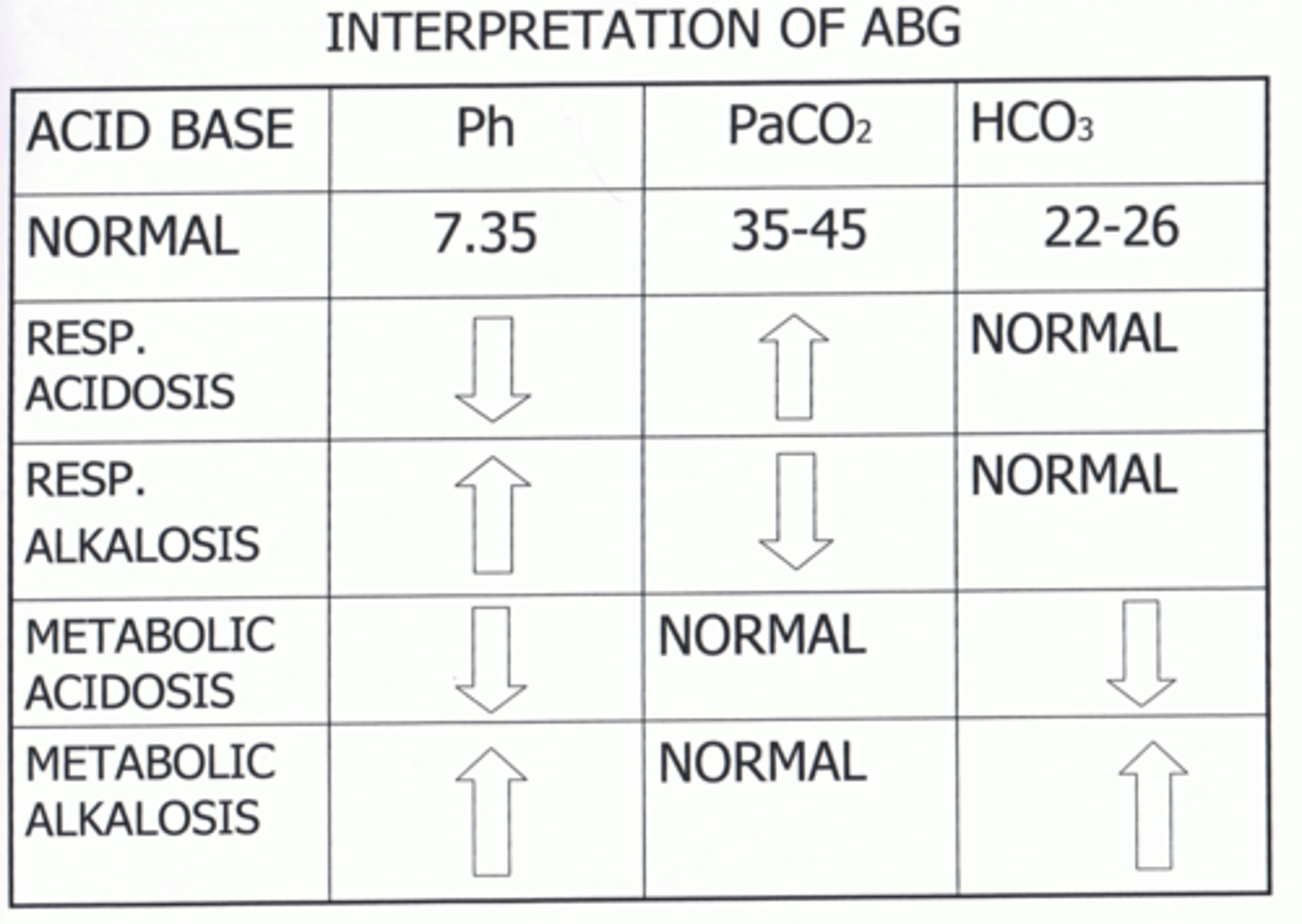
A nurse is reviewing ABG lab results of a patient who is in respiratory distress. The results are pH 7.47, PaCO2 32 mm Hg, HCO3 22 mm Hg. The nurse should recognize that the patient is experiencing which of the following acid-base imbalances?
a) Respiratory acidosis
b) Respiratory alkalosis
c) Metabolic acidosis
d) Metabolic alkalosis
Resp Alkalosis (B) (increased pH and decrease PaCO2, Possible causes- hyperventilation, fever, respiratory infectio
Continuous bubbling in the water seal
chamber indicates air leak in the system.
Tx for pneumothorax, hemothorax, pleural effusion
What is the life-threatening complication that can occur with a chest tube, when air is trapped in the pleural cavity under positive pressure causing a decrease in venous return to the heart?
Tension Pneumothorax.
You are caring for a patient on a mechanical ventilator who is getting weaned off.What are signs that the patient is NOT tolerating being weaned off the mechanical ventilator?
Tachypnea
"Air Hunger"
Decreasing SpO2 (usually <90%).
Labored Breathing
Bradypnea
🕵️♂️ Risk Factors: 3 Conditions Related to ARDS
Sepsis
Pneumonia
COVID-19
describe 3 nursing actions to maintain oxygenation
Prone Positioning
Encourage Coughing and Deep Breathing
Frequent Repositioning & Ambulation:
identify twocomplications with ARDS
MODS (Multiple Organ Dysfunction Syndrome): Because the lungs can't provide enough oxygen, other organs (like the kidneys and liver) begin to fail. 🛑
Ventilator-Induced Lung Injury (Barotrauma):
What do you delegate to CNA for an intubated patient?
Oral care 🪥
Vital signs monitoring 📈
Repositioning the patient
Agitated intubated patients often require the RN to do what?
The RN should NOT immediately medicate the patient. Instead, you must perform a thorough assessment to find the cause. It could be "air hunger," ventilator dyssynchrony, pain, or the need for repositioning
If your patient with a pneumothorax has low BP you can associate what other issue with this?
If a patient with a pneumothorax develops low blood pressure, you should immediately suspect a Tension Pneumothorax causing Obstructive Shock.
List 3 clinical manifestations of flail chest?
Asymmetrical/Paradoxical Chest Movement:
The injured area moves in while the rest of the chest moves out during inspiration. 📉
Severe Pain: Especially upon inhalation.
Respiratory Distress: Tachypnea and low oxygen saturation
For a chest tube, which requires intervention? Bubbling in suction-control chamber or water seal chamber?
Bubbling in the Water Seal Chamber requires intervention if it is continuous, as this indicates an air leak. 💨 Bubbling in the suction-control chamber is generally normal as it shows the suction is working.