Comprehensive HIV and Viral Infection Structure, Transmission, and Treatment
1/15
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
16 Terms
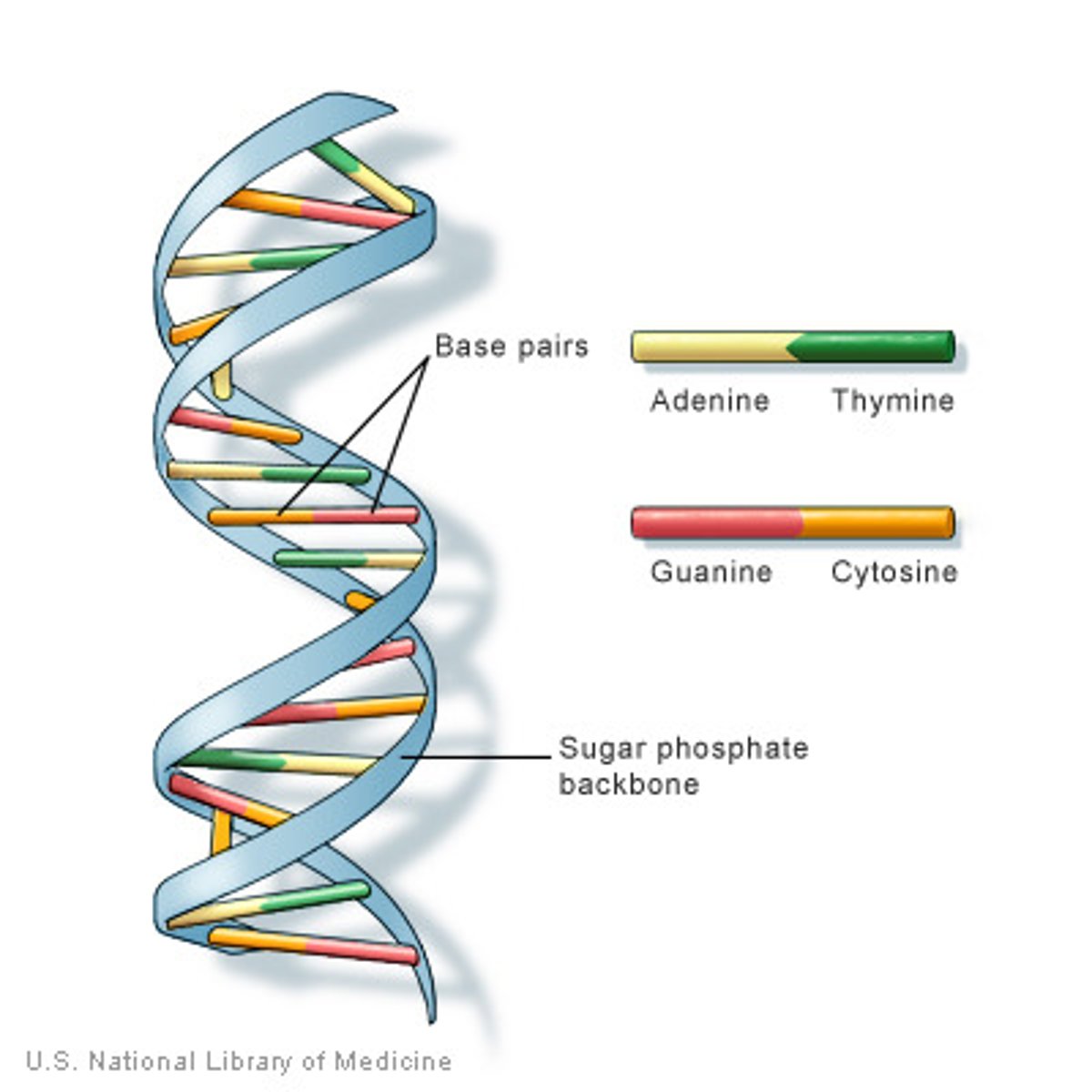
What is the basic structure of a Virion?
Genetic material (DNA or RNA) is contained within a protein coat called a capsid. Some viruses also have an outer lipid envelope derived from the host cell membrane.
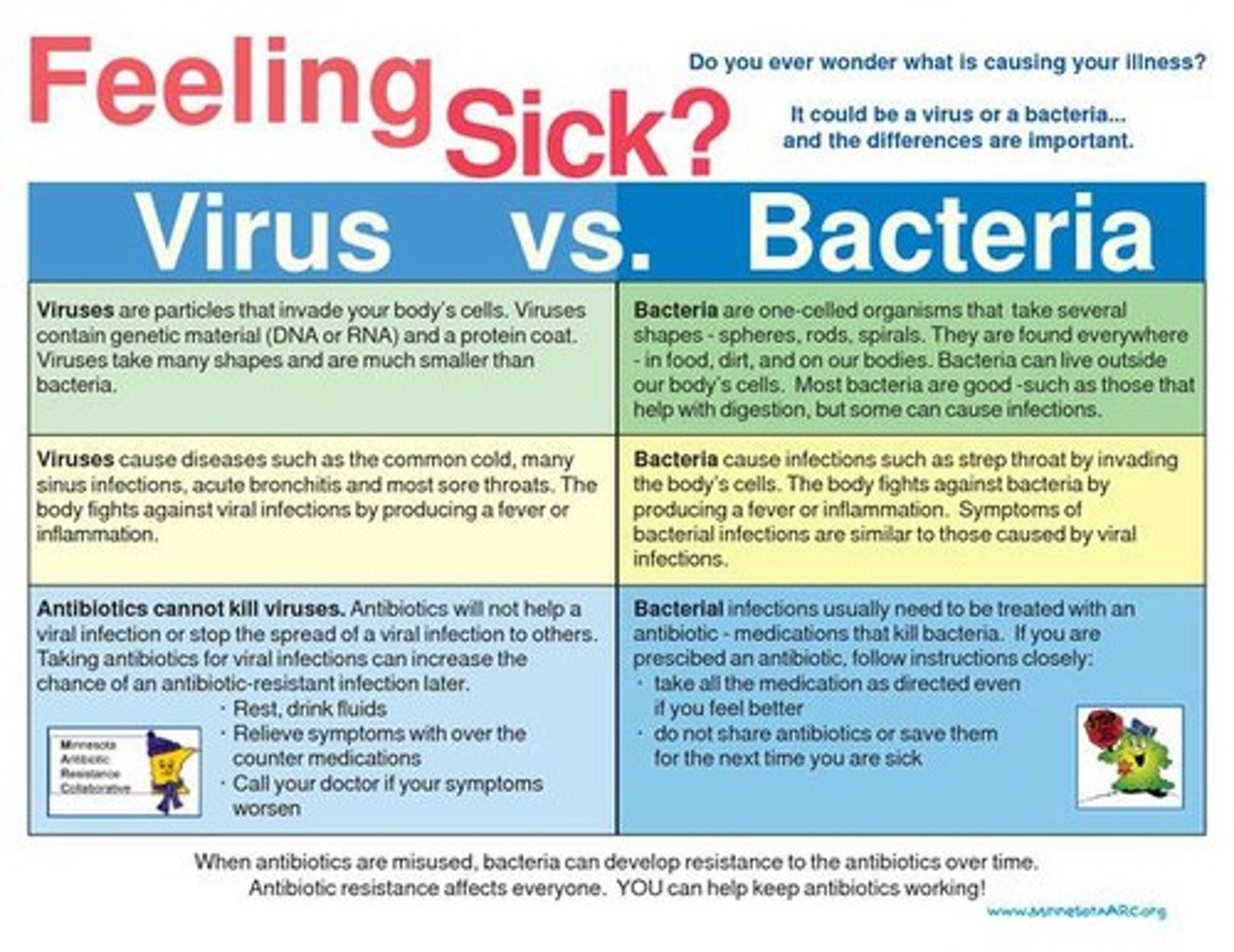
Why do antibiotics not work against viruses?
Viruses lack their own metabolic machinery (no cell wall, ribosomes, or independent replication). Antibiotics target bacterial structures that viruses do not possess.
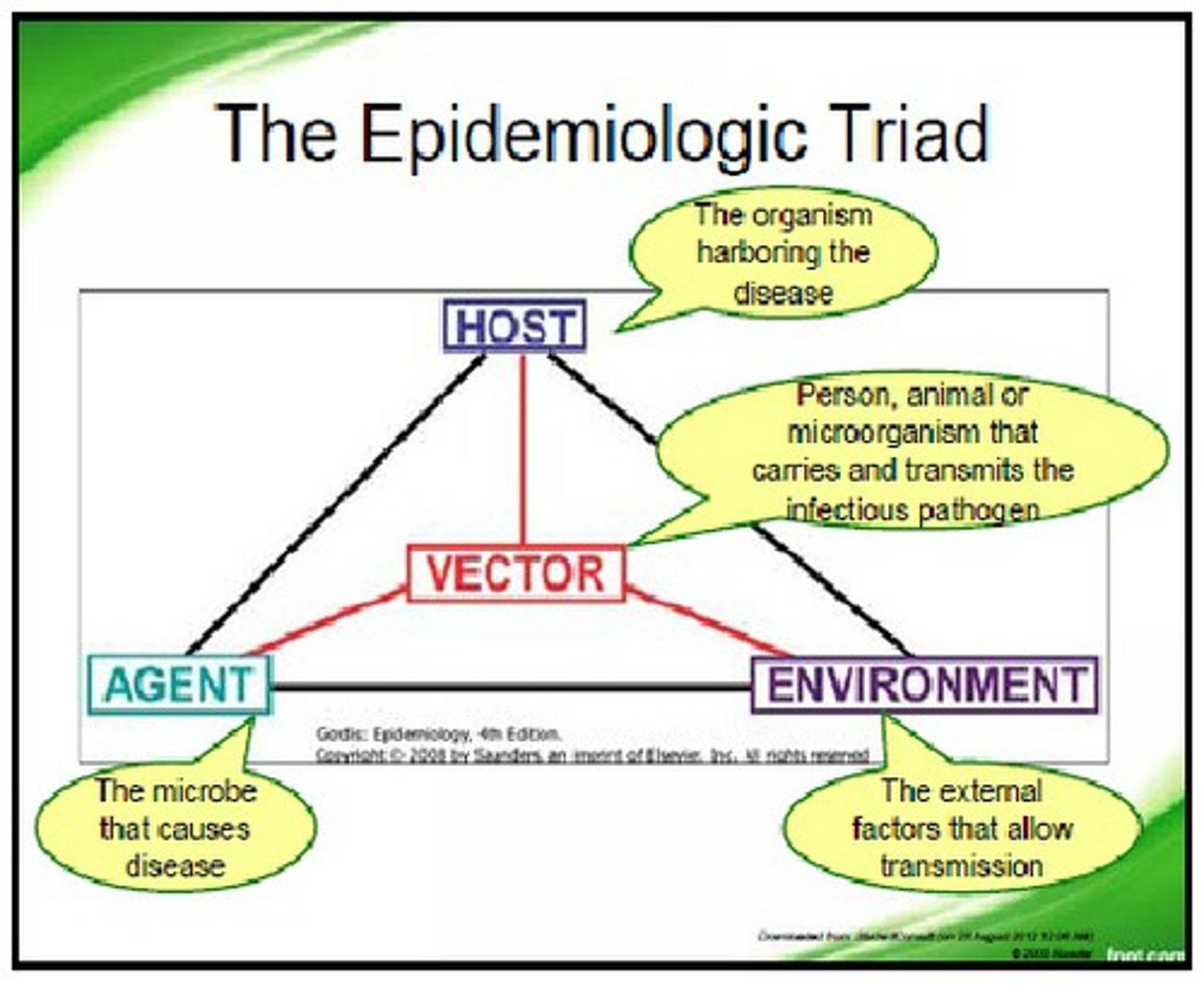
Define the Epidemiological Triad of viral spread.
The interaction between three factors: The Agent (the virus's infectivity/virulence), The Host (age, immune status, genetics), and The Environment (sanitation, climate, social behavior).
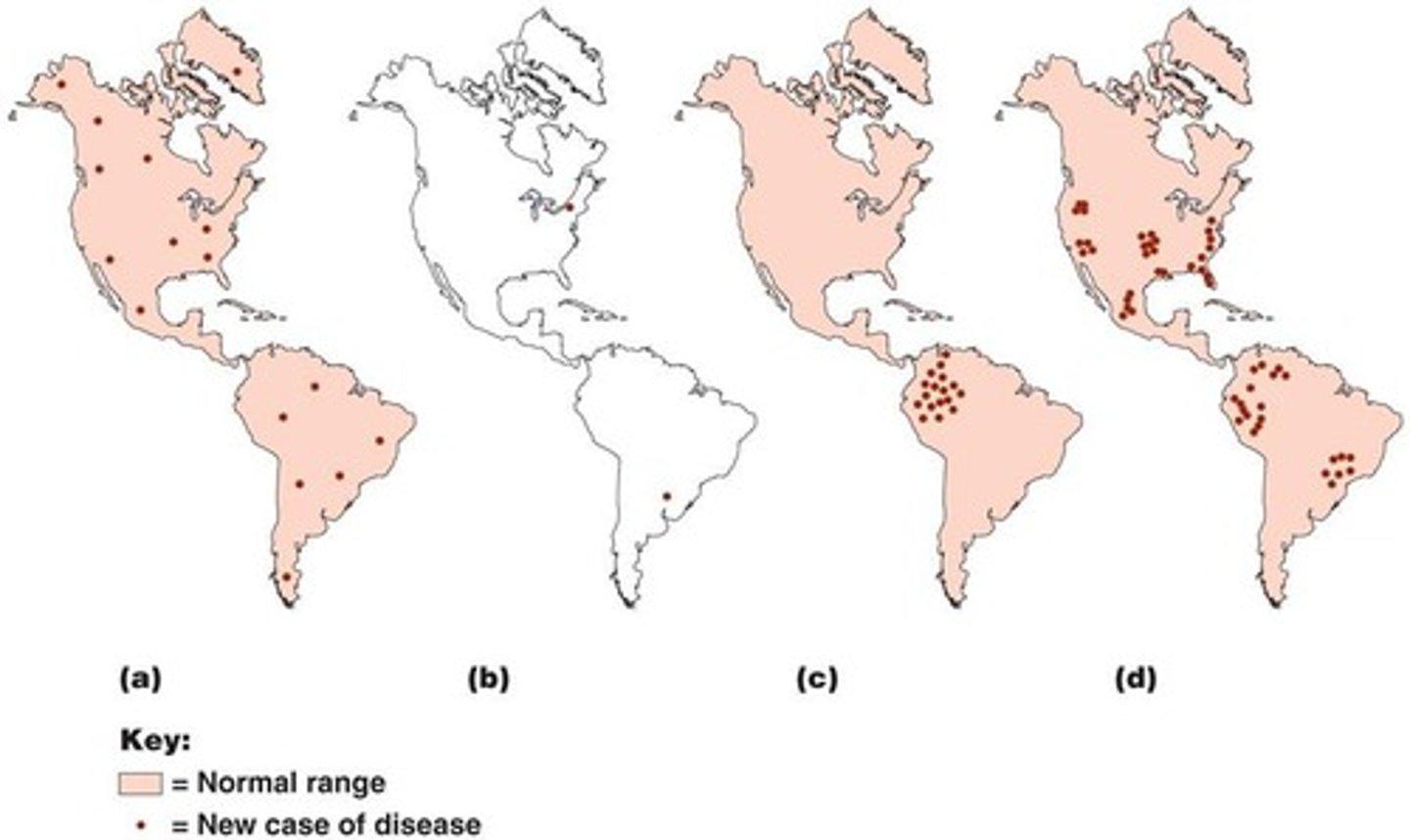
Define: Sporadic, Endemic, Epidemic, and Pandemic.
Sporadic: Irregular, occasional cases. Endemic: Persistent background level. Epidemic: Level exceeding expectations in a specific area. Pandemic: Epidemic spread over several countries or continents.
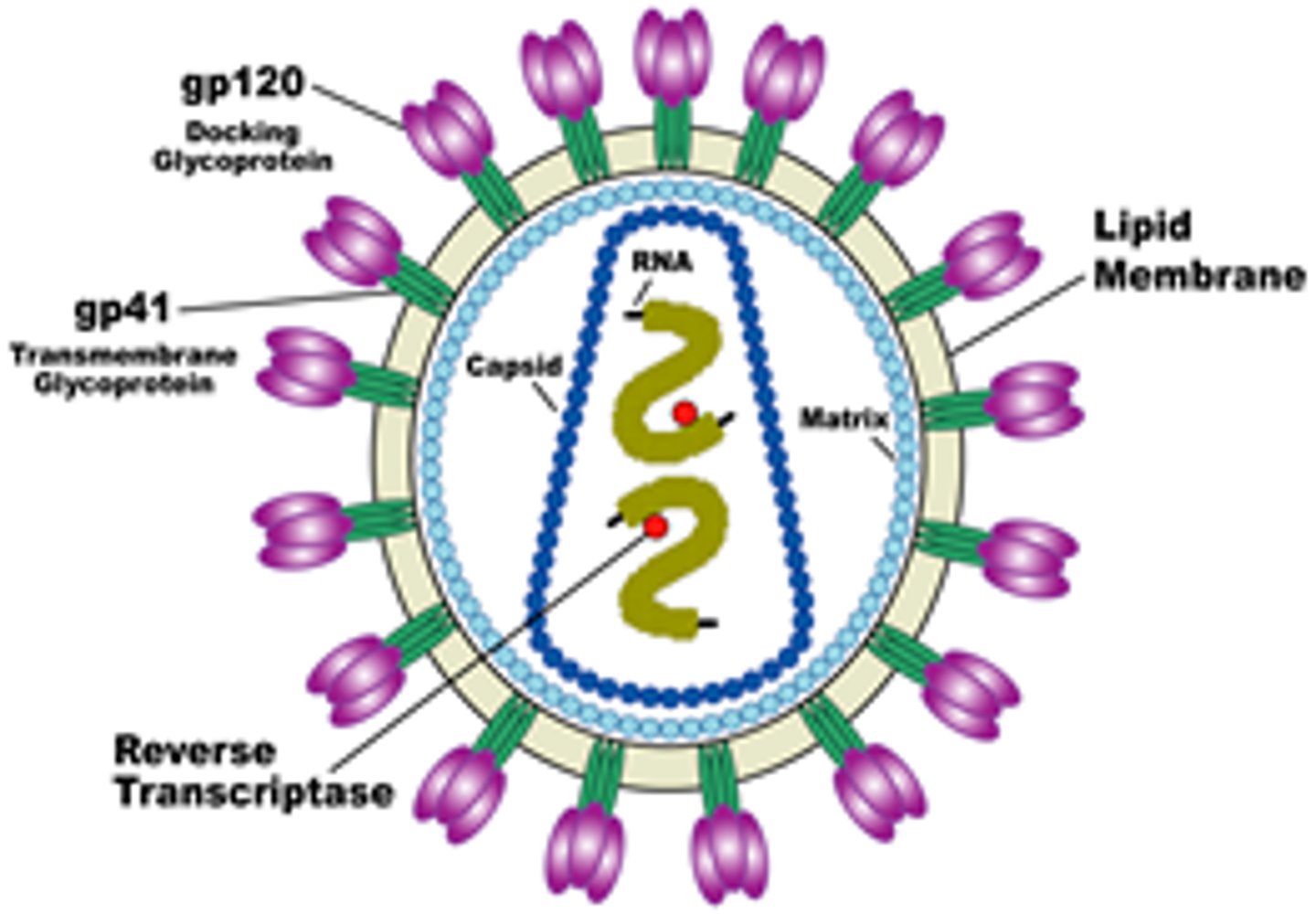
What are the key structural components of HIV?
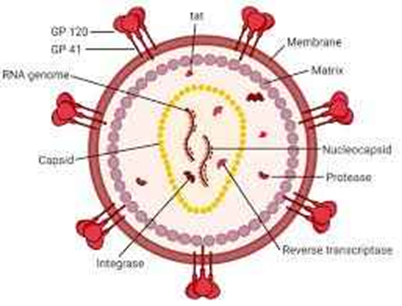
Envelope: Lipid membrane with gp120/gp41 (for cell entry). Capsid: Protein shell (p24). Genome: Two strands of RNA. Enzymes: Reverse Transcriptase, Integrase, and Protease.
How does HIV enter the host cell (The 'Lock and Key')?
Viral gp120 binds to the CD4 receptor (the lock) and a co-receptor (CCR5 or CXCR4). gp41 then mediates the fusion of the viral envelope with the host cell membrane.
How do host mutations (e.g., CCR5-Δ32) result in HIV resistance?
If the co-receptor (CCR5) is mutated or absent, the HIV 'key' cannot turn the 'lock.' The virus cannot fuse with or enter the cell, rendering the host naturally resistant.
Describe the Retroviral Replication Cycle.
Reverse Transcriptase converts viral RNA to DNA. Integrase inserts this DNA into the host genome. Protease cuts long protein chains into functional units for new virions.
Why is HIV infection persistent and currently incurable?
Because it integrates its DNA into the host's own genome, creating latent reservoirs that can remain dormant for years, evading both the immune system and drugs.
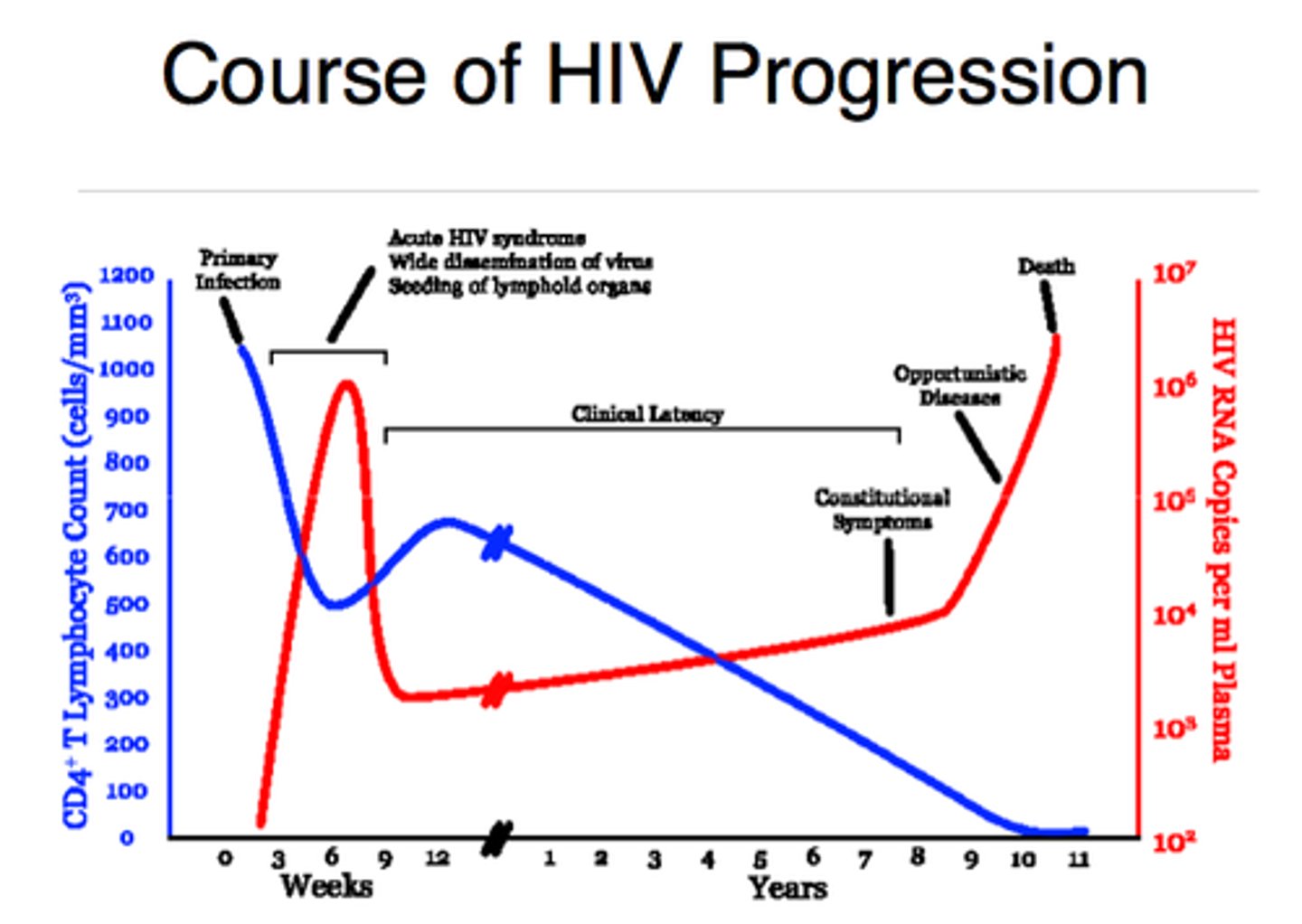
What is the primary clinical marker of HIV progression?
The CD4+ T-cell count. As the count drops (especially below 200 cells/mm³), the patient moves from the latent phase to AIDS, becoming vulnerable to opportunistic infections.
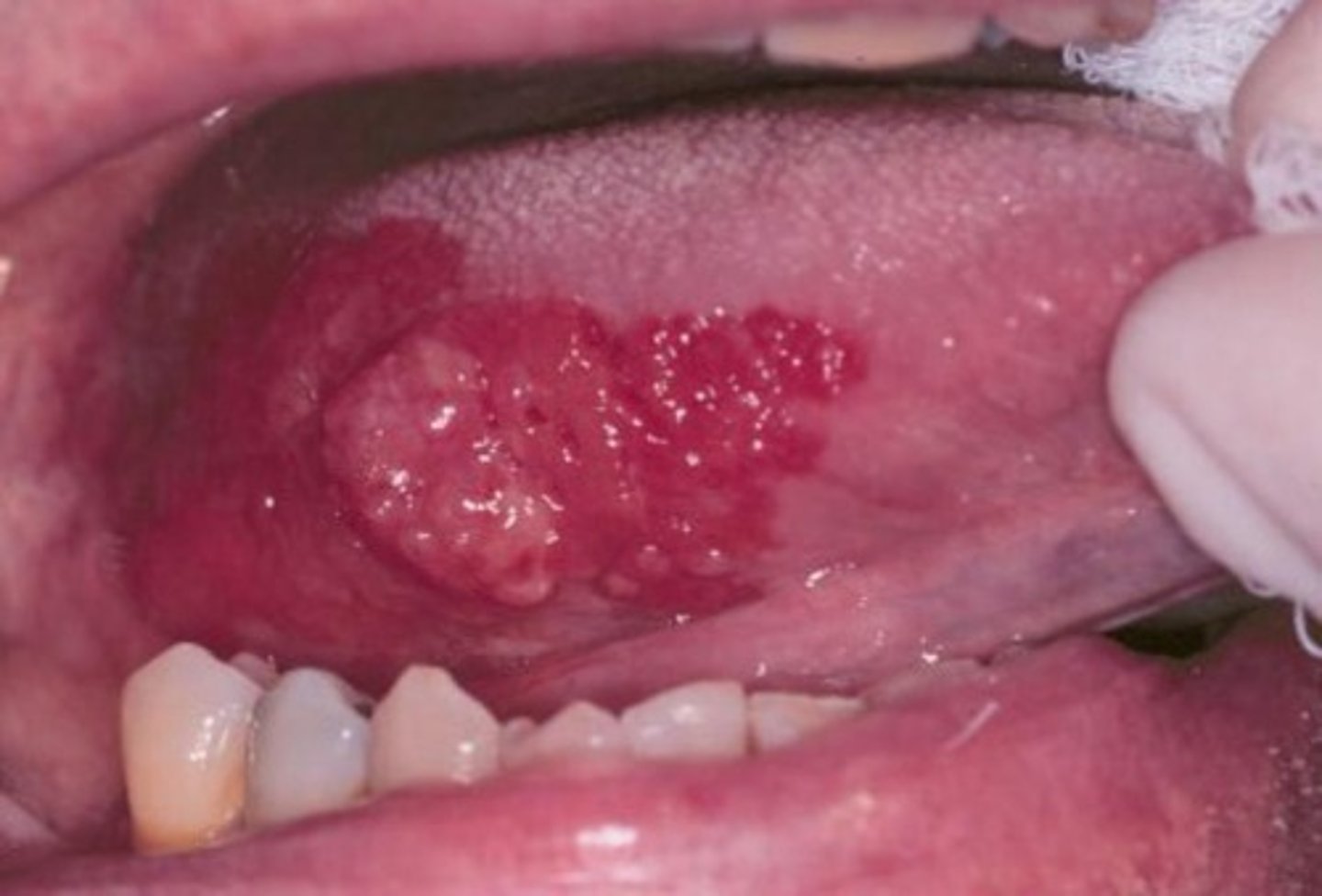
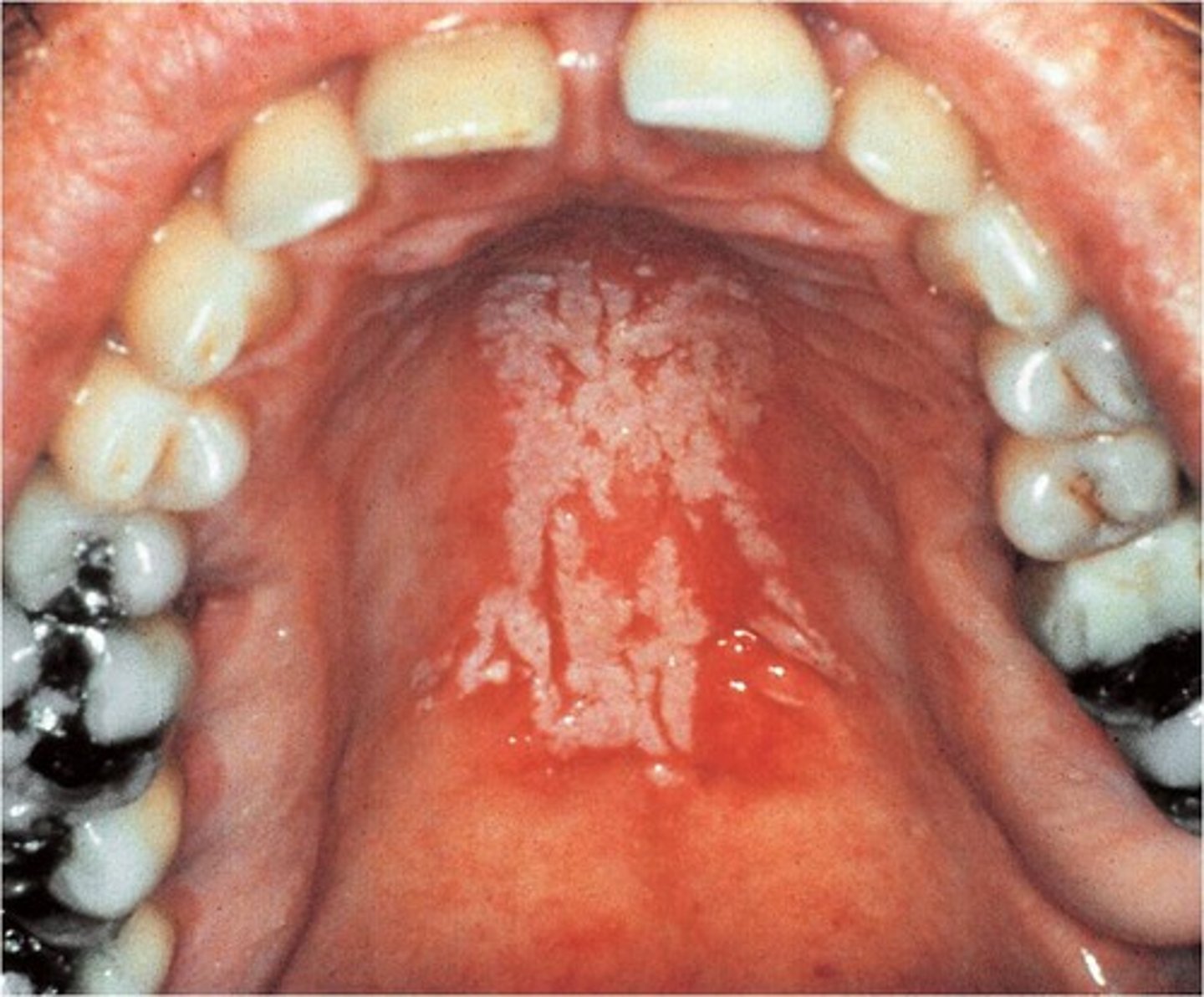
What are Opportunistic Infections and Cancers?
Diseases that take advantage of a crippled immune system, such as Pneumocystis pneumonia, Kaposi's Sarcoma, or EBV-related smooth muscle tumors.
How does ART (Antiretroviral Therapy) function?
It is a combination of drugs (e.g., NRTIs, Protease Inhibitors, Integrase Inhibitors) that block different stages of the life cycle, keeping the viral load 'Undetectable.'
What is the clinical significance of 'U=U'?
Undetectable = Untransmittable. A person with an undetectable viral load due to successful ART cannot sexually transmit HIV to partners.
How is HIV diagnosed in the laboratory?
Typically via a 4th-generation antibody/antigen (p24) test. Early diagnosis is vital to prevent the spread of the 'Window Period' and to initiate ART.
How does HIV stigma impact Global Health?
Stigma discourages testing and disclosure, leading to late diagnosis, mental health issues, and continued community transmission.
Why can a persistent headache be an 'AIDS-defining' symptom?
A chronic headache in an immunocompromised patient can signal EBV-related brain tumors or opportunistic meningitis, indicating the immune system can no longer control common viruses.