chapter 20
1/43
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
44 Terms
Pericardium
Consists of fibrous pericardium and serous pericardium
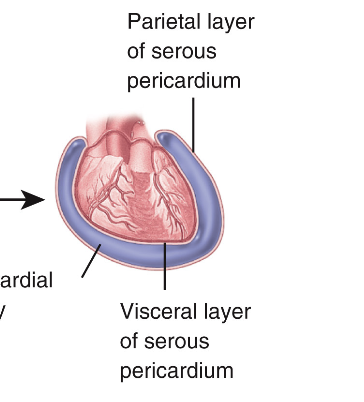
Fibrous Pericardium
Prevents overstretching of the ❤ , protection, anchors ❤ to mediastinum. Made of inelastic dense irregular connective tissue.
serous pericardium
Has 2 layers, Parietal pericardium + Visceral pericardium. Separated by Pericardial cavity (fluid filled space)
3 layers of heart
Epicardium, Myocardium, Endocardium
Pericarditis, Myocarditis, Endocarditis
Inflammation of the 3 layers of heart
Heart Pathway
Right atrium
Right ventricle
Pulmonary arteries/trunk
Pulmonary capillaries (gas exchange)
Pulmonary veins
Left atrium
Left ventricle
Aorta
Systemic capillaries (gas exchange)
Cava (back to right atrium)
Really Rough Plump Penls Penis Poop, Lets Let Aaron Suck Cock
Fibrous Skeleton
4 connective tissue rings surrounding the heart valves, fused together and merged with the interventricular septum
Myocardial Ischemia
Reduced blood flow to the myocardium. Can cause hypoxia + pain in chest, neck, etc
Myocardial Infarction
Heart attack, blocked coronary artery causing death of tissues, Treatment = thrombolytic injection angioplasty, bypass grafting
Autorhythmic Fibers
repeatedly generate spontaneous action potentials that then trigger heart contractions
Heart Conduction
SA node
Atrioventricular node
right/left Bundle Branches
Subendocardial conducting network
Suck A Big Sperm
Artifical Pacemakers
sends out small electrical current to stimulate the heart to contract
Epinephrine
Can modify heart rate, force of contraction and blood vessel size to increase blood flow during stress
Action Potential in a Ventricular Fiber
rapid depolarization, plateau, and repolarization
Rapid Depolarization in Ventricular Fiber
Na rushes into the cell, causes electrical charge to ↑, triggers cell to contract
Plateau in Ventricular Fiber
Ca2 flows in cells (keeping it ↑), K+ starts flowing out (bring ↓), balance then keeps cell contracted longer
Repolarization in Ventricular Fiber
Ca2 channel close, K+ flows out, charge ↓, cell relax
ATP Production in Cardiac Muscle
via aerobic cellular respiration (most) and creatine phosphate (some)
Electrocardiogram (EKG or ECG)
recording of the electrical changes that accompany each heart beat
Action Potential Propagation Through the Heart - 1
P wave = Depolar of atrial contractile fibers
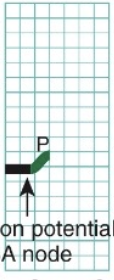
Action Potential Propagation Through the Heart - 2
Atrial systole (contract)
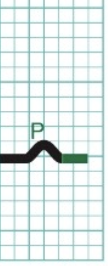
Action Potential Propagation Through the Heart - 3
QRS = Depolar of ventricular contractile fibers
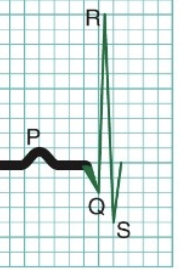
Action Potential Propagation Through the Heart - 4
Ventricular systole (contraction)
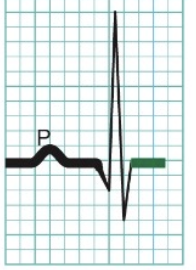
Action Potential Propagation Through the Heart - 5
T waves = Repolar of ventricular contractile fibers
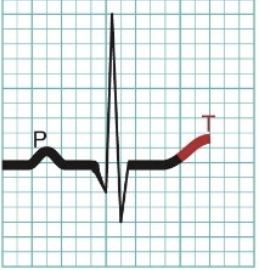
Action Potential Propagation Through the Heart - 6
Ventricular diastole (relaxation)
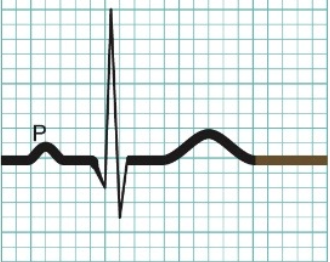
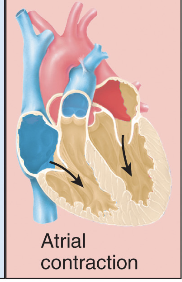
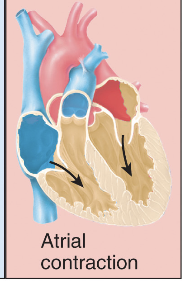
Phase of cardiac cycle - 1
Atrial contraction - Atria squeeze blood ↓ → ventricle. Ventricle are relax and filling up
Phase of cardiac cycle - 2
Isovolumetric (same vol) contraction - Ventricles strat contracting, pressure ↑, Biscupid valve close (no backflow into atria), no blood leave yet (vol same)
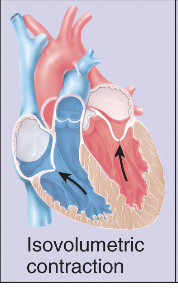
Phase of cardiac cycle - 3
Ventricular ejection -Ventricular pressure gets ↑ enough to force aortic valve open, blood gets pumped out into aorta and pulmonary artery (Pumping phase)
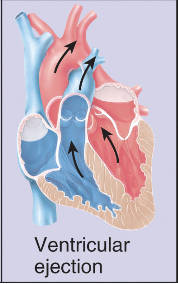
Phase of cardiac cycle - 4
Isovolumetric (same vol) relaxation - Ventricles relax, pressure drops, aortic valve close (no backflow from aorta), no blood moving (vol same)
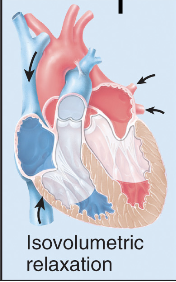
Phase of cardiac cycle - 5
Ventricular filling - Bicuspid valve opens, blood flows from artia back into ventricles, ventricles refill
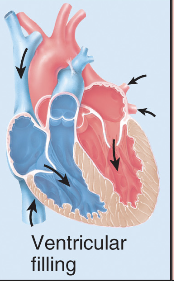
Phase of cardiac cycle - 6
Atrial contraction - cycle repeats
Isovolumetric
All valves closed, no blood moving, just pressure changing
Cardiac Output
CO (mL/min) = SV (mL/beat) x HR (beats/min)
Stroke Volume (SV)
amount of blood pumped out of ventricle in one beat
Preload
Stretch of ventricles b4 contraction, depends on end diastolic volume (EDV), More filling = ↑ SV.
Ex: Slow HR = more filling = bigger SV
Contractility
Strength of ventricular contraction
↑ Ca²⁺ = stronger contraction = ↑ SV
Afterload
Pressure in aorta + pulmon trunk that must be overcome for semilunar valve open, lower afterload = ↑ SV
Ex: ↑ BP = ↑ after load = ↓ SV
End Diastolic Volume (EDV)
the amount of blood in a ventricle right before it contracts
Coroanry Artery Disease
Blocks coronary arteries, causes hypoxia
Atherosclerotic plaques:
Structures developed in arteries, fat deposits, arteries become clogged, can occur in coronary arteries (coronary artery disease)
Congenital Heart Disease
Foramen ovale does not close upon birth
Arrthymia
Lack of normal heart rhythm, examine ECG to see arrythmia or stethoscope to hear irregular rhythm
Congestive heart failure
Left, right or both ventricles do not contract strong enough, does not pump enough blood throughout body counteracted by the devices previously mentioned