Lymphatic System Study Guide
1/156
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
157 Terms
pathogenic
disease causing
immune system
cell pop that inhabit all organs/defends the body from agents of disease
lymphatic system
network of organs and vein like vessels
functions of the lymphatic system
fluid recovery, immunity, lipid absorption
fluid recovery
fluid continually filters from the blood capillaries to tissue space
immunity
excess filtered fluid picks up foreign cell/chem from the tissues
lipid absorption
lacteals in small intestine absorbs dietary lipids that are not absorbed by blood capillaries
edema
swelling of body tissues caused by excess fluid trapped inside them
lymphedema
a chronic condition characterized by, usually, arm or leg swelling caused by a buildup of protein-rich lymph fluid when the lymphatic system is damaged or blocked, often after cancer treatment
elephantiasis
a tropical parasitic disease caused by microscopic, thread-like worms transmitted through mosquito bites
components of the lymphatic system
lymph, lymphatic vessels, lymphatic tissues, lymphatic organs
lymph
recovered fluid, clear colorless fluid, similar to plasma but contain much less protein
lymphatic vessels
transport the lymph
lymphatic tissues
composed of aggregated of lymphocytes and macrophages that populated many organs in the body
lymphatic organs
defense cells are especially conc in these organs
separated from surrounding organs by connective tissues capsules
lymphatic capillaries
closed at one end
tethered to surrounding tissue by protein filament
endothelial cell loosely overlapped
allow bacteria/cells entrance to lymphatic capillary
create valve like flaps that open when interstitial fluid pressure is high, close when low
route of lymph flow
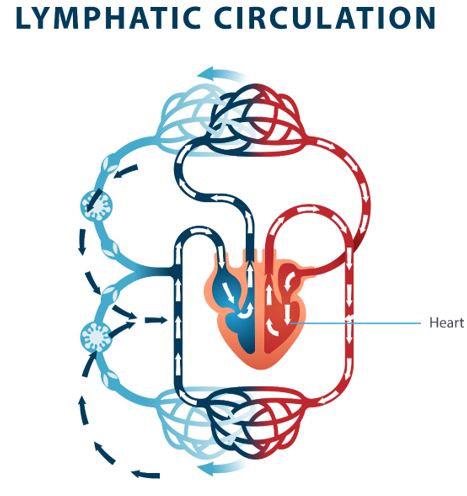
collecting vessels
course through many lymph nodes
6 lymphatic trunks
drain major portion of body (jugular, subclavian, bronchomediastinal, intercostal, intestinal, lumbar)
right lymphatic duct
union of right jugular, subclavian, bronchomediastinal lymphatic trunks
thoracic duct
on left side, larger/longer
begins as prominent sac in abdomen-cisterna chyli
receives lymph from below diaphragm, left arm, left side of head, neck, thorax
pathway of lymph flow from the right arm, left head and from the left leg
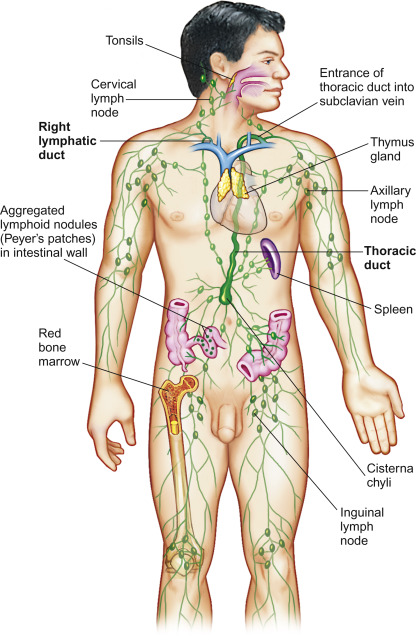

lymph flow at ___ and ___
low pressure, speed
each collecting ducts drain to ___
subclavian vein
valves
prevent backwards flow
moved along primarily by ___ of lymphatic vessels
rhythmic contractions
flow aided by ___
skeletal muscle pump
thoracic pump
aid flow from abdominal to thoracic cavity
rapidly flowing bloodstream
subclavian veins draws lymph to it
exercise significantly inc lymphatic return
lymphatic (lymphoid) tissue
aggregations of lymphocytes in mucous membrane/various organs
diffuse lymphatic tissue
simplest form
lymphocytes are scattered
prevalent in body passages open to exterior (respiratory, digestive, urinary, reproductive tracts)
lymphatic nodules (follicles)
dense mass of lymphocytes/macrophages that congregate in response to pathogens
lymph nodes: tonsils, appendix
payer patches
dense clusters in the ileum
primary lymphatic organs
red bone marrow and thymus
site where T and B cells become immunocompetent
able to recognize/respond to antigens
secondary lymphatic organs
lymph nodes, tonsils, spleen
immunocompetent cells populate these tissues
red bone marrow involved in
hemopoiesis-blood formation
immunity
thymus
very large in fetus
after age 14 begins involution(shrinkage)
elderly mostly composed of fatty/fibrous tissue
member of both endocrine/lymphatic system
contains developing T-lymphocytes
secrete hormones that regulate T-cells developement (thymopoientin/ thymosins)
capsules gives off trabeculae, divide parenchyma to cortex and medulla
label a lymph node
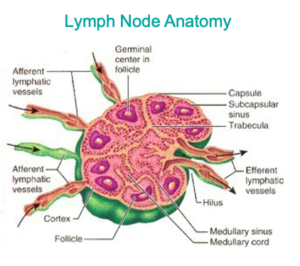

lymph nodes
organs that filter lymph and acts as T and B cell activation
mostly numerous lymphatics organs (450 in adults)
enclose with fibrous capsule with trabeculae that divide interior to compartments
stroma of reticular fibers/reticular cells
fewer efferent vessels, slow flow through nodes
reticular cells/macrophages phagocytize foreign matter
lymphocytes respond to antigens
common sites for metastatic cancer
tonsils
covered by epithelium
pathogens get into deep pits (crypts), encounters lymphocytes
there are 5
palatine tonsils
pair at the posterior margin of oral cavity
most common infected
tonsillitis-inflammation of tonsils
tonsillectomy- removal of tonsils
lingual tonsils
pair at the root of tongue
pharyngeal tonsil (adenoids)
single tonsil on back wall of nasopharynx
spleen
inferior to diaphragm, dorsal to stomach
highly vascular-vulnerable to trauma
ruptured spleen requires splenectomy
spleen diagram
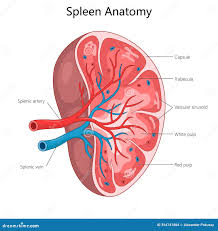
red pulp
sinuses filled with erythrocytes
white pulp
rich in lymphocytes, macrophages
functions of spleen
blood production in fetus
blood reservoir
RBC disposal
immune reactions- filters blood/quickly to detect antigens
first line of defense
external barriers: skin, mucous membranes
second line of defense
non specific defense
leukocytes/macrophages, antimicrobial proteins, immune surveillance, inflammation, fever
effective against broad range of pathogens
third line of defense
immune system
defeat pathogen and leaves the body with memory so it can defeat it faster in the future
nonspecific defenses
broadly effective, no prior exposure
external barriers
inflammation,fever
specific defenses
results from prior exposure
protects against 1 particular pathogen
immune system
external barriers
skin, mucous membrane, subepithelial areolar tissue
skin
dry/poor nutrient
toughness of keratin
defensins-peptides attack microbes
lactic acid- component of sweat
mucous membrane
stickiness of mucus
lysozyme-enzyme destroy bacterial cell wall
subepithelial areolar tissue
tissue gel is a viscous barrier of hyaluronic acid
hyaluronidase- enzyme used by pathogen to circumvent hyaluronic acid defenses
phagocyte
WBC that engulf/absorb waste material in the blood stream/tissue
5 types of leukocytes
neutrophils, eosinophils, basophils, monocytes,lymphocytes
neutrophils
wander in tissue/phagocytize bacteria
create killing zone
degranulation- lysosome discharge to tissue fluid, trigger respiratory burst
create O2-, H2O2
eosinophils
found in mucous membrane
phagocytize antigen-antibody complexes, allergens, inflammatory chem
block excess inflammation, limit action of histamine
antiparasitic effects- aggregate/release enzymes to parasites
basophils and mast cells
aid mobility/action of WBC by release of histamine,heparin,leukotrienes
histamine (vasodilator)
inc blood flow to infected tissue
heparin (anticoagulant)
prevent immobilization of phagocytes
leukotrienes
activate/attract other leukocytes
lymphocytes %
contains 80% T-cells, 15% B-cells, 5% NK cells
T/B cells are part of ___ immune response
specific
natural killer (NK) are ___ specific
non
monocytes
move from blood to connective tissue/transform to macrophages
macrophages
phagocytic cells
wandering macrophages
actively seek pathogens
widely distributed in loose connective tissue
fixed macrophages
only phagocytize pathogens that come to them
microglia-central nervous system
alveolar macrophages(dust cells)-lungs
hepatic macrophages- liver
interferons
polypeptides secreted by cells invaded by viruses
antiviral effect
don’t benefit the cell that secrete them
interferons diffuse to neighboring cell/stimulate them to produce antiviral proteins
activate NK cells/macrophages, destroy infected host cells
anticancer effect
activated NK cells can destroy cancer cells
4 method of pathogen destruction
inflammation, immune clearance, phagocytosis, cytolysis
3 routes of complement activation
classical, alternative, lectin pathways
Membrane Attack Complex
creating holes in target cell
electrolytes leak out, water flow in rapidly →cell rupture
complement protein form ring in plasma membrane of target cell causing cytolysis
immune surveillance
phenomenon in which natural killer cells continually patrol the body on the lookout for pathogens/disease host cell
fever
promotes interferon activity
accelerate metabolic rate/tissue repair
inhibit pathogen reproduction
fever over 104F can be dangerous
antipyretics
fever reducing medications inhibit PGE2
stage of fever
onset (body temp rise), stadium(body temp oscillate), defervescence (body temp returns to normal)
Reye syndrome
serious disorder in children younger than 15 following an acute viral infection such as chickenpox/influenza
swelling of brain neurons, fatty infiltration of liver/other viscera, pressure of swelling brain
can be triggered by aspirin
inflammation
defensive response to tissue injury
limit spread of pathogens, destroys them, removes debris, initiates tissue repair
-itis suffix
cardinal sign of inflammation
redness(erythema)-caused by hyperemia (inc blood flow)
swelling (edema)- cause by inc capillary permeability/filtration
heat-caused by hyperemia
pain (-algia)- caused by inflammatory chem secreted by damaged cell, pressure on nerves
cytokines
class of chems that regulates inflammation/immunity
secreted mainly by leukocytes
alter physiology/behavior of receiving cell
act at short range, neighboring cells (paracrines) or same cell that secrete them (autocrines)
includes: interferons, interleukins, tumor necrosis factor, chemotactic factors ,etc
3 major process of inflammation
mobilization of body defenses, containment/destruction of pathogens, tissue cleanup/repain
what happens in the first phase of inflammation – mobilization of defenses
most immediate req for dealing with tissue injury to get the defensive leukocytes to the site quickly
hyperemia
inc blood flow
local vasodilation due to vasoactive chems
margination
leukocytes adhere to blood vessel wall
diapedesis/emigration
leukocytes crawl through gaps in endothelia cells/enter tissue fluid
endothelia cells separate causing ___
inc capillary permeability
fibrinogen
filters into tissue fluid gets activated to form fibrin
clot
forms sticky mesh that walls off microbes
heparin
prevents clotting at injury site
edema
contributes to tissue cleanup
swelling compresses veins/reduces venous drainage
force open valves of lymphatic capillaries, promoting lymphatic drainage
lymphatics collect/remove bacteria, dead cells, proteins, tissue debris better than blood capillaries
specificity
immunity directed against a particular pathogen
memory
reexposed to the same pathogen, body reacts so quickly that there is no noticeable illness
humoral immunity
antibody mediated
cellular immunity
cell mediated