A&P II Respiratory system
1/145
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
146 Terms
respiratory system
organ system that takes in air and expels if from the body
respiration
ventilation of the lungs (breathing)
gas exchange, communication, olfaction, acid-base balance, blood pressure regulation, blood and lymph flow, platelet production, blood filtration, and expulsion of abdominal contents
functions of the respiratory system
gas exchange
oxygen and carbon dioxide exchanged between blood and air
communication
speech and other vocalizations
olfaction
sense of smell
acid-base balance
influences pH of body fluids by eliminating carbon dioxide
blood pressure regulation
assists with synthesis of angiotensin II, a hormone that regulates blood pressure
blood and lymph flow
breathing creates pressure gradients between thorax and abdomen that promote flow of lymph and blood
platelet production
more than half of platelets are made by megakaryocytes in lungs
blood filtration
lungs filter small clots
expulsion of abdominal contents
breath-holding assists in urination, defecation, and childbirth
nose, pharynx, larynx, trachea, bronchi, and lungs
priciple organs of the respiratory system
conducting zone
passages that serve only for airflow (no gas exchange)
respiratory zone
regions that participate in gas exchange
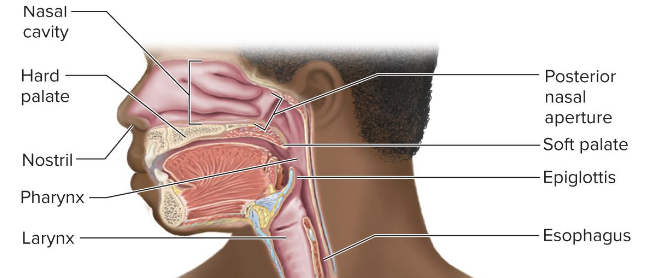
upper respiratory tract
airway from nose through larynx (nose, pharynx, and larynx)
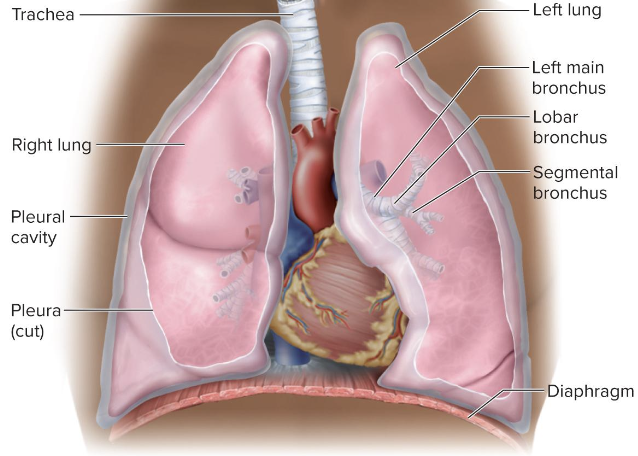
lower respiratory tract
regions from trachea through lungs (trachea, bronchi, lungs)
nose
warms, cleanses, and humidifies inhaled air; detects odors; and serves as a resonating chamber that amplifies voice
nasal bones and maxillae
superior half of nose
hyaline cartilage
inferior half of nose
nasal septum
divides nasal cavity into right and left nasal fossae
vestibule
small, dilated chamber just inside nostrils, lined with stratified squamous epithelium
guard hairs or vibrissae
stiff hairs that block insects and debris from entering nose
goblet cells
produce most of the mucus, supplemented by mucous glands in lamina propria
ciliated cells
have motile cilia that propel that mucus posteriorly toward pharyx to be swallowed
olafactory glands
secrete serous fluid to assist diffusion of odor molecules to receptors on the cilia
pharynx
muscular funnel extending about 13cm from posterior nasal apertures to larynx, divided into 3 regions
nasopharynx
posterior to nasal apertures and above soft palate; receives auditory tubes and contains pharyngeal tonsil; 90 degree downward turn traps large particles; passes only air and is lined by pseudostratified columnar epithelium
oropharynx
space between soft palate and epiglottis; contains palatine tonsils; passes air, food, and drink, and is lined by stratified squamous epithelium
laryngopharynx
posterior to larynx, from epiglottis to cricoid cartilage; espohagus begins at that point; passes air, food, and drink, and is lined by stratified squamous epithelium
larynx
cartilaginous chamber about 4cm long; primary function is to keep food and drink out of airway; also involved in production of sound, so commonly called the “voice box”
epiglottis
flap of tissue that guards superior opening of larynx; at rest, it stands almost vertically; during swallowing extrinsic muscles pull larynx upward; tongue pushes epiglottis down to meet it; closes airway and directs food to esophagus behind it; vestibular folds of the larynx play greater role in keeping food and drink out of the airway
epiglottic cartilage
most superior; spoon-shaped supportive plate in epiglottis
thyroid cartilage
shield-shaped and largest laryngeal cartilage; contains laryngeal prominence (Adam’s apple); testosterone stimulates growth, larger in males
cricoid cartilage
ring-like shape; connects larynx to trachea
vestibular folds
play no role in speech, but close the larnyx during swallowing; supported by the vestibular ligaments
vocal cords (vocal folds)
produce sound when air passes between them; contians vocal ligaments covered with stratified squamous epithelium, suited to endure vibration and contraction
glottis
the vocal cords and the opening between them
trachea
tube that connects larynx to bronchi; commonly called the “windpipe”; rigid tube 12cm long and 2.5cm in diameter; anterior to esophagus; supported by 16 to 20 C-shaped rings of hyaline cartilage- prevent collapse during inhalation; opening in cartilage rings faces posteriorly toward esophagus; allows esophagus to expand as swallowed food passes by
trachealis
muscle spans opening in rings; contracts or relaxes to adjust airflow
carina
lowermost tracheal cartilage has internal medina ridge
mucociliary escalator
mechanism for debris removal; mucus traps inhaled particles, upward beating cilia moves mucus to parynx to be swallowed
mucosa
lined by ciliated pseudostratified columnar epithelium; contains mucus-secreting cells, ciliated cells, and stem cells
submucosa
connective tissue beneath the tracheal epithelium contains lymphoid nodules, mucous and serous glands, and the tracheal cartilages
adventitia
outermost layer of trachea; fibrous connective tissue that blends into adventitia of other, nearby organs (esophagus)
tracheotomy
to make a temporary opening in the trachea and insert a tube to allow airflow; prevents asphyxiation due to upper airway obstruction
intubation
when a patient is on a ventilator, air is introduced directly into trachea; air must be filtered and humidified
base of lung
broad concave portion resting on diaphragm
apex of lungs
tip that projects just above the clavicle
costal surface
pressed against the ribcage
mediastinal surface
faces medially toward the heart
hilum
slit through which the lung receives the main branches, blood vessels, lymphatics, and nerves
right lung
shorter than left because liver rises higher on the right; has 3 lobes- superior, middle, and inferior lobes; horizontal fissure separates superior and middle lobes, and oblique fissure separates middle and inferior lobes
left lung
tall and narrow because the heart tilts toward the left and occupies more space on this side of mediastinum; has indentation to accomodate heart- cardiac notch; has 2 lobes- superior and inferior lobes, separated by a single oblique fissure
bronchial tree
a branching system of air tubes in each lung; expands from main bronchus to 65,000 terminal bronchioles
main (primary) bronchi
arise from fork of trachea; right main bronchus is wider and more vertical than left main bronchus
lobar (secondary) bronchi
a lobar bronchus serves each lobe of the lung; right main bronchus gives off 3 branches: superior, middle, inferior lobar bronchi; left main bronchus gives off 2 branches: superior and inferior lobar bronchi
bronchopulmonary segment
functionally independent unit of lung ventilated by a segmental bronchus
bronchioles
continuations of the airway that lack supportive carilage and are 1mm or less in diameter
pulmonary lobule
portion of lung ventilated by one bronchiole
alveolar sacs
clusters of alveoli around a central space
alveoli
microscopic air pouches in the lungs, each about 0.2 to 0.5 mm in. diameter
squamous (type 1) alveolar cells
thin cells allow rapid gas diffusion between air and blood; cover 95% of alveolar surface area
great (type 2) alveolar cells
round to cuboidal cells that cover the remaining 5% of alveolar surface; repair the alveolar epithelium when the squamous (type 1) cells are damaged; secrete pulmonary surfactant
pulmonary surfactant
mixture of phospholipids and proteins that coats the alveoli and prevents them from collapsing during exhalation
alveolar macrophages (dust cells)
most numerous of all cells in the lungs; wander lumens of alveoli and connective tissue between them; keep alveoli free from debris by phagocytizing dust particles; millions of dust cells die each day as they ride up the mucociliary escalator to be swallowed and digested witht their load of debris
respiratory membrane
thin barrier between the alveolar air and blood
pulmoary circiut
serves to unload carbon dioxide from blood so it can be exhaled, and pick up oxygen from inhaled air
bronchial arteries
arise from aorta, supply lung tissue with blood supply
bronchial veins
drains the blood into aztgos vein of thorax
right-to-left shunt
some bronchial venous blood mixes with pulmonary venous blood, diluting the oxygen content somewhat
pleura
serous membrane that lines thoracic wall and forms surface of lung
visceral pleura
forms surface of the lung
parietal pleura
adheres to mediastinum, inner surface of the rib cage, and superior surface of the diaphragm
pleural cavity
potential space between pleurae
pleural effusion
pathological seepage of fluid into the pleural cavity
reduaction of friction, creation of pressure gradient (assists with lung inflation), and compartmentalization (prevents spread of infection throughout organs)
functions of the pleurae and pleural fluid
diaphragm
prime mover of respiration
internal and external intercostal muscles
assist diaphragm
normal quiet respiration
energy-saving passive process achieved by the elasticity of the lungs and thoracic cage
valsalva maneuver
breathing technique used to help expel contents of certain abdominal organs
ventral respiratory group (VRG)
in medulla; primary generator of the respiratory rhythm
dorsal respiratory group (DRG)
in medulla; modifies the rate and depth of breathing
pontine respiratory group (PRG)
in pons; modifies rhythm of ventral respiratory group by outputs to both VRG and DRG; adapts breathing to special circumstances such as sleep, exercise, vocalization, and emotional responses
central chemoreceptors
brainstem neurons that respond to changes in pH of cerebrospinal fluid
peripheral chemoreceptors
cartoid and aortic bodies; respond to the oxygen and carbon dioxide and the pH of blood
stretch receptors
in smooth muscle of bronchi and bronchioles, and in the visceral pleura; respond to inflation of the lungs
inflation (Hering-Breuer) reflex
triggered by excessive inflation; protective reflex that inhibits inspiratory neurons and stops inspiration
irritant receptors
nerves endings amid the epithelial cells of the airway; respond to smoke, dust, pollen, chemical fumes, cold air, and excess mucus; trigger protective reflexes such as bronchoconstriction, shallower breathing, breath-holding (apnea), or coughing
breaking point
when carbon dioxide levels rise to a point where automatic controls override one’s voluntary will when holding breath
atmosperic (barometric) pressure
the weight of the air above us
intrapulmonary pressure
air pressure within lungs
boyle’s law
at a constant temperature, the pressure of a given quantity of gas in inversely proportional to its volume
intrapleural pressure
the slightly negative pressure that exists between the 2 pleural layers
charle’s law
the volume of a gas is directly proportional to its absolute temperature
bronchodilation
increase in diameter of bronchus or bronchiole; increases airflow
bronchoconstriction
decreases in diameter of bronchus or bronchiole; decrease airflow
pulmonary compliance
ease with which the lungs can expand; change in lung volume relative to a given pressure change
infant respiratory distress syndrome (IRDS)
premature babies lacking surfactant are treated with artificial surfactant until they can make their own
physiological (total) dead space
sum of anatomical dead space and any pathological dead space