ANAT 335 Exam 3
1/25
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
26 Terms
Myocardium
cardiac muscle cells
Cellular structure of cardiac muscle
striations from regular arrangements of myofibrils (sacromeres)
branched at ends usually
intercalated disks: provide mechanical and electrical connections between cardiac muscle cells
desmosomes
gap junctions
cardiac muscle is a functional syncytium (many cells acting as one)
Cardiac desmosomes
at intercalated disks and provide structural support (spot welds)
Cardiac gap junctions
at intercalated disk and have protein channels linking the cytosols of adjacent cells; small molecules like ions can quickly pass from cell to cell
Excitation-Contraction (EC) coupling in cardiac muscle
Excitation: electrical signal (action potentials)
EC coupling: chemical signals (intracellular Ca2+ release or Ca2+ transient)
Contraction: mechanical signal (contraction)
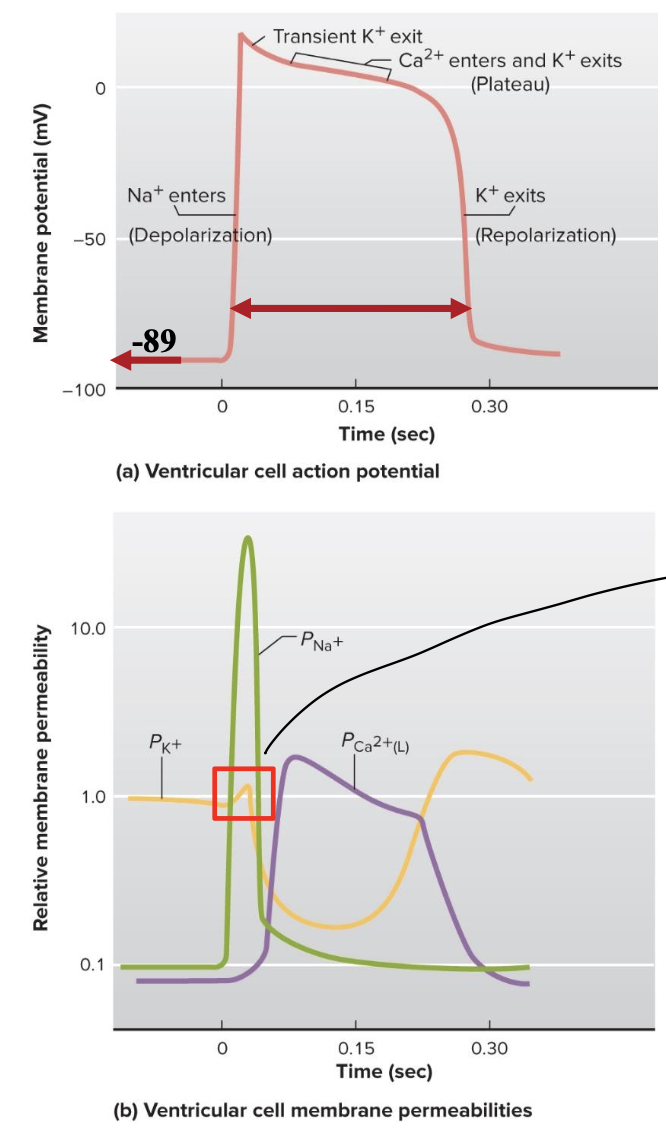
Excitation= action potential in a ventricular cardiac cell
very negative resting membrane potential (-89mV) due to lots of K+ leak
current enters from neighboring cell through GAP junctions (these replace need for graded potentials)
rapid opening of voltage gated Na+ channels is responsible for the rapid depolarization phase
prolonged plateau of depolarization is due to slow, prolonged opening of voltage-gated Ca2+ channels (L-TYPE CHANNELS)
slower opening of voltage-gated K+ channels is responsible for the repolarization phase
long duration of action potential due to L-type channels
L-type channels
L=long lasting
slow prolonged opening of voltage gated Ca2+ channels and same thing as DHPRs in t-tubule
cause plateau of depolarization
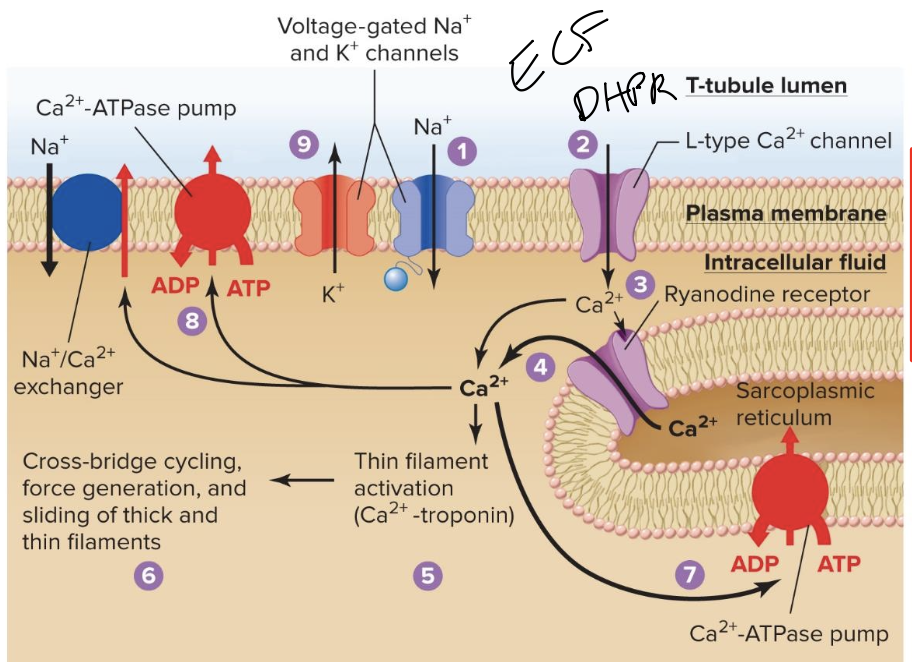
Steps of excitation
The membrane is depolarized by Na+ entry as an action potential begins= excitation, no neuronal input is required
Depolarization opens L-type Ca2+ channels in T-tubules
small amount of “trigger” Ca2+ enter the cytosol, contributing to cell depolarization. That trigger Ca2+ binds to and opens ryanodine receptor Ca2+ channels in sarcoplasmic reticulum membrane
Ca2+ flows into the cytosol, increasing Ca2+ concentration
Binding of Ca2+ to troponin exposes cross bridge binding sites on thin filaments
cross bridge cycling causes force generation and sliding of thick and thin filaments (contraction)
Ca2+-ATPase pumps return Ca2+ to the sarcoplssmic reticulum
CA ATPase pumps and Na/Ca exchangers remove Ca from the cell
The membrane is repolarized when K+ exits to end the action potential
Timing of action potentials in cardiac muscle
prolonged refractory period prevents tetanus of cardiac muscle
can not summate force in cardiac muscle, this allows time for ventricles to relax and fill with blood prior to the next heartbeat
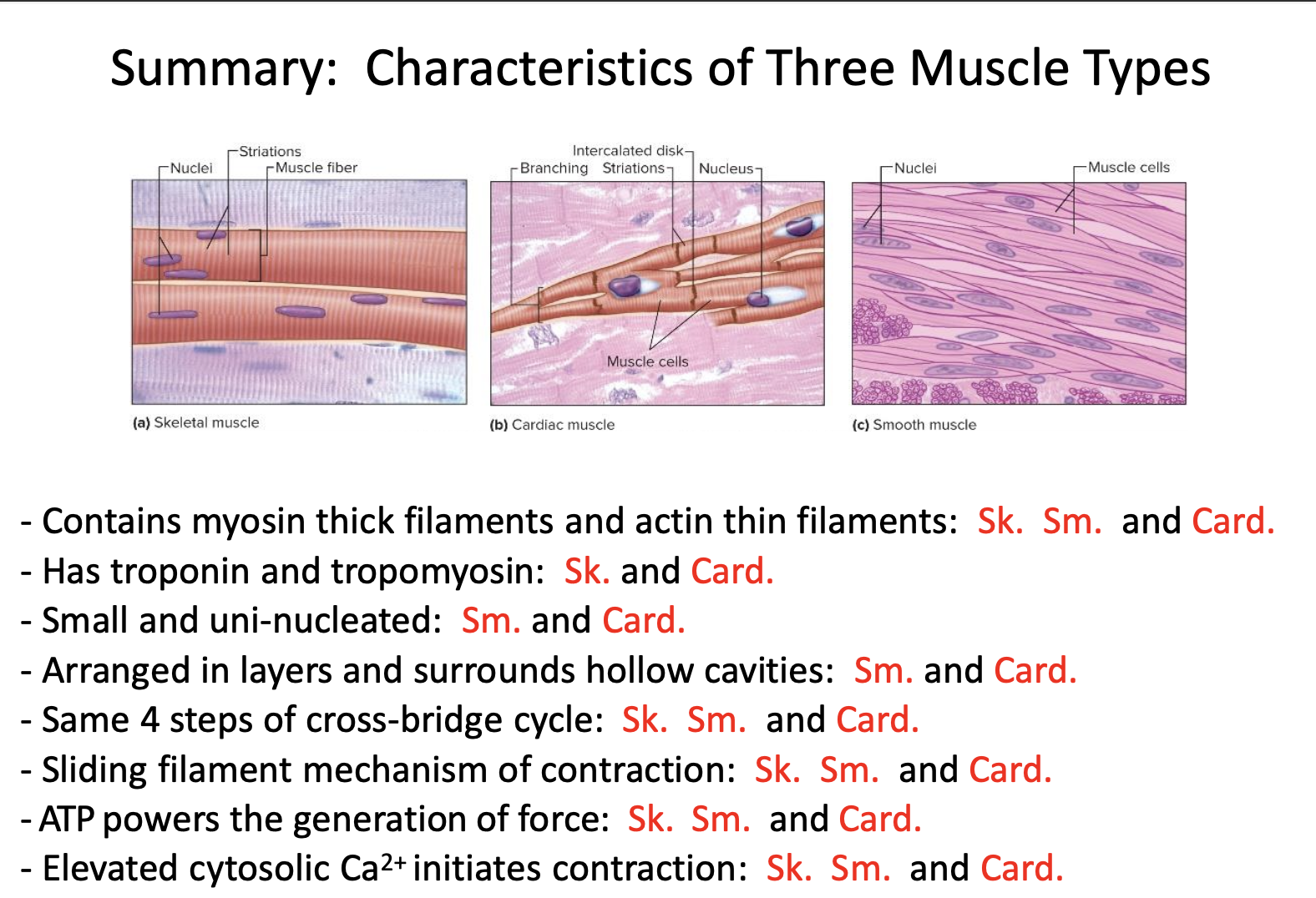
Summary of muscle types table
Cardiovascular system attributes
role in homeostasis is the main transport system
we need circulatory system because diffusion of solutes 100 micrometers or more would be too slow and inefficient
has three parts: heart, blood vessels, and blood
Heart
the biological pump; generates force to move blood; 2 parts (electrical and mechanical)
Blood
the fluid connective tissue through which O2/CO2/wastes/ nutrients and messengers like hormones are transported
Blood vessels
the “tubing” through which blood flows; they play and active role in the movement of blood
Parts of blood
total blood volume ~5.5L
Plasma is 55% (~3.0L) part of ECF, least dense “lightest”
“Buffy coat”: has WBC and platelets; insignificant volume, middle of centrifudge
RBC/hematocrit is ~45% (2.5L). Mainly involved in gas transport. Heaviest layer
Erythrocytes (RBC)
biconcave disks
large surface area for smaller volume
7 micrometer in diameter
carries hemoglobin
organelles are extruded (no DNA, DNA in buffy coat)
Blood differentiation
Reticulocyte differentiates into RBC for oxygen transport
Megakaryocyte differentiates into platelets for clotting
Promyelocyte differentiates into WBC for immunity defense
Bone marrow lymphocyte precursor differentiates into B and T lymphocytes for immunity defense
Components of the circulatory system
2 pumps and 2 circulatory systems (heart is a dual pump)
systemic circulation is out in the body
pulmonary circulation is the blood going to and coming from lungs
artery: carries blood away from the heart
vein: carries blood towards the heart
left side of heart is thicker than right because left pumps to systemic circulation
perfusion: passage of blood through a vascular bed; blood moves by bulk flow from high to low pressures
most vascular beds are in parallel, but pulmonary circulation is in series
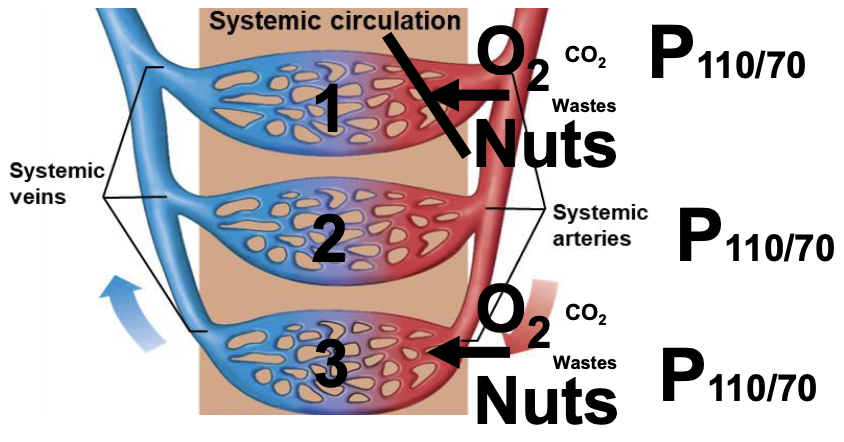
Capillary beds in series vs parallel
most beds are in parallel because this means equal amounts of O2, nutrients and waste go through the capillaries
in series the capillary at the end would have barely any nutrients and be mostly wastes
Endothelium
inside part of myocardium lining the chambers
Pericardium
outside part of heart
the pericardial space/fluid is between pericardium and myocardium
Types of cardiac muscle cells
pacemaker cells
conducting cells
contractile cells
pacemaker cells
small fraction of cardiac muscle cells that have automaticity; SA node normally determines the heart rate
SA node: 100-120 APs/min
AV node: 60-80 APs/min
Conducting cells 30-50 APs/min
Conducting cells
techinally all cardiac cells are conducting cells because they all conduct potentials
small fraction are specialized to rapidly spread the electrical stimulus throughout the chambers
bundle of HIS, right and left bundle branches, and Purkinje fibers
Contractile cells
99% of cardiac muscle cells whose activity allows blood to be pumped out of the heart