Lecture 37 - Dermal Infections and Nails
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
what are protective mechanisms of the skin
Epidermis forms protective barrier
Sebaceous glands secrete oily sebum providing an acidic pH of 5.5 that is unfavourable for microbial growth
Normal flora of the skin competes with potential pathogenic organisms
Effective immune cells: Langerhans cells, mast cells and macrophages in the dermis
what are the 4 main types of skin infections
bacterial
viral
fungal
parasitic
what are the most common bacteria causing skin infections
Staphylococcus and Streptococcus species.
what comorbidities increase susceptibility to bacterial infections
diabetes, vascular insufficiency, and being immunocompromised Intravenous drug use may increase risk
what are complications of bacterial skin infections
Skin breakdown
Abscess formation
Sepsis (can be life-threatening)
Septic emboli
Scarring or postinflammatory hyperpigmentation
Infections due to resistant bacteria (eg, methicillin-resistant Staphylococcus aureus/MRSA) may be more difficult to treat.
what is impetigo characterized by
Characterized by pustules and honey-coloured crusted erosions.
Secondary infection of wounds or other skin lesions with the same pathogens is called ‘impetiginization’.
Classified into non-bullous (starts with one lesion, limited erythema, lesions burst and form honey colored crust, patients generally feel well) and bullous impetigo (quick bullae formation, ruptures and oozes yellow fluid, systemic symptoms may be present)
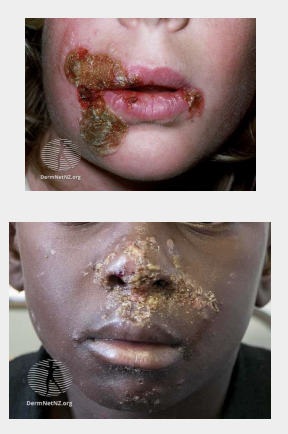
is impetigo contagious
yes
what organism causes impetigo
Staph aureus
Strep pyogenes
what is the appearance of impetigo as it develops
The first sign of impetigo is a patch of red, itchy skin. Pustules develop on this area, soon forming crusty, yellow-brown sores that can spread to cover entire areas of the face, arms, and other body parts.
how long does impetigo last
Impetigo is considered self-limiting (~2-3 weeks to heal) but antibiotics provide quicker resolution and prevents the spread
what are non-pharm treatments for impetigo
Avoid sharing clothing and towels
Frequent hand-washing, hot wash bedding, towels etc.
Avoid close contact with others when you have impetigo
Antiseptic washes to cleanse area may be recommended (chlorhexidine)
when is systemic antibacterial treatment needed for impitego
Patient has systemic symptoms (e.g.fever)
Widespread disease
Immunocompromised
Renal disease
Valvular heart disease
No improvement with topical treatment
what should be done before applying a topical antibacterial
impetigo crusts should be removed with warm water or saline compresses or soap-and-water washes
what topical antibiotics can be used for impetigo
Mupirocin
Fusidic acid
Polysporin®
how is mupirocin used for
Effective against gram-positive organisms only
Apply BID–TID × 5 days or until all lesions are healed
how is fusidic acid used
Effective against gram-positive organisms only
Apply BID–TID × 5 days or until all lesions are healed
how is polysporin used
E.g. polymyxin B, bacitracin, gramicidin and neomycin
Inferior to mupirocin and fusidic acid
Apply TID for up to 7 days or until all lesions are healed
when might recurrent impetigo occur
may occur when there is S. aureus carriage in the anterior nares or perineum
how should you treat a positive culture of impetigo
5-day eradication regimen consisting of topical mupirocin applied to the nares 2–3 times daily and daily washing with topical chlorhexidine or hexachlorophene (particularly the perineum and axilla)
what systemic antibiotics can be used for impetigo - MSSA
Usually 7 day regimen with any of the following: amoxicillin/clavulanate, cefadroxil, cephalexin and cloxacillin
what systemic antibiotics can be used for impetigo - MRSA
Doxycycline, clindamycin or sulfamethoxazole/trimethoprim
what are monitoring and follow up considerations for impetigo
Patients are no longer considered infectious approximately 48 hours after initiation of therapy
Monitor for development of systemic symptoms
Monitor for vesicle, crust and bullous resolution
Monitor for development of hypo or hyper pigmentation from infection
Resolution of symptoms should occur within a week, refer if persistent symptoms or recurrent
what is folliculitis
Small, raised, inflamed, pruritic pustules less than 5 mm in diameter
Noninfectious causes may be termed “pseudofolliculitis” and are induced by friction and/or occlusion (e.g., hair removal)
what is the most common cause of folliculitis
Staph aureus
other organisms may be causative such as Pseudomonas (exposure to hot tub/swimming pool)
what is a skin abscess
a collection of pus within the dermis and deeper skin tissues. Painful, tender, inflamed nodule
May have overlying pustule surrounded by a rim of inflammation and edema. Spontaneous drainage of pus may occur
what are Furuncles
a subtype of an abscess which occurs in skin containing hair follicles. Extension into dermis and subcutaneous tissue. Commonly: MSSA or MRSA.
what is a carbuncle
subtype of an abscess which occurs in skin containing hair follicles. Interconnecting multiple furuncles that coalesce into a single purulent mass are termed a carbuncle. Commonly: MSSA or MRSA.
what are non-pharm treatments for folloculitis/abscesses
Lesions will spontaneously rupture, however, carbuncles may needs to be incised
Warm water or saline compresses to promote drainage
Wash area with soap and water to decrease bacterial colony
Cover with sterile dressing
Drainage from lesions can spread infection to other parts of the body or to other people!
Wash items touching lesion daily
what are phamrmacological treatments for folliculitis and abscesses
Topical antibiotic regimens as seen in impetigo
Topical clindamycin/benzoyl peroxide formulations have also been prescribed for folliculitis
what are systemic antibiotics considered in folliculitis and abscesses
Inadequate clinical response to incision and drainage
Multiple lesions
Lesions in an area where drainage may be difficult
Associated comorbidities
Immunosuppression
Systemic signs of infection (fever, tachypnea, tachycardia, leukocytosis)
what are oral antibiotic options for folliculitis and abscesses
Sulfamethoxazole/trimethoprim (SMX/TMP), doxycycline, minocycline and clindamycin
MSSA: Cephalexin or cloxacillin
when should IV antibiotics be considered for folliculitis and abscesses
Immunocompromised patients
Patients who fail oral antibiotic therapy combined with incision and drainage and who exhibit signs of severe systemic infection
what are monitoring and follow up parameters for folliculitis and abscesses
Monitor for development of boils and lesions with pus
Systemic symptoms (e.g. fever resolution)
Pain resolution
Recurrent infection development
Allergy to medications (drug eruptions)
what is cellulitis
Infection from an entry point such as a wound, maceration between toes, fingers
Unilateral often and most commonly found in limbs
First sign of infection, feeling unwell with fever, chills and shakes.
Systemic symptoms are soon followed by the development of a localised area of painful, inflamed, swollen skin.
Skin may also be dimpled, warm to touch, blistering, and abscess, ulceration or purpura (red, purple or brown, non-blanchable spots caused by bleeding into the skin) may be present.
what are non-pharm treatments for cellulitis
Elevation of affected area helps to reduce edema
Cool, wet compresses can be used to relieve local discomfort.
Given the higher recurrence rates for lower-extremity cellulitis, contributing factors (e.g., edema, stasis dermatitis, interdigital tinea pedis) should be identified and treated in all patients
Daily compression stocking use in patients with chronic lower extremity edema have been shown to reduce recurrent cellulitis (15% vs. 40%)
what oral antibiotics can be used for cellulitis (mild-moderate disease)
Cephalexin PO x 5 days OR Cefuroxime PO x 5 days
Allergy to above: Clindamycin, cloxacillin
what are monitoring and follow up considerations for cellulitis
After initiation of cellulitis treatment, the affected area can appear to worsen (i.e., deepening of erythema and extension beyond demarcated area) within the next 24–48 hours before clinically improving.
No improvement within 48-72 hours, refer immediately (redo culture and sensitivity and adjust therapy)
what viruses cause palmar/plantar warts
HPV Types 1, 2, 27, 57
Thick, endophytic, sloping sides, central depression
Can be painful
what viruses cause common warts
HPV Types 1, 2, 4, 27, 57
Fingers, knees, elbows, nailfold
Hyperkeratotic, exophytic, dome shaped, punctate black dots
what viruses cause flat warts
HPV Types 3, 10, 28 and 29
Skin colored or pink on white skin, smooth surface, flat topped
Mainly dorsal hands, arms and face
what is the treatment paradigm for warts
Confirm it is a wart (do not forget about the mimics) - refer for a biopsy
Start with topical therapy (i.e salicylic agents and/or physical modalities)
Progress to alternative topical/physical therapies for refractory disease
what are non-pharm treatments for warts
Discussed in PMCO 1
salicylic aicd, OTC products
what are Rx treatments for warts
Cantharidin (0.7%) (in office)
Bleomycin sulphate (0.1–1 units/mL) intralesional injection (in office)
Imiquimod 5% cream
5-Fluorouracil 5% cream
DPCP (in office)
Topical Retinoid
Cimetidine
what are monitoring and follow up parameters for warts
Warts may take 3-4 months to resolve
Monitor for resolution of size of warts
Monitor for change in shape or color of wart - could suggest that this is not a wart!
Signs of infection (redness, pus, pain)
Warts that continue to grow quickly require further assessment
rIritation to topical agent
Address any pigmentary changes (hypo- or hyperpigmentation)
Failure in response - check for adherence and how the patient uses the medication
what is Onychomycosis
fungal infection of the nail
The distal end and sides of the nail lift or become discoloured and crumble.
Flaky, white patches and pits appear on the top of the nail plate.
Discolouration of the nail, eg, yellow, white, grey, or green discolouration
Ridging, crumbling, and sometimes eventual complete nail plate destruction.
Scaling occurs under the nail.
what are pathogens that commonly cause Onychomycosis
Dermatophytes (Epidermophyton, Microsporum and Trichophyton genera) Yeasts (mainly Candida)
how is Onychomycosis diagnosed
Direct microscopy (potassium hydroxide [KOH] examination of scrapings from the nail bed)
Biopsy (nail tissue/clippings with periodic acid–Schiff stain)
Culture
what are non-pharm treatments for Onychomycosis
Wearing footwear and socks that minimize humidity
Don’t share nail clippers or foot wear
Keeping nails clean and cut short
Prevent further physical trauma to nails
what is the typical duration of treatment for Onychomycosis
3-6 months
what are monitoring parameters for Onychomycosis
Complete clinical cure = 0% nail plate involvement ■
Clinical improvement = <5–10% nail plate involvement
Incomplete clinical response = >10% nail plate involvement (reassessment is required)
Monitor for irritation from topical agents or adverse effects from systemic agents
Monitor for recurrence of a nail infection or a concurrent skin infection
what agents are used for Onychomycosis
Efinaconazole 10% solution
Ciclopirox olamine 8% lacquer
Propylene glycol 66.4%/urea 20%/lactic acid 10% solution
Itraconazole
Terbinafine
how long does resolution of Onychomycosis take
approx 12 months
solution of the fungal infection takes months (~12 months) ○ Pharmacist can check in monthly or at refills
Measure distance of outgrowth of disease-free nail (normal growth rate is 1.5–2 mm/month)