Midterm 1 Path 3610
0.0(0)
Studied by 2 peopleCard Sorting
1/144
Earn XP
Description and Tags
Last updated 6:01 PM on 2/17/23
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
145 Terms
1
New cards
Pathogenesis of Disease
__________ involves three steps.
1. Cause: Providing a cause
2. Mechanisms: Outlining the mechanisms involved
3. Outcome: Clinical signs or lesions.
1. Cause: Providing a cause
2. Mechanisms: Outlining the mechanisms involved
3. Outcome: Clinical signs or lesions.
2
New cards
Homeostatsis
is a state where cells are able to cope with the physiological demands placed upon them.
* Increased demand results in increased response - or adaptation. If the demand (or an insult) exceeds the ability of the cell to adapt, injury occurs.
* Increased demand results in increased response - or adaptation. If the demand (or an insult) exceeds the ability of the cell to adapt, injury occurs.
3
New cards
3 responses to demand
_____________ - adaptation, reversible injury, and irreversible injury and cell death.
4
New cards
Single cell death, apoptosis
cells die and shrink
5
New cards
coagulation, necrosis
cells stay the same
6
New cards
hydropic degneration and oncotic necrosis
cells swell
7
New cards
Free radicals
are molecules that have an unpaired electron, and they release considerable energy. The most common free radical is derived from oxygen and is called oxygen derived free radicals (ODFR).
8
New cards
endogenous and natural scavengers
There are many _______________________ of free radicals including vitamin A, C and E, and glutathione.
9
New cards
Healing
of an injury to an organ involves regeneration and fibrous tissue formation in variable amounts.
10
New cards
Regeneration
occurs when the injured cells are able to be replaced with cells of an identical or similar type
11
New cards
Fibrosis (scarring)
is when the cells are replaced with fibrous tissue.
* requires an intact architecture or extracellular matrix (connective tissue scaffold) of the organ.
* Without a normal matrix, fibrous (scar) tissue forms in the organ.
* requires an intact architecture or extracellular matrix (connective tissue scaffold) of the organ.
* Without a normal matrix, fibrous (scar) tissue forms in the organ.
12
New cards
the 4 stages of the cell cycles are:
1. G1 (presynthetic)
2. S (DNA synthesis)
3. G2 (premitotic)
4. M (mitotic)
13
New cards
Resting cells
are in the G0 phase
14
New cards
G1 stage
they enter the cell cycle they enter at the ____________
15
New cards
Terminally differentiated
cells are generally not capable of division (are nondividing). They are also called **permanent** cells.
16
New cards
Permanent cells
_________________ include neurons, the muscle cells of the heart (myocardiocytes; myocardium) and skeletal muscle.
17
New cards
continuously dividing tissues; labile
____________ also called _________cell types, have stem cells that proliferate and replace the mature or terminally differentiated cells. These terminally differentiated cells are short-lived, and incapable of replication.
18
New cards
quiescent or stable cells
Many organs are composed of cells that are__________________________ that are present in a resting state and, when injured, have cells that are able to divide.
19
New cards
Hypertrophy
____________ is an increase in cell size or tissue size because of an enlargement in the size of the cell or cells.
* ___________ the opposite is atrophy.
* ___________ the opposite is atrophy.
20
New cards
Atrophy
In ___________ a tissue or a cell reduces its size. In an organ or tissue, this can be by a reduction of the number of cells or the size of cells. It is usually a response to decreased demand.
21
New cards
Hyperplasia
__________ is an increase in the number of cells and it is a common response to increased demand of cells that are continuously dividing (labile).
22
New cards
Metaplasia
_________ is when, under sufficient demand usually chronic irritation, one cell type changes to another.
23
New cards
Degeneration
_____________ is the result of an injurious process that results in impairment of cell function from which recovery can occur (reversible injury).
24
New cards
cell swelling; hydropic degeneration
The most common manifestation of cell injury is **________________**__**.**__ Most cells swell because they cannot control entry or loss of water (hence the name ____________________________).
* This is usually because they lose the ability to maintain ions such as Na+ and K+ concentrations because of membrane damage, loss of energy production, or a failure of ion pumps.
* This is usually because they lose the ability to maintain ions such as Na+ and K+ concentrations because of membrane damage, loss of energy production, or a failure of ion pumps.
25
New cards
Fatty degeneration; fatty change
Those cells that are capable of processing fat can lose their ability to metabolize and transport fat. Fat accumulates and causes the cell to swell. Some rupture and die. **_________________or __________________** is a manifestation of this type of reversible injury.
26
New cards
Accidental cell death and regulated cell death
Cell Death is divided into 2 groups:
27
New cards
Accidental Cell Death (ACD)
______________ is the “instantaneous and catastrophic demise of cells exposed to severe insults of physical, chemical, or mechanical nature”.
28
New cards
Regulated cell death
**________________** is when death occurs from activation of molecular machinery (subroutines) be they preprogrammed or not. There is a lethal trigger.
29
New cards
Programmed cell death
Physiological regulated cell death is **____________________,** which is thus a subset of regulated cell death. It occurs in embryological / post embryological, physiological and homeostatic situations (metamorphosis, cornification of skin),
30
New cards
necrosis; necrotic
Cell death was called _____ and dead tissue was _________
31
New cards
coagulation, liquefactive, caseous, gangrenous
These appearances of necrosis include:
32
New cards
Coagulative necrosis
**__________________** is a morphological descriptor to describe what happens when cells die and remain the same size and have the characteristics of living cells (meat in the supermarket is dead but looks the same as live muscle).
33
New cards
Liquefactive necrosis
___________________ is when the tissue is rendered liquid by enzymatic dissolution.
34
New cards
Caseous necrosis
_________________ is when tissue partially liquefies or was liquid and dehydrates.
35
New cards
Gangrenous necrosis
___________________ is when there is coagulative necrosis that proceeds to liquid by bacterial action (moist gangrene) or becomes dry and mummified following infarction, and gas gangrene when contaminating bacteria causes necrosis and produces gas.
36
New cards
Apoptosis, autophagy, and necrosis
_________________________________share biochemical pathways, and represent a continuum – which process occurs is dependent on the insult and cell type and physiological state, particularly in the level of intracellular ATP.
37
New cards
Apoptotic cells
________________ have nuclear fragmentation, cellular shrinkage, fragmentation and engulfment by surrounding cells.
38
New cards
Autophagy
______________ occurs when parts of the cytoplasm and damaged organelles are bound by membranes to become autophagosomes. These then fuse with lysosomes that contain digestive enzymes. This occurs in a specific sequence prior to the destruction of the nucleus.
39
New cards
cell swelling; cell swelling
Cells that die from _________ do so if the acute_____________ (previously called hydropic degeneration) proceeds to the point of no return (becomes irreversible).
40
New cards
regulated cell death
Activation of ___________________ is divided into initiation and execution phases.
* The initiation can be extracellular or external (extrinsic) or intracellular or internal (intrinsic) to the cell.
* The initiation can be extracellular or external (extrinsic) or intracellular or internal (intrinsic) to the cell.
41
New cards
necrosis
The second cause of __________ in frostbite is vasoconstriction and resultant ischemia.
* Blood vessels constrict as a direct response to cold.
* Blood vessels constrict as a direct response to cold.
42
New cards
Ischemia
lack of blood flow
* literally means ‘to keep back blood’ or ‘the stopping of blood’.
* is often the result of vasoconstriction.
* literally means ‘to keep back blood’ or ‘the stopping of blood’.
* is often the result of vasoconstriction.
43
New cards
infarction; infarct
When tissue dies due to ischemia
* Brain, heart and kidney are the major ones organs with this type of circulation. Infarction can be the result of obstruction of an artery (**arterial ________**) such as occurs in a heart attack (myocardial infarction).
* Brain, heart and kidney are the major ones organs with this type of circulation. Infarction can be the result of obstruction of an artery (**arterial ________**) such as occurs in a heart attack (myocardial infarction).
44
New cards
hypoxia
reduction in oxygen tension in the tissues
45
New cards
Vascular system
The _________________ is a transportation system for cells, nutrients, and wastes, and it is important in maintaining a normal fluid and electrolyte balance.
46
New cards
blood
The fluid in the vascular system of mammals is _______.
47
New cards
RBC, WBC,platelets, plasma
The main components of blood are
48
New cards
Plasma
_____ is composed of fluid, proteins, electrolytes and many other substances. The ________ proteins are albumin, clotting proteins and the globulins. The globulins include immunoglobulins.
49
New cards
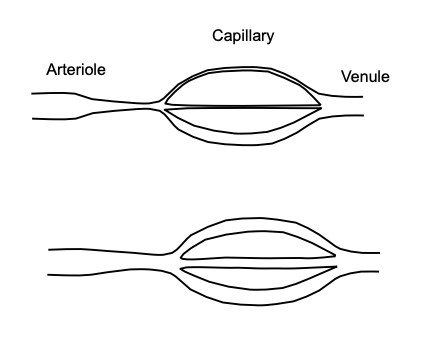
Capillaries
_____________ are composed of endothelial cells that form a barrier between the intravascular space and the extravascular space
50
New cards
Blood pressure
____________ is created by elastic and muscular forces exerted by the vessel wall (peripheral resistance) and the heart (cardiac output) such that __________________ equals peripheral resistance times cardiac output.
51
New cards
Arteries
Blood pressure is highest in the ___________.
* __________ divide into smaller vessels until the capillary bed is reached.
* __________ divide into smaller vessels until the capillary bed is reached.
52
New cards
lymphatic system
Excessive fluid in the extravascular space is removed by a specialized vascular system called the _________________.
53
New cards
Edema
________ is an excessive amount of fluid in a tissue (interstitial or extracellular space) or a body cavity or space. Another name for excess fluid in a body cavity is effusion.
* formed when more fluid enters the interstitial space between the cells than is being removed.
* formed when more fluid enters the interstitial space between the cells than is being removed.
54
New cards
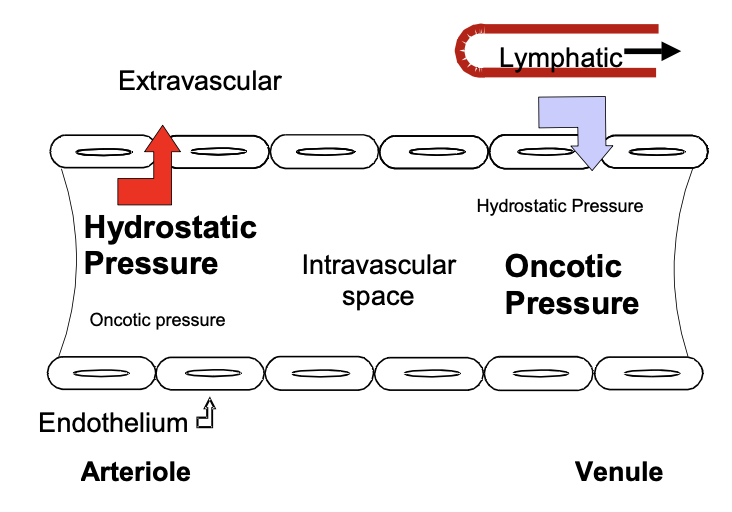
increased, reduced, increased, lymphatic, increased
The usual mechanisms and causes of edema are
1. __________ venous hydrostatic pressure
(postural edema and heart failure
2. __________ intravascular oncotic pressure
(hypoproteinaemia)
3. ___________ endothelial permeability
(inflammation)
4. ___________ obstruction (lymph node removal)
5. __________ total body water/sodium retention (menses, renal failure)
1. __________ venous hydrostatic pressure
(postural edema and heart failure
2. __________ intravascular oncotic pressure
(hypoproteinaemia)
3. ___________ endothelial permeability
(inflammation)
4. ___________ obstruction (lymph node removal)
5. __________ total body water/sodium retention (menses, renal failure)
55
New cards
Inflammatory edema (edema of inflammation)
_________________________ is the most common cause of edema and it is mostly the result of altered permeability of the endothelium. Direct damage to the endothelium, as in burns, increases permeability.
56
New cards
Noninflammatory edema
_______________________________ occurs when there are alterations to the forces at the venous end of the capillary, either with a reduction in oncotic pressure or an increase in venous hydrostatic pressure.
57
New cards
increased hyrdrostatic pressure
In people, edema is often caused by **___________________________** on the venous side, either by venous obstruction by postural causes or heart failure.
58
New cards
hypoproteinemia
Another major cause of edema is **______________**, a reduced amount of protein (usually albumin) in the blood.
59
New cards
hypoalbuminaemia
With ___________________, oncotic pressure in the intravascular space is reduced, and there is less attraction for fluid to re-enter the blood vascular system.
60
New cards
Kwashiorkor
Children that are severely malnourished are hypoproteinaemic and may have a ‘pot belly’ (ascites) and peripheral edema. The condition is called _____________. Other causes of hypoproteinemia include protein-losing renal and intestinal disease.
61
New cards
Sodium and water retention; sodium
Another common cause of edema is **____________________**. This occurs in people with renal disease and frequently with women of childbearing age where hormonal changes (aldosterone) associated with menstruation results in the retention of _________, an increase in the total extracellular fluid of the body, and the so-called bloated feeling and appearance.
62
New cards
lymphatic obstruction
The final cause of edema seen in people is **______________________**.
* occurs when a lymph node is removed in the staging of cancer, and the lymphatic vessel is therefore obstructed.
* occurs when a lymph node is removed in the staging of cancer, and the lymphatic vessel is therefore obstructed.
63
New cards
elephantiasis
* Less common these days is the disease called _______________. It is caused by a parasite that lives within the lymphatics of the legs. In either of these two cases, the tissues drained by an obstructed lymphatic vessel develop edema.
64
New cards
Hyperaemia
__________ is anactive process where the arteriole opens to allow a greater amount of blood into the capillary beds of a tissue. Nerves or chemicals (chemokines) cause the sphincter to open, usually in response to an injury or some other stimulus.
* ex. blushing
* ex. blushing
65
New cards
congestion
_____________ is a passive process where blood builds up in capillaries and is usually caused by obstruction of veins.
66
New cards
Haemorrhage
____________ is a very dramatic vascular disturbance. Haemorrhage means the release of blood or red blood cells from the vascular system.
* is a swelling (-oma) of blood.
* is a swelling (-oma) of blood.
67
New cards
External haemorrhage
____________________is visible outside the body or within the stomach and intestines.
68
New cards
internal haemorrhage
_____________________ is into body cavities or
into tissues.
into tissues.
69
New cards
a haematoma, an ecchymosis, petechia (smallest)
Internal haemorrhage into tissues will form
70
New cards
Ecchymosis
_________ is a variant in between petechia and haematoma. ___________ is a group of petechia that appear as though blood was wiped on the tissue with a paintbrush - they are often also called paintbrush haemorrhages.
71
New cards
Thrombus; postmortem clot
A **__________** is a blood clot that develops within the vessels of a living organism. The clot that forms in vessels after death is called the **_________________.**
72
New cards
Haemostasis'; endothelial cells, platelets, coagulation proteins
**_____________** or the stopping of haemorrhage is a normal function of the blood. The three major components to haemostasis are __________________________________
73
New cards
Endothelial cells; procoagulative
**______________** are very active in haemostasis.
* They are normally anticoagulation.
* When endothelial cells are damaged, they become ________________ and this is a responsive mechanism to ensure that any breach of the endothelium is dealt with very quickly so there is a minimal loss of blood.
* They are normally anticoagulation.
* When endothelial cells are damaged, they become ________________ and this is a responsive mechanism to ensure that any breach of the endothelium is dealt with very quickly so there is a minimal loss of blood.
74
New cards
Thromboplastin or Factor III
When damaged endothelial cells release tissue factor (_________________________) which is the major procoagulative factor.
75
New cards
Platelets
___________ are cell membrane bound fragments of the cytoplasm of megakaryocytes of the bone marrow. They circulate in the blood stream in high numbers.
* ____________ recognize breaches in the endothelial layer, adhere to collagen and extracellular matrix, secrete substances such as thromboxane that further stimulate platelet function, and they aggregate to form a temporary or primary plug.
* ____________ recognize breaches in the endothelial layer, adhere to collagen and extracellular matrix, secrete substances such as thromboxane that further stimulate platelet function, and they aggregate to form a temporary or primary plug.
76
New cards
Aggregation
___________ is facilitated by the plasma protein fibrinogen. A deficiency of platelets usually manifests itself by petechial haemorrhages.
77
New cards
Coagulation proteins; coagulation
__________________ are found in the blood, and most are produced in the liver. They form a _____________ cascade. These proteins circulate in an inactive form and are usually activated at a phospholipid surface
78
New cards
Calcium
__________ is an essential component in haemostasis and some anticoagulants bind calcium. A deficiency of factors in the coagulation cascade can cause prolonged bleeding including nose bleeds and hematoma formation.
79
New cards
Thrombogenesis; endothelial injury, altered blood flow, hyper coagulable states
______________ is the process whereby blood clots are formed. There are several situations where thrombogenesis commonly occurs:_________________________________
80
New cards
Endothelial Injury
________________ such as occur with atherosclerosis or trauma, induces the endothelium to become procoagulant. Tissue factor and Factor VII combine to initiate coagulation.
81
New cards
Altered blood flow
________________ can induce the formation of thrombi. Stagnation of blood, especially in the legs of people after surgery, allows anticoagulant substances normally in the blood to be exhausted. Without continuous resupply, thrombi may form.
82
New cards
Hypercoagulability
__________________ is where the blood becomes increasingly susceptible to coagulation. They include exposure to smoke, obesity, travelling or sitting for long periods, suffering from chronic diseases, having major surgery or injury and suffering from some forms of cancer.
83
New cards
disseminated intravascular coagulation (DIC)
The ultimate expression of thrombogenesis is a condition of hypercoagulability where there are widespread (disseminated) thrombi (intravascular coagulation) that is commonly called **______________________________.**.
84
New cards
Embolism
__________ is a general term to denote a clustering or aggregation of a substance within the blood stream.
* Other emboli include bubbles of gas (the bends), air, bone marrow (a complication of a fracture), or clusters of neoplastic cells.
* Other emboli include bubbles of gas (the bends), air, bone marrow (a complication of a fracture), or clusters of neoplastic cells.
85
New cards
Shock
_______ is a circulatory disturbance that is a widespread hypoperfusion of tissues resulting from reduced cardiac output and or reduced effective circulating blood volume.
86
New cards
1. cardiogenic shock - There is failure of the
heart to pump blood.
2. Hypovolaemic shock -
3. Blood maldistribution - there is reduced
peripheral vascular resistance and pooling of blood in the peripheral circulation. causes include neurogenic shock, anaphylactic shock, septic shock
Shock can be divided into:
87
New cards
the extent of damage, the tissue, and host factors.
Repair begins immediately - within seconds. The form of the repair is dependent on
88
New cards
Inflammation
____________ is the phase where the injurious substance is neutralized or removed, and sets in motion the events that permits reconstitution.
89
New cards
Repair
_______ is this reconstitution of the damaged tissue by **regeneration** of the original tissue, or **replacement** of tissue with fibrous tissue (scarring).
90
New cards
plasma and WBC
The basic components of inflammation are
91
New cards
white blood cells
The **__________________** are the cellular components of inflammation that include the neutrophils (because they do not stain with acid or basic stains), monocytes, platelets, eosinophils (stain with acidophilic stains such as eosin), and lymphocytes.
92
New cards
Acute inflammation
__________________ typically lasts minutes to days and is dominated by the components of plasma and neutrophils.
93
New cards
Chronic inflammation
____________________ takes much longer, is dominated by lymphocytes, plasma cells and macrophages, and usually has an element of fibrosis.
94
New cards
Chemical mediators
Inflammation is driven by chemicals, and these chemicals are called the **_________________** of inflammation (also called chemokines). They are responsible for orchestrating the response, controlling the response, and finally resolving the response.
95
New cards
rubor, or redness, tumour or swelling, calor or heat, dolor or pain, and loss of function.
The clinical signs of inflammation are based on the **cardinal signs**. These include
96
New cards
vascular; permeability; cellular
There are three main components of acute inflammation:
1. **_________** changes that result in increased blood flow,
2. increased **_____________** of the microvasculature, and
3. **________** changes that result in leukocyte emigration and accumulation.
1. **_________** changes that result in increased blood flow,
2. increased **_____________** of the microvasculature, and
3. **________** changes that result in leukocyte emigration and accumulation.
97
New cards
chemotaxis
The leukocytes, especially neutrophils, are attracted to the site of injury by chemicals and the process is called **____________**. Neutrophils swarm to bacteria or whatever chemotactic factor is present.
98
New cards
phagocytosis
Once a neutrophil or macrophage has recognized a foreign agent or substance, it attaches to that substance, engulfs it, and kills or degrades it. This process of recognition, attachment, engulfment, and killing or degradation is called **_____________**.
99
New cards
mediators
_________ are very tightly regulated and are
very short lived because many of them may have harmful effects particularly if they are produced to excess.
very short lived because many of them may have harmful effects particularly if they are produced to excess.
100
New cards
Histamine
________ is one of the most well-known mediators of inflammation. __________ and like substances are produced by mast cells in tissues. They are vasodilatory and they increase permeability.
Antihistamines are used to inhibit them.
Antihistamines are used to inhibit them.