Female Reproductive System
1/16
Earn XP
Description and Tags
Produces + maintains sex cells, transport for fertilization, produce + secrete hormones, nurture + protect fetus
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
17 Terms
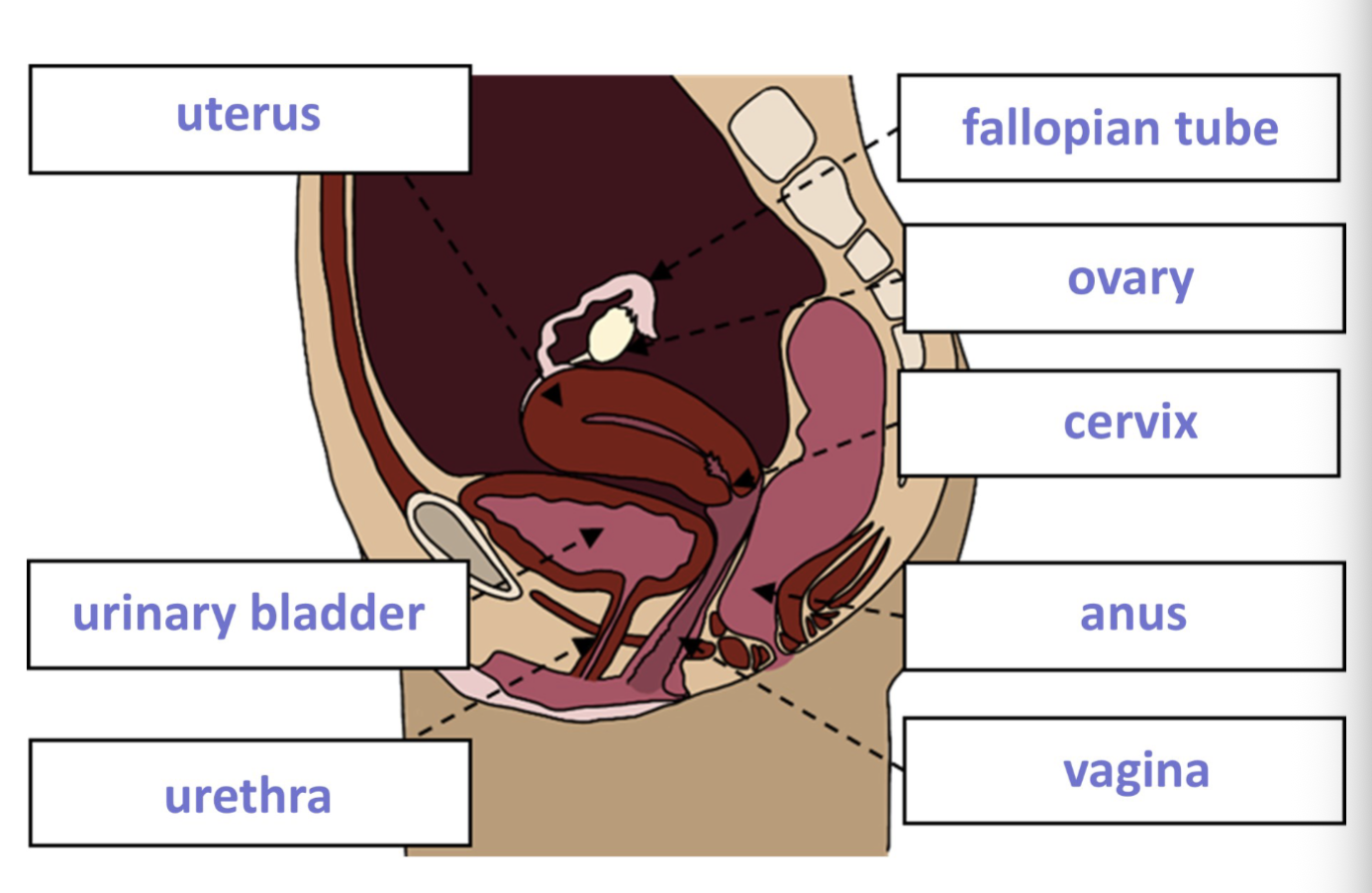
Ovaries
2, almond shape, egg production/storage, filled with ovarian follicles each holding an immature egg (oocyte), each month a follicle ripens + releases egg (ovulation), secrete hormones (gonads, estrogen, progesterone, small amount testosterone), meiosis (oogenesis, create 1 oocyte + 3 polar bodies, millions at birth, 300-400 released during lifetime)
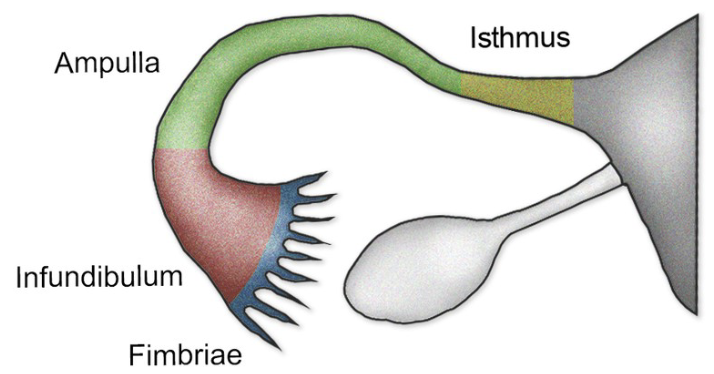
Fallopian Tubes
10 cm long, receive ovulated egg from ovaries, fertilization space, filled with cilia to move egg, lined with smooth muscle to push egg toward uterus (1 week), infundibulum (end of tube not connected to ovary), fimbriae (fingerlike projections on infundibulum, propel egg into tube), ectopic pregnancy (implantation in tube)
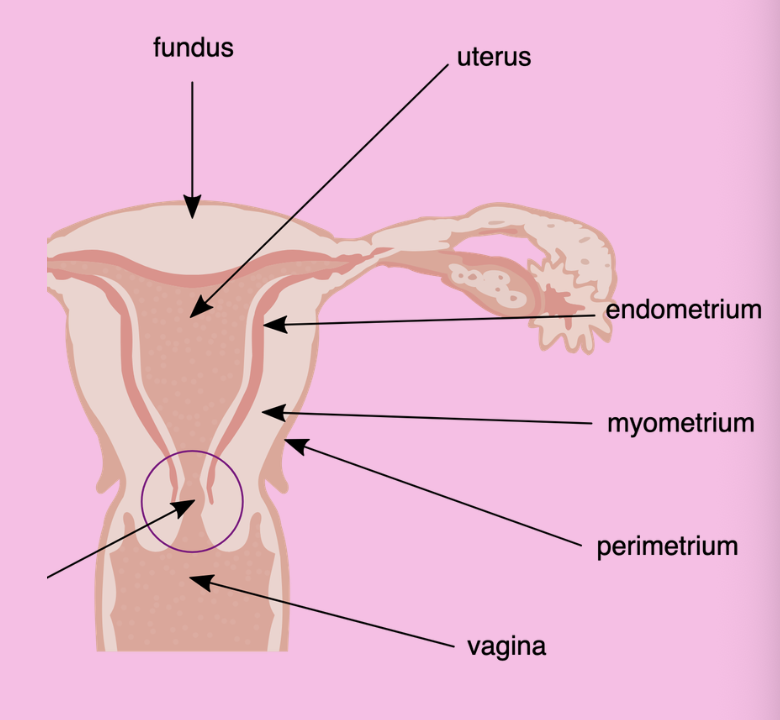
Uterus
Womb, inverted pear, receives egg so fetus develops, hollow with thick muscle walls, 3 layers: endometrium (receives/captures/nourishes fertilized egg, inner mucus layer where implantation occurs, eggs burrow into lining), myometrium (smooth muscle), perimetrium (outer, covers uterus to protect against friction)
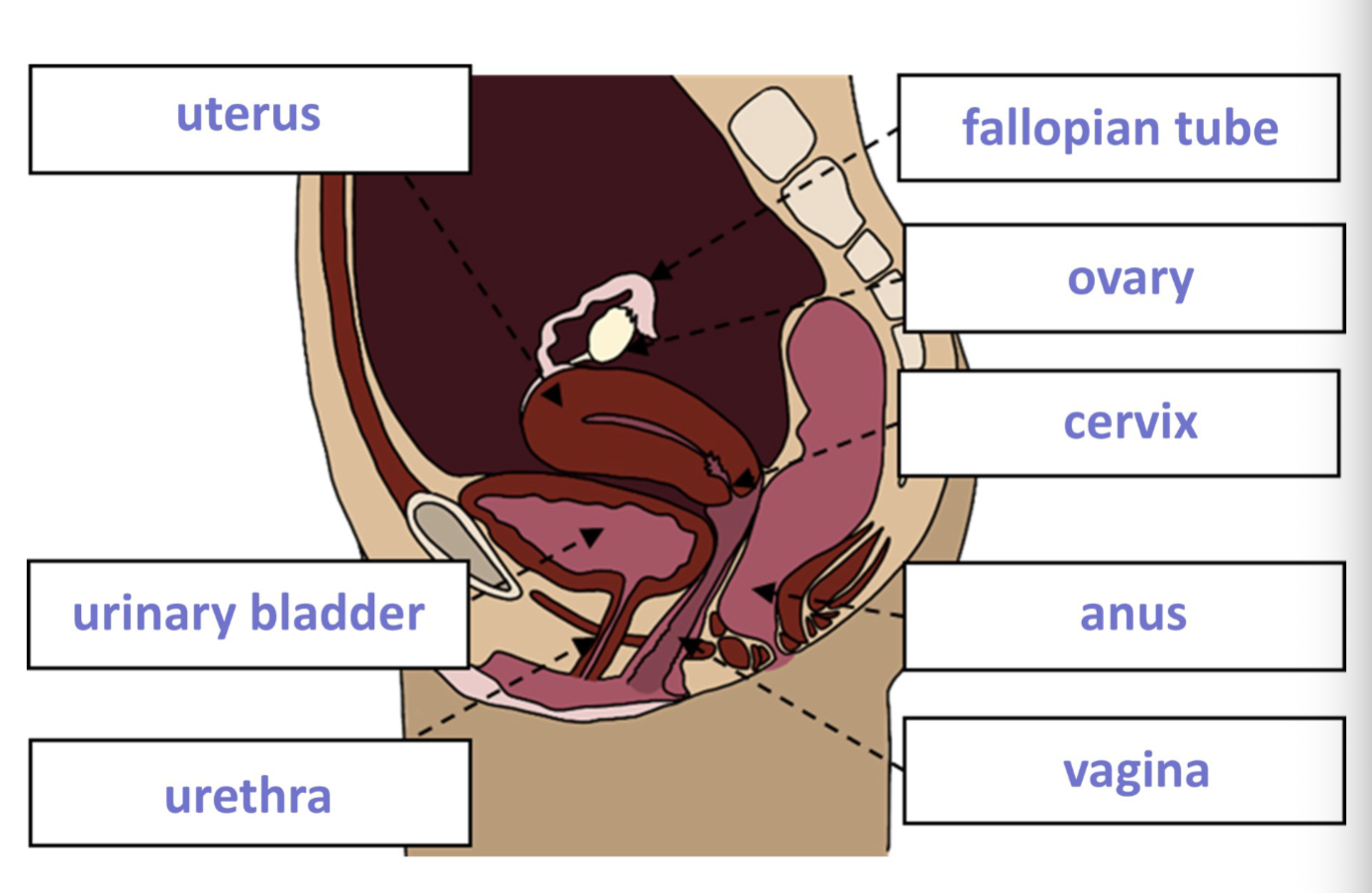
Cervix
Neck of uterus, leads to vagina, filled with mucus to prevent bacteria from vagina entering uterus, opens during menstruation + birth
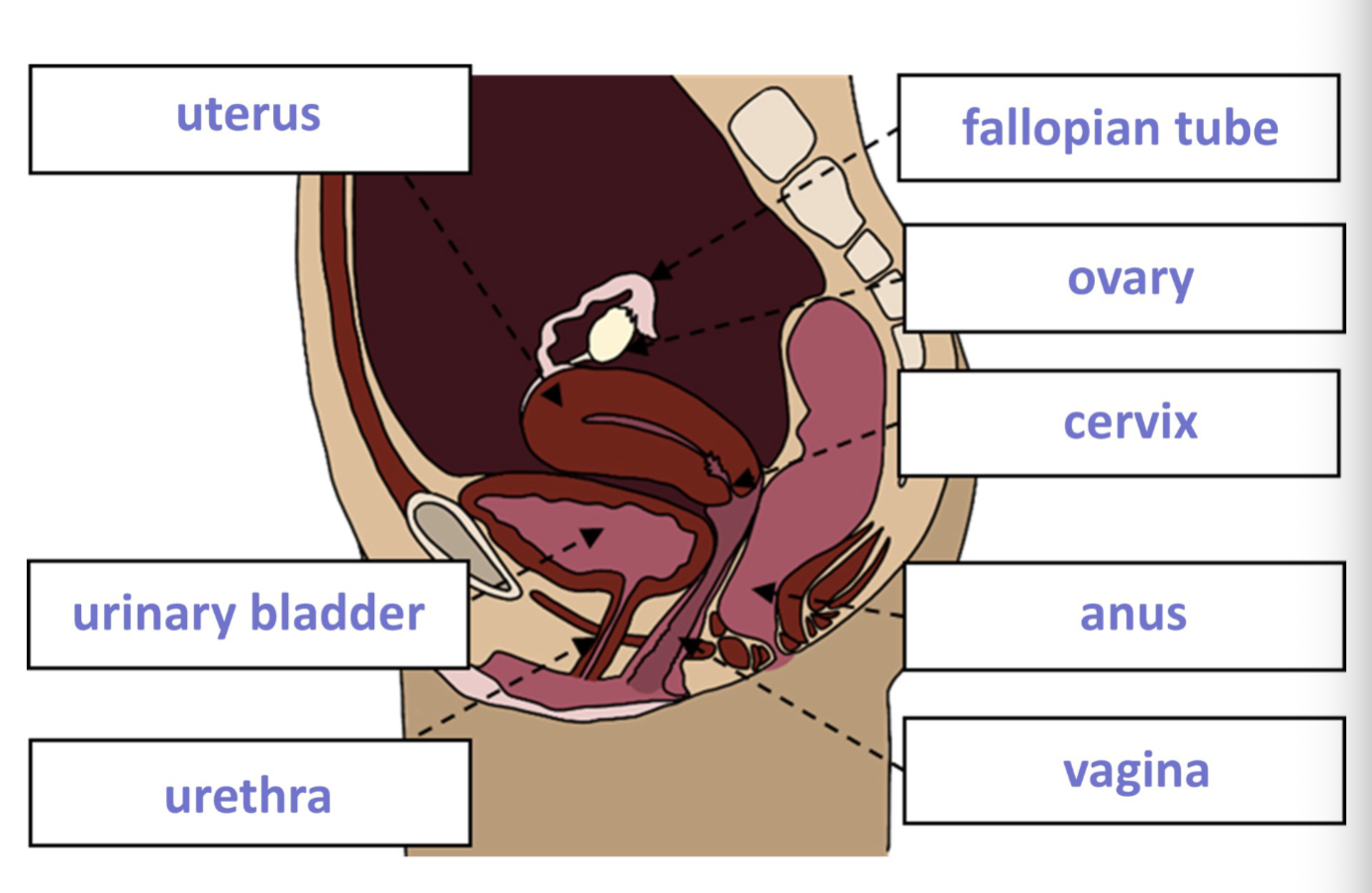
Vagina
Fibromuscular tube extending outside, receives semen/transports offspring/menstruation, hymen (thin membrane, outer cover, protective barrier against bacteria for infants), 3 layers: mucus (protects, lubricates), muscular (controls contraction), fibrous (elastic tissue binds vagina to surrounding pelvic structures like bladder/rectum)
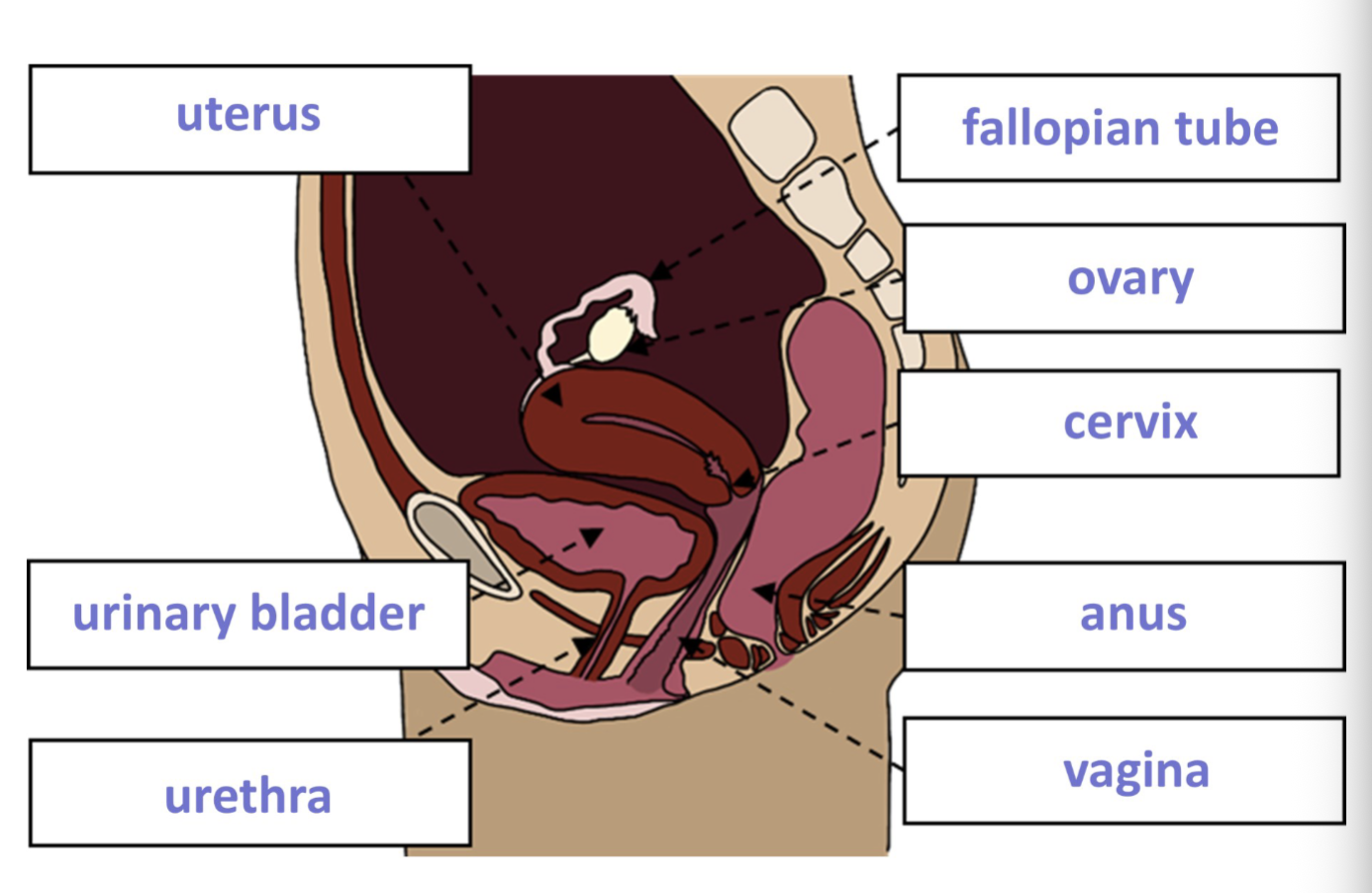
Ovarian Ligament
Attaches ovaries to uterus to hold them in place
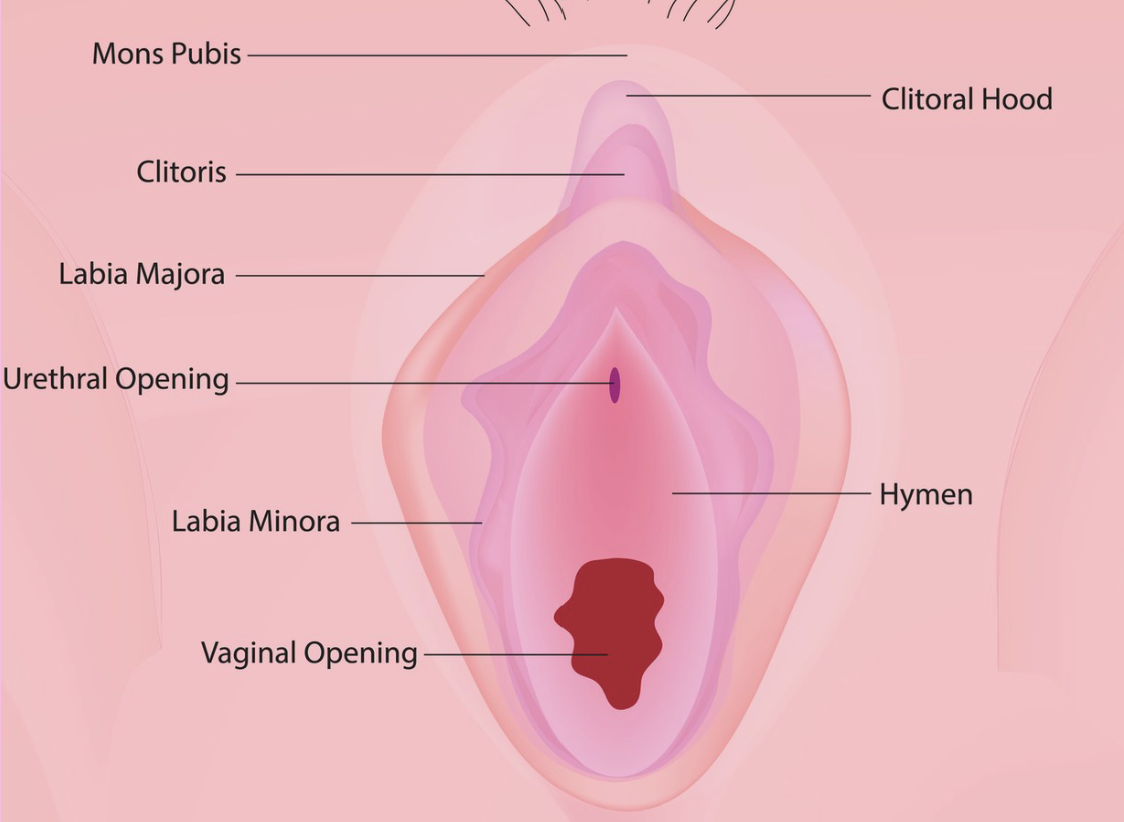
External Accessory Organs - Vulva
Labia majora (protects exterior reproductive organs made of adipose tissue like male scrotum), labia minora (flat inner folds made of connective tissue with blood vessels), clitoris (erectile tissue + nerve fibers like corpus cavernosa + glands covering in male penis), vestibule (space enclosed by labia minora including vaginal + urethral openings), vestibular gland (secretes mucus like male’s bulbourethral gland)
Ovarian Cycle
Maturation + ovulation of egg, every 28 days, same time as uterine cycles
Follicular Phase
1-14 days, follicles grow due to hypothalamus release of GnRH to trigger release of FSH + LH (gonadtropins) from pituitary which impact ovaries, FSH triggers follicle growth/mature/release of estrogen (secondary sex characteristics, rebuild of uterine lining rebuilds) in ovaries, ovary enlarges to become primary follicle, follicle grows + fills with fluid from oocyte bulging outward, spike in LH at end (stimulates ovulation + testosterone)
Ovulation
Day 14 of follicular phase, oocyte ruptures from follicle, spike in LH triggers oocyte’s rupture from mature follicle into fallopian tube, oocyte lasts 24 hours, sperm may fertilize egg in time period, one egg per month, hyperovulation (LH surge causes multiple eggs to ovulate)
Luteal Phase
14-28 days, follicle turns into corpus luteum (tiny endocrine gland) that produces high levels of estrogen + progesterone (triggers drop in FSH + LH to prevent 2nd ovulation) for 2 weeks, uterine lining thickens in preparation for embryo, corpus luteum continues producing hormones for months if egg was fertilized, if not it disintegrates to stop producing estrogen + progesterone (made by corpus luteum, change in reproductive cycle, regulates gonadotropins, increase uterus lining, keeps myometrium lining inactive if implantation occurs, prepares break to produce milk)
Uterine Cycle
Menstrual, so uterus is ready for fertilized egg, repeats every 28 days + lines up with ovarian cycle
Menstrual Phase
1-4/5 days, menstruation/menses, bleeding, estrogen + progesterone low to cause uterus to shed all but deep parts of endometrium from uterine wall, 3-5 days bleeding, 1/4-1/2 cup blood lost, oduring follicular phase of ovarian cycle as follicles grow, ends due to growing follicles releasing estrogen that builds endometrium
Proliferative Phase
4/5-14 days, growth, endometrium rebuilds due to rising estrogen + progesterone, nice/thick bed for fertilized egg to implant in uterus, ends as ovulation occurs
Secretory Phase
15-28 days, continues growth + vascularization to prepare for fertilized egg, endometrium grows thick from estrogen + progesterone from corpus luteum, fertilized egg reach uterus day 21 when endometrium is thickest, implant of fertilized egg keeps high estrogen + progesterone through pregnancy with thick endometrium to support embryo, no fertilized eggs means corpus luteum degenerates with drop in progesterone + estrogen + beginning of menstruation again
Secondary Sex Characteristics
Enlargement of accessory reproductive system, develop breasts, hair growth, fat to thigh/buttocks, change in vascularization to pelvis, widens pelvis
Birth Control Effectiveness
Implants, IUDs, sterilization, vasectomy → injectables → pills, patch, vaginal ring → LAM→ condoms → diaphragm → cervical cap, sponge, female condoms → withdrawal, fertility awareness → spermicides