Oral Medicine OSCE (extended version)
1/206
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
207 Terms
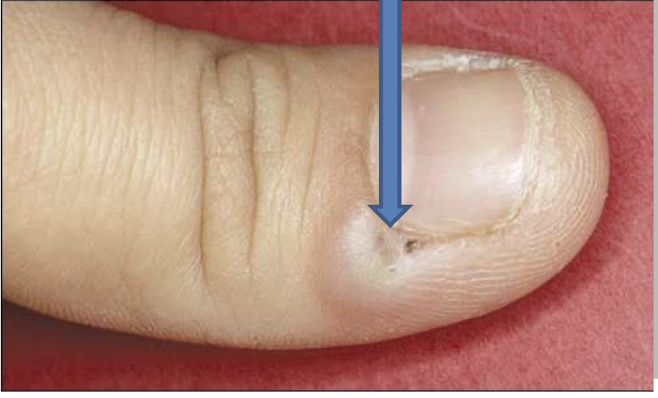
what is this lesion and how is it caused
herpetic whitlow
direct contact with an infected lesion without gloves
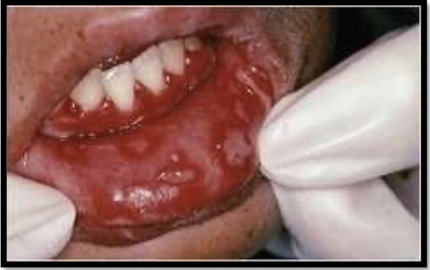
what is this lesion
acute herpetic gingivostomatitis
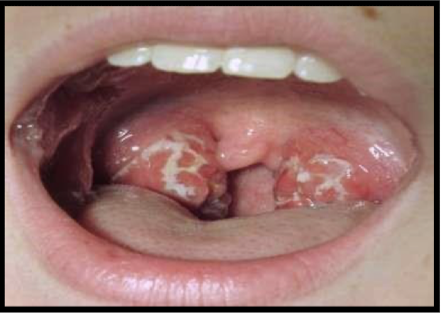
what is this lesion associated with and what are they called
acute herpetic gingivostomatitis
vesicles on the tonsilar pillars
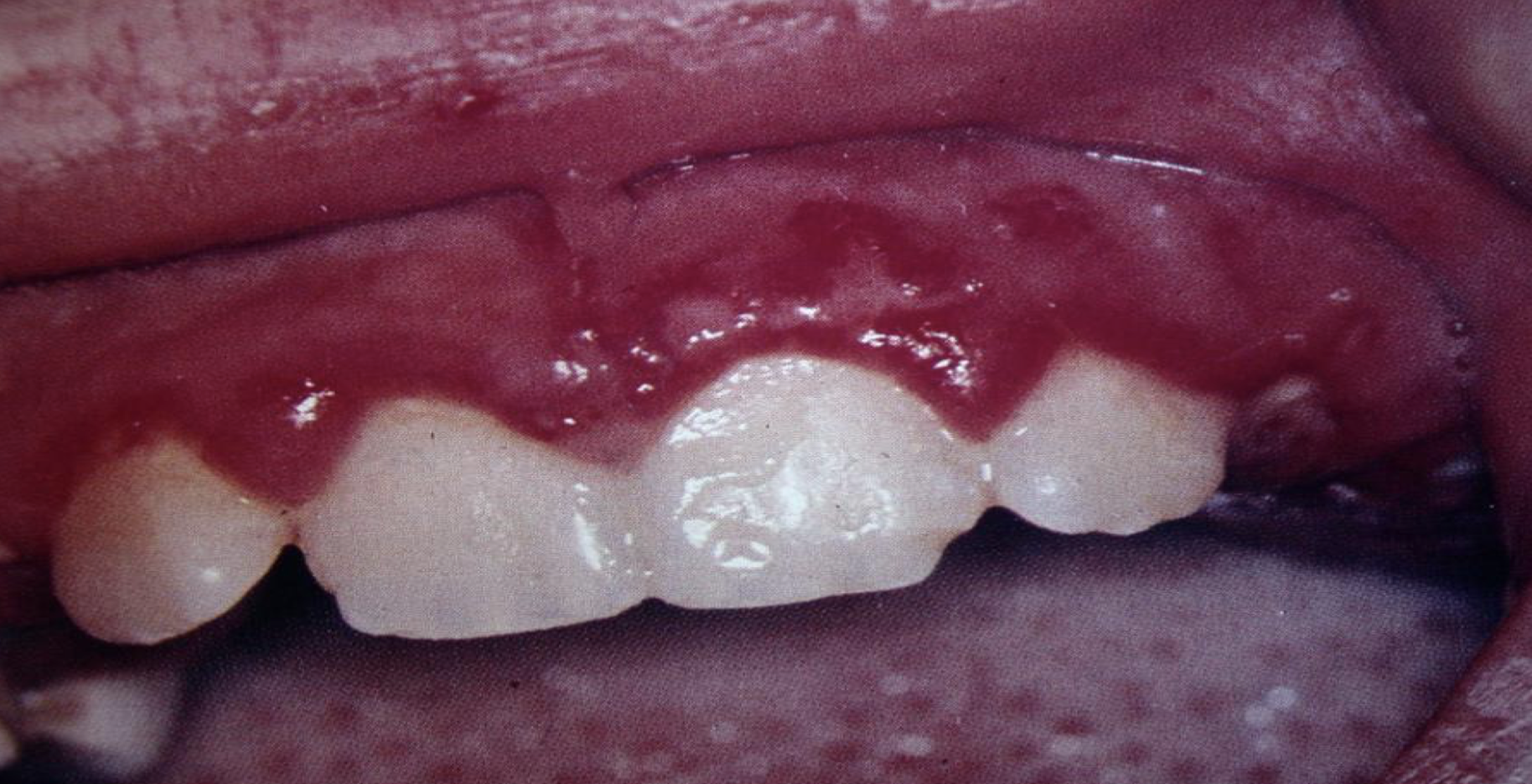
what is this lesion and what is it associated with
acute marginal gingivitis
HSV 1
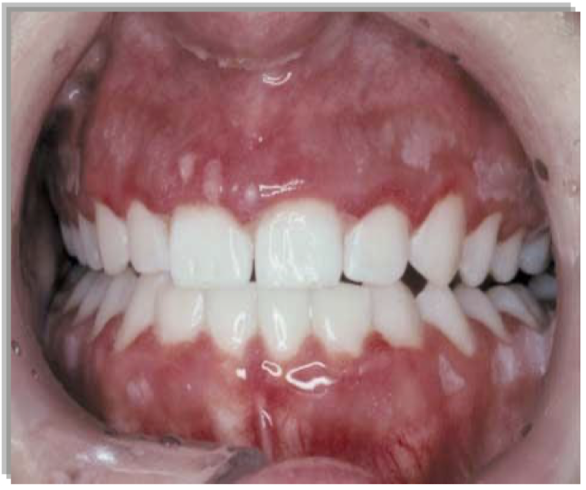
what is this lesion and what is it associated with
Acute marginal gingivitis
HSV-1
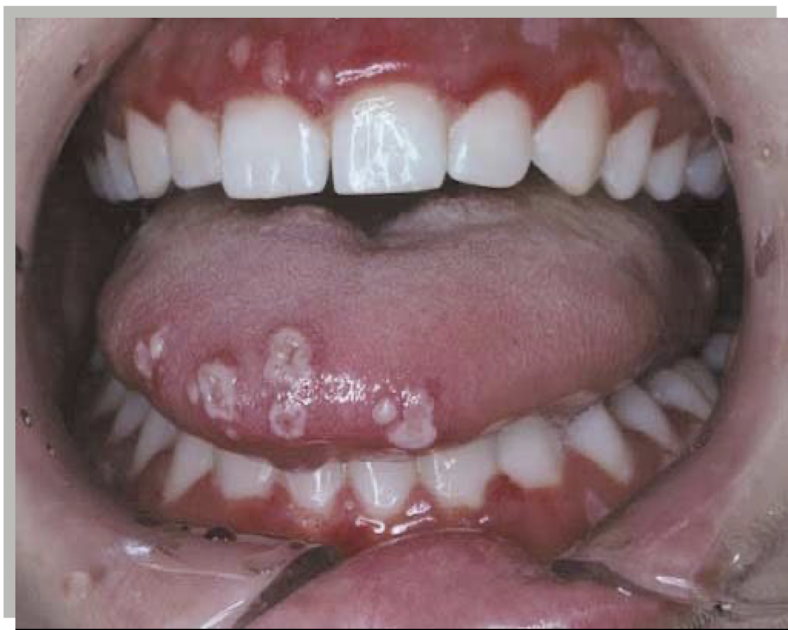
what is this lesion and what is it associated with
acute generalized gingivitis
HSV 1
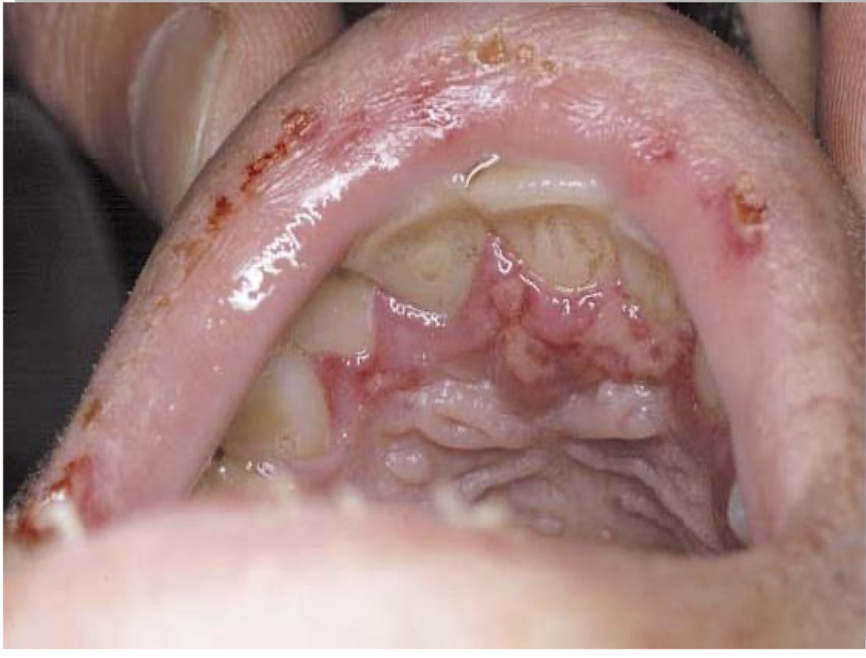
what is this lesion
recurrent intraoral herpes simplex
vesicles/ulcers
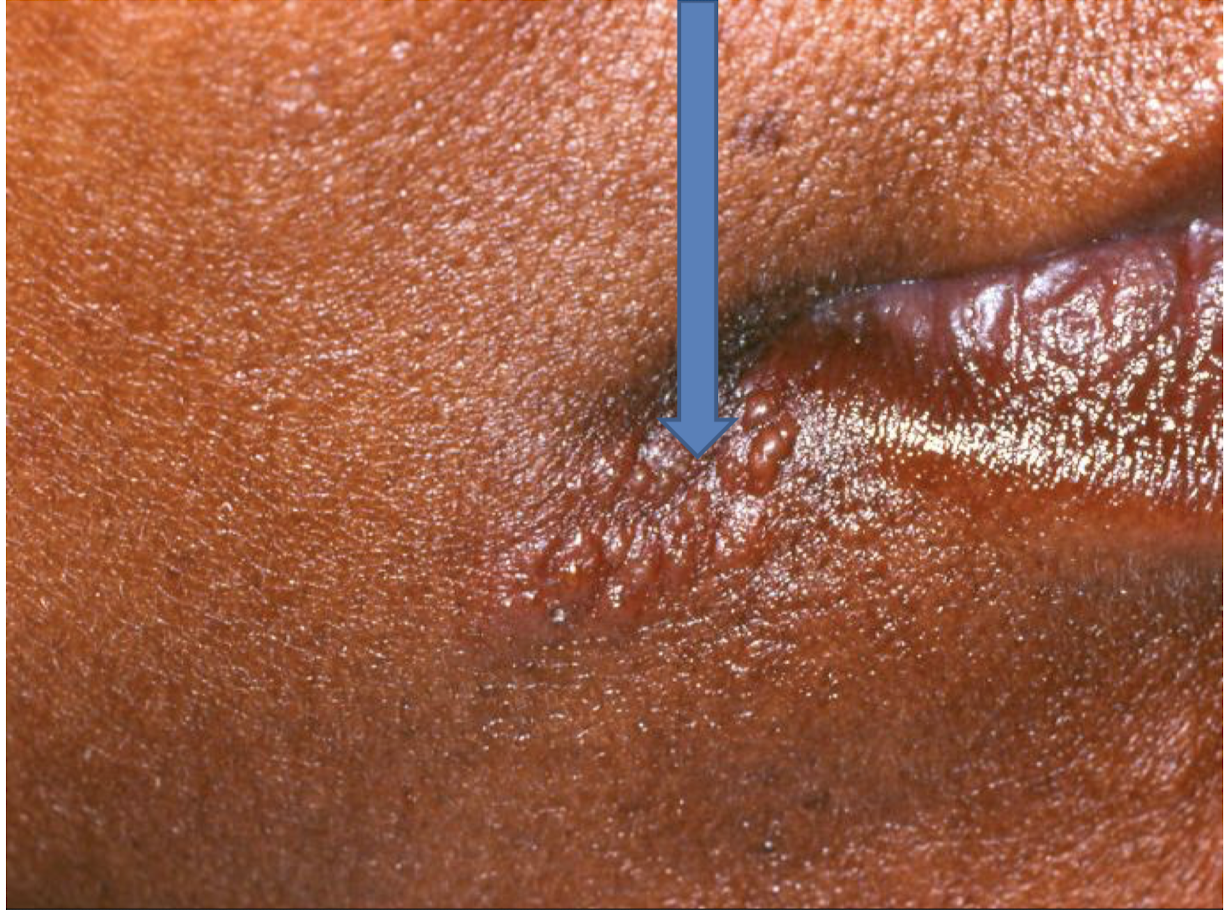
what is this lesion
herpes labialis
vesicles
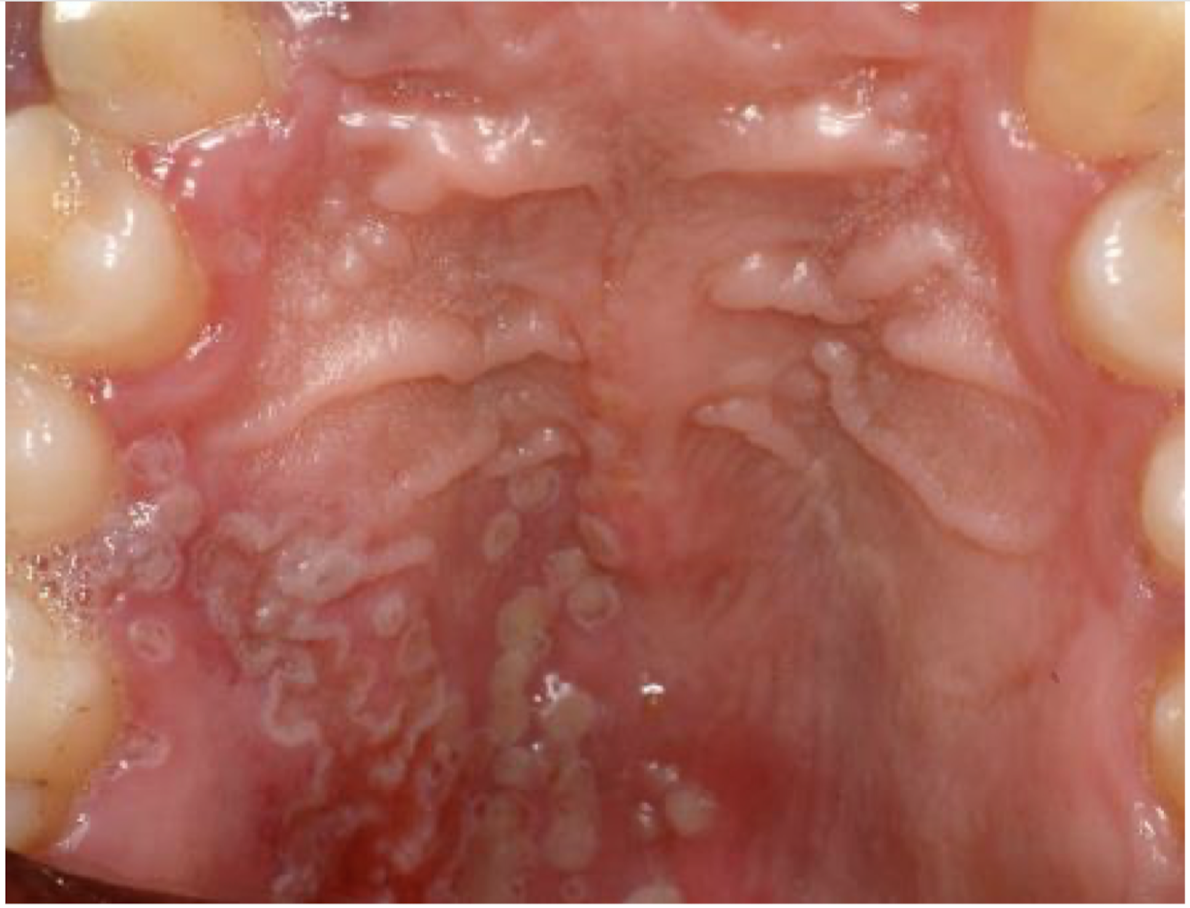
what is this lesion
recurrent intraoral herpes simplex
vesicles
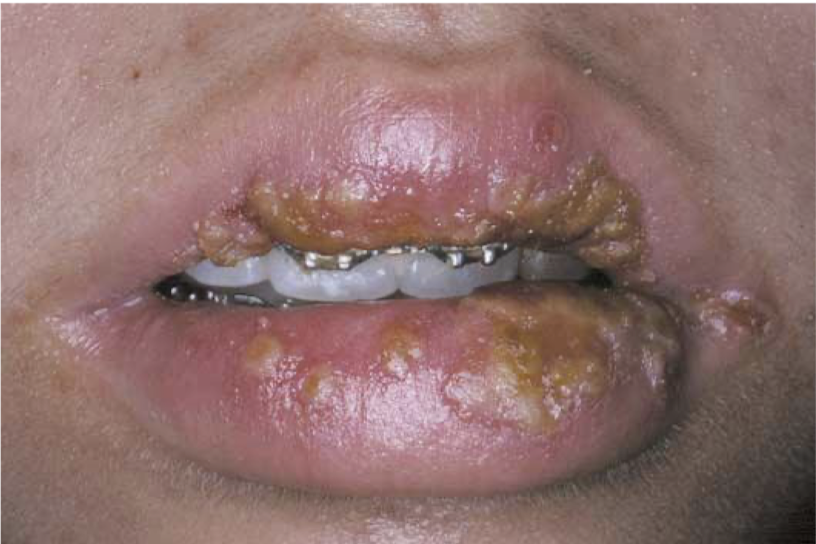
what is this lesion associated with and how did it form
recurrent intraoral herpes simplex
coaslesced vesicles
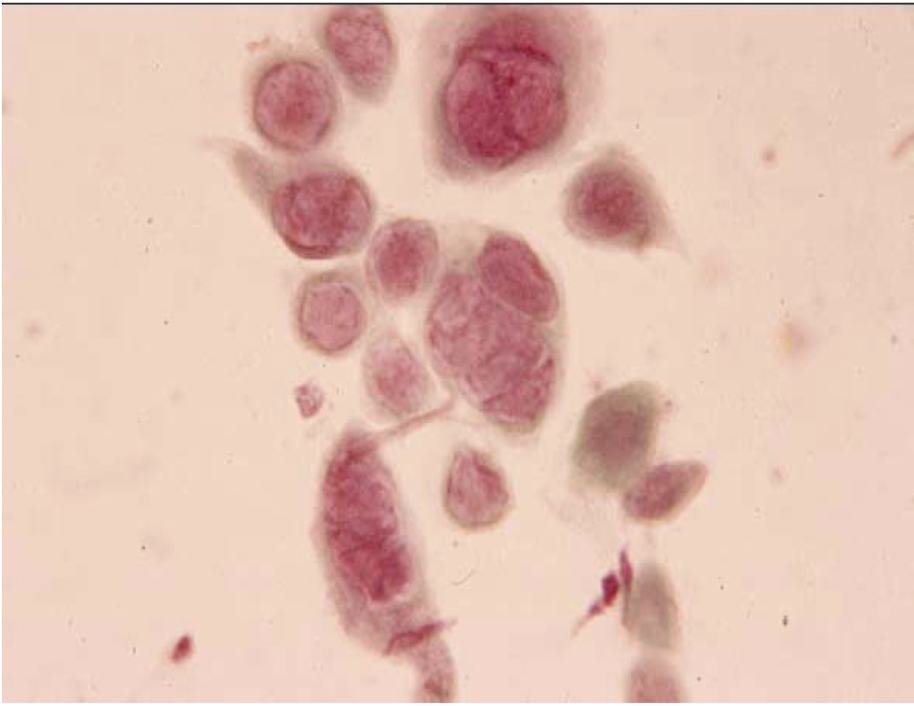
what are these cells called and which disease can you see these cells
multinucleated giant cells
herpes simplex virus

what is this medicine used for and what is the dose
herpes simplex virus
Acyclovir suspensions/ cream 5g 5 times a day

what is this medicine used for and what is the dose
Acyclovir (Zovirax) - Herpes simplex virus
400 mg TID (3x a day) × 7days

what is this medicine and what is the dose
penciclovir 1% - Herpes Simplex Virus
every 2 hours
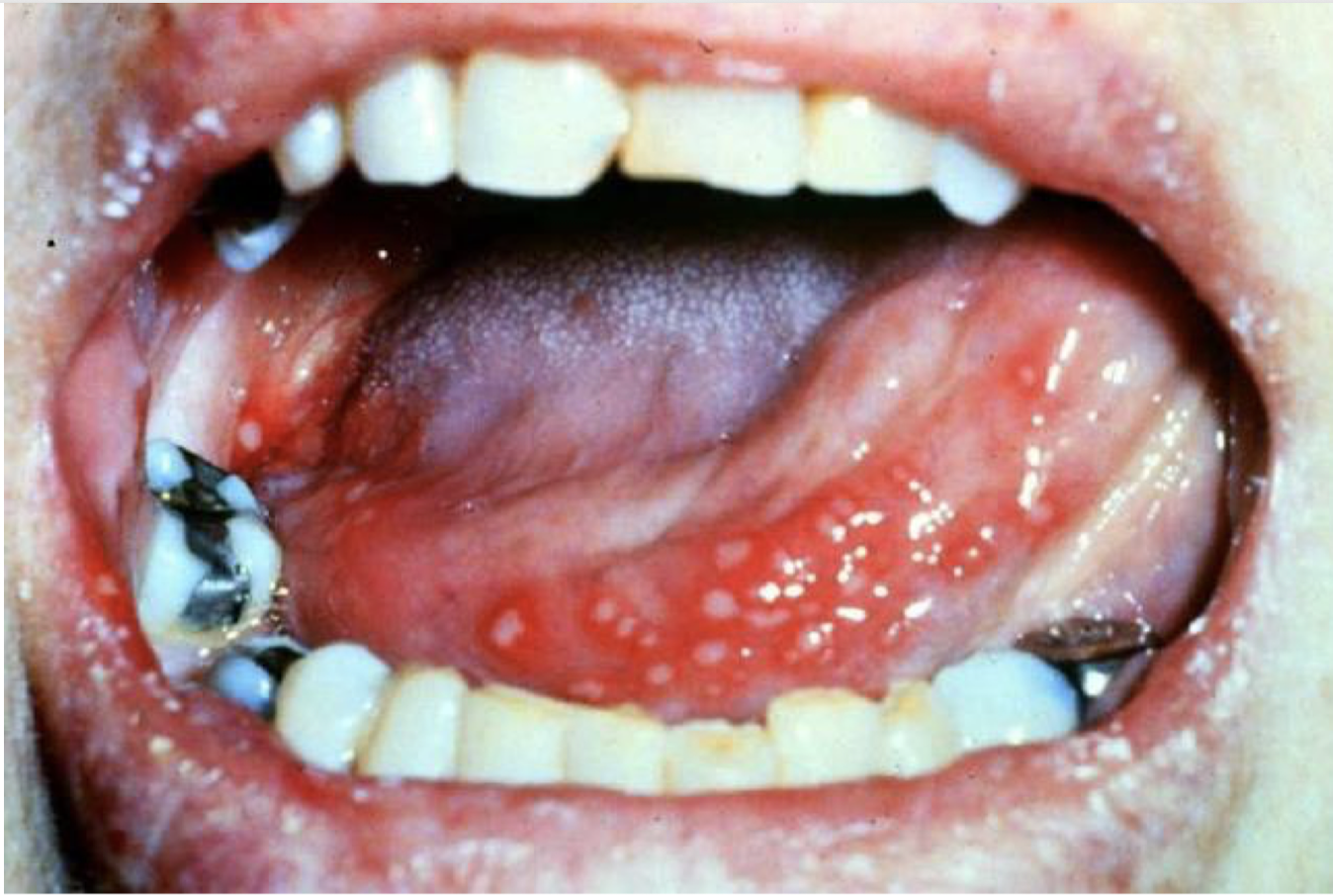
what are these lesions associated with
Herpangina - Coxsackie A4
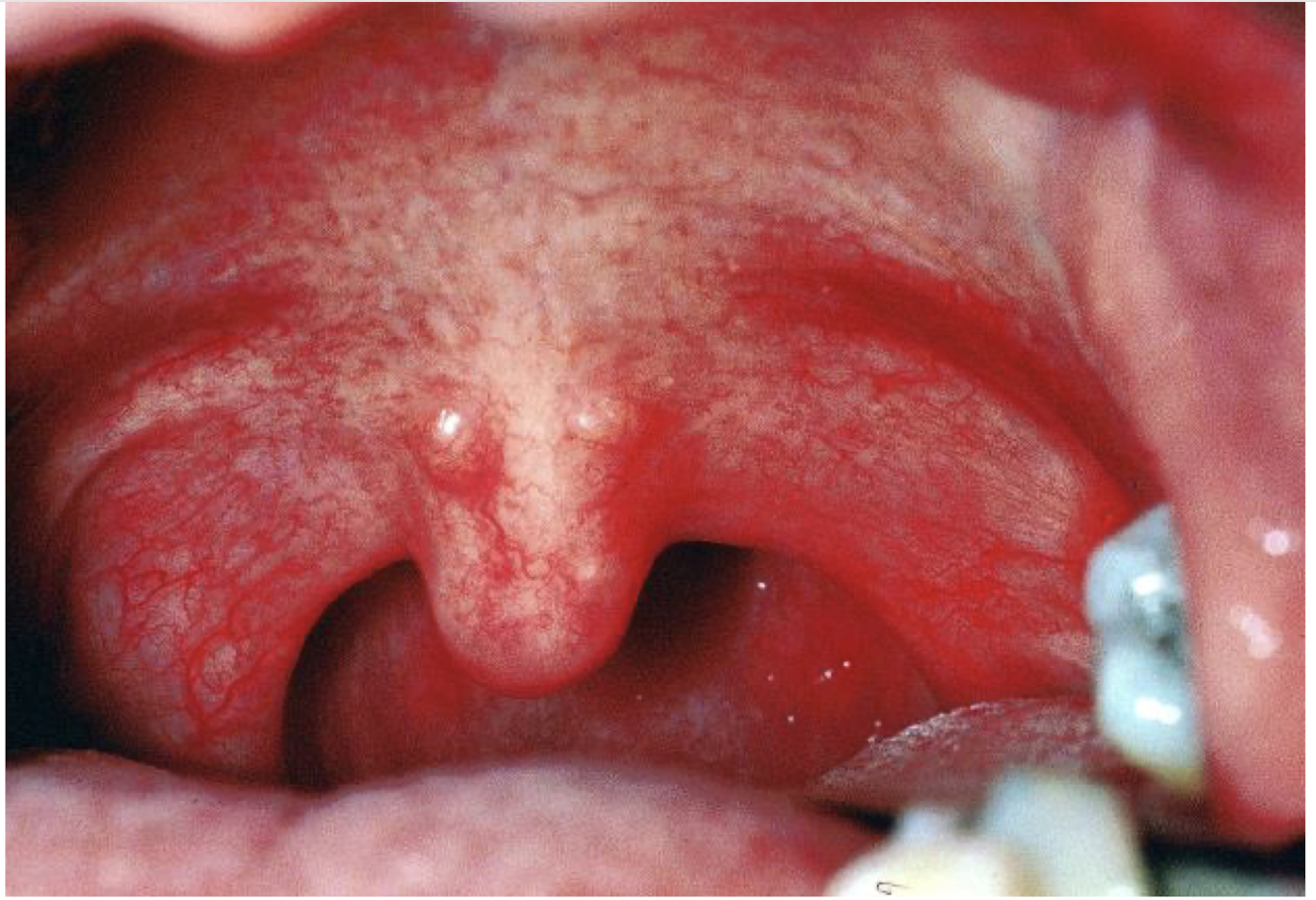
what are these lesions associated with
Acute lymphonodular pharyngitis - Coxsackie A10
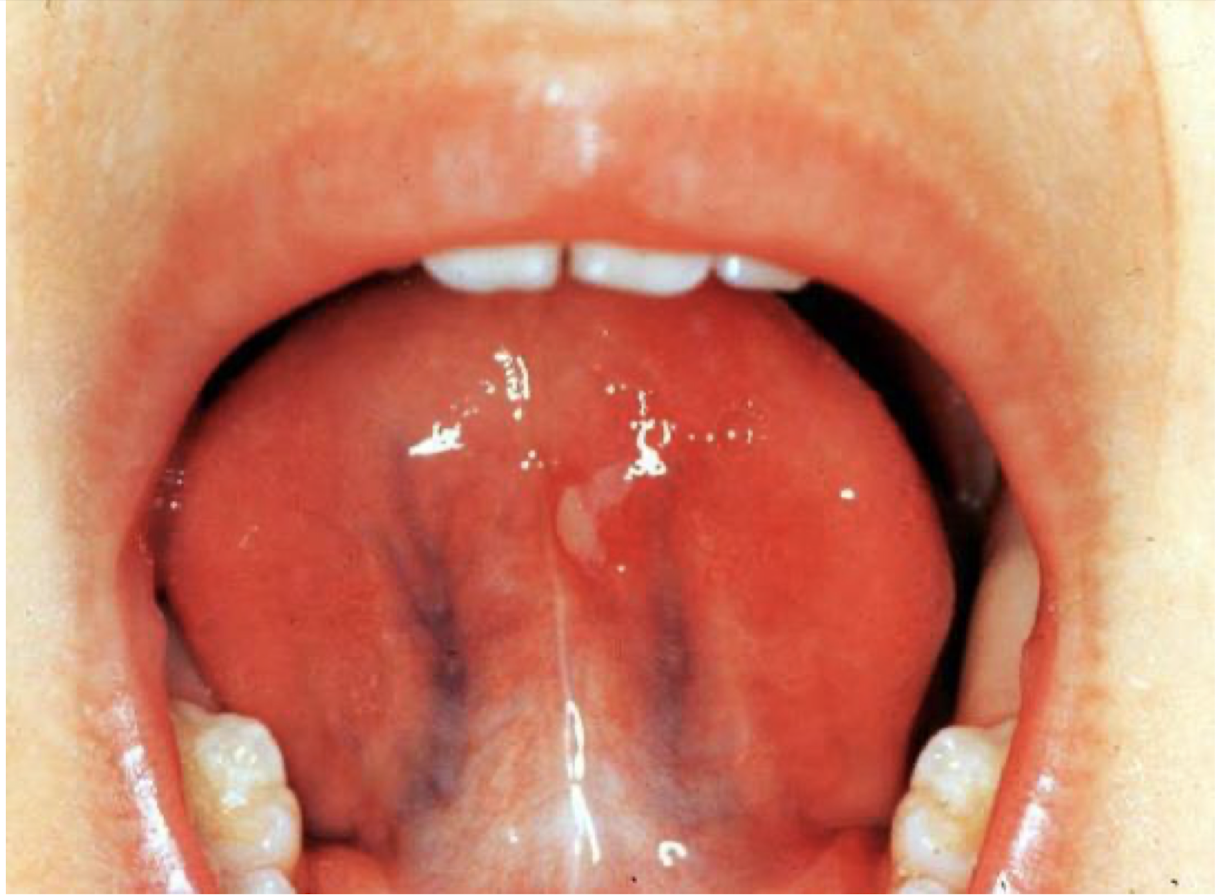
what is this lesion and what is it associated with
oral vesicle/ulcer
hand foot and mouth disease - A16
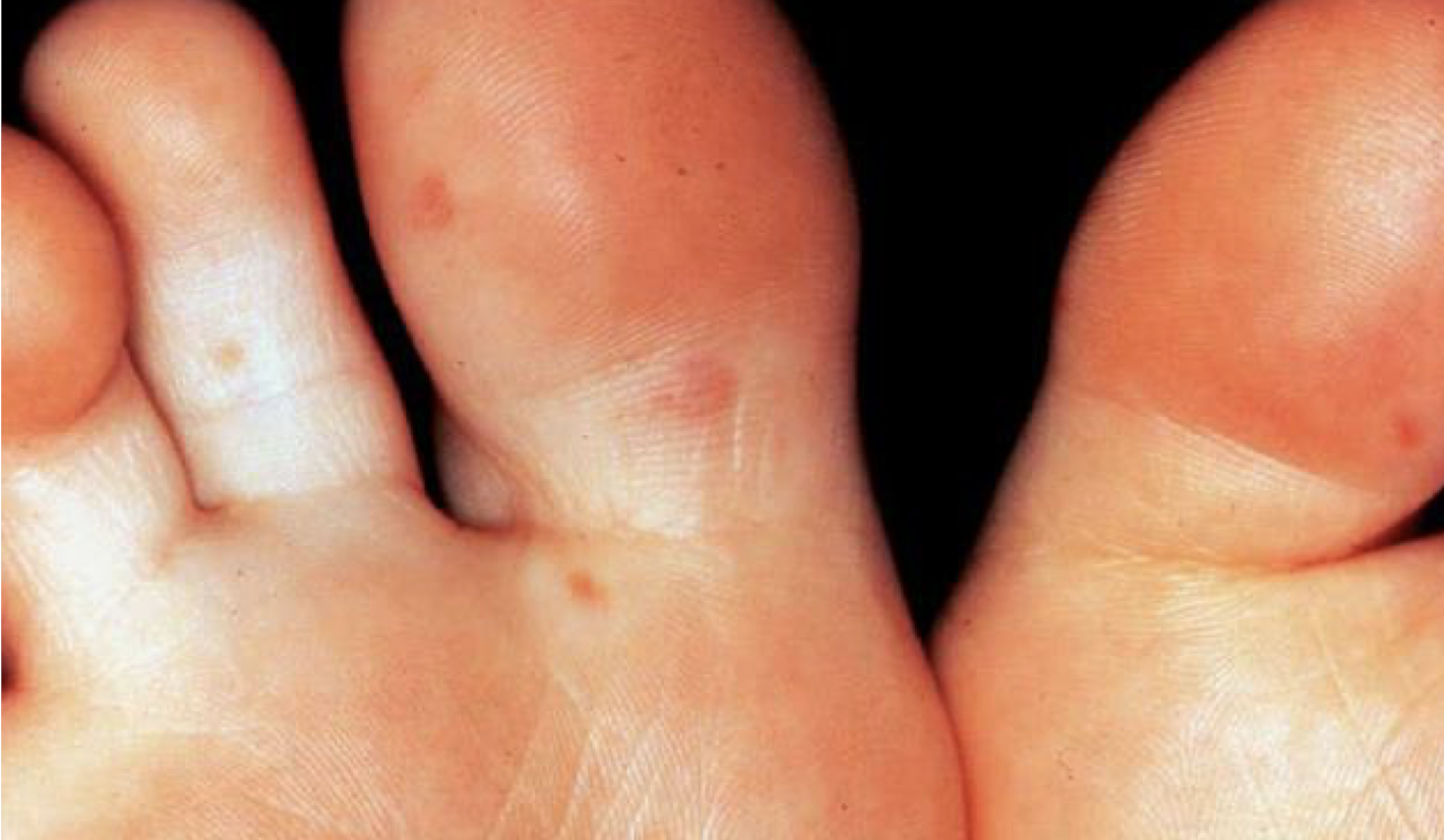
what are these lesions associated with
hand foot and mouth disease
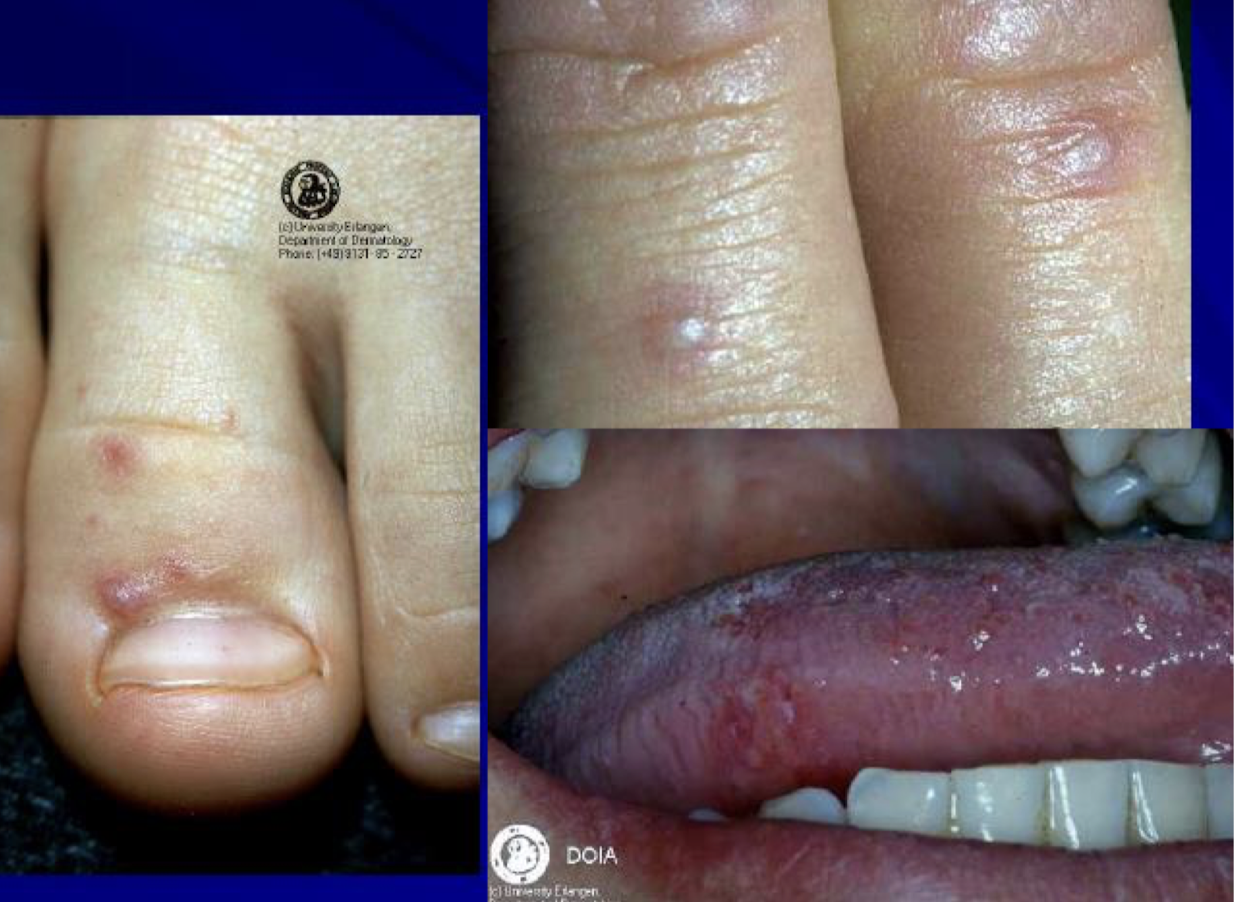
what are these lesions associated with
hand foot and mouth disease
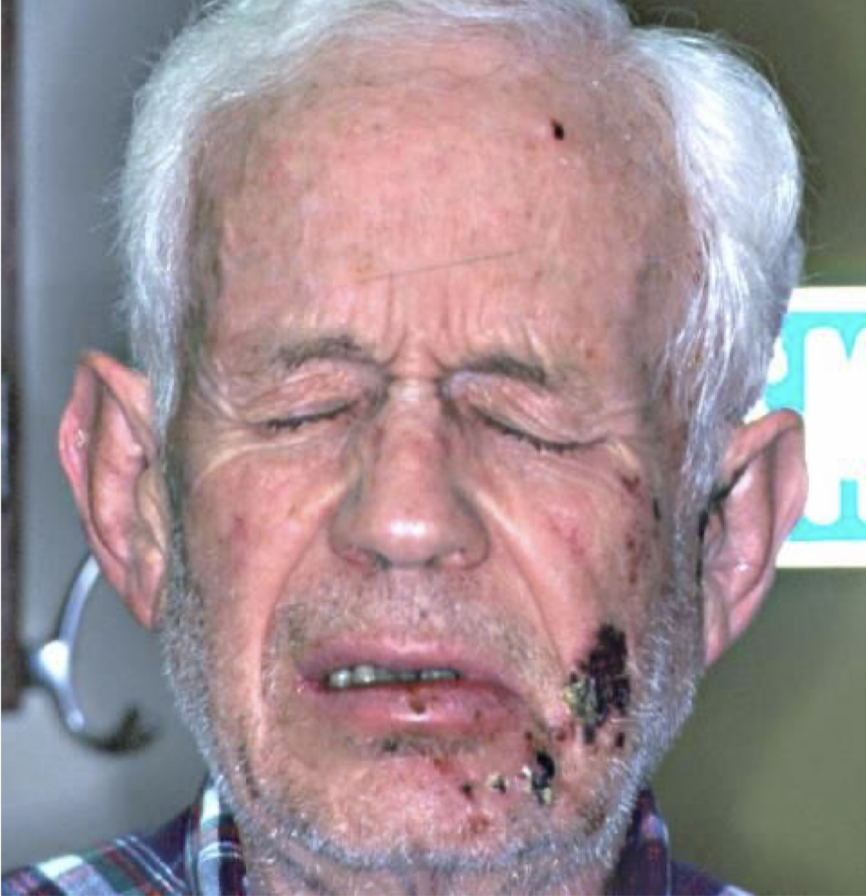
what is this lesion associated with and why is it black
shingles/herpes zoster
the vesicles turned into ulcers which turned into scabs
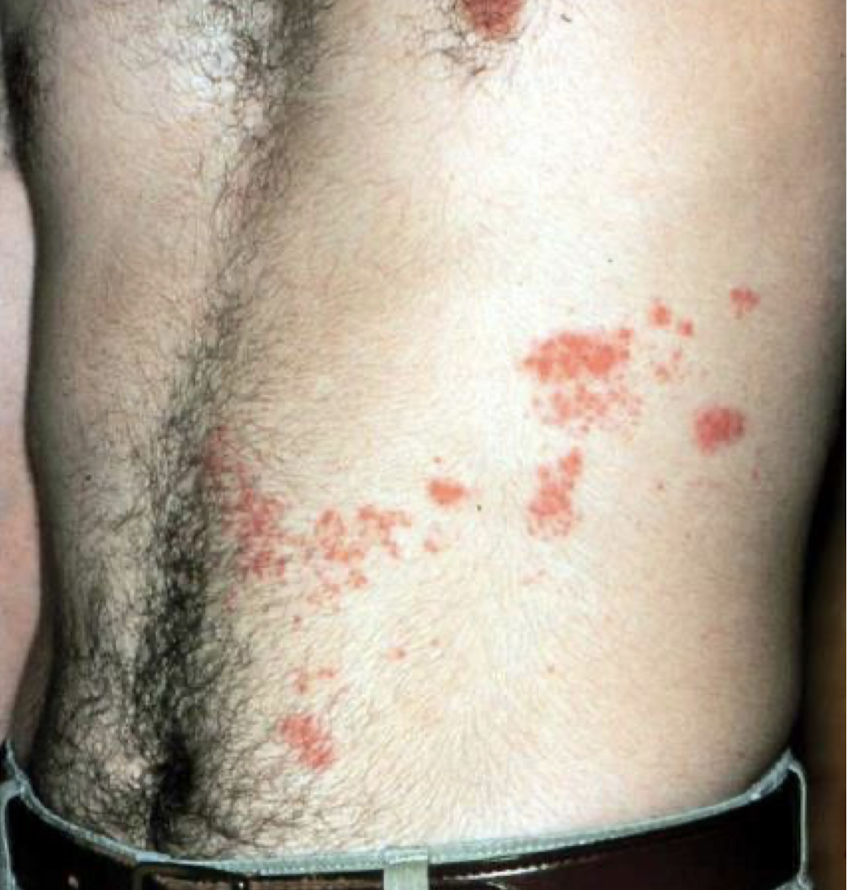
what are these lesions associated with and what is it called
shingles/herpes zoster
post-herpetic neuralgia
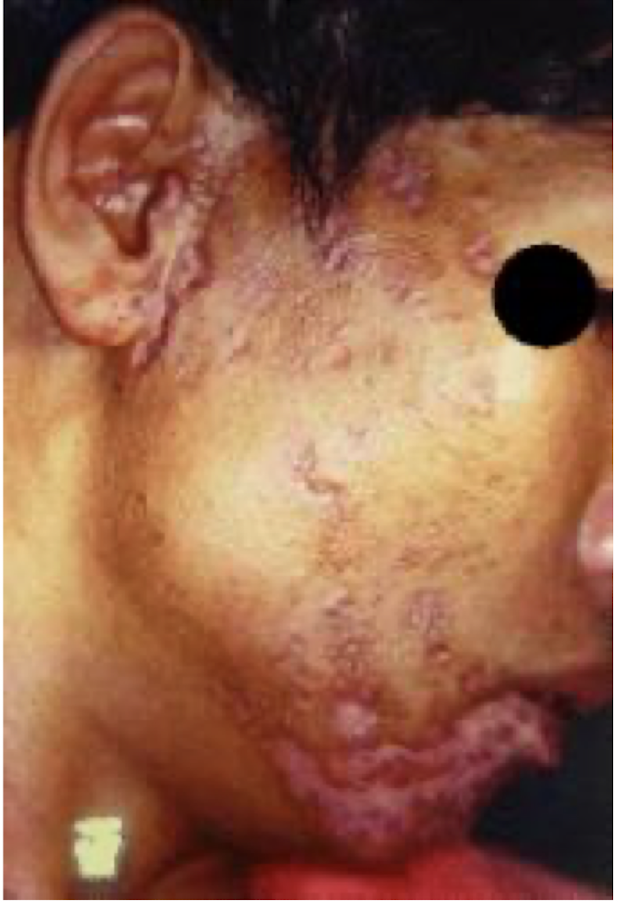
what are these lesions associated with
herpes zoster/shingles
post-herpetic neuralgia
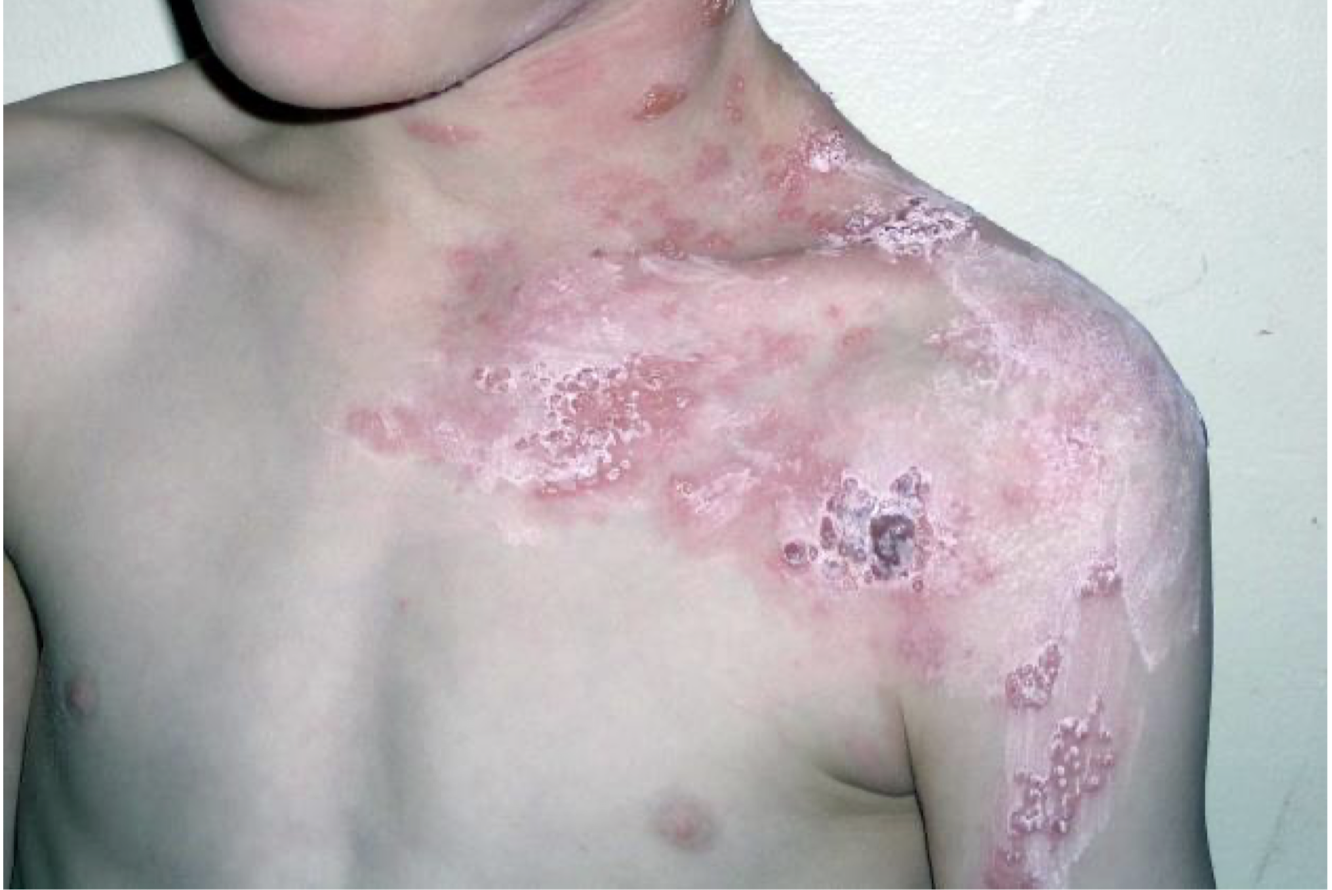
what is this lesion associated with
herpes zoster/shingles
post-herpetic neuralgia (spinal nerve)
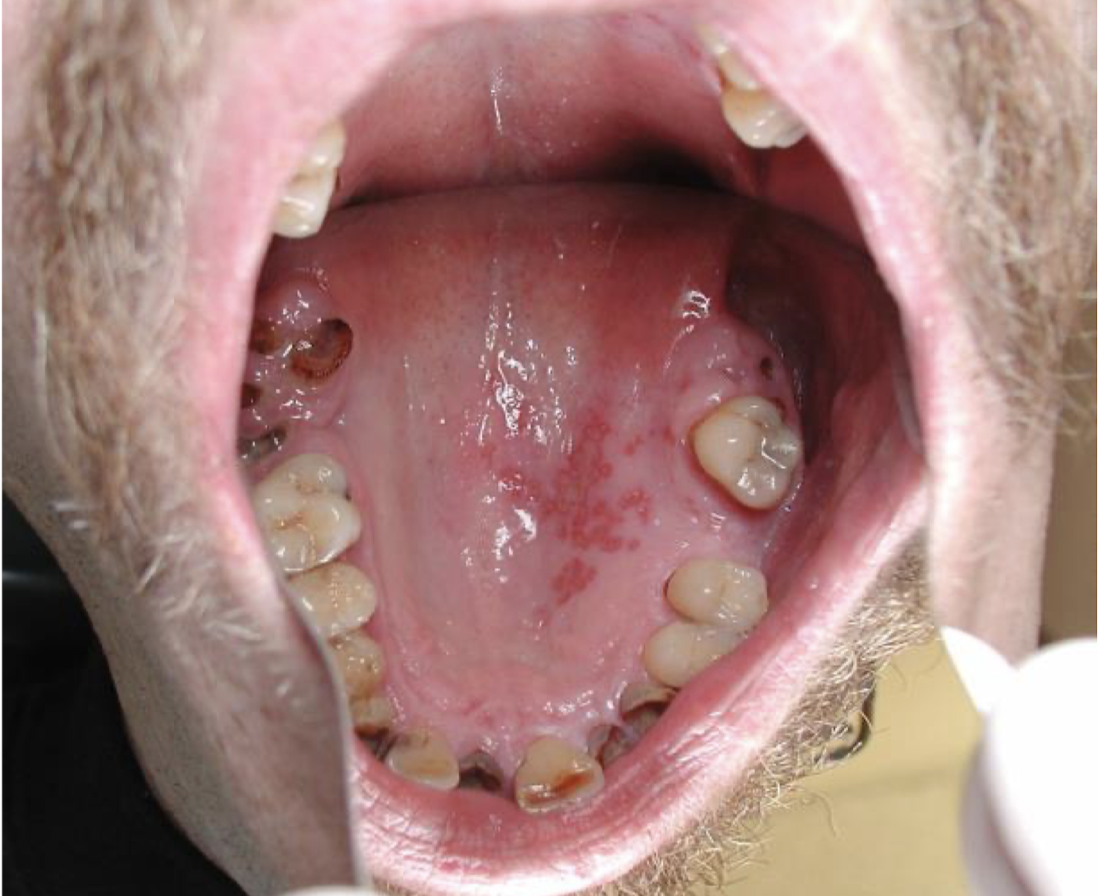
what virus is this lesion associated with and how do you determine?
Herpes Zoster (shingles)
the lesion doesnt cross the midline
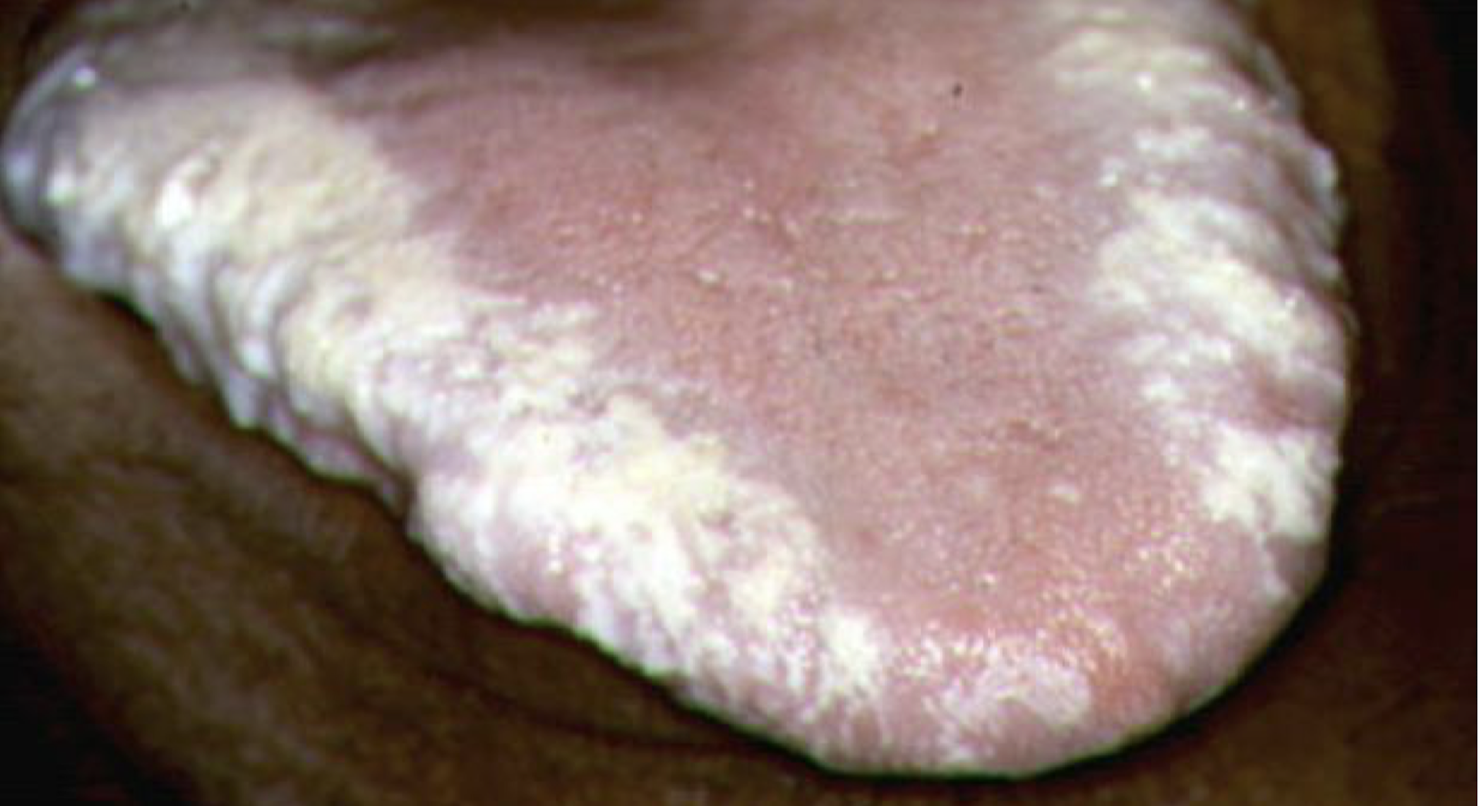
what is this lesion called and what virus is it associated with
oral hairy leukoplakia
Epstein-Barr virus
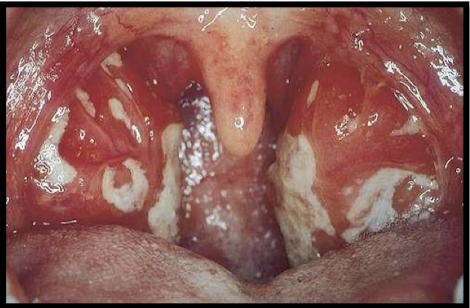
what is this associated with
pharyngitis and tonsilitis
infectious mononucleosis/glandular fever
epstein barr virus
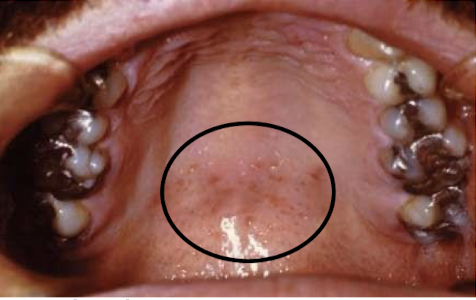
what are these lesions associated with
Infectious mononucleosis/glandular fever
Epstein Barr Virus
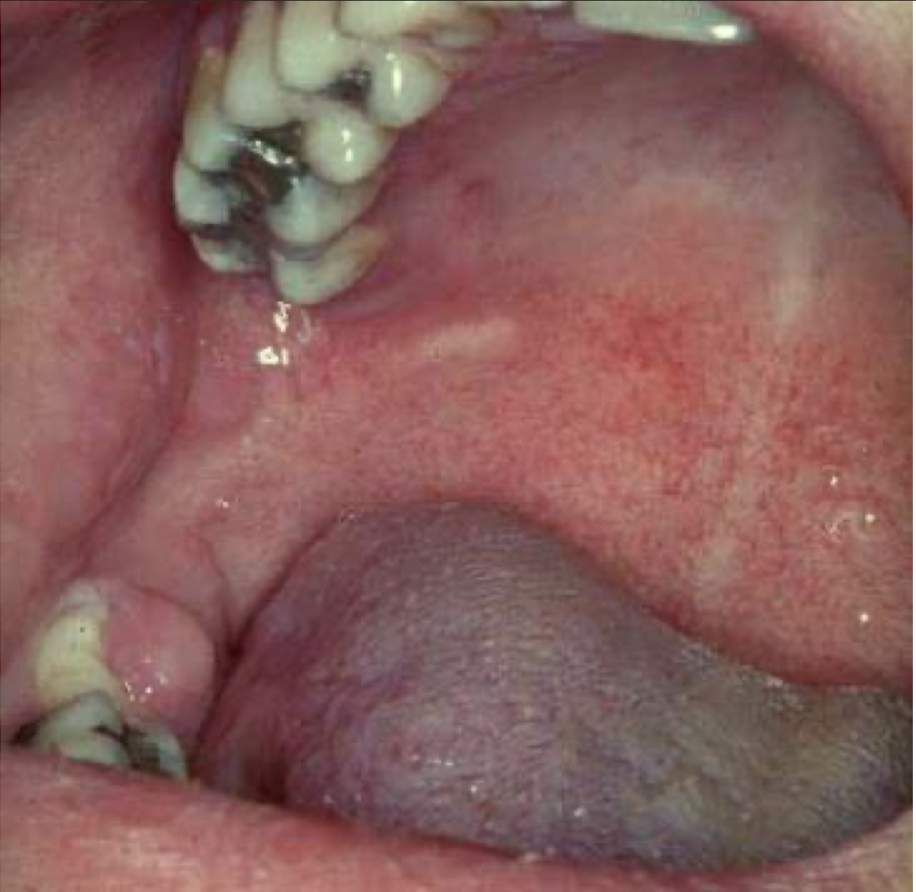
what are these lesions associated with
Rubeola/measles
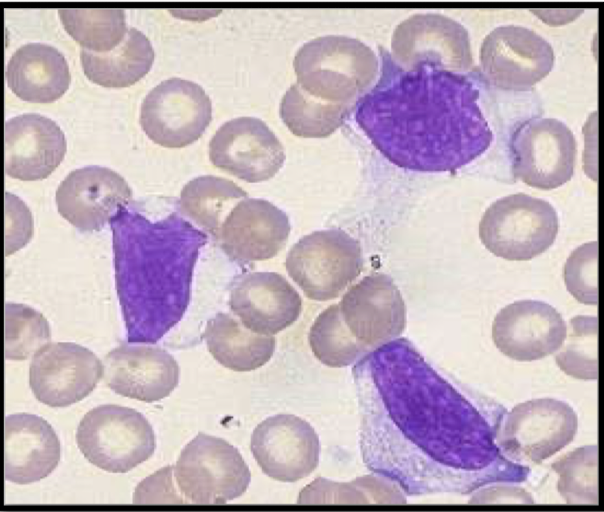
what are these cells and what are they associated with
Downey cells - atypical lymphocytes
infectious mononucleosis/EBV
Viral infections causing oral ulceration
HSV-1, HSV-2, Varicella zoster virus
Human herpes viruses list
HSV-1, HSV-2, VZV (HHV-3), CMV, EBV (HHV-4), HHV-6, HHV-7, HHV-8
HSV-1 common locations
Above the waist
HSV-2 common infection
Genital infection, venereal transmission, mother to newborn
Peak age of primary HSV-1 infection
2–3 years
Herpetic whitlow definition
HSV infection of fingers from direct contact (e.g., dentist without gloves)
Prodromal symptoms of primary oral herpes
Fever, headache, malaise, nausea, vomiting (1–2 days before)
Initial lesion of primary oral herpes
Small thin-walled vesicles like drops of dew on inflammatory base
What happens to HSV vesicles
They rupture → shallow round ulcers → coalesce into larger irregular lesions
Key diagnostic sign of primary HSV
Generalized acute marginal gingivitis with edematous inflamed gingiva
Vesicle size in HSV lesions
1–3 mm diameter
HSV intraoral predilection site
Heavily keratinized gingiva
Acute herpetic gingivostomatitis age
6 months – 5 years (peak 2–3 years)
Why HSV rare before 6 months
Maternal anti-HSV antibodies protection
Systemic signs of acute herpetic gingivostomatitis
Anterior cervical LN, chills, fever 103–105°F, sore throat, malaise, headache
Location of vesicles in acute herpetic gingivostomatitis
Tonsils and posterior pharynx
Recurrent HSV definition
Reactivation of latent virus, not reinfection
Triggers for recurrent HSV
Trauma, fever, immunosuppression, menstruation
Lab diagnosis cytology finding HSV
Multinucleated giant cells and ballooning degeneration
Stains used for HSV cytology
Giemsa, Wright’s, Papanicolaou
Most definitive HSV test
Virus isolation in tissue culture
Antibody titer significance in HSV
4-fold rise indicates primary infection
Drug of choice for HSV
Acyclovir within 72 hours
Acyclovir dose systemic HSV
400 mg TID for 7 days
Topical acyclovir concentration
5% ointment every 3 hours during day
Topical anesthetic for HSV
Dyclonine hydrochloride 0.5%
Diphenhydramine mixture for HSV
Diphenhydramine 5 mg/ml + milk of magnesia
What must be avoided in HSV
Corticosteroids contraindicated
Supportive care HSV
Analgesics, hydration, antipyretics
Drugs reducing HSV pain
Gabapentin, carbamazepine, phenytoin
Mechanism of acyclovir
Incorporates into viral DNA and stops chain elongation
Other antivirals for HSV
Valacyclovir, vidarabine
Coxsackie virus type
RNA virus
Coxsackie groups
Group A and Group B
Oral infections mainly caused by
Coxsackie Group A
Three Coxsackie oral diseases
Herpangina, Hand-foot-mouth disease, Acute lymphonodular pharyngitis
Herpangina season
June to October epidemics
Herpangina age
3–10 years
Herpangina incubation
2–10 days
Herpangina symptoms
Fever, chills, anorexia, sore throat, dysphagia
Herpangina lesion sites
Posterior pharynx, tonsils, faucial pillars, soft palate
Herpangina less common sites
Buccal mucosa, tongue, hard palate
Herpangina ulcer size
1–2 mm ulcers after rupture
Cytology difference herpangina vs HSV
No multinucleated giant cells or ballooning degeneration
Herpangina treatment
Self-limiting, hydration, topical anesthesia
Acute lymphonodular pharyngitis virus
Coxsackie A10
Lesion in lymphonodular pharyngitis
Yellow-white nodules, no vesicles or ulcers
HFMD (hand foot and mouth disease) oral findings
Vesicles and ulcers
HFMD skin findings
Non-pruritic macules, papules, vesicles on hands and feet extensor surfaces
HFMD complications
CNS involvement, myocarditis
VZV other name
HHV-3
VZV primary disease
Chickenpox (varicella)
VZV reactivation disease
Shingles (herpes zoster)
Chickenpox incubation
14 days
Where VZV remains latent
Dorsal root ganglia and cranial nerve ganglia
Who gets herpes zoster
Elderly, immunosuppressed, HIV, immunosuppressive therapy
Herpes zoster prodromal period
2–4 days pain/tingling
Herpes zoster lesion pattern
Unilateral vesicles along single dermatome
Healing time herpes zoster
Scab in 1 week, heals in 2–3 weeks
Most common complication HZ (herpes zoster)
Post herpetic neuralgia (PHN)
Oral HZ involvement
Division of trigeminal nerve
Ramsay Hunt syndrome definition
Geniculate ganglion HZ + Bell’s palsy + ear and oral vesicles
Topical Post-herpetic neuralgia relief
Lidocaine, capsaicin
EMLA cream use
Topical anesthetic for PHN
Capsaicin mechanism
Depletes substance P neurotransmitter
Drugs for PHN
Amitriptyline, nortriptyline, doxepin, desipramine
Most reliable VZV test
Fluorescent antibody stained smear
VZV antiviral dose
Acyclovir 800 mg five times/day for 1 week
EBV other name
HHV-4