Psych/Nuero Final: Cav MS, ALS, MG
1/113
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
114 Terms
CNS
Multiple Sclerosis (MS): autoimmune, inflammatory disease of __
relapsing-remitting
4 Different Types of MS:
1. ____-____ (most common!!, unpredictable attacks which may or may not leave permanent deficits followed by periods of remission)

primary progessive
4 Different Types of MS:
2. ____ ____ (steady increase in disability without attacks)

secondary progressive
4 Different Types of MS:
3. ___ ____ (initial relapsing-remitting that suddenly begins to have decline WITHOUT periods of remission)

progressive-relapsing
4 Different Types of MS:
4. ____-___ (steady decline since onset with superimposed attacks)

cognitive
MS Symptoms
1. ___ dysfunction
vision
MS Symptoms
2. ___ problems
balance
MS Symptoms
3. ___ issues
fatigue
MS Symptoms
4. chronic ___
depression
MS Symptoms
5. ____
myelin sheath
What Happens In MS
In multiple sclerosis, the immune system attacks and destroys the ___ ___ around nerves in the CNS, leading to loss of nerve signal conduction and formation of scarred demyelinated areas called plaques.
milieu, antigen
2 Steps Required to Induce Immune Reponse in MS
1. a pro-inflammatory ___ (ie "soup") in the CNS
2. ___-drive acquired immune response
T, B
Immune Reponse in MS
1. Antigens released from the CNS are taken up and presented by dendritic cells, which then prime → ___ and ___ cells in peripheral lymphoid tissues.
clonal expansion
Immune Reponse in MS
2. After the T and B cells are primed → they rapidly multiply (___ ___) in the lymphoid tissue
CNS
Immune Reponse in MS
3. After clonal expansion in the lymphoid tissue → T and B cells infiltrate the ___
IgG, antigen
Immune Reponse in MS
4. After infiltrating CNS → B cells re-encounter their antigen, mature to plasma cells, and release large amounts of ___ antibodies, which bind to soluble or membrane-bound __ on expressed cells
brain, damage
Immune Reponse in MS
5. After infiltrating CNS → CD8+ T cells invade the ___ and encounter their specific peptide ligand which prompts direct __ to expressing cells
inflammatory cytokines, attract
Immune Reponse in MS
6. After infiltrating CNS → CD4+ T cells encounter antigens presented by microglial cells, which lead to increased production of ____ ___ that then ___ other immune cells (like macrophages)
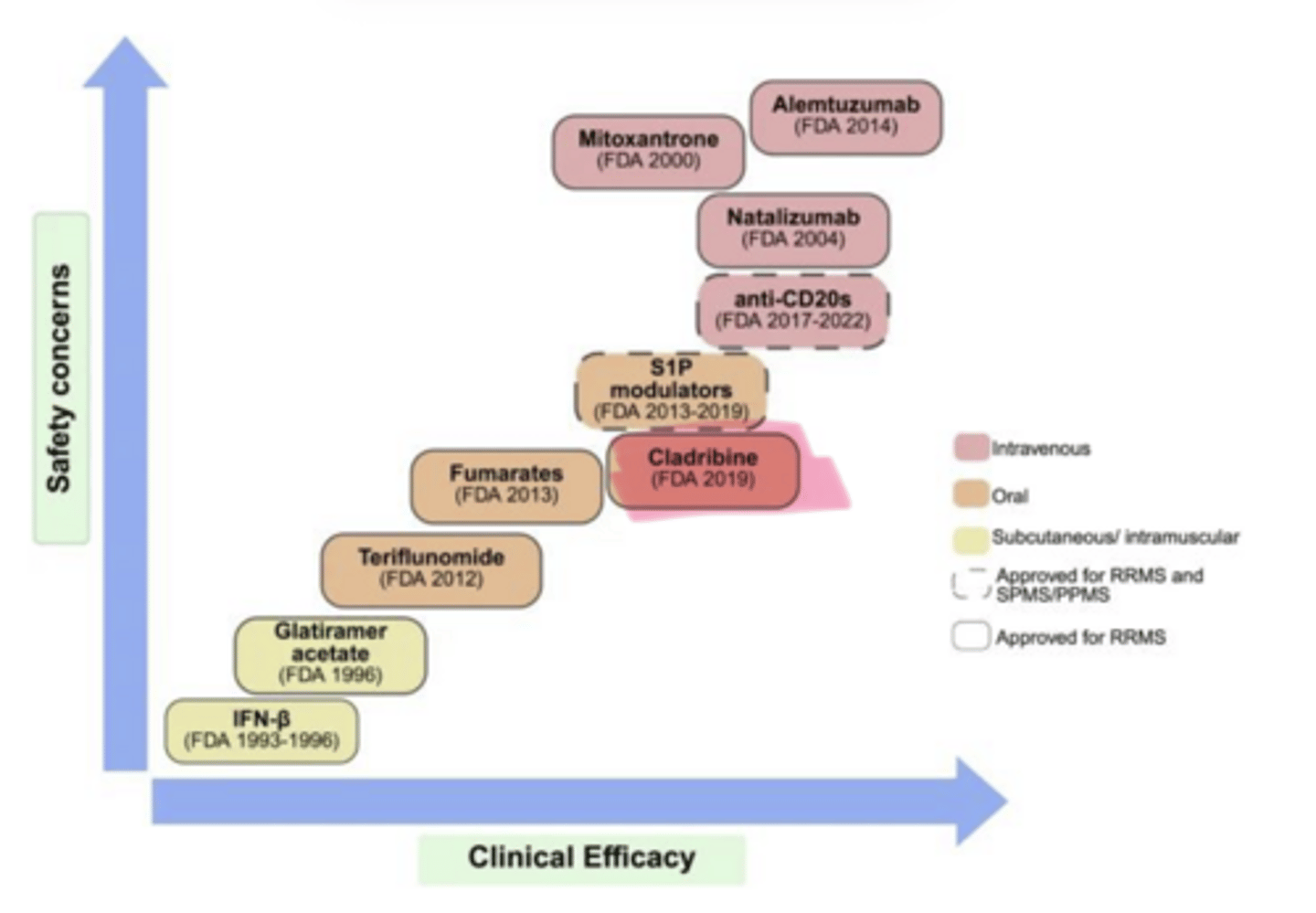
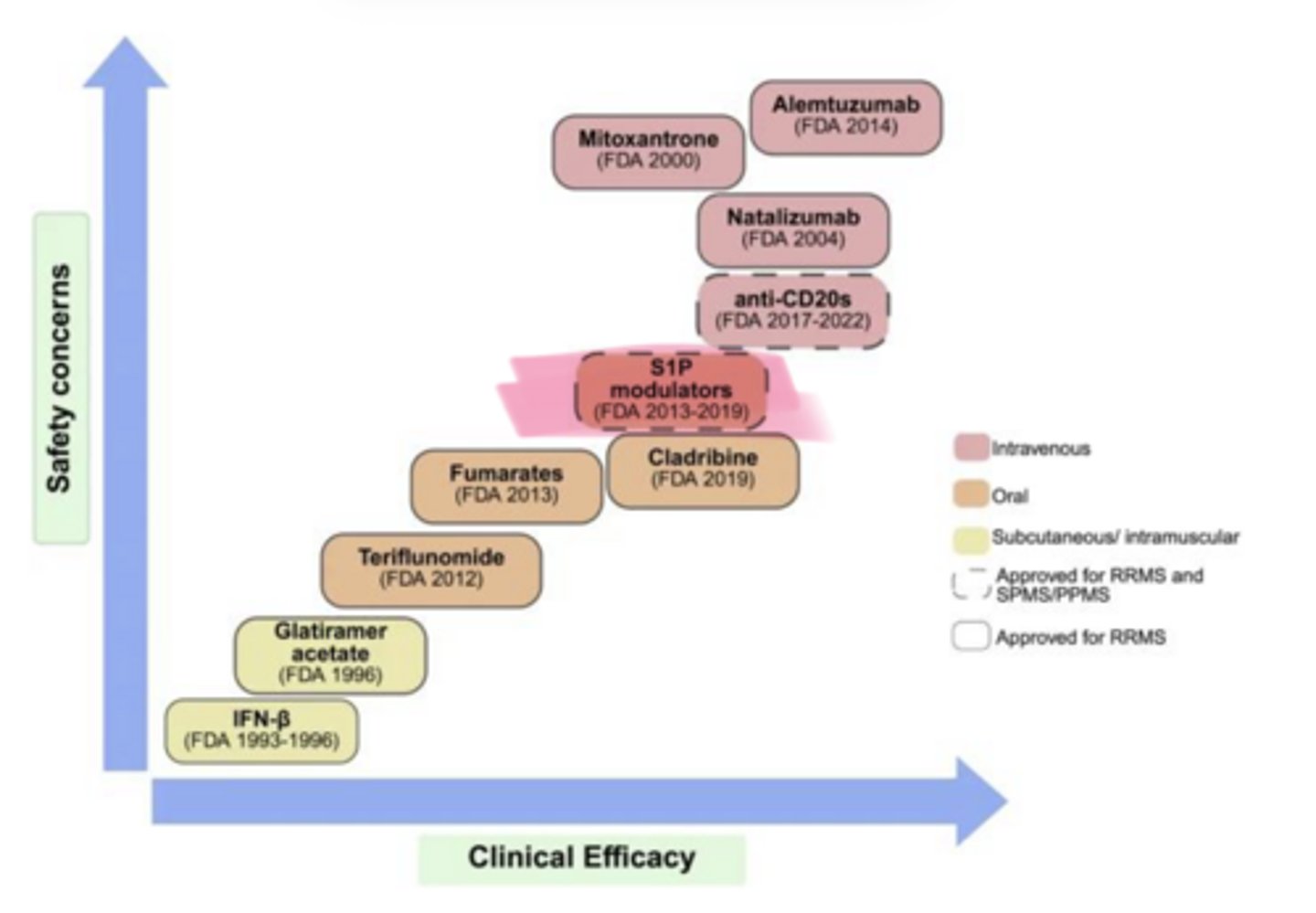
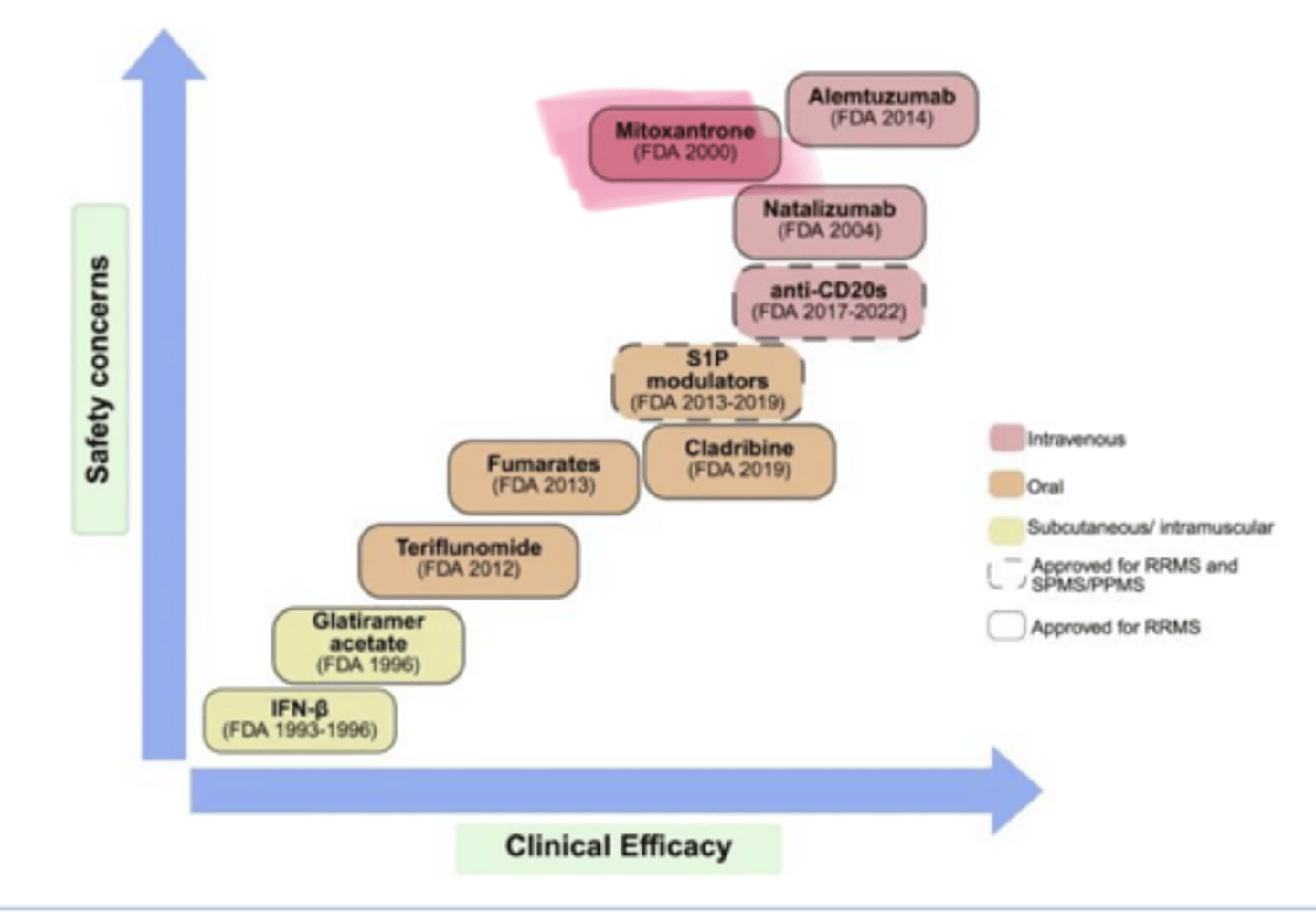
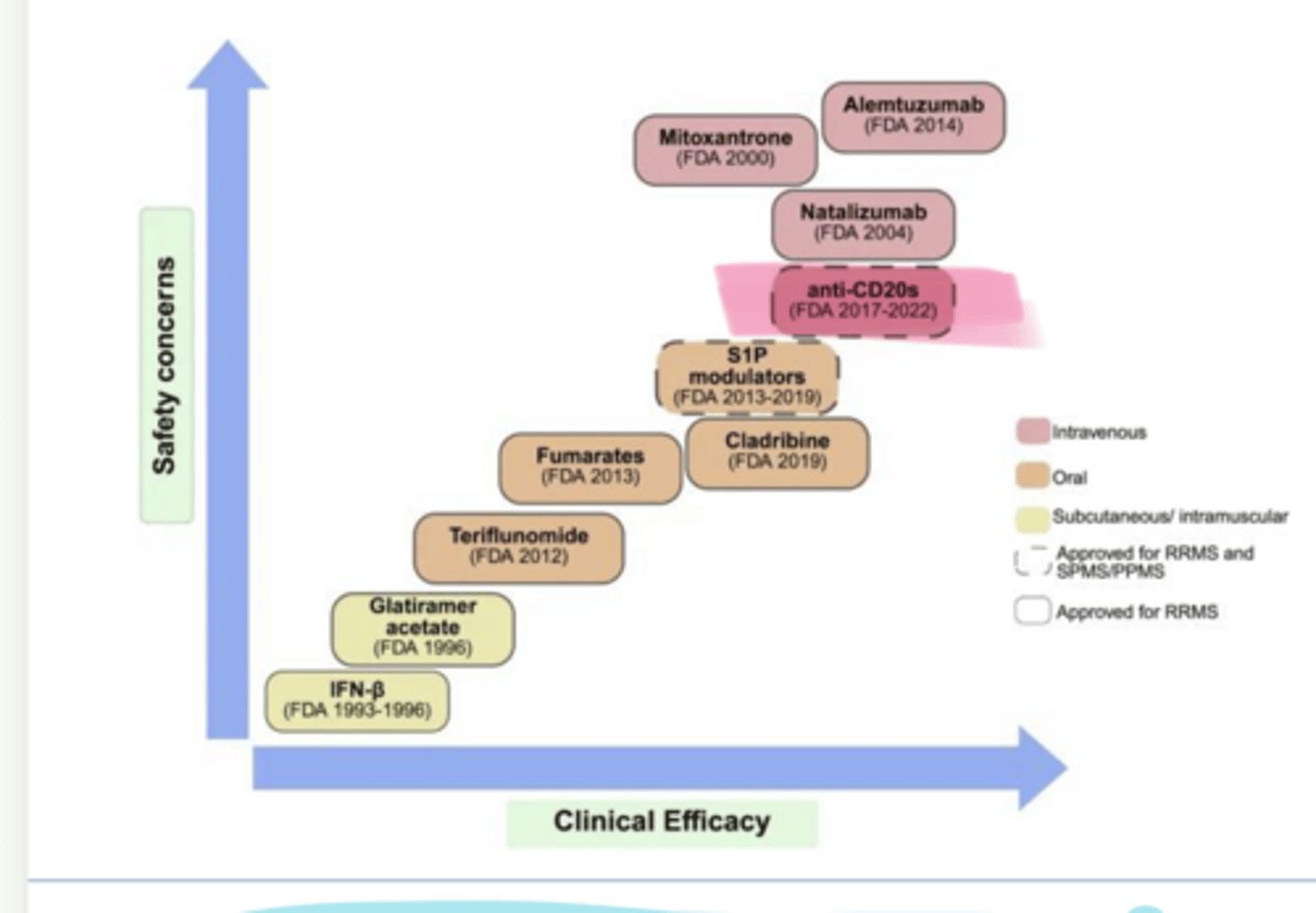
safety
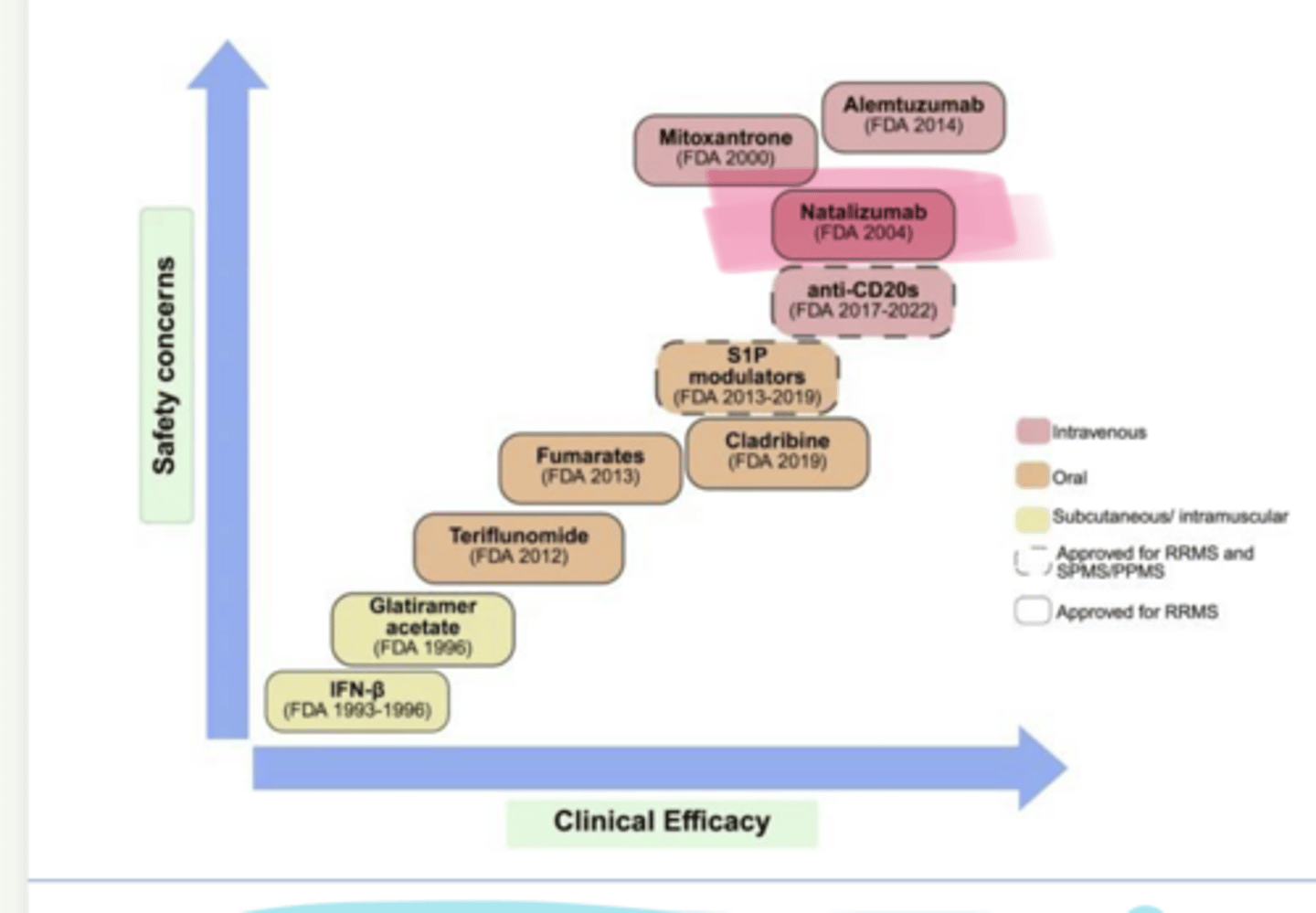
As clinical efficacy of MS Treatments increases, so does ___ concerns
1a, 1b
Interferon β-___ (Avonex, Rebif) and Interferon β-___ (Betaseron) are used in multiple sclerosis
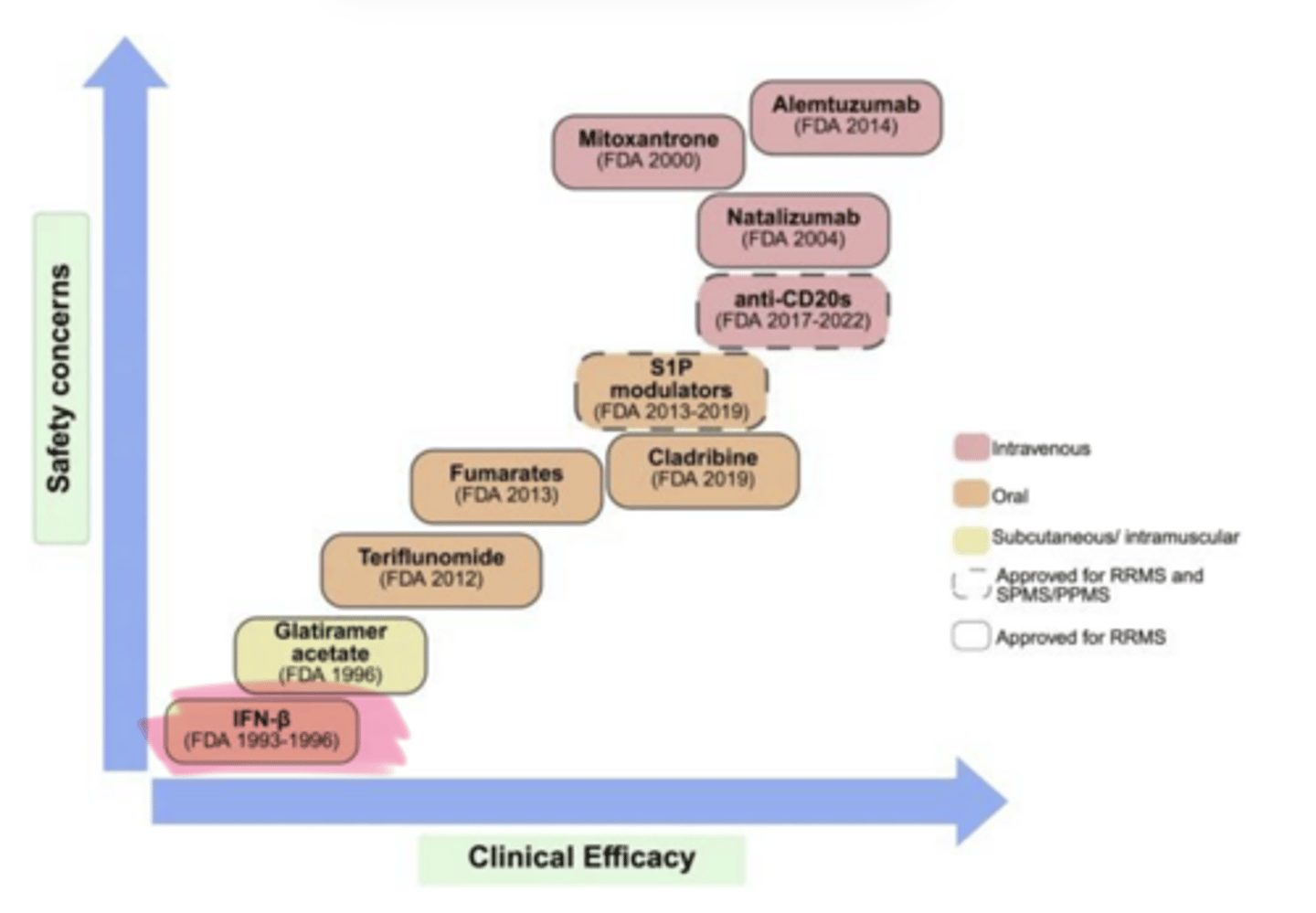
activation, adhesion, penetration
How do IFNβ drugs work in the periphery?
1. decreases T cell ____
2. decreases T cell ___ and ___ of the BBB
presentation, cytokine
How do IFNβ drugs work in the CNS?
3. decreases antigen ___
4. promotes anti-inflammatory __ production
Th1, proliferation
How do IFNβ drugs work in the CNS?
5. decreases ___ cytokine release
6. decreases B-cell ___
damage
How do IFNβ drugs work in the CNS?
7. decreases bystander ___
Glatiramer
____ (Copaxone) is used in multiple sclerosis
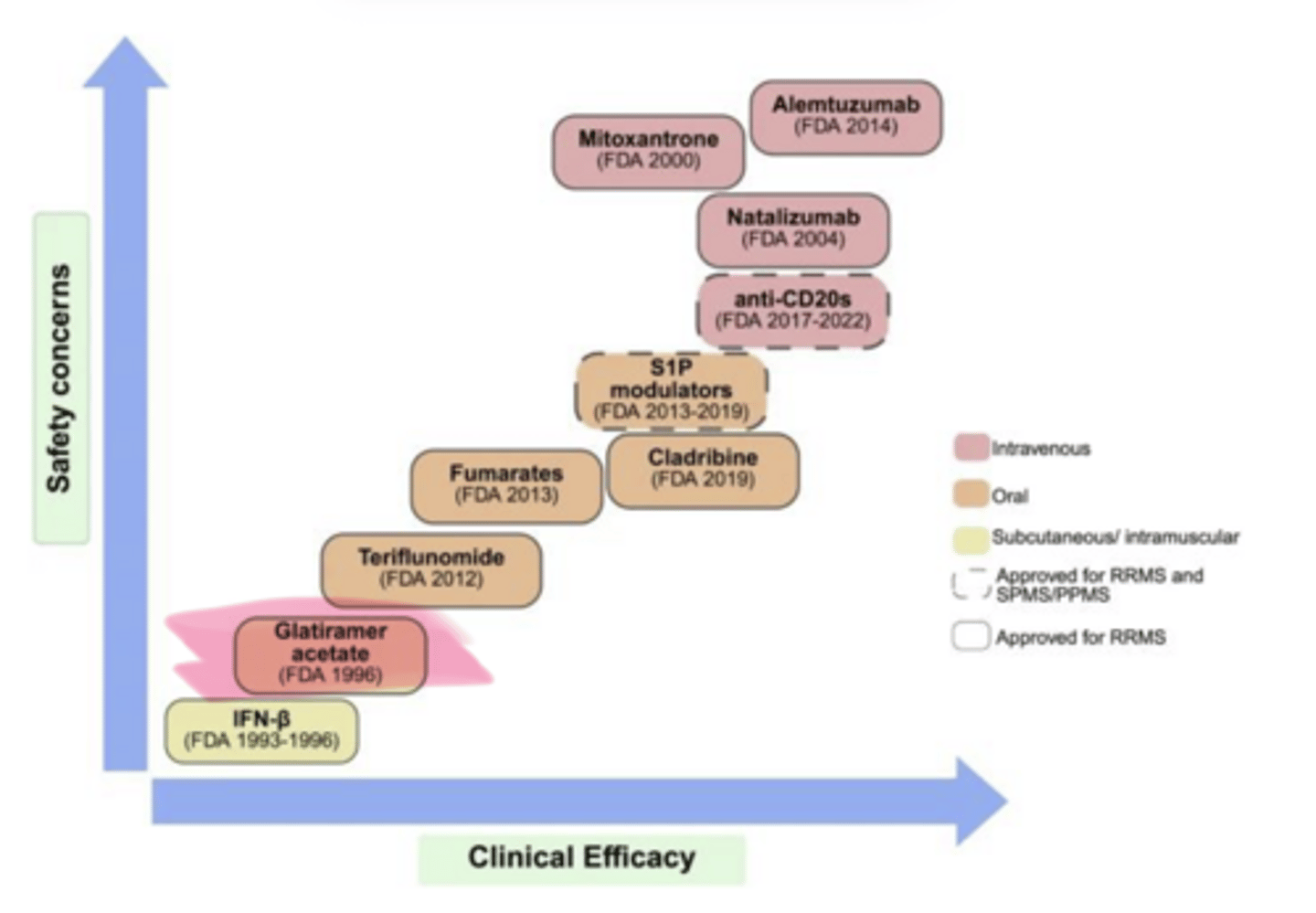
BBB
Glatiramer cannot penetrate the ___
decoy
Glatiramer acetate acts in the periphery as a "___" antigen (it resembles myelin basic protein, so T cells react to it instead of attacking the actual myelin in the CNS.)
Th2
Glatiramer shifts T-cell response from pro-inflammatory Th1 cells to anti-inflammatory ___ cells
cytokines, trophic
Glatiramer
-the anti-inflammatory Th2 cells migrate into the CNS and release anti-inflammatory ____ and ___ factors (promote neuronal/glial survival)
bystander suppression
Glatiramer
-the result of peripheral Th2 cells crossing the BBB and releasing anti-inflammatory cytokines and trophic factors = "____ ____"
inflammation
"bystander suppression" refers to the reduction of ____ as a result of peripheral Th2 cells crossing the BBB and releasing anti-inflammatory cytokines and trophic factors
Teriflunomide
____ (Aubagio) is used in multiple sclerosis
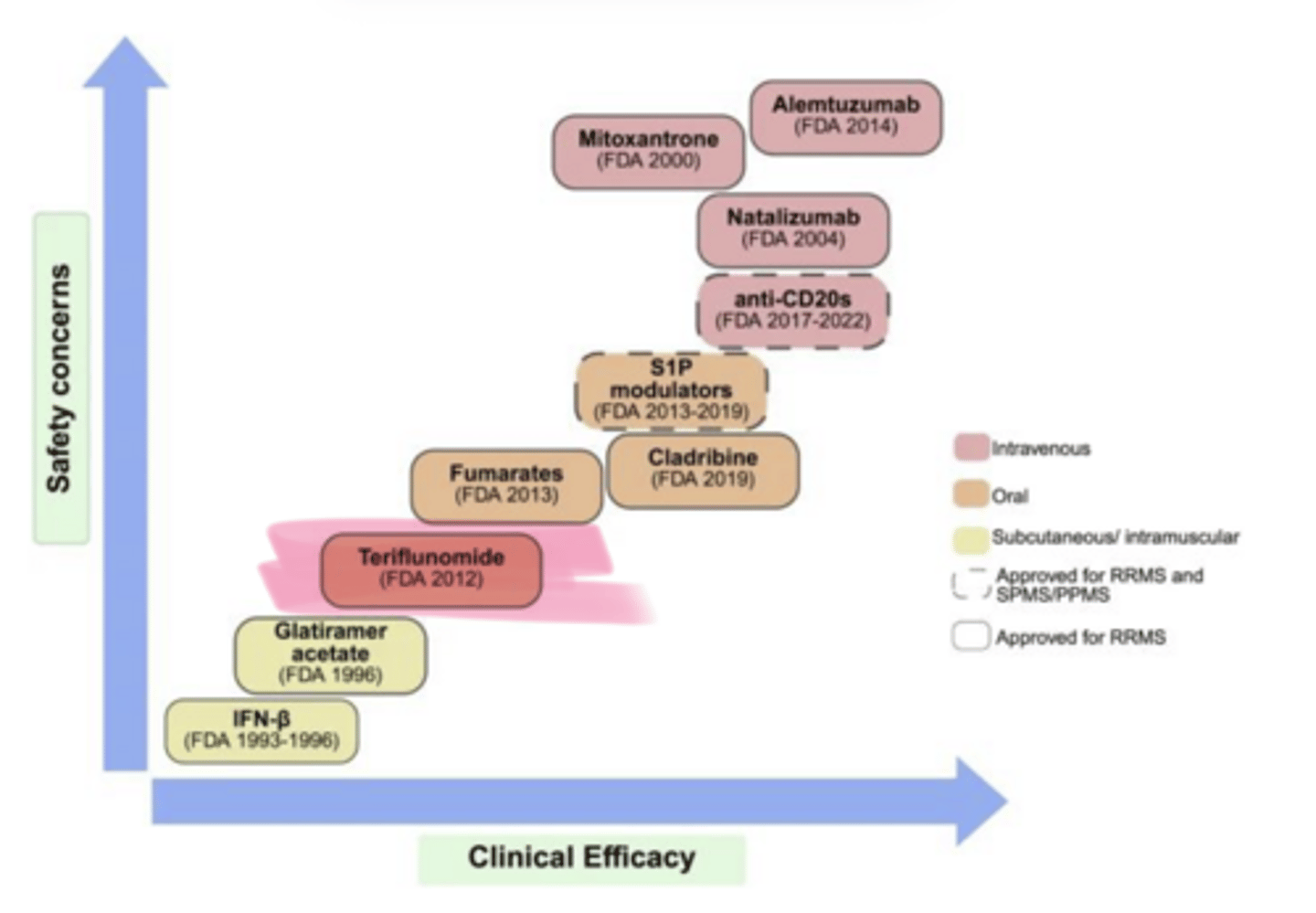
DHODH, pyrimidine
Teriflunomide MOA
1. Inhibits dihydroorotate dehydrogenase (___) in mitochondria → resulting in decreased de novo ___ synthesis)
glycoproteins, phospholipids, nucleotides
Teriflunomide inhibits DHODH to decrease pyrimidine synthesis → effect = less production of ___, ___, and ___, which ultimately impairs cell function and leads to cell death.
JAK-STAT, cytokines
Teriflunomide MOA
2. Inhibits ___-___ signaling pathway → resulting in decreased production of pro-inflammatory ___
Dimethyl Fumarate
____ ___ (Tecfidera) is used in multiple sclerosis
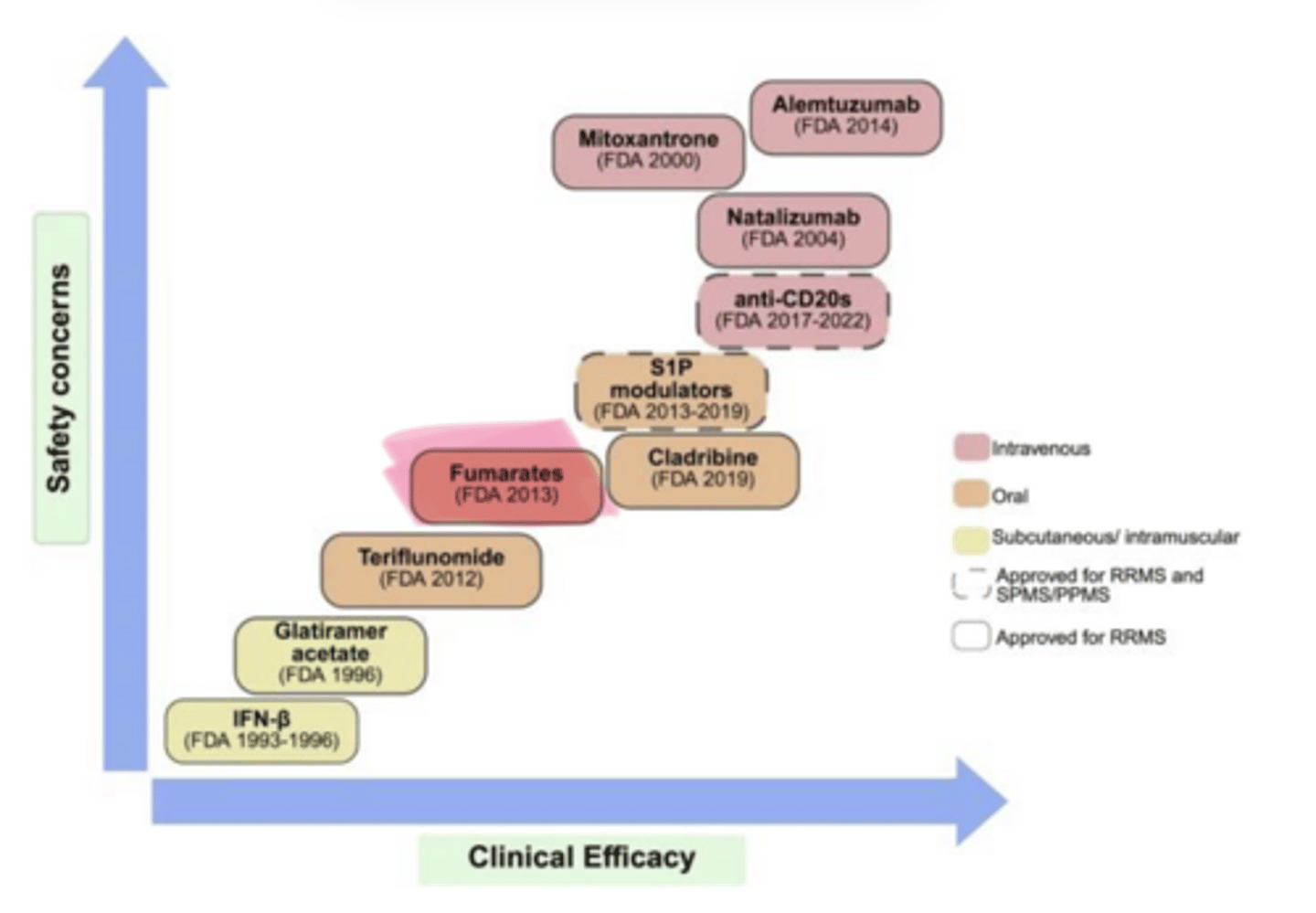
TH2, bystander suppression
Dimethyl Fumarate
-MOA is similar to glatiramer → Shifts immune balance in the periphery by increasing ___ anti-inflammatory cells and decreasing pro-inflammatory T and B cells to promote ___ ___ in the CNS
CNS
Dimethyl Fumarate
-Remember glatiramer cannot cross BBB. The key difference with dimethyl fumarate is that it can enter the ___
kinase
Dimethyl Fumarate
-After entering the CNS, the drug activates ___ signaling pathway (ERK pathway) to support neuronal and glial cell survival
oxidative stress
Dimethyl Fumarate
-By activating kinase pathways, it increases anti-apoptotic and antioxidant factors, which reduces ___ ___ and inflammation in the brain.
Cladribine
____ (Mavenclad) is used in multiple sclerosis
kinases
Cladribine is activated by ___
phosphotases
Cladribine is inactivated/degraded by ___
somatic
Cladribine
-in ___ (normal body) cells, there is low kinase and high phosphatase, meaning cladribine gets inactivated/degraded and has minimal efffect
lymphocytes
Cladribine
-is preferentially activated in ___ due to higher kinase and lower phosphatase activity,
DNA
Cladribine MOA
-selectively accumulates in lymphocytes, where it disrupts ___ synthesis/repair and causes cell death.
Fingolimod, Siponimod
____ (Gilenya) and ___ (Mayzent) are used in multiple sclerosis
S1R
Fingolimod, Siponimod
-Normally, T cells are activated in lymph nodes and are signaled to leave (egress) by ___ binding to its receptor
S1P
Fingolimod, Siponimod MOA
-prevent T cell egress from lymph nodes by antagonizing ___ receptors
Mitoxantrone
____ (Novantrone) is used in multiple sclerosis
DNA
Mitoxantrone
-intercalates (ie inserts itself) into __
non-specific cytotoxic
Mitoxantrone
-In DNA, has a __-___ ___ effect ("like dropping a bomb on immune response")
T, B, macrophages
Mitoxantrone Effects in DNA:
1. ↓ proliferation of __ cells, __cells, and ___
antigen
Mitoxantrone Effects in DNA:
2. Impairs ___ presentation
pro-inflammatory cytokines
Mitoxantrone Effects in DNA:
-↓ secretion of ___-___ __
ocrelizumab, ofatumumab, ublituximab
____ (Ocrevus), ____ (Kesimpta), and ____ (Briumvi) are used in multiple sclerosis
CD20, B
Ocrelizumab, Ofatumumab, and Ublituximab bind to ___ on __ cells
depletion
Ocrelizumab, Ofatumumab, and Ublituximab bind to CD20 on B cells. This results in ___ of B cells
antibody, complement, apoptosis
Ocrelizumab, Ofatumumab, and Ublituximab deplete B cells in 3 ways:
1. ___-dependent cell-mediated cytotoxicity
2. ___-mediated cytotoxicity
3. ___ induction
Natalizumab
____ (Tysabri) is used in multiple sclerosis
T
Natalizumab
-Monoclonal antibody against α4β1 integrin on __ cells (not CD20 like the B-cell drugs)
VCAM-1
Natalizumab
-Blocks T-cell adhesion to ___ on endothelial cells
CNS
Natalizumab
-Final effect = decreased T-cell entry into the ___ (therefore decreased inflammation and myelin damage)
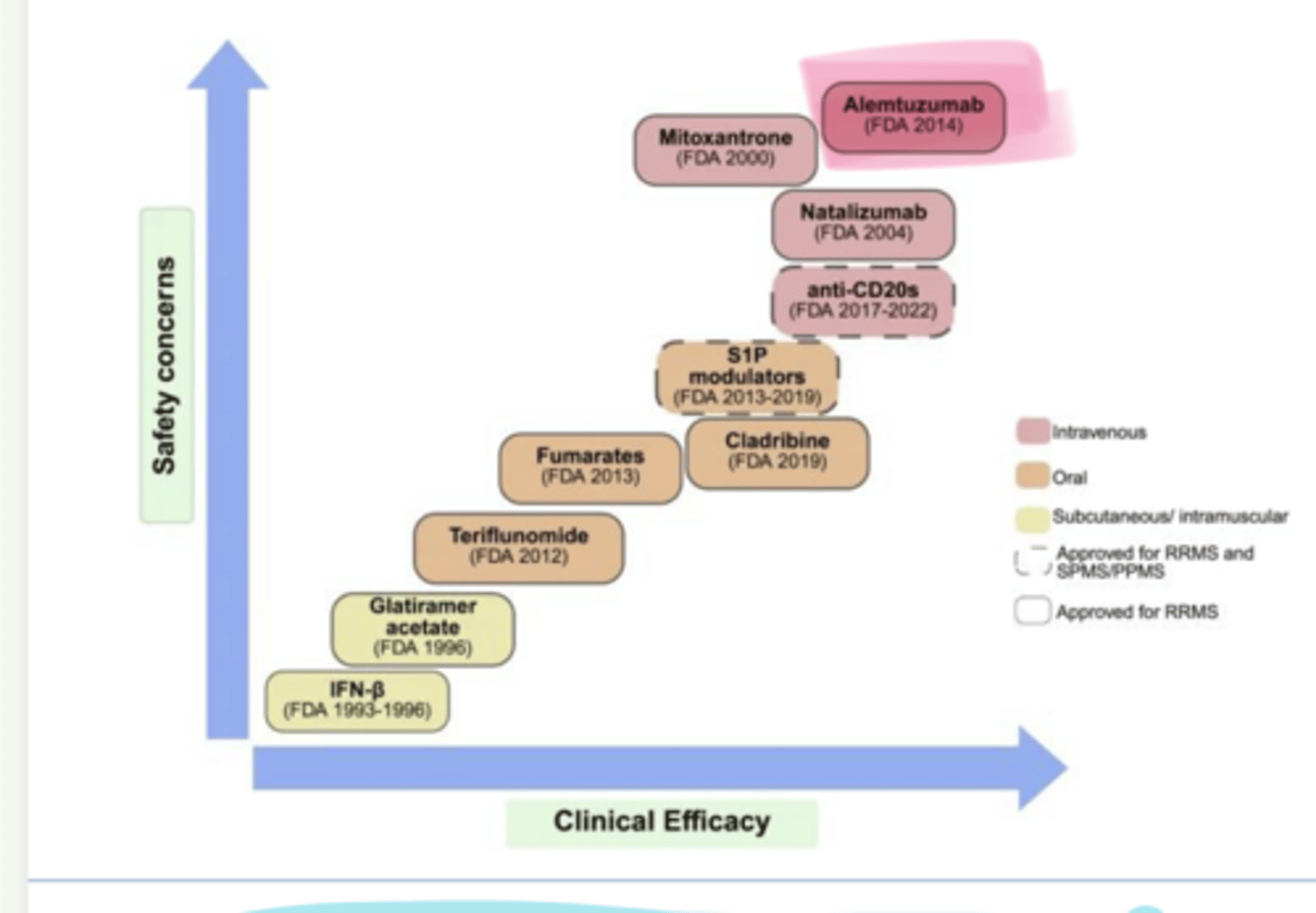
Alemtuzumab
_____ is used in multiple sclerosis
CD52
Alemtuzumab
-Monoclonal antibody against ___ on lymphocytes (B and T cells)
complement, antibody
Alemtuzumab
-Causes lymphocyte depletion via ___-mediated cytotoxicity and
___-dependent cellular cytotoxicity
ALS
Amyotrophic Lateral Sclerosis = __
weakness, atrophy, respiration
ALS
-rapid, progressive muscle ___
-muscle ___
-spasticity
-compromised ___
sensory, cognitive, autonomic
ALS-the following are spared
-___
-___
-___
progressive, fatal
ALS is ___ and usually ___
upper, lower
ALS
-a disease of __ and ___ motor neurons (patients have varying degrees of both)
stiffness, spasticity
ALS
-upper motor neuron disease → causes ___ called ___
weakness, muscle, twitching
ALS
-lower motor neuron disease → causes ___, loss of ____ (atrophy), and muscle ___ (fasciculations)
speech, swallowing, tongue
Bulbar ALS → primarily affects muscles involved in __, ___, and __ movements
sporadic, genetic
ALS can be __ or __
infection, glutamate, free radical
Sporadic ALS Etiology
-viral ___
-autoimmunity
-excitotoxicity (____ uptake)
-___ ___ toxicity
SOD1
Genetic ALS Etiology
1. mutation in ___ (superoxidase dismutase 1, which protects from damage from the toxic free radical superoxide)
aggregates
Genetic ALS Etiology
-the mutated SOD1 ____ ("forms clumps in brain")
TARDBP, FUS, ANG
Genetic ALS Etiology
2. mutation in ___, ___, ___ (control RNA transcription an splicing)
OPTN
Genetic ALS Etiology
3. mutation in ____ (optineurin gene) that leads to apoptosis
glutamate
ALS Disease Progression-Early Stage
Astrocytes normally remove excess ___, but in ALS this system fails → leading to increased glutamate and Ca²⁺ influx → neuronal toxicity
EAAT2
ALS Disease Progression-Early Stage
___ = glutamate transporter located on astrocytes
aggregation
ALS Disease Progression-Early Stage
-Protein ___ (e.g., SOD1 mutations) leads to mitochondrial dysfunction and impaired axonal transport
toxic
ALS Disease Progression-Symptomatic Stage
-___ factors are released from activated microglia/astrocytes
muscle
ALS Disease Progression-End Stage
-involves caspase-mediated apoptosis of motor neurons with microglial phagocytosis, leading to severe __ atrophy and respiratory failure.
Riluzole
____ (Rilutek, Exservan, Tiglutik) is a glutamate antagonist used in ALS
glutamate sodium
Riluzole
1. Main mechanism = Decreases ___ release by blocking voltage-gated ___ channels → reduces neuronal firing in glutamate pathways
reuptake
Riluzole
2. Increases ___ of glutamate
receptor
Riluzole
3. Weakly blocks glutamate __
IV
Riluzole is an oral drug that has limited BBB penetration due to P-gp efflux, whereas Edaravone is given ___, and therefore better reaches the CNS
free radical scavenger
Edaravone
-MOA = ___ ___ ___ (antioxidant that neutralizes oxidative stress to neuron damage)
SOD1
Tofersen is approved for ALS who have been identified to have mutant __
oligonucleotide, RNA
Tofersen
-an antisense ___ (ASO) that targets the __ produced by mutated SOD1 genes
production
Tofersen
-blocks transcription of RNA to stop toxic SOD1 protein ___
medicare
Tofersen
-$150,000-200,000 per year, but covered under __ for qualified patients
neuromuscular
Myasthenia Gravis is an autoimmune disease where antibodies target nicotinic acetylcholine receptors at the ___ junction
respiratory
Myasthenia Gravis (MG)
-ptosis (drooping of eyelids), diplopia (double vision), difficulty speaking/swallowing, extremity weakness
-severe disease that affects all muscles including ___
acetylcholine, MuSK
Myasthenia Gravis involves antibodies against nicotinic __ receptors and/or ___
neuromuscular junctions
MuSK
-a receptor tyrosine kinase crucial for forming and maintaining ___ ___ (the connections between nerves and muscles)
agrin, acetylcholine
MuSK
-activated by ___, a nerve derived protein, and plays a key role in clustering ___ receptors and other proteins in the synapse